Abstract
Objective:
To evaluate retrospectively the outcomes of partial lower axillary lymph node dissection caudal to the intercostobrachial nerve in patients with clinically node-negative (N0) breast cancer.
Methods:
Numbers of dissected and metastatic nodes, overall and disease-free survival rates, postoperative complication rates, and axillary recurrence were compared between patients who underwent breast cancer surgery with partial axillary node dissection (n = 1043) and historical controls who underwent conventional dissection (n = 1084).
Results:
The 5-year overall and disease-free survival rates were 95.6% and 89.7%, and 94.9% and 88.4%, respectively, in the partial dissection and conventional dissection groups; the differences were not significant. Mean duration of surgery (41.6 min versus 60.9 min), intraoperative blood loss (28.0 ml versus 51.3 ml), volume of lymphatic drainage at 2 weeks postoperatively (488 ml versus 836 ml), and persistent arm lymphoedema (0.0% versus 11.8%) were significantly different between the partial and conventional dissection groups, respectively.
Conclusions:
Partial axillary lymph node dissection was associated with similar survival rates (but lower postoperative complication rates) compared with conventional axillary dissection and is recommended in patients with N0 breast cancer.
Keywords
Introduction
Axillary lymph node harvesting is recommended as standard treatment in breast cancer to control local recurrence and classify lymph node metastasis (pN stage).1 – 4 Several studies have indicated that routine complete axillary lymph node dissection does not improve the survival rate after breast cancer surgery in patients who are clinically node negative (N0).2,5– 7 The National Surgical Adjuvant Breast and Bowel Project B-04 trial found no significant differences in 10-year survival rates between patients who underwent radical mastectomy with axillary dissection and those who underwent simple mastectomy without axillary dissection;5,6 this was despite histo -pathological examination demonstrating metastasis in ∼40% of patients without clinical axillary node metastasis. Similarly, a meta-analysis demonstrated that combined axillary dissection and radiotherapy did not improve survival after surgery. 8 Sentinel node biopsy (SNB) with selective axillary lymph node dissection has now become the standard of care in patients with N0 breast cancer.2,3,9,10 The American College of Surgeons Oncology Group Z0011 randomized controlled trial 7 and a large retrospective study from the National Cancer Data Base 11 reported no differences in disease-free or overall survival rates between selected patients with microscopic sentinel node metastasis who underwent axillary dissection and those who did not.
A randomized controlled study comparing level I with level III axillary lymph node dissection found no differences in disease-free and overall survival rates, despite evidence of metastasis in 4.7% and 7.4% of the level II and III nodes, respectively, in patients who underwent level III dissection. 12 These findings indicate that the objective of axillary dissection should be limited to local axillary control, particularly in early breast cancer, in order to minimize postoperative complications.
Sentinel node biopsy is associated with lower morbidity than complete axillary lymph node dissection.13 – 15 The procedure of partial lower axillary lymph node dissection, which involves dissection of only the level I nodes caudal to the intercostobrachial nerve, has been developed to reduce further the rates of postoperative seroma and arm lymphoedema occurring after SNB. The aim of the present study was to examine axillary recurrence, postoperative complications (arm lymphoedema and postoperative seroma), and overall and disease-free survival rates after partial lower axillary lymph node dissection, compared with conventional level I to level III axillary lymph node dissection, in patients with N0 breast cancer.
Patients and methods
Study Population
This was a retrospective observational study that sequentially enrolled all patients with cytohistologically-confirmed N0 breast cancer who were scheduled to undergo mastectomy or breast-conserving surgery and partial lower axillary lymph node dissection, at the Kodama Breast Clinic, Kyoto, Japan between January 2001 and December 2008. Historical control data were obtained from all patients who underwent breast cancer surgery with conventional axillary lymph node dissection at the same institution, and by the same surgeons (H.K. and K.M.), between January 1994 and December 2000. Patients' disease levels were staged according to the International Union Against Cancer classification system. 16
Patients in both the study and historical control groups received 800 mg doxifluridine (Furtulon® R: a 5-fluorouracil prodrug) orally three times daily for 2 years as postoperative adjuvant therapy. Patients with oestrogen receptor/progesterone receptor-positive breast cancer received 200 mg tamoxifen orally once daily for 2 years.
All patients and their families were fully informed of the study aim, treatment programme and expected clinical outcomes (such as overall and disease-free survival and complication rates). Written informed consent was then obtained from each participant. As all patients received the same treatment during the study period and the results were compared with historical controls, it was not considered necessary to obtain Institutional Review Board approval for the study design.
Assessment of Postoperative Complications and Survival
Postoperative complications (lymphatic drainage and arm lymphoedema) were assessed by comparing a subgroup of consecutive patients from the conventional axillary lymph node dissection group during the year 2000 with a subgroup of the same number of consecutive patients from the partial dissection group during the year 2001. Arm circumference was measured at 3 months and 1 year postoperatively. Arm lymphoedema was defined as an increase in arm circumference of > 3 cm compared with the contralateral arm and was classified as persistent (an increase lasting for ≥ 1 year) or transient (an increase lasting for 3 months but resolving within 1 year).
Lymphatic drainage was assessed by measuring the total volume of fluid collected by an indwelling drain at 2 weeks postsurgery. Five-year overall and disease-free survival rates of patients who underwent partial dissection were compared with historical controls. Overall survival was defined as the time from surgery until death from any cause; disease-free survival was defined as the time from surgery until death or first documented recurrence of breast cancer.
Partial Lower Axillary Lymph Node Dissection
During breast cancer surgery, the intercostobrachial nerve was identified at the lateral border of the pectoralis muscle in the axilla. The nerve was retracted using tape, and the axillary tissue caudal to the nerve divided into two to three parts. After focal radiofrequency ablation using a needle, the caudal axillary tissue was excised (Fig. 1). Focal ablation is an important part of this procedure, as it prevents leakage of lymphatic fluid from the remaining mammary and axillary tissues, thus minimizing the occurrence of postoperative axillary seroma.
Schematic diagram showing partial lower axillary lymph node dissection. Complete interruption between the upper and lower parts of the axillary tissue is essential to reduce the volume of postoperative lymphatic fluid collection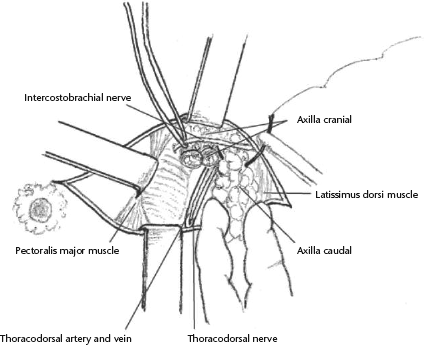
Statistical Analyses
Baseline and clinical characteristics and postoperative complications were compared between the partial and conventional dissection groups using the Student's t-test for continuous variables or the χ2-test for categorical variables. Overall and disease-free survival rates were calculated according to the life-table method and compared between surgical groups using the log rank test. All statistical analyses were performed using the StatView statistical package, version 4.5 (SAS Institute Inc., Cary, NC, USA). A P-value < 0.05 was considered statistically significant.
Results
A total of 1043 patients with cyto histo -logically-confirmed N0 breast cancer who underwent partial lower axillary lymph node dissection and 1084 historical controls who underwent conventional dissection were included in this analysis. There were no significant differences in the baseline patient characteristics of age, menopausal status and preoperative tumour stage between the partial and conventional dissection groups (Table 1).
Demographic and clinical characteristics of patients with node-negative breast cancer who underwent partial or conventional axillary lymph node dissection

Data presented as mean ± SD or n of patients.
Disease levels staged according to the International Union Against Cancer classification system. 16
Statistical analyses were undertaken using the Student's t-test for continuous variables or the χ2-test for categorical variables.
T, tumour; Tis, carcinoma in situ (ductal carcinoma in situ, lobular carcinoma in situ or Paget disease of the nipple with no associated tumour mass); N, node; BCS, breast-conserving surgery; NS, no statistically significant between-group differences (P ≥ 0.05).
Significantly more nodes were dissected in the conventional dissection group compared with the partial dissection group (P < 0.0001; Table 1). Numbers of metastatic lymph nodes following partial or conventional dissection are shown in Table 2. Even though there was a significant difference in overall postoperative N stage between patients who underwent conventional compared with partial dissection (P = 0.0003; Table 1), there was no significant between-group difference in the proportion of patients without nodal metastasis (pN0) across all patients with 0 – 3 metastatic nodes (i.e. patients with pN0 cancer plus those with pN1 cancer) between the two groups (79.5% [802/1009] versus 81.1% [821/1012], respectively; Table 2).
Number of metastatic axillary lymph nodes following partial or conventional dissection in patients with node-negative breast cancer

Data presented as n (%) of patients.
Statistical analyses were undertaken using the χ2-test for categorical variables.
Comparison between partial dissection group (n = 1043) and conventional dissection group (n = 1084).
Despite a significant difference in the overall recurrence rate between the conventional and partial dissection groups (P < 0.001; Table 3), there was no significant between-group difference in the recurrence rate of axillary node metastases. The postoperative follow-up period was shorter in the partial dissection group compared with the conventional dissection group (Table 3). There were only six cases (0.6%) of axillary node recurrence in the partial dissection group and there were no identifiable trends in clinical characteristics in these patients (Table 4), which included three N0 cases. At the time of writing, these six patients were all alive.
Clinical course of patients with node-negative breast cancer following partial or conventional axillary lymph node dissection

Data presented as median or n (%) of patients.
Statistical analyses were undertaken using the χ2-test for categorical variables.
ND, not determined; NS, no statistically significant between-group differences (P ≥ 0.05).
Clinical characteristics of six patients with node-negative breast cancer who experienced axillary lymph node recurrence following partial dissection

Disease levels staged according to the International Union Against Cancer classification system. 16
DFS, disease-free survival; pT, postoperative tumour stage; pN, postoperative node stage; ER, oestrogen receptor; M, mastectomy; BCS, breast-conserving surgery.
Postoperative complications (lymphatic drainage and arm lymphoedema) were compared between 110 consecutive patients who underwent conventional axillary lymph node dissection during the year 2000 and 110 consecutive patients who underwent partial dissection during the year 2001 (Table 5). The mean total volume of fluid collected by an indwelling drain at 2 weeks after surgery was significantly lower in the partial dissection group than the conventional dissection group (P < 0.001). Persistent arm lymphoedema was significantly less frequent in the partial dissection group than the conventional dissection group (P < 0.0001).
Postoperative complications in patients with node-negative breast cancer following partial or conventional axillary lymph node dissection

Data presented as mean ± SD or n (%) of patients.
Statistical analyses were undertaken using the Student's t-test for continuous variables or the χ2-test for categorical variables.
There were no significant differences between the surgical groups with respect to the 5-year overall survival rates or the 5-year disease-free survival rates (Fig. 2).
(A) Overall survival and (B) disease-free survival in patients who underwent breast cancer surgery and partial dissection (group A; n = 1043) or conventional axillary lymph node dissection (group B; n = 1084). There were no significant differences in the overall or disease-free survival rates between the two surgical groups as determined by log rank test (P ≥ 0.05)
Discussion
Developments in surgical treatments, systemic therapy and radiation therapy result in a need for frequent re-evaluation of local therapy for breast cancer. Clinical trials previously conducted at the Kodama Breast Clinic have explored postoperative outcomes following the dissection of smaller areas of axillary lymph nodes, compared with conventional dissection. Between 1995 and 1997, a randomized controlled trial of 514 patients with N0 or N1 breast cancer compared outcomes in patients who underwent level III dissection (Kodama's method) 17 with patients who underwent level I dissection only (Auchincloss' method). 18 There were no significant differences in the 10-year survival rates between the two groups. 12 In a preliminary study in 2000, level I nodes on the cranial and caudal sides of the intercostobrachial nerve were separately dissected in 100 patients with N0 breast cancer, and the numbers of dissected nodes with or without metastasis in each of these areas were examined (Kodama H, unpublished). The results showed that the presence or absence of axillary node metastasis could be determined in 94% of cases by dissection limited to the area caudal to the intercostobrachial nerve. Node metastasis in the area cranial to the intercostobrachial nerve was found in only 8% of patients. This was comparable with the reported false-negative rates of 5 – 10% for SNB.2,3,14,19 Considering that the major objective of axillary dissection is to obtain information regarding lymph node metastasis,2,3 and that failure to clear all node metastases in the upper part of the axilla has no impact on prognosis,7,11,20 these data suggested that partial dissection limited to the area caudal to the intercostobrachial nerve might be adequate. The present study, therefore, aimed to compare clinical outcomes in patients with N0 breast cancer who underwent breast cancer surgery (mastectomy or breast-conserving surgery) and partial or conventional axillary lymph node dissection.
No significant differences in the 5-year overall or disease-free survival rates between the partial dissection group and the conventional dissection group were observed in the present study. The median observation period was, however, shorter in the partial dissection group than in the conventional dissection group. These data suggest that the prognosis following partial dissection was adequate. Five-year survival rates were consistent with those reported in other trials comparing patients who underwent axillary dissection with those who did not.6,7,10,11,21
In a randomized trial involving women with clinically negative axillary nodes, postoperative axillary node recurrence occurred in 15% of patients who did not undergo axillary dissection, requiring them to undergo a secondary node dissection.
6
There were only six cases (0.6%) of postoperative axillary node recurrence in the partial dissection group included in the present study. This was similar to the results of another study that reported a recurrence rate of 0.9% (four of 425 cases) in patients with microscopic sentinel node metastasis who underwent SNB only.
20
Meta-analyses have shown that the rates of axillary recurrence in patients who were sentinel lymph node-negative (48 reports) or sentinel lymph node-positive (six reports) treated without axillary lymph node dissection were comparable, at 0.3% and 0.5%, respectively.22,23 The degree of interruption of the lymphatic pathway from the breast to the axilla differs between patients who are treated with no axillary dissection, partial dissection or SNB; SNB causes the most interruption. Lymphatic drainage to any remaining axillary metastatic nodes is prevented by disruption of the lymphatic pathway. This inhibits postoperative growth of the nodes and increases the likelihood of metastases being missed (Fig. 3). Disruption of the lymphatic pathway also results in postoperative lymphoedema and seroma in some patients who undergo SNB.13–15 In partial dissection, tissues on the cranial side of the intercostobrachial nerve are left intact and the lymphatic vessel located alongside the axillary vein is not damaged. Postoperative lymphatic leakage is also prevented by ablation of the axillary tissues. As a result, the patients in the present study who underwent partial dissection did not experience postoperative arm lymphoedema. In contrast to some previously published reports, subcutaneous accumulation of lymphatic fluid in the axilla was markedly reduced following partial dissection in the present study.24,25 The prevention of lymphatic fluid leakage following partial dissection minimizes breast deformation and results in cosmetic improvements in cases of breast-conserving surgery. Furthermore, partial dissection gives an indication of the number of metastatic lymph nodes, which cannot be obtained by SNB.
Schematic diagram showing the theoretical mechanism by which growth of axillary lymph node metastases is reduced following partial axillary lymph node dissection or sentinel node biopsy. Interruption of the flow of lymphatic fluid into the metastatic axillary lymph nodes reduces the growth of metastases
This present study had some limitations: first, it was a retrospective observational study comparing the study group with a historical control group of patients who had undergone conventional axillary node dissection, which is no longer the current standard of care; secondly, differences in follow-up times between the two surgical groups limited the ability to compare outcomes. A prospective randomized trial comparing SNB with partial axillary dissection would provide further information to clarify any differences in outcomes between the two procedures.
Overall, the results from the present study suggest that partial dissection is associated with similar survival rates to conventional axillary dissection, but with a shorter duration of surgery, and less intraoperative blood loss and postoperative lymphatic drainage. Postoperative node recurrence after partial dissection was comparable with previously published results for node recurrence after SNB. 20 There was no evidence, however, of postoperative arm lymphoedema following partial dissection as is observed after SNB, and partial dissection has the added advantage of giving an indication of the number of metastatic nodes. Further research is required to determine the optimal extent of axillary dissection in patients with N0 breast cancer, particularly in terms of intra- and postoperative outcomes.
In conclusion, data from the present study suggest that partial axillary dissection in patients with N0 breast cancer results in similar survival rates and reduced complication rates compared with conventional dissection. Partial dissection also compares favourably with the outcomes of SNB. The authors therefore recommend partial lower axillary lymph node dissection, limited to the area caudal to the intercostobrachial nerve, in patients with N0 breast cancer.
Footnotes
Conflicts of interest: The authors had no conflicts of interest to declare in relation to this article.
