Abstract
Objectives
A systematic review and meta-analysis to evaluate the effect of human chorionic gonadotropin (hCG) intrauterine injection before embryo transfer on the outcome of in vitro fertilization (IVF) and intracytoplasmic sperm injection (ICSI).
Methods
Searches of PubMed®, EMBASE®, EBSCO, Web of Science®, SCOPUS® and Cochrane Central Register of Controlled Trials were conducted to retrieve relevant randomized controlled trials (RCTs). Data were extracted and analysed.
Results
The meta-analysis included five RCTs (hCG group n = 680; control group n = 707). Intrauterine hCG injection significantly increased rates of biochemical, clinical and ongoing pregnancy compared with controls. There were no between-group differences in implantation or miscarriage rates.
Conclusion
Women undergoing IVF/ICSI may benefit from intrauterine hCG injection before embryo transfer.
Keywords
Introduction
Implantation is a complex biological interaction between embryo and endometrium that is critical to successful pregnancy. 1 Inappropriate implantation is the cause of two-thirds of in vitro fertilization (IVF) failures. 2 Implantation is regulated by many factors, the most important of which is the human chorionic gonadotrophin (hCG) concentration. 3 A positive correlation has been found between hCG concentration in embryo culture medium and implantation rate, suggesting that hCG secreted by embryos may be a useful biomarker for embryo selection in IVF. 4 Early embryonic hCG secretion is beneficial to implantation.5–8
Intrauterine injection of hCG (500 IU/ml) significantly inhibits insulin-like growth factor binding protein 1 and macrophage colony-stimulating factor, while leukaemia inhibitory factor, vascular endothelial growth factor and matrix metallopeptidase 9 are significantly stimulated. 9 These multiple effects appear to precede the classical endocrine role of hCG, and may be directly involved in the regulation of implantation.7,9
In animal models, systemic administration of hCG at the time of embryo transfer significantly increases pregnancy rate. 10 Intrauterine hCG injection is associated with significant proimplantation changes of the endometrium during the window of receptivity in normal cycling baboons, and induces a favourable uterine environment for embryo implantation. 11
Intrauterine injection with hCG (500 IU/ml) prior to embryo transfer significantly improves rates of implantation and pregnancy in IVF/ICSI (intracytoplasmic sperm injection). 12 Several other studies have been performed to assess the role of hCG intrauterine injection before embryo transfer in assisted reproduction.13–16
The aim of the present meta-analysis was to evaluate the effects of intrauterine hCG injection before embryo transfer on the outcome of IVF/ICSI.
Materials and methods
Literature search
Searches of PubMed®, EMBASE®, EBSCO, Web of Science®, SCOPUS® and Cochrane Central Register of Controlled Trials (CENTRAL) were performed from date of inception to December 2014 using the search strategy: (‘human chorionic gonadotropin’ or ‘hCG’ or ‘recombinant hCG’ or ‘rhCG’) AND (‘intrauterine’ or ‘intrauterine injection’ or ‘endometrial infusion’) AND (‘assisted reproductive techniques’ or ‘ART’ or ‘IVF’ or ‘ICSI’ or ‘in vitro fertilization’ or ‘intracytoplasmic sperm injections’ or ‘embryo transfer’). A combination of text words and specific database indexing terminology were used.
Inclusion and exclusion criteria
Studies were considered eligible if they met the following criteria: (i) randomized controlled trial (RCT); (ii) patients intended to undergo embryo transfer; (iii) comparison made between intrauterine hCG injection or no injection or placebo; (iv) data regarding pregnancy outcomes were reported. Exclusion criteria were: (i) experimental group containing other therapy; (ii) comparison made between different hCG doses; (iii) review articles; (iv) nonprospective comparative studies; (v) data unavailable for meta-analysis. Only original publications were included; conference abstracts and dissertations were not considered. No language restrictions were applied.
Data extraction
The initial electronic database searches to identify potentially relevant articles for inclusion were performed by two independent reviewers (H.Y. and J.H.). In cases of insufficient data, authors were contacted for information. Any disagreements were discussed and resolved by consensus or arbitration by a third independent reviewer (W-C.H.).
All retrieved titles and abstracts were examined; those with the possibility of meeting the inclusion criteria were kept for further evaluation. Final inclusion decisions were made on examination of full manuscripts. Reference lists of retrieved articles were screened in order to identify additional studies.
Primary outcomes were clinical pregnancy rate and implantation rate. Secondary outcomes included biochemical pregnancy rate, miscarriage rate and ongoing pregnancy rate.
Quality assessment
The quality of each study was assessed according to the modified Jadad scale. 17 The scale ranges between 0 and 7, and evaluates four aspects of RCTs: adequacy of randomization; concealment allocation; blinding; reporting of participant withdrawals and drop outs. A score of 0 represents the poorest methodological quality; a score of 7 represents the strongest methodological quality. Articles with 1–3 points in total were considered to be of low quality; those with 4–7 points in total were considered to be of high quality.
Statistical analyses
Data were combined for meta-analysis using RevMan® version 5.1 (Cochrane Collaboration, Oxford, UK). Dichotomous data were expressed as odds ratio (OR) with 95% confidence intervals (CIs). Statistical heterogeneity was assessed by I2 statistic, such that I2 ≥ 50% indicated substantial heterogeneity. 18 Study data were combined using a fixed-effects model when heterogeneity was negligible, or a random-effects model in the case of significant heterogeneity. P-values < 0.05 were considered statistically significant.
Results
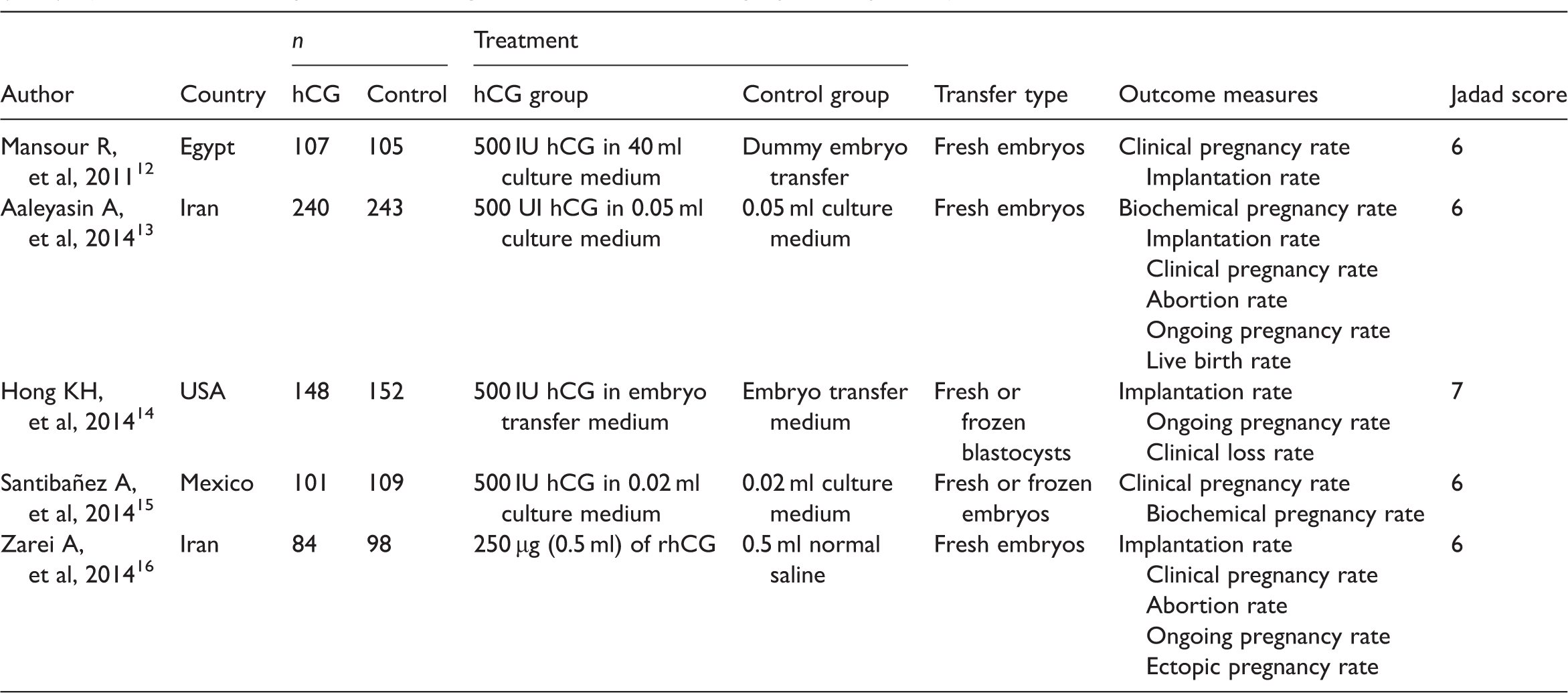
The process of literature identification and selection is summarized in Figure 1. After exclusion of ineligible articles, the final meta-analysis included five RCTs (hCG group n = 680; control group n = 707).12–16 Characteristics of the included trials are shown in Table 1.
Flow diagram indicating results of the literature search and study selection process for a meta-analysis conducted to evaluate the effect of intrauterine human chorionic gonadotrophin (hCG) injection before embryo transfer during in vitro fertilization/intracytoplasmic sperm injection. Principal characteristics of studies included in a meta-analysis conducted to evaluate the effect of intrauterine human chorionic gonadotrophin (hCG) injection before embryo transfer during in vitro fertilization/intracytoplasmic sperm injection.
Data regarding clinical pregnancy rates were reported by four studies (hCG group n = 532; control group n = 555).12,13,15,16 Pooled analysis found that clinical pregnancy rates were significantly higher in the hCG group compared with the control group. (OR 2.07; 95% CI 1.61, 2.66; I2 = 0%, Pheterogeneity = 1.0; Figure 2).
Forest plot of clinical pregnancy rate in patients undergoing in vitro fertilization/intracytoplasmic sperm injection, with or without intrauterine human chorionic gonadotrophin (hCG) injection before embryo transfer (n = 1087). M-H, Mantel–Haenszel; CI, confidence interval.
Implantation rates were reported by two trials (hCG group n = 388; control group n = 395),13,14 with no significant between-group difference found (OR 1.63; 95% CI 0.87, 3.08; I2 = 87%, Pheterogeneity = 0.006; Figure 3).
Forest plot of implantation rate in patients undergoing in vitro fertilization/intracytoplasmic sperm injection, with or without intrauterine human chorionic gonadotrophin (hCG) injection before embryo transfer (n = 783). M-H, Mantel–Haenszel; CI, confidence interval.
Biochemical pregnancy rates were reported by two trials (hCG group n = 341; control group n = 352).13,15 Meta-analysis found that biochemical pregnancy rates were significantly higher in the hCG group than the control group (OR 2.10; 95% CI 1.55, 2.85; I2 = 0%, Pheterogeneity = 0.80; Figure 4).
Forest plot of biochemical pregnancy rate in patients undergoing in vitro fertilization/intracytoplasmic sperm injection, with or without intrauterine human chorionic gonadotrophin (hCG) injection before embryo transfer (n = 693). M-H, Mantel–Haenszel; CI, confidence interval.
Data regarding rate of miscarriage were reported by three studies (hCG group n = 472; control group n = 493),13,14,16 with no significant between-group difference found (OR 1.44; 95% CI 0.84, 2.45; I2 = 0%, Pheterogeneity = 0.88; Figure 5).
Forest plot of miscarriage rate in patients undergoing in vitro fertilization/intracytoplasmic sperm injection, with or without intrauterine human chorionic gonadotrophin (hCG) injection before embryo transfer (n = 965). M-H, Mantel–Haenszel; CI, confidence interval.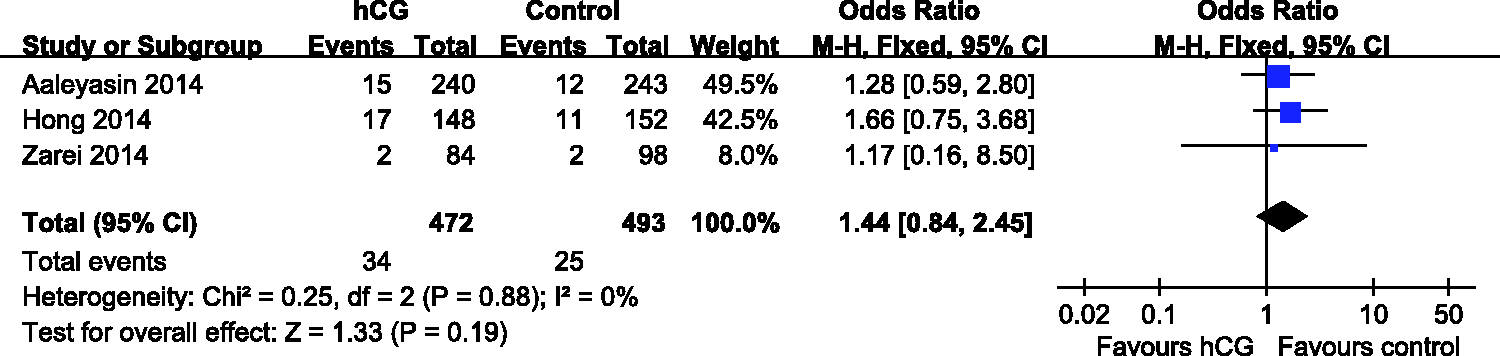
The rate of ongoing pregnancy was reported by three studies (hCG group n = 472; control group n = 493).13,14,16 Ongoing pregnancy rates were significantly higher in the hCG group than in the control group (OR 1.78; 95% CI 1.36, 2.33; I2 = 22%, Pheterogeneity = 0.28; Figure 6).
Forest plot of ongoing pregnancy rate in patients undergoing in vitro fertilization/intracytoplasmic sperm injection, with or without intrauterine human chorionic gonadotrophin (hCG) injection before embryo transfer (n = 965). M-H, Mantel–Haenszel; CI, confidence interval.
Discussion
Human chorionic gonadotropin (hCG) is the first known human embryo-derived signal through which the embryo influences immunological tolerance and angiogenesis at the maternal–fetal interface.3,19–21 It modulates receptivity of endometrial stromal cells and endothelial cell proliferation and migration by regulating interleukin-1 receptors during implantation. This function has an impact on angiogenesis, by a pathway that promotes embryonic growth.5,22,23 hCG also induces endometrial angiogenesis at the site of implantation by upregulating hCG receptors. 22
Intrauterine hCG infusion and in vitro treatment of human endometrial epithelial cells has been shown to upregulate proteins involved in implantation.9,24 The hCG infusion into the endometrial cavity was dys-synchronous with the timing of physiological embryonic hCG secretion, 9 which typically begins at the morula stage. Local treatment with granulocyte colony-stimulating factor or autologous peripheral blood mononuclear cells is known to improve IVF/ICSI outcomes.25–30
To the best of our knowledge, this is the first meta-analysis evaluating the efficacy of intrauterine hCG injection before embryo transfer in IVF/ICSI. Our analysis indicated that intrauterine hCG injection resulted in significantly higher rates of biochemical pregnancy, clinical pregnancy and ongoing pregnancy compared with untreated women. There was no effect on implantation or miscarriage rates. The analysis of implantation rate should be interpreted with caution, however, because although four of the five trials showed significantly higher implantation rates, the pooled results were not significant because the original data for three trials could not be obtained from the authors.12,15,16
The validity and interpretation of any meta-analysis depends largely on the quality and homogeneity of the included studies. Although the trials included in our analysis were all of high quality, there were differences in study population, hCG type and time of administration, type of embryo transferred and embryo transfer technique. Although no heterogeneity was observed in the analysis of biochemical pregnancy rate, clinical pregnancy rate, ongoing pregnancy rate or miscarriage rate, there was significant heterogeneity in the analysis of implantation rate. In addition, due to the small number of RCTs included in this meta-analysis, it was not possible to perform funnel plots to examine publication bias, or carry out subgroup analyses or meta-regression analyses.
It has been shown that intrauterine hCG infusion (500 IU/ml) at the time of blastocyst-stage embryo transfer (fresh or frozen) does not significantly improve sustained implantation or delivery rates. 14 Interventions found to be beneficial at the cleavage stage should be cautiously assessed before implementation at the blastocyst stage. The present meta-analysis cannot assess whether infusion of hCG at an earlier stage, such as day 3, would enhance implantation of embryos transferred at the blastocyst stage.
In conclusion, this systematic review and meta-analysis shows that patients undergoing IVF/ICSI may benefit from intrauterine hCG injection before embryo transfer. Larger scale RCTs are required to confirm these findings.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
