Abstract
OBJECTIVES:
To investigate the prevalence of detrusor after-contraction (DA-C) in children with posturination dribbling, and compare the outcomes of pharmacological treatment and pelvic floor biofeedback training.
Methods:
Children with posturination dribbling underwent urodynamic studies. Patients with DA-C were randomly allocated to one of two groups: pelvic floor biofeedback training or 1 mg tolterodine, orally, twice daily. Treatment was continued for 12 weeks.
Results:
The study included 45 children. DA-C was present in 39 patients (86.6%), 30 (76.9%) of whom also exhibited detrusor overactivity. Pelvic floor biofeedback training resulted in a significantly better response than tolterodine, in terms of reduction in the number of posturination dribbling events in the month after completion of treatment.
Conclusions:
DA-C is closely associated with posturination dribbling in children. Pelvic floor biofeedback training should be considered the initial treatment option in these patients.
Introduction
Posturination dribbling in children is problematic for patients and their families. The exact cause is unknown, but it may be due to detrusor after-contraction (DA-C). 1 The definition, prevalence and significance of DA-C are all unclear, however. 2 DA-C is usually described as a sudden increase in detrusor pressure after the cessation of voiding detrusor contraction, in the absence of urinary flow. 1 The aim of the present study was to investigate the prevalence of DA-C in children with posturination dribbling. In addition, the short-term outcomes of two treatment regimens (pelvic floor biofeedback training and pharmacological therapy with tolterodine) were evaluated and compared.
Patients and methods
Study Population
Children with posturination dribbling who attended the Department of Urology, Xiangya Hospital, Central South University, Changsha, China, between November 2008 and December 2010, were recruited to the study. Inclusion criteria were: (i) normal urinary tract; (ii) normal urinalysis; (iii) normal renal function; (iv) ≥ 5 episodes of postmicturition dribbling in the month prior to enrolment. Patients with overt or suspected neurological conditions, any other urological problem, urinary tract infection, constipation, vaginal voiding and those receiving any medical treatment were excluded.
The study was approved by the Institutional Review Board of Central South University, and the parents of all participants provided written informed consent prior to enrolment.
Clinical Evaluation
Children were interviewed using a semistructured, open-ended format to allow them ample opportunity to characterize their experiences (including personal histories and detailed symptoms). Residual urine volume was measured after voluntary urination using a catheter with a syringe attached. Urodynamic studies were performed according to published guidelines (Aquarius TT; Laborie, Mississauga, Ontario, Canada).3,4 Bladder compliance, detrusor overactivity and urinary flow pattern were recorded. Low bladder compliance was defined as a bladder compliance of < 20 ml/cmH2O. 4 DA-C was defined as a contraction of ≥ 15 cmH2O after cessation of the voiding contraction. Any urine flow accompanying the DA-C was noted. An electromyelogram (EMG) of the external anal sphincter was performed using an anal electrode (PRB055; Laborie).
Treatment
Patients diagnosed with DA-C were divided into two treatment groups according to a computer-generated random-number scheme: pelvic floor biofeedback training or tolterodine (1 mg, orally, twice daily). Both treatments were carried out for 12 weeks.
Biofeedback training was administered via a system that allowed simultaneous recording of urine flow, abdominal pressure and anal EMG (Urostym; Laborie), and was performed as described. 5 An anal electrode was used to indicate changes in EMG and a balloon catheter was placed in the rectum to measure abdominal pressure. Patients were taught to perceive relaxation and contraction of the anal sphincter, and instructed to contract while simultaneously maintaining stable abdominal pressure. Once the patient understood this procedure they chose the optimal position for relaxation of the pelvic floor muscles. They were then instructed to urinate when sitting with the thighs spread (to relax the perineum), while leaning forward slightly with a straight back. Each training session was 20 – 30 min, and was repeated two or three times per week.
Adverse effects of both regimens were noted. A physician (X.Y. Z.), who was blinded to the treatment allocation, evaluated the outcome 1 month after the completion of treatment. The number of posturination dribbling events in the month immediately following treatment was recorded, with 0 events defined as complete cure, 1 event as ‘significant' improvement, 2 – 4 events as partial improvement and ≥ 5 events as no response.
Statistical Analyses
Data were presented as n (%). Comparisons between patients with or without DA-C were made using Fisher's exact test. Ridit analysis was used for between-treatment comparisons. Data were analysed using SPSS® software, version 11.0 (SPSS Inc., Chicago, IL, USA) for Windows®. A P-value < 0.05 was considered to be statistically significant.
Results
The study included 45 children with posturination dribbling (31 females/14 males; median age 11 years, range 8 – 14 years). Table 1 presents baseline demographic and clinical characteristics of the patients, stratified according to the presence or absence of DA-C. Detrusor overactivity was significantly more prevalent in patients with DA-C than in those without DA-C (P < 0.01; Table 1). There were no other between-group differences in demographic or clinical characteristics. The urodynamic study findings of a 12-year-old boy with DA-C are shown in Fig. 1. DA-C was diagnosed in 39/45 patients (86.6%), 38 of whom exhibited posturination dribbling that was visible to the investigator. Urine flow during dribbling was detected by the flow meter in only eight of these cases. None of the six children without DA-C exhibited posturination dribbling during urodynamic studies.
Representative urodynamic study of bladder voiding in a 12-year-old boy with posturination dribbling. The amplitudes of voiding contraction and detrusor after-contraction (DA-C) were 95 and 35 cmH2O, respectively. A small urine flow produced by DA-C was observed in the urine flow curve (Qura). Residual urine volume was 0 ml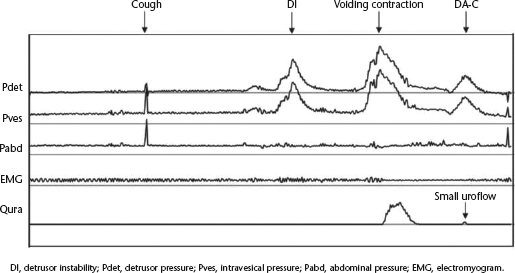
Baseline demographic and clinical characteristics of children with posturination dribbling, stratified according to the presence or absence of detrusor after-contraction (DA-C)
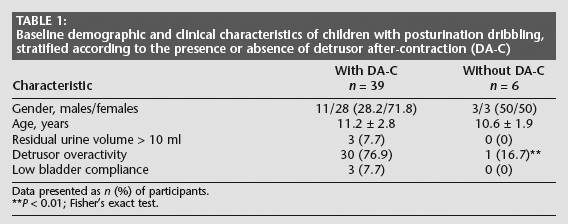
Data presented as n (%) of participants.
P < 0.01; Fisher's exact test.
Demographic and treatment outcome data for the patients with DA-C are shown in Table 2. None of the patients in the biofeedback training group experienced any discomfort, but one child discontinued treatment due to difficulty in comprehending the procedure. In the tolterodine group, one child complained of thirst and two discontinued treatment due to nausea and vomiting. All three patients who discontinued treatment were included in the final evaluation, in order to comply with intent-to-treat analysis, and their symptoms were found to be unchanged (no response). Both treatment regimens resulted in symptom improvement, but the response to biofeedback training was significantly better than the response to tolterodine (P = 0.012; Table 2).
Demographic characteristics and treatment outcomes of children with posturination dribbling and detrusor after-contraction (DA-C) receiving either pelvic floor biofeedback training or tolterodine a treatment for 12 weeks

Data presented as n (%) of participants or mean ± SD.
1 mg tolterodine, orally, twice daily.
Postmicturition dribbling events in the month immediately following completion of treatment: 0, complete cure; 1, significant improvement; 2 – 4, partial improvement; ≥ 5, no response.
P = 0.012, response to biofeedback training vs. tolterodine; Ridit analysis.
Discussion
Detrusor after-contraction is present in 0.5% of paediatric urodynamic studies, 6 but the prevalence, significance and optimum treatment remain unclear. 2 The reported prevalence of DA-C varies widely, possibly due to between-study differences in definitions and populations.6 – 9 There is no standard definition of DA-C, with some studies using fixed or relative values7 – 9 and others setting no limits. 6 The present study defined DA-C as a contraction of ≥ 15 cmH2O after the voiding contraction had ended. Using this definition, 86.6% of children with posturination dribbling were found to have DA-C in the present study, suggesting a close relationship between dribbling and DA-C.
The significance of DA-C is unclear, with some studies indicating no functional significance or diagnostic value.7,8 It has been suggested that DA-C may be an artefact of catheter insertion in urodynamic studies. 2 Others have found evidence that DA-C is an intrinsic increase in detrusor pressure. 8 The small urine flow following DA-C observed in some children in the present study supports this finding, and reflects the symptom of posturination dribbling during daily life. In most children in the present study, the dribbling of a few drops of urine was below the sensitivity of the urine flow meter. The six children without DA-C who did not exhibit dribbling during the urodynamic study nevertheless experienced dribbling in daily life, and it is possible that DA-C is an irregular occurrence in these children.
Research has suggested a correlation between detrusor overactivity and DA-C, 8 but there is limited pathophysiological evidence for this relationship. In the present study, 30/39 (76.9%) of patients with DA-C but none of the patients without DA-C exhibited detrusor overactivity. Detrusor overactivity and DA-C appear to be closely correlated, but further evidence is required to determine whether DA-C is a separate clinical entity. A study in neurologically abnormal adults and children suggested that DA-C was an additional contraction interrupting an incomplete detrusor contraction. 9 It is not possible to extrapolate these findings to neurologically intact patients, however.
To our knowledge, there have been no studies regarding treatment of DA-C. Posturination dribbling in children is not a malignant condition but does affect health-related quality of life, and deserves thorough evaluation and suitable intervention. DA-C is more common in children than in adults,7,8 and may be caused by delays in maturation of the nervous system.10,11 It is possible that DA-C in children is due to the insufficient development of bladder control. Anticholinergic drugs and behavioural modification techniques have been widely used for treating functional voiding disorders in children.12,13 The present study used tolterodine rather than oxybutynin because of its favourable side-effect profile in children.14,15 Although all children responded to tolterodine, adverse effects (thirst, nausea and vomiting) occurred in three participants, two of whom discontinued treatment.
Cognitive pelvic floor training with biofeedback is the first-choice treatment for most cases of dysfunctional voiding in neurologically normal children, after failure of simple conservative measures. 16 The cognitive elements in pelvic floor training assist in the development of bladder control. Biofeedback training had a better short-term outcome than tolterodine, in the present study. Difficulties in comprehending the treatment protocol can cause problems in some children, however, and one child in the present study discontinued the programme because they could not follow the procedure.
The present study has several limitations. Urodynamic studies were not performed after treatment completion, and ethical considerations meant that it was not possible to include a control group of children without posturination dribbling. In addition, the study included a small number of patients and a short-term follow-up period. Further longer-term studies, with larger patient cohorts, are therefore required.
In conclusion, DA-C is closely associated with posturination dribbling in children, and pelvic floor biofeedback training should be considered the initial treatment option in these patients.
Footnotes
Conflicts of interest: The authors had no conflicts of interest to declare in relation to this article.
