Abstract
Background:
Mindfulness and compassion are therapeutically relevant and can be increased through different forms of meditation practices. However, meditation practice needs time and commitment. These resources are often limited in patients with mood disorders. Therefore, efficacious remedies that increase mindfulness and compassion could provide therapeutic options. This study aimed to investigate the relationship between psychedelic experiences induced by an ayahuasca-inspired N,N-dimethyltryptamine (DMT)/harmine formulation on mindfulness and compassion in healthy subjects.
Methods:
This study applies a randomized, double-blind, placebo-controlled within-subjects design in a laboratory setting with 31 healthy participants. Each subject received a formulation comprising DMT + harmine, harmine + placebo, and placebo only on three different study days. Primary outcomes were mindfulness (MINDSENS) and compassion (SOCS).
Results:
A significant effect of the drug on mindfulness (
Conclusions:
In line with previous studies on traditional botanical ayahuasca, our findings support the notion that the DMT/harmine formulation might have therapeutic potential through its ability to acutely enhance mindfulness and compassion. Continuing studies in therapeutic settings are needed to further elucidate the mechanisms of action of ayahuasca-inspired formulations.
Background
Improvement of mindfulness- and compassion-related capabilities through different forms of meditation practices can lead to better psychological well-being (Brown and Ryan, 2003; Coffey et al., 2010; Goldberg et al., 2022; Khoury et al., 2013; Reangsing et al., 2021). Meditation practice needs time, commitment, and motivation, which is often limited in patients with mood disorders (e.g., depression, bipolar disorder, anxiety, and addiction disorders). Therefore, rapid-acting, safe, and efficacious therapies that increase mindfulness could help patients to better deal with those mental disorders. From a psychotherapeutic perspective, meditation and mindfulness practice became a central element of the so-called third wave of cognitive behavioral therapies. Programs like acceptance and commitment therapy, mindfulness-based cognitive therapy (MBCT), mindfulness-based stress reduction, or compassion-focused therapy (CFT) facilitate competences like observing, non-reacting, decentering, and self-compassion (see methods) and are promising approaches for the treatment of anxiety, depression, and pain (Goyal et al., 2014; Pots and Chakhssi, 2022).
The recent resurgence of psychedelic research (Tullis, 2021) has brought forth promising results in the treatment of mood and anxiety disorders (Carhart-Harris et al., 2016, 2021; Gasser et al., 2015; Gukasyan et al., 2022; von Rotz et al., 2023). Several systematic reviews and meta-analyses have been conducted, showing the promising potential of psychedelic-assisted therapies (Andersen et al., 2021; Ko et al., 2023; Luoma et al., 2020; Reiff et al., 2020; Romeo et al., 2021). Notably, the indigenous plant medicine ayahuasca shows a rapid antidepressant action in patients with treatment-resistant depression in placebo-controlled trials (Palhano-Fontes et al., 2019; Zeifman et al., 2019). General improvement of mental health is frequently reported by experienced ayahuasca users (Sarris et al., 2021), especially enhancement of emotional empathy due to both pharmacological and non-pharmacological (e.g., ceremonial setting) factors (Uthaug et al., 2021). Improved outcome measures in clinically depressed patients (van Oorsouw et al., 2022) as well as increased mindfulness-related and self-compassion capabilities in healthy subjects (Domínguez-Clavé et al., 2016; Soler et al., 2016) after ingestion of ayahuasca or ayahuasca analogues have been found. These findings are well in line with other serotonergic psychedelics that showed potential to enhance mindfulness, alongside positive effects on prosocial behaviors and empathy for others (Jungaberle et al., 2018).
The molecule N,N-dimethyltryptamine (DMT) is the main psychoactive compound in ayahuasca and shares a structural similarity with the 5-HT2A receptor agonist psilocybin (O-phosphoryl-4-hydroxy-N,N-dimethyltryptamine) and the endogenous neurotransmitter serotonin (5-hydroxytryptamine). Unlike other psychedelics, DMT has been found in the brain of rats (Dean et al., 2019) and seems to be endogenously produced in humans (Barker, 2022; Barker et al., 2012; Franzen and Gross, 1965; Kärkkäinen et al., 2005). However, it is still unclear what the physiological role of DMT is (e.g., under which circumstances it is being produced) and if it reaches sufficient brain concentrations to produce any subjective effects in humans. Nonetheless, DMT is widely spread throughout nature in around 60 identified plants, for example, in
The pharmacological and non-pharmacological mechanisms of action of ayahuasca and DMT-based formulations remain poorly understood. The ingestion of ayahuasca induces an altered state of consciousness (lasting 2–5 h) that shares a similarity to dream-like states with elevated introspective awareness (Riba et al., 2001) and changed perspectives on thoughts and feelings comparable to mindfulness-based training outcomes (Baer et al., 2006). This, in turn, may support certain forms of detachment from maladaptive thoughts or emotions, also called “decentering,” which is a core feature of the therapeutic potential of mindfulness practices (Fresco et al., 2007).
According to Grossman, 2008 (2011) and Van Dam et al. (2018), mindfulness is a complex construct and difficult to measure (low reliability). It is therefore suggested that the measurement of compassion could be more accurate, precise, and reliable (Gu et al., 2020). Compassion in this work is clearly defined by five subdimensions, namely recognizing suffering, understanding the universality of suffering, feeling for the person suffering, tolerating uncomfortable feelings, and motivation to act/acting to alleviate suffering (see methods). CFT (Gilbert, 2014; Pots and Chakhssi, 2022) is a recently developed therapeutic approach that is particularly suited for individuals characterized by the tendency to negatively evaluate and judge aspects of the self. Several meta-analyses demonstrate efficacy for compassion-based interventions in various (non)-clinical populations with moderate to large effects on depression and well-being (Kirby et al., 2017; Millard et al., 2023; Wakelin et al., 2022; Wilson et al., 2019). Hence, self-compassion and compassion with others may provide a valuable resource to cope with difficult emotions and thoughts during psychedelic experiences and to reduce suffering in clinical populations.
This study aimed to evaluate mindfulness- and compassion-related capabilities after the intake of an ayahuasca-inspired formulation containing intranasal DMT and sublingual harmine (DMT/HAR) compared to harmine alone (HAR) and placebo (PLA) in healthy subjects using a double-blind, placebo-controlled, randomized trial design. We expected to find a significant increase in mindfulness (MINDSENS), self-compassion (SOCS-S), and compassion with others (SOCS-O) after the DMT/HAR intervention, with less pronounced effects in the HAR condition compared to PLA. We expected these effects to be stronger for high versus low responders to DMT/HAR (high- vs low-sensitivity group).
Methods
Study design
The trial applied a double-blind, randomized, placebo-controlled, within-subjects study design in 31 healthy subjects with three conditions: (1) DMT + harmine (DMT/HAR), (2) placebo + harmine (HAR), and (3) placebo + placebo (PLA). An overview of the study design with the timepoints, interventions, and assessments relevant for this publication is shown in Figure 1.
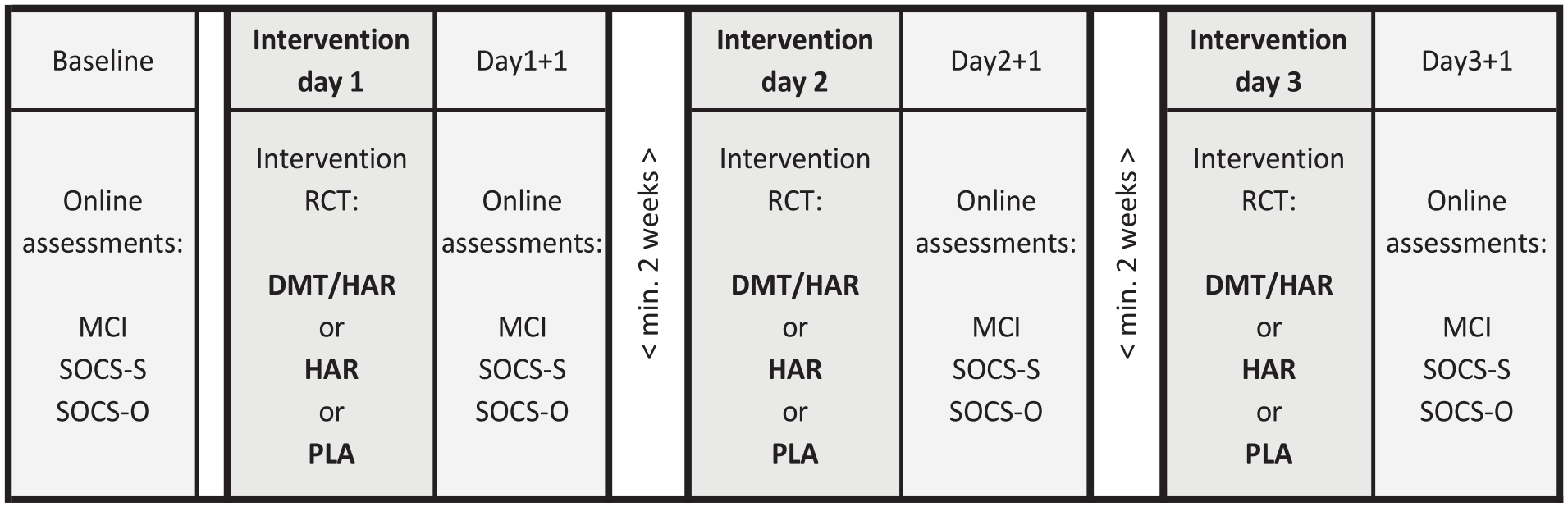
Study plan overview.
Setting
The study was conducted during the daytime in the rooms of the Human Sleep Laboratories. The soundproof and temperature-controlled rooms were set up in a comfortable living room atmosphere and equipped with dimmable lights and a sound system (see Supplemental Figure 4). Technical monitoring and measuring devices were installed. Throughout all study days, a standardized playlist containing non-stimulating background music was played to provide a feeling of comfort and relaxation. It was an individual setting with one participant in the room. A medically trained experimenter was present all the time to supervise the participants.
Study drug
We explored novel parenteral administration routes and delivery mechanisms, specifically designed to deliver purified forms of harmine and DMT, extracted from the plant
Thirty minutes after administration of harmine HCl (100 mg; mg/kg body weight:
Participants and permissions
A total of 37 healthy male participants were recruited after a thorough medical and psychological screening day. Six dropped out (four before the first intervention day, two after the first intervention day; they decided not to participate further because of the time commitment); drop-outs were replaced. In all, 31 participants (25.39 ± 4.21 years) completed all three intervention days and were considered for the analysis. The following criteria were required for inclusion: (i) age 20–40, (ii) BMI 18.5–30, (iii) male sex to avoid the potential impact of menstrual cycle on blood chemistry—because of blood chemistry analyses reported elsewhere (Mueller, Aicher and Dornbierer, 2025), (iv) no current or previous history of somatic, neurological, or psychiatric disorder, assessed during medical and psychiatric screening, (v) no family history of psychosis, bipolar, or other severe psychiatric disorders, (vi) no acute or chronic medication intake that could interact with the study drug, and (vii) no current or regular drug intake. A detailed overview of the demographics of participants, including their previous drug experience and their motivation to participate in the study, can be found in Supplemental Tables 1–4. Participants received monetary compensation (320.- CHF ≅ € total, or 60.- CHF ≅ € per completed intervention day). All participants provided written informed consent according to the Declaration of Helsinki.
Outcome measures
The following questionnaires were applied:
The questionnaire consists of a 20-item scale for others (SOCS-O) and a 20-item scale for self (SOCS-S). Scores on both scales show adequate internal consistency, interpretability, floor/ceiling effects, and convergent and discriminant validity. The items are scored on a 5-point Likert-type scale, ranging from
Statistical analyses
The data were analyzed with R Studio version 2021.09.2+382 (RStudio Team, 2019). The main subjective outcome measures were mindfulness (measured with the MCI), self-compassion (measured with the SOCS-S), and compassion with others (measured with the SOCS-O). According to a median split of the maximum subjective intensity ratings in the DMT/HAR conditions, participants were grouped into low versus high sensitivity to the study drug. For our hypotheses concerning the main subjective outcome measures, (generalized) linear mixed models (estimated using REML and nloptwrap optimizer) were fitted with the R lme4 package (Bates et al., 2015) to predict the outcome measures with drug condition (DMT/HAR, HAR, PLA) and sensitivity (high vs low) and the interaction of drug and sensitivity. By fitting the models on a standardized version of the dataset, standardized parameters were obtained. A type III repeated measures analysis of variance with Satterthwaite’s method table was produced to detect the main and interaction effects. Post hoc pairwise analyses to explore the significant effects were performed using the emmeans package (Lenth et al., 2021). Degrees of freedom (
Results
Mindfulness per condition
Results on the MCI global score and all subscales are shown in Table 1. In the following subsection, the results for the global score are described. The results of the global score by drug condition, grouped by sensitivity to the drug, are visualized in Figure 2. A notable number of observations (
Mindfulness (MCI) and compassion (SOCS) by drug condition and sensitivity to the drug.
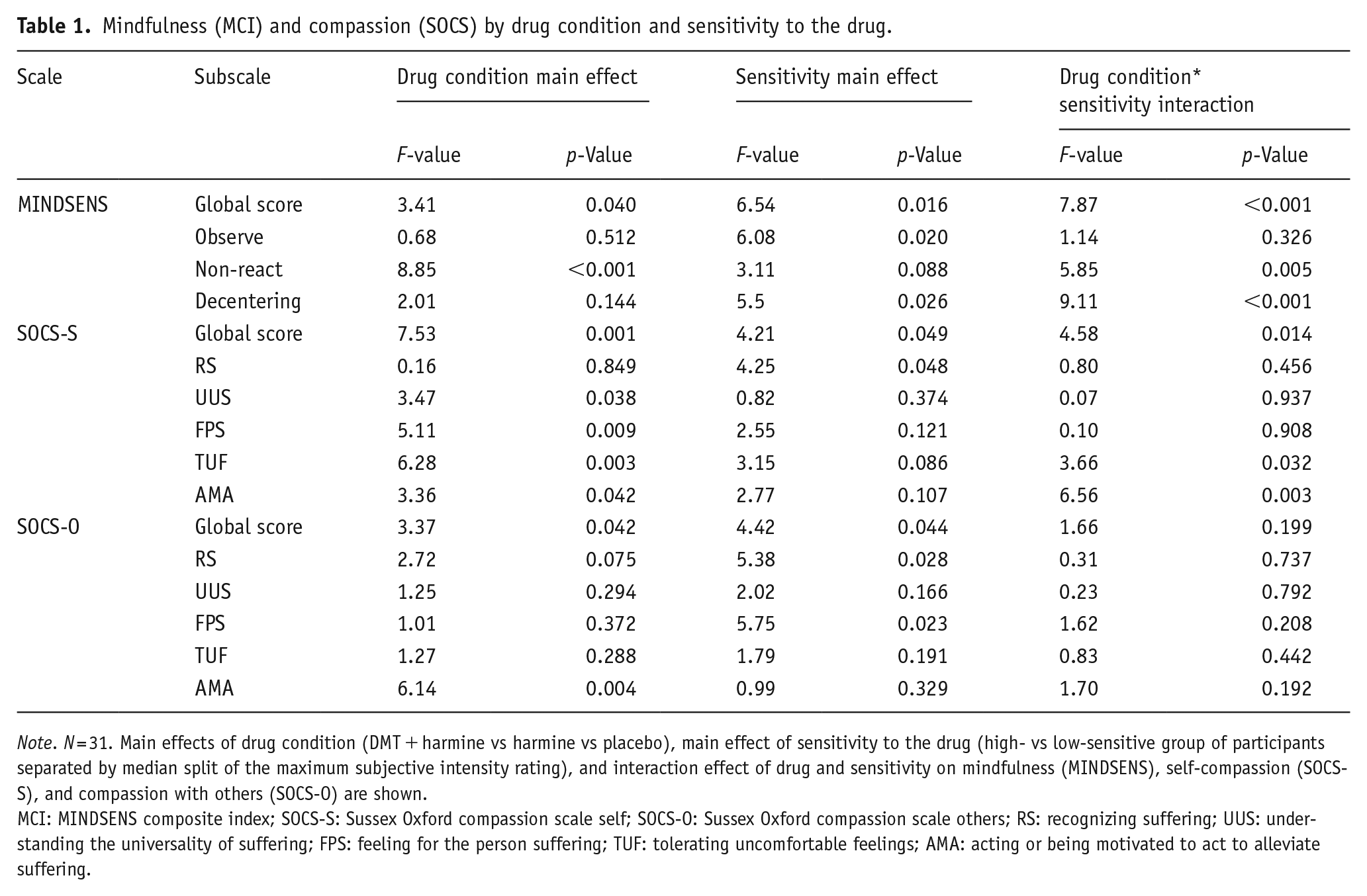
MCI: MINDSENS composite index; SOCS-S: Sussex Oxford compassion scale self; SOCS-O: Sussex Oxford compassion scale others; RS: recognizing suffering; UUS: understanding the universality of suffering; FPS: feeling for the person suffering; TUF: tolerating uncomfortable feelings; AMA: acting or being motivated to act to alleviate suffering.
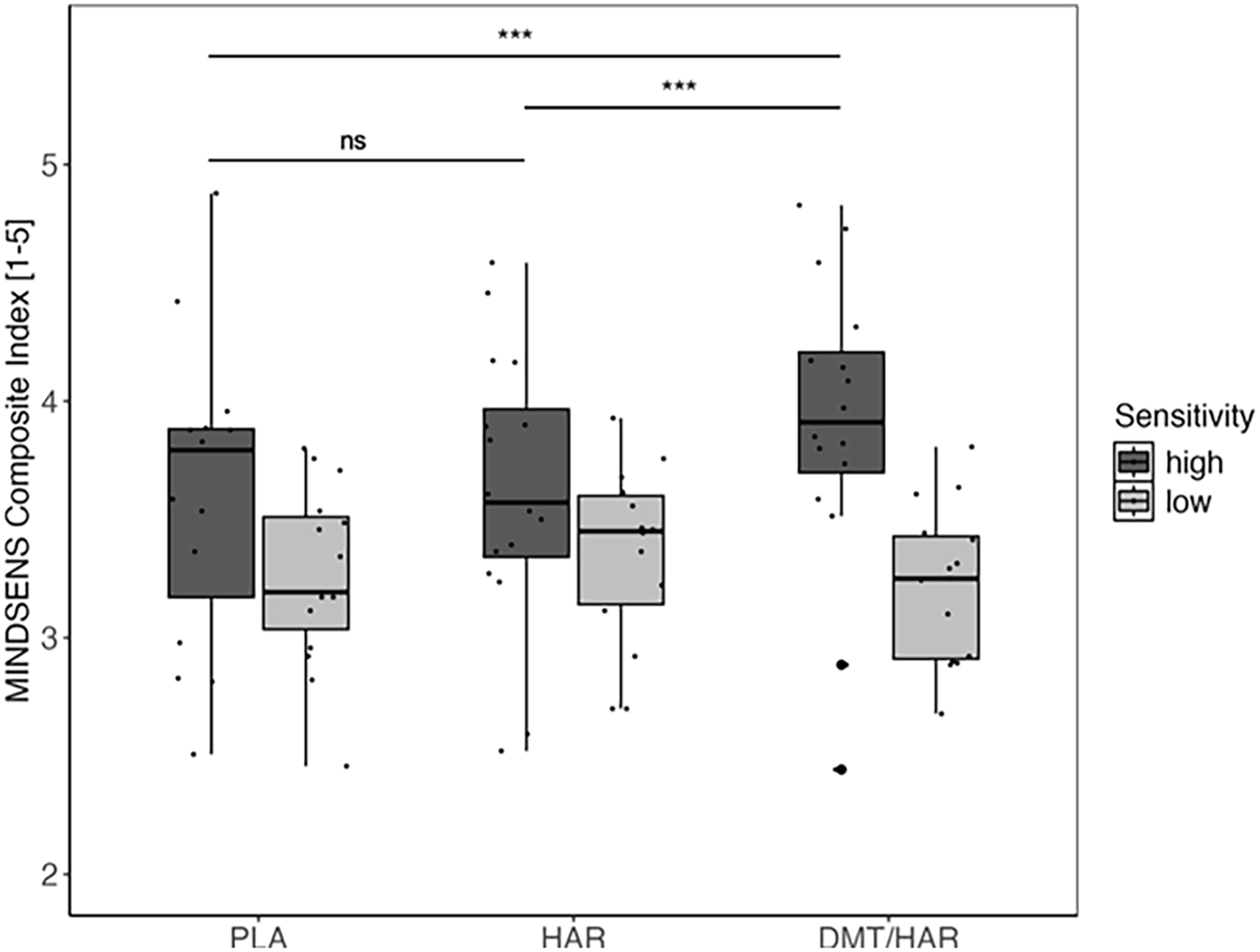
MCI global scores by drug condition and grouped by sensitivity to the drug.
MCI global score
The model’s total explanatory power was substantial (conditional
Post hoc tests revealed that participants showed significantly higher levels of MCI in DMT/HAR compared to PLA (
While the differences between the drug conditions were not different in the low-sensitivity group (DMT/HAR − HAR:
Compassion per condition
Results on the global score and subscales of SOCS-S and SOCS-O are shown in Table 1. In the following subsection, the results of the global score for both scales are described. The results of the global score by drug condition grouped by sensitivity are visualized in Figures 3 and 4. A notable number of observations (
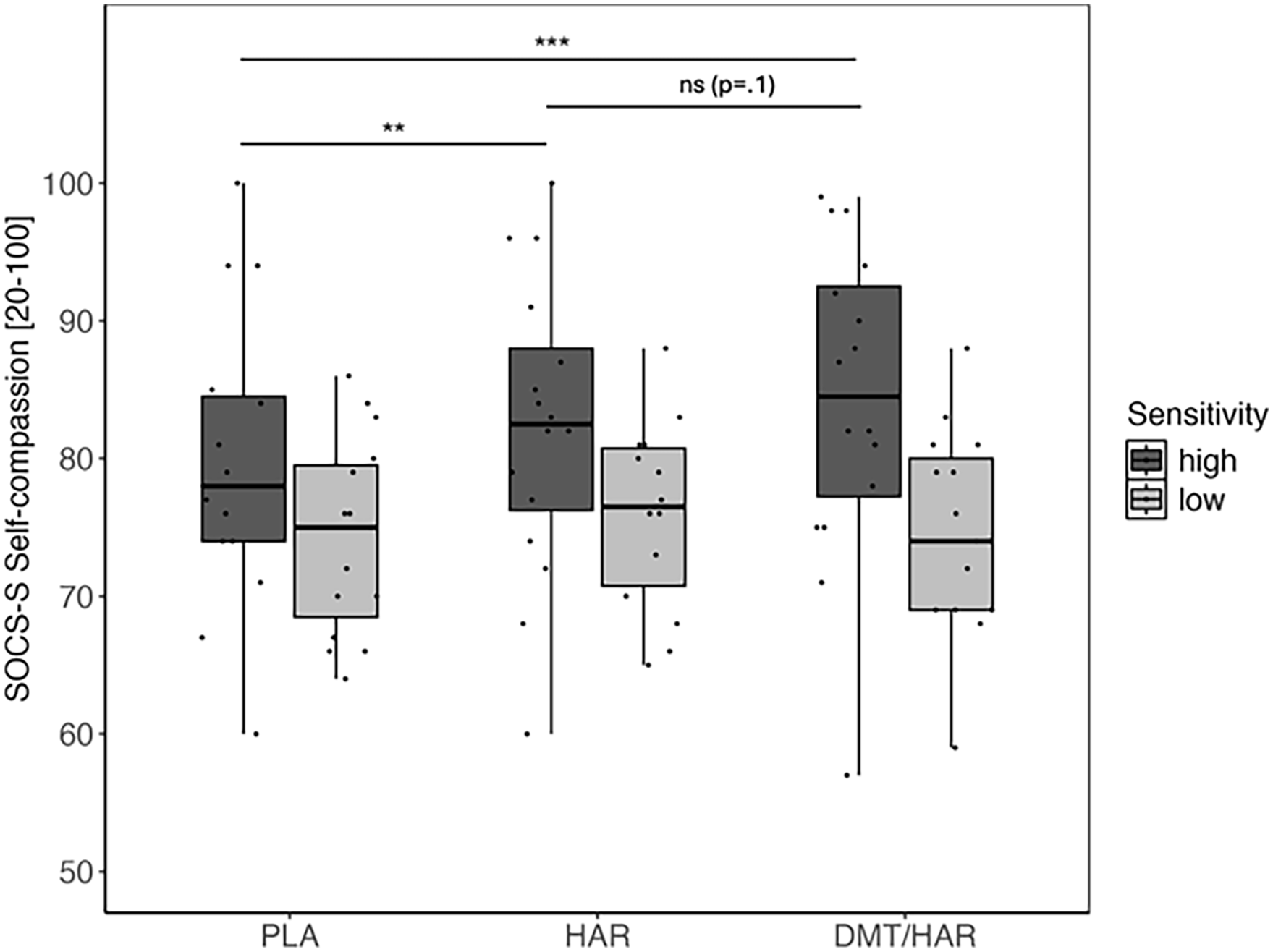
SOCS-S global scores by drug condition and grouped by sensitivity to the drug.
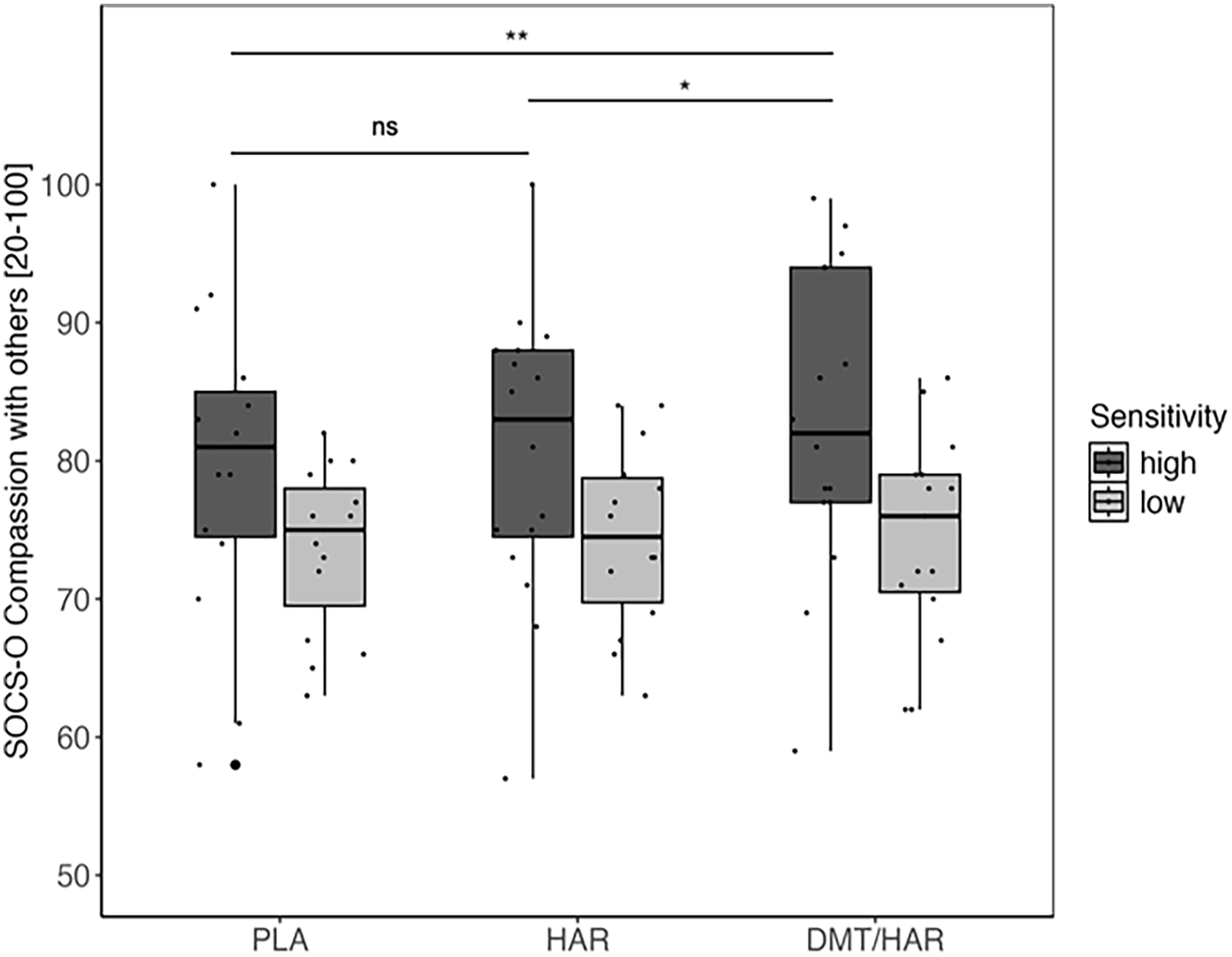
SOCS-O global scores by drug condition and grouped by sensitivity to the drug.
SOCS-S global score
The model’s total explanatory power was substantial (conditional
Post hoc tests revealed that participants showed significantly higher levels of SOCS-S in DMT/HAR (
While the differences between the drug conditions were not different in the low-sensitivity group (DMT/HAR − HAR:
SOCS-O global score
The model’s total explanatory power was substantial (conditional
Post hoc tests revealed that participants showed significantly higher levels of SOCS-O in DMT/HAR compared to PLA (
While the differences between the drug conditions were not different in the low-sensitivity group (DMT/HAR − HAR:
Discussion
This randomized, placebo-controlled, double-blinded study aimed to evaluate mindfulness- and compassion-related capabilities after the intake of an innovative ayahuasca-inspired formulation (containing DMT and MAO-inhibitor harmine; DMT/HAR) and harmine (HAR) against placebo (PLA) in healthy subjects to explore potential therapeutic change mechanisms. Our findings indicate an acute increase in mindfulness- and compassion-based outcome measures, comparable to changes in meditation practitioners, since the MCI was originally developed to assess the effects of long-term meditation practice. Our study indicates that short-term enhancement in mindfulness abilities can be reached not only by meditation practice, but also by a pharmacological intervention with DMT/HAR in a controlled laboratory setting, even without concomitant mindfulness training. Following our initial hypothesis, we found a significant drug effect with specifically higher mindfulness and compassion scores in DMT/HAR and less pronounced effects in HAR, compared to PLA. Significant effects for HAR could only be found for self-compassion. Participants from the high-sensitivity group were more likely to report differences in mindfulness, self-compassion, and compassion with others when DMT/HAR was compared to HAR or PLA, but not participants from the low-sensitivity group. No lasting effects in the 1-month and 4-month follow-up were found.
Regarding the specific mindfulness subscales, decentering and observing abilities were increased in the high-sensitivity group, and a highly significant drug effect was found for non-reacting. Non-reacting describes a state of mind in which one allows thoughts and feelings to come and go without getting caught up in them, which, in turn, is therapeutically valuable (Baer et al., 2006; Thomas et al., 2013). Decentering on the other hand is defined as the capacity to step outside one’s personal perspective of a lived experience and to disidentify from the content of thoughts (Fresco et al., 2007) or in other more specific words it is the capacity to recognize one’s thoughts and emotions as temporary events of the mind (Soler et al., 2014). This allows patients to consider thoughts and emotions in a detached manner rather than statements that are necessarily true (Fresco et al., 2007). Hence, increased decentering abilities could explain the therapeutic effect of interventions with psychedelics like ayahuasca in depression (de Osório et al., 2015; Domínguez-Clavé et al., 2016; Sampedro et al., 2017; Sanches et al., 2016; Soler et al., 2016), a disorder that is associated with impaired decentering abilities, in other work also called reduced metacognitive awareness (Teasdale et al., 2002).
Regarding the SOCS-O (compassion with others) subscales, recognizing suffering and feeling for the person suffering were also significantly increased in the high-sensitivity group. In the SOCS-S (self-compassion) subscales, only the recognizing suffering subscale was significantly increased in the high-sensitivity group. Testing for drug effects, most of the subscales of SOCS-S (four out of five) were significantly increased, which indicates that DMT/HAR has a stronger effect on self-compassion compared to compassion with others and mindfulness. Interestingly, self-compassion increased in both the DMT/HAR and HAR conditions. This finding could be explained via the nonspecific serotonergic stimulation effects that are described for the MAO-A inhibitor harmine (Herraiz et al., 2010). Moderately elevated levels of serotonin in the synaptic cleft may reduce anxiety/stress and promote general feelings of empathy and tenderness toward oneself. Comparable findings of adaptive self-attitudes such as increased emotional empathy and self-compassion were observed after ingestion of nonspecific serotonergic substances such as MDMA (Kamboj et al., 2018). Cultivating self-compassion brings understanding toward oneself in instances of perceived inadequacy or suffering (Neff, 2003) and is an important mediator of the positive effects of MBCT interventions on depressive symptoms (Kuyken et al., 2010). Therefore, augmenting CFT with pharmacological interventions that enhance compassion and social connection could be especially suitable for people who have a compromised capacity for experiencing and expressing affiliative motives and emotions, that is, those with high levels of self-criticism and shame (Pots and Chakhssi, 2022). Ayahuasca-inspired formulations might be particularly well suited to support attitudes of openness and acceptance toward physical and mental discomfort by enhancing compassion for self and others, which is a valuable skill set for navigating physical and mental crises and coping with stress in everyday life.
It is possible that the sensitivity to the substance and experiential aspects depends on certain predispositions, such as personality traits. For instance, the trait of absorption, which refers to an individual’s openness to a variety of cognitive, perceptual, and imagistic experiences, was found to strongly predict several experiences measured in previous studies (Studerus et al., 2012). Interestingly, trait absorption was not only associated with the ability to reach peak experiences but also found to be elevated in meditation practitioners (Garcia-Campayo et al., 2022). Hence, further research examining personality traits and their influence on the ability to reach intense psychedelic experiences and their association with outcome measures, such as mindfulness, is essential.
Furthermore, depression or other psychiatric disorders (or also somatic diseases) may impact an individual’s sensitivity to both mindfulness-based interventions and the pharmacological treatment with DMT/HAR. Depression and also anti-depressive medication might alter neurobiological mechanisms and increase or decrease sensitivity to the DMT/HAR. Further clinical trials with patients are necessary to explore effective doses for patients with mood disorders or other indications. Based on these doses, further studies should investigate whether patients experience effects on mindfulness, compassion, or other therapy-relevant mechanisms induced by DMT/HAR.
In summary, our results provide an explanatory mechanism that could contribute to similar benefits reported in prior studies for ayahuasca in the treatment of addiction and depression (de Osório et al., 2015; Thomas et al., 2013). It is worth mentioning that prior studies showing benefits associated with long-term ayahuasca use could be confounded by participants being members of a religious group or taking ayahuasca in a ceremonial context (Bouso et al., 2012; Fábregas et al., 2010). The present results obtained in a non-ceremonial, controlled laboratory setting, where participants engaged in neurobehavioral tasks, support the notion that ayahuasca-inspired pharmacological formulations, such as those containing DMT and harmine, may transiently increase mindfulness- and compassion-related capabilities independent of context. Despite these significant acute drug effects, we could not find any long-term effects, which may be due to the fact that the study was not embedded in a therapeutic or mindfulness-based setting. Psychedelic-induced states of enhanced mindfulness tend to be short-lived and strongly support the notion of concomitant training and integration to stabilize and maintain more adaptive mental states in everyday life (Scheidegger, 2021a).
Limitations and future research
Our study has some limitations that need to be considered. First, the participant sample was quite homogeneous with regard to gender (male only), age (25 ± 4), educational status (highly educated), and ethnicity, which limits generalization of the findings. There is limited transferability to therapeutic contexts as the study was conducted in a laboratory setting with healthy participants. This study shows a transient increase in mindfulness and compassion in a non-meditation context that was not focused on mindfulness and compassion. It remains an open question for future research to investigate the magnitude and duration of DMT/HAR-induced mindfulness and compassion in a meditation context with meditation practitioners of various expertise levels (which we did in a follow-up study, see Meling et al., 2024). Moreover, the chosen dose range for DMT and harmine was moderate, as participants were expected to repeatedly participate in neurobehavioral tasks during the dosing session, which may have confounded and diminished the overall effects on mindfulness and compassion due to a high level of distraction. Further dose–response studies with higher dose ranges in appropriate settings would be informative to evaluate the therapeutic properties of ayahuasca-inspired formulations. Furthermore, the intensity of the subjective effects of the study drug might, in many cases, lead to an unblinding, at least in the high-sensitivity group, which can be considered another limitation of this work, as it may enhance expectation, respectively, placebo effects. This is a common issue in psychedelic research in general (Muthukumaraswamy et al., 2021). Blinding efficacy was not assessed in this study, which is a limitation.
To conclude, this study shows further evidence supporting that ayahuasca-inspired formulations like DMT/HAR may have the potential to induce acute increases in mindfulness and compassion. The adaptive effects of ayahuasca on psychological functioning are particularly aligned with mindfulness-based approaches that aim to increase compassion, awareness, and psychological flexibility in the service of achieving core life values. Ayahuasca-assisted therapy might work as a catalyst to support such transformative learning processes in the framework of a process-oriented psychotherapy (Mithoefer et al., 2021; Scheidegger, 2018, 2021b; Wheeler and Dyer, 2020). Further research in psychiatric populations is needed to corroborate the prevailing results.
Supplemental Material
sj-docx-1-jop-10.1177_02698811251344689 – Supplemental material for Enhancing mindfulness and compassion through an ayahuasca-inspired formulation containing N,N-DMT and harmine
Supplemental material, sj-docx-1-jop-10.1177_02698811251344689 for Enhancing mindfulness and compassion through an ayahuasca-inspired formulation containing N,N-DMT and harmine by Helena D Aicher, Ilhui A Wicki, Daniel Meling, Michael J Mueller, Dario A Dornbierer and Milan Scheidegger in Journal of Psychopharmacology
Footnotes
Acknowledgements
We thank Dila Suay, Luzia Caflisch, Alexandra Hempe, and Camilla Steinhart for their help with the study conduction; Claudius Elsner and Jovin Mueller for their medical supervision of the participants during the study days. We thank Hanspeter Landolt for providing the research facility and infrastructure. And we thank our study participants.
Author contributions
HDA: conception and design of the study, study management, data acquisition, data analysis, interpretation of results, drafting the article, revision of the article, and final approval of the version to be submitted. IAW: data acquisition, interpretation of results, drafting the article, revision of the article, and final approval of the version to be submitted. DM: data acquisition, interpretation of results, revision of the article, and final approval of the version to be submitted. MJM: study management, data acquisition, revision of the article, and final approval of the version to be submitted. DAD: conception and design of the study, study management, data acquisition, revision of the article, and final approval of the version to be submitted. MS: conception and design of the study, interpretation of results, revision of the article, and final approval of the version to be submitted.
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: HDA, IAW, MJM, and DM declare that they have no conflict of interest. DAD and MS declare that they co-founded Reconnect Labs, an academic spin-off at the University of Zurich, focused on the development of psychedelic medicines for mental health.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: We gratefully acknowledge grant funding that supported this publication from the SNSF Swiss National Science Foundation (HD Aicher, Grant P0ZHP1_191935; M Scheidegger and D Meling, Spark CRSK-1_196833), from the Bioentrepreneur Fellowship UZH (DA Dornbierer, BIOEF-18-009), from the Forschungskredit PostDoc UZH (M Scheidegger, Grant No. FK-18-052), from the BIAL Foundation (M Scheidegger and D Meling, No. 333/20), from the Reconnect Foundation (D Meling), and from private donations (MJ Mueller). The content is solely the responsibility of the authors and does not necessarily represent the official views of the funders.
Research ethics and patient consent
The study was conducted according to the World Medical Association Declaration of Helsinki. The study was approved by the Cantonal Ethics Committee of the Canton of Zurich (Basec-Nr. 2018-01385) and the Swiss Federal Office of Public Health (BAG-Nr (AB)-8/5-BetmG-2019/009268).
Clinical trial registration
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
