Abstract
Objective
Betatrophin is a newly identified circulating protein that is significantly associated with type 2 diabetes mellitus (T2DM), adiposity, and metabolic syndrome. The aim of this study was to investigate whether betatrophin levels and polycystic ovary syndrome (PCOS) were associated.
Methods
Circulating betatrophin levels were measured in 162 patients with PCOS and 156 matched control females using specific enzyme-linked immunosorbent assay kits. Correlations between betatrophin levels and PCOS incidence as well as multiple key endocrine PCOS parameters were analyzed using multiple statistical methods.
Results
Betatrophin levels were significantly increased in patients with PCOS (685.3 ± 27.7 vs. 772.6 ± 42.5 pg/ml). When sub-grouping all investigated subjects according to the presence of insulin resistance, women with PCOS and insulin resistance exhibited markedly higher betatrophin concentrations. Furthermore, betatrophin levels were significantly correlated with fasting insulin levels and homeostatic model assessment of insulin resistance only in females with PCOS (r = 0.531 and r = 0.628, respectively).
Conclusion
We provide the first report that betatrophin is strongly associated with PCOS. This study suggests that betatrophin may potentially serve as an independent predictor for the development of PCOS in at-risk women, especially those with insulin resistance.
Introduction
Polycystic ovary syndrome (PCOS) is the primary cause of anovulatory infertility 1 and affects up to 10% of women of reproductive age. 2 The exact pathophysiology of PCOS is complex and remains largely unclear. However, the aetiology of PCOS is underpinned by both insulin resistance and hyperandrogenism, with insulin resistance exacerbating hyperandrogenism. 3 Insulin resistance occurs in approximately 80% of women with PCOS and occurs independently of obesity. 4 Furthermore, women with PCOS are believed to be at an increased risk of developing type 2 diabetes mellitus (T2DM). 5 A recent meta-analysis of 13 studies reported a 4-fold increased risk of T2DM in women with PCOS. 6 Thus, PCOS is a well-defined clinical model of insulin resistance and the pre-diabetic state.
Betatrophin, also known as angiopoietin-like protein (ANGPTL8), is a newly identified circulating protein predominantly produced in the liver and adipose tissue. Betatrophin is induced as a result of insulin resistance, 7 therefore attracting increasing attention. Betatrophin was reported to promote pancreatic beta cell proliferation and improve metabolic control by increasing the beta cell division rate in insulin resistant mice. 7 However, in humans, the associations of serum betatrophin levels with diabetes, obesity, and lipid profiles remain controversial.8,9 Some studies have suggested that circulating betatrophin levels are elevated in T2DM as well as type 1 diabetes,10–17 correlating with lipid profiles, 18 while others reported that betatrophin levels were reduced in subjects with diabetes. 19 Accumulating evidence suggests that betatrophin is significantly associated with adiposity, type 2 diabetes, and the metabolic syndrome.17,18,20
To date, there have been no reports on the relationship between betatrophin and PCOS. In fact, most women with PCOS display impaired glucose tolerance and are at higher risk for developing T2DM. 21 Moreover, betatrophin has a close relationship with insulin resistance and T2DM.8,14,17 These observations raise the question of whether abnormal betatrophin might associate with PCOS. Therefore, the present study aimed to detect circulating betatrophin levels in subjects with PCOS and healthy control female patients. We also evaluated the association between betatrophin levels and clinical, hormonal, and metabolic variables to achieve a better understanding of the relationship between betatrophin and PCOS.
Patients and methods
Study participants
This case-control study was approved by the Institutional Ethical Review Board of Yantai Yuhuangding Hospital (H20130381). Written informed consent was obtained from all patients before the initiation of the study. We included 162 women with a diagnosis of PCOS and 156 non-hirsute ovulatory women (regular cycles and luteal phase progesterone levels higher than 3.8 ng/mL), ranging from 18 to 45 years of age, in the study at our clinic between February 2013 and November 2015. PCOS diagnosis was determined according to the Rotterdam PCOS Consensus criteria. 22 Each subject underwent a complete medical examination and an endocrine profile and haematological, hepatic, and renal function analysis. Women with body mass index (BMI) ranging from 18.0 to 40.0 kg/m2 were selected for the study. We made further subgroupings based on the presence of insulin resistance, defined as a homeostatic model assessment (HOMA) index of ≥2.4. 23 None of the women from either group had received any drugs known to interfere with hormone levels, blood pressure, or metabolic variables for at least 3 months before the study. Women with diabetes, liver or kidney disease, thyroid dysfunction, or pregnancy were excluded.
Biochemical and hormonal assays
Blood samples were obtained during the mid-follicular phase of the menstrual cycle after at least 12 hours of fasting. Blood samples from all subjects were separated immediately by centrifugation at 4000 × g for 10 min and stored at −80℃ until analysis. Automated chemiluminescence immunoassay systems were used for measuring luteinizing hormone (LH), follicle-stimulating hormone (FSH), total testosterone (ADVIA Centaur, Siemens Healthcare Diagnostics, Eschborn, Germany), dehydroepiandrosterone sulfate, and sex hormone–binding globulin (SHBG) (Immulite 2000 XPi, Siemens Healthcare Diagnostics). The free androgen index (FAI) was estimated by dividing total testosterone (nmol/L) by SHBG (nmol/L) × 100. Low-density lipoprotein cholesterol was estimated indirectly with the Friedewald formula. 24 Total cholesterol, high-density lipoprotein cholesterol, triglyceride, and glucose levels were determined by colorimetric-enzymatic methods (Siemens Advia System, Deerfield, IL, USA). Intra- and inter-assay coefficient of variation values for these parameters were <5% and <8%, respectively.
Glucose tolerance test
In all subjects, a 3-h oral glucose tolerance test was used to evaluate insulin resistance and β-cell function. After a 12-h overnight fast, patients ingested 75 g glucose, and glucose and insulin concentrations were determined at baseline and after 30, 60, 90, 120, and 180 min. For this study, we used only fasting insulin and glucose to determine the HOMA index. Insulin resistance was calculated using the HOMA-insulin resistance (HOMA-IR) formula: glucose (mmol/L) × fasting insulin (mU/L)/22.5. 25 Fasting insulin was evaluated using a chemiluminescence immunometric assay and commercial kit (Immulite 2000 Analyzer; CPC). Fasting glucose was measured using a glucose oxidase assay (Tosoh Corp., Tosoh, Japan).
Measurement of betatrophin
Fasting serum betatrophin levels were assessed using enzyme-linked immunosorbent assay (ELISA) kits (EIAab Science, Wuhan, China; Catalogue No. E11644h). The procedures were in accordance with the manufacturer’s instructions. ELISAs were performed in duplicate, and samples with coefficient of variation values exceeding 5% were excluded.
Statistical analysis
SPSS version 20.0 (SPSS, Chicago, IL) was used for all analyses. Data are presented as mean ± SD or median [interquartile range]. Differences between groups were evaluated using the unpaired two-tailed Student’s t-test for data with Gaussian distributions. The Mann-Whitney U test was used to compare group medians for data with non-Gaussian distributions. Bivariate relations between betatrophin levels and covariates were analysed with Spearman’s Rank Correlation Coefficient. A forward stepwise multiple linear regression model was used to test which variables were independent predictors of betatrophin level. We made further subgroupings based on the presence of insulin resistance, defined as a HOMA index ≥2.4. Betatrophin concentrations were compared between multi-groups with one-way analysis of variance followed by LSD-t tests. Data were considered statistically significant at P < 0.05.
Results
Anthropometric characteristics, hormone concentrations, and metabolic profiles of control patients and patients with PCOS.
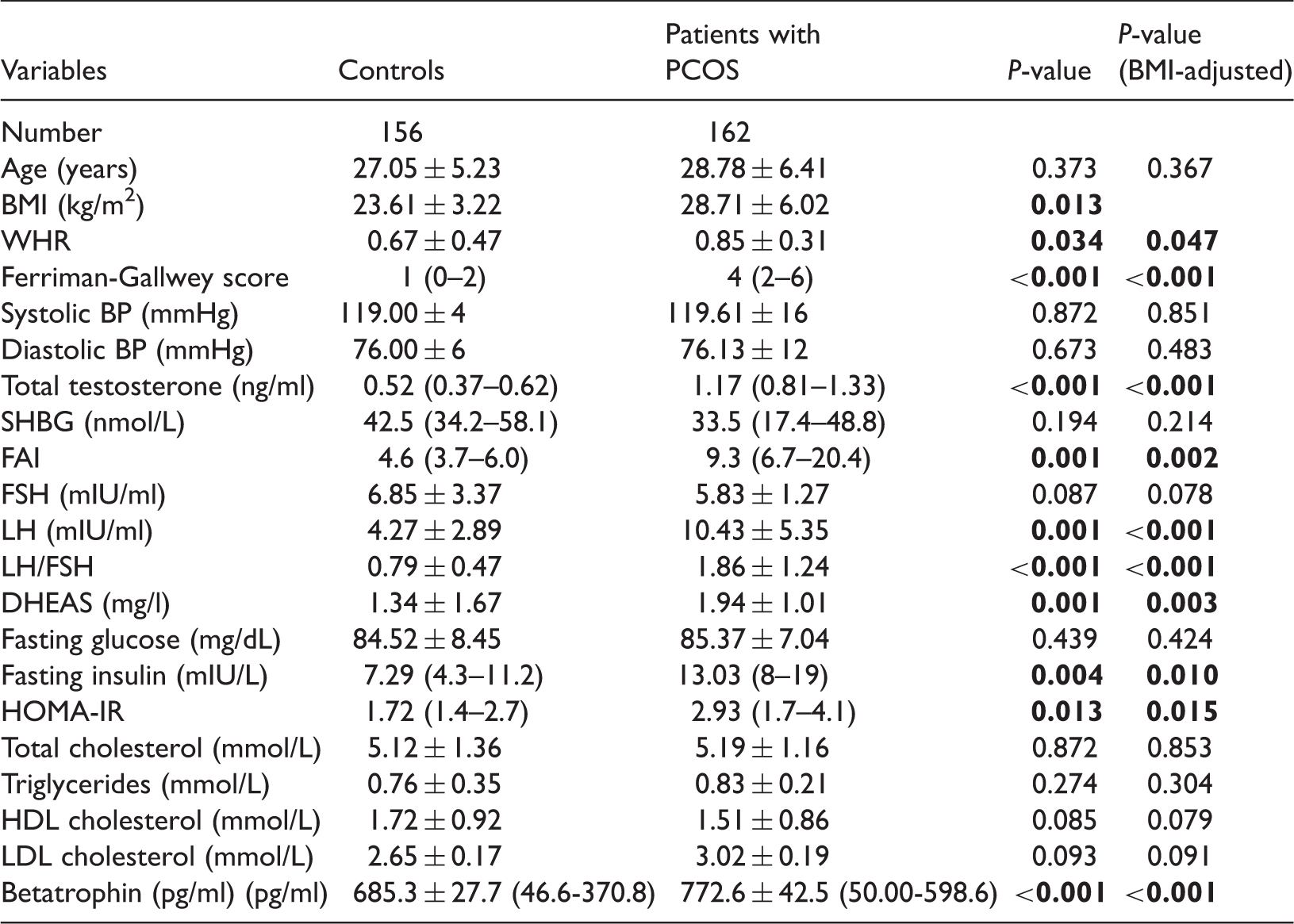
Abbreviations: BMI, body mass index; WHR, waist to hip ratio; BP, blood pressure; SHBG, sex hormone–binding globulin; FAI, free androgen index; FSH, follicle stimulating hormone; LH, luteinizing hormone; DHEAS, dehydroepiandrosterone sulfate; HOMA-IR, homeostasis model assessment of insulin resistance; HDL, high-density lipoprotein; LDL, low-density lipoprotein. Values are expressed as mean ± SD or median (interquartile range). P-values were obtained from unpaired two-tailed Student’s t-test or Mann-Whitney U-test. Clinical indexes with significant differences (P < 0.05) are in bold.
Notably, betatrophin concentrations were significantly higher in patients with PCOS than those in control patients (Table 1, P < 0.001). Further separation of the subjects according to the presence of insulin resistance revealed a significant difference in betatrophin concentrations between the four groups (Figure 1). One-way analysis of variance demonstrated significantly different betatrophin levels between the groups (F = 21.14, P < 0.01). Further analysis with the LSD-t test revealed significantly higher betatrophin levels in patients with PCOS and insulin resistance compared with those in patients with PCOS and control patients without insulin resistance (832.7 ± 98.2 vs. 775.5 ± 66.2 pg/ml, P = 0.013 and 832.7 ± 98.2 vs. 662.9 ± 72.0 pg/ml, P < 0.001). However, betatrophin levels did not differ significantly between control patients with insulin resistance and those without (769.4.7 ± 43.1 vs. 735.3 ± 72.0 pg/ml).
Betatrophin levels in women with PCOS and control women according to insulin resistance status. Data are expressed as means ± SD. *P < 0.05, one-way analysis of variance followed by LSD-t tests.
To study the potential association between PCOS and fasting insulin levels, we further conducted a one-way analysis of covariance using betatrophin levels as the dependent variable, PCOS as the independent variable (two levels), and fasting insulin as the covariate (data not shown). This analysis (between-subjects factor: PCOS, control) indicated that the main effect of PCOS (F = 0.115) was statistically significant (F = 7.03, P = 0.013). Furthermore, the main effect of insulin concentration was also statistically significant (F = 9.83, P = 0.003), but no statistically significant interaction between the two factors was identified (F = 2.33).
Partial Pearson’s or Spearman rank correlation coefficients of betatrophin concentrations and subject characteristics.
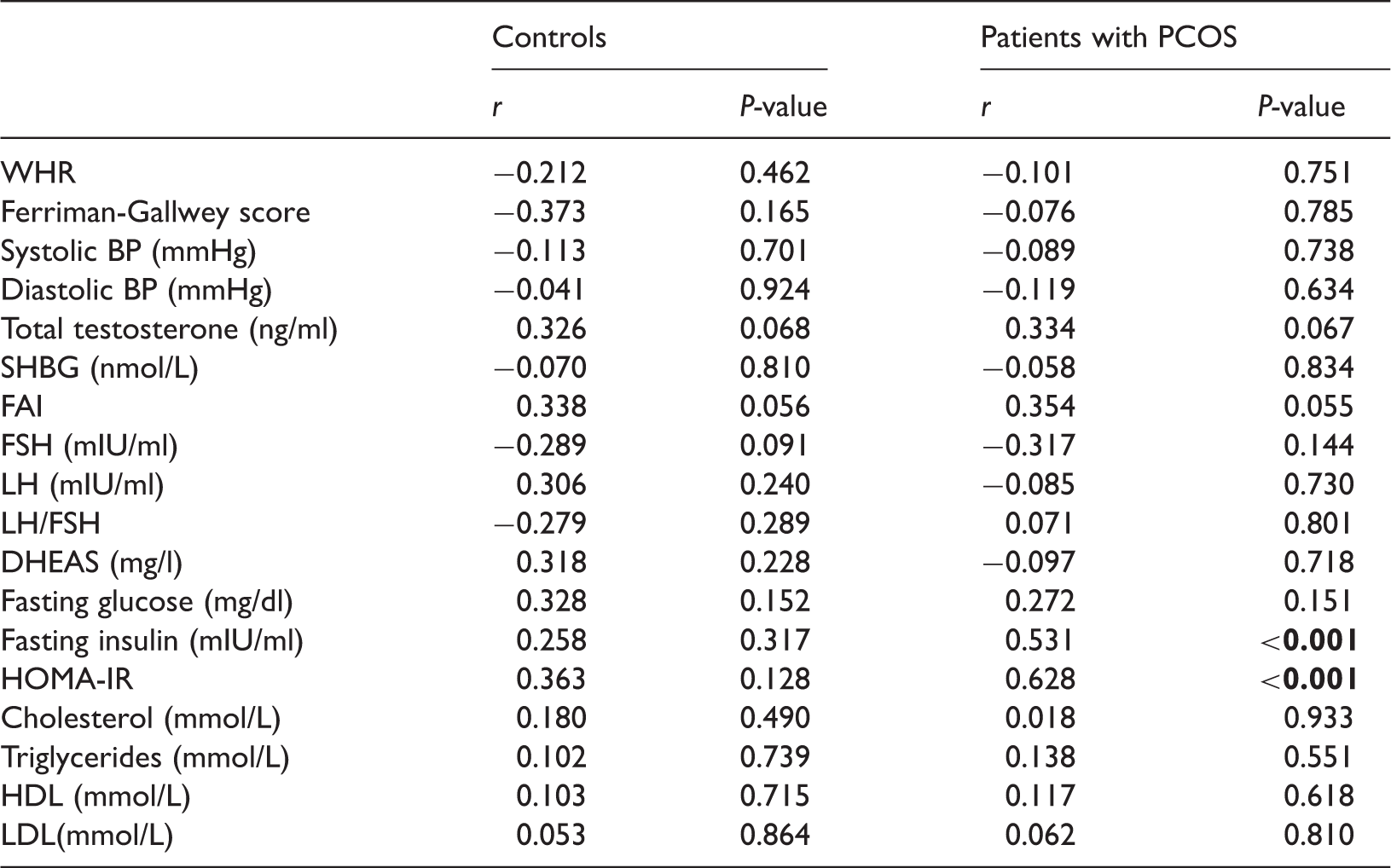
Abbreviations: WHR, waist to hip ratio; BP, blood pressure; SHBG, sex hormone–binding globulin; FAI, free androgen index; FSH, follicle stimulating hormone; LH, luteinizing hormone; DHEAS, dehydroepiandrosterone sulfate; HOMA-IR, homeostasis model assessment of insulin resistance; HDL, high-density lipoprotein; LDL, low-density lipoprotein. The correlation coefficient (r) and P-value were adjusted for age and body mass index. Clinical indexes with significant differences (P < 0.001) are in bold.
Results of a multivariate linear regression analysis of selected variables performed for betatrophin concentrations in patients with PCOS.

Abbreviations: BMI, body mass index; HOMA-IR, homeostasis model assessment of insulin resistance; FAI, free androgen index. Clinical indexes with significant differences (P < .05) are in bold.
Discussion
In the present study, our data demonstrated that betatrophin levels were significantly increased in patients with PCOS. When we sub-grouped subjects according to the presence of insulin resistance, women with PCOS and insulin resistance exhibited higher betatrophin concentrations. A one-way analysis of covariance demonstrated that both fasting insulin levels and PCOS diagnosis correlated with betatrophin levels. Furthermore, betatrophin levels were significantly correlated with fasting insulin levels and HOMA-IR only in patients with PCOS.
Betatrophin has recently been introduced as a novel potent stimulator of β-cell replication and improved glucose tolerance by increasing the β-cell division rate in mouse models of insulin resistance. 7 There is evidence suggesting that betatrophin expression can be induced by a high-fat diet and insulin, resulting in increased serum triglyceride levels and insulin resistance instead of improved glucose metabolism.13,26 However, several reports have indicated that betatrophin was increased in T2DM and type 1 diabetes mellitus,10–17 indicating that betatrophin could be a potent diagnostic biomarker for T2DM. 27 Of note, a recent meta-analysis demonstrated that circulating betatrophin levels in patients with T2DM were higher than those of non-diabetic adults in the non-obese, but not in the obese, population. 8 This finding suggests that betatrophin plays a role in the pathogenesis of insulin resistance and T2DM. In addition to T2DM, Ebert et al. 15 determined that women with gestational diabetes mellitus had significantly higher betatrophin levels compared with those of healthy pregnant controls. Furthermore, gestational diabetes mellitus status positively predicted circulating betatrophin levels. Additionally, mounting evidence from recent animal-based studies has suggested that betatrophin associates with lipid metabolism. Mice lacking betatrophin had a 70% reduction in plasma triglyceride levels compared with those of littermate control subjects. 26 However, to date, no studies have examined whether betatrophin is associated with PCOS, though growing evidence has suggested that insulin resistance and dyslipidaemia play critical roles in its pathophysiology.
As indicated in this study, we determined that circulating betatrophin levels were markedly increased in Chinese patients with PCOS compared with those in the control group. Moreover, a Spearman rank analysis demonstrated that serum betatrophin levels were significantly positively associated with indexes of insulin resistance, including fasting insulin levels and HOMA-IR. These findings corroborate those of a previous population-based study that indicated that serum betatrophin levels were elevated in patients with T2DM and associated with insulin resistance. 14 However, it is unclear whether increased betatrophin expression is a compensatory response or only a marker of insulin resistance in PCOS. Notably, increased circulating betatrophin levels were identified in women with PCOS and insulin resistance but not in control women with insulin resistance. Nonetheless, the increased betatrophin levels in subjects with PCOS are interesting and raise the question regarding the actual function of betatrophin, particularly after recent reports confirming that betatrophin does not affect beta cell expansion in mice 28 or humans. 29 Additionally, it is postulated that betatrophin as a novel hormone may be involved in the generation of an atherogenic lipid profile. 18 However, beyond glucose metabolism, we did not find that betatrophin levels significantly associated with the lipid profile. Therefore, it would appear that different mechanisms are involved in the regulation of betatrophin levels in PCOS. However, we cannot exclude the possibility that elevated betatrophin levels may be associated with other etiological factors in PCOS, which may affect insulin resistance. In a recent study, Yi et al. 27 determined that betatrophin could be a potent diagnostic biomarker for T2DM in an indigenous Chinese population, implying that betatrophin might be the driving cause of the disease. More studies are required to determine the mechanisms underlying the role of betatrophin in PCOS.
Similarly, Calan M et al. 30 and Song S et al. 31 revealed that betatrophin levels were higher in patients with PCOS than those in the control group. Moreover, Calan M et al. 30 demonstrated a positive correlation between betatrophin levels and HOMA-IR in patients with PCOS and control subjects, which is consistent with our present result. However, Song S et al. 31 determined that serum betatrophin levels were negatively correlated with HOMA-IR. Conversely, Erbag G et al. 32 in a small sample study (30 patients with PCOS and 27 without PCOS) identified significantly lower betatrophin levels in patients with PCOS. In the same study, betatrophin levels displayed a strong negative correlation with HOMA-IR. The different findings may be related to the use of different ELISA kits, different ethnic groups, or the design and sample size of each study.
To evaluate which parameters were independently associated with betatrophin levels in PCOS, a multiple regression analysis was performed. We identified HOMA-IR as the only parameter that remained statistically significant. We therefore conclude that insulin resistance was the primary contributing factor to elevated betatrophin concentrations in this cohort of patients with PCOS. Thus, betatrophin levels are evidence of a PCOS-associated disorder rather than a PCOS diagnosis, possibly indicating a state of oxidative stress and inflammation, and are strongly associated with insulin resistance in patients with PCOS.
The limitations of the present study included the relatively small sample size, which precluded stratification of groups by BMI for comparison, and the cross sectional nature, which prevented us from establishing causality. Another limitation in our study is the lack of assessment of betatrophin levels on different days of the menstrual cycle in subjects. Therefore, further studies are required to investigate the associations between betatrophin levels and clinical phenotype and pro-inflammatory markers in normal-weight versus obese women with PCOS, as well as to better characterize betatrophin secretion throughout the menstrual cycle.
In conclusion, we have provided the first evidence that serum betatrophin concentrations were markedly increased in patients with PCOS compared with those of control subjects. Our findings also suggest a possible association between betatrophin levels and PCOS. However, additional studies are needed to elucidate the role of betatrophin in PCOS development and determine whether targeting betatrophin could hold promise for PCOS treatment.
Footnotes
Acknowledgements
The authors sincerely thank all of the patients for their participation in the study and all of the staff in the Department of Reproductive Medicine for their assistance in every step of this study.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial or not for-profit sectors.
