Abstract
Objective:
To compare the feasibility and safety of thoracoscopic thymectomy with conventional sternotomy thymectomy for thymoma without myasthenia gravis.
Methods:
Data from 70 patients diagnosed with thymoma, who underwent thoracoscopic thymectomy (n = 25, Group T) or sternotomy thymectomy (n = 45, Group S) between March 2002 and March 2008, were retrospectively evaluated.
Results:
Mean follow-up durations were 78.0 ± 21.9 months and 70.0 ± 23.6 months in Groups T and S, respectively. No deaths occurred in Group T; seven deaths occurred in Group S, all > 1 month post follow-up. Durations of chest intubation and hospitalization were significantly shorter in Group T than in Group S. No significant between-group difference in the incidence of operative complications was observed. Tumour recurrence-free rates at 5 and 7 years postsurgery were 96% (both years) in Group T and 95% (both years) in Group S.
Conclusions:
Long-term follow-up indicates that thoracoscopic thymectomy for thymoma without myasthenia gravis is effective and is well tolerated, and associated with low rates of operative complications and recurrence.
Introduction
Thymoma is a common primary tumour of the anterior mediastinum that accounts for 20 – 30% of all mediastinal neoplasms.1,2 Management of thymoma usually consists of surgery involving thymectomy via median sternotomy. 3 Thoracoscopic surgery is a form of minimally invasive surgery that is known to be effective for the management of patients with mediastinal disease.3–8 Thoracoscopic thymectomy was introduced as an alternative to conventional thymectomy in patients with myasthenia gravis, in whom it has been demonstrated to be effective, with a good safety profile.9–11 The safety and feasibility of this procedure for thymoma without myasthenia gravis has not, however, been previously studied.
The present retrospective study evaluated the feasibility and safety of thoracoscopic thymectomy compared with sternotomy thymectomy in patients with thymoma without myasthenia gravis, who had been prospectively registered in the Asan Medical Centre database, Seoul, South Korea.
Patients and methods
Study Population
All patients diagnosed with thymoma who underwent thoracoscopic or sternotomy thymectomy between March 2002 and March 2008, and were registered on the Asan Medical Centre database, Seoul, South Korea, were included in this study. This registry prospectively includes details of patients' baseline characteristics, preoperative computed tomography (CT) scan results, surgical procedures and perioperative complications. Exclusion criteria in this study included: previous treatment with neoadjuvant chemotherapy; diagnosis of myasthenia gravis or type B3 or C thymomas, according to the World Health Organization (WHO) classification; 12 thymectomy by open thoracotomy; pleural metastasis. Patients who underwent thoracoscopic surgery were eligible for inclusion if, on CT scan, tumours were located in the anterior mediastinum and under the innominate vein, were < 5 cm in diameter at the widest point, a and had a distinctive fat plane between the tumour and surrounding tissue. Patients were not excluded from the study if there was evidence of tumour invasion into the lung and/or pericardium, because resection of such tumours is not difficult.
Retrospective review and collation of the data was approved by the Institutional Review Board of the Asan Medical Centre (No: 2008-0558), which waived the need for informed patient consent.
Tumour size < 5cm was not an absolute inclusion criterion. Larger tumours could be included if preoperative discussions between coauthors concluded that thorascopic removal would be safe.
Histological and Pathological Staging
Using the WHO classification, thymomas were classified into one of five subtypes (A, AB, B1, B2 or B3). 12 Type A thymomas are composed of neoplastic spindle-shaped epithelial cells without atypia or lymphocytes; type AB thymomas are similar to type A but with a foci of lymphocytes. Type B thymomas consist of plump epithelioid cells and are divided into three further subtypes, defined by an increasing proportion of epithelial cells and increasing atypia: B1 thymomas resemble normal thymic cortex with areas similar to thymic medulla; B2 thymomas have scattered neoplastic epithelial cells with vesicular nuclei; B3 thymomas are composed predominantly of epithelial cells exhibiting mild atypia and resemble well-differentiated thymic carcinoma. Thymic carcinomas are designated as type C thymomas.
Pathological staging of tumours was determined on the basis of the Masaoka system. 13 Stage I thymomas are macroscopically encapsulated tumours with no microscopic capsular invasion; stage II thymomas show macroscopic invasion into surrounding fatty tissue or mediastinal pleura, or microscopic invasion into the capsule; stage III thymomas exhibit macroscopic invasion into neighbouring organs such as the pericardium, great vessels or lung; stage IVa thymomas exhibit pleural or pericardial metastasis; stage IVb thymomas are characterized by lympho -genous or haematogenous metastases.
Surgical Techniques
Thoracoscopic thymectomy was performed using a three-port endoscopic technique by the same surgical team. After induction of general anaesthesia using propofol (2 mg/kg, administered intravenously) with one-lung ventilation, the patient was placed in either the left or right semilateral decubitus position. The semilateral position was preferred due to the ease of converting to median sternotomy from this position, if necessary (in cases such as massive bleeding or severe adhesions, for example). A thoracoscopic port was placed at the mid axillary line through the fifth intercostal space; an instrument port was positioned at the anterior axillary line through the third or fourth intercostal space; a working port was placed at the anterior axillary line through the fifth intercostal space. The thoracoscopic and instrument ports were approximately 1 cm in length and the mean length of the anterior working port was 3.19 cm. Tumour dissection started from the pericardial area towards the base of the neck. Residual normal thymus tissue was removed, together with the tumour. A pathologist assessed the dissected tumour postoperatively. In patients undergoing sternotomy, standard surgical procedures 14 were used.
Statistical Analyses
Data were presented as frequencies or means ± SD. Comparisons of patient characteristics between the two surgical groups were made using the Mann–Whitney U-test for continuous variables and Pearson's χ2-test for categorical variables. Mortality and recurrence of thymoma over time were plotted using Kaplan–Meier curves. All statistical analyses were performed using SPSS® statistical software, version 18.0 (Korean version; SPSS Inc. Chicago, IL, USA) for Windows®. A P-value of < 0.05 was considered to be statistically significant.
Results
A total of 141 patients were diagnosed with thymoma and underwent thymectomy, 68 of whom were excluded for the following reasons: myasthenia gravis (n = 36); treatment with neoadjuvant chemotherapy (n = 17), classification of thymoma as WHO subtype B3 (n = 5); thymectomy by open thoracotomy (n = 10). Five patients who underwent thorascopic thymectomy failed to meet the inclusion criteria fully because their tumours were > 5 cm in diameter at the widest point along their major axes. However, these tumours were < 5 cm in diameter along their minor axes and the coauthors decided they could easily be removed, therefore they were included in the further analysis.
The patient cohort eligible for retrospective review consisted of 28 patients who underwent thoracoscopic thymectomy (Group T) and 45 patients who underwent thymectomy via sternotomy (Group S). Three patients in Group T were excluded from further analysis (two underwent sternotomy conversion and one patient had pleural metastasis). The two sternotomy conversions were due to severe pleural adhesions, which could not be dissected using thoracoscopic instruments. The study groups were well matched with respect to gender, mean age, surgical positioning and duration and follow-up duration (Table 1).
Baseline patient characteristics and peri- and postoperative outcomes in patients with thymoma without myasthenia gravis, who underwent thoracoscopic (Group T) or sternotomy (Group S) thymectomy

Data presented as mean ± SD (range) or n patients.
P-values determined using the Mann–Whitney U-test for continuous variables and Pearson's χ2-test for categorical variables.
Both patients had thymoma of WHO subtype B1.
Two patients with chylothorax and one with wound dehiscence.
NA, not applicable; WHO, World Health Organization; NS, not statistically significant (P 0.05).
Duration of chest intubation and length of hospital stay were significantly shorter in patients in Group T compared with Group S (P < 0.001; Table 1). Fewer patients in Group T were treated with postoperative radiotherapy compared with those in Group S, but this difference was not significantly different (Table 1). Significantly more patients in Group S died during follow up (all > 1 month postsurgery: mean 51.7 ± 15.8 months [range 5.5 – 78.6 months]), compared with no deaths in Group T (P = 0.033; Table 1). Causes of death were cardiac in two cases and pneumonia, bowel perforation, cerebrovascular accident, asthma attack and disease progression (one case each).
Mean tumour size, measured preoperatively by a CT scan and postoperatively by a pathologist, was significantly smaller in Group T group than in Group S (P < 0.001; Table 2). Preoperative CT scans also showed evidence of local invasion in no patients in Group T compared with four patients in Group S (P = 0.044; Table 2). Three of these patients had suspected mediastinal fat invasion; one had invasion abutting the great vessel. Three patients in Group S experienced operative complications compared with no patients in Group T (Table 1), but this difference did not reach statistical significance.
Preoperative computed tomography (CT) findings in patients with thymoma without myasthenia gravis, who underwent thoracoscopic (Group T) or sternotomy (Group S) thymectomy

Data presented as mean ± SD or n patients.
P-values determined using the Mann–Whitney U-test for continuous variables and Pearson's χ2-test for categorical variables.
NS, not statistically significant (P 0.05).
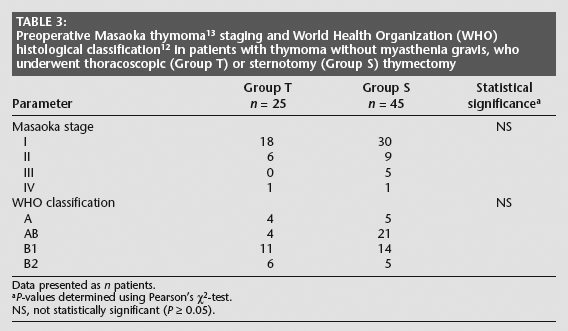
There were no significant between-group differences in Masaoka stage or WHO classification of thymoma (Table 3).12,13 None of the patients in Group T had Masaoka stage III disease compared with five patients in Group S, including one patient each with lung involvement, parietal pleural involvement, direct invasion of the lymph nodes, pericardial involvement, and pericardial and lung involvement. One patient in each group had stage IV disease, consisting of distant lymph node metastases. Two patients in Group S experienced tumour recurrence, both in the pleura.
Data presented as n patients.
P-values determined using Pearson's χ2-test.
NS, not statistically significant (P 0.05).
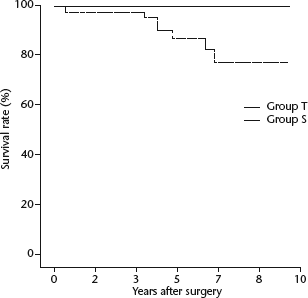
Tumour recurrence-free rates were not significantly different between groups: 2-, 5-and 7-year recurrence-free rates were 100%, 96% and 96% respectively in Group T, and 98%, 95% and 95% respectively in Group S (Fig. 1). Patients in Group T experienced improved survival rates compared with patients in Group S (P = 0.033); the 2-, 5- and 7-year survival rates in Group T and Group S were 100%, 100% and 100%, and 98%, 87% and 77%, respectively (Fig. 2).
Kaplan–Meier curves showing tumour recurrence-free rates in patients without myasthenia gravis who underwent thoracoscopic (Group T) or sternotomy (Group S) thymectomy. There were no significant between-group differences in recurrence-free rates (log-rank test) Kaplan–Meier curves showing survival rate in patients without myasthenia gravis who underwent thoracoscopic (Group T) or sternotomy (Group S) thymectomy. The survival rate was significantly higher in Group T compared with Group S (log-rank test)
Discussion
The present study demonstrated that, compared with sternotomy thymectomy, thoracoscopic thymectomy for thymoma without myasthenia gravis was associated with similar risks of operative complications and tumour recurrence, but lower mortality rates during follow-up. These findings suggested that the safety of thoracoscopic thymectomy was comparable with conventional open thymectomy. Similar to other published studies, the present study showed that patients undergoing thoracoscopic thymectomy experienced a shorter duration of chest intubation and hospitalization.15,16 Patients were excluded from participation in the present study if they had myasthenia gravis or thymomas that either resembled (WHO type 3B) or were (WHO type C) well-differentiated thymic carcinomas, any of which could influence survival and confound the results.17,18 Myasthenia gravis is not a prognostic factor for thymoma, but the majority of published studies suggest (either through trends or statistically significant findings) that it is associated with significantly better survival compared with no myasthenia gravis. 18 Patients with types B3 or C thymoma demonstrate intermediate or worse survival rates than other classification subtypes.19,20
Thymoma is a slow-growing tumour and the average time to recurrence is ∼ 5 years.21,22 Long-term follow-up studies may therefore be necessary to describe accurately the safety, feasibility and efficacy of surgical techniques such as thoracoscopic thymectomy. The present study sought to obtain clinical outcomes over a 3-year period and, as such, patient enrolment was restricted to those who underwent surgery before March 2008.
Thymoma treatment aims to achieve complete resection, which is one of the most important prognostic factors associated with this malignancy.14,21,22 Many surgeons are reluctant to perform thoracoscopic thymectomy because of concerns regarding incomplete resection. This procedure has, however, been shown to be as effective as sternotomy with respect to thymoma recurrence and survival, with follow-up periods of between 1 and 75 months 5 or 33.9 ± 19.7 months. 23 These studies5,23 reported no deaths and one recurrence, which were comparable with our 3-year findings (one recurrence and no deaths in Group T). Furthermore, thoracoscopic thymectomy has considerable advantages for patients, including minimal incision size, less pain, and more rapid recovery compared with standard (sternotomy) techniques.15,16 No significant differences were observed, with respect to mean operative time and incidence of operative complications, between patients in the present study who underwent thoracoscopic or sternotomy thymectomy. Durations of postoperative hospital stay and chest intubation were, however, significantly shorter in Group T. A three-port endoscopic technique was used in Group T, and the size of the thoracoscopic and working ports were small and did not require retraction during surgery. These advantages of thoracoscopy would facilitate better cosmetic outcomes and less pain for patients.
From a safety and efficacy perspective, it is important that patients are screened to ensure that they are suitable for thoracoscopic thymectomy. The type of thymectomy performed on patients in the present study was determined based on CT findings, with tumour location and size being the most important factors indicating that thoracoscopic surgery was feasible. Patients were indicated for thoracoscopic thymectomy if the tumour was located in the anterior mediastinum and under the innominate vein; the thoracoscopic view is poor for tumours located above the innominate vein, making their removal by this method difficult and dangerous. Tumour size in the present study, as determined by preoperative CT scan, was significantly smaller in patients in Group T compared with Group S. To be eligible for inclusion in thoracoscopic surgery, tumours generally had to be < 5 cm in diameter at the widest point. Five patients who underwent thorascopic thymectomy had tumours that were > 5 cm along their major axes, however. These cases were included in the present analysis because the tumours were < 5 cm along their minor axes and could be removed through an anterior working port. Large tumour size is not an absolute contraindication for thoracoscopic thymectomy and is not associated with poor safety findings. 24
In the present study, the incidence of tumour recurrence during follow-up did not differ significantly between the groups, although a significant difference in survival rate (favouring thoracoscopic thymectomy) was observed. It is not possible to conclude that thoracoscopic thymectomy was safer than sternotomy thymectomy, since only one patient in Group S group died from disease progression and patients in Group S appeared to have more severe disease than those in Group T. These results indicated that the safety and efficacy of thoracoscopic thymectomy were comparable with that for conventional (i.e. sternotomy) procedures.
Several limitations were associated with the present study. The analysis was retrospective in nature and patients were not randomized to the different surgical groups. Although the groups were well matched with respect to the majority of preoperative characteristics there was a trend towards less severe tumours (according to Masaoka staging 13 ) in Group T compared with Group S. Furthermore, mass size was smaller in Group T than in Groups S, which may also have influenced the long-term results. A randomized study including more patients would overcome these limitations.
In conclusion, the present study reports on the long-term outcomes of thoracoscopic thymectomy compared with conventional thymectomy, for thymoma without myasthemia gravis. Sternotomy thymectomy is a mainstay of surgical treatment for thymoma, but the results described here show that thoracoscopic thymectomy is associated with several advantages including smaller incisions, reduced length of postoperative hospital stay, no operative complications, low rates of tumour recurrence and longer survival ( 7 years, postoperatively). In general, the long-term outcomes of thoracoscopic thymectomy were comparable with those of sternotomy thymectomy. These findings indicate that thoracoscopic thymectomy is effective and well tolerated, and may represent the best treatment modality for thymoma without myasthenia gravis, in tumours of ∼ 5 cm in diameter.
Footnotes
The authors had no conflicts of interest to declare in relation to this article.