Abstract
Tourette's syndrome is a complex neuropsychiatric disorder, characterized by tics. Bilateral globus pallidus internus (GPi) deep brain stimulation (DBS) has been considered to be an effective treatment for refractory Tourette's syndrome. Postoperative outcomes are described after 12 months’ follow-up in a 41-year-old male patient and a 22-year-old male patient with Tourette's syndrome, both of whom underwent unilateral electrode implantations into the right GPi for DBS. These patients were diagnosed with Tourette's syndrome in childhood and, despite long-term therapy with a range of antipsychotic medications, continued to experience disabling tics in adulthood. Improvements in tic severity of 58.5% and 53.1% were observed at 12 months in the older and younger patient, respectively; improvements were determined by the Yale Global Tic Severity Scale. Both patients also experienced reductions in tic frequency and reported improvements in their health-related quality of life. Improvements in tics were similar to previous reports involving patients who underwent bilateral GPi DBS. These cases suggest that unilateral DBS of the right GPi is effective and might be a viable surgical choice for some patients with Tourette's syndrome.
Introduction
Tourette's syndrome is a chronic neuropsychiatric disorder that is characterized by multiple motor and phonic tics, with onset in early childhood. 1 Tics are involuntary repetitive muscle contractions that produce stereotyped movements (motor tics) or sounds (phonic tics). 2 Since the first report of tic reduction by deep brain stimulation (DBS) of the globus pallidus internus (GPi), 3 other clinical studies have supported the effectiveness of bilateral DBS of this region for the treatment of tics.4,5 The therapeutic benefit of unilateral GPi DBS in treating Tourette's syndrome has rarely been examined. The present report describes postoperative outcomes in two patients with Tourette's syndrome who underwent unilateral DBS of the right GPi. Published literature on cases of bilateral DBS in Tourette's syndrome is reviewed and the benefits of the unilateral procedure are discussed in this context.
Case Reports
Two patients attending Beijing Institute of Functional Neurosurgery, Xuanwu Hospital, Capital Medical University, Beijing, China, had been diagnosed with Tourette's syndrome in childhood, according to the Diagnostic and Statistical Manual of Mental Disorders Edition IV (DSM-IV). 6 The Tourette's syndrome Diagnostic Confidence Index (DCI), which produces a score of between 0 and 100 as a measure the lifetime likelihood of Tourette's syndrome, was assessed in each patient. 7 Lack of effective therapy or unbearable side-effects led both patients to seek DBS treatment. Coexisting conditions (such as attention deficit hyperactivity disorder or obsessive compulsive disorder) were not evident in either patient. Neither patient was experiencing, or had previous history of, other neurobehavioural problems, anxiety or depression.
Surgical procedures were performed according to the Declaration of Helsinki and were approved by the Institutional Review Board at Xuanwu Hospital. Both patients gave informed consent for the reporting of their data.
Case 1
Patient 1, a 41-year-old, right-handed man, first presented at Xuanwu Hospital in February 2010. Tourette's syndrome had first manifested when the patient was 11 years old; he had no family history of the condition and was normal at birth. Biochemical examination of the blood showed no abnormalities; muscular tension of the extremities was normal. The patient had a Tourette's syndrome DCI score of 64. His tics first appeared as frequent throat clearing, and had gone through periods of worsening and improvement over the years. During adulthood, his most disabling symptoms were constant vocal tics and motor tics (such as repetitive hitting and wrist rotating), involving the upper extremities. These disabling tics first manifested at the age of 30 years. The patient had experienced repeated episodes of chronic pharyngitis for the previous 10 years, which may have occurred as a result of his frequent vocal tics. Long-term medication had not resulted in substantial symptom improvement; treatment with haloperidol (1 mg, twice daily for 6 months) and topiramate (200 mg, twice daily for 8 months) had been tried for < 6 months, with no obvious effect. The patient had been treated with tiapride (300 mg/day) for 9 years, which produced a mild suppression of tics but was associated with severe drowsiness, which limited his ability to perform cognitive tasks and led to discontinuation of the medication 1 year before he presented to our hospital. Patient 1 underwent surgery for unilateral electrode implantation for DBS in February 2010.
Case 2
Patient 2, a 22-year-old right-handed man, first presented at Xuanwu Hospital in February 2011. The patient had no signs of sore throat or tonsillitis before disease onset, and a neurological examination was normal. He had a Tourette's syndrome DCI score of 95. Tics first manifested as vocal tics and eye blinking when he was 4 years old; symptoms had gone through periods of worsening and improvement over the intervening 18 years. The most disabling tics, experienced by the patient at the age of 13 years, affected the muscles of the face and neck: these consisted of vocal tics such as grunting, coughing and grimacing. Treatment with a range of antipsychotic medications during the disease course had failed to ameliorate the patients' symptoms; tiapride (100 mg three times daily for 3 years), haloperidol (1 mg three times daily for 2 years), risperidone (1 mg twice daily for 1 year) and clonazepam (2 mg twice daily for 2 years) had been taken, with no obvious effect. He had discontinued these medications for 2 years before he presented to our hospital. At the time of surgery, the patient was a full-time college student and he reported a fear of continually disturbing the class (due to his vocal tics) as being a major impairment. Patient 2 underwent surgery for unilateral electrode implantation for DBS in February 2011.
Surgical Procedure for Electrode Implantation in GPI
A standard stereotactic surgical procedure for GPi localization 8 was performed using a stereotactic frame (CRW–FR, Radionics, Burlington, MA, USA). Three-dimensional coordinates for the GPi were obtained according to the Schaltenbrand–Wahren atlas8,9 guided by sagittal magnetic resonance imaging (MRI; Siemens 1.5 T Sonata, Siemens, Erlangen, Germany). The target was defined 20 – 22 mm lateral to the anterior commissure–posterior commissure (AC–C) line, 2 mm anterior to the midcommisural point and 4 – 6 mm below the AC–PC line. A quadripolar electrode (model 3387, Medtronic, Minneapolis, MN, USA) was implanted under local anaesthesia with 1% lidocaine, with both patients conscious and cooperative with neurosurgeons (X-H.Z., J-Y.L.). The electrode was subsequently connected to a Soletra pulse generator (Medtronic), implanted under general anaesthesia (2 – 3 mg/kg/h propofol and 0.05 – 0.15 μg/kg per min remifentanil) in the subclavicular region. The pulse generator was implanted immediately after electrode implantation. Postoperative MRI and axial MRI confirmed the position of electrode and whether there was evidence of any surgical complications, such as asymptomatic intracranial haemorrhage.
Postoperative Assessments Following Implantation
Testing for electrode contact was performed 1 week after electrode implantation; contact and stimulation parameters were optimized 4 weeks after initial testing, to obtain maximum clinical benefit with minimal side-effects 4 weeks later.
Tic severity was determined 7 days prior to surgery and at 3, 6 and 12 months postsurgery, using the Yale Global Tic Severity Scale (YGTSS) atlas. 10 Improvement in tic frequency by DBS was determined at the 12-month follow-up consultation in both patients: the frequency of motor and phonic tics was quantified with the stimulator on (On); the stimulator was then switched off for 24 h (Off) and the frequency of motor and phonic tics was counted again; the stimulator was then switched on (On II) and a second assessment was performed 24 h later. Patients and an expert assessor were blinded to the condition of the stimulator. Percentage improvement in tic frequency was determined by the calculation: (presurgery frequency – [postsurgery frequency/presurgery frequency]) × 100.
Postoperative MRI and Stimulation Parameters
Postoperative MRIs in both patients demonstrated electrode localization in the posterolateral ventral GPi and showed no evidence of surgical complications (Fig. 1). Both patients received monopolar stimulation (case served as anode with contact 2 as active contact). In Patient 1 and Patient 2, respectively, the parameters were 3.5 V and 2.8 V (stimulation amplitude), 90 μs and 90 μs (pulse width), and 160 Hz and 130 Hz (stimulation frequency).
Axial magnetic resonance images of the brains of patients with Tourette's syndrome, following implantation of a quadripolar electrode into the globus pallidus internus (GPi) for deep brain stimulation. Images show the electrode tip in the posterolateral ventral GPi in: (A) Patient 1, a 41-year-old male; (B) Patient 2, a 22-year-old male
TIC Severity and Frequency
Both patients responded well to DBS: improvement in bilateral tics was sustained over a 12-month follow-up period. The effects of DBS on tics and social impairment, as determined by the YGTSS, are summarized in Table 1. Reductions of 58.5% and 53.1% in the YGTSS total scores were determined in Patients 1 and 2, respectively, after 12 months' DBS (Fig. 2A).
The DCI systematically assesses several aspects of the clinical history of tics and provides a score of between 0 and 1 00 that allows clinicians to measure the likelihood that a person meets criteria of Tourette's syndrome. 7
Total Yale Global Tic Severity Scale Score = motor tic severity + vocal tic severity + impairment. 10
After turning off the stimulator for 24 h, both patients experienced increases in tic frequency (Fig. 2B) that decreased to previous levels when the stimulator was switched to the On II condition.
The effects of right globus pallidus internus deep brain stimulation (DBS) in a 41-year-old male (Patient 1) and a 22-year-old male (Patient 2) with Tourette's syndrome on: (A) tic severity as determined by Yale Global Tic Severity Scale (YGTSS)
10
total scores (total YGTSS = motor tic severity + vocal tic severity + impairment) over 12 months of follow-up; and (B) tic frequency after 12 months of DBS. The frequency of motor and phonic tics was quantified with the stimulator on (On), switched off for 24 h (Off), and switched on (On II) for a second assessment 24 h later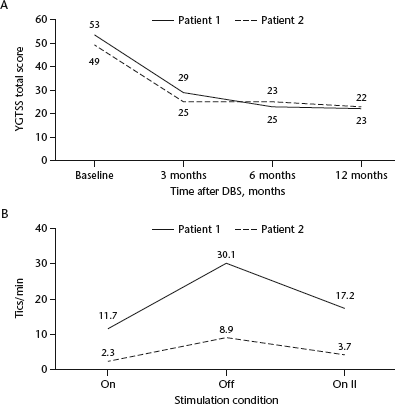
Both patients reported improvements in their health-related quality of life. No severe adverse effects of surgery were observed in either patient.
Discussion
Tourette's syndrome is a relatively common neuropsychiatric disorder, with prevalence rates in the range of 0.05 – 3% and a male : female preponderance of 4.3 : 1.11,12 The condition is often underdiagnosed and, as a consequence, many patients do not receive adequate care. 13 Published studies indicate that up to 80% of patients with Tourette's syndrome experience a significant tic decrease during adolescence; 14 although a small proportion of patients exhibits tic worsening in adulthood. 15 The pathophysiology of Tourette's syndrome remains unclear but, based on the model of movement disorders being related to basal ganglia dysfunction, tics have been proposed to result from a reduction in the normal inhibitory output of the basal ganglia. 16 According to this theory, altered neuronal activity of striatal neurons leads to uncontrolled inhibition in basal ganglia output neurons, which in turn disinhibits motor areas, causing unwanted movements such as tics. 17
Many patients with Tourette's syndrome fail to respond to standard pharmacological or behavioural therapies. 18 DBS could be considered as an alternative treatment in these patients, and bilateral GPi DBS is currently one of the most commonly used surgical procedures. 19 The present report described two cases of Tourette's syndrome in which right unilateral GPi DBS was performed. Following these procedures, both patients experienced considerable improvement in tic severity and frequency: outcomes were similar to the results obtained with bilateral GPi DBS for Tourette's syndrome (Table 2).5,20– 23
Effectiveness of bilateral globus pallidus internus deep brain stimulation on tic symptoms in five studies involving patients with Tourette's syndrome

Mean reduction in tic severity determined using the Rush Video-based Tic Rating Scale. 24
Mean improvement in tic severity determined using the Yale Global Tic Severity Scale. 10
Mean improvement in tic severity determined using Yale Tourette Syndrome Scale. 25
Unilateral DBS was the preferred treatment for the present cases due to the misgivings of each patient regarding operative outcomes and the high costs associated with bilateral DBS. We estimate that the average yearly cost of bilateral GPi DBS treatment in China is almost 100-fold higher than that of conventional medication, and approximately twice as expensive as unilateral DBS, although we are unable to provide firm data on this.
In both patients described here, bilateral GPi DBS implantation was carried out in two stages, with the unilateral electrode implanted at the first stage. As a consequence, the risk of surgical complications (such as intracranial haematoma or infection) and any hardware problems related to unilateral DBS were anticipated to be lower than those seen following bilateral DBS procedures. 26 The decision to perform the right unilateral procedure was also based on structural pathology findings in Tourette's syndrome. In a morphological study using magnetization transfer imaging, white matter was reduced in the right medial frontal gyrus and cingulate gyrus in Tourette's syndrome, and this reduction was related to tic severity. 27 Another morphometric study has demonstrated that white matter was significantly increased in the right ventroposterolateral part of the thalamus in patients with Tourette's syndrome compared with healthy age- and sex-matched controls. 28 Furthermore, it has also been reported that DBS of the right nucleus accumbens was associated with an improvement in tics. 29
It has been documented that the majority of right-handed individuals have left-hemisphere language dominance. 30 Electrode implantation can cause intracerebral haemorrhage. 31 Thus, electrode implantation in the left hemisphere is more likely to be associated with a higher proportion of language complications than implantation in the right hemisphere. Given these pathophysiological, anatomical and clinical considerations, electrodes were implanted into the right GPi as the target for DBS in the present cases, as this may be less likely to cause functional damage and complications than implantation into the left GPi. Microlesions can develop as a result of bilateral electrode implantation into the GPi, and the effects mediated by these microlesions may be apparent for ≤ 6 months following implantation. 32 Given these observations, the effects of bilateral GPi DBS may not be directly comparable with unilateral GPi DBS, even when the implantable pulse generator is switched off. The present cases are the only ones to demonstrate responses with right GPi DBS.
Interest in the use of unilateral DBS as a potentially better treatment choice compared with bilateral DBS, in patients with movement disorders, is increasing. 33 Observations in the present cases are, therefore, clinically relevant and suggest that unilateral DBS of the right GPi is effective for some patients with Tourette's syndrome. Unilateral DBS is a less aggressive and less expensive procedure, and may be associated with fewer postoperative complications, compared with bilateral DBS.
Footnotes
Acknowledgements
This work is supported by grants from the National Natural Science Foundation of China (Nos 30770746 and 81171061).
The authors had no conflicts of interest to declare in relation to this article.

