Abstract
We describe the case of a 21-year-old male with hypocalcaemia, hyperphosphataemia, recurrent limb twitch, deafness, proteinuria, increased serum creatinine and urea nitrogen levels, and shrinkage of both kidneys. Brain computed tomography showed intracranial calcifications. The patient was diagnosed with hypoparathyroidism, sensorineural deafness and renal dysplasia (HDR) syndrome. DNA sequence analysis of the GATA3 gene showed a novel de novo mutation, c. 529dupC (p. Arg177profs*126), in exon 2, resulting in a frameshift mutation with a premature stop codon after a new 126 amino acid sequence. We provide further evidence that HDR syndrome is caused by haploinsufficiency of GATA3.
Introduction
*These authors contributed equally to the study.
Genetic mutations resulting in haploinsufficiency of the GATA3 (GATA binding protein 3) gene can lead to HDR syndrome. 6 In humans, GATA3 is expressed in the parathyroid, kidney, inner ear, thymus and central nervous system. 7 The GATA3 protein forms three major functional regions via space folding, including a specific DNA binding and recognition region, transcriptional activation region and nuclear localization region. The transcriptional activation region includes two activation domains (TA1 and TA2) and two zinc finger DNA-binding domains (ZnF1 and ZnF2). Functional studies have found that ZnF2 is essential for DNA binding, while ZnF1 stabilizes binding and mediates interactions with GATA zinc-finger binding proteins (FOG).8,9
Several GATA3 mutation types are associated with HDR syndrome, including deletion, base substitution, frameshift, insertion and splice mutation. We report the clinical manifestations and laboratory findings of a 21-year-old male with HDR syndrome resulting from a novel GATA3 mutation.
Case report
A 19-year-old male presented at the Department of Endocrinology, First Affiliated Hospital of Third Military Medical University, Chongqing, China, in March 2012 recurring limb twitches and weakness, and a 2-year history of foamy urine and renal dysfunction. He exhibited spontaneously twitching limbs without loss of consciousness, which ceased after a few seconds and then recurred. The patient started speaking with normal pronunciation and clear articulation aged 1 year, but at 2 years of age was found to show a poor or absent response to sound and was diagnosed with mixed deafness at a local hospital. Hearing was improved by use of a hearing aid, and the patient could communicate normally and go to school. Recurring limb twitching (without loss of consciousness) began following a fever when he was 2 years old, and was treated by parentally administered calcium supplementation. In 2010, the patient began to exhibit foamy urine with no obvious cause, and his serum creatinine level was substantially elevated. Abdominal colour Doppler ultrasonography revealed small kidneys and calcification of the liver, and the patient was diagnosed with chronic nephritis by the local hospital.
The patient was the first child born to his mother, and was the product of her first pregnancy. He was delivered normally at full term and weighed around 3 kg. His mental and physical development was similar to that of his peers, although he was not as tall. His parents were not consanguineous. The family medical history was unremarkable, and the patient had no siblings.
Physical examination found that binaural hearing was decreased, and the patient wore a hearing aid. His teeth were irregularly arranged, with dental fluorosis. His neck was symmetrical and there was no palpable mass. The thyroid, heart, lungs and abdomen were normal. There was no obvious oedema of the lower limbs. Chvostek’s sign was negative; Trousseau’s sign was positive. During the examination, while the patient was conscious, he exhibited tetanic spasm and involuntary dance-like movements of the hands and feet; the symptoms ceased spontaneously after a few seconds. The interval between attacks varied from tens of minutes to several hours.
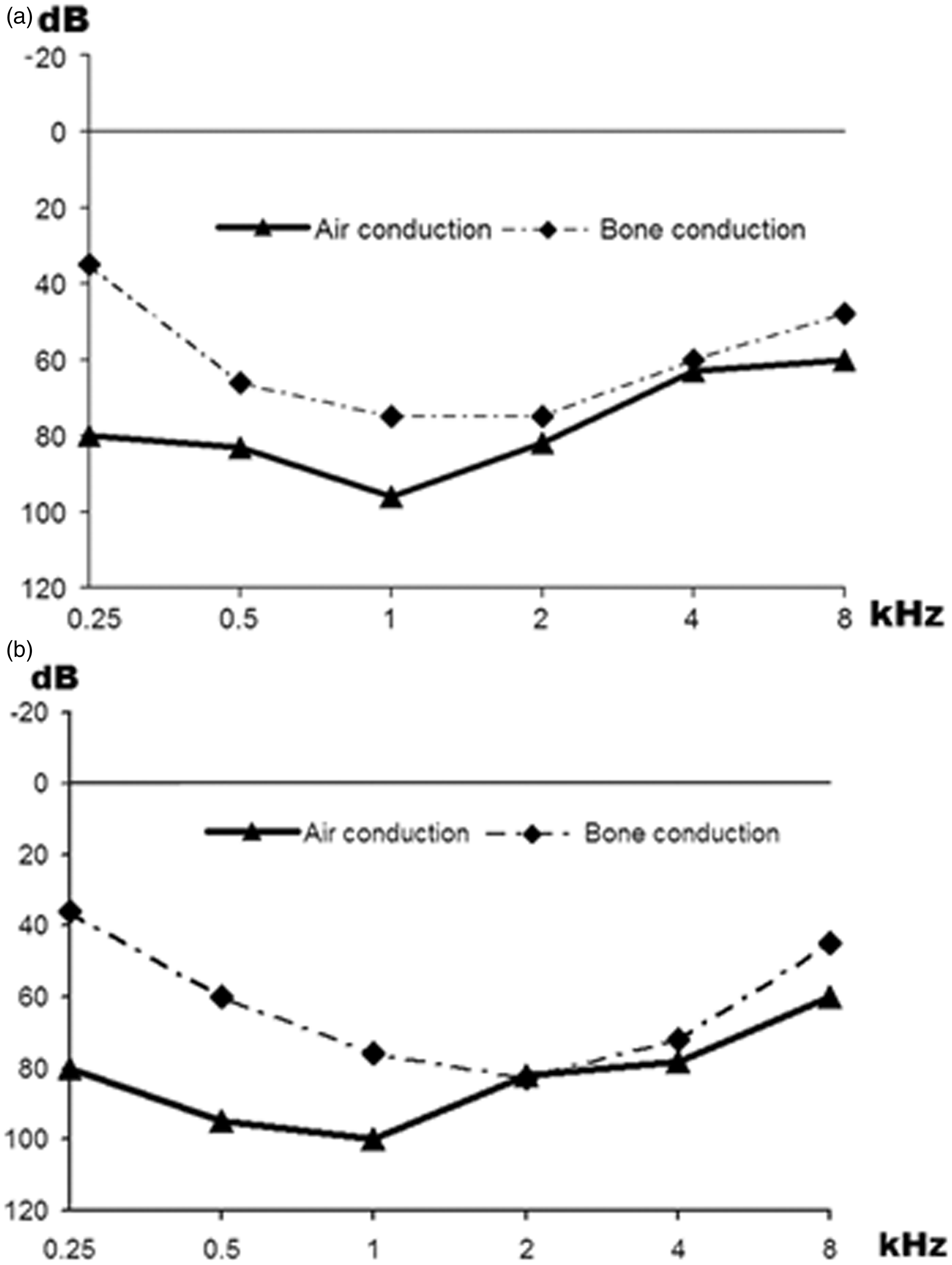
Laboratory examinations revealed serum calcium 1.86 mmol/l (normal range 2.1–2.6 mmol/l), serum phosphate 1.71 mmol/l (0.81–1.55 mmol/l), serum creatinine 215 µmol/l (40–97 µmol/l), serum urea nitrogen 14.3 mmol/l (1.7–8.3 mmol/l), 24-h urine protein 388 mg(10–150 mg) and intact parathyroid hormone 9.96 pg/ml (15–65 pg/ml; PTH Elecsys kit; Roche, Basel, Switzerland). Kidney and urinary tract ultrasonography indicated shrinkage and sparse blood flow in both kidneys, without hydronephrosis, stone or space-occupying lesions. Renal function imaging indicated that the glomerular filtration rate (GFR) of the left and right kidney was 10.63 ml/min and 23.51 ml/min, respectively, after correction for height and body weight. Total GFR was 34.14 ml/min (normal lower limit 90.0 ml/min for both kidneys and 45.0 ml/min for a single kidney). Computed tomography of the brain and abdomen found substantial calcium deposits in the brain and shrinkage in the kidneys (Figure 1). Audiological examination indicated that the patient had bilateral mixed deafness (Figure 2).
Computed tomography image of the brain and abdomen of a male patient with hypoparathyroidism, sensorineural deafness and renal dysplasia (HDR) syndrome showing multiple intracranial calcification in the brain (a) and shrinkage in the kidneys (b). Audiological examination of a 19-year-old male patient with hypoparathyroidism, sensorineural deafness and renal dysplasia (HDR) syndrome indicating bilateral mixed deafness. (a) Right ear; (b) left ear.
The patient was admitted to hospital for re-examination in November 2014. Genetic analysis of GATA3 was performed using DNA extracted from peripheral blood of the patient and his parents, with their consent. Direct sequencing of the exon encoding region of GATA3 gene was performed, and a comparison was made with the reference sequence (NM_001002295.1 and NG_015859.1). A de novo novel heterozygous mutation in exon 2 of the GATA3 gene was detected in the patient (c. 529 dupC [p. Arg177profs*126]). The mutation was absent from both of his parents and an unrelated patient with primary hypoparathyroidism (Figure 3). This de novo frameshift mutation resulted in a premature stop codon after a new 126 amino acid sequence.
Gene sequencing of GATA3 (GATA binding protein 3) in: (a) a 21-year-old male patient with hypoparathyroidism, sensorineural deafness and renal dysplasia (HDR) syndrome; (b) the patient’s father; (c) the patient’s mother; and (d) an unrelated patient with primary hypoparathyroidism. Arrow indicates a de novo, heterozygous c.529dupC mutation in the patient.
The patient and his parents provided written informed consent to report this case, and the report was approved by the ethics committee of the First Affiliated Hospital of Third Military Medical University, Chongqing, China.
Discussion
Since GATA3 was first identified, 51 mutations have been described in patients with HDR syndrome. 10 Mutations can be stratified into three categories according to function: (i) GATA3 truncation/deletion or ZnF2 deletion, causing loss of DNA binding ability (90% of mutations); (ii) ZnF1 deletion, reducing GATA3 DNA binding affinity; (iii) GATA3 protein conformational changes or loss of interaction with FOG.11,12 Mutations can include total gene deletion, nonsense mutation, intragene deletion, intragene insertion and splice mutation. 13 The mutation identified in our patient was a novel heterozygous mutation in exon 2 of GATA3, c. 529dupC (p. Arg177profs*126), a frameshift mutation resulting in a premature stop codon, and therefore a truncated protein lacking both ZnF1 and ZnF2.
Our patient demonstrated the typical triad of HDR syndrome, including recurrent hypocalcaemia, hyperphosphataemia, intracranial calcification, and calcification of the right liver, all caused by hypoparathyroidism. Patients with HDR syndrome can experience epileptic seizures, stiffness, limb spasms, cerebral infarctions and recurrent kidney stones. 14 Post mortem examination found hypoplasia or complete absence of parathyroid glands in some patients with HDR syndrome. 15 Oral vitamin D and calcium supplementation can be useful in treating this disease, by improving calcium absorption and correcting hypocalcaemia caused by increased renal excretion of calcium. The recurrent limb twitching in the present case may be due to the lack of regular vitamin D supplementation.
Hearing loss in patients with HDR syndrome is bilateral, symmetrical sensorineural deafness. 16 The degree of hearing loss and the age of onset vary, however. Our patient exhibited mixed deafness, which was successfully ameliorated by the use of a hearing aid. Hearing damage is not progressive in HDR syndrome. 17
Kidney manifestations of HDR syndrome vary, and can include diffuse proliferative glomerulonephritis or focal segmental glomerular sclerosis, with most patients eventually developing renal failure. 18 In the present case, the main symptoms of renal dysplasia were increased creatinine and urea nitrogen, reduced bilateral renal filtration function, shrinkage and sparse blood-flow signals in both kidneys. Ultrasonography examinations performed 2 years apart revealed a degree of progression and aggravation of renal dysfunction in our patient.
In conclusion, our patient exhibited the typical triad of HDR syndrome. Gene sequencing discovered a novel mutation in exon 2 of GATA3 (*c. 529dupC [p. Arg177profs*126]), resulting in GATA3 haploinsufficiency. Further study is required to understand the functional and structural changes of proteins involved in this disorder and their associations with phenotypic spectrum. Deafness is the characteristic manifestation of HDR syndrome, and patients with deafness and twitch should receive audiometry, serum calcium, phosphorus and parathyroid hormone tests, as well as renal radiographic examinations. The prognosis of these patients is usually associated with renal function. The protection of renal function should therefore be the focus of treatment in HDR syndrome in order to prolong the survival time of patients.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This work was supported by research grants from the National Natural Science Foundation of China (No.81270870).
