Abstract
Background:
Trauma-informed palliative care aims to improve end-of-life experiences by recognising and responding to the presence of psychological trauma. While many practitioners support the approach, they also acknowledge the need to build a stronger evidence base.
Aim:
To: (1) understand the methodology and defining features of existing research; (2) describe how the impact of psychological trauma at the end-of-life is understood; and (3) describe the nature of, and challenges to, palliative care approaches that recognise and respond to such trauma.
Design:
A systematic scoping review was conducted following the Joanna Briggs Institute guidelines. The review protocol was registered on Open Science Framework.
Data sources:
Eight electronic databases were systematically searched; evidence sources that considered psychological trauma in an end-of-life context were included.
Results:
Ninety-nine sources (13 countries) were identified. 40% were clinical case studies. Cancer was the primary diagnosis for the majority of patients in 55 sources and 24 sources focussed on veterans. Six ways of describing the impact of psychological trauma at the end-of-life were identified. Few sources (n = 20) implemented trauma-informed care; 15 of these were clinical case studies. Though trauma-informed palliative care was not always explicitly present, six palliative care approaches to recognising and responding to psychological trauma, and five main challenges to its effective implementation, were identified.
Conclusions:
Limited research has been conducted on trauma-informed palliative care. However, the review identified a substantial body of evidence that describes concepts relevant to its approach. These findings provide a valuable starting point for future research.
Keywords
Trauma-informed care is a philosophical framework that can be applied to any service or organisation, including health and social care systems.
Since 2018 palliative care professionals have been advocating for a trauma-informed approach to palliative care services.
Arguments in support of the implementation of trauma-informed palliative care focus on the prevalence of psychological trauma in the palliative care population and the myriad of ways this can negatively impact the end-of-life experience.
As the first known systematic scoping review of trauma-informed palliative care, this paper identified 99 relevant evidence sources from 13 countries.
Whilst the identified evidence sources described many concepts related to trauma-informed palliative care, there is limited evidence informing the conceptualisation and implementation of the approach.
In addition to the frequently cited negative impacts of psychological trauma at the end-of-life, some evidence sources also highlighted potentially positive impacts.
Further research is needed before trauma-informed palliative care can be fully conceptualised and implemented in practice.
Conceptualising trauma-informed palliative care will require an appreciation of how it may differ from general trauma-informed care approaches, as well as how it overlaps with existing principles of palliative care.
Implementing trauma-informed palliative care will require an honest evaluation of the resources and time it requires and whether this can be effectively achieved within the limits of a palliative care setting.
Introduction
‘Trauma-informed care’ was first proposed as a philosophical framework of significant relevance to contemporary palliative care in 2018. 1 Since then, an increasing momentum has gathered among palliative care professionals for this approach to be adopted at both individual practitioner and organisational service levels.2–14
As an approach, trauma-informed care has its origins in the work of two North American clinical psychologists, who, in the early 2000s, described it as a ‘vital paradigm shift’ for the mental health and substance abuse service system. 15 (p3) Highlighting the pervasiveness and persistence of psychological trauma in this system, as well the nuanced ways it can negatively impact the service experience, the authors encouraged organisations to become ‘trauma-informed’. 15 This meant creating policies, practices, and procedures which acknowledge the role of trauma in an individual’s life, and which strive to avoid re-traumatising both service users and staff. 16 In 2014, the US Substance Abuse and Mental Health Services Administration (SAMHSA) formalised the framework, providing background research and definitions around psychological trauma as well as four assumptions and six principles for trauma-informed care. 17
According to SAMHSA, psychological trauma is defined as that which ‘results from an event, series of events, or set of circumstances that is experienced by an individual as physically or emotionally harmful or life threatening and that has lasting adverse effects on the individual’s functioning and mental, physical, social, emotional, or spiritual well-being’ (p. 7). 17 While a particular event can be a physical trauma (i.e. a serious body injury), organisations such as the UK Trauma Council have highlighted that psychological trauma can arise from any number of incidents that are usually beyond a person’s control. These can include (but are not limited to): sexual or physical abuse or assaults, terrorist attacks, war, natural disasters, traffic collisions, fires, kidnap, death of a close friend or family member, painful or frightening medical procedures, racism and other forms of hatred and/or discrimination. 18
Discussions around psychological trauma frequently refer to two further concepts: adverse childhood experiences (ACEs) and post-traumatic stress disorder (PTSD). Although these terms will be used throughout this scoping review, is important to acknowledge that these are research topics that give rise to ongoing debates.19,20 In the context of trauma-informed care, research on the prevalence and lifelong impact of adverse childhood experiences (potentially trauma-inducing events that occur during childhood) is often cited as a key rationale for the implementation of the approach. 21 Similarly, research on the prevalence and impact of PTSD, one of the trauma and stressor-related disorders categorised in the 2022 text revision of the Diagnostic and Statistical Manual, 22 is also put forward as grounds for embracing the framework. 1 Alisic et al. 23 suggest that some, but not all, individuals who experience psychological trauma will develop PTSD, meaning they will experience symptoms including intrusions, avoidance, changes in cognition and mood, arousal, and reactivity that endure for more than 1 month. 22
The US Substance Abuse and Mental Health Services Administration’s conceptualisation of trauma-informed care is based on six principles (safety; trustworthiness and transparency; peer support; collaboration and mutuality; empowerment, voice, and choice; and cultural, historical and gender issues) and four assumptions (realisation, recognition, response, resisting re-traumatisation). 17 This conceptualisation has now been endorsed in a number of national government policies and applied to a variety of health and care services.24,25 While there is still only minimal reference to these principles in national or international palliative care guidance, 26 many professionals have advocated for their use in palliative care service design and delivery.1–5,13,14 Aside from the generalised arguments that trauma-informed care should be an integral part of all health and care services, these papers provide specific arguments for the implementation of trauma-informed palliative care, including: the characteristics of the palliative care population and their increased likelihood of experiencing psychological trauma,1,2,9,27 the myriad of ways that psychological trauma may negatively impact the palliative care experience, 1 and the synergies that potentially exist between the ethos of palliative care and the trauma-informed approach.4,9
Despite the widespread support, there is a lack of evidence examining whether trauma-informed palliative care is needed, how it is currently being defined and implemented, and what measures should be used to determine its effectiveness. 2 Consequently, this scoping review will act as a starting point, aiming to understand the relevance of a trauma-informed approach to palliative care and to establish future directions for meaningful research. It is important to note from the outset that although the scope of contemporary palliative care has widened, 28 for the purposes of this review ‘palliative care’ will be taken to be synonymous with end-of-life care.
Methods
Scoping review methodology is recommended for emerging areas of research that require answers to broad questions through the analysis of a heterogeneous selection of evidence sources. 29 The objectives of a scoping review can include: to identify and synthesis the types of available evidence; to clarify key concepts; to investigate research conduct; and to identify and analyse knowledge gaps to inform future practice, policy and research. 30 For these reasons, a scoping review methodology was chosen to answer the wide-ranging questions around trauma-informed palliative care.
The review followed the most recent Joanna Briggs Institute (JBI) guidelines 31 and has been reported in line with the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) Checklist (Supplemental Material 1). The scoping review was registered on Open Science Framework. 32
Review questions
The primary review question was: how do existing evidence sources express the potential for a trauma-informed approach to end-of-life palliative care for patients and their carers? This was drawn out into four secondary questions:
What type of research has been undertaken and what are the defining features?
How is the impact of psychological trauma at the end-of-life described?
How are approaches to palliative care that recognise the impact of psychological trauma described?
How are challenges to the effective delivery of palliative care that recognises the impact of trauma described?
Search strategy
A search of eight electronic databases (Embase, PsycINFO, Scopus, SocINDEX, ProQuest Thesis & Dissertations, Lens.org, CINHAL and Medline) was conducted in April 2025. This selection of databases was chosen as together they cover a wide range of evidence sources, including international studies and unpublished literature. This is aligned with guidance that suggests a scoping review should aim to be as comprehensive as possible in its search strategy, including articles that other methodologies with tighter eligibility criteria might exclude. 33
After analysing previous reviews of trauma-informed care,34–37 as well as keywords used in articles discussing trauma-informed palliative care,1,2,4,5 a combination of subject terms and free-text terms was chosen. A subject specific librarian validated the search strategy, an example of which can be found in Supplemental Material 2.
Eligibility criteria
The development of the eligibility criteria (Table 1) was guided by the Population, Concept and Context (PCC) framework. 33
Eligibility criteria.
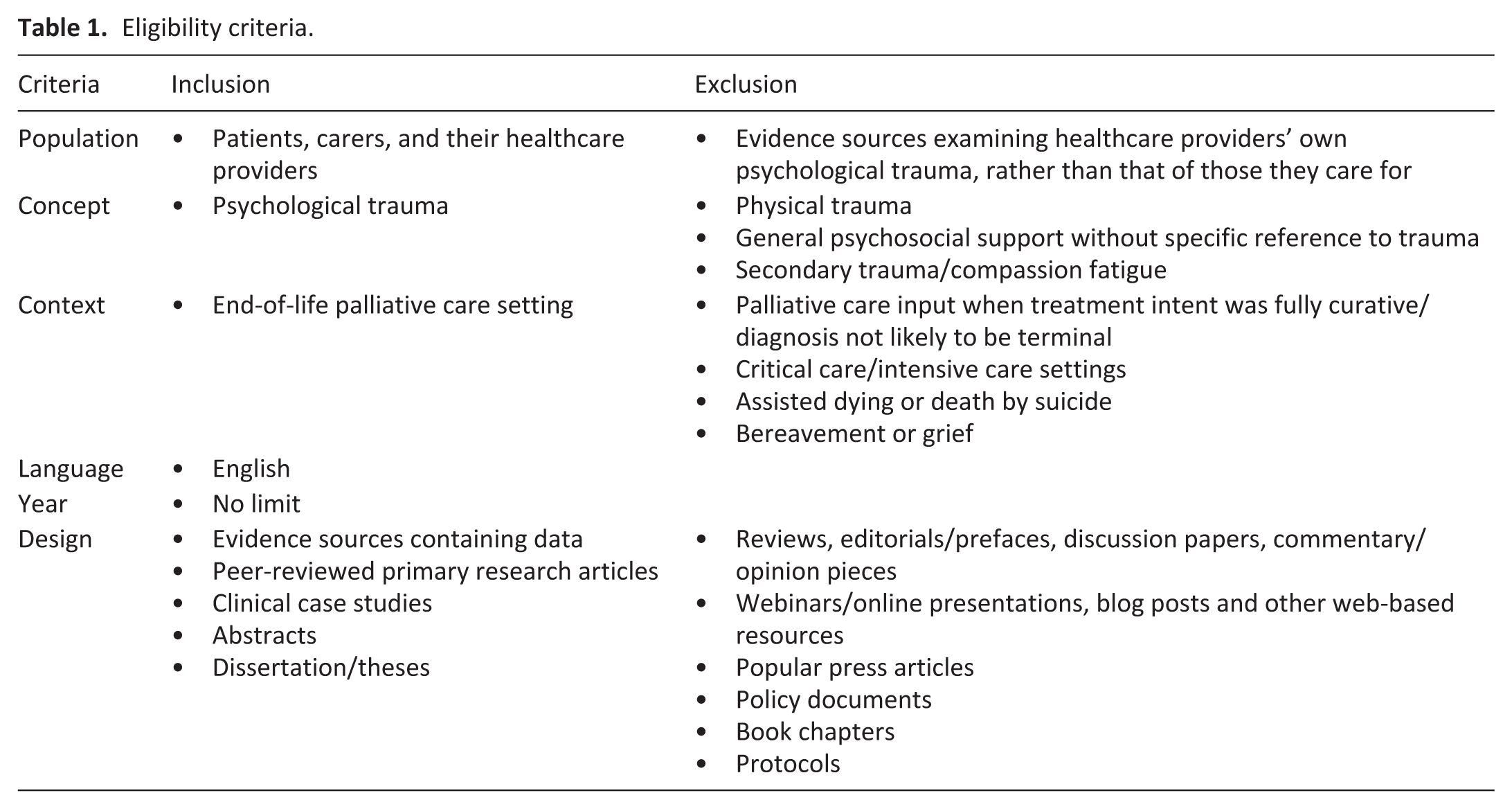
Although in theory a scoping review can include any type of evidence source, limits should be imposed based on a researcher’s knowledge on what would be most appropriate for answering the review questions. 33 The exclusion criteria outlined in Table 1 were primarily used to focus the scoping review and ensure that a manageable number of evidence sources were chosen for analysis. The researcher acknowledges that, unfortunately, this has meant that some highly relevant topics (e.g. bereavement and secondary trauma) have not been covered in this review. Given the breadth of these omitted topics, they could justifiably be the focus of future scoping reviews on specific aspects of trauma-informed palliative care.
Data extraction and analysis
Initially, a standardised data extraction form with accompanying guidance was developed and tested for each type of evidence source (Supplemental Material 3 and 4). Data were extracted into a customised table including author (s; year), primary professional field, country, aim, methodology and type of evidence source if relevant, study population and sample size, other defining features, and explicit mention of trauma-informed care. Following the Joanna Briggs Institute guidelines, 29 no formal quality appraisal was included. This preliminary extraction allowed for a basic analysis of the results using frequency counts and descriptive summary statistics. It also allowed for extraction of relevant information related to any defining features of the study (e.g. cancer as primary patient diagnosis; focus on people with lived experience of homelessness) and whether trauma-informed care was explicitly defined, recommended, or implemented.
Since a scoping review should not aim to conduct a meta-analysis or a thematic synthesis, 33 basic qualitative content analysis was used to identify descriptions in the evidence sources relevant to the review questions. 38 This is an appropriate method when included studies are heterogenous in nature, as it can be applied to any evidence source or study design. 38 It is also recommended when the review seeks to identify key characteristics or factors related to a concept or when the objective is to inform the development of a conceptual framework or theory. 38 Secondary review questions 2–4 were analysed separately, using an inductive process of open coding to describe data content 33 (Supplemental Material 5). A coding framework was then developed to allow for a second extraction and organisation of the data into categories (Supplemental Material 6-8). As permitted in the JIB guidance literature, it was decided to count the frequencies of qualitative codes and categories. 31 Though higher frequencies do not necessarily correspond with higher relevance, it was felt that this approach added value by providing an indication of commonly used descriptions across evidence sources.
Results
The search yielded 5409 results (4547 after de-duplication in EndNote). After screening in Rayyan by title and abstract, the full text of 551 evidence sources were assessed against the inclusion and exclusion criteria. One evidence source was not retrieved, and 99 were included in the review. The PRISMA flow diagram 39 summarising this is in Supplemental Material 9, while the preliminary data extraction of evidence sources is presented in Table 2.
Preliminary data extraction of evidence sources identified in the scoping review.
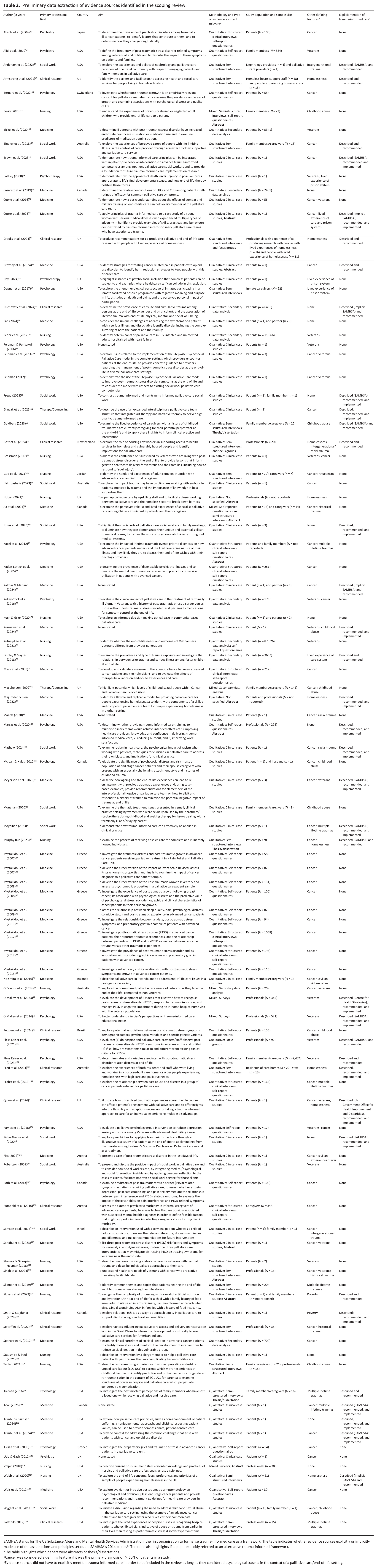
SAMHSA stands for The US Substance Abuse and Mental Health Services Administration, the first organisation to formalise trauma-informed care as a framework. The table indicates whether evidence sources explicitly or implicitly made use of the assumptions and principles set out in SAMHSA’s 2014 paper. 17 The table also highlights if a paper explicitly referred to an alternative trauma-informed framework.
The table highlights which papers were abstracts or thesis/dissertations.
Cancer was considered a defining feature if it was the primary diagnosis of > 50% of patients in a study.
Evidence sources did not have to explicitly mention trauma-informed care in order to be included in the review as long as they considered psychological trauma in the context of a palliative care/end-of-life setting.
What type of research has been undertaken and what are the defining features?
The data relevant to this secondary research question are summarised in Table 3. The majority of evidence sources were from the United States (62%, n = 61), followed by Greece (n = 10), the United Kingdom (n = 8), Canada (n = 6), Australia (n = 5), and Austria (n = 2). Seven further countries had one evidence source each: Brazil, Israel, Japan, Jordan, New Zealand, Rwanda, and Switzerland. It should be noted that the 10 quantitative studies conducted in Greece were conducted by one main research team; however, they were considered sufficiently distinguishable to all be included.
Research type and defining features.
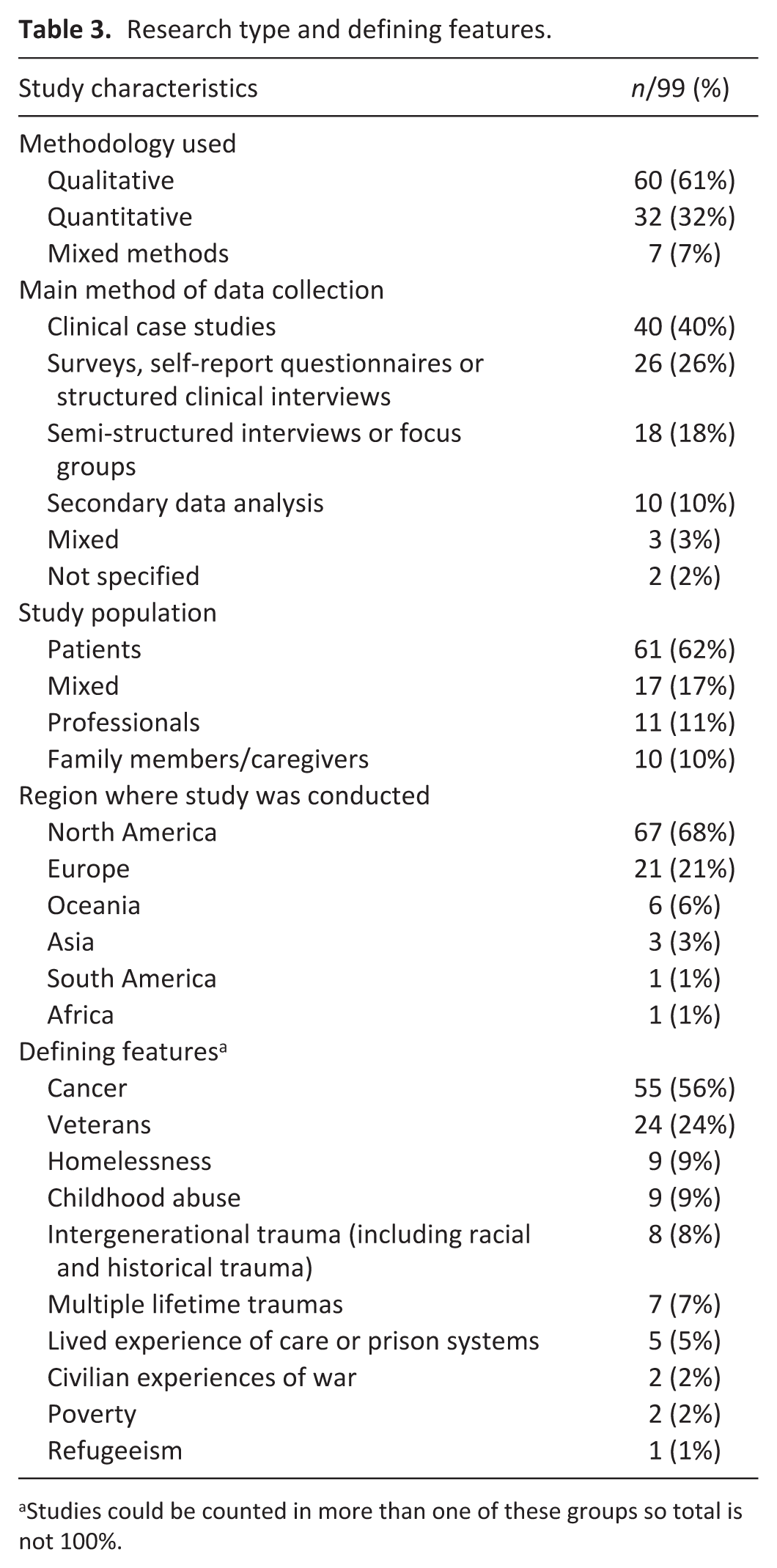

Studies could be counted in more than one of these groups so total is not 100%.
Nearly half of the evidence sources (43%, n = 43) were published in the past 5 years; one-fifth (n = 20) were recent papers from 2024 or 2025. The most common professional fields of the primary authors were medicine (n = 33), psychology (n = 17), nursing (n = 16) and social work (n = 14). Other professional fields included academic research (n = 11), psychiatry (n = 4), psychotherapy (n = 2). and therapy/counselling (n = 2).
The majority of the evidence sources were qualitative (61%, n = 60), with two-thirds of these employing a clinical case study approach (n = 40). The remaining evidence sources were quantitative (n = 32) or employed mixed methods (n = 7); the most frequent methodologies used in these two groups of sources were surveys, self-report questionnaires, or structured clinical interviews (n = 26). There were 14 abstracts and four theses/dissertations.
Patients were the primary study population for the majority of evidence sources (n = 61, 62%). Other evidence sources focussed on professionals (n = 11), family members/caregivers (n = 10), or a mixture of the three populations (n = 17). As expected given the heterogenous nature of the identified evidence sources, a wide variation in sample size was evident: none of the clinical case studies looked at more than eight individuals, whereas one secondary data analysis of deceased veterans included 87,526 records. 76
Cancer
Cancer was the primary diagnosis for all or the majority of patients in over half of the evidence sources (n = 55), including 24 clinical case studies.4,7–9,11,50,52,59–61,64,66,72,81,83,84,96,105,109,110,121,123,125,129 Quantitative and mixed methods papers generally used surveys, self-report questionnaires, and/or structured clinical interviews to determine the prevalence or impact of psychological distress, post-traumatic stress disorder (PTSD), or post-traumatic growth (PTG) for cancer patients or caregivers at the end-of-life.40,41,44,71,78,87–95,99,101,103,104,107,108,124,128 Some of the papers aimed to investigate whether cancer itself could be a traumatic event leading to PTSD. Results varied: in one study no advanced cancer patients met the diagnosis for PTSD, 40 in a second 2.4% of advanced cancer patients did, 71 and in a third looking at 170 advanced cancer patients with PTSD, the majority (66.7%) reported that their cancer diagnosis was the most traumatic event for them. 93 Three qualitative papers used in-depth interviews to explore psychological trauma in end-of-life cancer patients from the perspectives of informal caregivers, 47 refugees, 65 and those with lived experience of homelessness. 86 Two further qualitative papers focussed on professionals’ view of providing end-of-life cancer care to those who had experienced some form of historical trauma.112,116
Veterans
Twenty-four evidence sources focussed on the veteran population, most often in relation to PTSD. This included 12 clinical case studies8,9,48,50,58–60,64,75,106,110,111, five secondary data analyses based on medical records46,57,73,76,97, two quantitative studies administrating self-report questionnaires to family members41,101, one quantitative evaluation of a palliative psychology group intervention, 104 two mixed methods evaluations of a professional education needs,12,98 and two qualitative papers looking at hospice and palliative care clinicians’ perceptions of veteran end-of-life care.100,112 Some of these studies considered how a veteran’s age or war era might impact PTSD prevalence and presentation.46,100,101,111
Other defining features
Psychological trauma in the context of homelessness was a defining feature of nine qualitative evidence sources.8,43,51,63,67,80,86,102,127 Further sources described individuals with lived experience of homelessness even if it was not the main focus. Evidence sources on childhood abuse included six qualitative papers62,75,84,85,119,129, one mixed methods study looking at the effect of child maltreatment on caring for a patient at the end-of-life, 45 one audit of patient notes, 79 and one quantitative study exploring the relationship between adverse childhood experiences and post-traumatic stress symptoms in advanced cancer patients. 99 Intergenerational trauma, including historical and racial trauma, was the focus of seven qualitative papers42,63,81,83,109,112,116 and one mixed methods study exploring the palliative care experiences of Chinese immigrants. 68 Other identified traumas included poverty,114,115 lived experience of the care and prison systems,11,48,53,54,77 refugeeism, 65 and civilian experiences of war.96,105 In a number of evidence sources, patients or family members had experienced multiple traumas across their lifetimes. These included five qualitative papers7,113,120,121,130, one quantitative paper exploring the relationship between any form of past abuse and distress across five palliative care domains, 103 and another quantitative study examining the relationship between the number of traumatic events experienced and cancer patients’ likelihood of acknowledging their terminal illness or discussing end-of-life wishes with providers. 70
The remaining three secondary review questions were answered through basic quantitative content analysis. The full coding and coding frameworks for each question can be found in Supplemental Material 6-9; this fulfils item 17 of the PRISMA-ScR checklist to present relevant data for each individual evidence source. In addition, Tables 4 to 6 summarise the results by presenting frequency counts of the identified codes and categories as well as an example of the overall category.
Describing the impact of psychological trauma at the end-of-life.
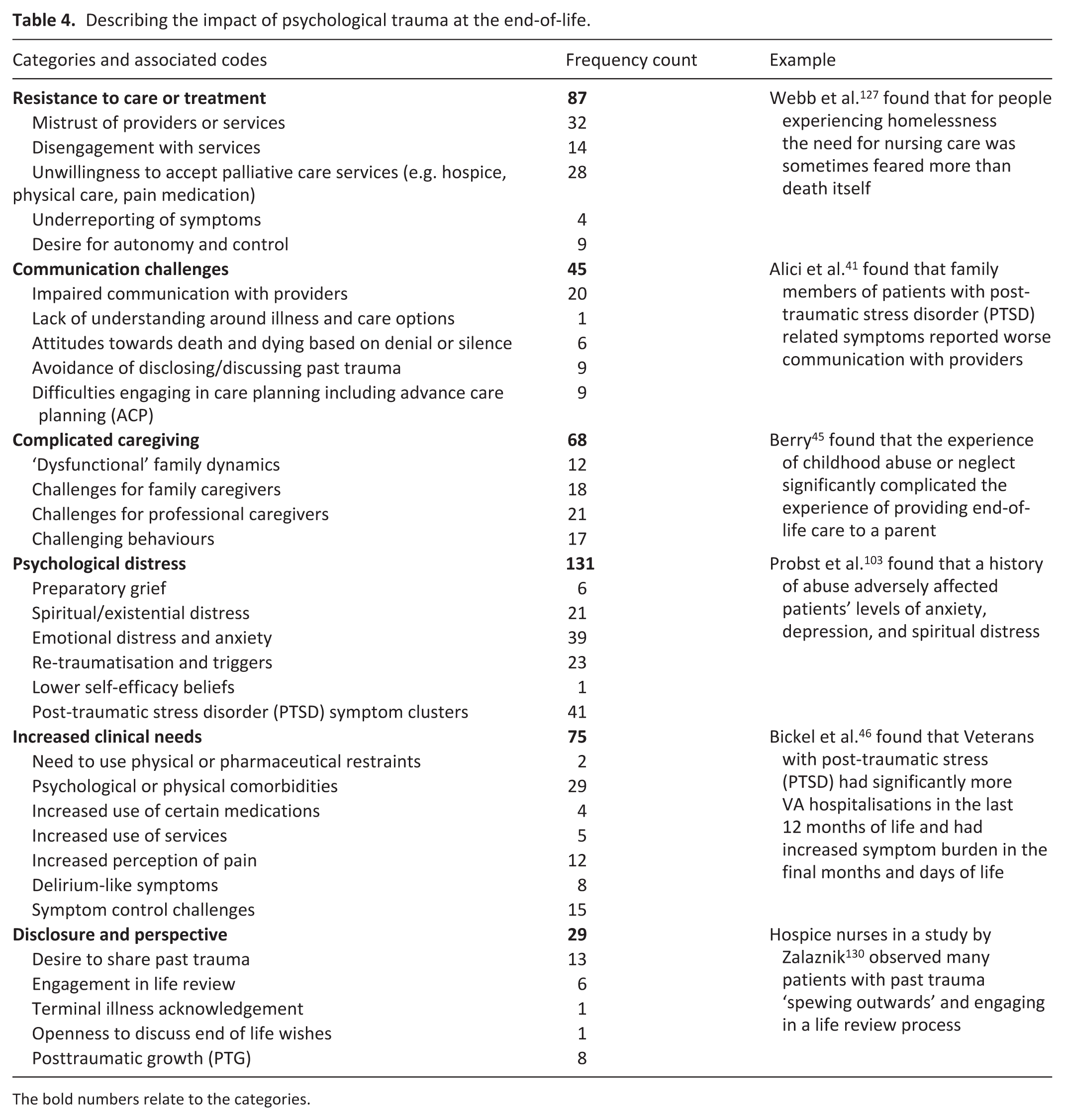

The bold numbers relate to the categories.
Describing approaches to palliative care that recognise the impact of psychological trauma.
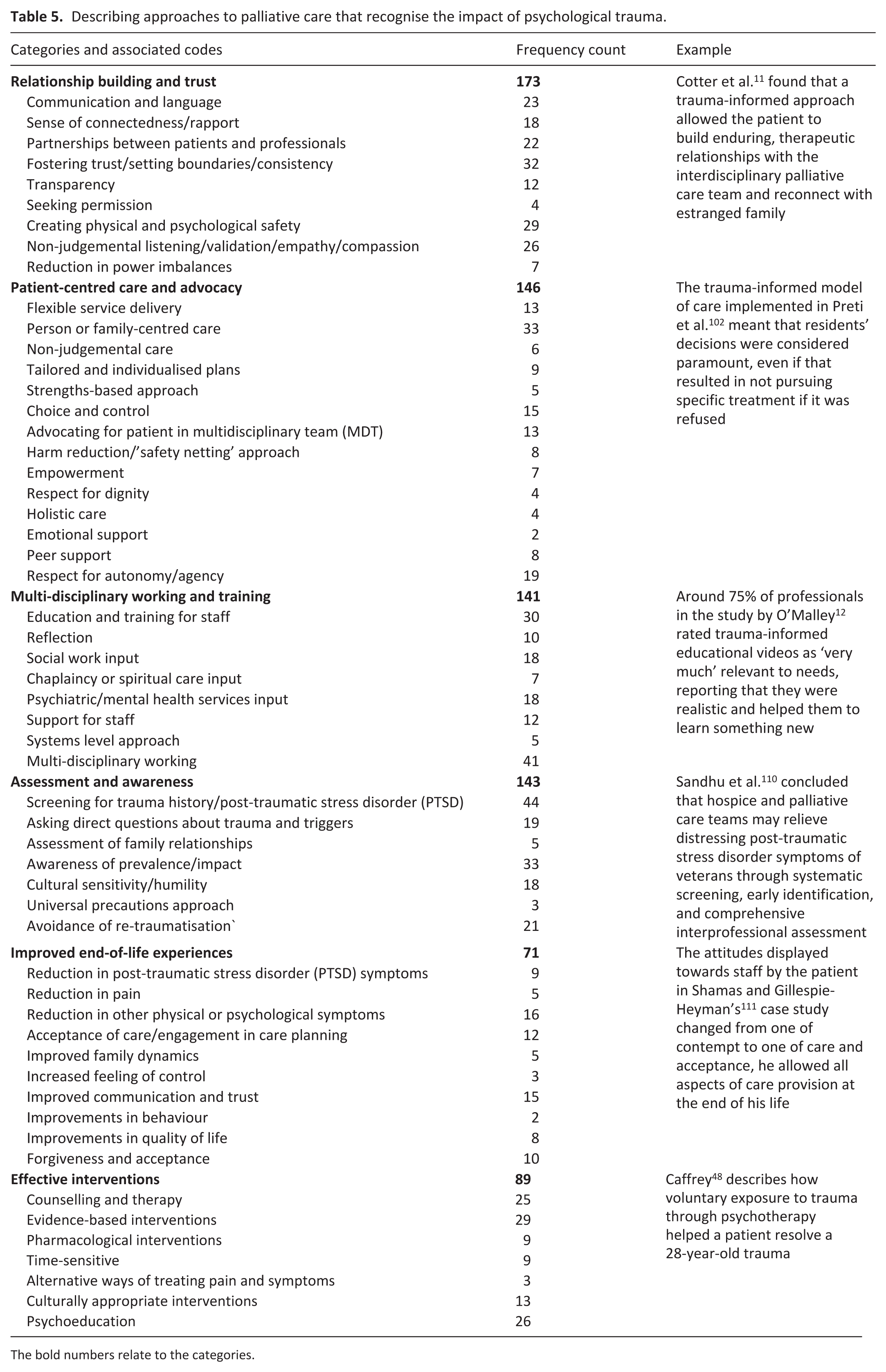

The bold numbers relate to the categories.
Describing challenges to the effective delivery of palliative care that recognises the impact of trauma.
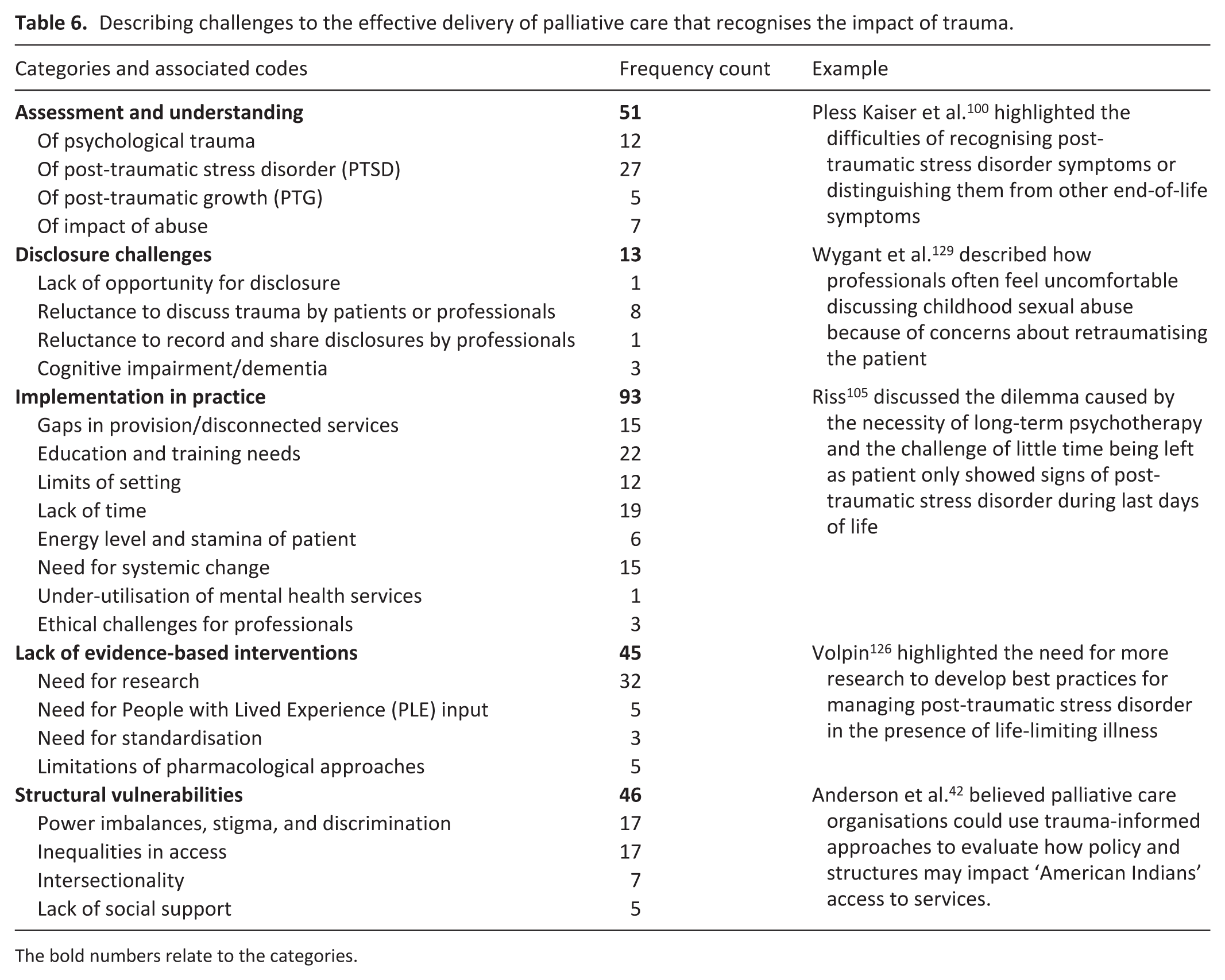
The bold numbers relate to the categories.
How is the impact of psychological trauma at the end-of-life described?
The vast majority of evidence sources (n = 93) described the impact of psychological trauma at the end-of-life, generating 32 codes and six categories (Table 4). After ‘psychological distress’, the most frequent category was ‘resistance to care or treatment’. While five of the six categories focussed on negative impacts, the last, ‘disclosure and perspective’ described potentially positive concepts such as posttraumatic growth.
How are approaches to palliative care that recognise the impact of psychological trauma described?
Thirty-six evidence sources explicitly named or described ‘trauma-informed care’ as a relevant approach to palliative care. Of these, 11 cited the SAMHSA definition 17 and another four implicitly referred to its core concepts (e.g. safety, trustworthiness). Only 20 studies implemented ‘trauma-informed care’, 15 of these were clinical case studies. There was variation in the degree of implementation within the case studies: six papers mapped the principles of trauma-informed care to the described interventions4,7–9,121,123, one used Feldman’s ‘Stepwise Psychosocial Palliative Care’ (SPCC) model 60 as a roadmap for applying the approach, 5 and six described the approach more vaguely.10,61,69,75,83,115 Two case studies were supplementary abstracts that did not provide full details of how trauma-informed principles were utilised.11,122 The other evidence sources implementing ‘trauma-informed care’ were two qualitative studies focussed on the provision of palliative care for people experiencing homelessness,80,102 and three studies (one quantitative, two mixed-methods) examined the effectiveness of trauma-informed training on palliative care professionals.12,82,98 The remaining 16 studies that named or described ‘trauma-informed care’ recommended rather than implemented the approach.
Though only a small proportion of sources explicitly implemented ‘trauma-informed’ palliative care, a far greater number did so implicitly, in the sense that they were implementing palliative care that recognised the impact of psychological trauma. Ninety-three sources provided relevant descriptions that led to the identification of 55 codes and 6 categories (Table 5). The most frequent category was ‘relationship building and trust’, followed by ‘patient-centred care and advocacy’, ‘assessment and awareness’ and ‘multi-disciplinary working and training’.
How are challenges to the effective delivery of palliative care that recognises the impact of trauma described?
Eighty evidence sources described challenges to the effective delivery of palliative care that recognises the impact of trauma. This led to the identification of 24 codes and 5 categories (Table 6). By far the most frequent category was ‘Implementation in Practice’, this included 22 papers describing the need for education and training of staff. Challenges in the assessment and understanding of psychological trauma, post-traumatic stress disorder, post-traumatic growth, and the impact of abuse were described 51 times across papers. Descriptions of challenges related to structural vulnerabilities were captured in codes including ‘inequalities in access’ and ‘power imbalances, stigma, and discrimination’.
Discussion
Main findings
The scoping review identified 99 relevant evidence sources from 13 countries, the majority of which were conducted in the US. Around 40% of sources were clinical case studies of palliative care patients and/or their caregivers. Cancer was the primary diagnosis for the majority of patients in 55 sources. Many sources (n = 24) focussed on veterans; other areas of focus included the lived experiences of homelessness, care and prison systems, childhood abuse, intergenerational trauma, and poverty. Six ways of describing the impact of psychological trauma at the end-of-life were identified, the most frequent after ‘psychological distress’ being ‘resistance to care or treatment’. Few sources (n = 20) implemented trauma-informed care: 15 were clinical case studies and the only three that evaluated its effectiveness did so in relation to staff training and education rather than the experiences of patients or family members. Though trauma-informed palliative care was not always explicitly present, six palliative care approaches to recognising and responding to psychological trauma, and five main challenges to its effective implementation, were identified.
What this review adds
As far as can be determined, this is the first systematic scoping review of evidence sources around trauma-informed palliative care. Given the relative lack of evidence about effectiveness, it echoes the call from practitioners and researchers to build a stronger evidence base for this approach. 2 A substantial body of international studies that describe concepts relevant to the conceptualisation and implementation of trauma-informed palliative care have been identified.
The review identified a wide range of traumatic experiences that may impact the end-of-life experience. At the same time, given the prominence of cancer patients and veterans, the results do not fully represent the wider palliative care population. It is important that future studies on trauma-informed palliative care do not generalise findings from these sub-groups and strive for wider coverage. 5 As some authors have noted, trauma arising from different sources may correlate with different impacts, suggesting that a standardised framework may not be appropriate.55,103 Many evidence sources in this review focussed on post-traumatic stress disorder (PTSD). However, past trauma is associated with a range of psychological difficulties aside from PTSD that may impact the end-of-life experience, for example depression, dissociative identity disorder, and psychosis.56,131 Among these disorders, PTSD is an outlier in the sense that a tangible traumatic event must be named in order for a diagnosis to be made. 22 Given that the use of diagnostic categories is now contested in some international contexts, including the UK, 132 it is worth questioning if there is an over-emphasis on PTSD in the trauma-informed palliative care literature. At the very least, there is an argument to move away from using structured clinical interviews and self-report questionnaires to access for PTSD in palliative care populations. Aside from the recognised limitations of these approaches in general,133,134 PTSD may present differently at the end of life. In one focus group study, the descriptions of symptoms experienced by veterans receiving palliative care broadly aligned with existing DSM-5 criteria for post-traumatic stress, but ‘revealed specific presentations relevant to the end of life setting such as resistance to care, agitation, restlessness, and effects of delirium’ (p. 205). 100 Other evidence sources emphasised the importance of narrative approaches that could facilitate disclosure of trauma and help patients reconcile with its impact at the end-of-life.79,113,130 There is a need for palliative care services to develop and evaluate assessment tools that can capture a broader understanding of psychological trauma.
Some features of the psychological trauma identified in this review, such as resistance to care, reflect similar points raised in discussion papers advocating for trauma-informed palliative care. However, the basic qualitative content analysis also highlighted aspects of trauma-informed care not considered in previous papers, namely the potential positive impacts of psychological trauma on the end-of-life experience. These include post-traumatic growth,44,48,54,87,89,90,120,130 terminal illness acknowledgement, 70 and an openness to discuss end of life wishes. 70 According to theories of post-traumatic growth, depending on their specific circumstances, some people who experience trauma may respond with an improved sense of self or ability to relate to others. 135 While these positive changes can often co-exist with negative responses, 136 the possibility that people may engage more rather than less with palliative care services and providers should not be ignored. As Mystakidou et al. comment, ‘. . . an exclusive focus on the negative effects of trauma may influence how therapists approach clients and how clients see themselves, leading both to ignore the positive changes that may result from traumatic life-events’ (p. 664). 89 These insights do not detract from any arguments calling for the implementation of trauma-informed palliative care but serve as a reminder to avoid overly pathologizing those who may receive it.
Within this review, the descriptions of palliative care that recognise the impact of psychological trauma highlight both a challenge and an opportunity for those wishing to create a fully conceptualised model of trauma-informed palliative care. The challenge will be finding a way to organise the Venn diagram of concepts that has emerged. Many of the descriptions in the identified evidence sources mirror the principles of trauma-informed care as set out by the US Substance Abuse and Mental Health Administration (e.g. ‘creating psychological and physical safety’, ‘fostering trust’, ‘choice and control’) as well as general principles of palliative care (e.g. ‘person-centred’, ‘holistic’ and ‘multi-disciplinary’). At the same time, there are additional descriptions that might distinguish trauma-informed palliative care from trauma-informed care in general (e.g. ‘time-sensitive’) as well as palliative care in general (e.g. ‘screening for trauma history’). Any meaningful conceptualisation will need to carefully consider these overlaps and divergences. There is an opportunity, however, to carve out a distinct and meaningful position for trauma-informed palliative care. It is widely recognised that contemporary palliative care, for all its successes, has not yet fully addressed issues around inequalities in access. 137 Many of the evidence sources in this review described the impact of psychological trauma on those experiencing structural vulnerabilities. This presents a possibility to conceptualise trauma-informed palliative care as a way for existing services to better engage with groups they have traditionally been unable to reach in the past. However, evidence to support this positioning is currently lacking. This is clear from the results of this scoping review: beyond the subjective observations made in clinical case studies, the only identified papers evaluating the effectiveness of trauma-informed palliative care were three evidence sources examining the impact of education and training on professionals. Research that evaluates the impact of trauma-informed palliative care on end-of-life experiences is needed. Future studies may want to consider employing outcomes currently used in the evaluation of general palliative care such as quality of life, avoiding crises, and effective care transitions.
This review highlights a number of obstacles to integrating trauma-informed practices into existing palliative care service. In theory, the many overlaps between trauma-informed care and good palliative care should mean that ‘(w)hen trauma is recognised by a hospice and palliative care team, enacting the principles. . . should be seamless’. 9 (p.331) In reality, the identified evidence sources described a wide variety of implementation challenges. It is particularly important to note the trauma-informed challenges that are unique to the palliative care setting, such as the fact that distressing symptoms of psychological trauma may emerge in the last days of life without having shown any previous expression, and that other conditions at the end of life, such as dementia, might conceal its diagnosis. 105 The lack of time as well as the physical capacity of patients to engage means that trauma-informed palliative care has to be realistic in its goals and adapt its interventions. Regarding resources, it cannot be assumed that palliative care services are in a position to effectively implement trauma-informed care. To offer one example: 18 of the identified evidence sources cited social work input in their descriptions of palliative care that recognises the impact of psychological trauma. This is not surprising given that 14 of the papers were authored by social work practitioners or researchers. However, it is important to recognise that social work roles and qualifications vary internationally. This review was dominated by evidence sources from North America, a continent where licenced clinical social workers are considered to be qualified mental health professionals who can diagnose and treat mental health and behavioural conditions and provide services such as counselling and psychotherapy.138,139 In other settings, including the UK, these responsibilities fall outside of the social work remit and may not be a standardised part of palliative care services. Potential limitations such as these need to be properly considered; as Ricks-Aherne et al. note, ‘self-assessment of capacity is essential for organisational level implementation of trauma-informed care’. 5 (p.326)
Strengths and weaknesses/limitations of the study
The broad inclusion criteria allowed by this scoping review allowed for the identification of a substantial number of evidence sources. While this is a strength in terms of comprehensiveness, it also leads to limitations. The highly heterogeneous nature of evidence sources created challenges when analysing the data: as an example, codes found in one-person clinical case studies were given equal weight to those found in quantitative studies investigating tens of thousands of patients. In addition, it was sometimes difficult to distinguish descriptions of ‘good palliative care’ from descriptions of palliative care that recognises the impact of psychological trauma, for example when reporting codes such as ‘emotional support’ or ‘psychoeducation’. The findings may therefore potentially overemphasise the need to focus specifically on psychological trauma rather than viewing this as a natural subset of the ‘holistic’ approach that palliative care services wish to provide. The wide inclusion criteria may also have impacted the extent to which the review’s aims were achieved. Other approaches, such as a qualitative review focussed on the thematic analysis of clinical case studies, may have helped produce more specific findings.
Conclusion
Trauma-informed palliative care is an emerging field that is receiving increasing attention and support from palliative care professionals. This scoping review identified a substantial body of international evidence sources that describe concepts that align with those put forth in discussion papers advocating for a trauma-informed approach to palliative care. At the same time, it highlighted areas that these papers did not, including the potentially positive impacts of previous trauma on the end-of-life experience.
It is clear that more research is needed before trauma-informed palliative care can be fully conceptualised and implemented. There is a need to look beyond advanced cancer, veterans, and post-traumatic stress disorder, and to consider the most effective way to evaluate the prevalence and impact of psychological trauma. Conceptualising trauma-informed palliative care will require an appreciation of how it may differ from general trauma-informed care approaches, as well as how it overlaps with existing principles of palliative care. Implementing trauma-informed palliative care will require an appreciation of the resources and time it requires within the limits of palliative care patients and settings. These tasks are not straight-forward, but they are worth pursuing, especially given the potential of trauma-informed palliative care to improve the end-of-life experience for those living and dying with structural vulnerabilities. The results of this scoping review provide a valuable starting point for the design and realisation of future studies in this area.
Supplemental Material
sj-xlsx-1-pmj-10.1177_02692163261425837 – Supplemental material for Trauma-informed palliative care: A systematic scoping review of evidence sources describing concepts relevant to an emerging field of practice
Supplemental material, sj-xlsx-1-pmj-10.1177_02692163261425837 for Trauma-informed palliative care: A systematic scoping review of evidence sources describing concepts relevant to an emerging field of practice by Rebecca Salama, Jane Simpson, Fiona J. R. Eccles and Maddy French in Palliative Medicine
Footnotes
Ethical considerations
Research ethics committee approval was not required for this scoping review.
Consent to publication
The research team consent to open access publication so that the findings are readily accessible to healthcare professionals, policy and decision-makers, and the public.
Author contributions
RS developed the study protocol, completed the search process, extracted and analysed data, and wrote the manuscript. JS, FE, and MF reviewed the study protocol and reviewed, edited, and approved the final version of the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The corresponding author (RS) receives a PhD studentship provided by the Faculty of Health and Medicine at Lancaster University.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
