Abstract
Objective
Exclusive breastfeeding is safe and beneficial for healthy infants; it is the optimal feeding method during the first 6 months of life. Infants should be complementary fed in conjunction with breastfeeding until 12 months of age or longer. The aim of the present study was to analyse the duration of breastfeeding through 12 months of age.
Methods
Participants were 1679 women from 42 randomly selected hospitals in Poland. The data were obtained from surveys, including a paper and pencil interview that was conducted after mothers delivered in the hospital and before discharge. Computer aided telephone interviews were administered at 2, 4, 6 and 12 months.
Results
There was a high rate of initiating breastfeeding after birth (97%), a rapid abandonment of exclusive breastfeeding (43.5% at 2 months, 28.9% at 4 months and 4% at 6 months) and an onset of formula feeding during the first days of life, which is contrary to current recommendations.
Conclusions
It is necessary re-educate mothers, medical staff who care for mothers and children during the perinatal period, and other specialists.
Keywords
Introduction
Breastfeeding is safe and beneficial for all infants, and is recommended by the World Health Organization (WHO) as the optimal way of feeding infants. 1 Exclusive breastfeeding during the first 6 months of life is recommended by the WHO and American Academy of Pediatrics (AAP).1,2 Infants should receive complementary food with continued breastfeeding from 6 months onwards. The Polish Society for Paediatric Gastroenterology Hepatology and Nutrition made recommendations for the nutrition of newborns and infants, including breastfeeding.3,4 This statement supports the recommendation of the WHO, AAP and the European Society for Paediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) and is adapted according to Polish conditions.3–5
There is abundant data available supporting the conclusions that hospital practices influence both the onset and continuation of breastfeeding after discharge.6–11 The Ten Steps to Successful Breastfeeding programme is carried out by Baby Friendly Hospitals, and guarantees a rise of exclusive breastfeeding rates. The WHO/UNICEF Baby Friendly Hospitals Initiative (BFHI) is implemented in every facility, and provides maternity services and care for newborn infants. It is provided in conjunction with governmental support and breastfeeding promotional action to achieve the same positive results seen in Sweden and other Scandinavian countries.6,12–14
The BFHI has only been implemented in 25% of Polish hospitals. This is because there is a lack of governmental breastfeeding promotion and support. However, there are non-governmental Polish organizations that promote successful breastfeeding. Breastfeeding promotion and support have not been provided by any Polish pro-health project over the last few years.
Since 2012, the Polish 10 Steps to Successful Breastfeeding programme has been associated with standards for maternal and neonatal care. All Polish facilities that provide maternity services and care for newborn infants are obligated to breastfeeding protection, promotion and support. However, official data for Polish infants’ nutrition, including breastfeeding and exclusive breastfeeding, are not gathered.
The aim of the present study was to analyse the breastfeeding rates of mothers of newborns and infants through 12 months of age. This study was based on a survey conducted with a representative population of Polish mothers who delivered healthy infants; all mothers delivered infants who were at least 37 weeks gestational age.
Material and methods
A total of 100 obstetric hospitals (out of over 400 functioning facilities) were randomly selected. These hospitals were invited to participate in the study titled Breastfeeding Newborns and Infants up to 12 Months of Life: An Assessment of Polish Lactation Practices as Part of Standards for Maternal and Neonatal Care.
The scientific project was accepted by the Nutricia Foundation, The Scientific Council of Foundation (PR 10/2013Z) and the Ethics Committee of Wroclaw Medical University (Nr 874/2012, 577/2013, 142/2014).
The research was conducted at 42 obstetric hospitals. The hospital managers and seniors registers of both obstetric and neonatal units accepted the conditions of the research. There were additional hospitals that did not respond to the invitation, or did not receive approval from their hospital managers to participate in the project.
The hospitals were surveyed by a market research company, TNS (Warsaw, Poland).
A paper and pencil interview was used during hospitalisation in the maternity units. Content and face validity of the questionnaire was established through piloting and revision with a group of new mothers hospitalised in University Hospital, Wrocław. Both questionnaire forms and ballot boxes (to return completed paper questionnaires) were delivered to hospitals by TNS. Mothers completed questionnaires without staff help; this approach minimized the influence of the staff on the survey. Physicians analysed medical records and the clinical status of both mothers and children. Only mothers who gave birth to healthy newborns after 37 weeks gestational age were interviewed. The survey was conducted from 31 March 2014 through 31 May 2015. A total of 1679 women were studied, and 1679 questionnaires were completed. Data were collected on the day of discharge from the hospital, which was the second day after vaginal delivery or the fourth day after caesarean section. Written consent was obtained from all participating women.
The questionnaire consisted of 20 questions. The first question asked about socioeconomic data, the subsequent course of childbirth and the clinical state of the newborn. The additional questions asked about mother and newborn care in the delivery room (skin-to-skin contact, time and period of the first breastfeeding) and maternity unit (rooming-in); there were also questions about breastfeeding and supplementary bottle-feeding.
Computer aided telephone interviews were used for next data collection (after 2, 4, 6 and 12 months). The study concluded in May 2015. The computer aided telephone interviews included multiple-choice items about infant nutrition, including exclusive breastfeeding and reasons for not breastfeeding.
Number of mothers participating in the study.

Results
Patient demographics
Mothers’ age, place of living, and education were analysed. The majority of the mothers were 25–35 years old (75% of respondents); 70% lived in cities, and 90% had completed secondary and university education.
Sociodemographic data of the mothers.

The survey and statistical analysis were conducted by TNS. The results included descriptive statistics; specifically, frequencies, arithmetic means and standard deviations are reported. Data were analysed using the IBM SPSS Statistics, version 19 (IBM Corp., Armonk, NY). There was consistency between the various components of the primary end point; however, significance was reached only for prevention. The t-test column proportions were used for significance testing.
Newborn feeding
Ninety-seven percent of women started breastfeeding in hospitals, and 55% of newborns were supplementary bottle-fed (both formula and breast milk). Ten percent of infants were fed glucose or water while waiting for mothers to breastfeed. Only 10% of newborns were supplementary bottle-fed with breast milk. Finally, 75% of newborns were exclusively breastfed at discharge.
Infant feeding at 2 months
At 2 months, 58% of infants were breastfed, but only 43.5% were exclusively breastfed. The majority of women who stopped breastfeeding did so during the first month after birth. The main reason women stopped breastfeeding was they thought their baby was not getting an adequate volume of breast milk (56%). In addition, 16% of mothers thought they were not producing enough milk, and switched to formula.
Infant feeding at 4 months
At 4 months, 41% of infants were breastfed, but only 28.9% were exclusively breastfed. Infants were either bottle-fed formula or received supplementary formula. Mothers indicated the following reasons for not exclusively breastfeeding: infants were not getting an adequate volume of breast milk (35%); infants lost interest in nursing or began to wean themselves (17%); or the mother’s breast milk supply ended (20%).
The majority of mothers stopped breastfeeding by the time their infant was 3 months old.
Infant feeding at 6 months
At 6 months, 38% of infants were breastfed, but only 4% were exclusively breastfed.
Sixty-two percent of mothers gave their infants pot meals: 51% were fed grain cereal for babies, and 45% of mothers introduced other solid meals. The most common reason for stopping breastfeeding was a mother’s sense that infants were not getting an adequate volume of breast milk.
Infant feeding at 12 months
Seventeen percent of infants were breastfed for 12 months. Food other than breast milk and formula was also introduced into infants’ diets. Most mothers introduced: other food (23%), grain cereal for babies (19%), meals for infants and toddlers (16%), and juice/herbal tea for infants (15%). For mothers who continued to breastfeed through 6–12 months, the average duration of breastfeeding was 40.3 weeks. (Figure 1)
Percentage of newborns and infants breastfed and exclusively breastfed through 12 months of life. Blue bars indicate breastfed. Red bars indicate exclusively breastfed.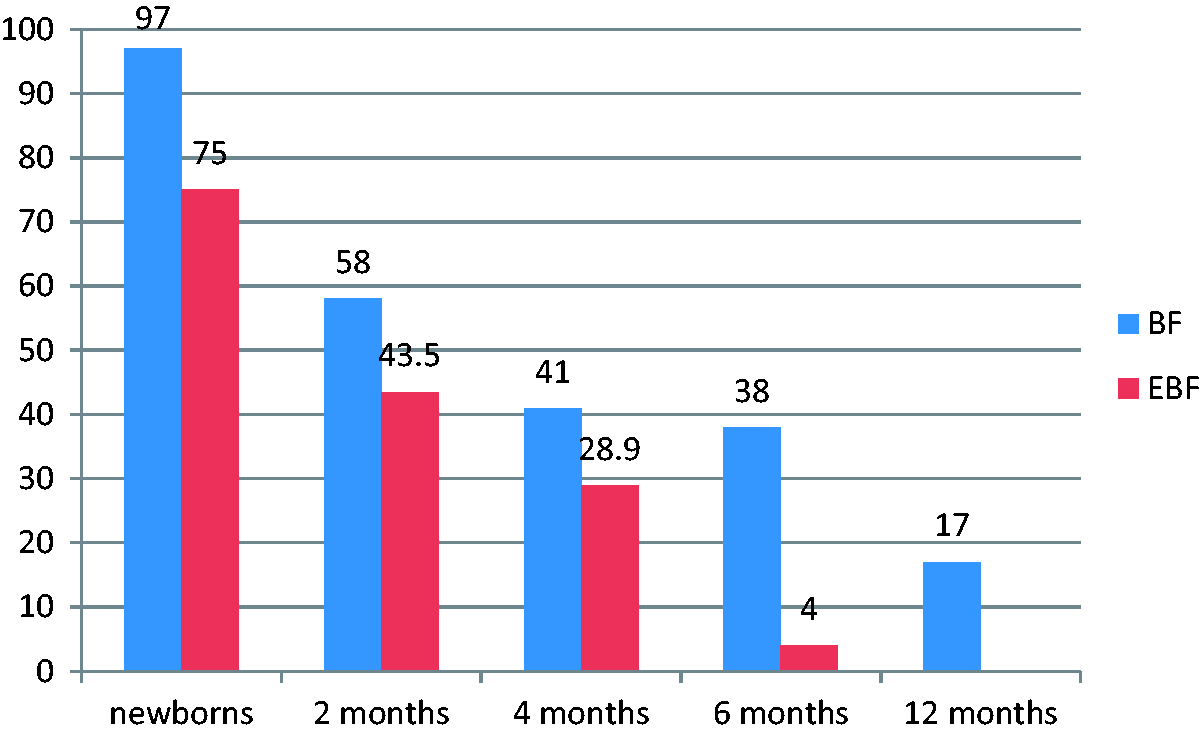
Women stopped breastfeeding for various reasons, including: concerns that infants were not getting an adequate volume of breast milk; infants lost interest in breastfeeding; and mothers needed to go back to work or school.
Discussion
The current study was conducted with a large, representative population of mothers from different types of obstetric hospitals in Poland. This is the first study about breastfeeding and infant nutrition during the first 12 months postpartum to be conducted in Poland in the last several years.
A study by Mikiel-Kostyra from 1997 showed that 92% of mothers started breastfeeding; however, only 68% exclusively breastfed their infants (exclusive breastfeeding was defined as no formula supplementation). 15 Cattaneo et al. 12 also conducted a study from 1998–2007, and demonstrated that less than 80% of Polish newborns were exclusively breastfed on hospital discharge day. A total of 134 mothers were also studied in 2007; this research showed that 97.7% of mothers started breastfeeding with a small sample, but 50% of newborns were supplementary bottle-fed formula. 16 In 2012, Bernatowicz- Łojko et al. 17 conducted a study in the Kujawsko-Pomorskie area and focused on the high rate (99%) of hospital breastfeeding initiation. Ninety-nine percent of neonates born at term were breastfed through the time they were discharged, but only 87% were exclusively breastfed. Only 65% of neonates born at term were exclusively breastfed during their time in the hospital. The majority of neonates born at term (74.6%) were supplementary bottle-fed on the first day of life. There were two main reasons for this: mothers’ request and doctors’ orders.
Mothers’ main reasons for supplementary bottle-feeding were: concerns that infants were not getting an adequate amount of breast milk (60%), and problems with infants’ latching and sucking technique (15%). [17]
In the current study, data were collected in 2014 from 1679 mothers of healthy infants, with a gestational age of at least 37 weeks. The results indicated that 97% of mothers started breastfeeding, which is consistent with previous research. Unfortunately, more than half of newborns were supplementary bottle-fed, primarily with formula, during hospitalisation. Despite the high percentage of women breastfeeding their infants at hospital discharge (97% of breastfeeding, 75% of exclusively breastfeeding), only 43.3% continued breastfeeding when their infants were 2 months old. Mothers indicated that they were concerned that their infant was not getting enough breast milk (60%); this was also the main reason for stopping breastfeeding when infants were 2 (55%) and 4 (57%) months.
A study by Bernatowicz- Łojko et al. 17 showed that 57% of infants at 4 months of age were exclusively breastfed, which is comparable to our own findings (62%).
In the current study, only 4% of mothers exclusively breastfed through 6 months, which is the recommendation of the WHO. In a study by Bernatowicz- Łojko et al., 17 14% of mothers exclusively breastfed until their infant was 6 months old; this is three times longer than the mothers who exclusively breastfed in the current study. Data collected by Bernatowicz-Łojko et al. were comparable to the European median (13%),12–14 while the data presented herein on exclusive breastfeeding at 6 months is consistent with research on European countries with lower breastfeeding rates (according to Bagci Bosi et al. 14 report); these countries include Greece (1%), Finland (1%) and the UK (1%).
A potential reason for the low rate of breastfeeding in the UK is that there is no national breastfeeding programme. Moreover, few British hospitals implement the Ten Steps to Successful Breastfeeding programme. 14
Polish breastfeeding practices do not comply with the National Maternal and Neonatal Care Programme/WHO recommendations; this is especially true for the rates of exclusive breastfeeding through first 6 months of life. Only 25% of Polish hospitals implement BFHI standards (www.laktacja.pl). Breastfeeding support interventions are associated with an increase in any and exclusive breastfeeding rates. 18 There is a lack of obligatory lactation training for Polish medical staff, both doctors and midwives. 19 Therefore, breastfeeding counselling should be reimbursed by the Polish National Health Service.
It is also important to note that some experts and advisory committees are not fully aligned with the WHO global recommendation for exclusively breastfeeding. For instance, ESPGHAN published a medical position paper on complementary feeding; they concluded that “exclusive breastfeeding for 6 months is a desirable goal and in any case complementary feeding should not be introduced before 17 weeks and not later than 26 weeks of life”. 4 This scientific opinion may have influenced Polish GPs and paediatric practices.3–5,15
The results of the current study indicate that 17% of infants were breastfed at 12 months, which is comparable to the results reported by Bernatowicz-Łojko (18%); however, it is dissimilar to European data.14,17
The WHO exclusively breastfed recommendations are important to consider. 6 In Poland, both the Infants Feeding Schedule from 2009 and the Polish Society for Paediatric Gastroenterology Hepatology and Nutrition recommendations from 2014 were applied during the data collection period.3,5
The implementation of education programmes on new infants feeding schedules and paediatricians’ monitoring of good feeding practices did not improve the percentage of exclusively breastfed infants. The last set of data indicates that exclusively breastfed rates decreased in Poland dramatically.
Currently, education for pregnant and breastfeeding women is provided by midwives (Polish perinatal care standards, antenatal schools), and should help improve the current rates. Reimbursement for lactation counselling may also be crucial.10,11,17,20,21
Health care professionals should recommend formula feeding only in special situations, and not routinely as appears to be the case in maternity units. Good nutrition is essential for growth and development during the first 12 months of life. When developing infants are fed with appropriate types and amounts of food, health is promoted. Caregivers’ positive and supportive feeding attitudes and techniques will help infants develop healthy attitudes toward foods, themselves, and others.
According to de Alameida et al., 21 a lack of professional support interventions for breastfeeding leads to dramatic reductions in breastfeeding. Midwives provide perinatal education, breastfeeding information and breastfeeding consultation to both pregnant and breastfeeding mothers. Proper nutrition according to the current Infants Feeding Schedule is essential for the growth and development that occurs during the first 12 months of life. Positive and supportive feeding attitudes help infants develop healthy attitudes toward food and affect health during adulthood. The cooperation is required between different health care professionals who know the current recommendations regarding infant nutrition, such as general practitioners, paediatricians and gynaecologists. Paediatricians, together with other professionals, can promote breastfeeding to ensure healthy nutrition and development.
Footnotes
Acknowledgments
We would like to thank the following individuals for their participation in and commitment to the project.
Klinika Neonatologii Uniwersytecki Szpital Kliniczny we Wrocławiu – A. Szczygieł, D. Paluszyńska;
SPZOZ w Świdnicy – A. Dziedzic;
Wojewódzkie Centrum Szpitalne Kotliny Jeleniogórskiej – R. Jaworska- Bobkier;
Szpital Powiatowy Sp. z o.o. Chełmża – I. Pachoń;
ZOZ w Brodnicy – T. Napiórkowska, M. Rutkowska;
SPZOZ w Łukowie – B. Koślacz;
Szpital Wielospecjalistyczny im. dr. Ludwika Błażka Inowrocław – R. Sobiechowska;
Uniwersyteckie Centrum Zdrowia Kobiety i Noworodka WUM – K. Balcerak, K. Płaza-Piekarzewska; Centrum Medyczne „Żelazna” w Warszawie – K. Osuch;
Centrum Dializa Sp. z. o. o. Sosnowiec, Szpital Pszczyna – B. Zięcina- Krawiec;
Samodzielny Szpital Kliniczny, CMKP – M. Wilińska;
WSS im. NMP w Częstochowie – J. Warzycha, M. Baryła;
SPZOZ Szpital Wielospecjalistyczny w Jaworznie – I. Pietruszewska;
Krapkowickie Centrum Zdrowia Sp. z o. o. – S. Kostka;
Specjalistyczny Szpital Wojewódzki Ciechanów – G. Salomon, J. Zuchora;
Szpital Rejonowy im. dr. Józefa Rostka w Raciborzu – G. Urban;
WSS im. F. Chopina Rzeszów – J. Gdula;
SPSK nr1 we Wrocławiu – M. Berghausen-Mazur;
Szpital Specjalistyczny im. A. Falkiewicza we Wrocławiu – A. Owczarek;
WSS we Wrocławiu-Oddział Neonatologiczny – E. Jasiak-Pałczyńska;
SPSK nr 4 w Lublinie – M. Kostuch;
WSS im. M. Pirogowa w Łodzi – J. Parnowska;
Szpital Specjalistyczny nr 2 w Bytomiu Oddział Noworodkowy – P. Gazy;
Powiatowy Szpital Specjalistyczny w Stalowej Woli – L. Piotrowska;
Szpital Miejski w Piekarach Śląskich p.w. św.Łukasza – J. Wojcieszczyk-Bacia;
Szpital Wielospecjalistyczny, Sp. Z o.o. w Gliwicach – M. Kamińska-;
Pilśniak;Wojewódzki Szpital im. św. Ojca Pio w Przemyślu – A. Łukasiewicz;
Szpital Specjalistyczny im. L. Rydygiera w Krakowie sp. zo.o. – T. Strzelecki;
Wojewódzki Szpital Zespolony w Koninie – A.Wrzesińska;
Szpital Specjalistyczny im. Św. Rodziny w Warszawie – K. Dziadkiewicz;
Instytut Matki i Dziecka Klinika Neonatologii – K. Nowicka;
Zespół Opieki Zdrowotnej w Oławie – Z. Wesołowska;
Sosnowiecki Szpital Miejski sp. z o.o. – M. Ufel;
Miejski Szpital Zespolony Olsztyn – M. Reinert;
Wojewódzki Szpital Specjalistyczny w Olsztynie – J. Meller;
WSS w Legnicy – J. Górecka-Andrzejewska, R. Cimochowicz;
Szpital Wojewódzki im. Św. Łukasza SPZOZ w Tarnowie;
Specjalistyczny Szpital Ginekologiczno – Położniczy im. E. Biernackiego Wałbrzych;
Szpital w Knurowie Sp z o.o – K. Głębicka-Szczygieł;
Szpital Kliniczny im. Prof. Kornela Gibińskiego ŚUM – Z. Walencka;
Wojewódzki Szpital Specjalistyczny nr 2 Jastrzębie Zdrój – J. Stępień;
ZOZ w Świętochłowicach Spółka z o.o. – B. Wolnicka.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received a grant from the Nutricia Foundation PR 10/2013Z.
