Abstract
Objective
To evaluate serum micro RNA-143 (miR-143) levels in patients with sepsis or non-infectious systemic inflammatory response syndrome (SIRS), and investigate its possible diagnostic or prognostic value.
Methods
Serum was obtained from patients with sepsis or SIRS and healthy control subjects. Relative miR-143 expression was determined using quantitative real time polymerase chain reaction. The diagnostic and prognostic value of serum miR-143 was evaluated.
Results
Serum miR-143 levels were significantly higher in patients with sepsis (n = 103) than patients with SIRS (n = 95) and healthy controls (n = 40). There were significant positive correlations between serum miR-143 level and SOFA and APACHE II scores in patients with sepsis (r = 0.794 and r = 0.825, respectively). Serum miR-143 had a sensitivity of 78.6% and specificity of 91.6% for distinguishing between sepsis and SIRS. There was no association between serum miR-143 and 28-day survival in patients with sepsis.
Conclusion
Serum miR-143 is elevated in patients with sepsis, and may be a useful biomarker for distinguishing between sepsis and SIRS.
Keywords
Introduction
Sepsis is a serious medical condition characterized by the simultaneous presence of infection and systemic inflammatory response syndrome (SIRS). 1 Despite progress in diagnostic and therapeutic techniques, sepsis remains the main cause of death for patients in intensive care units (ICUs), with a 30-day mortality rate of 47%. 2 Blood microbiological culture analysis is the gold standard to distinguish sepsis from SIRS without infection, but this technique is time-consuming and has a low early positive rate (14.9 % during days 1–5 after sepsis diagnosis). 3 Thus, biomarkers for the early diagnosis and accurate assessment of patients with sepsis are urgently required.
MicroRNAs (miRs) are a class of endogenous, noncoding, single stranded, small, regulatory RNA molecules of approximately 22 nucleotides in length 4 that regulate gene expression at the posttranscriptional level by inducing mRNA degradation or translational repression. 5 MiRs contribute to most basic biological processes, and aberrant miR expression has been observed in many human disease states including sepsis.6,7 More importantly, miRs are stably expressed in human serum or plasma. 8 Circulating miRs have been used as diagnostic and prognostic biomarkers in many diseases.9,10 Plasma levels of miR-150, 11 miR-146a, 12 miR-574-5p, 13 miR-15a 14 and miR-16 14 have been found to have prognostic or diagnostic value in sepsis.
MiR-143 is associated with sepsis in mouse lung, 15 as well as in human leukocytes after lipopolysaccharide (LPS) infusion. 16 Sepsis is a complex disease involving multiple organs and tissues, and changes in leukocyte miR expression may not be reflected in circulating miR levels.17,18 To our knowledge, the clinical significance of serum miR-143 levels in patients with sepsis has not been studied. The aim of the present study, therefore, was to evaluate serum miR-143 levels in patients with sepsis or non-infectious SIRS, and investigate its possible diagnostic or prognostic value.
Patients and methods
Study population
The study recruited patients with sepsis or SIRS undergoing treatment at the Department of Critical Care Medicine, Cangzhou Central Hospital, Cangzhou, Hebei Province, China, between January 2011 and May 2014. Patients were diagnosed on the basis of blood microbiological culture results, according to the definitions of the American College of Chest Physicians/Society of Critical Care Medicine. 19 Inclusion criteria were: two or more of (i) temperature > 38℃ or < 36℃; (ii) heart rate > 90/min; (iii) respiratory rate > 20/min or PaCO2 < 32 mmHg; (iv) white blood cell count > 12000/mm3, < 4000/mm3, or > 10 % immature (band) forms. Patients aged younger than 18 years or who could not receive adequate treatment due to economic hardship were excluded. In patients with sepsis, disease severity was assessed via SOFA (sepsis-related organ failure assessment) score 20 and APACHE II score 21 on day 1 after ICU admission, and all patients were followed-up for 28 days A control group of healthy volunteer subjects with no known medical condition or infection at the time of the study were recruited from the Health Screening Centre, Cangzhou Central Hospital, Cangzhou, Hebei Province, China.
The study was approved by the research ethics committee of Cangzhou Central Hospital, and all subjects provided written informed consent.
RT–PCR
Blood samples (5 ml) were obtained at the time of initial blood microbiological culture in patients, and at the time of health screening in the control subjects. Blood was centrifuged at 3500 × g for 10 min at room temperature immediately after collection to completely remove cell debris, then transferred to RNase/DNase-free tubes and stored at −80℃ until further processing.
Serum total RNA was extracted using TRIzol solution (Invitrogen, Carlsbad, CA, USA) according to manufacturer’s instructions, and cDNA was synthesized using a One Step Prime-Script miRNA cDNA Synthesis Kit (Takara Bio Inc., Shiga, Japan). Real-time quantitative PCR (RT–qPCR) was performed using a SYBR Prime-Script miRNA qPCR Kit (Takara Bio Inc., Shiga, Japan) with an ABI PRISM 7500 Sequence Detection System (Applied Biosystems, Foster City, CA, USA). Cycling conditions were 95℃ for 5 min, followed by 40 cycles of 95℃ for 15 s and 60℃ for 60 s. All PCR reactions were performed in triplicate, and U6 snRNA was used as an internal control. Expression levels of miR-143 were calculated relative to U6 mRNA using the equation 2−ΔC
CRP and PCT assays
Serum C-reactive protein (CRP) was quantified via scattering turbidimetry (CardioPhase hsCRP, Siemens, Munich, Germany), and procalcitonin (PCT) was quantified using an enzyme-linked fluorescence analysis kit (VIDAS B.R.A.H.M.S. PCT kit, bioMerieux SA, Marcy l’Etoile, France), according to the manufacturers’ instructions.
Statistical analyses
Sample size was calculated using the formula N = (Uα/δ)2 × (1–P) × P, assuming an estimated sensitivity of 80% and specificity of 90% for the validity of serum miR-143 as a biomarker for discriminating between sepsis and SIRS. We set α = 0.05, and δ = 0.08. Accordingly, the minimum sample size was 96 for the sepsis group and 54 for the SIRS group.
Data were expressed as mean ± SD or median (range). Differences in serum miR-143 levels were analysed using unpaired Student’s t test (between two groups) or one-way analysis of variance (ANOVA; between three groups). Pearson’s correlation analysis was used to analyse the relationship between serum miR-143 levels and clinical scores. Receiver-operating characteristic (ROC) curves were used to assess the diagnostic value of serum miR-143 levels for sepsis vs SIRS, and the area under curve (AUC) was calculated. Statistical analyses were performed using SPSS® version 16.0 (SPSS Inc., Chicago, IL, USA) for Windows®, and P-values < 0.05 were considered statistically significant.
Results
Demographic and clinical characteristics of patients with systemic inflammatory response syndrome (SIRS) or sepsis included in a study evaluating the value of micro RNA-143 (miR-143) in sepsis diagnosis and prognosis.

Data presented as n, mean ± SD, or median (range).
P < 0.01 vs SIRS, bP < 0.01 vs control, cP < 0.001 vs SIRS; unpaired Student’s t-test.
Relative to U6 mRNA expression.
CRP, C-reactive protein; PCT, procalcitonin; ICU, intensive care unit.
Data regarding miR-143 expression levels in patients with sepsis are shown in Figure 1. Patients with high SOFA scores (≥7) or APACHE II scores (≥ 10) had significantly higher serum miR-143 levels than those with low SOFA (< 7) or APACHE II scores (< 10) (P = 0.008 and Figure 1(b) P = 0.004, respectively; Figure 1(a) and Figure 1(b)). There was no significant difference in serum miR-143 levels between those patients who died and those who survived (at 28 days; Figure 1(c)). There were significant positive correlations between miR-143 level and SOFA score (r = 0.794, P < 0.01), and miR-143 level and APACHE II score (r = 0.825, P < 0.01).

The AUC of the ROC for miR-143 was 0.91 (95% CI 0.86, 0.95; Figure 2), higher than that of both PCT (AUC 0.89; 95% CI 0.84, 0.93) and CRP (AUC 0.82; 95% CI 0.74, 0.82). When using a cut-off level of 15.9 for serum miR-143, sensitivity was 78.6% (95% CI 69.5, 86.1) and specificity was 91.6% (95% CI 84.1, 96.3).
Receiver operating characteristic (ROC) curve for serum micro RNA-143 (miR-143), C-reactive protein (CRP) and procalcitonin (PCT) for diagnosis of sepsis vs systemic inflammatory response syndrome (SIRS).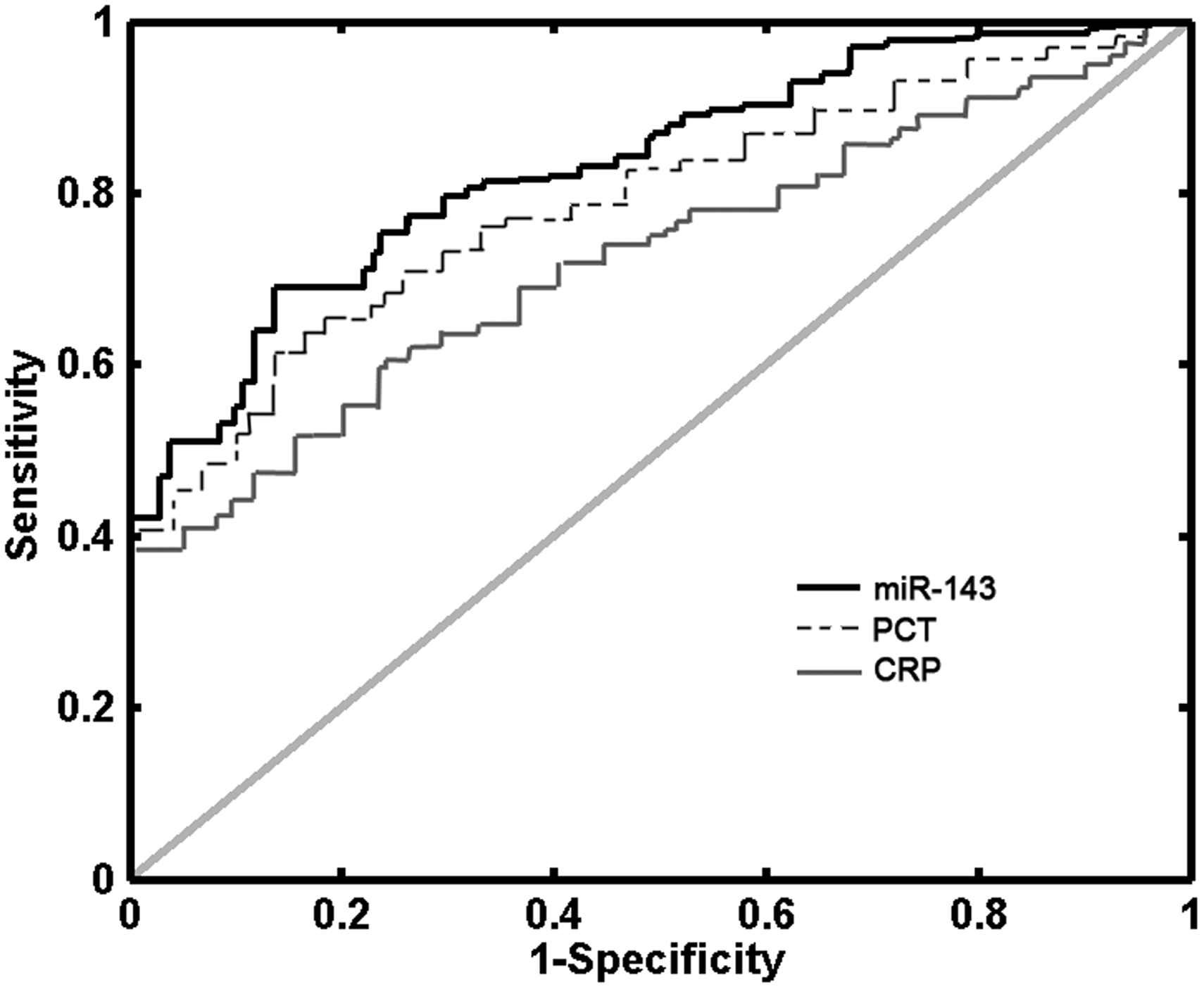
Discussion
Circulating levels of several miRs, including miR-146a and miR-15a, may assist in the differential diagnosis of sepsis and SIRS.12,14 In addition, serum miR-574-5p and miR-133a are prognostic predictors in sepsis,13,22 and serum miR-122 is associated with coagulation disorders in sepsis. 23 Levels of miR-25 are related to SOFA score and oxidative stress in patients with sepsis. 24 Serum miR-143 levels were increased in both patients with sepsis and those with SIRS compared with normal controls in the present study. More importantly, miR-143 levels could distinguish between sepsis and SIRS. High levels of miR-143 were positively correlated with SOFA and APACHE II scores. To our knowledge, this is the first study to analyse serum miR-143 levels and their diagnostic value in sepsis.
There is a known association between miR-143 and the human immune response. 16 In addition, miR-143 has been shown to regulate the anti-inflammatory effect of mesenchymal stem cells and may therefore be a potential therapeutic target. 25 Functional studies of miR-143 have largely focused on its role in carcinogenesis and cancer progression, and little is known about its effect on the immune response. It is therefore important to identify more miR-143 target genes in order to clarify its role in immunoregulation.
The present study has several limitations, including the retrospective design and relatively small sample size. In addition, we did not evaluate the source or mechanism(s) of action of miR-143 during sepsis, nor whether a combination of miR-143 and other biomarkers might be more practical in the differential diagnosis of sepsis and SIRS.
In conclusion, serum miR-143 is elevated in patients with sepsis, and may be a useful biomarker for distinguishing between sepsis and SIRS. Large-scale prospective studies are required to confirm our findings.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
