Abstract
Objective
To examine the relationship between nutritional intake and bone mineral density (BMD) in postmenopausal Korean women.
Methods
Dietary intake was recorded in postmenopausal Korean women using a semiquantitative questionnaire. The frequency of consumption of various food groups and nutrient intake were calculated. BMD T-scores were measured at the lumbar spine, femoral neck and total hip using dual-energy X-ray absorptiometry. Associations between T-scores and dietary intake were analysed using partial correlation coefficients and multiple linear regression analysis.
Results
A total of 189 postmenopausal women were included in the study. β-Carotene intake was positively correlated with the lumbar spine T-score. Sodium and vitamin C intake were positively associated and folate intake negatively associated with the femoral neck T-score. Sodium, zinc and vitamin C intake were positively correlated and potassium intake was negatively correlated with the total hip T-score. Vegetable intake showed a positive association with the femoral neck and total hip T-scores.
Conclusion
In postmenopausal Korean women, β-carotene, vitamin C, zinc and sodium intakes were positively associated with bone mass. Furthermore, frequency of vegetable consumption was positively associated with femoral neck and total hip T-scores.
Introduction
Osteoporosis is a common condition that was estimated to affect over 38% of females aged 50 years and older in the Korean population in the Korea National Health and Nutrition Examination Survey undertaken from 2008 to 2011. 1 The prevalence of osteoporosis increases after the menopause, with the reduction in oestrogen secretion in postmenopausal women resulting in decreased bone density that can lead to osteoporosis. 2 According to a population projection, nearly half of the females in South Korea will be postmenopausal by 2030. 3
Bone mass is associated with various lifestyle factors such as diet, physical activity and smoking.4,5 Adequate nutrient intake is important for the prevention of osteoporosis in postmenopausal women. 4 It is generally accepted that balanced diets that include adequate dairy products contribute to healthy bone status. 6 Several studies have demonstrated that particular nutrients, especially calcium and vitamin D, are associated with bone mineral density (BMD). 7 Calcium and vitamin D supplementation in the elderly was shown to reduce bone loss in the femoral neck, spine and total body over a 3-year study period and was also associated with a reduced incidence of non-vertebral fractures. 8 Further studies have assessed the relationship between bone density and other specific nutrients, including vitamins and essential fatty acids. 9 Antioxidant vitamins and carotenoids, which occur in abundance in vegetables, may have positive effects on bone health, possibly because of their alkaline-forming properties.10–12 However, the association between bone mass and the intake of vegetables and other particular nutrients in postmenopausal Korean women is not well understood. The present study aims to examine the relationships between vegetable intake and bone mass in postmenopausal Korean women, and to further investigate the association between various nutrients and indexes of bone mass to provide nutritional recommendations for the prevention of osteoporosis.
Subjects and methods
Subjects
In this cross-sectional, hospital-based study, postmenopausal Korean women aged 50–75 years who had attended the gynaecology department of one of 10 hospitals in Seoul, Republic of Korea, for a regular health examination or for management of chronic diseases from April 2009 to October 2009 were recruited. Subjects were excluded if they had recently changed their diet or had chronic diseases such as diabetes mellitus, chronic kidney disease, rheumatoid arthritis, thyroid disease, parathyroid disease or malignancy. Subjects who had taken medications known to affect bone metabolism (including corticosteroids) within the past 3 months were also excluded.
All study participants provided written informed consent. The study protocol was reviewed and approved by the institutional review board of the Soonchunhyang University Hospital (Ethics Committee reference number SCHUH 2009-49) as a representative of the 10 hospitals involved in the study.
Anthropometric measurements and assessment of BMD
In all study participants, BMD was measured at the lumbar spine (L1–L4), femoral neck and total hip using dual-energy X-ray absorptiometry (Lunar Prodigy Advance whole body bone densitometer, GE Healthcare, Chicago, USA). The T-score was derived from a comparison between the measured BMD values and the mean BMD of healthy young females. 13 Body weight and height were measured to the nearest 0.1 kg and 0.1 cm using a scale or wall-mounted extensometer, respectively, by trained nurses. Height and weight measurements were recorded after an overnight fast, with the subjects wearing lightweight hospital gowns and no shoes. Body mass index (BMI) was calculated from the weight in kilograms divided by the height in metres squared.
Measurement of covariates and dietary assessments
Data was obtained using structured questionnaires administered by trained nurses or dieticians. Age and smoking habits were recorded, with subjects being categorized as non-smokers or smokers (including former smokers).
The dietary intake of nutrients and foods was measured using a semiquantitative food-frequency questionnaire (SFFQ) that covered 103 types of commonly consumed Korean foods selected from the 1998 National Health and Nutritional Survey of the Korean population. 14 The validity and reliability of the SFFQ in the Korean population has been verified. 15
The SFFQ was used to document the previous year’s food consumption habits. Study participants were given detailed instructions on estimating portion size, using pictorial representations to aid standardization. Frequency of intake was categorized as never or seldom, once a month, two or three times a month; one or two times a week, three or four times a week, five or six times a week, once a day, twice a day, or three or more times a day. The selected frequency category for each food was then used to calculate the daily intake. Nutrient intakes were calculated using a computer-aided nutritional analysis program (CAN-Pro 3.0, The Korean Nutrition Society, Seoul, Republic of Korea), apart from vitamin D intake, which was estimated using a Korean reference database. 16
The intakes of energy (calories), protein (total protein, animal protein, vegetable protein, isoflavone), fat (total fat, animal fat, plant fat, total fatty acids, saturated fatty acids, monounsaturated fatty acids, polyunsaturated fatty acids, omega-3, omega-6), carbohydrate, fibre, vitamins (A, B1, B2, B6, niacin, folate, riboflavin, C, D, E) and minerals (calcium, phosphorus, iron, sodium, potassium, zinc) were calculated for each study participant. Foods were categorized based on similarity of nutrient profiles or culinary usage into 12 groups: grain, fruit, seafood (excluding fish), fish, vegetables, mushrooms, dairy products, meat, soup or pot stew, tea, sugar and nuts.
Statistical analyses
Results were given as the mean ± SD. Normality for continuous variables was tested using the Shapiro–Wilk test. As all the nutrient intakes and food frequencies were abnormally distributed, natural log transformation was performed, following which all the variables were normally distributed.
After adjusting for age, BMI and energy intake, the partial correlation coefficient was calculated to determine correlations between the lumbar spine, femoral neck and total hip T-scores and nutrient intakes. To examine correlations between BMD and food frequencies, partial correlation analysis adjusted for age and BMI was performed. Backward stepwise selection using the variables found to be related to BMD on partial correlation analysis was conducted to determine which variables were independent and significant predictors of BMD. These variables were then investigated using multiple linear regression analysis. A P-value < 0.05 was considered to be statistically significant. All analyses were performed using SPSS software version 17.0 (SPSS Inc., Chicago, USA).
Results
General characteristics of the postmenopausal study participants (n = 189).

Data presented as mean ± SD or number of subjects (%).
Nutrient intake in postmenopausal women (n = 189).

Data presented as mean ± SD.
Frequencies of consumption of food groups in postmenopausal women (n = 189).
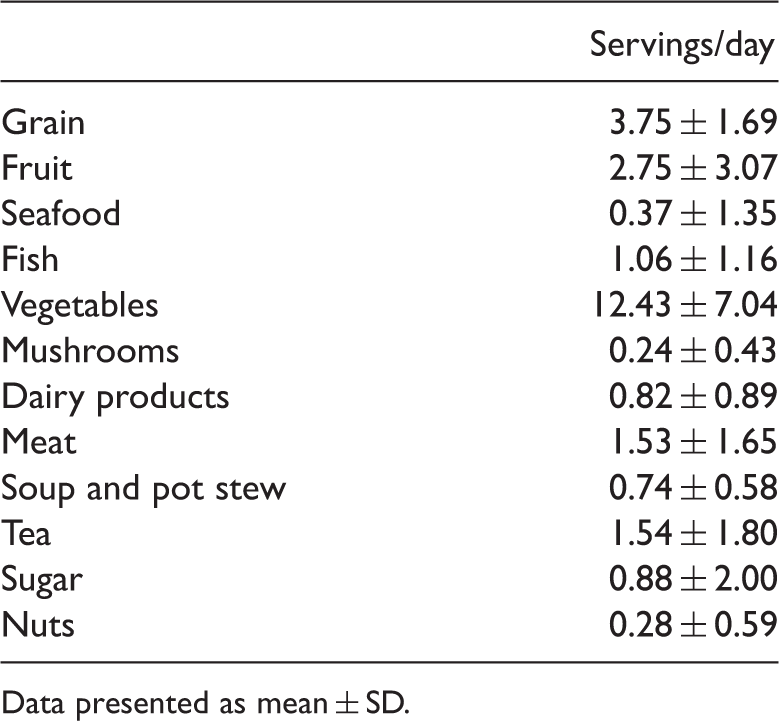
Data presented as mean ± SD.
Partial correlation coefficients adjusted for age, body mass index and energy intake between bone mineral density T-scores of the lumbar spine, femoral neck and total hip and daily nutrient intakes in postmenopausal women (n = 189).
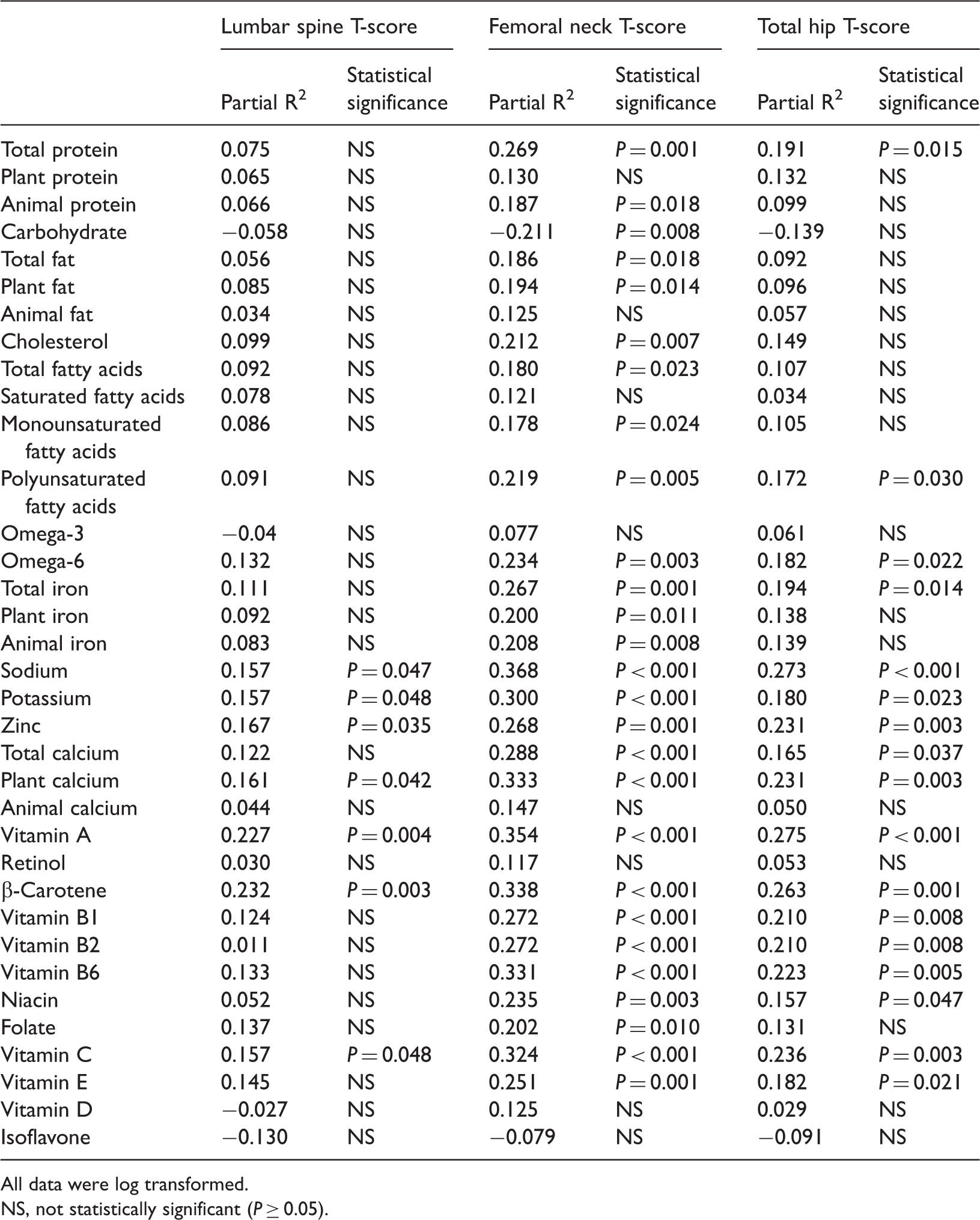
All data were log transformed.
NS, not statistically significant (P ≥ 0.05).
Partial correlation coefficients adjusted for age and body mass index between bone mineral density T-scores of the lumbar spine, femoral neck and total hip and frequencies of consumption of food groups in postmenopausal women (n = 189).
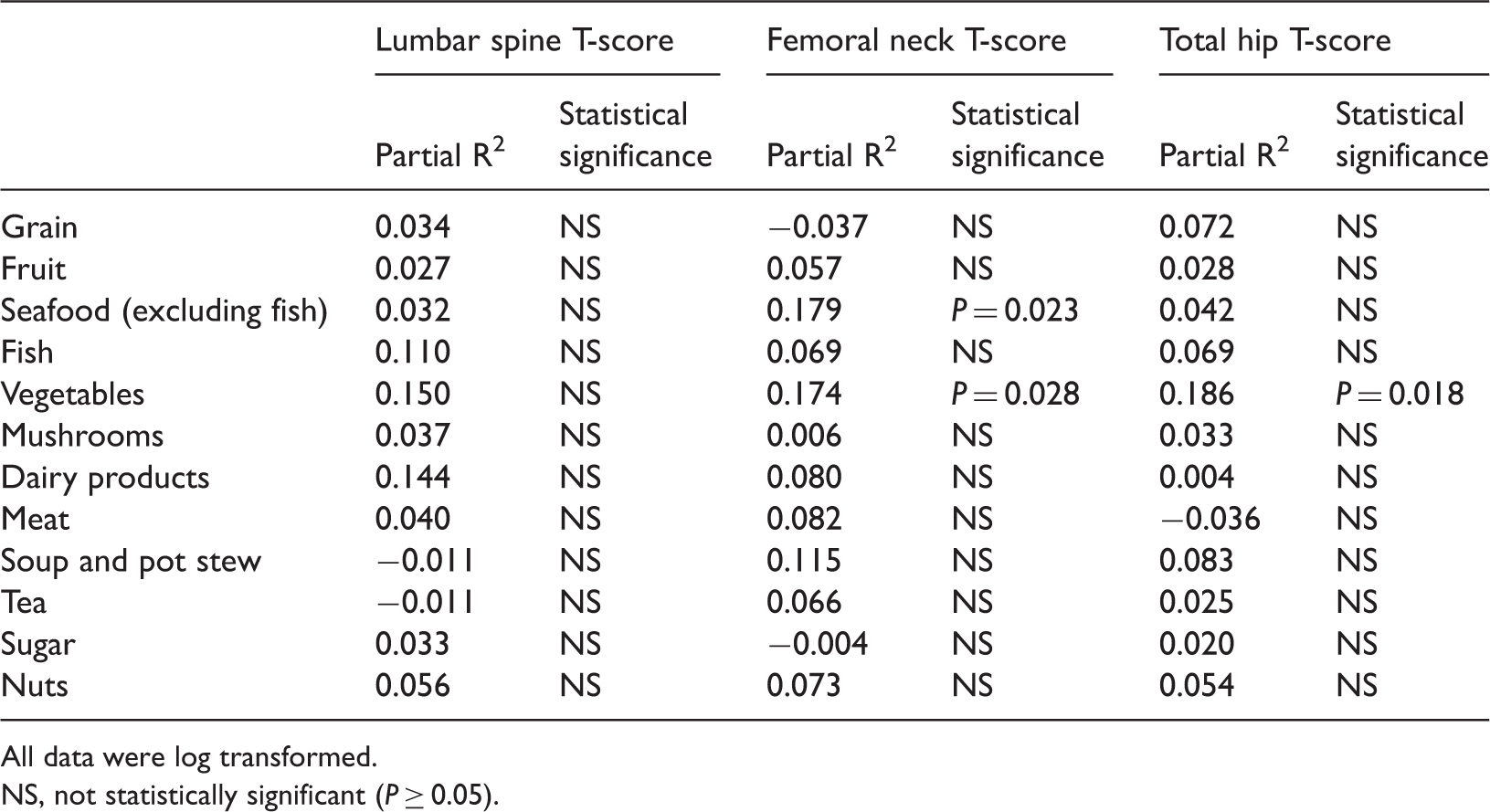
All data were log transformed.
NS, not statistically significant (P ≥ 0.05).
Independent variables found on multiple linear regression analysis of the associations between bone mineral density T-scores of the lumbar spine, femoral neck and total hip and daily nutrient intakes, age and body mass index.
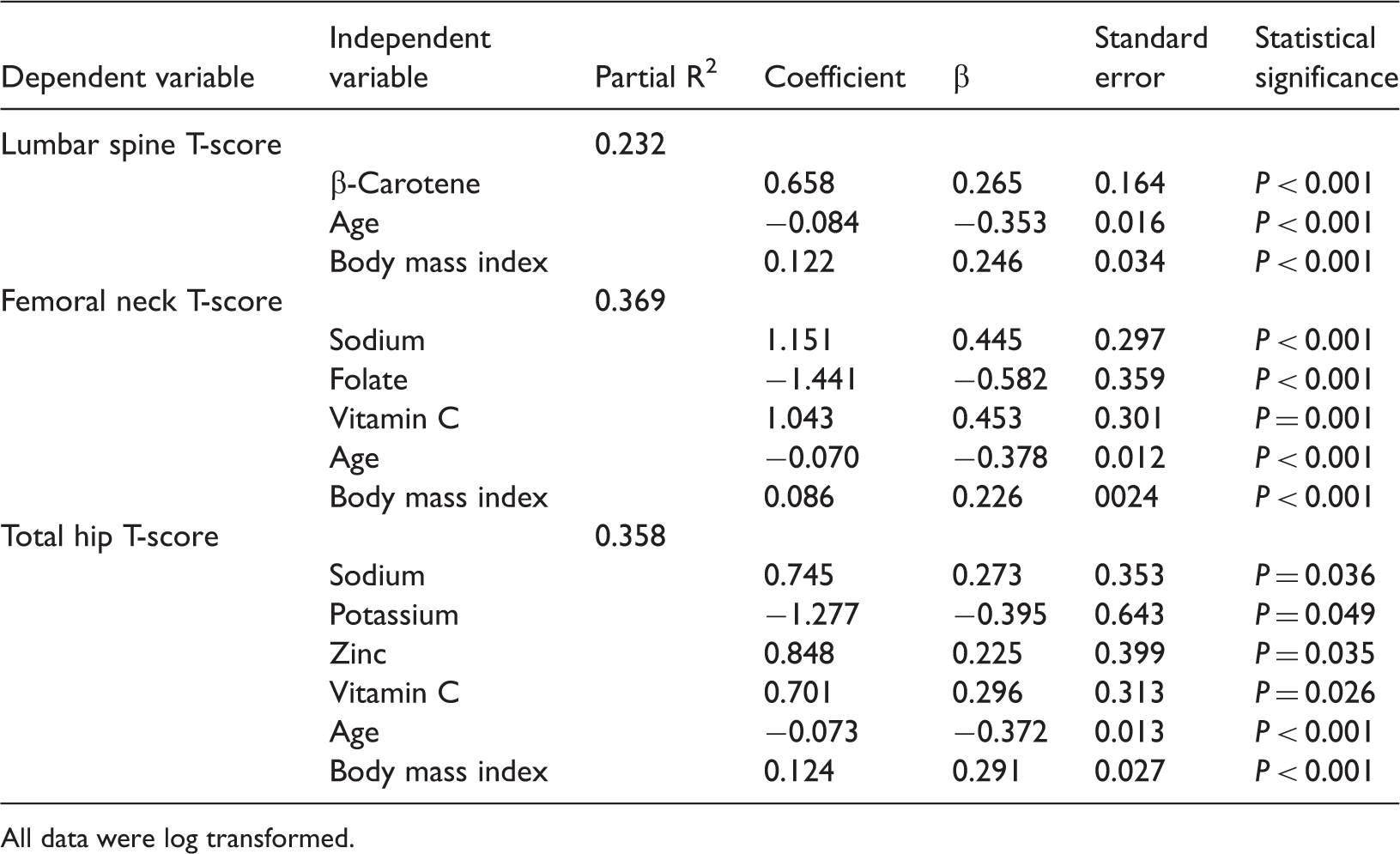
All data were log transformed.
Independent variables found on multiple linear regression analysis of the associations between bone mineral density T-scores of the lumbar spine, femoral neck and total hip and frequencies of consumption of food groups, age and body mass index.
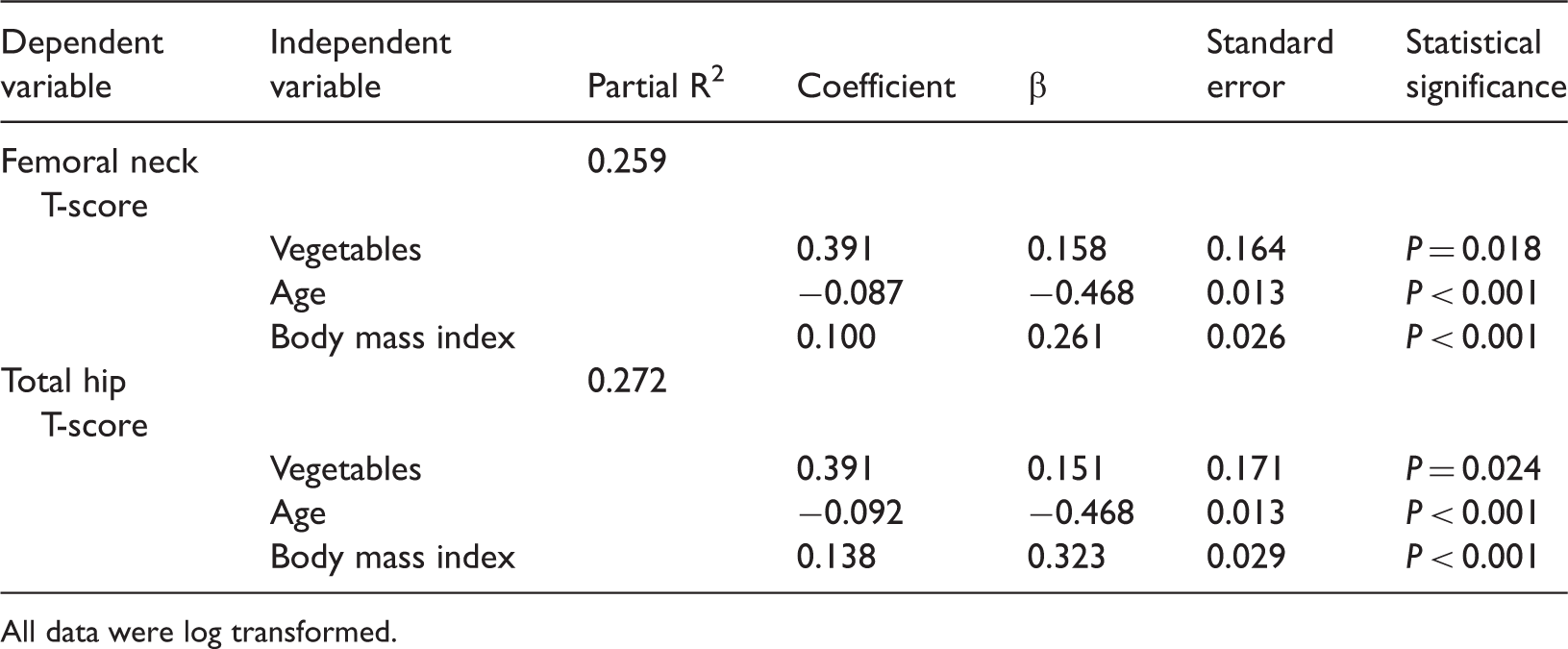
All data were log transformed.
Discussion
Nutrition can be an important modifying factor in the development and maintenance of bone mass. Effective prevention and treatment of osteoporosis in postmenopausal women is also dependent on nutritional factors.
In the present study, multiple regression analyses of food frequencies and BMD showed that the frequency of vegetable consumption was significantly associated with the T-score of the femoral neck and total hip. These results are in agreement with those of other studies. In a nationwide, community-based study of farmwomen in Japan, a high intake of green and dark yellow vegetables positively correlated with BMD whereas a high intake of meat tended to be inversely associated with BMD. 17 Vegetable intake may be an important factor in increasing BMD because vegetables are a good source of alkalizing nutrients, which can inhibit bone resorption and reduce urinary calcium excretion. 18 Antioxidant vitamins can also reduce oxidative stress, which is known to have a negative impact on BMD.10,19 Vitamin C has been found to be essential for the stable formation of collagen and osteoblast differentiation. 20 In addition, alkaline ions (dietary potassium and magnesium) and fruit and vegetables have been reported to be associated with a higher BMD in elderly subjects. 21
Multiple linear regression analyses of individual nutrients and BMD in the present study revealed that β-carotene intake was positively associated with the T-score of the lumbar spine. It has been previously reported in postmenopausal women that dietary β-carotene intake was positively associated with lumbar spine bone mass 22 and that serum β-carotene was positively correlated with radial BMD. 23 The role of dietary antioxidant carotenoids in osteoporosis is not yet well documented. These exist in abundance in vegetables, and serum levels of carotenoids have been shown to increase with increasing frequency of reported servings of vegetables. 12 Therefore a high intake of vegetables rich in antioxidant carotenoids might be beneficial for bone health in postmenopausal women.
Positive correlations between dietary vitamin C intake and the T-score of the femoral neck and total hip on multiple linear regression analysis were observed in the present study. This may be due to the metabolic effects of vitamin C, which is known to stimulate procollagen, enhance collagen synthesis and stimulate alkaline phosphatase activity, a marker for osteoblast formation. 20 Many studies have reported a potentially beneficial role for vitamin C in the prevention of low BMD.24,25 Vitamin C supplements have been shown to have a beneficial effect on levels of BMD, especially among postmenopausal women. 20
Vitamin D is a well-known beneficial nutrient for bone health. However, the beneficial effect of vitamin D on bone mass may depend on the level of intake and other factors. A meta-analysis suggested that low-dose vitamin D (<400 IU/day orally) was ineffective for fracture prevention, with a decrease in risk only occurring in elderly individuals receiving 700 IU or more per day. 26 In the present study, the average intake of vitamin D was 240 IU, which represents only 60% of the recommended Korean dietary reference intake for postmenopausal women. 27 The present study therefore suggests that too low an intake of vitamin D may be ineffective for bone health.
Folate is effective in normalizing homocysteine levels because it is critical for the conversion of the amino acid methionine to cysteine. 28 Elevated levels of homocysteine may increase the risk of osteoporosis because homocysteine interferes with collagen cross-linking, which can lead to poor bone quality. 29 Gjesdal et al. 30 reported that high levels of homocysteine and low levels of folate were negatively associated with BMD in women but not in men. However, in the present study, folate intake was negatively associated with the T-score of the femoral neck on multiple linear regression analysis. Additional research is needed to confirm the possible roles of folate and homocysteine in postmenopausal women before specific recommendations can be made for the prevention or treatment of osteoporosis.
In the present study, dietary zinc intake was significant positively associated with the T-score of the total hip on multiple linear regression analysis. Zinc is involved in the stimulation of bone formation by osteoblasts and the inhibition of bone resorption by osteoclasts. 31 Associations between BMD and zinc supplements have been reported in patients with thalassaemia. 32
Many clinical studies have demonstrated that sodium intake is negatively associated with BMD due to sodium causing an increase in renal calcium excretion. 33 In the present study, multiple linear regression analysis showed that sodium intake was positively associated with the T-score of the femoral neck and total hip, which does not support a detrimental effect on BMD for dietary sodium. Excessive sodium intake is a common nutritional problem in Korea; the mean ± SD sodium intake of the study participants was 4436 ± 2041.17 mg/day, despite the fact that the World Health Organization (WHO) recommends a maximum daily intake of 2000 mg. 34 It is possible that dietary sodium intake may be positively correlated with other nutrients in the Korean dietary pattern, and the association of higher sodium intake with a higher BMD needs further evaluation.
Potassium was positively correlated with BMD using simple correlation analysis. However, multiple linear regression analysis showed that potassium intake was negatively associated with the T-score of the total hip. Potassium is important for calcium homeostasis, particularly the urinary conservation and excretion of calcium. 35 In a cross-sectional study, higher potassium intake was significantly associated with higher BMD in both men and women. 21 The mean ± SD potassium intake of the study participants was 3183.59 ±1252.60 mg/day, which is considerably lower than the WHO recommended daily intake of 3510 mg. 36 Further investigation is required to determine the influence on bone health in postmenopausal women of potassium intake within the range of current recommendations.
Milk and other dairy foods are a major source of calcium and other essential nutrients. Milk has an abundance of protein, phosphorus and calcium, which are crucial for bone formation. Many studies in Korea and elsewhere, both epidemiological and experimental, have shown that drinking milk improves bone health. 37 However, the present study did not show a positive correlation between dairy food intake and the T-score of various skeletal sites. This could be partially explained by the lack of dairy food in many common Korean dishes. The recommended Korean dietary guideline for adults and the elderly is one or two servings of dairy products per day, 27 but in the present study the participants’ intake of dairy products was low, with an average consumption rating of only 0.82 servings per day.
According to the report of Choi et al., 38 the prevalence of osteoporosis in Korean adults is higher than in Caucasians; the prevalence was 38% in Korean females aged 50 years and older. Park et al. 1 reported that the BMD at every skeletal site was significantly lower in Korean females than in those in the US. They suggested that these differences in prevalence may be related to the different skeletal sizes common to each race, but may also be related to differences in nutritional intake, including the intake of calcium, and activity between these populations. Dietary recommendations are likely to be helpful, but further prospective studies are required to make firm recommendations with respect to osteoporosis. Understanding the relationships between nutrients may be an important step toward the identification of dietary factors related to the prevention of osteoporosis, especially in postmenopausal women.
The focus of the present study was to investigate correlations between dietary nutrients and BMD T-scores in postmenopausal Korean women. However, it is difficult to draw firm conclusions concerning the factors that influence BMD due to the cross-sectional nature of the study and the small sample size. In addition, the intake of nutrients was based solely on responses to the SFFQ and so accuracy was limited. However, since the questionnaire covered the previous year’s consumption, the results may better reflect long-term nutritional intake than responses that only relate, for example, to the previous 24 h. The present study did not measure levels of oestrogen and parathyroid hormone, which are known to be significantly associated with BMD,2,39 but the questionnaire responses did identify other factors, such as smoking habits, that may have an impact on BMD in postmenopausal women. Due to the complexity of the roles of dietary nutrients in bone health, further investigations of the mechanisms underlying these relationships may improve understanding of the epidemiological data.
In conclusion, the present study in postmenopausal Korean women found that β-carotene, vitamin C, zinc and sodium intake were positively associated with BMD, and that the frequency of vegetable consumption was positively associated with femoral neck and total hip T-scores.
Footnotes
Acknowledgements
We express our sincere thanks to Professor Kirk Olgin, Glendale Community College, California, USA, for correcting the manuscript. We also thank Dong Won Byun (College of Medicine, Soonchunhyang University Hospital) for his contributions to the data collection.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
