Abstract
Objective
To investigate in vivo confocal microscopy (IVCM) to diagnose hidden corneal foreign bodies.
Methods
Male Kunming mice (n = 25; 12 weeks old) were anaesthetized prior to the insertion of five different materials (spiny wood, rusty iron, sharp stone, sharp glass fragment and human hair fragment) into the cornea by different traumatic processes. A separate mouse was used for each corneal foreign body. The corneas of the mice were scanned 24 h later by a laser scanning IVCM to establish the characteristics (shape, reflectivity and depth in the cornea) of each foreign body. These findings were used to help screen and identify corneal foreign bodies in patients. Corneal smears and scraping cultures were performed in cases of probable corneal infection.
Results
Animal models for the five different foreign particles were established successfully, with each showing distinctive characteristics. These animal results were used to diagnose 41 patients with suspected corneal foreign bodies who were negative by slit lamp examination, but positive by IVCM (observational case series). The most prevalent type of hidden foreign body was plant material (51.2%), followed by metal (29.3%). Ten patients with corneal foreign bodies developed fungal keratitis, found using IVCM.
Conclusions
Laser IVCM is an effective and reliable tool for the diagnosis of hidden corneal foreign bodies.
Introduction
Foreign particles in the cornea are common occupational ocular injuries that are generally caused by pricking accidents or cutting activities.1,2 Patients generally report a prior trauma to the cornea that is accompanied by severe pain. The majority of corneal foreign bodies are metal scraps, plant fragments and stone particles, all of which can be important vectors of corneal infection.3,4 Large corneal foreign bodies are easily detected with a slit lamp examination, but smaller corneal foreign bodies or corneal foreign bodies with infectious keratitis can be difficult to detect and diagnose by routine examination, and are termed ‘hidden corneal foreign bodies’. In vivo confocal microscopy (IVCM) combines fast scanning time with high resolution, and has been used for the in vivo study of the anatomic properties of the cornea in normal and pathological states, including morphological changes after surgery.5–8
This study consisted of two parts. The first was the characterization of common corneal foreign bodies in a mouse model by Heidelberg Retina Tomograph III (HRT III) and Rostock Cornea Module (RCM) IVCM. The same technology was then used for patients presenting with hidden corneal foreign bodies in an observation case series to detect and identify the foreign bodies, and to evaluate the role of laser scanning IVCM in their diagnosis.
Materials and methods
Detection of corneal foreign bodies in mice
Twelve-week-old male Kunming mice (n = 25; weight 36–40 g; from the Laboratory Animal Center of Zhengzhou University, China) were used as a mouse model to identify corneal foreign bodies. The study protocol was approved by the Institutional Animal Care and Use Committee of Henan Eye Institute and all mice were handled in accordance with the Association for Research in Vision and Ophthalmology (ARVO) Statement for the Use of Animals in Ophthalmic and Vision Research.
Mice were anaesthetized with an intraperitoneal injection of pentobarbital sodium solution (50 mg/kg body weight). So that the characteristics of the animal model should be as close as possible to clinical cases, spiny wood, rusty iron and sharp stones were used to scuff the central cornea of the mice before the foreign body was implanted using a stereoscopic microscope (SteREO Discovery V8, Carl Zeiss Meditec, Oberkochen, Germany). The sharp glass fragments were implanted directly in the cornea, and the human hair fragment was implanted after keratomy using a diamond blade for refractive surgery. Five separate mice were used for each corneal foreign body. Each animal was evaluated by slit lamp examination 24 h later and corneal findings were recorded for analysis. The investigator (Z. Xu) was responsible for the implantation of material in the mice eyes, and L. Wang and X. Yu were responsible for the subsequent examination by slip lamp and by IVCM, respectively.
Five different kinds of corneal foreign body models were established and then scanned by a Heidelberg HRT III–RCM laser scanning IVCM (Heidelberg Engineering, Heidelberg, Germany), equipped with a 670 nm wavelength diode laser. The IVCM was operated by a trained professional investigator (X.Y.) using the sequence scanning mode, which allowed images to be repeatedly acquired at different focus positions, enabling the construction of a three-dimensional image.9–11 The scanned images were recorded for analysis.
Detection of hidden corneal foreign bodies in patients
Patients presenting sequentially at the Outpatient Department of the Henan Eye Institute, Zhengzhou, Henan, China between January 2011 and January 2013 with a suspected corneal foreign body, based upon their history and examination with a slit lamp by at least one cornea specialist, were enrolled in this study. Written informed consent was obtained from each patient in accordance with the tenets of the Declaration of Helsinki. The study protocol was approved by The Ethics Committee of Henan Eye Institute. Exclusion criteria included younger patients who were unlikely to be able to keep still for the HRT III–RCM examination or those who were unwilling to undergo this examination, and patients with nystagmus, corneal perforation or active endophthalmitis.
Clinical examination of each patient enrolled in this study included predisposing risk factors, detailed history, slit lamp examination, clinical photography and examination with IVCM. Scanning was carried out to identify different kinds of hidden corneal foreign bodies: identification was based on the characteristics of the corneal foreign bodies in the animal model. Corneal smears and scraping cultures were performed if the patient was suspected of having a corneal infection by a cornea specialist. The corneal scrapings were viewed as wet mount preparations using 10% potassium hydroxide and Giemsa.12–14
Data analyses
The Statistical Package for Social Sciences (SPSS® version 17.0; SPSS Inc, Chicago, IL, USA) was used for statistical analyses. Age was expressed as mean ± SD. The data were evaluated using independent sample t-tests. Scanning images were acquired and recorded by Heidelberg Eye Version 1.5.10.0 (Heidelberg Engineering GmbH, Heidelberg, Germany) and image analysis was performed using Nikon NIS-Elements Advanced Research version 3.2 (Nikon Corporation, Tokyo, Japan).
Results
In this study, five different kinds of corneal foreign body models were established successfully in mice. Under IVCM, the different foreign bodies in mice corneas were detected and their appearance noted (Table 1 and Figure 1).
Representative in vivo confocal microscopy images of foreign bodies in mice cornea: (a) a spiny plant foreign body (arrow) was detected at a depth of 24 µm; (b) a piece of iron (arrow) was observed at a depth of 39 µm; (c) highly reflective stone granules (arrows) were located at a depth of 43 µm; (d) highly reflective and knife-edged glass foreign body was detected at a depth of 75 µm; (e) reflective hair fragment (arrow) was observed at a depth of 63 µm. The scale bar is 50 µm in length. The in vivo confocal microscopy findings of implanted corneal foreign bodies in 12-week-old male Kunming mice.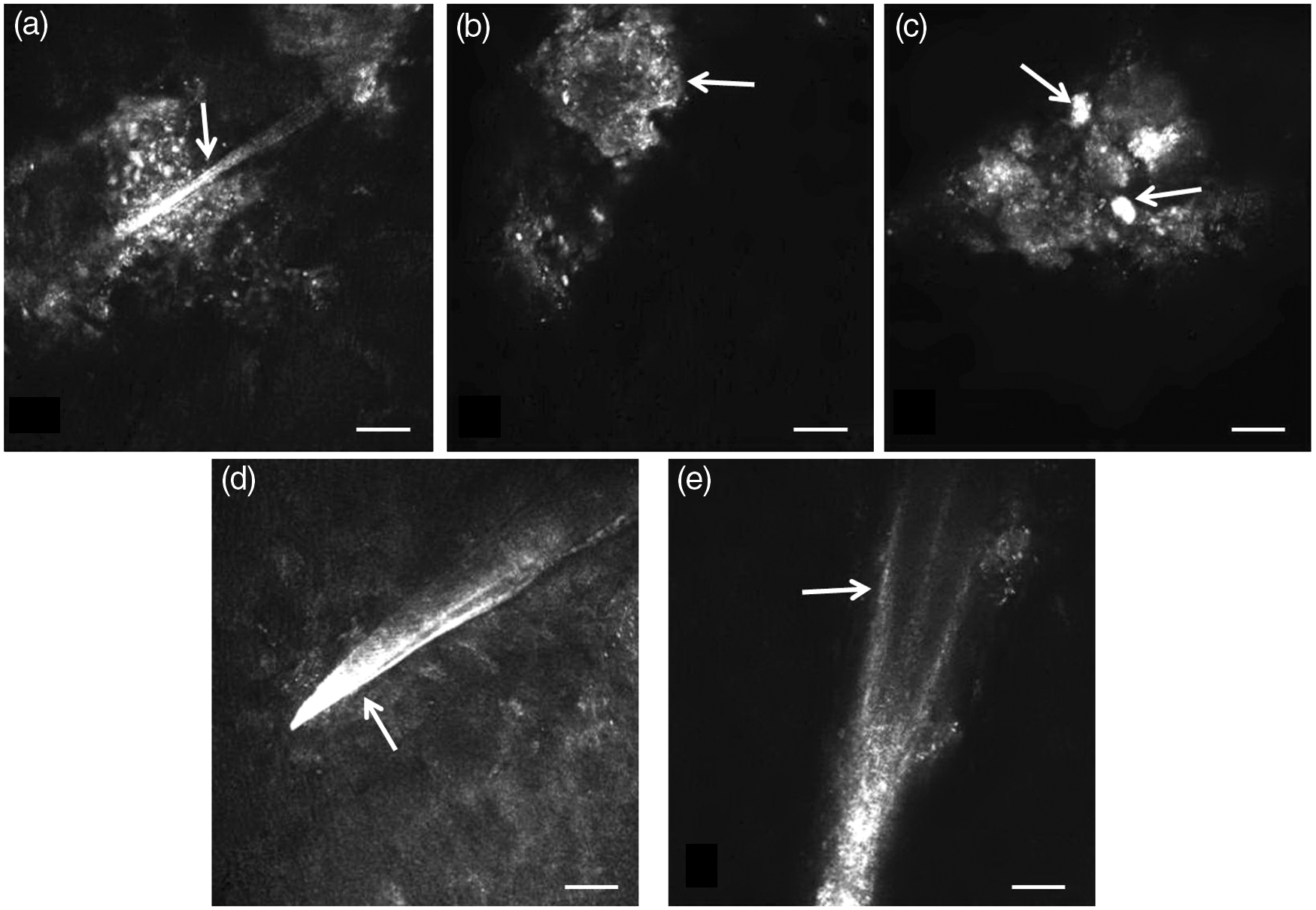

In total, 537 patients were diagnosed with corneal foreign bodies, based on their history and examination with a slit lamp. A further 45 patients, who were negative on slit lamp examination by a corneal specialist (L. Wang), were then examined with HRT III–RCM. The IVCM results diagnosed 41 eyes of 41 patients with hidden corneal foreign bodies; the remaining four patients were still undiagnosed after examination.
Of the 41 patients, 23 (56.1%) were men and 18 (43.9%) were women, and an approximately equal ratio of right and left eyes were affected. The patients ranged in age from 7 to 68 years (men: 42.58 ± 18.63, women: 34.25 ± 14.52, P = not significant, independent samples t-test). When the predisposing risk factors were analysed, a prior incident of trauma to the cornea was reported in 39 patients.
Based on the characteristics of the foreign body under IVCM (Figure 2), 21 patients (21/41, 51.2%) were diagnosed as having a corneal foreign body of plant origin and eight of these were complicated by concurrent corneal infection, 12 patients (29.3%) had a metallic corneal foreign body, five (12.2%) had stone, one (2.4%) had glass, and one (2.4%) had an eyelash fragment. Small parts from a bee sting (one patient, 2.4%) caused the remaining corneal lesion. In the majority of cases, the metal corneal foreign bodies were embedded more deeply than the plant ones. These corneal foreign bodies were removed by surgery and the cornea lesions healed within several weeks. The characteristics of the removed foreign bodies were consisted with the IVCM findings.
In vivo confocal microscopy images of hidden corneal foreign bodies in representative patients: (a) highly reflective spiny foreign body (arrow), the triangle shows a corneal nerve, scanned at a depth of 64 µm; (b) flaky metal foreign bodies (arrows) detected at a depth of 135 µm; (c) several highly reflective stone granules (arrows), located at a depth of 234 µm; (d) highly reflective and knife-edged glass foreign body (arrow), observed at a depth of 66 µm; (e) tiny particles (arrow) from a bee sting, observed at a depth of 97 µm; (f) a tiny eyelash fragment (arrow) at a depth of 449 µm in the cornea. The scale bar is 50 µm in length.
In this study, 10 patients were diagnosed as having corneal foreign bodies and fungal keratitis by IVCM. Although small corneal infiltrations were detected in these cases under a slit lamp, corneal foreign bodies were not found. Smear microscopy showed hyphae in only two patients, with the other eight cases testing negative. Bacterial infection was excluded by Giemsa staining. Corneal foreign bodies and bright hyphae were detected in the corneal lesions of all 10 patients using laser IVCM.
Discussion
In this study, 41 patients were diagnosed with corneal foreign bodies by laser scanning IVCM following inconclusive results using a slit lamp. The slit lamp technique may have failed to detect foreign bodies in the cornea of these patients because of the size and the shape of the corneal foreign bodies (most likely when a plant corneal foreign body is involved), infiltrative corneal lesions or other opaque lesions, which can cover the corneal foreign body, particularly tiny ones, or the presence of corneal foreign bodies associated with severe corneal infections.
Although IVCM has been used for clinical applications in ophthalmology for more than 20 years, HRT III–RCM represents a new generation of machine.15–18 In this study, high resolution laser IVCM was used to diagnose different kinds of concealed corneal foreign bodies. Results showed that glass corneal foreign bodies were more highly reflective than other foreign bodies and had a knife-edged appearance. The reflection from metal corneal foreign bodies was lower than that from glass foreign bodies; the metal foreign bodies had sharp edges and were shaped as chunks or chippings.19,20 The most common type of hidden corneal foreign body was plant matter, which was seen as spiny, exhibited a lower reflectivity than the other foreign bodies described and had a tendency to prick into the superficial cornea. Plant foreign bodies are important vectors of corneal contamination – the fungal keratitis in eight patients was caused by plant foreign bodies, which correlates with values found in studies by Wang et al. and Xie et al.21,22
In one rare case, the patient was stung in the cornea by a bee. When this occurs, the venom and toxins from the bee sting are injected into the cornea and can cause pathological effects at the ocular surface, including conjunctive hyperemia, corneal edema and bullous keratopathy.23–25 The retained sting should be removed carefully by an ophthalmologist, and any home remedies, such as a patient's partner using a cotton bud to abrade the stinger, should be avoided, as these may result in bee sting segments within the cornea and continued inflammation. Using the laser IVCM to scan the lesions on the cornea in this case revealed activated keratocytes, hydropic keratocytes, inflammatory cells and highly reflective particles which may have been bee sting segments.26,27 Severe corneal bee stings can lead to posterior eye complications, including iris atrophy, cataract formation, optic neuritis and papilloedema.28–30
The IVCM images of the corneal foreign body models in the mouse model allowed the identification and diagnosis of 41 patients with hidden corneal foreign bodies. Removal of the foreign bodies from the patients confirmed the confocal findings – all hidden corneal foreign bodies were consistent with the scan diagnosis.
The clinical symptoms and corneal lesions in the four patients for whom a corneal foreign body was not found by either slit lamp examination or by IVCM were assumed to be caused by other pathogenic factors. Three patients were successfully treated with anti-inflammatory therapy and the fourth was successfully treated with antifungal agents.
In this study, IVCM led to better management of patients by identifying the composition of the hidden corneal foreign body. Plant and metal corneal foreign bodies should be removed as early as possible to avoid a serious inflammatory response or a corneal infection; glass foreign bodies always have a sharp edge and can easily penetrate into the anterior chamber of the eye, and so should also be removed as soon as possible. In addition, IVCM can confirm whether a corneal fungal infection is present, and can provide the exact location and quantity of corneal foreign bodies that need to be removed. However, the number of animals included in the mouse model in our study was small, as was the number of patients: animal models including a greater number of mice should be established, and studies with a greater number of patients should be carried out to confirm our findings.
This study shows that IVCM plays an effective and reliable role in the diagnosis of hidden corneal foreign bodies. We recommend that IVCM should be used in: patients with a history of incident corneal trauma and suspected corneal foreign body with slit lamp examination; patients with an incident of corneal trauma and nonhealing lesions despite receiving intensive topical antimicroorganism and anti-inflammatory therapy; patients with corneal trauma, especially plant trauma and clear corneal infiltrations; patients undergoing surgical removal of corneal foreign bodies but with a persistent inflammatory reaction in the lesion. There should be an increase in the role of IVCM in diagnosing corneal foreign bodies.
Footnotes
Declaration of conflicting interest
The authors have no conflicts of interest to declare in relation to this article.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
