Abstract
Objective
Deep brain stimulation (DBS) for treatment of advanced Parkinson’s disease (PD) has two anatomical targets: the subthalamic nucleus (STN) and the globus pallidus internus (GPI). The clinical effectiveness of these two stimulation targets was compared in the present study.
Methods
A systematic review and meta-analysis was performed to evaluated the postoperative changes in the United Parkinson’s Disease Rating Scale (UPDRS) on- and off-phase, on-stimulation motor scores; activities of daily living score (ADLS); and levodopa equivalent dose (LED) after STN and GPI stimulation. Randomized and nonrandomized controlled trials of PD treated by STN and GPI stimulation were considered for inclusion.
Results
Eight published reports of eligible studies involving 599 patients met the inclusion criteria. No significant differences were observed between the STN and GPI groups in the on-medication, on-stimulation UPDRS motor score [mean difference, 2.15; 95% confidence interval (CI), −0.96–5.27] or ADLS (mean difference, 3.40; 95% CI, 0.95–7.76). Significant differences in favor of STN stimulation were noted in the off-medication, on-stimulation UPDRS motor score (mean difference, 1.67; 95% CI, 0.98–2.37) and LED (mean difference, 130.24; 95% CI, 28.82–231.65).
Conclusion
The STN may be the preferred target for DBS in consideration of medication reduction, economic efficiency, and motor function improvement in the off phase. However, treatment decisions should be made according to the individual patient’s symptoms and expectations.
Introduction
Parkinson’s disease (PD) is a severely disabling condition for which current drug therapies do not always achieve satisfactory results. Neurosurgeons worldwide have made many attempts to alleviate the symptoms of PD by performing pallidotomy,1–4 thalamotomy, 5 or subthalamotomy 6 and high-frequency deep brain stimulation (DBS) of the subthalamic nucleus (STN), globus pallidus internus (GPI), and ventro-intermedial nucleus.7–10
Because the most effective management of advanced PD has not been established, management varies among clinical centers. DBS is widely applied because of its safety and comparative effectiveness. 7 Electrical stimulation can produce a functional lesion within a focal area of the brain. In the present study, two targets within the brain were stimulated for treatment of PD: the STN and the GPI. DBS of the STN has gained substantial popularity at most PD specialty centers. Many studies11–14 have revealed that STN stimulation can markedly improve patients’ motor function. However, serious adverse events have also been reported, including infection, depression, mood changes, and psychosis requiring intervention.12,15–18 GPI stimulation can also reportedly enhance patients’ motor function and time spent in the on state.12,19 Serious complications of DBS of the bilateral GPI include hematomas, infection, and equipment issues.21,22
In this comprehensive systematic review and meta-analysis, we compared the clinical advantages of DBS of the STN versus GPI for the treatment of PD. A better understanding of target selection is critical to guide treatment decision-making and patient expectations.
Methodology
Search criteria
All full-text published randomized and nonrandomized controlled trials comparing the United Parkinson’s Disease Rating Scale (UPDRS) on-phase motor score, UPDRS off-phase motor score, activities of daily living score (ADLS), and levodopa equivalent dose (LED) between patients who underwent DBS of the STN versus GPI were included. Case reports containing fewer than five patients, comments, letters, editorials, protocols, guidelines, animal studies, and cadaver articles were excluded.
Search strategy
The Medline, Embase, Cochrane Library, Ovid, and CBM databases were searched for English-language articles published from September 1993 to September 2013. Unpublished studies were excluded. The prespecified search terms were “Parkinson’s disease,” “deep brain stimulation,” “subthalamic nucleus,” “globus pallidum,” “randomized controlled trials,” “random,” “control,” and “trials.” Titles, abstracts, and subject headings were searched. The reference lists of all included articles and review papers were scrutinized for additional publications. In addition, we reviewed the references from all articles identified in the aforementioned search to include any additional papers related to the outcomes of DBS that may have been missed.
Search selection
Two reviewers independently assessed the titles and abstracts of each identified citation. The full texts of potential articles were ordered and evaluated against the eligibility criteria. Any disagreements were resolved by discussion.
Data extraction
Each reviewer independently extracted data from each included paper. All data were tabulated onto a predefined spreadsheet. All articles were anonymized with respect to author name, institution, journal title, and year of publication to blind reviewers during the processes of data extraction, appraisal, and analysis.
Outcome measures
The outcome measures were the changes in the on-phase UPDRS motor score, off-phase UPDRS motor score, ADLS, and LED from preoperatively to >3 months postoperatively. The primary focus of this meta-analysis was the off- and on-medication, on-stimulation UPDRS motor scores (Part III, motor examination section of the UPDRS). 23 This is the most commonly reported parameter in DBS studies and reflects the effect of stimulation on patients’ motor function. The motor subscale comprises 14 items with a score ranging from 0 to 104. The UPDRS ADLS is self-reported by patients and focuses on activities such as walking, writing, dressing, and speaking; the total score ranges from 0 to 52. The changes in the ADLS were weighted by the time spent in either the on or off phase. 24 Measurement of the LED involves conversion of antiparkinson medication doses into comparable levodopa doses. 25
Statistical analysis
The mean difference and 95% confidence interval (CI) of each outcome were assessed by comparing the STN and GPI groups, and the statistical heterogeneity was measured using the I2 statistic. The I2 test for heterogeneity was used to measure the proportion of total variation in the study estimates due to heterogeneity rather than sampling error. If significant heterogeneity was found among the studies based on interpretation of the I2 test, a random-effects model was applied. If no significant heterogeneity among studies was found, a fixed-effects model was applied. The meta-analysis was then carried out using RevMan software (version 5.0 for Windows; Copenhagen: The Nordic Cochrane Centre, the Cochrane Collaboration, 2008). P values of <0.05 were considered statistically significant. We attempted to contact the original authors to acquire detailed data. For missing standard deviations of changes from baseline, we referred to the Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (section 16.1.3.2).
Results
Search strategy
The database search, snowballing, and contact with experts yielded a total of 431 articles. After excluding 423 nonpertinent titles or abstracts, 8 studies22,24,26–32 were retrieved in complete form and assessed according to the selection criteria (Figure 1). In total, 599 patients were included; 300 underwent STN stimulation and 299 underwent GPI stimulation. The mean age of the patients in all eight studies was >40 years, and all follow-up periods were >3 months. The general characteristics of the patients among the eight studies are shown in Table 1.
A QUORUM Chart. Characteristics of the patients in the eight studies included in the meta-analysis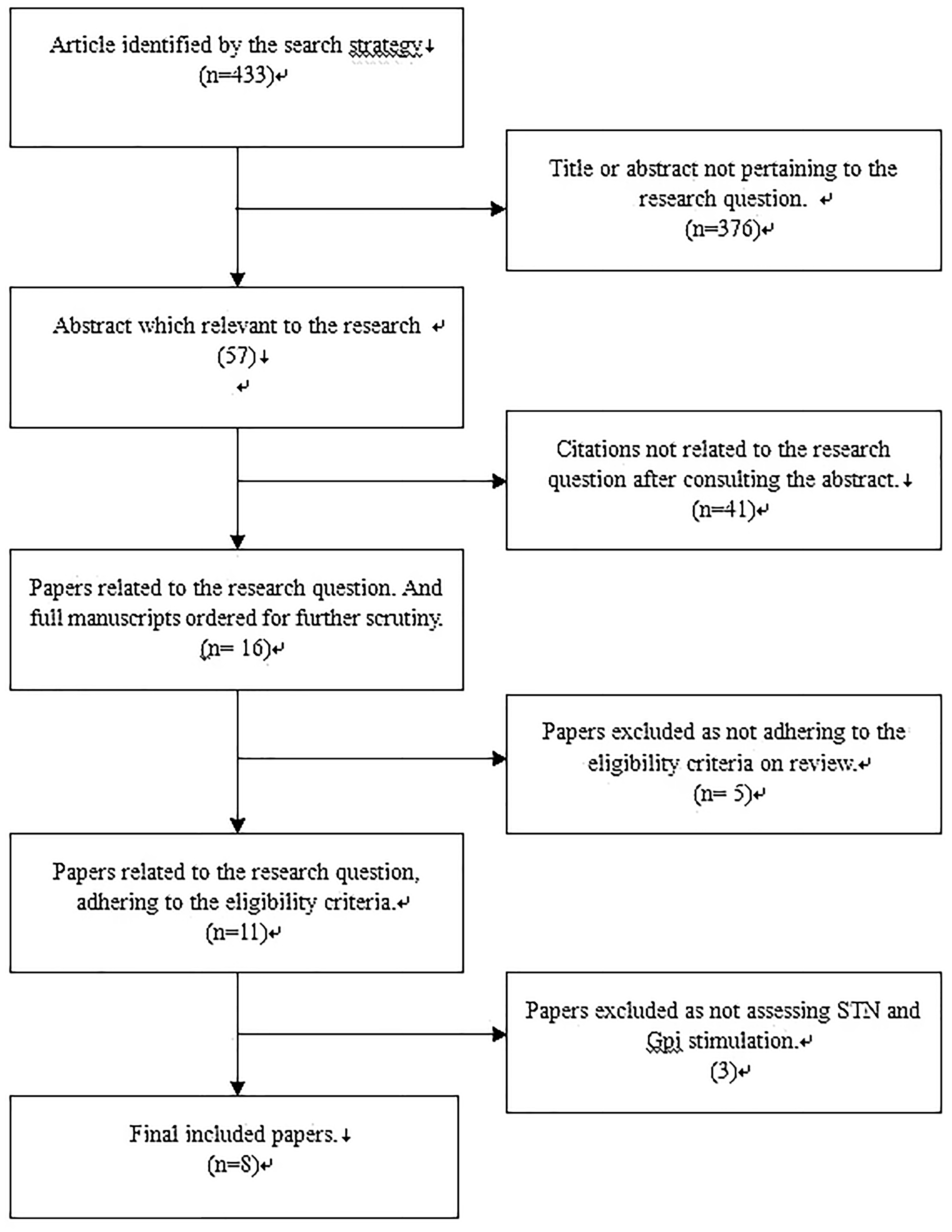

Outcome measures
Changes in UPDRS motor scores
Four studies24,28,30,32 conducted a <1-year follow-up to record the changes in the UPDRS motor score in the on phase. Our meta-analysis showed no significant difference between the STN and GPI groups (mean difference, 2.15; 95% CI, −0.96–5.27) (Figure 2(a)). Six studies22,24,26,28,29,30,32 recorded the change in the UPDRS motor score in the off phase. A meta-analysis of the six studies that recorded the changes in the UPDRS motor score in the off phase showed a significant difference in favor of STN stimulation (mean difference, 1.67; 95% CI, 0.98–2.37; P < 0.01) (Figure 2(b)).
(a) Meta-analysis of the mean difference of the changes of UPDRS motor scores on phase postoperation in STN stimulation vs.GPI stimulation. There is no significant difference between the two groups, with a mean difference of 2.15, 95%CI (−0.96,5.27); (b) Meta-analysis of the mean difference of the changes of UPDRS motor scores off phase postoperation in STN stimulation vs.GPI stimulation. STN is significantly associated with a decrease in the UPDRS motor scores, with a relative risk of 1.67, 95%CI (0.98,2.37).
Changes in ADLS
Four studies24,28,30,32 performed a <1-year follow-up to record the ADLS. Our meta-analysis showed no significant difference in the change in the ADLS between STN and GPI stimulation (mean difference, 3.40; 95% CI, −0.95–7.76) (Figure 3(a)).
(a) Meta-analysis of the mean difference of the changes of ADL scores postoperation in STN stimulation vs.GPI stimulation. There is no significant difference between the two groups, with a mean difference of −1.1, 95%CI [−2.6 to 0.4]; (b) Meta-analysis of the mean difference of the reduction of LEDs postoperation in STN stimulation vs. GPI stimulation. This meta-analysis showed a mean difference across the two groups of 130.24, 95% CI (28.82, 231.65), clearly favouring STN.
Changes in LED
Five studies26,27,28,31,32 recorded the LED reduction. Our meta-analysis showed significant differences in the LED in favor of STN stimulation (mean difference, 130.24; 95% CI, 28.82–231.65; P < 0.05) (Figure 3(b)).
Critical appraisal
Risk of bias among the included studies
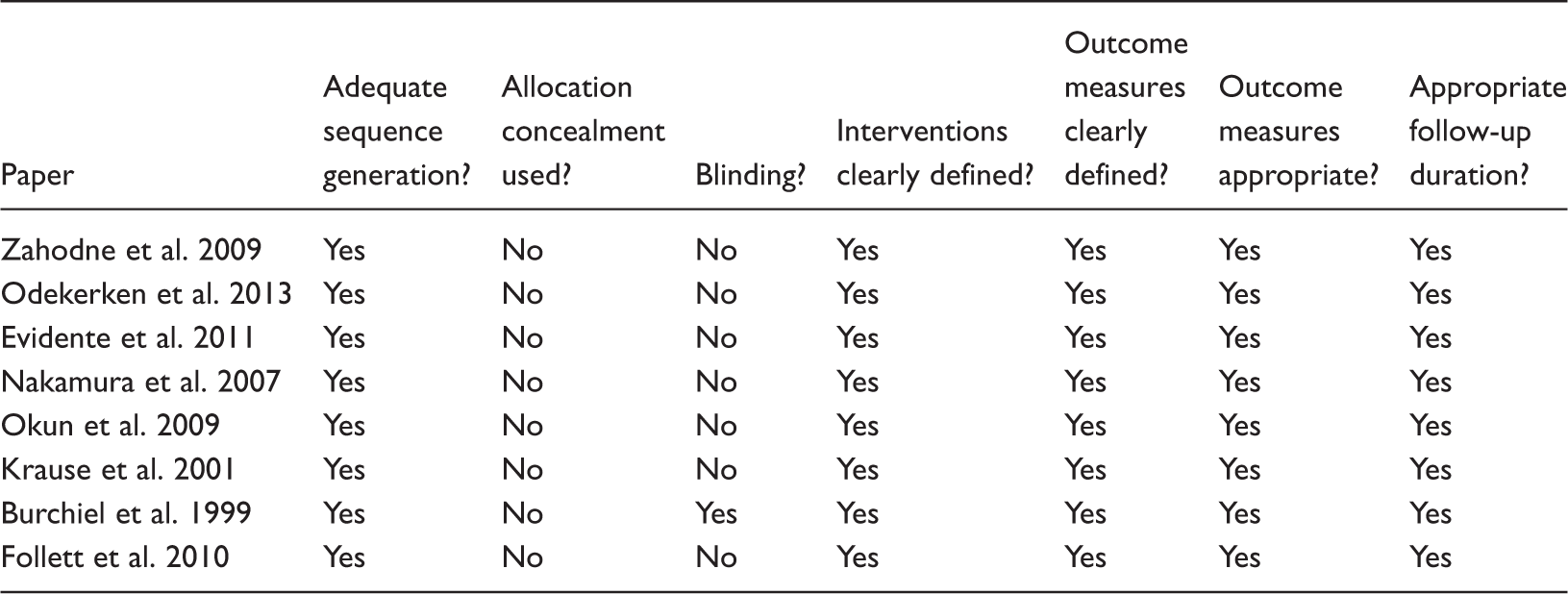
Discussion
The available data from the studies reporting the effects of DBS of the STN and GPI show that both targets have certain benefits. However, many factors must be considered to determine which target is the most appropriate. Among these factors are complications, side effects, motor function, cognition, mood, activities of daily living, medication reduction, and even economic factors.
Major complications of DBS include hemorrhage, infection, and hardware-related failure. Benabid et al. reported that hemorrhage occurred in 8.4% (range, 0.2%–12.5%) of 526 patients who underwent DBS and that only 0.6% had permanent deficits.33,34 Death directly attributable to the surgical procedure is extremely rare in the setting of DBS, but it has been reported. 35 In one study, spontaneous intracerebral hemorrhage occurred before insertion of the electrode during a DBS procedure, and the cause may have been related to amyloid angiopathy. 36 The infection rate varies widely among studies from 1% to >15%.3,37–39 Skin infections adjacent to the inserted material are mostly superficial at the site of the pulse generator and occurred in 15% of published cases. The stimulator and related hardware should be removed in patients with infection. Hardware-related complications such as lead breakage, extension wire failure, premature battery consumption, or malfunction of the pulse generator 40 can lead to discontinuation of treatment and the need for reoperation. 41
Because the operation process and implanted device are basically the same between DBS of the STN and GPI, these factors contribute little difference to the postoperative complication rates. Likewise, the side effects caused by stimulation of the two targets appear to be similar. For example, an acute postoperative confusional state may occur in up to 10% of patients, 36 and some patients who have undergone DBS (STN or GPI) gain weight.42,43 However, some longer-term studies have also suggested that the adverse effects of DBS are usually transient and reversible.
According to our meta-analysis, DBS of both the STN and GPI can improve the motor function of patients with PD by either pallidal or subthalamic stimulation. However, although no differences were observed in the on phase, significant differences were seen in the off phase; STN was more effective in terms of motor function improvement in the off phase, which is in accordance with many published studies.24,38,29,30,32,44,45 Follett et al. reported that 24 months postoperatively, the results in the on medication state did not differ significantly according to the surgical target; a reduction of 11.8 points was observed in the pallidal-stimulation group, and a reduction of 10.7 points was observed in the subthalamic-stimulation group (difference, −1.1; 95% CI, −4.3–2.1; P = 0.50). However, the UPDRS Part III score in the pallidal-stimulation group decreased by 1.2 points, whereas that in the subthalamic-stimulation group increased by 0.8 points, suggesting that the improvement in long-term motor function after stimulation of the STN is not superior to that after stimulation of the GPI and still needs further exploration. The ADLS is another primary evaluation parameter used in patients undergoing DBS and reflects the general living status of patients with PD. In our meta-analysis, the difference in the ADLS between the two target groups was not significant, and the result remained unchanged in the long term (difference, −1.1; 95% CI, −2.6–0.4).
PD is associated with relatively high rates of mood and cognitive dysfunction, and DBS of the STN and GPI has been proven to mildly ameliorate mood dysfunction and cognitive decline, particularly in verbal fluency tasks.41,46 Some controlled studies have provided evidence that DBS of the STN may lead to cognitive or psychiatric sequelae.15,17,18,26 Okun et al. 31 performed a comparative trial focusing on cognition and mood performance in patients with PD who underwent stimulation of the STN versus GPI. They found that stimulation of the STN resulted in worse verbal fluency on the letter task and was associated with a higher number of mood/cognitive/surgical adverse events. Interestingly, in a recent randomized trial of bilateral stimulation of the STN versus GPI with cognition/behavior as the primary outcome, Odekerken et al. 24 found no significant differences in the two targets with much larger numbers of patients. Both sites are cognitively safe, and overall target-related differences in cognitive outcomes are small. Nevertheless, the most recent meta-analysis suggested that all declines were found in psychomotor speed, memory, attention, executive functions, and overall cognition in patients who underwent DBS of the STN; DBS of the GPI resulted in fewer neurocognitive declines than DBS of the STN. 33
Quality of life shows more improvement when patients with PD are treated with a combination of DBS plus optimal medication than with optimal drug therapy alone. 7 However, researchers have divergent opinions regarding the effect of the two stimulation targets on quality of life. Using the 39-item Parkinson’s Disease Questionnaire, some researchers have found no significant difference between the two stimulation targets. 27 Other researchers consider that greater improvements in quality-of-life measures are achieved with GPI stimulation.32,47
Although medication reduction is not considered the primary goal of DBS, reductions in medication doses postoperatively may lead to improvements in medication-related side effects, including cognitive slowing, sleepiness, impulse control disorder, mania or hypomania, and dyskinesia. On average, the use of dopaminergic medications decreases more in patients undergoing subthalamic than pallidal stimulation.27,28,31,32 The present meta-analysis also confirmed that STN stimulation has advantages over GPI stimulation in terms of medication reduction.
The cost of DBS is an important factor to consider. The average stimulation amplitudes and pulse widths of STN stimulation are lower than those of GPI stimulation, allowing for potentially longer intervals between pulse generator replacement among patients undergoing subthalamic stimulation, with an attendant reduction in the long-term costs of therapy and a reduction in risks associated with surgical replacement of pulse generators. 27 Meanwhile, the cost also decreases due to a dramatic drop in the cost of medication and a probable lower frequency of hospital admissions required for medication adjustments.48,49
Limitations
Several factors may bias the findings of the current study. First, bias can be introduced in retrospective reviews without randomized, prospectively matched groups. Second, the reported infection rate was strongly biased by the duration of follow-up among the studies, and various types of infections continued to occur over time. Therefore, studies with very short follow-up times (3–6 months) showed the lowest infection rates, and studies with longer follow-up times showed higher cumulative infection rates. Third, because the interventionists were surgeons, the interventionists and assessors were poorly blinded to which surgery was being performed. Therefore, this permitted bias. Furthermore, the process of patient randomization was poorly described in the reviewed studies; only one study clearly acknowledged that patient assignment was concealed prior to group allocation. Other potentially confounding factors include the operative decisions and techniques of the different surgeons. Additional well-designed multicenter clinical trials that can minimize bias are needed, especially for evaluation of the long-term outcomes of the two stimulation targets.
Conclusion
Based on our meta-analysis and other available data in the literature, the STN may be the preferred target for DBS in consideration of motor function improvement, medication reduction, and economic efficiency, although GPI stimulation has some advantages in terms of mood and cognition. Treatment decisions should be individualized and based on patients’ specific symptoms and expectations.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
