Abstract
Objective
To identify the prognostic factors for local recurrence of giant cell tumor of bone (GCTB) through assessment of the preoperative imaging features of the tumor border.
Methods
Patients with GCTBs treated with intralesional procedures in the proximal tibia and distal femur were prospectively enrolled and then followed up for at least 2 years. The GCTBs were grouped according to their preoperative imaging features. GCTBs treated with en bloc resection were enrolled for investigation of the pathologic basis of specific imaging features. Differences between rates were evaluated by the chi-square test or Fisher’s exact test; independent factors were identified by multivariate logistic regression analysis.
Results
Fifty-three patients were enrolled and successfully followed up. Relapse occurred in 22 patients. Patients with a “paintbrush borders” sign (n = 21) had a significantly higher rate of local recurrence (71.43%) than patients without this sign (21.88%). The “paintbrush borders” sign was identified as an independent prognostic factor for local recurrence. Other imaging features were not significantly associated with recurrence. The “paintbrush borders” sign showed a correlation with local invasion of bone.
Conclusion
The “paintbrush borders” sign on preoperative magnetic resonance imaging is an independent prognostic factor for local recurrence of GCTB.
Keywords
Introduction
Giant cell tumor of bone (GCTB) is one of the most prevalent bone tumors, accounting for 20% of all musculoskeletal tumors in East and Southeast Asia compared with approximately 5% in Western countries.1,2 GCTB exhibits locally destructive behavior that leads to significant osteolysis,3,4 and it is mainly treated with curettage. As an intermediate tumor with a tendency for local invasion, GCTB treated with curettage has a high rate of local recurrence (13%–65%) and thus poses a great challenge for clinical treatment.5,6
Prognostic factors for local recurrence play a key role in the preoperative planning of surgical procedures. We reviewed the literature regarding prognostic factors for local recurrence of GCTB but obtained far too few reliable results. Authors seldom draw unanimous conclusions, and the prognostic factors for GCTB remain ambiguous and controversial. Previously reported prognostic factors include age,5,7 location, 2 Campanacci classification,8,9 soft tissue extension,6,10 and pathologic fracture. 11 However, all of these disease-related factors were excluded in other equivalent studies.12–15 Additionally, most of these studies were retrospective with limited sample sizes.
The presence of a residual tumor after surgery has been considered responsible for recurrence 6 ; therefore, the imaging features of the tumor border, which are potentially associated with the liability of the residual tumor, are worthy of clinical investigation. Medical imaging is a noninvasive method that can provide diverse information regarding GCTB, 16 including its characteristics and impact on surrounding regions. A radiographic classification of bone tumor margins has been developed.17,18 However, anatomic overlap can obscure abnormalities, and the classification has a limited capacity to evaluate soft tissue. Radiographs are limited to determination of the relationship between bone tumors and their surrounding structures and the extent of disease in the intact marrow cavity. 18 Magnetic resonance imaging (MRI) is especially valuable for evaluation of musculoskeletal tumors because of its heightened sensitivity to soft tissue disease and multiplanar image acquisition.19–21
In the present study, we investigated the preoperative imaging features of the GCTB border, including peritumoral edema, the “paintbrush borders” sign, bony ridges, and loss of the bone cortex. In accordance with some authors,16,22–24 we recommend establishment of a new and standardized evaluation system to investigate the prognostic factors of GCTB. The knee is the site of predilection for GCTB 12 and is a major weight-loading joint. Therefore, we investigated prognostic factors through prospective enrollment of patients with GCTB around the knee joint. The patients were followed up for at least 2 years. Furthermore, preoperative imaging features were investigated through their correlation with gross pathologic sections of surgical specimens.
Materials and methods
Patients
This study was approved by the institutional review board of our hospital, the methods were carried out in accordance with the relevant guidelines and regulations, and written informed consent was obtained from all patients for the use of their clinical and imaging data in this study. The study design is presented in Figure 1. The eligibility requirements were histopathologically confirmed GCTB; tumor location in the proximal tibia and distal femur; performance of intralesional curettage with polymethylmethacrylate (PMMA) packing, which is the preferred standard treatment for GCTB and is performed consistently by a subgroup of orthopedic specialists in our hospital; performance of MRI and computed tomography (CT) examination before surgery; and a follow-up duration of >2 years. Patients with GCTB were prospectively registered in this study from January 2005 to July 2015. Among them, patients with pathological fractures and soft tissue masses were excluded. Patients with GCTBs treated with en bloc resection were enrolled only for investigation of the pathologic basis of specific imaging features.
Flow chart of study design. *GCTB border, including peritumoral edema, the “paintbrush borders” sign, bony ridges, and loss of the bone cortex. GCTB, giant cell tumor of bone; CT, computed tomography; MR, magnetic resonance.
Imaging procedures
CT examinations were performed with a 64-slice CT scanner (LightSpeed VCT; General Electric Medical Systems, Milwaukee, WI, USA) according to a routine protocol. The bone window, soft tissue window, and two-dimensional acquisition were used for observation.
MRI examinations were performed on a 1.5-T superconducting whole-body imager (SIGNA; General Electric Medical Systems) with dedicated knee coils.
A combination of axial, sagittal, and coronal images was obtained using the following sequences: spin-echo T1-weighted (repetition time [TR] range/echo time [TE] range, 450–600 ms/15–20 ms), fast spin-echo T2-weighted (TR range/TE range, 3500–4000 ms/80–120 ms), and fat-suppressed fast spin-echo T2-weighted (TR range/TE range, 3500–4000 ms/80–120 ms). The field of view, slice thickness, and interslice gap varied depending on the diseased region and tumor size. The imaging matrix ranged from 192 × 256 to 256 × 256.
All patients routinely underwent anteroposterior and lateral plain radiographs for reexamination.
Objective features and groups
Preoperative imaging features, including peritumoral edema, the “paintbrush borders” sign, formation of bony ridges, and loss of the bone cortex, were observed in the axial, sagittal, and coronal planes.
Bony ridges were defined as focally thickened bone trabeculae or ridge formation on the bone rim, visible on CT scans. The bone window was effective for observation of bony ridges. Patients were classified into the positive group if bony ridges were found, regardless of the number of bony ridges.
GCTB margins are often relatively well-defined or show irregular penetration. The “paintbrush borders” sign was descriptively defined as the presence of penetrating irregular margins with a “paintbrush” appearance protruding toward the bone, visible on MRI. Because of the stark contrast between the high signal intensity of the bone marrow and the low signal intensity of tumor tissue, T1-weighted images more effectively showed irregular protrusions than did other sequences. Patients were classified into the positive group if the “paintbrush borders” sign was found, irrespective of the number or shape of the sign.
Peritumoral edema appeared as high signal intensity on fat-suppressed MRI and indicated the presence of joint effusion and edema. GCTBs were classified into two grades: grade A was defined as massive edema or significantly high signal intensity on fat-suppressed T2-weighted images, and grade B was defined as limited edema or minimally increased signal intensity on fat-suppressed T2-weighted images.
Cortical bone destruction can be detected by CT or MRI. In this study, loss of the bone cortex was defined as discontinuity (shown as low signal intensity) of the normally high-density bone cortex on the MRI bone window.
All these features were evaluated using noncontrast MRI/CT and interpreted by three senior musculoskeletal radiologists (Y.L., 17 years of experience; J.Z., 23 years of experience; and X.D., 25 years of experience). The radiologists discussed the findings until consensus was reached. If consensus could not be reached, the majority opinion was used for analysis. GCTBs were classified into positive and negative groups according to the preoperative imaging features.
Intralesional procedure
The intralesional procedure performed in each patient was explicitly recorded in the medical records. All 55 patients underwent intralesional curettage conducted by a senior orthopedic surgeon (J.X., 19 years of experience). A wide cortical window was created, and the tumor tissue was removed with a curette. The remainder of the tumor cavity was then eliminated with a high-speed burr. Phenol was applied in the borders of the cavity with a cotton-tipped applicator and then neutralized with alcohol in 31 patients; the remaining 24 patients were treated without an additional adjuvant. Finally, the tumor cavity was carefully packed with PMMA filling.
Follow-up and recurrence
All patients underwent annual reexamination by X-ray or MRI regardless of whether they were symptomatic. Patients who were unable to be re-examined in our hospital were followed up by telephone, letter exchange, or in-person visits. All patients were followed up for at least 2 years.
Extension of the radiolucent zone on radiographs after bone cement filling was a reliable indicator of possible local recurrence. The recurrent tumor, which was represented by high signal intensity around the PMMA on T2-weighted imaging, could be directly identified. The patients were immediately re-examined if any tumor-associated symptoms (abnormal pain and swelling) occurred after surgery. Recurrent GCTBs were diagnosed by pathological results. Follow-up could be halted if the GCTB recurred.
Correlation with pathology
Surgical specimens were obtained from two patients treated by en bloc resection. According to the acquired images, formalin-fixed, paraffin-embedded specimens were sectioned and stained with hematoxylin and eosin.
Statistical analysis
Statistical analysis was performed using SPSS Statistics for Windows, Version 22.0 (IBM Corp., Armonk, NY, USA). Categorical variables are presented as percent and absolute number of patients. The distributions of the frequencies of dichotomous attributes in each group were assessed using the chi-square test or Fisher’s exact test, as appropriate. Independent factors were identified by multivariate logistic regression analysis. All P values were two-sided, and a value of <0.05 was considered statistically significant.
Results
Patient characteristics
Sixty-seven consecutive patients prospectively registered in this study. Among them, five patients with pathological fractures and four patients with soft tissue masses were excluded. Therefore, 58 patients were eligible for this study (30 men and 28 women; median age, 29 years; age range, 18–64 years). The patients were grouped according to their preoperative imaging features (Figures 2–4), including peritumoral edema, the “paintbrush borders” sign, bony ridges, and loss of bone cortex. The characteristics of all patients are detailed in Table 1.
A 59-year-old man with a giant cell tumor of bone in the proximal tibia treated with curettage. No sign of recurrence was found after 9.5 years of follow-up. (a) Axial computed tomography shows spine-like high-density bony ridges (white arrows). (b) Coronal and (c) sagittal T1-weighted images show the “paintbrush borders” sign, characterized by protrusions (black arrows) extending toward the bone from the edge of the tumor. (d) Sagittal fat-suppressed T2-weighted image shows minimal and limited peritumoral edema, which was classified as grade B in this study. Patient characteristics.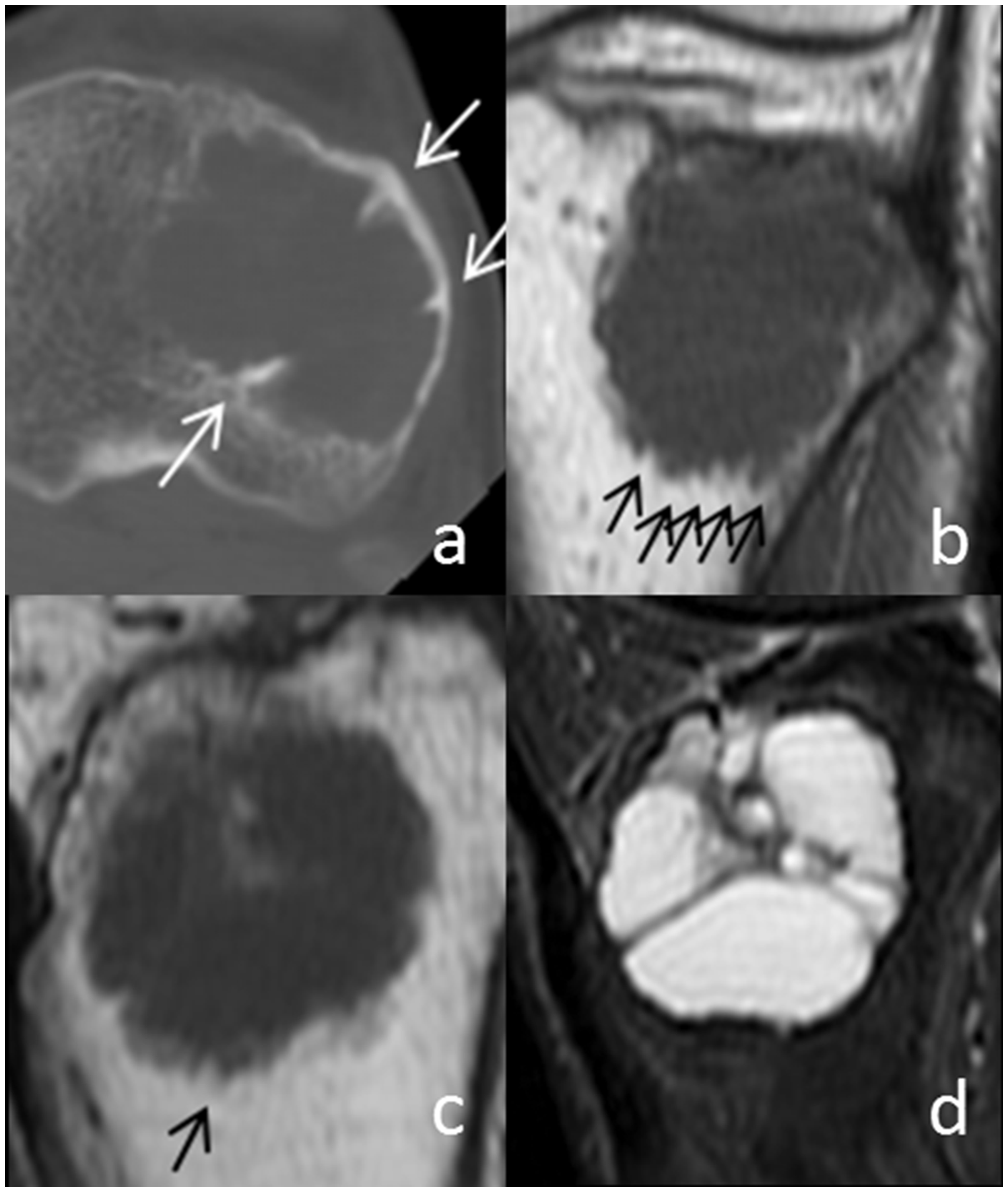

Follow-up and local recurrence
Fifty-three patients (91.38%) were followed up successfully, while five patients were lost to follow-up. Twenty-two patients (43.75%) were finally diagnosed with recurrence (average time of recurrence, 22.82 months), of whom 19 patients (86.36%) developed recurrence within 2 years (average, 15.05 months). For the remaining three patients with recurrence, the time of recurrence was beyond 2 years (during the fifth year postoperatively in two patients and during the eighth year postoperatively in one patient). For the patients without recurrence, the follow-up period ranged from 2.0 to 9.5 years (average, 5.61 years).
Prognosis of local recurrence
Analysis of factors influencing local recurrence.

Statistically significant difference (P < 0.05).
Multivariate logistic regression analysis of risk factors for local recurrence.

Statistically significant difference (P < 0.05).
B, regression coefficient; df, degree of freedom; Exp(B), exponentiated regression coefficient
Control of confounding factors
Twenty-nine of 31 patients treated with additional adjuvants were successfully followed up. The recurrence rates were not significantly different between the patients with and without an additional adjuvant. The recurrence rates were also not significantly different between the patients enrolled in earlier years and those enrolled in later years (Table 2).
Comparison of preoperative imaging features with pathology
Gross pathologic sections were made and visually matched with the acquired images. The lengths of the protrusions varied from 1.5 to 3.6 mm on MRI, according to our database. In one of the patients who underwent en bloc resection, the lengths of the protrusions varied from 1.2 to 3.3 mm on gross pathologic sections and from 1.6 to 3.2 mm on MRI. Multinucleated giant cells were uniformly distributed among monocytes within the protrusions (Figure 4), and the “paintbrush borders” sign on preoperative MRI correlated with the gross pathologic sections (Figure 5). In addition, bony ridges and loss of the bone cortex were clearly observed on CT. However, edema could not be evaluated because the pathological sections were dehydrated.
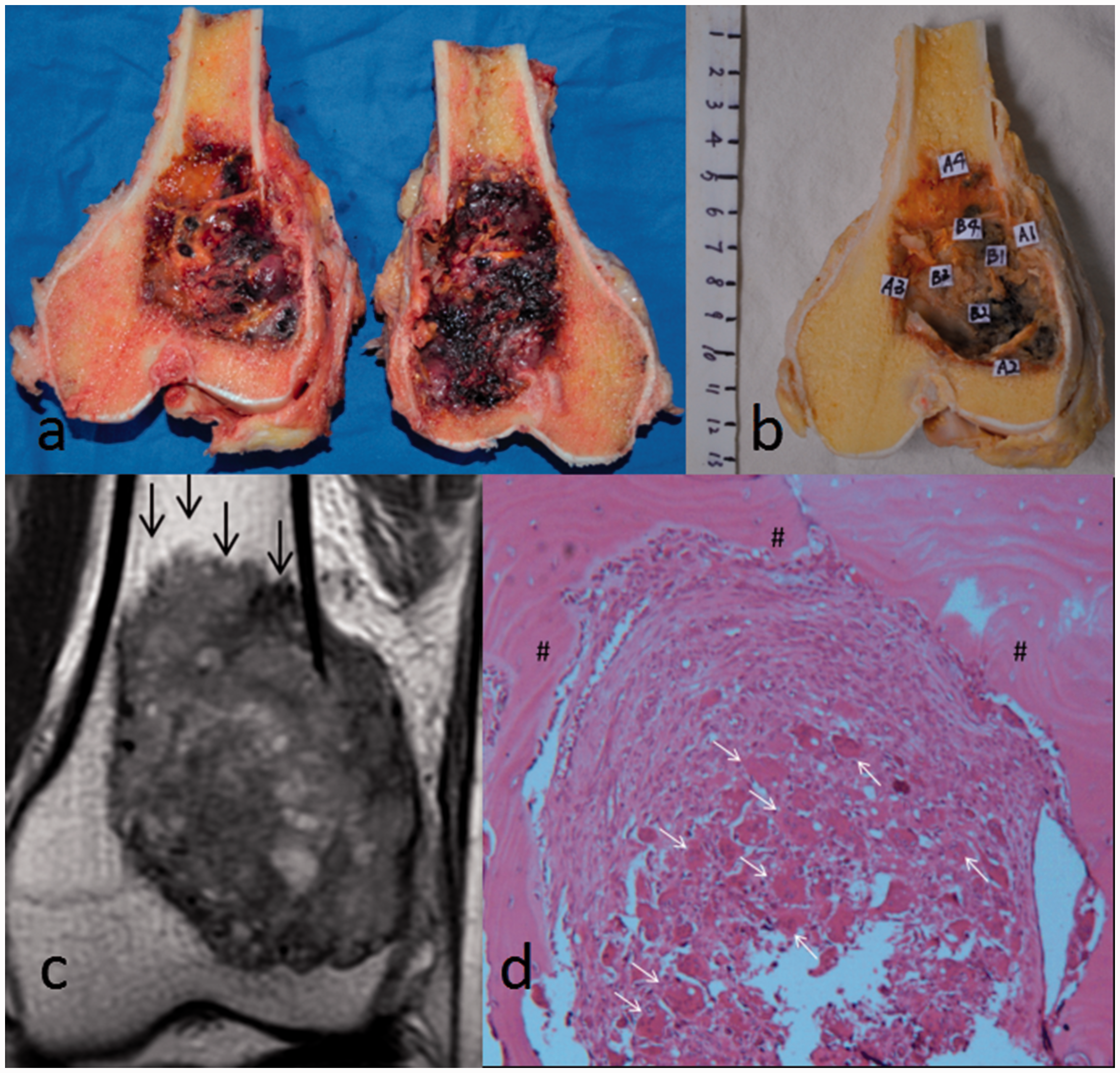
A 64-year-old woman with a 6-month history of knee pain. Local recurrence was confirmed after 1 year of follow-up. (a) Coronal T1-weighted image shows “paintbrush-like” irregular margins protruding toward the bone (black arrows). (b) Coronal fat-suppressed T2-weighted image shows massive peritumoral edema and joint effusion (white arrows), which was classified as grade A in this study. (c) Sagittal T2-weighted image shows a homogeneous region with high signal intensity (white arrows) indicating local relapse in the region of the penetrating irregular margins. (d) The surgical specimen was dissected to examine its correlation with the sagittal image, and recurrent tumor tissue as confirmed around the bone cement. A 23-year-old woman with a giant cell tumor of bone treated with en bloc resection. (a, b) The surgical specimen was dissected to examine its correlation with the coronal image, and pathological samples were taken from this coronal section. (c) Coronal T2-weighted image shows the “paintbrush borders” sign at the upper aspect of the tumor (black arrows). (d) Photomicrograph (label A4 in Figure 4(c)) shows the tumor histology with typical multinuclear giant cells (white arrows) among numerous mononuclear cells protruding toward the bone tissue (#) (hematoxylin–eosin stain; original magnification, 100×).
Discussion
This study is the first to identify the MRI feature of the “paintbrush borders” sign as an independent prognostic factor for local recurrence of GCTB after intralesional curettage. This sign, which is characterized by marginal infiltration on MRI, pathologically confirmed to represent invasion of bone around the tumor.
Intralesional procedures are a preferred approach to GCTB but are challenged by local recurrence. Residual tumor tissue is associated with local recurrence after surgery and is a vital concern when performing intralesional procedures.5,6 This inspired us to focus on the MRI and CT features of the tumor border to explore prognostic factors associated with residual tumors. However, despite the fact that the Lodwick grading system and modified Lodwick–Madewell grading system are well established, our literature review revealed no studies evaluating the preoperative MRI features of the border of GCTBs. 25 The present study is the first to evaluate the association between the preoperative MRI features of the border of GCTBs and the prognosis of these tumors.
The “paintbrush borders” sign is a common feature that can be found on conventional MRI but has been neglected in previous studies. This sign should be correlated with pathological findings to determine its clinical value. Therefore, we explored the pathologic basis of the “paintbrush borders” sign on MRI and found osteoclastic giant cells uniformly distributed among monocytes within the protrusions. Gross pathologic sections showed that the “paintbrush borders” sign represented invasion of bone around the lesion. The gross pathologic sections visually matched the specific findings on the images.
Invasion of bone around a GCTB could be interpreted as one cause of residual tumors. The penetrating irregular margins might decrease the effect of intralesional treatment. We have herein provided reliable evidence to substantiate the viewpoint that residual tumors may be a major culprit in local recurrence and identified the “paintbrush borders” sign as an independent prognostic factor for local recurrence of GCTBs. When penetrating irregular margins are detected by MRI in the clinical setting, surgeons should consider the presence of a GCTB and make every effort to thoroughly eliminate residual tumor tissue in the region of the irregular protrusions. This prospective study of GCTBs has provided evidence that inclusion of this novel sign on preoperative MRI might help to guide surgical treatment and reduce local recurrence.
With respect to the molecular prognostic factors of GCTB, the expression of some osteolysis-associated factors might be elevated in GCTB with the “paintbrush borders” sign. It can be reasonably speculated that osteoclast activity and its related factors, such as the receptor activator of nuclear factor kappa-B ligand (RANKL)/RANK/osteoprotegerin signaling pathway, matrix metalloproteinases, and tumor necrosis factor-α, might be pivots between osteolysis/formation of the “paintbrush borders” sign and local recurrence. In one study of bone malignancies, nuclear factor I-B, RANK, and RANKL co-overexpression was identified as a potential discriminating factor of a poor prognosis. 26 Kumta et al. 27 demonstrated that matrix metalloproteinase 9 expression in GCTBs was well correlated with local recurrence. Further research is required to clarify these findings.
Unexpectedly, the other three peripheral features (bony ridges, peritumoral edema, and loss of the bone cortex) failed to predict outcomes. This could be explained as follows. 1) Although bony ridges cause difficulty performing curettage, they can be worn smooth with a high-speed burr, substantially reducing their clinical impact. 2) Theoretically, peritumoral edema is a reaction to the tumor activity and is associated with the aggressiveness of GCTB. Based on our negative result, however, we speculate that many confounding factors, such as osteosclerosis, also play roles in the development of edema. 3) Loss of the bone cortex is a result of the aggressiveness of GCTB. Additionally, Chen et al. 10 demonstrated the role of soft tissue masses in prognosis of GCTB. However, we did not arrive at the same conclusion in terms of loss of the bone cortex. In the early stage before the formation of a soft tissue mass, adjacent bone invasion is more amenable to clinical treatment. Surgeons should always select a bone window containing loss of the bone cortex or a thinner bone cortex to perform surgery.
The impact of demographic factors on local recurrence is also an important factor associated with clinical management. Siddiqui et al. 2 reported that local recurrence of GCTB in the proximal tibia (recurrence rate of 60%) is higher than that in other locations. This could explain why our overall recurrence rate (43.75%) seems extremely high. However, the higher rates of local relapse in the proximal tibia were mostly derived from statistical analyses without convincing investigations to explain these findings. Kivioja et al. 7 reported age as a prognostic factor for local recurrence of GCTB and found a correlation between higher age and lower local recurrence rates. These findings coincide with those obtained by Klenke et al., 5 who reported that age was an independent risk factor for recurrence regardless of the disease status and chosen treatment. In the current study, however, we did not reach the same conclusions regarding the role of these demographic factors.
We consider the present investigation to be a standardized study in terms of the following two aspects. First, we enrolled patients with GCTBs around the knee to exclude the impact of the tumor site. Second, the surgical procedures were consistent among all patients.
However, the application of phenol and the long duration of this prospective study probably interfered with the investigation and might be considered confounding factors. To control for confounding factors, the impact of the application of phenol on the prognosis was excluded by the correlation analysis. Klenke et al. 5 reported that local phenol use did not improve recurrence-free survival. On the other hand, the local recurrence rates in the former and latter years were 43.48% and 40.00%, respectively, with no significant difference.
GCTB is generally known to recur within 2 years28,29; therefore, our follow-up period was set at >2 years. Of the 22 patients with recurrence, 19 (86.36%) patients developed recurrence within 2 years (average, 15.05 months), and the remaining 3 patients developed recurrence after the 2-year follow-up (2 developed recurrence in the fifth year postoperatively, and 1 developed recurrence in the eighth year). For the patients without recurrence, the follow-up duration ranged from 2.0 to 9.5 years (average, 5.61 years).
This is the first study to evaluate the role of the MRI features of the tumor border in predicting local recurrence of GCTB. However, the study has some limitations. The main limitation is that although this single-center study was standardized by enrolling only patients with GCTB around the knee, the number of patients with GCTB was relatively small. To the best of our knowledge, however, the GCTBs mainly recurred within 2 years. We cannot exclude the possibility of long-term recurrence without extending the study duration.
In conclusion, the MRI feature of the “paintbrush borders” sign was discovered as an independent prognostic factor for local recurrence of GCTB. Pathologically, penetrating irregular margins on preoperative MRI were correlated with bone invasion around the GCTB. Careful evaluation of the GCTB border by MRI might help to raise surgeons’ awareness about the risk of penetrating irregular margins and guide surgical treatment to ensure thorough elimination of residual tumors in the region of the protrusions.
Footnotes
Authors’ contributions
Guarantor of the integrity of the entire study: Xiaoyi Ding Study conception: Xiaoyi Ding, Yifeng He Study design: Xiaoyi Ding, Yifeng He Literature search: Yifeng He, Lianjun Du Clinical studies: Yifeng He, Jianqiang Xu, Ji Zhang Experimental studies: Fei Yuan, Jun Wang, Ji Zhang Data acquisition: Yong Lu, Jun Wang, Yifeng He, Ji Zhang Imaging analysis/interpretation: Xiaoyi Ding, Lianjun Du, Yifeng He Statistical analysis: Yifeng He, Ji Zhang, Jun Wang Manuscript preparation: Yifeng He, Ji Zhang Manuscript editing: Yifeng He, Ji Zhang Manuscript revision/review: Xiaoyi Ding, Lianjun Du, Yong Lu
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
Funding was received from the Science and Technology Commission of Shanghai Municipality (Project Number: 134119a2402).
