Abstract
Objective:
A retrospective study to evaluate intraoperative electron beam radiotherapy (IOERT) as a primary treatment modality for stage IIB cervical squamous cell carcinoma.
Methods:
Patients underwent treatment with IOERT (n = 78) or radical radiotherapy (RT; n = 89). Patients in the IOERT group received 20 Gy external beam radiotherapy (EBRT) in 10 fractions, intracavitary brachy -therapy (7 - 14 Gy, in patients with tumours ≥ 4 cm in diameter) and simple hysterectomy/selective lymphadenectomy with 18 - 20 Gy IOERT. Patients in the RT group received 50 Gy EBRT in 25 fractions followed by intracavitary brachytherapy (35 - 40 Gy).
Results:
Median duration of follow-up was 92 months. IOERT resulted in significantly better 5- and 10-year overall survival, disease-free survival and local control rates, as well as fewer rectal and bladder complications, compared with RT.
Conclusion:
IOERT is an effective primary treatment for stage IIB cervical squamous cell carcinoma.
Introduction
Cervical cancer is the second most common cancer in women, with 80% of cases occurring in developing countries. 1 Approximately 25% of patients relapse after 5 years, and locoregional failure accounts for > 50% of these relapses. 2 The 2-year survival rate following local recurrence of cervical cancer is poor, at ∼22% regardless of treatment. 3 Recurrent cervical cancer is associated with pain, anorexia, vaginal bleeding, cachexia and psychological sequelae. 4 It is therefore important to improve the local control rate during primary treatment, to reduce the risk of recurrence or distal metastasis.
Cisplatin-based concomitant chemo -radiotherapy has been shown to be more effective than radiotherapy alone for locally advanced cervical cancer,5 – 8 and is the standard treatment for this disease. 9 It is thought that concurrent chemotherapy improves local control by enhancing the effects of radiation.10 – 12 Chemoradiotherapy is associated with increased acute toxicities and may therefore result in undesirable radiotherapy treatment breaks. 9 The benefit over radiotherapy alone is small, particularly in developing countries where ancillary medical care is poor. 13 Alternative methods for improving local control are therefore required.
Intraoperative electron beam radiotherapy (IOERT) is used for the treatment of cancers at various sites,14,15 including salvage of recurrent cervical cancer. 11 As a primary treatment modality, a combination of preoperative chemo -radiation, surgery and IOERT resulted in 92% local control after 10 years. 16 The aim of the current retrospective study was to evaluate the use of IOERT versus radical radiotherapy (RT) in patients with stage IIB cervical squamous cell carcinoma, in terms of survival, recurrence, metastasis and adverse effects.
Patients and methods
Study Population
All patients with cervical cancer who were undergoing radiation treatment at the Department of Radiation Oncology, First Affiliated Hospital, Medical College of Xi'an Jiaotong University, Xi'an, China, between June 2001 and May 2007, were considered for inclusion in this retrospective study. Inclusion criteria were: (i) histologically proven squamous cell carcinoma; (ii) tumours classified as International Federation of Gynecology and Obstetrics stage IIB 17 ; (iii) aged < 75 years; (iv) no evidence of pelvic or para-aortic lymph node metastasis on computed tomography (CT) scan; (v) no evidence of metastasis on chest X-radiography; (vi) normal liver and kidney function; (vii) normal blood count; (viii) haemoglobin level > 9 g/l. Patients with nonsquamous cell carcinoma or previous radiotherapy to the pelvis were excluded from this analysis.
All patients underwent pretreatment investigations including Eastern Cooperative Oncology Group performance status, 18 gynaecological examination under general anaesthesia, cystoscopy and biopsy. Tumours were graded according to American Joint Committee on Cancer criteria. 19
The study was approved by the Ethics Committee of the Medical College of Xi'an Jiaotong University, Xi'an, China, and all patients provided written informed consent for treatment.
Treatment
A radiation oncologist and gynaecological surgeon provided each patient with identical information regarding treatment options; the patient was then allowed to choose between IOERT (with hysterectomy) and RT (without hysterectomy).
Radical radiotherapy comprised a total dose of DEQD2 (equivalent dose in 2 Gy fractions) 50 Gy external beam radiotherapy (EBRT), delivered in 2 Gy fractions five times a week for 5 weeks, using 6 – 10 MV parallel opposed anterior–posterior fields. The initial 30 Gy of radiotherapy was delivered to the entire pelvis, with central shielding (minimum width, 4 cm) applied for the remaining 20 Gy. The borders of the radiation field were the L4/L5 junction (superior), 1 cm below the obturator foramen (inferior) and 2 cm beyond the pelvic brim (lateral). Intracavitary temporary brachytherapy was performed weekly, beginning 28 days after initiation of EBRT, and twice weekly after completion of EBRT until week 7. Tandem and ovoid applicators (Nucletron, Veenendaal, Netherlands) were used to deliver a total dose of DEQD235 – 40 Gy high dose rate iridium-192 in 5 – 6 insertions, to International Commission on Radiation Units and Measurements (ICRU) reference point A. 20 Calculations of dwell times and ICRU bladder and rectal point doses were performed via orthogonal X-radiography after each insertion. Bladder and rectal point doses were limited to DEQD280 and DEQD275 Gy, respectively. Treatment was completed within 7 weeks.
Patients in the IOERT group received a total dose of DEQD220 Gy EBRT, delivered in 10 fractions of 2 Gy five times a week for 2 weeks, as described above. In addition, intracavitary temporary brachytherapy (one or two insertions of 7 Gy each, as described above) was performed 1 week after the initiation of EBRT, in cases where the tumour was ≥ 4cm in diameter. Simple hysterectomy with dissection of palpable pelvic lymph nodes was performed in all patients 1 – 2 weeks after EBRT. A 12 MeV electron beam (Clinac 1800; Varian Medical Systems, Palo Alto, CA, USA) and applicator 21 were used to deliver 18 – 20 Gy of radiation (DEQD236 – 50 Gy) to the pelvic cavity during surgery, with the field borders at the bifurcation of common iliac vessels (superior), 2 cm inferior to the vaginal vault (inferior), and 1 cm beyond the lateral margin of external and common iliac vessels (lateral). The bladder, intestines and sigmoid colon were shifted out of the radiation field, and the rectum was shielded with 6-mm thick lead.
Follow-up
After completion of treatment, patients were followed-up at 3-month intervals for 1 year, 6-month intervals for 3 years and annually thereafter. Investigations included complete blood count, chest X-radiography, abdominopelvic CT, gynaecological examination and biopsy where necessary. Overall survival was defined as the time from the end of treatment until death from any cause. Disease-free survival was defined as the time from the end of treatment until recurrence or metastasis. Local control was defined as the time from the end of treatment until recurrence.
Statistical Analyses
Between-group differences in recurrence, metastasis and complications were made using the χ2-test. Survival times were calculated using the Kaplan–Meier method and compared using the log-rank test. Statistical analyses were performed using SPSS® version 12.0 (SPSS Inc., Chicago, IL, USA) for Windows®. A P-value < 0.05 was considered statistically significant.
Results
The study population comprised 167 patients (IOERT n = 78; RT n = 89). Baseline demographic, clinical and tumour characteristics are shown in Table 1. There were no significant between-group differences in age, ECOG performance status, anaemia (defined as a haemoglobin level < 10 g/dl) or tumour characteristics. All patients completed the planned course of treatment. The median overall duration of follow-up was 92 months (range 16 – 155 months). A total of 49 patients in the RT group and 66 patients in the IOERT group were recruited ≥ 10 years prior to the conclusion of the study, and were included in calculations of 10-year survival and recurrence.
Baseline demographic, clinical and tumour characteristics of patients included in a study to compare intraoperative electron beam radiotherapy (IOERT) with radical radiotherapy (RT) for primary treatment of stage IIB 17 cervical squamous cell carcinoma

Data presented as median (range) or n (%) of patients.
ECOG, Eastern Cooperative Oncology Group.
No statistically significant between-group differences (P ≥ 0.05); χ2-test.
The 5- and 10-year overall survival, disease-free survival and local control rates were significantly higher in patients who underwent IOERT compared with those who received RT (P < 0.01 for all comparisons; Table 2). Kaplan–Meier curves for disease-free and overall survival are shown in Fig. 1.
Kaplan–Meier survival analysis of patients with stage IIB
17
cervical squamous cell carcinoma undergoing primary treatment with intraoperative electron beam radiotherapy (IOERT) or radical radiotherapy (RT). (A) Disease-free survival; (B) overall survival
Overall and disease free-survival and local control rates in patients with stage IIB 17 cervical squamous cell carcinoma who underwent primary treatment with intraoperative electron beam radiotherapy (IOERT) or radical radiotherapy (RT)
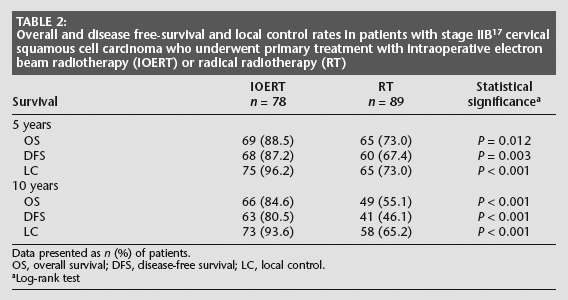
Data presented as n (%) of patients.
OS, overall survival; DFS, disease-free survival; LC, local control.
Log-rank test
The rates of local recurrence and distal metastasis at 5 and 10 years after completion of treatment are shown in Table 3. IOERT was associated with better locoregional control (cervix/vagina and pelvic lymph nodes) than radiotherapy at both 5 and 10 years (P < 0.05 for all comparisons). There were no significant between-group differences in the rates of metastasis (para-aortic lymph nodes, lung or liver) at 5 or 10 years after the completion of treatment.
Rates of recurrence or distal metastasis in patients with stage IIB 17 cervical squamous cell carcinoma 5 and 10 years after primary treatment with intraoperative electron beam radiotherapy (IOERT) or radical radiotherapy (RT)

Data presented as n (%) of patients.
NS, not statistically significant (P ≥ 0.05).
χ2-test.
The use of IOERT was associated with significantly fewer cases of radiation-induced rectal or bladder injury than RT (P < 0.05 for both comparisons; Table 4). There were no significant between-group differences in the incidence of pelvic pain and peripheral neuropathy, hydronephrosis or oedema of the lower leg.
Complications in patients with stage IIB 17 cervical squamous cell carcinoma following primary treatment with intraoperative electron beam radiotherapy (IOERT) or radical radiotherapy (RT)
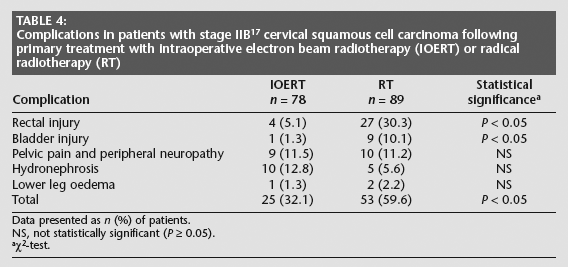
Data presented as n (%) of patients.
NS, not statistically significant (P ≥ 0.05).
χ2-test.
Discussion
This retrospective study of IOERT as primary treatment for cervical cancer indicated significantly improved overall survival, disease-free survival and local control compared with RT. The 5-year overall survival and disease-free survival rates for cervical cancer have been reported as 72.2% and 65.8%, respectively, 2 which are comparable with to the findings in the RT group, in the current study. Overall and disease-free survival rates were significantly higher in the IOERT group than in the RT group (Table 2), but further studies in a clinical trial setting are required in order to confirm this finding. Locoregional control rates at 5 and 10 years were significantly higher following IOERT compared with radiotherapy. There was no between-group difference in the rate of distal metastasis in the present study, which was expected due to the local nature of IOERT.
Intraoperative electron bean radiotherapy delivers a single high dose of radiation (18 – 20 Gy; DEQD236 – 50 Gy). Studies have revealed that stereotactic body radiotherapy provides greater than expected efficacy than can be predicted from clonogenic cell inactivation alone. 22 A single high dose of radiation allows delivery of a large equivalent dose of radiation to the tumour, such that a single dose of IOERT is 1.5 – 2.5 times more effective than the same total dose of fractionated EBRT.23 – 25 In addition, IOERT is applied during surgery, rather than at a much later time point (as is required with conventional EBRT), in order to avoid interfering with wound healing. 26 An additional advantage of IOERT is that the risk area can be assessed intraoperatively, allowing tailoring of the radiation field. The fact that the patient is unconscious and immobile during surgery further increases the accuracy of IOERT.27,28
Both treatment methods in the present study resulted in approximately the same dose of radiation being delivered to ICRU point A. The total dose delivered to point A by RT was DEQD280 Gy, comprising DEQD230 Gy EBRT and DEQD250 Gy brachytherapy. IOERT delivered a total dose of DEQD276 – 80 Gy (EBRT DEQD220 Gy + IOERT DEQD236 – 50 Gy). It is possible that the improved local control in IOERT was a result of surgical removal of the tumour and the ability to deliver radiation accurately to areas at risk of microscopic disease. The rates of bowel and bladder injury were lower in the IOERT group than in the RT group, probably due to the careful shielding employed during irradiation. In addition, some patients in the IOERT group received brachytherapy after a comparatively low dose of EBRT (8 – 16 Gy, compared with 30 Gy in the RT group), with the result that most of the high-dose region was likely to fall within the gross tumour. This is compared with the RT group, where the tumour would have shrunk significantly by the time that brachytherapy was delivered.
The use of combined surgery and RT is not recommended for the treatment of early stage cervical cancer 29 because of the increased risk of severe toxicities. 30 Data regarding the rate of complications after IOERT are inconclusive, with some showing no difference in complications 31 and others finding an increase in adverse effects. 32 The reduced rate of adverse effects with IOERT compared with radiotherapy in the present study may be due to the use of simple hysterectomy with limited nodal dissection, rather than radical hysterectomy and complete pelvic lymph node dissection, thus reducing the duration of surgery and limiting the extent of injury to healthy tissue. In the IOERT group in the present study, the radiation dose to the bowel and bladder was limited by moving the organs away from the applicator during irradiation, and the known low level of radiation leakage (5%) from the applicator itself. 21
In the present study, the incidence of pelvic pain and peripheral neuropathy was similar in both treatment groups. The rates of chronic pelvic pain and peripheral neuropathy following IOERT have been shown to range between 10 and 30%.16,33,34Rates of other complications, including hydronephrosis and oedema of the lower leg, were also similar between the groups. All cases of toxicity were managed using conservative treatment.
This study has several limitations. First, its retrospective and nonrandomized nature may have resulted in selection bias: fitter patients could have chosen surgery and patients with more comorbidities could have chosen radiation alone, leading to differences in overall survival. Secondly, chemo radio -therapy is recommended for treatment of locally advanced cervical cancer, but none of the patients in the current study received concurrent chemotherapy. It is therefore unclear what impact, if any, this would have had on the outcome. Thirdly, the grading of toxicities was not performed consistently and it was therefore not possible to report any data regarding the severity of adverse events. Finally, the optimal IOERT dose is not known. Doses ranging from 10 – 30 Gy have been reported.31,35,36 Whether a lower dose would reduce toxicities, or a higher dose would further improve local control, is not known.
In conclusion, the present study findings indicate that IOERT is an effective treatment for stage IIB cervical squamous cell carcinoma, resulting in enhanced local control and improvements in disease-free and overall survival compared with RT, without an increase in complications. IOERT does not prevent distant metastasis, however, and more effective systemic therapies should be evaluated.
Footnotes
Conflicts of interest: The authors have no conflicts of interest to declare in relation to this article.
Acknowledgements
This work was supported by grants from the National Natural Science Foundation of China (No. 81071838), Shaanxi Province Department of Health Key Program (No. 2010A02) and the Foundation of the First Affiliated Hospital of Medical College of Xi'an Jiao Tong University (No. 2010YK3).
