Abstract
Objective
To investigate the predictive baseline factors for a successful outcome following one dose of intravitreal triamcinolone acetonide (IVTA) in patients with macular oedema (ME) caused by branch retinal vein occlusion (BRVO).
Methods
This retrospective study enrolled patients with ME (macular retinal thickness [MRT] ≥ 300 µm) due to BRVO who still had ME 3 months after grid laser photocoagulation. Patients were divided according to treatment into an IVTA group and a laser-only group. The resolution of ME was documented at months 3 and 6.
Results
A total of 154 eyes with ME were investigated: IVTA group (90 eyes) and laser-only group (64 eyes). Predictive factors for successful IVTA treatment were younger age, shorter duration of ME, initial onset ME, accompanied by serous retinal detachment, few concomitant systemic diseases and nonischaemic BRVO. A broken foveal capillary ring was related to a poor treatment outcome. Eyes with cystoid spaces in the outer plexiform layer were more likely to have a good treatment response.
Conclusion
IVTA is effective for resolving ME due to BRVO after grid laser photocoagulation treatment.
Keywords
Introduction
Branch retinal vein occlusion (BRVO) is a common retinal vascular disease with an expected incidence of 0.5–1.2%. 1 One of the major causes of visual impairment in patients with BRVO is the development of macular oedema (ME), which occurs in ∼60% of cases. 2 The standard treatments for ME due to BRVO (which are prompt grid laser photocoagulation in eyes without dense macular haemorrhage and deferral of photocoagulation in eyes with dense macular haemorrhage) are based on the Standard Care versus Corticosteroid for Retinal Vein Occlusion (SCORE) study recommendations. 3 However, some eyes may be resistant to grid laser photocoagulation, especially when combined with haemorrhage or serous retinal detachment (SRD). 3 Despite using standard care, >30% of patients with BRVO-induced ME showed macular retinal thickness (MRT) >250 µm measured by optical coherence tomography (OCT) at 36 months post-treatment. 3
Intravitreal injection has been used for various retinal vascular diseases and has become the most frequently used treatment for ME.4–7 Some studies have shown promising results when using intravitreal injections of either triamcinolone acetonide (TA) or antivascular endothelial growth factor (anti-VEGF) agents.4–7 Studies have shown no significant differences in best corrected visual acuity (BCVA) and MRT values between intravitreal injections of an anti-VEGF agent and TA from baseline to 12 months after the initial injection.4–7 In contrast, other studies have demonstrated different outcomes after intravitreal injections of these two agents for ME secondary to BRVO.3,8 One study showed that intravitreal TA (IVTA) may improve macular sensitivity and morphology in patients with either ischaemic or nonischaemic BRVO. 8 However, in the SCORE study, there was no difference in visual acuity at 12 months for the TA groups compared with the standard care group. 3
Although repeated intravitreal injections have been used in the treatment of ME, no definite conclusion has been established for this strategy. 9 Research has demonstrated that both 3-monthly intravitreal injections of an anti-VEGF agent bevacizumab and two IVTA injections 2 months apart could be effective in respect to both visual and anatomical outcomes. 9 Response to TA differs among eyes with oedema, with some only needing one injection, while others often need repeated injections. 10 A study of the treatment of ME associated with BRVO reported that 22% of patients in the IVTA group required reinjection for recurrent ME. 10 Reasons for the variable response to IVTA remain unknown. Therefore, a clearer understanding of the multiple factors that are potentially associated with the response to IVTA treatment, in particular the factors that are associated with a good response to one dose of TA, might help medical personnel to better predict the prognosis of IVTA treatment and to select the most appropriate treatment for the individual patient. For example, using multiple anti-VEGF agent injections is likely to increase the cost of treatment, which may not be affordable to patients in some countries. ME is caused by multiple factors, including not only VEGF and but also other inflammatory factors, so some patients might be refractive to anti-VEGF treatment although they might respond to steroid treatment.11,12 Studies have evaluated the clinical characteristics and morphological predictive factors that are associated with the prognosis of ME.13–16 For example, a report demonstrated that several baseline characteristics might predict a better visual acuity outcome: these include young patient age, short duration of ME and no history of coronary artery disease. 17 Different morphological patterns in uveitic ME might represent different stages in uveitis-associated cystoid ME progression and the initial morphological appearance can be linked to clinical prognosis after treatment. 11 However, this previous study did not investigate the correlation between morphological pattern and the prognosis of ME caused by BRVO. 11
This study investigated the potentially predictive baseline factors, including morphological pattern, for a successful outcome following one dose of IVTA in patients with ME caused by BRVO.
Patients and methods
Study population
This retrospective, uncontrolled review study enrolled consecutive patients with ME (MRT ≥ 300 µm) due to BRVO in the Department of Ophthalmology, Ningxia Eye Hospital, Ningxia People’s Hospital, Yinchuan, Ningxia, China between January 2009 and December 2013. Patients who had received initial standard treatment for BRVO (grid laser photocoagulation) in whom ME remained present after 3 months were divided into an IVTA group and a laser-only group, based on the treatment that they had received. Inclusion criteria were: (i) patients with ME due to BRVO; (ii) received initial standard treatment; (iii) BCVA at least 20/40 or less after initial standard treatment; (iv) received one dose of IVTA without a second injection within the 6 months after the first injection (IVTA group only); (v) patients who had received initial standard treatment for BRVO with no other treatment other than at least one grid photocoagulation within the previous 3 months (laser-only group). Patients in the IVTA group were further subdivided into a ‘resolution group’ and a ‘relapsing group’, according to the MRT response to treatment at month 6. Baseline morphological features of ME due to BRVO in both IVTA subgroups were analysed. The following exclusion criteria were applied: (i) a history of retinal surgery; (ii) glaucoma; (iii) previous intravitreal anti-VEGF injection; (iv) pseudophakic eyes were excluded if the ME occurred within 6 weeks after cataract surgery; (v) those with retinal neovascularization at baseline.
The study was approved by the Ethics Committee of Ningxia Eye Hospital, Ningxia People’s Hospital, Yinchuan, Ningxia, China and adhered to the tenets of the Declaration of Helsinki. All patients provided written informed consent after they were informed about the risks/benefits of grid laser photocoagulation therapy and IVTA (which was offered as part of their routine therapy for ME), and for the use of their baseline and follow-up data from medical records for this retrospective analysis.
Investigational methods
Serous retinal detachment was defined as the presence of the retinal posterior surface elevated over a nonreflective cavity with minimal shadowing of the underlying tissues. 12 On OCT, it demonstrated typical accumulation of subretinal fluid, resulting in neurosensory retinal detachment covering the central 6 mm × 6 mm. In the IVTA group, the criterion for being in the ‘resolution group’ was that the MRT decreased <250 µm without recurrence; and the ‘relapsing group’ included patients with ME refractory to treatment and those with recurrent ME. Recurrence of ME was defined as an increase in the MRT ≥100 µm after initial recovery. Ischaemic BRVO was defined as that causing greater than a total of five disc diameters of nonperfusion on fluorescein angiography. Initial onset ME was defined as the occurrence of ME within the first 3 months after the first onset of BRVO. Chronic recurrent ME was defined as ME that recurred after initial recovery or ME that first appeared 3 months after the first onset of BRVO. ME was divided into different types according to the main anatomical location of the oedema in the eye. 18 The diagnosis of BRVO was based on the results of clinical examination and/or fluorescein angiography. The diagnosis and recurrence of ME were monitored by clinical examination, fluorescein angiography and/or OCT. The types of ischaemic or nonischaemic BRVO were recorded by ophthalmologists based on the extent of venous occlusions on fluorescein angiography using a Heidelberg Retina Angiography 2 HRA-II device (Heidelberg Engineering, Heidelberg, Germany). Macular cube OCT data were obtained using a Cirrus™ HD-OCT device (Carl Zeiss Meditec, Dublin, CA, USA) using the macular cube 512 × 128 scan protocol. The MRT was automatically calculated as the mean thickness of the central circle with a diameter of 1 mm.
Study treatments
The Branch Vein Occlusion Study found that grid laser photocoagulation was effective for the treatment of ME, and patients in this study were routinely treated as previously described. 19 IVTA was performed as previously described. 8 In brief, 0.1 ml of preservative-free TA suspension containing 4 mg TA (Laboratorio Italiano Biochimico Farmaceutico Lisapharma, Erba, Italy) was injected into the vitreous cavity through the pars plana, 4 mm posterior to the limbus, using a 0.5 inch 30 gauge needle on a 1 ml tuberculin syringe. Topical antiglaucoma medications were administrated if intraocular pressure (IOP) was ≥21 mmHg after IVTA.
The following prognostic variables were studied: age, sex, history of cigarette smoking, initial onset ME/chronic recurrent ME, duration of ME, concomitant systemic diseases (hypertension, type 2 diabetes mellitus, hyperlipidaemia, coronary artery disease, and autoimmune disease), and the morphological characteristics of ME at baseline.
Statistical analyses
All statistical analyses were performed using the SPSS® statistical package, version 22.0 (SPSS Inc., Chicago, IL, USA) for Windows®. Data were presented as the mean ± SD, n (%) of patients or n (%) of eyes. A power analysis to determine the sample size for this study was conducted using pooled data from all cases that experienced standard treatment of ME caused by BRVO at the Ningxia Eye Hospital between 2009 and 2013. χ2-test and Student’s t-test were used to compare ME resolution in the IVTA group and laser-only group. Analysis of variance and binary logistic regression analysis were used to evaluate factors correlated with the successful resolution of ME. Different factors associated with response to IVTA in the subgroups were analysed using χ2-test. A P-value < 0.05 was considered to be statistically significant.
Results
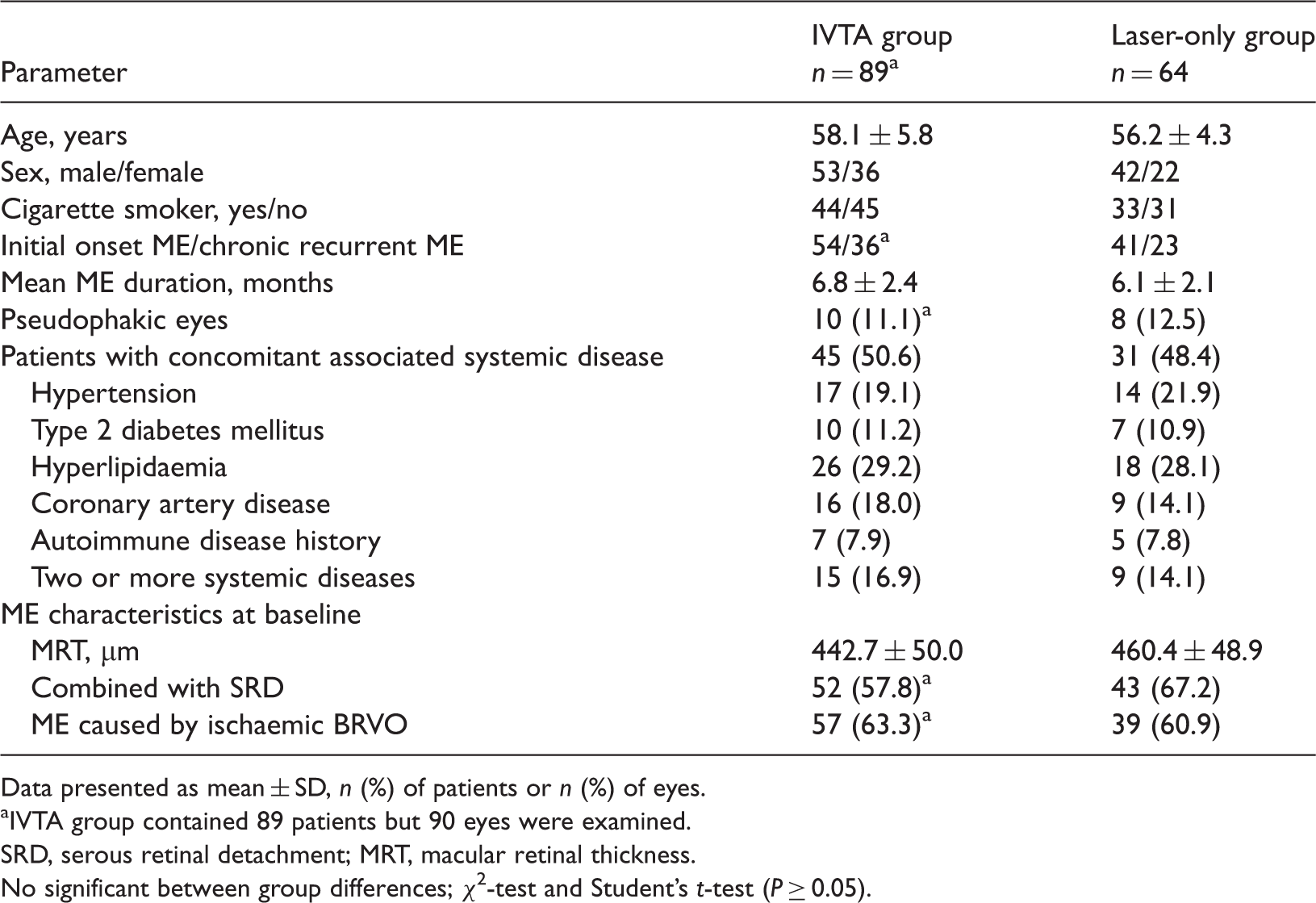
This retrospective study examined data from 154 eyes (153 consecutive patients) with ME due to BRVO, which were divided into the IVTA group (90 eyes; 89 patients; 53 male, 36 female) and laser-only group (64 eyes; 64 patients; 42 male, 22 female). Baseline demographic and clinical characteristics of the two groups are presented in Table 1. There were no significant differences between the two groups at baseline. In the IVTA group, 85 eyes received grid laser photocoagulation before IVTA for the treatment of BRVO-induced ME; four patients (five eyes) who were unable to have grid laser photocoagulation because of haemorrhage underwent grid laser photocoagulation after IVTA. No immediate procedure-related complications were observed during all IVTA injections. None of the patients in the IVTA group had history of glaucoma and 10 of 89 (11.2%) patients underwent cataract extraction with intraocular lens implantation prior to developing BRVO. ME was divided into different types according to the main location of the oedema; representative OCT images are shown in Figure 1.
Representative retinal optical coherence tomography images. (a) Patient with macular oedema and serous macular detachment (white arrow) due to branch retinal vein occlusion, with a cystoid space mainly located in outer plexiform layer (red arrow). (b) Complete regression of both macular oedema and serous macular detachment after one dose of intravitreal triamcinolone acetonide in the patient shown in A. (c) Patient with macular oedema, with a cystoid space mainly located in inner nuclear layer (red arrow). The colour version of this figure is available at: http://imr.sagepub.com Baseline demographic and clinical characteristics of patients with macula oedema (ME) due to branch retinal vein occlusion (BRVO), who received either routine grid laser photocoagulation treatment and one single intravitreal triamcinolone acetonide injection (IVTA group) or routine grid laser photocoagulation treatment only (laser-only group). Data presented as mean ± SD, n (%) of patients or n (%) of eyes. IVTA group contained 89 patients but 90 eyes were examined. SRD, serous retinal detachment; MRT, macular retinal thickness. No significant between group differences; χ2-test and Student’s t-test (P ≥ 0.05).
Comparison of outcomes over a 6-month monitoring period in patients with macula oedema (ME) due to branch retinal vein occlusion (BRVO), who received either routine grid laser photocoagulation treatment and one single intravitreal triamcinolone acetonide injection (IVTA group) or routine grid laser photocoagulation treatment only (laser-only group)

Data presented as mean ± SD or n (%) of eyes.
IVTA group contained 89 patients but 90 eyes were examined.
IVTA group versus laser-only group, χ2-test; cIVTA group versus laser-only group, Student’s t-test.
SRD, serous retinal detachment; MRT, macular retinal thickness; NS, no significant difference P ≥ 0.05.
In the IVTA group at month 6 of follow-up, visual acuity improved in 52 of 90 eyes (57.8%) and two of these eyes developed cataracts; in 28 eyes (31.1%), visual acuity remained the same (of these, three eyes developed cataracts); and visual acuity worsened in 10 eyes (11.1%; of these, four eyes developed cataracts). IOP was transiently elevated >21 mmHg in 11 of 90 eyes (12.2%), which received antiglaucoma medication during post injection follow-up. The IOP in 10 out of 11 eyes was controlled using topical medications, while one patient underwent a trabeculectomy.
Analysis of the association between baseline parameters and retinal response after one single intravitreal triamcinolone acetonide injection in patients (n = 89) with macula oedema (ME) due to branch retinal vein occlusion (BRVO)

Data presented as mean ± SD, n (%) of patients or n (%) of eyes.
Relapsing group contained 42 patients but 43 eyes were examined.
Binary logistic regression analysis.
Analysis of variance.
MRT, macular retinal thickness; SRD, serous retinal detachment; NS, no significant difference (P ( 0.05).
Comparison the morphology of macula oedema (ME) between the resolution and relapsing groups of patients (n = 90 eyes) with ME due to branch retinal vein occlusion (BRVO) who received one single intravitreal triamcinolone acetonide injection

Data presented as n (%) of eyes.
Relapsing group contained 42 patients but 43 eyes were examined.
Resolution group versus relapsing group; χ2-test.
Discussion
Recurrent or persistent ME is a difficult clinical problem that is often encountered during the treatment of BRVO.3,20–22 To date, there have been no reports about how to predict the ME recurrence rate after IVTA based on morphological patterns in BRVO. Studies have demonstrated that intravitreal corticosteroid injection is effective in reversing cystoid ME and improving visual acuity.20,21 A study that compared dexamethasone intravitreal implant, 0.7 mg (Ozurdex®, Allergan, Irvine, CA, USA) and TA for refractory cystoid ME due to retinal vein occlusion concluded that there was no difference between the two drugs regarding anatomical or functional outcomes or the incidence of side-effects, although the number of intravitreal injections were reduced by using Ozurdex®. 22 The current study retrospectively analysed baseline parameters in patients with BRVO-induced ME that might predict the successful resolution of ME following a single dose of IVTA.
As previous studies demonstrated that the effects of a single intravitreal injection could last for approximately 3–6 months in a nonvitrectomized, phakic patient, and was very effective in reversing cystoid ME and improving visual acuity in recent-onset nonischaemic retinal vein occlusion,21,23 the present study monitored the recurrence rate at 6 months after a single IVTA injection. The results of the present study demonstrated that IVTA significantly reduced the MRT from baseline to 6 months, and produced a significantly greater reduction, compared with standard care with grid laser photocoagulation. The rate of recovery of ME after IVTA in patients with SRD was also significantly higher compared with patients treated with standard care at both months 3 and 6. These current findings support the theory that a single IVTA injection can remain effective against ME for 3–6 months. An evidence-based systematic review of the natural history of 1608 cases of BRVO showed that 18–41% of ME at baseline resolved in 24 months. 24 However, that review did not analyse baseline demographic or clinical factors that might be predictive of treatment success. 24 The present study found that one single IVTA injection was more likely to be successful at resolving ME in younger patients, those with initial onset ME, those with a shorter duration of ME, those with concomitant SRD, those with fewer associated systemic diseases and in those with nonischaemic BRVO with an intact foveal capillary ring. IVTA is associated with some side-effects, such as elevated IOP, cataract development and sterile pseudoendophthalmitis of uncertain aetiology; and repeated IVTA injections could accelerate cataract progression. 21 However, medical personnel need to weigh up the risks of using IVTA injections compared with multiple injections of anti-VEGF agents, which may be costly and have short-term efficacy. 5 Research has demonstrated that one intravitreal bevacizumb injection might have little effect on improving retinal microcirculation in patients with ME secondary to acute BRVO at least 3 months after the injection. 25 Hence, under certain circumstances, an IVTA injection remains a useful method for the treatment of ME, in particular for patients who desire to resolve their ME with one injection. In a prospective randomized study, reduction in the macular thickness did not correlate completely with an increase in visual acuity, since numerous other factors (including nonperfusion and presence of haemorrhage) also affect vision. 26 As a consequence, this present study did not undertake a correlation analysis of visual outcome and macular thickness. If retinal cells have been lost due to capillary nonperfusion, or if intraretinal intercellular structures have been disrupted due to chronic ME and swelling, resolution of the oedema may only have a limited effect in raising visual function. 1 A better visual acuity outcome may be at least in part associated with less severe anatomical changes. 15 The SCORE study demonstrated no difference in visual acuity at 12 months between the IVTA group and the standard care group, even though some patients in the IVTA group had complications (such as cataracts and elevated IOP), which indirectly indicates that IVTA may be reducing ME to some extent. 3
Although there has been a report of two cases in which one IVTA injection successfully resolved ME due to central retinal vein occlusion, 27 to our knowledge, no study has been undertaken to systematically analyse a cohort of patients to determine the outcome of one IVTA injection for the treatment of BRVO. There has also been no report about the correlation between different retinal morphological characteristics and the success rate of one IVTA injection in patients with BRVO-induced ME.
In the present study, the relationship between SRD and the outcome of one IVTA injection was analysed because SRD can occur as a complication of venous occlusive disease. 28 The pathogenesis of SRD remains to be elucidated. Evidence suggests that obstruction of the retinal venous outflow leads to a consequent increase in intravascular pressure, especially in the capillaries and postcapillary venules. 29 The capillary nonperfusion and tissue ischaemia caused by venous occlusion then leads to the production of chemical intermediates that increase vascular permeability. 30 Therefore, both increased intravascular pressure and vascular permeability play key roles in SRD development. 30 Meanwhile, the barrier function of the external limiting membrane is lost due to traction on the Müller cell cone in the formation of SRD. 28 As a result of the disruption of the inner blood–retinal barrier and the external limiting membrane becoming permeable to fluid and albumin, the retinal pigment epithelium cannot remove excess fluid and the barrier function is lost, which leads to fluid reaching the subretinal space in large amounts, with the resultant subfoveal detachment. 31 Some authors have suggested that the visual prognosis is poor for BRVO patients with SRD.28,32,33 However, the results from IVTA injection suggest that it is effective for the resolution of SRD due to release of the traction of the Müller cell cone. 30 IVTA injection has been shown to alleviate the breakdown of the inner blood–retina barrier through inhibition of cell-mediated inflammation, leukocyte adhesion and extravasation, and downregulation of the secretion of VEGF in rats. 34 The present study demonstrated that ME combined with SRD was a predictor of a good prognosis for ME resolution, which was consistent with previous reports that most SRD occurred in recent onset BRVO.25,32,35
A prospective observation of uveitis-associated cystoid ME concluded that the initial morphological appearance was linked with clinical prognosis. 11 Increased retinal blood flow in the occluded venules before injection might be associated with a reduction of ME after intravitreal bevacizumab. 25 As the ischaemic type of BRVO is generally correlated with a poor prognosis, 36 the morphological pattern was further analysed in this type; although it should be noted that some patients with ischaemic BRVO in the present study did have a good response to IVTA treatment. The present analysis of the resolution and relapsing subgroups (Table 4) demonstrated that a broken foveal capillary ring correlated with a poor prognosis, which may partially support the theory that the disruption of retinal blood flow may play an important role in recurrent ME.
As previous studies reported that the frequency of ME in the outer plexiform layer and inner nuclear layer was significantly higher than in all other layers following retinal vein occlusion,18,36 these two locations were further analysed in the present study. The results showed that cystoid spaces located in the outer plexiform layer correlated with a good prognosis, which was in agreement with a previous study that reported that cystoid spaces were located mainly in the inner nuclear layer in longstanding BRVO compared with those located in the outer plexiform layer in recent onset BRVO. 36 Moreover, this present study also demonstrated that venous obstruction in the inferotemporal quadrant correlated with a good prognosis following IVTA injection compared with superotemporal quadrant obstruction.
This current study had a number of limitations. First, it was a retrospective study. Secondly, it only included a limited number of patients. Thirdly, the follow-up period was limited to 6 months. Larger, prospective comparative studies with longer term follow-up are necessary to clarify the factors correlated with the likelihood of success of treatment for BRVO-induced ME.
In conclusion, these findings suggest that a single IVTA injection could be used to treat ME caused by BRVO if the patient has the following predictive factors for a successful outcome: younger age, shorter duration of ME, initial onset ME, accompanied by SRD, few concomitant systemic diseases and nonischaemic BRVO. If repeat injections are required, alternative medications such as a sustained release steroid implant or an anti-VEGF agent might be a better choice.
Footnotes
Acknowledgements
The authors would like to thank Xunlun Sheng for valuable discussion of this research.
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This study was supported by a grant from the Shandong Nature Sciences Foundation (no. ZR2015HM026).
