Abstract
Isolated syphilitic cervical lymphaden -opathy (SCL) is a rare presentation of syphilis. Two patients with isolated SCL are presented here with a review of the literature. The first patient was a 72-year-old man with a mass (diameter 5 cm) in the right neck region for 26 days. Serological tests, imaging studies and pathological examination of the mass after surgical excision confirmed the diagnosis of isolated SCL. The second patient was a 48-year-old man with a mass (diameter 4 cm) in the right neck region for 1 month. The diagnosis of isolated SCL was made on the basis of serological tests, cervical ultrasound and pathological examination of the mass after surgical excision. Complete excision resulted in a satisfactory outcome in both patients. Isolated neck masses without associated clinical manifestations or adverse personal history are a diagnostic challenge, and SCL is easily overlooked in the differential diagnosis. Unusual masses should always remind clinicians of this infectious disease and a comprehensive diagnostic strategy is recommended. Nonroutine syphilitic serological tests should be performed in patients suspected of having SCL, and the histopathological and immunohistochemical characteristics may help to confirm the diagnosis.
Introduction
Since it was first clearly described in the 15th century, syphilis has been a major public health problem. 1 After a massive syphilis epidemic in the first half of the 20th century, syphilis was almost eliminated in China 50 years ago. However, because of substantial changes in society such as economic and social reforms, the incidence of sexually transmitted diseases is once again increasing in China. At present, syphilis is the most commonly reported communicable disease in Shanghai, China's largest city.2,3
Syphilis is caused by the spirochaete bacterium Treponema pallidum, which is transmitted mostly by sexual intercourse but sometimes from mother to child. It is known as a ‘great imitator', with numerous and complex clinical manifestations and a waxing and waning disease course.1,4
The natural history of syphilis is artificially divided into a series of overlapping stages to facilitate therapeutic decision making and medical intervention. Primary syphilis is defined by the presence of a chancre at the site of inoculation, which typically develops about 21 days after exposure and is often accompanied by regional lymphadenopathy. Secondary syphilis presents with haematogenous dissemination of the spirochaetes, causing more widespread clinical manifestations that especially involve epithelial surfaces, including rash, alopecia, condylomata lata and mucous patches. Systemic symptoms include fever, malaise and generalized lymphadenopathy. The signs of primary and secondary syphilis may resolve spontaneously without treatment. Patients then enter the latent stage of infection, which is subdivided into early and late stages. The latent stage is asymptomatic and is characterized by seroreactivity without clinical evidence of the disease. If left untreated for several years after infection, 30% of patients will eventually develop tertiary syphilis, which includes benign gummas, cardiovascular disease and neurosyphilis.1,4,5
The genital area is the most common site of chancres, but head and neck manifestations may be seen at any stage of syphilis. The diagnosis of syphilis may surprise a patient who initially visits an otolaryngologist or stomatologist, especially when only the cervical lymph nodes are involved. 6 Here, two patients with isolated syphilitic cervical lymphadenopathy (SCL) are presented and the associated literature is reviewed.
Case reports
Publication of these cases was approved by the Committee on Ethics of Biomedicine Research, Second Military Medical University, Shanghai, China, and written informed consent was obtained from both patients.
Patient 1
A 72-year-old man presented to Changzheng Hospital, Shanghai, China, in November 2011 with a nontender mass in the right neck that had been progressively enlarging for 26 days. He had a 10-year history of hypertension and denied recent sexual activity or any other adverse personal history.
On physical examination, the patient had an egg-like mass 5 cm in diameter in the mid-jugular chain area. The mass was nontender, indurated and clearly bounded, without adhesions, nodules or alteration of skin colour. No other lymphadenopathy was found. No lesions were seen in the genital area or the oropharynx.
Computed tomography (CT) and magnetic resonance imaging (MRI) scans of the neck showed a right cervical mass medial to the sternocleidomastoid muscle and multiple enlarged surrounding small lymph nodes (Fig. 1). The MRI findings were suggestive of a metastatic tumour in the cervical lymph nodes. The toluidine red unheated serum test (TRUST) was negative, while the T. pallidum particle agglutination (TPPA) test was positive. Serological testing for HIV was negative. SCL was considered to be the most likely disease in the differential diagnosis.
(A) Axial and (B) coronal magnetic resonance imaging scans in patient 1 with syphilitic cervical lymphadenopathy, showing right neck mass with a diameter of 5 cm (white arrows), with several enlarged surrounding lymph nodes
The mass was excised surgically. Multiple enlarged small lymph nodes were seen in the right neck at operation. Intraoperative pathological examination of a frozen section showed lymph node necrosis with cellular proliferation.
Sections of the excised neck mass were embedded in paraffin and stained with haematoxylin and eosin. Pathological examination under light microscopy revealed marked follicular hyperplasia, obviously thickened lymph node capsules with fibrosis and hyalinosis, copious plasma cell and lymphocytic infiltration in the paracortical area and peripheral tissues of the capsule, a large area of coagulative necrosis and an epithelioid cell reaction.
Immunohistochemical study of the lymph nodes showed the following B-cell phenotypes: CD19+, CD20+, CD21+, CD79a+, Bcl-2+, Bcl-6+, CD5+, CD2+, MUM-1+ and CD3+, with a Ki-67 labelling index of 30%. These results were consistent with reactive follicular hyperplasia. B-cell lymphoma-2 (Bcl-2) expression was only slightly positive and was not confined to the germinal centre, supporting the exclusion of follicular lymphoma.
Patient 2
A 48-year-old man was admitted to Changzheng Hospital, Shanghai, China, in October 2011 with a history of a nontender mass in the right neck for a month. He had no specific past medical history and denied recent sexual activity.
Physical examination revealed a mass 4 cm in diameter in the right mid-jugular chain area. The mass was nontender, indurated, smooth and clearly bounded, without adhesions, nodules or alteration of skin colour. No other lymphadenopathy was identified in the inguinal or submaxillary groups. No lesions were seen in the genital area or oropharynx.
The patient had undergone an ultrasound examination of the neck 2 weeks before admission, which showed enlargement of several cervical lymph nodes posterior to the right sternocleidomastoid muscle, leading to a suspected diagnosis of metastatic carcinoma. The TRUST and TPPA tests were both positive and HIV serology was negative. SCL was considered to be the most probable diagnosis.
The mass was excised surgically. Multiple enlarged lymph nodes were seen in the right neck at operation. The largest of these was a fused lymph node 4 cm in diameter adhering tightly to the internal jugular vein, the sternocleidomastoid muscle and the submandibular gland. Intraoperative pathological examination of a frozen section showed lymphoepithelial lesions.
Sections of the excised neck mass were embedded in paraffin and stained with haematoxylin and eosin. Pathological examination under light microscopy revealed significant follicular hyperplasia, obviously thickened lymph node capsules with fibrosis, massive plasma cell and lymphocyte infiltration in the paracortical area and peripheral tissues of the capsule, and the presence of a noncaseating granuloma (Fig. 2).
Pathological findings revealed by haematoxylin and eosin staining in patient 2 with syphilitic cervical lymphadenopathy: (A) thickened or fibrotic lymph node capsules with infiltration of plasma cells in the capsule and the pericapsular area; (B) noncaseating necrosis in the lymph node; (C) numerous plasma cells infiltrating the paracortical zone; (D) follicular hyperplasia with a heterogeneous population of lymphoid cells varying from large germinal centre cells to small mature cells; (E) noncaseating granuloma with epithelioid histiocytes and giant cells; (F) vascular changes such as phlebitis and endarteritis with perivascular inflammatory infiltration; (G) thickened capsule with surrounding noncaseating granuloma (scale bars 100 μm)
Immunohistochemical study of the lymph nodes showed the following B-cell phenotypes indicative of follicular hyperplasia: CD19+, CD20+, CD21+, CD79a+, Bcl-2+, Bcl-6+, CD5+, CD2+, MUM-1+ and CD3+, with a Ki-67 labelling index of 5%. Bcl-2 expression was only slightly positive and was not confined to the germinal centre, supporting the exclusion of follicular lymphoma.
Antibiotic Treatment and Follow-Up
Both patients were treated with penicillin for a short period postoperatively and were then discharged. When followed up after 3 months, they were in good health with no recurrence or discomfort.
Discussion
Primary and secondary syphilis almost always present with regional or generalized lymphadenopathy. The inguinal lymph nodes are most commonly involved, usually in association with lesions in the genital area. Hartsock et al. 7 reported 20 cases of syphilitic lymphadenitis, of which 17 had inguinal group involvement. Turner and Wright 8 reported 21 patients with syphilis who presented with lymph node enlargement, all but one of whom had inguinal group involvement.
Syphilitic cervical lymphadenopathy has been reported only sporadically to date. To our knowledge, until the present report only 21 cases of SCL have appeared in the literature since the 1920s.7–21 The clinical features of these and the two present cases are summarized in Table 1. Most cases have involved adults with acquired syphilis (mean age 35 years, range 8 – 72 years), the exception being the earliest reported case, which was a child with congenital syphilis. A definite history of sexual activity was present in nine (39%) out of 23 cases. All 23 patients complained of swelling or enlargement of the cervical lymph nodes, with an isolated neck mass being the solitary manifestation of syphilis in seven patients (Table 2). In 11 patients (48%) there were associated oropharyngeal or otorhinological manifestations (Table 3). Serological tests for syphilis were performed in 16 (70%) of the 23 patients. Interestingly, all of the specific T. pallidum tests performed were positive.
Clinical characteristics of the 21 previously reported cases of syphilitic cervical lymphadenopathy and the two present cases

F, female; M, male; NA, not available; CL, cervical lymphadenopathy; CLN, cervical lymph node; NM, neck mass; +ve, positive; -ve, negative; FTA-ABS, fluorescent treponemal antibody absorption test; RPR, reactive plasma regain test; TPPA, Treponema pallidum particle agglutination test; TRUST, toluidine red unheated serum test; VDRL, Venereal Disease Research Laboratory test; CT, computed tomography; MRI, magnetic resonance imaging.
Isolated cervical lymphadenopathy as the single manifestation of syphilis in previously reported cases and in the two present cases of syphilitic cervical lymphadenopathy

F, female; M, male.
Oropharyngeal and otorhinological manifestations in previously reported cases of syphilitic cervical lymphadenopathy

F, female; M, male.
Pathological data were available in 15 (65%) of the 23 patients (Table 4). Only five (22%) of the case reports included imaging studies of the enlarged mass (three CT scans, one CT scan and MRI scan, and one ultrasound scan). Five patients (22%) underwent surgical excision, while 11 (48%) received only antibiotic therapy; eight of the latter patients had satisfactory outcomes, with either shrinkage of the mass or serological tests becoming negative.
Pathological characteristics of patients in previously reported cases and in the two present cases of syphilitic cervical lymphadenopathy
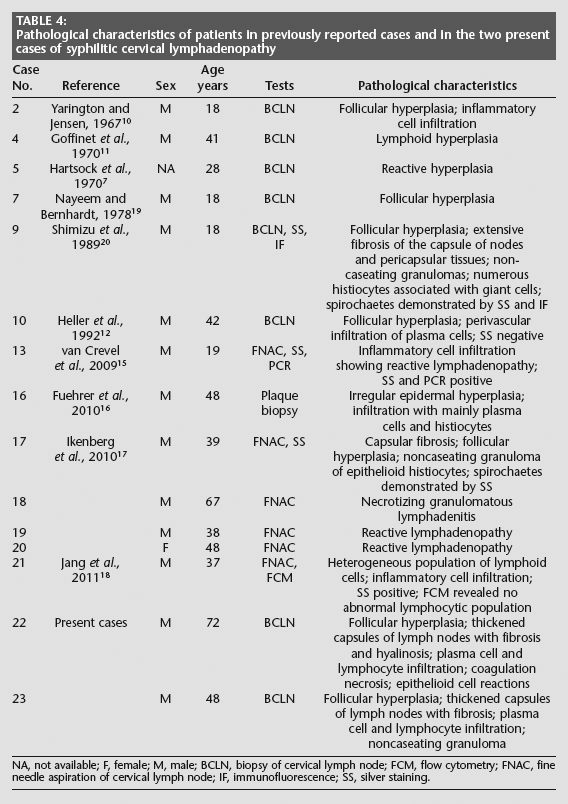
NA, not available; F, female; M, male; BCLN, biopsy of cervical lymph node; FCM, flow cytometry; FNAC, fine needle aspiration of cervical lymph node; IF, immunofluorescence; SS, silver staining.
There are many causes of neck masses; these have been summarized in the mnemonic ‘KITTENS' (K, congenital anomalies; I, infectious/inflammatory; T, trauma; T, toxic; E, endocrine; N, neoplasms; S, systemic diseases). 22 The ‘rule of 80' states that 80% of nonthyroid neck masses in adults are neoplastic, among which 80% are malignant. 23 An asymptomatic cervical mass is the presenting symptom in about 12% of head and neck cancers. 23 The risk of having a malignant neck mass becomes higher with increasing age. 24 Syphilis is a rare cause of neck mass, and is easily overlooked and difficult to identify. Given the age of the two patients presented here (72 and 48 years), their denial of adverse personal histories and the locations of their neck masses, malignancies were initially suspected in both cases. Their masses were mainly located in the mid-jugular chain area (level III, deep lateral cervical nodes), commonly indicating metastasis following well-defined patterns from a primary site in the oral cavity, pharynx or larynx. 24 The differential diagnosis of an infected neck mass includes sialadenitis, cervical abscess and lymphadenitis, with lymphadenitis being the most common cause. The various causes of cervical lymphadenitis include histiocytic necrotizing lymphadenitis (HNL), scrofula, cat scratch disease and mycobacterial infections.22,24 It is, therefore, a great challenge to distinguish SCL from other infections.
Associated symptoms and signs in the head and neck that are commonly seen in SCL include nonhealing ulcer in the oral cavity or oropharynx, persistent sore throat, dysphagia, a change in the voice and recent weight loss (Table 3). 24 T. pallidum can invade and cause infections of mucous membranes or skin. Head and neck manifestations of all stages of syphilis include otosyphilis, rhinitis, pharyngitis, laryngitis and tonsillitis, with the lips being the most common site of initial spirochaete inoculation and chancre formation. 6 Patients may have a higher risk of acquiring T. pallidum via the oropharyngeal pathway after orogenital sex. 12 Chancres in the head and neck can cause regional lymphadenopathy, which may facilitate the diagnosis of syphilis. Head and neck malignancies, however, also commonly present with similar manifestations, including nonhealing ulcers in the oral cavity or oropharynx, persistent sore throat, dysphagia, a change in the voice and recent weight loss, and must be excluded first. 24 Chancres are sometimes absent in syphilis; the two patients reported here both presented with isolated neck swelling without any other associated manifestations or a personal history of sexual activity, thus increasing the difficulty in diagnosis.
Before the advent of CT and MRI, lymphography was used in the diagnosis of syphilitic lymphadenitis, which was frequently misdiagnosed. 25 CT scanning with contrast is currently considered the imaging study of choice in the initial evaluation of a neck mass. It can demonstrate the origin and extent of deep, undefined masses and the enhanced scan can further delineate vascularity or blood flow. MRI scanning provides similar information to CT and is particularly useful for pulsatile masses and masses with a bruit or thrill. In contrast, ultrasonography has limited utility in the evaluation of neck masses in adults.23,24 However, the appearance of syphilitic lymphadenopathy in CT and MRI scans can be nonspecific. The MRI scan of one of the patients presented here (a 72-year-old man) was misinterpreted as showing a metastatic tumour in the cervical lymph nodes, which highlights the need for further exploration before arriving at a diagnosis.
Serological tests can help to provide more diagnostic clues. Tests for T. pallidum fall into two categories: nontreponemal and treponemal. Nontreponemal tests include the Venereal Disease Research Laboratory slide test, the unheated serum reagin test, the rapid plasma reagin test and the TRUST. They are relatively nonspecific and can give a positive result in several diseases, and so are used as primary screening tests for syphilis. Positive results need to be confirmed with specific treponemal tests, such as the T. pallidum haemagglutination assay, the TPPA test and the fluorescent treponemal antibody absorption test.1,26 The nontreponemal TRUST was positive in one of the patients presented here, while the treponemal tests were positive in both, establishing the diagnosis of syphilis and suggesting the probability of SCL. Other comprehensive serological tests, including the HIV test and the tuberculosis purified protein derivative test, are helpful in excluding AIDS and scrofula.
Pathological examination is of great value in confirming SCL as it can distinguish between inflammatory or reactive lesions and neoplasms. Syphilitic lymphadenitis was once classified into two types on the basis of histological changes: (i) a nonspecific, subacute, proliferative and exudative inflammatory reaction; (ii) a tuberculoid reaction, which is more closely related to the state of allergy of the individual than to the duration of the infection. 7 Although simple, this classification lacks the detailed information needed for differential diagnosis. On the basis of the reviewed literature10,11,19 and the present cases, the main pathological characteristics of syphilitic lymphaden -opathy include: (i) follicular hyperplasia with a heterogeneous population of lymphoid cells varying from large germinal centre cells to small mature cells; (ii) noncaseating granuloma with epithelioid histiocytes and giant cells; (iii) thickened or fibrotic capsules of lymph nodes with infiltration of plasma cells in the capsule and pericapsular area; (iv) vascular changes such as phlebitis and endarteritis with perivascular inflammatory infiltration; (v) other, less frequently seen features such as suppurative inflammation (Fig. 2).
The histopathological findings of syphilitic lymphadenitis are not always pathognomonic and the results can therefore be misleading. Certain pathological features can resemble other diseases such as follicular lymphoma, leprosis and tuberculous granuloma.8,11 In the present cases, the pathological differential diagnosis of SCL included cervical scrofula, HNL and lymphoma. Necrosis is commonly seen in both scrofula and HNL; however, scrofula always presents with caseating necrosis and positive acid-fast staining, which are absent in SCL. A well-maintained lymph node cortex is commonly seen in HNL, as is definite cell necrosis with abundant karyorrhectic nuclear debris in the paracortex, but infiltration of plasma cells or granulocytes is rare. 27 The plasma cell infiltration seen in SCL and the nuclear debris seen in HNL are of considerable value in the differential diagnosis. Follicular lymphoma always presents with uniform, densely packed follicles, which are frequently arranged back to back and obliterate the nodal architecture; 28 the absence of these features is helpful in excluding this condition.
Hartsock et al. 7 found that syphilitic lymphadenitis shows a considerable degree of inflammation and fibrosis of the capsular and pericapsular tissues. Turner and Wright 8 reported apparent lymphocyte depletion and histiocytic infiltration in the paracortical zones of lymph nodes. Lymphocyte depletion is associated with impairment of cell-mediated immunity, which may contribute to the persistence of spirochaetes within the tissues; however, the degree of paracortical lymphocyte depletion is unrelated to the duration or stage of syphilis. 8 The histopathological findings in the cases presented here were consistent with these reported features and further confirmed the especially thickened lymph node capsule as a typical pathological change in syphilitic lymphadenitis.
Immunohistochemistry provides clear evidence to support the exclusion of lymphoma and to establish the diagnosis when there is morphological uncertainty. In the patients presented here, the CD19+, CD20+ and CD79a+ phenotypes strongly indicated follicular hyperplasia. Large areas of noncaseating necrosis may suggest natural killer/T-cell lymphoma but this can be excluded by negative test results for perforin, granzyme-B and T-cell intracellular antigen. Follicular lymphoma is another consideration when there is marked follicular hyperplasia. CD21 and CD23 are normally expressed in follicular dendritic cells and are useful in demonstrating the follicular dendritic network. In reactive follicles, a dense follicular dendritic cell meshwork with polarization is seen, whereas follicular lymphoma presents with an expanded follicular dendritic cell meshwork. The absence of strongly positive Bcl-2 cells and low Ki-67 supports the exclusion of follicular lymphoma. Because of the low specificity of many of the currently available paraffin-reactive antibodies, 29 it is important to interpret the immunohistochemical results in the context of the morphological findings.
Treponema pallidum may be visualized in specimens using dark-field microscopy, immunofluorescence microscopy or conventional silver staining.8,15,17,26 Although false-negatives have been reported, 30 direct observations of spirochaetes can point to the correct diagnosis. Using silver staining, spirochaetes are most evident in the paracortical areas, especially in and around the walls of postcapillary venules; 8 however, silver staining was negative in both the patients presented here.
Inflammatory lymphadenopathy is typically self-limiting and resolves spontaneously over a period of weeks; 24 however, 15 – 40% of untreated patients with syphilis develop late and potentially life-threatening cardiovascular or neurological complications, 15 so active treatment for SCL is recommended. Approximately 35% (eight out of 23) of the reported cases were treated solely with penicillin and other antibiotics with satisfactory outcomes (either shrinkage of the mass or decreased titres in serological tests). Although surgical excision was conducted in five cases, including the two presented here, we suggest that antibiotic therapy should be used as the first step in the treatment of SCL of medium size, with surgical excision being performed if antibiotics fail. Rather than surgical biopsy, fine-needle aspiration may be sufficient for the diagnosis and may also be useful for monitoring therapy. Optimum therapies need to be further investigated, however, using evidence-based clinical studies.
In summary, the present report has described two rare cases of isolated SCL with no associated manifestations and no specific adverse personal history. Neck mass, with its various differential diagnoses, is an uncommon presentation of syphilis. In addition to specific nonroutine serological tests, in particular treponemal tests, the histopathological and immunohistochemical characteristics of SCL may help to establish the final diagnosis. A comprehensive workup (Fig. 3), including clinical manifestations, imaging studies, serological tests and pathological examinations, is recommended for the diagnosis of SCL. Once the diagnosis has been established, empirical antibiotic treatment should be administered before surgical excision.
Flowchart of the management of suspected syphilitic cervical lymphadenopathy (SCL) (CT, computed tomography; MRI, magnetic resonance imaging; PE, physical examination, FNA, fine-needle aspiration)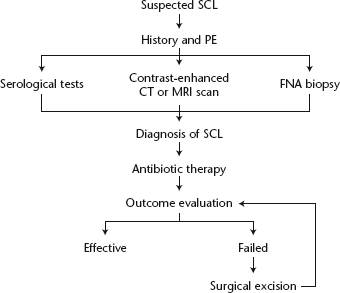
Footnotes
Acknowledgements
We thank Dr Yi Xu and Dr Wei-Jian Zhu for their help with the immunohistochemical studies.
The authors had no conflicts of interest to declare in relation to this article.
