Abstract
Objective
To examine patency of the cerebral anterior and posterior communicating arteries in patients with ischaemic stroke with or without diabetes mellitus.
Methods
This retrospective study included patients with acute ischaemic stroke treated between July 2011 and May 2016. Cerebral infarction was evaluated by magnetic resonance imaging. Anterior and posterior communicating-artery patency was determined using magnetic resonance angiography. Vessels were defined as patent or occluded.
Results
Out of 1 406 patients, incidence of vertebral basilar artery brain infarction and posterior cerebral artery brain infarction were significantly higher in patients with diabetes versus those without diabetes (35.5% versus 22.3% and 11.7% versus 6.8%, respectively). Among patients with posterior cerebral artery brain infarction, anterior and posterior communicating-artery patency rates were higher in patients with diabetes versus those without diabetes (66.7 versus 23.5% and 33.3% versus 5.9% [bilateral], respectively). Among patients with vertebral basilar artery infarction and posterior cerebral artery P1 segment infarction, patency rate of the anterior communicating artery was higher in patients with diabetes versus those without diabetes (55.7% versus 45.9%).
Conclusion
Among patients with ischaemic stroke, patency rate of the circle of Willis may be higher in patients with diabetes than those without diabetes.
Keywords
Introduction
Ischaemic stroke represents approximately 85% of all strokes. 1 and has a number of identified risk factors, comprising history of transient ischaemic attack (TIA), smoking, metabolic syndrome, heavy alcohol use, diabetes mellitus, high cholesterol levels, and carotid artery stenosis. 2 Among these, diabetes is a modifiable risk factor for a first ischaemic stroke.2,3 In the 1970’s, the Framingham study showed a 2.5-fold increase in the incidence of ischaemic stroke among male patients with diabetes and a 3.6-fold increase among female patients with diabetes, 3 and this increased risk has been confirmed by a number of subsequent studies.4–7
Patients with diabetes are more prone to ischaemic stroke occurring in the posterior cerebral circulation region compared with other brain regions. 8 The collateral brain circulation includes a secondary cerebral vessel network between the main cerebral arteries, and if obstruction occurs in a cerebral artery, the collateral vessels are able to stabilize the cerebral blood flow. 9 The cerebral collaterals can be divided into three levels: the first level includes the intracranial and extracranial communicating branches; the second level includes the circle of Willis; and the third level includes the leptomeningeal collateral vessel. 10
The circle of Willis has been suggested by a number of studies to play an important role in the risk of stroke.11,12 Indeed, an incomplete circle of Willis has been shown to increase the risk of stroke by 5.4–7.0 fold. 12 The anatomy of the circle of Willis also influences risk of ischaemia during carotid endarterectomy. 13
The influence of patency of the circle of Willis on risk of ischaemic stroke among patients with diabetes remains unclear. Thus, the aim of the present retrospective study was to examine patency of the cerebral anterior and posterior communicating arteries in patients with ischaemic stroke with or without diabetes, in order to determine the role of the circle of Willis in ischaemic stroke among patients with diabetes.
Patients and methods
Study population and design
This retrospective study included consecutive patients with acute ischaemic stroke treated between July 2011 and May 2016 at the Institute of Neurology, China Three Gorges University, Yichang, Hubei, China. Inclusion criteria comprised the following: (1) patients who underwent brain magnetic resonance imaging (MRI) on admission; (2) available MRI images and data; (3) symptoms and signs of ischaemic stroke, as determined by a neurologist; and (4) MRI was performed <7 days following symptom onset. Exclusion criteria comprised: (1) absence of diffusion-weighted MRI or magnetic resonance angiography (MRA) examination; (2) presence of haemorrhagic stroke; or (3) Moyamoya disease.
The present study was approved by the ethics review committee of China Three Gorges University. The need for individual informed consent was waived by the committee because of the retrospective nature of the study.
Magnetic resonance imaging
At the time of the study, the routine MRI protocol used at the Institute of Neurology, China Three Gorges University, for patients with acute ischaemic stroke comprised transverse T1-weighted imaging (FLASH sequence; repetition time [TR], 280 ms; echo time [TE], 2.5 ms), T2-weighted imaging (turbo spin echo; TR, 4000 ms; TE, 100 ms), diffusion-weighted imaging (echo planar imaging; TR, 3000 ms; TE, 90 ms), and fluid-attenuated inversion recovery (TR, 8500 ms; TE, 90 ms; and inversion time, 2200 ms) using a Signa 3.0-T TwinSpeed MRI system (GE Healthcare, Waukesha, WI, USA).
Classification of ischaemic stroke
Ischaemic stroke was categorized according to ischaemic site and amount of blood supply: (1) anterior circulation brain infarction, which included lesions from the internal carotid artery blood supply that affected the frontal lobe, parietal lobe, lateral temporal lobe, putamen, caudate nucleus, anterior limb of the internal capsule, genu of internal capsule, and the anterior 2/3 of the posterior limb of the internal capsule; (2) posterior cerebral artery brain infarction (excluding the P1 segment), which included the occipital lobe and the medial temporal lobe, and the 1/3 hypothalamus parts lateral to the posterior limb of the internal capsule; and (3) vertebral basilar artery infarction and posterior cerebral artery P1 segment infarction (VBABI), which included the medulla, pons, midbrain, cerebellum, and medial thalamus.
The presumed aetiology of the stroke was classified as cardioembolism, large artery atherosclerosis, or small vessel occlusion, according to the Trial of Org 10172 in Acute Stroke Treatment classification. 14
Patency of the circle of Willis
Patency of the anterior communicating artery was recorded as 1 (patent) or 0 (non-patent [occluded]) according to the MRA (3-dimensional time-of-flight [TOF]) evaluation. For the posterior communicating artery, bilateral occlusion was recorded as 0, unilateral occlusion was recorded as 1, and bilateral patency was recorded as 2.
Data collection
Data relating to cardiovascular risk factors were extracted from patient records. Hypertension was defined as blood pressure >140/90 mmHg taken twice within 5 min before cerebral stroke, or the patient being treated with anti-hypertensive medication. Diabetes was defined as fasting blood glucose level >7.1 mmol/l, or 2-h postprandial or oral glucose tolerance test 2-h blood glucose level >11.1 mmol/l. 15 Hyperlipidaemia was defined as total cholesterol level >5.2 mmol/l, or low-density lipoprotein cholesterol level >3.1 mmol/l, or triglyceride level >1.7 mmol/l. Hyperhomocysteinaemia was defined as blood homocysteine level >17 µmol/l. Hyperuricemia was defined as serum uric acid level >430 µmol/l. Stroke history was defined as having a medical history of TIA, ischaemic stroke, or haemorrhagic stroke. Family history of stroke was defined as a first-degree relative with a history of TIA, ischaemic stroke, or haemorrhagic stroke. Smoker was defined as currently smoking or smoking cessation within <6 months.
Statistical analyses
Continuous variables are presented as mean ± SD and were analysed using Student’s t-test. Categorical variables are presented as frequencies and percentages, and were analysed using Pearson’s χ2-test. The non-parametric Mann–Whitney U-test was used to analyse ordinal categorical variables. SPSS software, version 21.0 (IBM, Armonk, NY, USA) was used for all statistical analyses. Two-sided P-values <0.05 were considered statistically significant.
Results
Study group characteristics
Demographic and clinical characteristics of patients with acute ischaemic stroke with or without diabetes mellitus.

Data presented as mean ± SD, or n (%) prevalence.
Smoker, currently smoking or smoking cessation for <6 months; family stroke history, first-degree relative with a history of transient ischaemic attack (TIA), ischaemic stroke, or haemorrhagic stroke; stroke history, medical history of TIA, ischaemic stroke, or haemorrhagic stroke; hyperhomocysteinaemia, homocysteine >17 µmol/l; hyperuricemia, uric acid >430 µmol/l; hypertension, blood pressure >140/90 mmHg, or anti-hypertensive medication; hyperlipidaemia, total cholesterol >5.2 mmol/l, or low-density lipoprotein cholesterol >3.1 mmol/l, or triglyceride >1.7 mmol/l.
NS, no statistically significant between group difference (P > 0.05; Student’s t-test, Pearson’s χ2-test, or Mann–Whitney U-test).
Stroke characteristics
Comparison of cerebral infarction sites in 1 406 patients with acute ischaemic stroke with or without diabetes mellitus.

Data presented as n (%) incidence.
VBABI, vertebral basilar artery infarction and posterior cerebral artery P1 segment infarction.
Statistically significant between-group differences (P < 0.05; Pearson’s χ2-test).
Anterior and posterior communicating artery patency
Patency rates of anterior and posterior communicating arteries in 1 406 patients with acute ischaemic stroke with or without diabetes mellitus.

Data presented as n (%) prevalence.
Statistically significant between-group differences (P < 0.05; Pearson’s χ2-test or Mann–Whitney U-test).
Patency rates of the anterior and posterior communicating arteries according to infarction site in 1 406 patients with acute ischaemic stroke with or without diabetes mellitus.
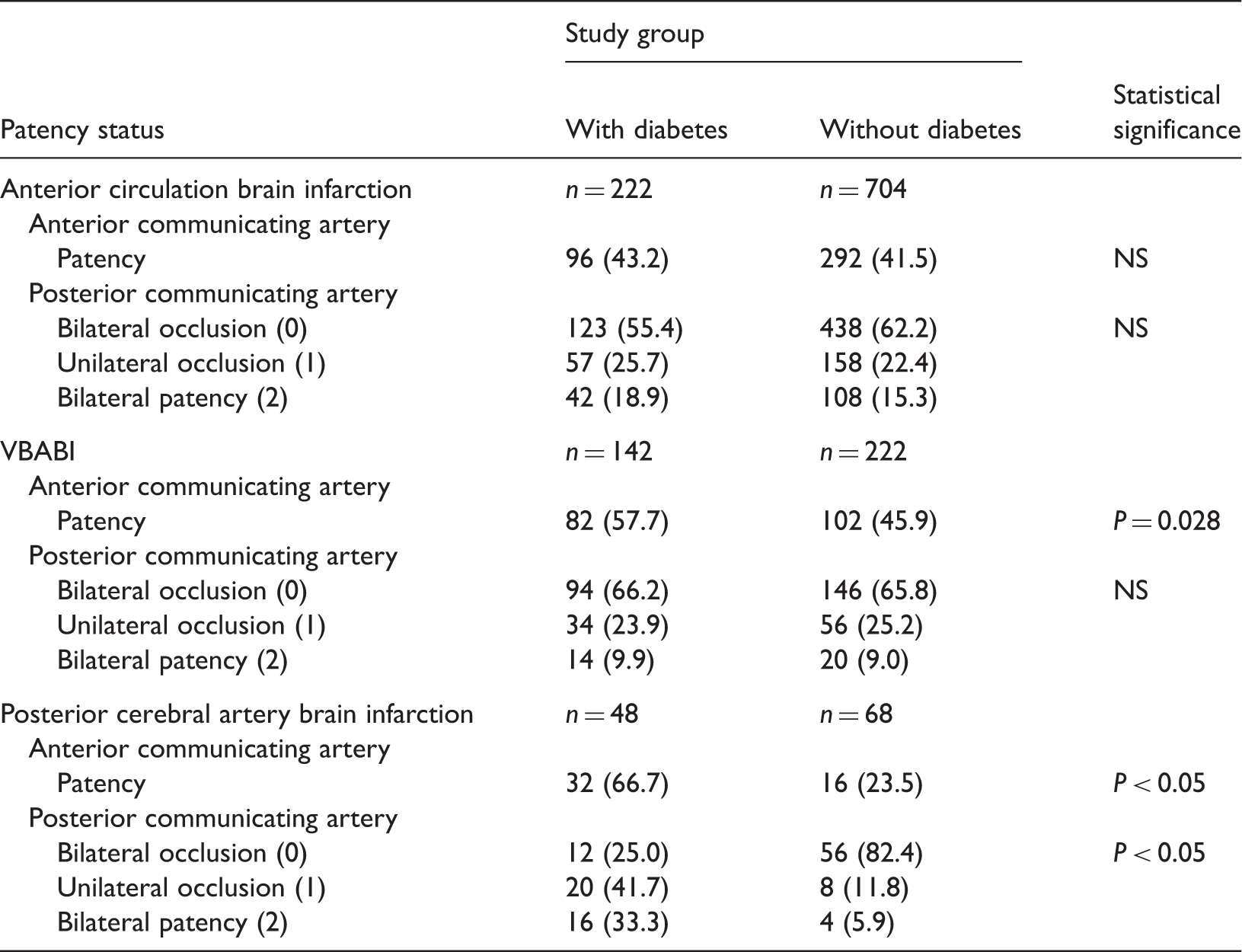
Data presented as n (%) prevalence.
VBABI, vertebral basilar artery infarction and posterior cerebral artery P1 segment infarction.
NS, no statistically significant between-group difference (P > 0.05; Pearson’s χ2-test or Mann–Whitney U-test).
In the VBABI subgroup (Table 4), the anterior communicating artery patency rate was significantly higher in patients with diabetes (57.7%) versus those without diabetes (45.9%; P = 0.028). There were no statistically significant differences between patients with or without diabetes in terms of bilateral posterior communicating artery occlusion (66.2% versus 65.8%), unilateral posterior communicating artery occlusion (23.9% versus 25.2%), or bilateral patency (9.9% versus 9.0%).
In the posterior cerebral artery brain infarction subgroup (Table 4), the anterior communicating artery patency rate was significantly higher in patients with diabetes (66.7%) versus those without diabetes (23.5%; P < 0.001). In terms of posterior communicating artery occlusion and patency, patients with diabetes displayed significantly higher rates of unilateral occlusion and bilateral patency, and significantly lower rates of bilateral occlusion than patients without diabetes (P < 0.001).
Discussion
Anatomy and patency of the circle of Willis play important roles in the risk of ischaemic stroke, 12 however, influence of the circle of Willis on this risk among patients with diabetes remains poorly understood. Thus, the present study aimed to examine patency of the anterior and posterior communicating arteries in patients with ischaemic stroke with or without diabetes. In the present study, incidence of VBABI and posterior cerebral artery brain infarction were higher among patients with diabetes than those without diabetes. Among patients with posterior cerebral artery brain infarction, patency rates of the anterior and posterior communicating arteries were higher in patients with diabetes than patients without diabetes. Among patients with vertebral basilar artery infarction and posterior cerebral artery P1 segment infarction, patency of the anterior communicating artery was higher in patients with diabetes than those without diabetes. Among patients with ischaemic stroke, therefore, the patency rate of the circle of Willis may be higher in patients with diabetes than in those without diabetes.
Risk factors for ischaemic stroke include age, hypertension, diabetes, and hyperlipidaemia. 2 Ischaemic stroke can be classified into either anterior or posterior circulation brain infarction, and the influence of risk factors for ischaemic stroke differs between the anterior and posterior infarction types.8,16 A study comparing risk factors between anterior and posterior circulation brain infarction 8 found that diabetes was associated with an increased incidence of posterior circulation brain infarction, however, the study used the Oxfordshire Community Stroke Project classification, 17 which is based on clinical symptoms and is less accurate than criteria based on imaging characteristics. 18 An investigation into the relationship between posterior circulation brain infarction and diabetes that used MRI, 19 showed that diabetes was associated with an increased frequency of brain stem infarction. The present study used diffusion-weighted MRI, considered to be a precise method, 20 to determine the stroke type. Due to the existence of the posterior communicating artery, the distal region of the posterior communicating artery P1 segment may receive blood from the anterior circulation. 4 Therefore, posterior circulation brain infarction was further classified into posterior cerebral artery brain infarction and vertebral basilar artery infarction and posterior cerebral artery P1 segment infarction (VBABI). The present study found that patients with diabetes had a higher frequency of VBABI, which is supported by a previous study. 19 The occurrence of posterior cerebral artery brain infarction was also higher in patients with diabetes than in patients without diabetes in the present study. The prognosis of posterior circulation brain infarction is poorer than that of anterior circulation brain infarction 21 and because the prevalence of diabetes is rapidly growing,22,23 morbidity and mortality associated with ischaemic stroke could increase in the future.
Collateral circulation is an important structure to sustain the balance and effectiveness of cerebral blood perfusion, 24 and impaired collateral circulation has been associated with ischaemic stroke.25,26 The circle of Willis is one of the primary structures of the cerebral collateral circulation, and the asymmetry of the circle of Willis results in asymmetrical blood flow, 27 which is an important risk factor for ischaemic stroke.12,13 In the present study population, patency rates of the circle of Willis were higher in patients with diabetes than in patients without diabetes. These results may be explained by the following: First, the causal relationship between patency of the posterior communicating artery and its compensation regions remains poorly understood, with a lack of longitudinal studies on the subject; Secondly, in the present study, patency of the posterior communicating artery was higher in patients with diabetes than in those without diabetes, which may be associated with the early occurrence of intracranial artery atherosclerosis in patients with diabetes, resulting in a pressure imbalance between the anterior and posterior circulations. The present study used the 3-dimensional TOF technique for MRA, however, which cannot show communicating arteries without blood flow. 28 Atherosclerosis in the posterior circulation has been suggested as a major risk factor for hypertension, diabetes, and metabolic syndrome, 29 but smoking and alcohol were considered to be risk factors for anterior circulation atherosclerosis, however, lacunar infarctions were not included in the study. Another study 30 showed that the occurrence of diabetes combined with posterior circulation atherosclerosis was higher than the occurrence of diabetes combined with anterior circulation atherosclerosis. Therefore, these two studies29,30 suggest that diabetes may result in more severe atherosclerosis of the posterior large vessels compared with anterior vessels, which supports the present study results. Nevertheless, because of technical limitations, the present study could not analyse the direction of blood flow in communicating arteries. Therefore, the metabolism level of the cerebral tissue and reverse blood flow towards the anterior circulation due to PCA distal infarction could not be excluded. Additional studies are necessary to elucidate these points. Nevertheless, even though previous studies have shown the involvement of the circle of Willis in the development of ischaemic stroke,12,13 the present retrospective study does not allow determination of the exact causality between the circle of Willis, diabetes, and ischaemic stroke. Additional studies are therefore necessary to elucidate this issue.
The present study has some strengths. First, posterior circulation brain infarction was further sub-classified into posterior cerebral artery brain infarction and VBABI, allowing a better refinement of the risk conferred by diabetes on the risk of ischaemic stroke. Secondly, diffusion-weighted MRI was used to determine the exact infarction sites, which may reflect the infarction sites more accurately, detect early cerebral infarction and asymptomatic cerebral infarction, and also could exclude patients without acute cerebral infarction. Finally, the sample size was relatively large, which may improve the reliability of the results.
The results of the present study are limited by the following: First, the retrospective nature of the study limits the interpretability of the data; Secondly, diffusion-weighted MRI was an inclusion criteria, which may result in selection bias because not all patients presenting with acute ischaemic stroke undergo diffusion-weighted MRI; Thirdly, patency of the communicating arteries was assessed by the MRA TOF method, which cannot reveal blood flow direction, nor can it discriminate between patency and hypoplasticity of the artery; Finally, no causal relationship could be determined because of the retrospective nature of the study.
In conclusion, patients with diabetes may be more prone to suffer from ischaemic stroke of the posterior circulation. Patency of the circle of Willis may be higher in patients with diabetes than in patients without diabetes.
Footnotes
Acknowledgements
The diagnosing neurologist for ischaemic stroke was Dr Jun Wei, MD, Institute of Neurology, China Three Gorges University.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
