Abstract
Objectives
To investigate the roles of high-mobility group box 1 (HMGB1) protein in lymphangiogenesis and lymphatic node metastasis in colon cancer.
Methods
Archival tumour specimens from patients with colon cancer were analysed in this retrospective immunohistochemical study. HMGB1, vascular endothelial growth factor C (VEGF-C) and podoplanin protein levels were analysed immunohistochemically. In vitro studies using the colon cancer cell line HCT116 were also undertaken to investigate the relationship between HMGB1, VEGF-C and nuclear factor (NF)-κB.
Results
Specimens from 70 patients with colon cancer were reviewed. The presence of positive HMGB1 immunohistochemical staining significantly correlated with lymphatic microvessel density, lymph node metastasis and VEGF-C immunohistochemical staining in colon cancer specimens. The presence of positive VEGF-C immunohistochemical staining significantly correlated with lymph node metastasis. The in vitro studies demonstrated that HMGB1 upregulated VEGF-C mRNA and protein in a dose-dependent manner in HCT116 cells, and that this was mediated via NF-κB.
Conclusions
HMGB1 immunohistochemical staining was significantly associated with lymphangiogenesis and lymphatic node metastasis in colon cancer. There was evidence that HMGB1 upregulates VEGF-C by activating NF-κB in a colon cancer cell line.
Keywords
Introduction
The lymphatic vascular system is crucial for the regulation of tissue fluid homeostasis, immune function and lipid metabolism. 1 A considerable amount of research has focused on the mechanism of lymphangiogenesis during embryonic development.2,3 Although research has clearly demonstrated that lymphangiogenesis also occurs in tumours, the details of the lymphangiogenic processes in tumours remain poorly understood.1,4–6
Accumulating evidence demonstrates that inflammation plays a key role in lymphangiogenesis.1,4,5,7 Angiogenesis and lymphangiogenesis have some initiating factors and biological mechanisms in common.1,4,5,7 High-mobility group box 1 (HMGB1, which is, a ubiquitous nuclear protein located in the nucleus, cell surface membranes, cytosol, and mitochondria) was found to play an important role in inflammation and tumour angiogenesis.8–11 HMGB1 can also be released into the extracellular space from tumour cells, 12 necrotic cells 13 or activated cells, especially macrophages.9,14 Released HMGB1 binds to cell surface receptors to activate signalling cascades to produce a functional response, such as angiogenesis.8–11
The aim of this current retrospective immunohistochemical study was to investigate the role of HMGB1 in lymphangiogenesis and lymph node metastasis, in patients with colon cancer.
Patients and methods
Patients and tumour specimens
This retrospective immunohistochemical study analysed archival tumour specimens excised from consecutive patients with colon cancer who underwent surgical excision by the Department of General Surgery, Southwest Hospital, Third Military Medical University, Chongqing, China between December 2003 and October 2004. Surgical specimens were retrieved from the archive of the Department of Pathology, Southwest Hospital. Patients who received radiotherapy or chemotherapy prior to surgery were excluded. Haematoxylin and eosin stained tissue sections from all available complete tumour specimens were reclassified by a pathologist without prior knowledge of patient data. Tumour differentiation was graded as follows: well, moderate or poor. 15 The study was approved by the Ethics Committee of Southwest Hospital. At the time that this work was undertaken, consent from patients was not required for a study of this nature.
Immunohistochemical analysis
As vascular endothelial growth factor C (VEGF-C) plays a key role in lymphangiogenesis and lymph node metastasis4,6,16 and podoplanin is a marker of lymphatic microvessel endothelial cells, 17 HMGB1, VEGF-C and podoplanin were assayed immunohistochemically. All surgical tumour specimens were subjected to routine pathological examination. Tissue samples were fixed in 10% neutral formalin, dehydrated in ethanol and embedded in paraffin wax. Tissue samples were cut into 5-µm-thick sections. After the sections had been deparaffinized and rehydrated in a descending series of alcohol dilutions, they were heated in an 1000-W microwave oven (Galanz, Foshang, China) at maximum power for 5 min in 0.01 mol/l citrate buffer (pH 6.0) for antigen retrieval, then cooled to room temperature. Immunohistochemical staining was performed using the LAB-SA double-staining kit (Beijing Zhongshan Jinqiao Biotechnology, Beijing, China) according to the manufacturer’s instructions. The slides were blocked with blocking buffer from the double-staining kit prior to incubation with the primary antibodies. The applied primary antibodies consisted of the following: goat antihuman HMGB1 (1 : 100 dilution; Santa Cruz Biotechnology, Santa Cruz, CA, USA,), goat antihuman VEGF-C (1 : 200 dilution; Santa Cruz Biotechnology), and mouse antihuman podoplanin (1 : 100 dilution; AngioBio, San Diego, CA, USA).
Immunohistochemical evaluation
Levels of HMGB1 and VEGF-C protein immunostaining were evaluated as previously described, based on the percentage and intensity of positively-stained cells.4,18,19 Five representative areas of each section were randomly selected and ≥200 cells in each area were counted. The mean immunostaining intensity was calculated using an Image-Pro Plus® image analysis system (Media Cybernetics, Rockville, MD, USA). A pathologist without prior knowledge of patient data evaluated all slides and selected one slide as the negative control. Slides with a lower percentage or intensity of positive cells than the negative control slide were considered as negative. Slides with both a higher percentage and higher intensity of positive cells than the negative control slide were considered as positive.
Lymphatic microvessel density (LMVD) was counted as previously described. 17 To be considered lymphatic, vessels had to satisfy all of the following criteria: (i) only a monolayer of podoplanin-positive endothelial cells; (ii) no obvious basal membrane; (iii) no surrounding layer of smooth muscle cells; (iv) no erythrocytic cells in the lumen. Podoplanin-positive endothelial cells that did not form luminal structures were not counted as lymphatic vessels. The distribution of lymphatic vessels was observed in the whole tissue section using a Nikon Eclipse® E400 light microscope at ×100 magnification (Nikon, Tokyo, Japan). Lymph vessels in four high-power fields (at ×200 magnification) were counted and the mean value was taken as the LMVD.
Cell culture
The human colon cancer cell line HCT116 was provided by the Department of Oncology, Southwest Hospital, Third Military Medical University, Chongqing, China. HCT116 cells were cultured in Dulbecco’s modified Eagle’s medium (Gibco® Cell Culture, Carlsbad, CA, USA) supplemented with 10% (v/v) fetal bovine serum, 100 IU/ml penicillin and 0.1 mg/ml streptomycin (all from Hyclone Laboratories, Logan, UT, USA) at 37℃ in an atmosphere containing 5% CO2, using a DNP-9162 incubator (Shanghaijinghong Company, Shanghai, China). The HCT116 cells were used for the transfection studies as described below.
Plasmid construction
The pSUPER.Neo.Retro.GFP RNA interference constructs were produced as previously described. 20 The sense strand of the inserted oligonucleotide for the nuclear factor (NF)-κB p65 subunit was as follows: 5′-gatcccc GCCCTATCCCTTTACGTCA ttcaagaga TGACGTAAAGGGATAGGGC ttttta-3′. The 19-nt of the target sequence is indicated in capitals in the oligonucleotide sequence.
Transfection studies
The plasmid was transfected into HCT116 cells using Lipofectamine® 2000 transfection reagent (Invitrogen, Carlsbad, CA, USA) according to the manufacturer’s instructions, as previously described. 20 Transfected cells were selected with 400 µg/ml G418 (Invitrogen), and were observed under an inverted fluorescence microscope (DM IRB; Leica, Solms, Germany) 3 weeks after transfection; clones were isolated using Scienceware® cloning discs (Sigma-Aldrich, St Louis, MO, USA).
Electrophoretic mobility shift assays
Parental, mock-transfected and transfected HCT116 cells were treated with or without 100 mg/l human HMGB1 full length protein (ab56525; Abcam, Cambridge, UK) for 8 h at 37℃. Their NF-κB activity was evaluated by electrophoretic mobility shift assays (EMSA). To obtain nuclear protein, 1.0 × 107 HCT116 cells were collected into a tube, then suspended and incubated in lysis buffer A (10 mM Tris-HCl [pH 7.5], 1.5 mM MgCl2, 10 mM KCl, 0.5 mM dithiothreitol [DTT], 0.5 mM phenylmethylsulphonyl fluoride, 0.1 mM Na3VO4, and 0.1% Triton X-100™) for 20 min on ice. The lysate was centrifuged at 5 000
The sequence of the sense strand of the double-stranded oligonucleotide probe for NF-κB was as follows: 5′-GCCATGGGGGGATCCCCGAAGTCC-3′ (Geneka Biotechnology, Montréal, Canada). 5 µg of nuclear extract was incubated at room temperature for 15 min in 20 μl of reaction buffer containing 10 mM Tris-HCl (pH 7.5), 1 mM MgCl2, 0.5 mM EDTA, 0.5 mM DTT, 50 mM NaCl, 4% glycerol with 32 P-labelled annealed oligonucleotide and 1 µg of poly(dI-dC). Complexes were resolved on 5% polyacrylamide gels in Tris-HCl-borate-EDTA buffer (pH 8.0) at 10 V/cm. Dried gels were exposed to Carestream® Kodak® BioMax® MS film (Kodak, Rochester, NY, USA) for 1–24 h at −70℃.
Semiquantitative RT–PCR
As VEGF-C plays a key role in lymphangiogenesis and lymph node metastasis,4,6,16 further experiments were undertaken to explore its mechanism of action in vitro. 1.5 × 106 HCT116 cells cultured in a 3.5-cm tissue culture dish were treated with a gradient concentration (1, 10, 20, 50 and 100 mg/l) of HMGB1 (Abcam) for 8 h at 37℃. The amount of VEGF-C mRNA was determined using the reverse transcription–polymerase chain reaction (RT–PCR) as described below.
Total RNA was extracted from 1.5 × 106 HCT116 cells using TRIzol® reagent (Invitrogen). First-strand cDNA was synthesized using 2 µg of total RNA using the TaKaRa RNA PCR Kit (AMV) Ver. 2.1 (TaKaRa Biotechnology, Shiga, Japan). cDNA (1 μl) was taken as a template for the PCR reaction in the presence of Taq polymerase (TaKaRa Biotechnology). The primers used were as follows: VEGF-C forward primer: 5′-CAC TTG CTG GGC TTC TTC TC-3′, reverse: 5′-GAG GTA GCT CGT GCT GGT-3′, amplification product 540 base pairs (bp). The housekeeping gene glyceraldehyde 3-phosphate dehydrogenase (GAPDH) was used as an internal standard. The primers used were as follows: GAPDH forward primer: 5′-CAA ATT CCA TGG CAC CGT CA-3′, reverse: 5′-GGA GTG GGT GTC GCT GTT GA-3′, amplification product 715 bp. The primers were synthetized by Sangon Biotech (Shanghai, China). In the PCR reaction, water was used as a negative control instead of cDNA.
Each gene was amplified by PCR on a PCR Sprint thermal cycler (Hybaid, Ashford, UK) using the following cycle: preliminary denaturation at 94℃ for 5 min, followed by 35 cycles of denaturation at 94℃ for 45 s, annealing for 45 s, and elongation at 72℃ for 45 s, followed by a final elongation step at 72℃ for 10 min. The annealing temperatures for VEGF-C and GAPDH were 49℃ and 53℃, respectively. PCR products were separated using 1.5% agarose gel electrophoresis and visualized using ethidium bromide staining and UV light.
Western blot analysis of VEGF-C in HCT116 cells
For the Western blot analysis, 1.5 × 106 HCT116 cells cultured in a 3.5-cm tissue culture dish were treated with a gradient concentration (1, 10, 20, 50 and 100 mg/l) of HMGB1 (Abcam) for 8 h at 37℃ and then lysed with lysis buffer (50 mM Tris-HCl [pH 8.0], 150 mM NaCl, 0.02% sodium azide, 1% NP-40, 100 µg/ml phenylmethylsulphonyl fluoride, 1 µg/ml aprotinin) on ice for 20 min. After removal of the cell debris by centrifugation (20 000
Western blot analysis of NF-κB p65 and VEGF-C in transfected HCT116 cells
In order to determine if NF-κB knockdown had been successful, parental, mock-transfected and transfected HCT116 cells (1.5 × 106 cells in a 3.5-cm tissue culture dish) were lysed with lysis buffer and Western blotting was performed as described above. Mouse antihuman NF-κB p65 antibody (1 : 1 000 dilution) and mouse antihuman GAPDH antibody (1 : 1 000 dilution) were purchased from Cell Signaling Technology. In order to determine if the upregulation of VEGF-C protein as a result of HMGB1 treatment of HCT116 cells was dependent on the presence of NF-κB activity, mock-transfected and transfected HCT116 cells were treated with 100 mg/l HMGB1 protein (Abcam) for 8 h at 37℃, then prepared for the Western blot analysis of VEGF-C as described above. GAPDH was used as the internal control protein in both experiments.
Statistical analyses
All statistical analyses were performed using the SPSS® statistical package, version 11.0 (SPSS Inc., Chicago, IL, USA) for Windows®. The χ2-test and Spearman’s rank correlation coefficient were used to analyse the relationship between VEGF-C and HMGB1 and other clinicopathological parameters. A P-value < 0.05 was considered statistically significant.
Results
Archival surgical resection specimens from 70 patients with colon cancer (51 male; 19 female) with a mean ± SD age of 54.29 ± 9.13 (range 34–72) years were analysed. Of the 70 tumour samples, 26 were well differentiated, 32 were moderately differentiated and 12 were poorly differentiated. Lymph node metastasis was present in 42 patients. All tumour samples underwent routine immunohistochemical staining for HMGB1 and VEGF-C proteins and podoplanin to identify lymphatic vessels (Figure 1). HMGB1 was visible both in colon cancer cells and in some tumour stromal cells. Positive immunohistochemical staining for HMGB1 was found in cell membranes, cytoplasm and nuclei, but was usually higher in the nuclei (Figure 1A). VEGF-C immunohistochemical staining was also present in colon cancer cells (Figure 1B). Lymphatic vessels consisted of one layer of podoplanin-positive endothelial cells (Figure 1C).
Representative photomicrographs showing positive immunohistochemical staining of high-mobility group box 1 (A), vascular endothelial growth factor-C (B) and podoplanin-positive endothelial cells lining lymphatic vessels (C) in archival samples of colon cancer tissue. The colour version of this figure is available at: http://imr.sagepub.com. Scale bar 100 µm.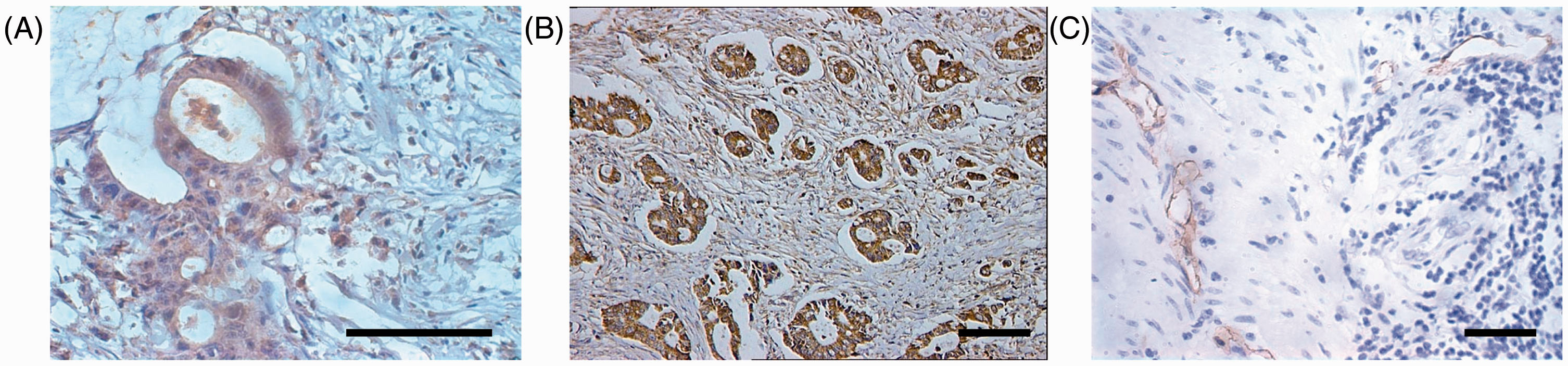
Spearman’s rank correlation coefficient analysis of the association between presence of immunohistochemical staining of high-mobility group box 1 (HMGB1) and vascular endothelial growth factor (VEGF)-C, and clinicopathological parameters in patients with colon cancer (n = 70).

NS, no statistically significant between-group differences (P ≥ 0.05).
Results of the RT–PCR analysis showed that treatment of HCT116 cells with HMGB1 increased the levels of VEGF-C mRNA in a dose-dependent manner (Figure 2A). Results of the Western blot were consistent with those of the RT–PCR, as treatment of HCT116 cells with HMGB1 increased the amount of VEGF-C protein in a dose-dependent manner (Figure 2B).
Treatment of HCT116 cells with high-mobility group box 1 (HMGB1) protein increased the production of vascular endothelial growth factor (VEGF)-C mRNA as demonstrated by reverse transcription–polymerase chain reaction (A) and protein as demonstrated by Western blot analysis (B). Glyceraldehyde 3-phosphate dehydrogenase (GADPH) and β-actin served as internal control proteins
To explore whether NF-κB was involved in the upregulation of VEGF-C by HMGB1, EMSA was employed to evaluate the activity of the NF-κB p65 subunit; Western blot analysis was used to measure levels of NF-κB p65 protein in HCT116 cells transfected with the pSUPER.Neo.Retro.GFP RNA interference construct, designed to knockdown NF-κB activity. Fluorescence microscopic analysis of the transfected HCT116 cells confirmed that 3 weeks after transfection the cells expressed green fluorescent protein (Figure 3A and B), which confirmed that transfection had been successful. Plasmid delivery of the small hairpin RNA used to knockdown NF-κB p65 mRNA in HCT116 cells was demonstrated to be successful using Western blot analysis (Figure 3C), which showed that the amount of NF-κB p65 protein in HCT116 cells transfected with a plasmid targeting NF-κB p65 (siNF-κB) was lower than in parental HCT116 cells and HCT116 cells mock-transfected with empty plasmid. When the same groups of HCT116 cells were treated with HMGB1, the EMSA results showed that although NF-κB activity was increased in all groups compared with the parental HCT116 cells not treated with HMGB1, it was lower in cells transfected with a plasmid targeting NF-κB p65 (siNF-κB) (Figure 4A). Results from the Western blot analysis demonstrated that VEGF-C protein levels were lower in HCT116 cells transfected with plasmid targeting NF-κB p65 (siNF-κB) than in HCT116 cells mock-transfected with empty plasmid following treatment with HMGB1 (Figure 4B).
Knockdown of nuclear factor (NF)-κB activity was investigated using plasmid delivery of small hairpin RNA (siNF-κB) into HCT116 cells. The transfected cells were photographed 3 weeks after transfection under an inverted fluorescence microscope using white light (A) or green fluorescence (B). NF-κB p65 protein levels were determined using Western blot analysis (C): lane 1, nontransfected parental HCT116 cells, lanes 2 and 3, two mock-transfected clones (Mock 1 and Mock 2); lanes 4 – 6, three transfected clones demonstrating NF-κB p65 knockdown (siNF-κB 1, siNF-κB 2 and siNF-κB 3). Glyceraldehyde 3-phosphate dehydrogenase (GADPH) served as internal control. The colour version of this figure is available at: http://imr.sagepub.com Treatment of parental and transfected HCT116 cells with 100 mg/l high-mobility group box 1 (HMGB1) protein for 8 h at 37℃ increased the activity of nuclear factor (NF)-κB as demonstrated by an electrophoretic mobility shift assay (A): lane 1, untreated nontransfected parental HCT116 cells, lane 2, treated nontransfected parental HCT116 cells, lane 3, treated mock-transfected HCT116 cells (Mock), and lane 4, treated transfected HCT116 cells (siNF-κB). Western blot analysis demonstrated that upregulation of vascular endothelial growth factor (VEGF)-C protein as a result of HMGB1 treatment of transfected HCT116 cells was dependent on the presence of NF-κB activity (B): lane 1, one mock-transfected clone (Mock), and lane 2, one transfected clone (siNF-κB). Glyceraldehyde 3-phosphate dehydrogenase (GADPH) served as internal control

Discussion
High mobility group (HMG) proteins form a group of highly conserved chromosomal proteins, which is subdivided into three families: HMGA, HMGB and HMGN. 21 The HMGB family plays an important role in the dynamic changes that take place in chromatin structure, and is also involved in the regulation of cellular processes, such as replication, transcription, recombination and DNA repair.8,21 One member of the HMGB family, HMGB1, consists of 215 amino acid residues, has a molecular weight of 3 kDa, and is a highly conserved nonhistone protein, having >98% homology in the mammalian genome.8,10,21
Initially, HMGB1 was thought to be a nuclear protein because it has high nonspecific affinity with DNA.8,21 HMGB1 serves as a DNA chaperone molecule, sustains nucleosome dynamics and chromosomal stability, participates in DNA repair and telomere maintenance and enhances transcription.8,10 Subsequently, HMGB1 was demonstrated to be present on cell surface membranes, within the cytosol and mitochondria, and to have a wide variety of functions.8,10 HMGB1 can be passively released from dead, dying, or injured cells or it can be actively secreted from cancer cells or immune cells.8,10,13,14,21 Several factors – including endotoxin, interleukin (IL)-1, tumour necrosis factor (TNF)-α and interferon (IFN)-γ – can stimulate HMGB1 secretion.7,8,10 In addition, macrophage engulfment of apoptotic cells may significantly induce HMGB1 secretion.8,22 Accumulating evidence suggests that HMGB1 strongly correlates with cancer and inflammation.8,13
Most of the factors that stimulate HMGB1 secretion, such as endotoxin, IL-1, TNF-α, and IFN-γ can induce angiogenesis.8,21,23–26 Tumour cells and macrophages are able to induce angiogenesis, so it might not be unexpected to find that HMGB1 can promote angiogenesis.5,9,11 Since angiogenesis and lymphangiogenesis have some initiating factors and biological mechanisms in common,1,4,5,7 HMGB1 might also play a role in lymphangiogenesis in colon cancers. The results of this current retrospective study showed that the presence of positive immunohistochemical staining for HMGB1 of archival surgical resection specimens of colon cancer was significantly correlated with LMVD and lymph node metastasis. These findings suggest that because LMVD and lymph node metastasis are indicators of lymphangiogenesis,4,6,27,28 HMGB1 might play a role in colon cancer lymphangiogenesis.
Vascular endothelial growth factor-C is one of central regulators of lymphangiogenesis and lymph node metastasis.4–6 VEGF-C is ubiquitously expressed in a variety of malignant tumours including colon cancer, lung cancer and breast cancer,4,6,16 and plays a dominant role in stimulating lymphangiogenesis via activation of a specific VEGF receptor.4,6,16,29 This present study showed that the presence of positive immunohistochemical staining for VEGF-C of archival surgical resection specimens of colon cancer significantly correlated with lymph node metastasis, which was consistent with other reports in murine models.4,29 A significant correlation was also found between the presence of positive immunohistochemical staining for HMGB1 and VEGF-C, in archival surgical resection specimens of colon cancer.
To further explore the relationship between HMGB1 and VEGF-C, in vitro experiments were undertaken using the HCT116 cell line. Treatment with HMGB1 upregulated both VEGF-C mRNA and protein levels in a dose-dependent manner in HCT116 cells. As VEGF-C is considered to promote lymphangiogenesis and lymphatic node metastasis,4,6 these findings suggest that HMGB1 might upregulate VEGF-C to promote lymphangiogenesis and lymphatic node metastasis in vivo.
It has been reported that NF-κB upregulates VEGF-C in some cancers, such as gastric cancer.30,31 Since both NF-κB and HMGB1 play a critical role in inflammation and are both activated by many common factors such as endotoxin, IL-1, TNF-α, and IFN-γ,7,8,10,32–36 this current study hypothesized that NF-κB might play a role in HMGB1-induced upregulation of VEGF-C in HCT116 cells. Treatment with HMGB1 increased the activity of NF-κB in parental and mock-transfected HCT116 cells, as demonstrated by EMSA. As expected, the increase in HMGB1-induced NF-κB activity was not as great in HCT116 cells transfected with a plasmid targeting the NF-κB p65 subunit (siNF-κB). The NF-κB knockdown experiment also demonstrated that HCT116 cells transfected with a plasmid targeting NF-κB p65 (siNF-κB) decreased the amount of VEGF-C protein compared with mock-transfected HCT116 cells, which suggests that HMGB1 upregulated VEGF-C production via activation of NF-κB.
In conclusion, this present study demonstrated that the presence of positive immunohistochemical staining for HMGB1 of archival surgical resection specimens of colon cancer was significantly correlated with LMVD and lymph node metastasis; the presence of positive immunohistochemical staining for VEGF-C was significantly correlated with lymph node metastasis; and the two proteins were significantly correlated with each other. In vitro experiments showed that HMGB1 activated NF-κB to upregulate VEGF-C in the colon cancer cell line HCT116. Since it is widely accepted that many cancer cells, including colon cancer cells, secrete VEGF-C to promote lymphangiogenesis and lymphatic node metastasis,4,6,19,29 these current data suggest that HMGB1 upregulates VEGF-C via activating NF-κB in colon cancer cells to promote lymphangiogenesis and lymphatic node metastasis.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
