Abstract
Objective
To determine the duration and obstacles to prolonged on-scene cardiopulmonary resuscitation (CPR), and establish how long a pair of emergency medical technicians (EMTs) can provide high-quality CPR.
Method
Intermediate-level EMTs in Gyeonggi-do Province, Republic of Korea completed a survey regarding on-scene CPR. EMTs undergoing routine training took part in a simulation using mannequins. Parameters including compression depth, total number and rate of compressions; occurrence of incorrect hand position and incomplete chest recoil were collected over 16 2-min cycles of CPR (32 min total), with EMTs working in pairs.
Result
The simulation study included 43 EMTs. The median duration of on-scene CPR was 3.7 min. Fear of decrease in performance was the main obstacle to continued CPR (n = 188/254 [74.0%]). Standards for high-quality CPR were met at each of the 16 steps of the simulation. Compression rate increased significantly with time. There were no significant changes in any other parameter.
Conclusion
Pairs of EMTs maintained high-quality CPR for 16 cycles (32 min) with no decrease in performance. Our findings could provide evidence to recommend guidelines for duration of on-scene CPR for cardiac arrest, particularly in countries where the level and number of ambulance crews are limited.
Introduction
The continuous performance of high-quality cardiopulmonary resuscitation (CPR) is essential to improve the survival of cardiac arrest patients. The quality of CPR is determined by six factors: compression depth, compression rate, accurate location, full chest recoil, minimization of interruptions, and adequate ventilation (Figure 1).1–4 Bystanders and emergency medical technicians (EMTs) may perform CPR on patients with out-of-hospital cardiac arrest. In the case of bystanders, the action of performing CPR has been emphasized over its quality.5–8 EMTs, however, are expected to perform high-quality CPR for a sufficient length of time, with the aim of achieving the return of spontaneous circulation (ROSC). Studies have indicated that CPR quality may decrease over time.9–13
Components of high-quality cardiopulmonary resuscitation.
The out-of-hospital cardiac arrest survival rate in the Republic of Korea is 3.3% for patients with cardiac aetiology. 14 In addition, the rate of prehospital ROSC following EMT treatment is only ∼1%, 14 possibly due to the short duration of CPR provided by EMTs at the scene (mean duration, 7 min). 15 This is not sufficient to achieve prehospital ROSC, which is a major survival factor in out-of-hospital cardiac arrest. 16
The aim of the present study was twofold. First, we carried out a survey of EMTs to determine the duration of and obstacles to prolonged on-scene CPR. Secondly, we performed a simulation study to establish for how long a pair of EMTs can provide high-quality CPR.
Patients and methods
Survey
An e-mail questionnaire comprising 27 items regarding EMT demographics, CPR duration at the scene and obstacles to CPR continuation was conducted with intermediate-level EMTs in Gyeonggi-do Province, Republic of Korea. Gyeonggi-do Province is ∼10 167 km2 and has a population of just over 11 million people. There are 962 intermediate-level EMTs and 221 ambulances, which transport a mean of 14.2 patients with out-of-hospital cardiac arrest per day (mean total, 834 patients per day).
The emergency medical service in the Republic of Korea is similar to an intermediate-level emergency transport service in the USA, in that each ambulance is staffed by two or three EMTs. All EMTs can provide basic life support with an automated external defibrillator (AED) and a trauma resuscitation kit.
Simulation study
Study design
The study included EMTs with 1 or 2 years’ experience who volunteered while attending a training course for high-quality CPR at the Gyeonggi-do Province Emergency Medical Education Academy, Suwon, Republic of Korea. The general purpose of the study was explained to the subjects while blinding the specific study process, data for collection and study results. No ethical approval was required because the study was performed during routine formal EMT education.
Laerdal Resusci Anne Skill Station (Laerdal Medical, Orpington, Kent, UK) mannequins were prepared and connected to the Laerdal Skill reporting system (Laerdal Medical) with both storage and printout functions. Compression depth and accuracy were shown visually. CPR was performed by teams of two EMTs who were briefed on a megaventricular fibrillation scenario in which a 62-year-old man with diabetes and hypertension (living in an 18th floor apartment) called EMTs because of chest pain, who then arrived at the scene to find the man unconscious. The scenario was prepared in advance and comprised 16 steps. Step 1 involved patient recognition (checking response, respiration and pulse), chest compressions during AED charging, and initial external defibrillation (followed immediately by chest compressions for 2 min by one EMT and laryngeal mask airway insertion by the other). Steps 2–16 each involved external defibrillation, followed by 2 min uninterrupted chest compressions by one EMT and positive-pressure ventilation with a back-valve mask by the other. The two EMTs reversed roles at the end of each step, so that each performed eight 2-min cycles of CPR for a total of 32 min (Figure 2).
Diagram indicating the design of a study to determine for how long a pair of emergency medical technicians can provide high-quality cardiopulmonary resuscitation.
Investigators acted as family members to simulate a genuine out-of-hospital cardiac arrest scenario, crying out and gesturing, in order to stress the EMTs, who gave prepared replies to these ‘family members’.
Data collection
Data regarding work experience, age, height and weight of the EMTs were collected. Compression depth, total number and rate of compressions, and occurrence of incorrect hand position and incomplete chest recoil were collected using the Laerdal Skill reporting system. After the simulation, subjects completed a survey regarding the point at which they felt fatigued and that CPR quality was affected, and perceived obstacles to continuation of CPR (both in the field and in the simulation setting).
Statistical analyses
Data were expressed as mean ± SD, median (interquartile range) or median (range). Between-sex differences in CPR performance were analysed using Student’s t-test or χ2-test, as appropriate. The general estimating equation model was used to adjust CPR data for age, sex, EMT level (basic or intermediate), and body mass index (BMI), and between-timepoint analyses of CPR data were made using a multivariate linear regression model. CPR data from the 16 cycles were grouped into four stages (four cycles per stage) and temporal changes in CPR quality were analysed using multivariate regression. All statistical analyses were performed using SPSS® version 15.0 (SPSS Inc., Chicago, IL, USA) for Windows®. P-values < 0.05 were considered statistically significant.
Results
Survey
The survey was completed by 254 EMTs. The median duration of on-scene CPR was 3.7 min (range 0–20 min), with a median of two cycles (range 0–10 cycles). The maximum duration of on-scene CPR was 5 min (range 0–35 min). Obstacles to the continuation of CPR included: fear of decrease in CPR performance (n = 188 [74.0%]); complaints of family members (n = 159 [62.8%]); musculoskeletal pain (n = 112 [44.1%]); pressure from team members to “load and go” (n = 102 [40.1%]); and lack of confidence (n = 45 [17.7%]).
Simulation study
Demographic characteristics of emergency medical technicians (23 pairs) included in a study to determine for how long they could provide high-quality cardiopulmonary resuscitation.

Data presented as median (interquartile range).
BMI, body mass index.
P < 0.001 vs male EMTs; Student’s t-test.
Data regarding CPR parameters at each step are shown in Figure 3. The standards of high-quality CPR (as shown in Figure 1) were met at each of the 16 steps. Compression rate significantly increased with time (P = 0.001), but there were no significant changes in any other parameter. There were no changes in any parameter over time when data were grouped into four stages of four steps each (Table 2).
Cardiopulmonary resuscitation (CPR) parameters over time, as performed by 23 pairs of EMTs for 16 cycles of 2 min (32 min total). Cardiopulmonary resuscitation (CPR) parameters as performed by 23 pairs of EMTs for 16 cycles of 2 min (32 min total), stratified into four stages of 4 cycles (8 min) each. Data presented as mean (95% confidence intervals). No statistically significant between stage differences (P ≥ 0.05; multivariate linear regression analysis).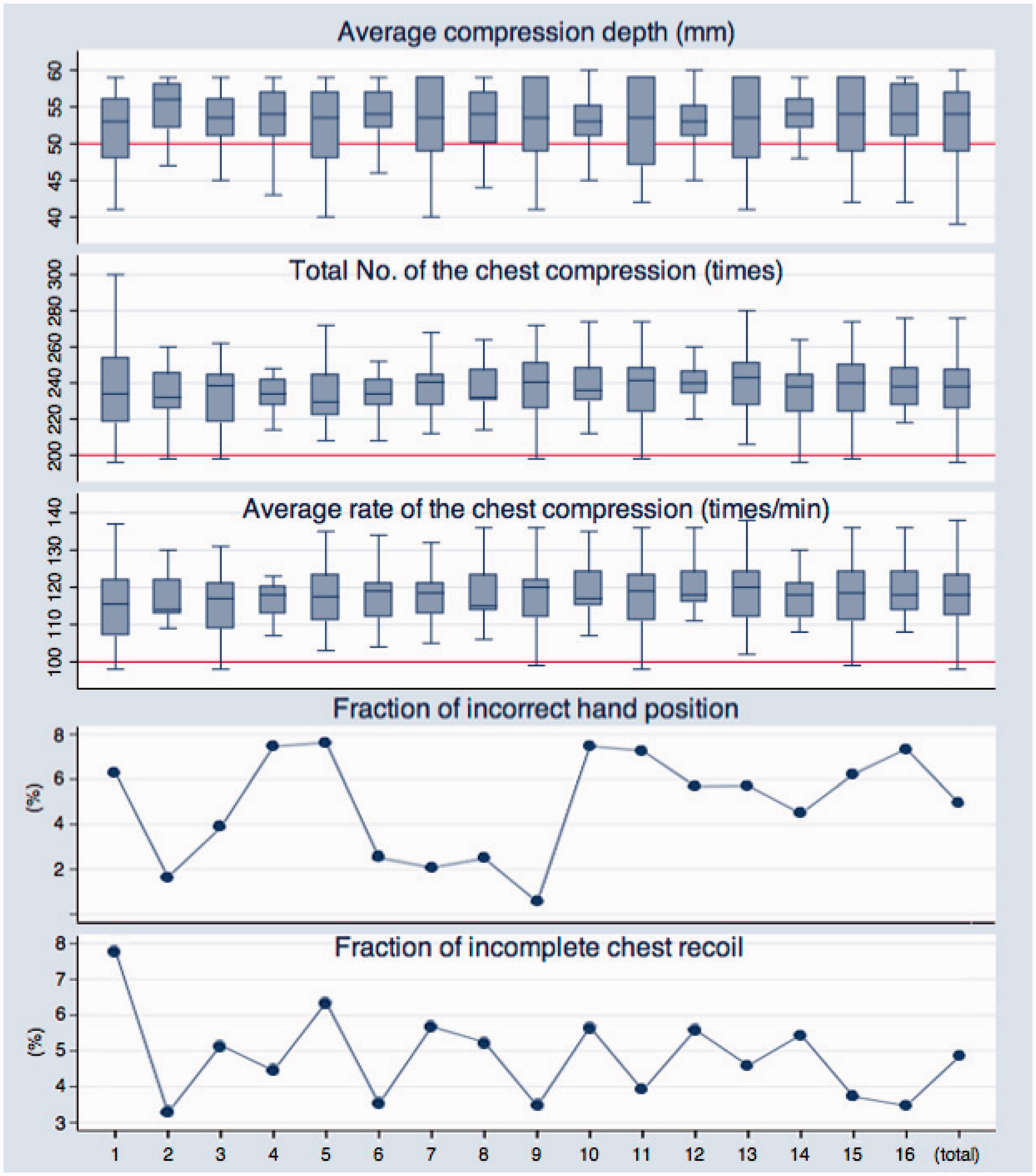
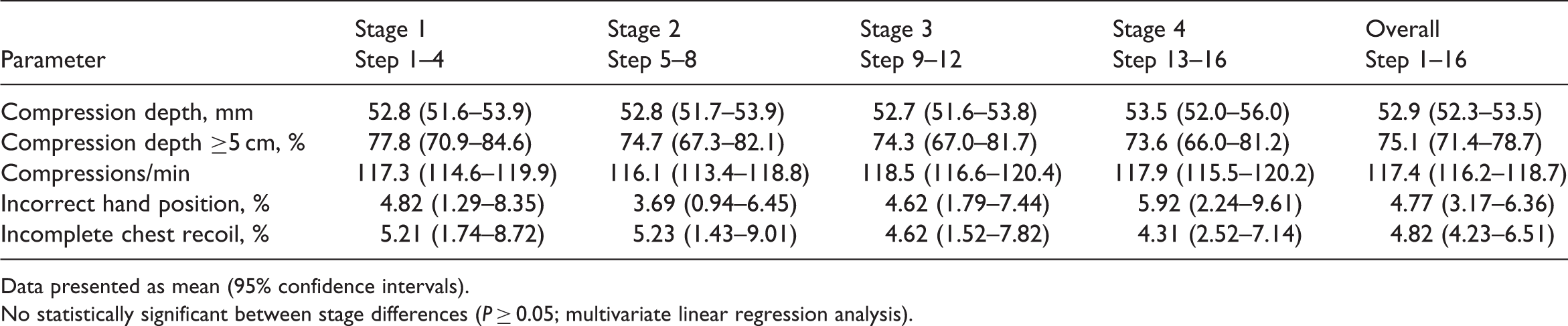
Cardiopulmonary resuscitation (CPR) parameters as performed by 23 pairs of EMTs for 16 cycles of 2 min (32 min total).

Data presented as mean ± SD.
Student’s t-test.
χ2-test.
General estimating equation model coefficients of factors affecting cardiopulmonary resuscitation (CPR) parameters, adjusted for age, sex, BMI and emergency medical technician (EMT) level, as performed by 23 pairs of EMTs for 16 cycles of 2 min (32 min total).
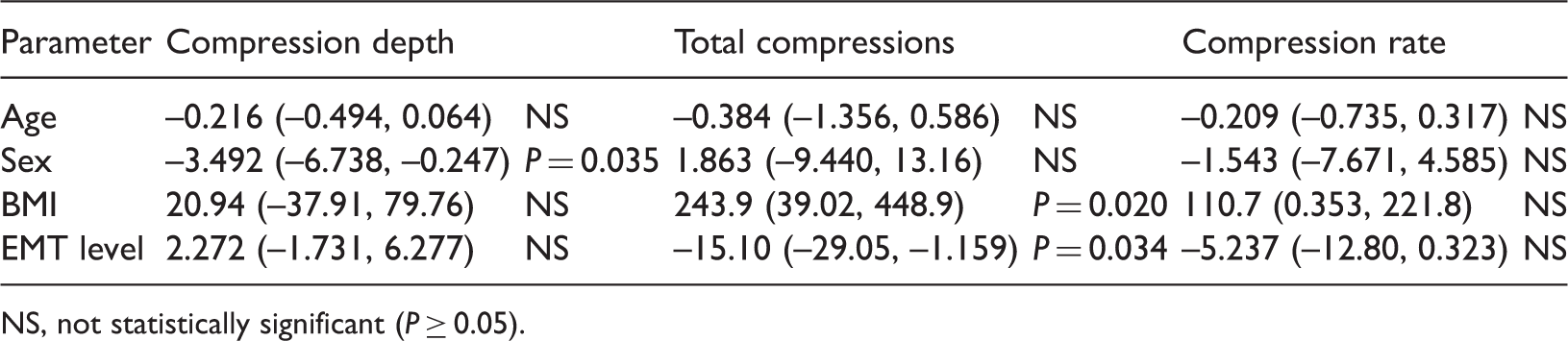
NS, not statistically significant (P ≥ 0.05).
The post-study survey found that the median expected onset of fatigue was 4.0 min (range 0–47 min) and the expected onset of reduced performance was 2.5 min (range 1–9 cycles). The reported obstacles to continuation of CPR were fear of decrease in CPR performance (n = 26 [60.5%]), complaints of family members (n = 25 [58.1%]), musculoskeletal pain (n = 19 [44.2%]), pressure from team members to load and go (n = 4 [9.3%]), and lack of confidence (n = 3 [7.0%]).
Discussion
The out-of-hospital emergency medical system varies between countries and even among regions within the same country. 17 Out-of-hospital management of cardiac arrest patients may also vary, depending on the country and region, 18 and there is no universal standard for the duration of on-scene CPR for patients in cardiac arrest. In many parts of the USA, paramedics perform CPR at the scene until the patient achieves spontaneous ROSC; 19 if ROSC is not achieved, health care providers terminate resuscitation and declare death at the scene. 20 In many European countries, doctors travel on board ambulances and treat cardiac arrest patients for the required time based on their judgement. 21
In the Republic of Korea and other Asian countries (including Malaysia, Japan, Singapore, and Taiwan), doctors do not travel on board ambulances and EMTs are not legally qualified to declare the death of a patient. EMTs may only provide basic life support, and use AEDs for rhythm analysis and defibrillation in patients with cardiac arrest. Unlike in the USA and Europe, the protocol in Asia allows for the provision of CPR at the scene for a relatively short period of time, followed by transport to hospital with ongoing CPR. 17 The mean duration of on-scene CPR in the Republic of Korea is 7.6 min, 15 which is shorter than in the US, Europe, and other Asian countries.17,22–24 Our survey revealed a median CPR duration of 3.7 min.
A shorter duration of on-scene CPR significantly affects survival, as well as the likelihood of good cerebral recovery. 16 It is difficult to provide high-quality CPR during transfer to hospital, due to frequent interruption in the ambulance.25–28 Patients with ventricular fibrillation cardiac arrest are likely to be in the circulatory phase when the EMTs arrive, emphasizing the importance of on-scene CPR to ensure return to the electrical phase. On-scene CPR is performed for 20 min in the US,29–30 whereas the 7.6-min mean duration of CPR in the Republic of Korea 15 is too short to achieve ROSC prior to transport.
Concern regarding decreased CPR performance was one of the main obstacles to the continuation of on-scene CPR in the present study. Unlike concerns regarding legal issues, adequate training and education can correct this misconception. This simulation study found no such decrease in CPR quality over time could help to dispel this myth. CPR performance parameters (compression depth, compression rate, hand position and chest recoil) satisfied the standards for high-quality CPR for 32 min in the present study. Our findings clearly show that pairs of EMTs working together are fully capable of providing high-quality CPR for 32 minutes. Further studies with a longer time period, involving EMTs of varied physical fitness levels, are required to determine the maximum duration of CPR that can be provided.
Our findings could provide evidence to recommend guidelines for duration of on-scene CPR for patients with cardiac arrest, particularly in Asian countries where the level and number of ambulance crews are limited. These data may also assist EMTs in the USA and Europe, to determine whether to call for backup.
This study had several limitations. First, this was a simulation study conducted on the floor using mannequins. Although stress and distraction from a patient’s family members were simulated by the actions of investigators, it was not possible to replicate all conditions and scenarios. Secondly, because all subjects participated in the simulation study simultaneously and were able to watch each other’s performance they had opportunities to correct their own performance and experimental bias cannot be ruled out. Thirdly, the fixed duration of the simulation study (32 min) meant that it was impossible to determine the point at which performance would deteriorate. However, 30 min of on-scene CPR is generally considered the maximum,29–31 and we believe that our findings can effectively be applied to real-world situations. Finally, this study used teams of two EMTs, which does not necessarily reflect reality. In some countries, ambulances are staffed with three EMTs, and some regions dispatch more than one team to critical patients. In these situations, the potential maximal CPR time at the scene may lengthen.
In conclusion, in a simulation situation, pairs of EMTs maintained high-quality CPR for 16 cycles (32 min) without any decrease in performance.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This study was supported by the 2013 Indang research grant of Inje University.
