Abstract
Objective
To evaluate results of the ‘pSORRIDI’ experience (which is a prevention campaign to evaluate the prevalence of comorbidities, multidisciplinary needs and appropriateness of the therapeutic approach for comorbidities) in patients already being treated for psoriasis.
Methods
Telephone interviews were conducted in patients with psoriasis, who then underwent comprehensive evaluation and investigation of comorbidities. If necessary, patients were referred to specialist cardiology, endocrinology and/or rheumatology services.
Results
Overall, 72.0% (54/75) of patients required a multidisciplinary consultation. Among patients referred to cardiology, therapeutic adjustment was needed in 33.3% (five of 15) patients and a redefined diagnosis in 26.7% (four of 15) cases. Among patients undergoing endocrinology evaluations, therapeutic adjustment and a redefined diagnosis were needed in 61.1% (11/18) and 33.3% (six of 18) patients, respectively; for rheumatology evaluations, therapeutic adjustment and a redefined diagnosis were needed in 76.2% (16/21) and 19.0% (four of 21) of patients, respectively.
Conclusions
Among patients with psoriasis, there may be a need for an improvement in the diagnosis of underlying comorbid conditions, and in disease management of both psoriasis and any comorbid conditions.
Introduction
Psoriasis is a chronic inflammatory condition affecting up to3% of the population worldwide. 1 Multiple studies have shown an association between psoriasis and several comorbid conditions such as cardiovascular disease, obesity, diabetes mellitus, hypertension, dyslipidaemia, metabolic syndrome, nonalcoholic fatty liver disease, anxiety, depression and inflammatory bowel disease. Such findings suggest that a multidisciplinary approach to psoriasis management might be required and that these comorbidities might also affect psoriasis treatment choice and monitoring.2–5 Early detection and treatment of comorbid conditions is important for the management of patients with psoriasis, to improve treatment adherence and therapeutic success.5,6
The aim of this present study was to evaluate the results of the ‘pSORRIDI’ experience, a prevention campaign that took place at the Department of Dermatology of the University of Rome Tor Vergata, Rome, Italy, which was designed to evaluate the prevalence of comorbidities, multidisciplinary needs and appropriateness of therapeutic approaches for comorbidities in patients already being treated for psoriasis.
Patients and methods
Patients
In October 2013, patients affected by psoriasis referred to the outpatient department at the University of Rome Tor Vergata underwent a telephone interview for an open multidisciplinary assessment related to psoriasis (an event funded by Pfizer Italia). Patients previously treated for psoriasis but lost to follow-up for >6 months were selected.
Evaluations and definitions
Participants underwent an initial dermatological evaluation with a questionnaire to record onset, duration and treatment of psoriasis with topical or systemic medication. Comorbidities and related treatments were also investigated using routine methods. Psoriasis severity was evaluated using the Psoriasis Area Severity Index (PASI) score 7 for skin manifestations and a visual analogue scale score (pain VAS), ranging between 0 and 100 for pain; there was no separate physiological assessment for joint involvement. Patients also received an interview with a psychologist (MP) and completed a health-related quality-of-life questionnaire using the Dermatology Life Quality Index. 8 Depending on the personal medical condition, patients were referred for one or more specialist consultations, which were performed by a cardiologist (MM), endocrinologist (SR) or rheumatologist (MSC) related to the Department of Internal Medicine of the University of Rome Tor Vergata.
The relevance of a specialist consultation was defined as an adjustment of the ongoing therapy for psoriasis or comorbid conditions, and/or the need for review or implementation of the diagnosis of the comorbid condition (i.e. diagnostic redefinition).
As routine clinical practice, written informed consent was obtained from all patients, allowing the use of clinical records for scientific investigation. The study, which was conducted in accordance with the ethical principles of the Declaration of Helsinki, did not require ethical committee approval.
Quantitative variables were expressed as mean ± SD. Categorical variables were presented as
Results
Demographic and clinical characteristics of patients with psoriasis (

Data presented as mean ± SD or
PASI, Psoriasis Area Severity Index; 7 VAS, visual analogue scale; DLQI, dermatology life quality index; 8 BMI, body mass index; IBD, inflammatory bowel disease; BPH, benign prostatic hypertrophy; HCV, hepatitis C virus.
All patients had failed to present for a routine dermatological visit during the previous 6 months and, in a large proportion of cases (44.0%; 33/75), declared themselves unsatisfied or moderately satisfied with their current treatment. Medical comorbidities were present in the study population. Hypertension, type 2 diabetes mellitus, dyslipidaemia and overweight or obesity (defined as a body mass index >25 kg/m2) were identified in 30.7% (23/75), 14.7% (11/75), 16.0% (12/75) and 16.0% (12/75) of patients, respectively; other noteworthy medical conditions are reported in Table 1.
A need for a multidisciplinary consultation was found in a large number of patients (54/75; 72.0%) and the relevance of the specialist visits (cardiology, endocrinology/metabolic or rheumatology) was a frequent finding. Among patients referred for a cardiology visit, the relevance was identified in 60.0% (nine of 15 patients); therapeutic adjustment was required in 33.3% (five of 15 patients) followed by a diagnostic redefinition in 26.7% (four of 15 patients) (Figure 1). Of interest, among patients undergoing an endocrinology/metabolic evaluation, relevance was identified in 94.4% (17/18 patients), with therapeutic adjustment and a redefined diagnosis needed in 61.1% (11/18) and 33.3% (six of 18) of patients, respectively. Furthermore, in the context of rheumatology visits, relevance was found in 95.2% (20/21 patients), and 76.2% (16/21) and 19.0% (four of 21) of patients required therapeutic adjustment and a redefined diagnosis, respectively.
Relevance and outcome of visits to disease specialists in patients with psoriasis (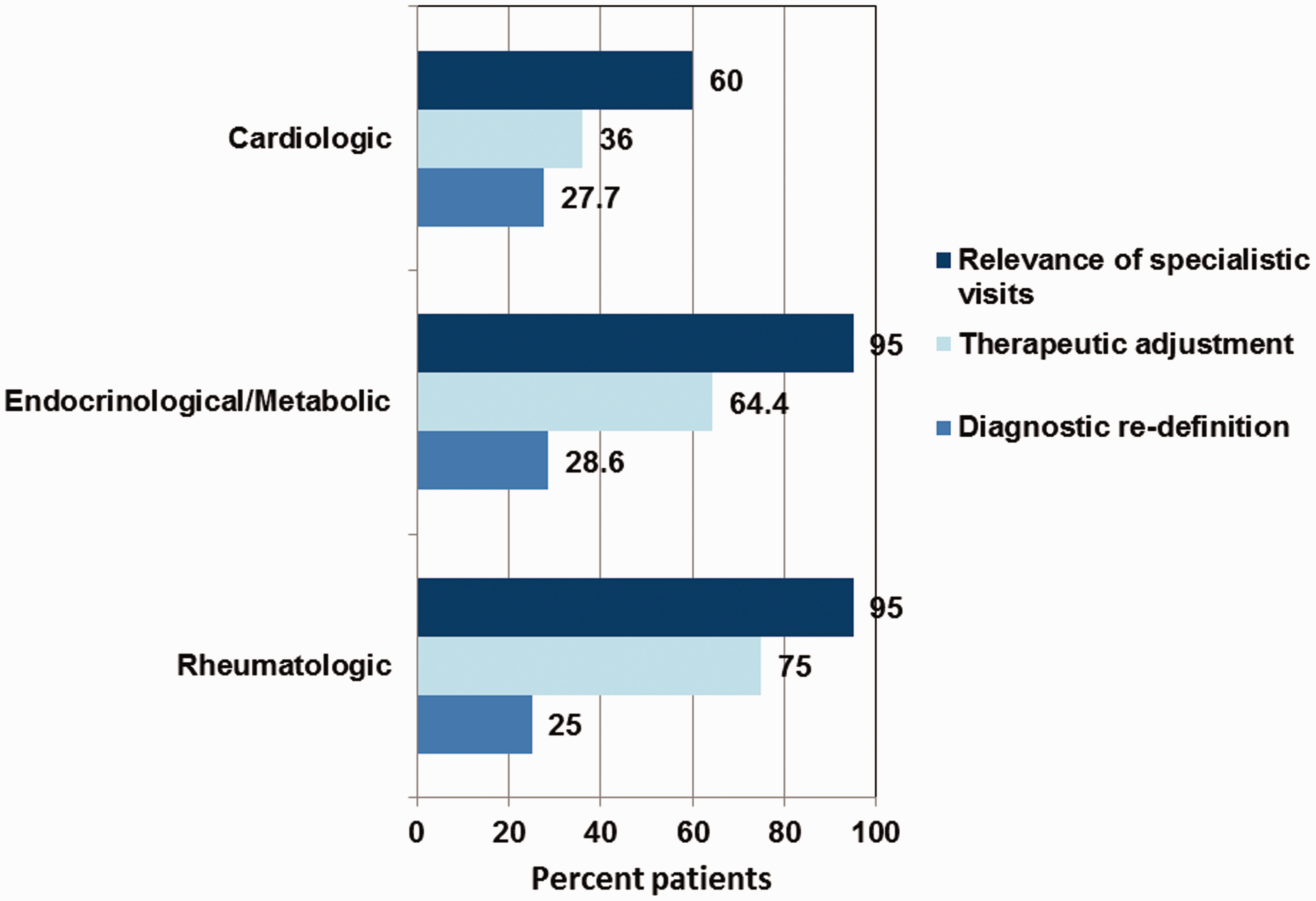
Discussion
Research over the past decade has demonstrated that a number of health risks and comorbid diseases, particularly inflammatory conditions, are associated with psoriasis; such conditions have the potential to increase morbidity and mortality, and adversely affect health-related quality-of-life.2–5 Accordingly, treatment adherence is a global parameter of therapeutic success, being influenced by drug efficacy and safety profiles; it is also dependent on external and subjective variables related to the patient’s underlying conditions and to the disease experience itself.6,9 As a consequence, a multidisciplinary approach to addressing the multiple problems of patients may improve treatment adherence and clinical observations.
Despite a good therapeutic effect, as expressed by a low mean PASI score, unmet needs were found in a large percentage of patients in the present study, in terms of diagnostic definition and treatment of comorbidities. The present study also showed a large background of unmet needs among patients with psoriasis and presenting with other underlying conditions; this was particularly true regarding those affected by endocrinological/metabolic disorders, or those with joint involvement, as demonstrated by the elevated rate of endocrinology and rheumatology consultations.
Several limitations may affect the validity of this study, being that it was a single-centre observation, involving a small sample size and with an absence of statistical analyses. Nevertheless this present study highlighted the importance of integrated multidisciplinary assessment and management for patients with psoriasis.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
Editorial assistance was provided by Gayle Robins on behalf of HPS–Health Publishing and Services Srl and funded by Pfizer Italia.
