Abstract
Background:
High-quality evidence suggests that specialist palliative care reduces the odds of dying in hospital. The economic implications have not been established.
Aim:
To evaluate the cost-effectiveness of home- and hospital-based specialist palliative care for adults with poor prognosis in England.
Design:
Health-economic decision-modelling using five-state Markov cohort models with a 24-h cycle and lifetime horizon.
Setting/participants:
We evaluated home- and hospital-based care separately. We modelled counterfactuals using Cochrane review evidence of treatment effects on place of death and quality of life. We estimated place of death distributions, utilisation, quality-adjusted life years, and unit and intervention costs from the literature.
Results:
Home-based care was associated with reduced costs of £7908 per person (95% confidence interval: −18,044 to 395) and increased quality-adjusted life years by 0.035 per person (0.033 to 0.037). Hospital-based care reduced costs by £6480 per person (−11,482 to −1671) and increased quality-adjusted life years by 0.033 per person (0.031 to 0.035). We estimated that for England in 2022, specialist palliative care supported over 20,000 people to die outside of hospital, saved approximately 1.5 million hospital bed days and reduced system expenditures by £817 million.
Conclusion:
Specialist palliative care reduces hospital bed days, deaths in hospital and healthcare costs, as well as improving quality of life, among adults in England. A minority who might benefit currently receive specialist palliative care and needs are growing rapidly. Expanding access may yield further gains, but bridging current gaps in access also requires new approaches to reaching and meeting the needs of underserved groups.
Specialist palliative care increases odds of dying outside hospital and improves patient quality of life, but this is a complex intervention and not all who might benefit receive specialist care.
Cost-effectiveness of specialist palliative care, and the economic implications of reduced hospital deaths, is a persistent question for research and policy. Prior systematic reviews identify a lack of modelling studies as a fundamental evidence gap.
We used decision modelling, a widely-used method in health economics that has not been routinely applied in evaluating palliative care. The key strength of this approach is the capacity to combine data from different sources to estimate cost-effectiveness when there is insufficient trial data to answer the question.
We found that both hospital-based specialist palliative care and home-based specialist palliative care for adults in England represent excellent value care, reducing the average cost per patient to the NHS while improving patient outcomes.
Specialist palliative care is currently accessed by less than half of people who might benefit in England. Expanding access would likely yield further cost-savings and improve outcomes for patients and families. However, mitigating current inequities in access and outcomes also requires new approaches to identifying, engaging and meeting the needs of underserved groups.
Other countries interested in applying these methods to their own data and services can consider using our methodological templates, which we have published open access.
Introduction
Background
Less than 1% of people die in high-income countries annually but this group accounts for 8%–10% of healthcare spending.1,2 Expenditures are primarily driven by acute hospital admissions and often yield poor value with widespread prevalence of potentially modifiable problems including unmanaged symptoms and fragmented care.3,4 People with serious medical illness largely prefer to be at home if adequate supports are available, 5 but most in high-income countries visit hospital in the last months of life and hospital is the most common place of death.3,4,6
Care for serious medical illness is provided by a range of intersecting health and social care providers. Specialist palliative care – defined as care for those with more complex needs which cannot be met by their primary or ‘core’ team alone, requiring a workforce with specialist skills and experience delivering palliative care as their main role 7 – is one intervention which may improve outcomes.8,9 In England, less than half of people who die from a non-sudden cause get specialist palliative care. 3
Economic evidence to inform improvement efforts is thin. 10 Primary studies are often underpowered for economic evaluation.10–12 There is potential for decision-modelling, combining evidence from a range of sources, to answer policy questions where primary data are insufficient.13,14 Systematic reviews of economic evaluations of palliative care specifically identify a lack of modelling studies as a key weakness in the evidence base.10,15
Objectives
To estimate the cost-effectiveness of home- and hospital-based specialist palliative care for adults in England.
Methods
Study design and intervention
This was an economic modelling study combining data on mortality, place of death, care utilisation, unit costs, quality of life, specialist palliative care receipt and treatment effect estimates. We chose cohort models as appropriate given study resources and data availability. 16 This study evaluated two models of specialist palliative care: at home, and in acute hospital. We evaluated each model of care separately as insufficient data were available on treatment effects for concurrent receipt of hospital and home specialist palliative care.
Specialist palliative care in England is delivered by multi-disciplinary teams comprising consultants, staff-grade doctors, specialist nurses and allied health professionals. 7 Teams specifically support patients with specialist palliative care needs, including complex symptom management, psychosocial concerns, advance care planning and training and support of the wider workforce in health and social care. We compared receipt of specialist palliative care to not receiving specialist palliative care, sometimes called usual care. Since treatment effect estimates are drawn from Cochrane reviews, we interpret our main results as reflecting timely, systematic care for an individual.
Population and setting
People with progressive life-limiting illness may benefit from palliative care at different points in their illness.7,17 Specialist palliative care is predominantly delivered in the last 3–6 months of life.18,19 We defined our study population as community-dwelling adults in England, where a clinician would not be surprised if they died in the next 3 months.18–20 We distinguished two analytic cohorts: those living at home (and so candidates for home/community palliative care), and those admitted to hospital (and so candidates for hospital palliative care). We excluded those living permanently in care homes as having different characteristics and patterns of care. 21 For population estimates on numbers of people and places of death, the most recently identified data came from 2022. 22
Model rationale and characteristics
Descriptive data on healthcare use and mortality are collected widely in high-income countries. Cochrane reviews found that both home- and hospital-based models of specialist palliative care significantly reduced the odds of dying in hospital.8,9 Interventions that reduce deaths in hospital are by definition also affecting time in hospital near end of life, but cost-effectiveness implications have not been explored.
If we have good evidence on where people spend time near end of life, their place of death and to what extent specialist palliative care affects this place of death, then we can combine these data to model patient flow between different places near end of life, and estimate the associated costs and outcomes with and without receipt of timely specialist palliative care. Based on meta-analysis of trial data for people with advanced illness, 23 we assumed that specialist palliative care does not affect survival in either direction and fixed survival across treatment counterfactuals so all differences in outcome reflect different time in different places and never differential survival.
We conducted the modelling in seven steps, detailed in the Supplemental Appendix. All but the first step were undertaken separately for each analytic cohort. First, we conceptualised a cohort Markov model with five states and a 24-h time cycle (Figure 1). The live states were defined as physical locations that adults with serious illness in England spend time: home, hospital, care home and hospice. Each of these locations has different cost and quality of life implications, and approximately 98% of deaths occur in one of these places. 22 At the start of each simulation, 100% of the cohort is in the place the intervention occurs: home for home-based care, hospital for hospital-based care. From that point on, the cohort can move between places (and die in any place) as indicated by Figure 1. In the UK context for seriously-ill adults, a hospice is a facility focused on providing specialist palliative care and a care home is a facility providing residential care with expert nursing support.
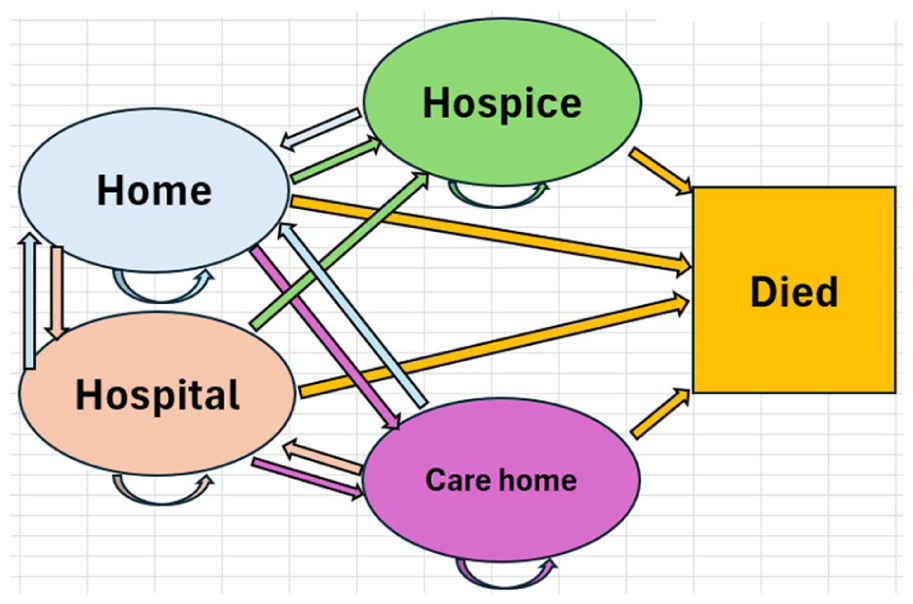
Overview of Markov model structure (24-h cycle).
Second, we identified cost and outcome parameters for each state. Third, we specified survival curves. Fourth, we estimated place of death, both for all relevant adults together and stratified by receipt of specialist palliative care. Fifth, we estimated admissions to hospital, care home and hospice, and bed days in each of these places, incorporating both survival and proximity-to-death effects. Sixth, we developed the models. We estimated transition probabilities that delivered model outcomes consistent with the place of death and healthcare utilisation estimated in the prior two steps. In estimating counterfactuals, we allowed treatment status to affect only transition probabilities from the place of care, holding all other parts of the model constant. Seventh, we combined model outputs with outcome parameters to derive results.
Measurement of quality of life, and valuation of resources and costs
We sought papers measuring health-related quality of life in older people in the UK with palliative care needs, using EuroQoL EQ5D5L. 24 We estimated quality-adjusted life years (QALYs) and quantified treatment effects as incremental cost-effectiveness ratios (ICERs). For resource use in institutions, we combined frequency data with unit costs (UK pounds (£), 2022). To estimate the formal costs associated with being at home, we combined frequency data and unit costs for outpatient care, primary care, and district and community nursing. 1 We estimated informal care costs using the substitution method for a community-based home care worker. 2 Where costs were identified for a year other than 2022, we adjusted using the UK Consumer Price Index (Health). 25
Treatment effects on quality of life and costs
We modelled two additional mechanisms by which specialist palliative care affects outcomes compared to usual care only:
Perspective, time horizon and discount rate
In primary analysis, we estimated formal care costs from the payer perspective. In secondary analysis we combined formal costs with informal care costs. We estimated QALYs from the patient perspective. We combined effects on costs and QALYs to estimate ICERs, interpreting these in the context of a willingness to pay of £25,000 to £35,000 per QALY. 28 We imposed a lifetime horizon, with a discount rate of 3.5%. 29
Uncertainty and additional analyses
In primary analyses, we applied the odds ratios of treatment effect on place of death and their 95% confidence intervals,8,9 generating estimated time in each place for those receiving specialist palliative care and those not. Combining these estimates of time in place with the relevant sets of unit costs and QALY values generates an average, lower and upper limit of the estimated effect on costs and QALYs, and the associated ICER.
In our secondary analyses, we repeated the primary analyses but added unpaid family care to the cost of being at home. This analysis quantifies the extent to which observed savings for the system are displaced to the household. In sensitivity analyses, we checked robustness of our primary results to purposively identified limitations in our data: the cost of a day in acute hospital, the cost of the intervention itself and uncertain QALY effects.
To quantify the estimated effects at the population level, we combined primary results with population-level need and specialist palliative care receipt. Since our primary analysis estimates treatment effects per clinical trials, that is, care provided in a systematic and timely way from a well-defined baseline, but real-world care provision occurs in a less coherent fashion with some patients receiving timely care and others receiving care very late in the disease trajectory, 18 we incorporated linear dose effects with a range from our primary analysis results (i.e. timely care) and zero (i.e. too late to have any effect).
Results
Study parameters
Untreated cost and outcome parameters
Estimated inputs by location/state in any untreated scenario are presented in Table 1.
Study parameters: cost and QALY inputs, base case, home- and hospital-based care evaluations.
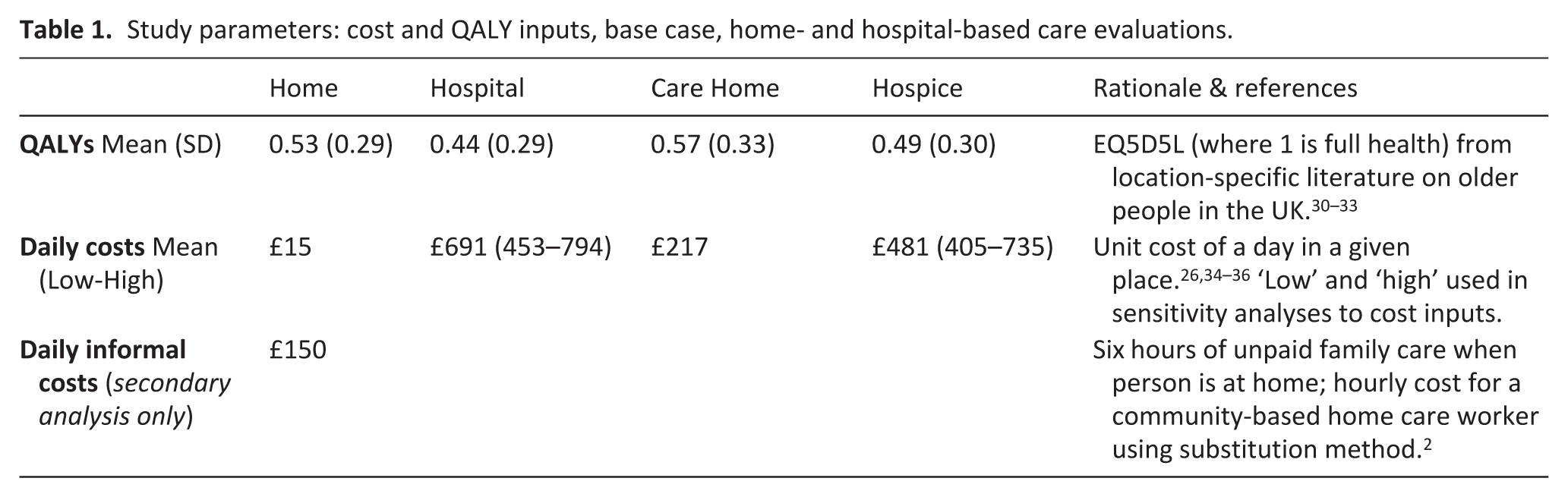
Informal costs were not estimated for hospital, care home and hospice; care in these places was assumed to be wholly provided by professional staff. For underlying data and references, see Supplemental Appendix.
Counterfactual treatment effect estimates
The parameters for how interventions changed outcomes are summarised in Table 2. Less than half of people living in the community near end of life whose death was expected received home specialist palliative care, and less than half of those admitted to hospital received hospital-based care. Cochrane review and other meta-analysed trial evidence found that home-based care increased the odds of dying in own home or hospice, and decreased the odds of dying in hospital or a care home. 9 Hospital specialist palliative care was found to increase odds of dying at home but evidence on dying in other places was not clear. 8 Both models of care were estimated to improve quality of life and we incorporated intervention costs per day in the place where care is provided.
Study parameters: Treatment prevalence and effect estimates.
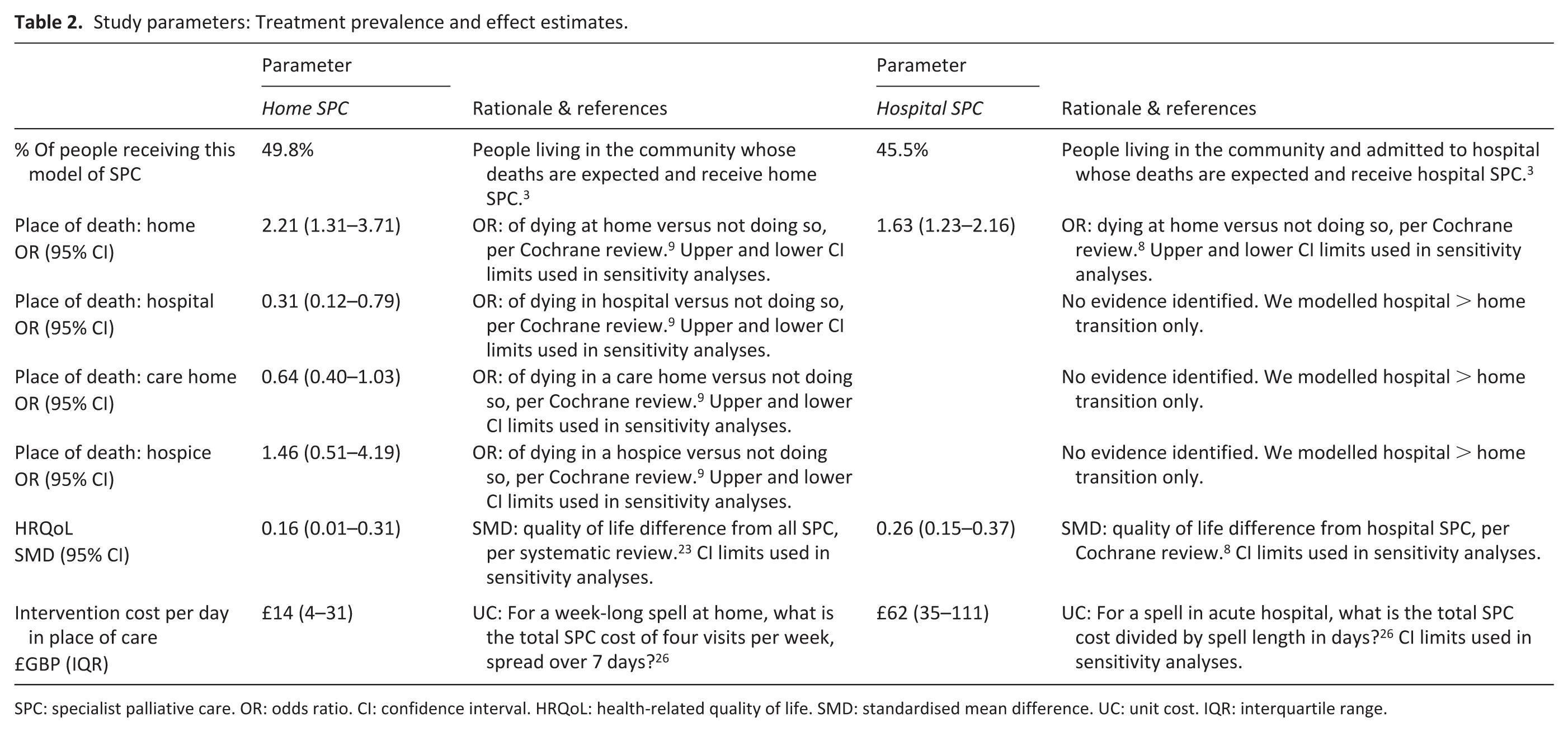
SPC: specialist palliative care. OR: odds ratio. CI: confidence interval. HRQoL: health-related quality of life. SMD: standardised mean difference. UC: unit cost. IQR: interquartile range.
Summary of main results
Main results are presented in Table 3.
Primary results.
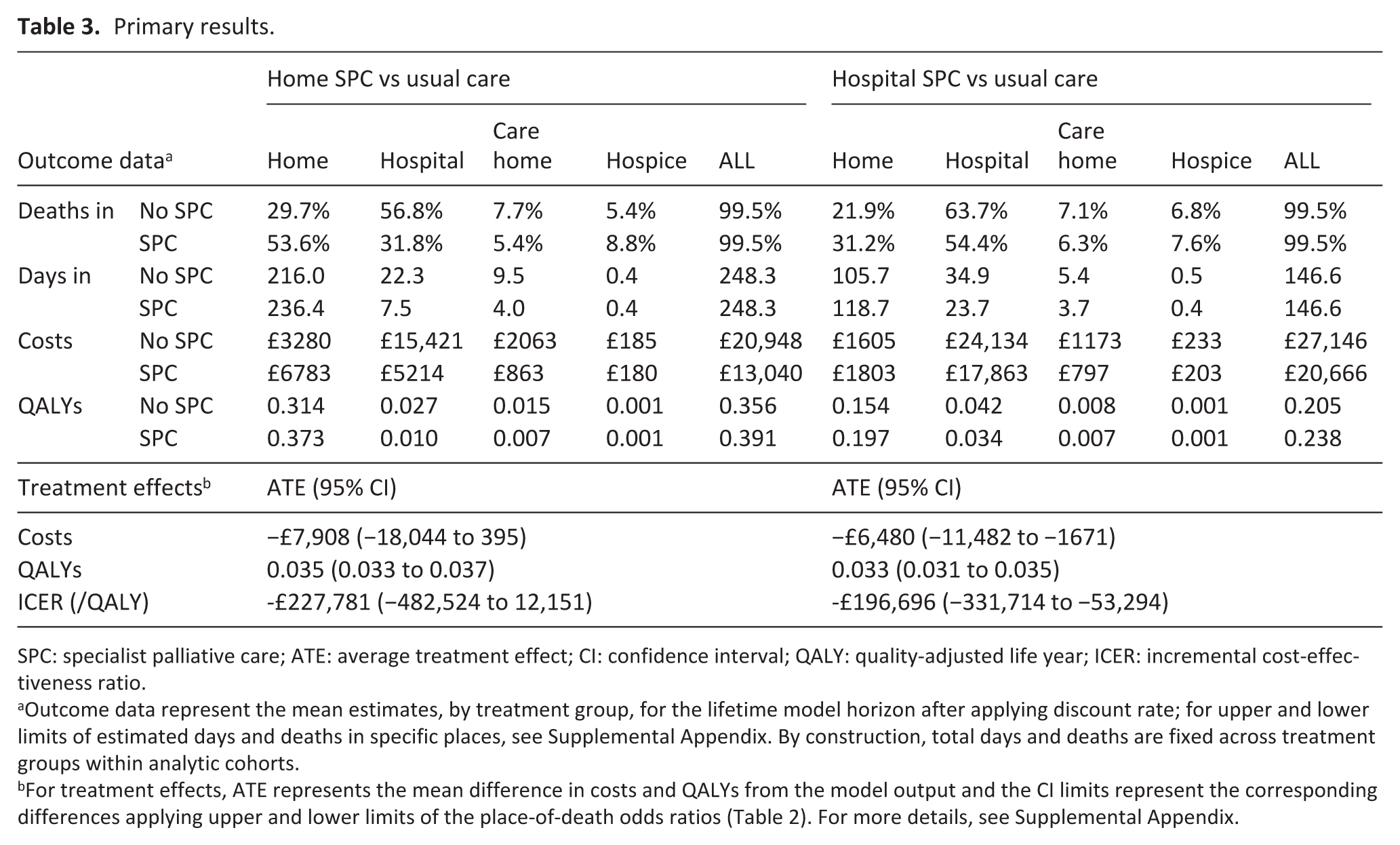
SPC: specialist palliative care; ATE: average treatment effect; CI: confidence interval; QALY: quality-adjusted life year; ICER: incremental cost-effectiveness ratio.
Outcome data represent the mean estimates, by treatment group, for the lifetime model horizon after applying discount rate; for upper and lower limits of estimated days and deaths in specific places, see Supplemental Appendix. By construction, total days and deaths are fixed across treatment groups within analytic cohorts.
For treatment effects, ATE represents the mean difference in costs and QALYs from the model output and the CI limits represent the corresponding differences applying upper and lower limits of the place-of-death odds ratios (Table 2). For more details, see Supplemental Appendix.
We estimated that, in reducing the odds of dying in hospital, formal costs were £7908 lower for home palliative care patients than usual care patients (95% CI: −18,044 to 395), while QALYs were higher by 0.035 (95% CI: 0.033 to 0.037). The corresponding ICER was −£227,781 per QALY (95% CI: −482,524 to 12,151). Total formal costs were £6480 lower for hospital palliative care patients than usual care patients (95% CI: −11,482 to −1671), while QALYs were higher by 0.033 (95% CI: 0.031 to 0.035). The corresponding ICERs were negative across the confidence interval, indicating that palliative care dominated usual care.
For both models, the estimated cost-savings come from reductions in acute hospital bed days and, to a lesser extent, reduced care home bed days. Increased costs associated with being at home are more than offset by the money saved by reduced time in hospital. QALY improvements are driven both by palliative care’s effect on outcome, and on the lower QALYs associated with being in hospital compared to being in other places.
Summary of secondary analysis
Secondary results, where the cost variable incorporates costs from the caregiver perspective, are presented in Table 4. In both cases, overall estimated effect on costs was smaller than in primary analysis, reflecting how palliative care increases days at home versus hospital, but results were substantively unaffected. At the mean, both models of care dominated the usual care comparator with negative ICERs.
Secondary analyses: Treatment effects of hospital and home SPC, including informal care costs.
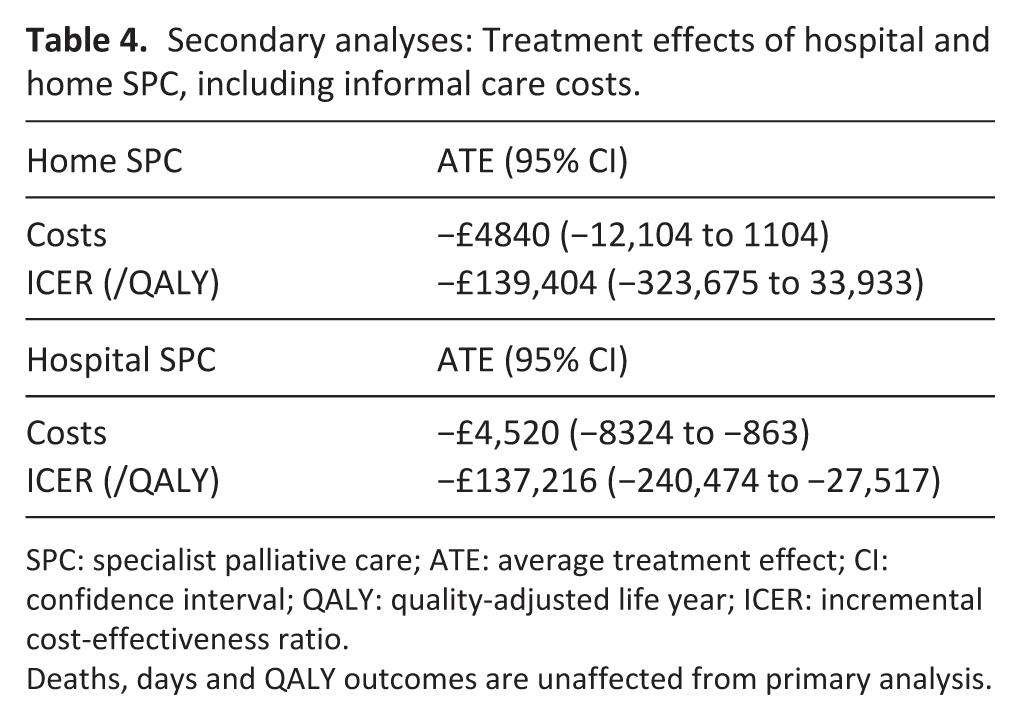
SPC: specialist palliative care; ATE: average treatment effect; CI: confidence interval; QALY: quality-adjusted life year; ICER: incremental cost-effectiveness ratio.
Deaths, days and QALY outcomes are unaffected from primary analysis.
Effect of uncertainty
We reran our primary analyses to test assumptions to the cost of a day in acute hospital; intervention costs; and the co-occurring uncertainty of QoL effects alongside place-of-death effects. Results were substantively unaffected at the mean. See Supplemental Appendix for further details.
Population-level estimates
The population-level implications of our results, combining primary analysis estimates with the number of people estimating to be receiving specialist palliative care, for the calendar year 2022 are presented in Table 5. We estimated that home-based care resulted in 17,098 fewer deaths in hospital (95% CI: −30,681 to −2985), 1.0 million fewer bed days (95% CI: −1.9 to −244,164 million) and £533.1 million lower costs for the NHS (95% CI: −1.2 billion to 31.2 million). We estimated that hospital-based care resulted in 3906 (95% CI: 6269 to −1627) fewer deaths in hospital, 491,601 fewer bed days (95% CI: −789,873 to −205,748) and £283.9 million lower costs for the NHS (95% CI: −503.4 to −73.5 million).
Population-level estimates: Treatment effects of home and home SPC on hospital deaths, bed days and healthcare costs in England annually (2022).
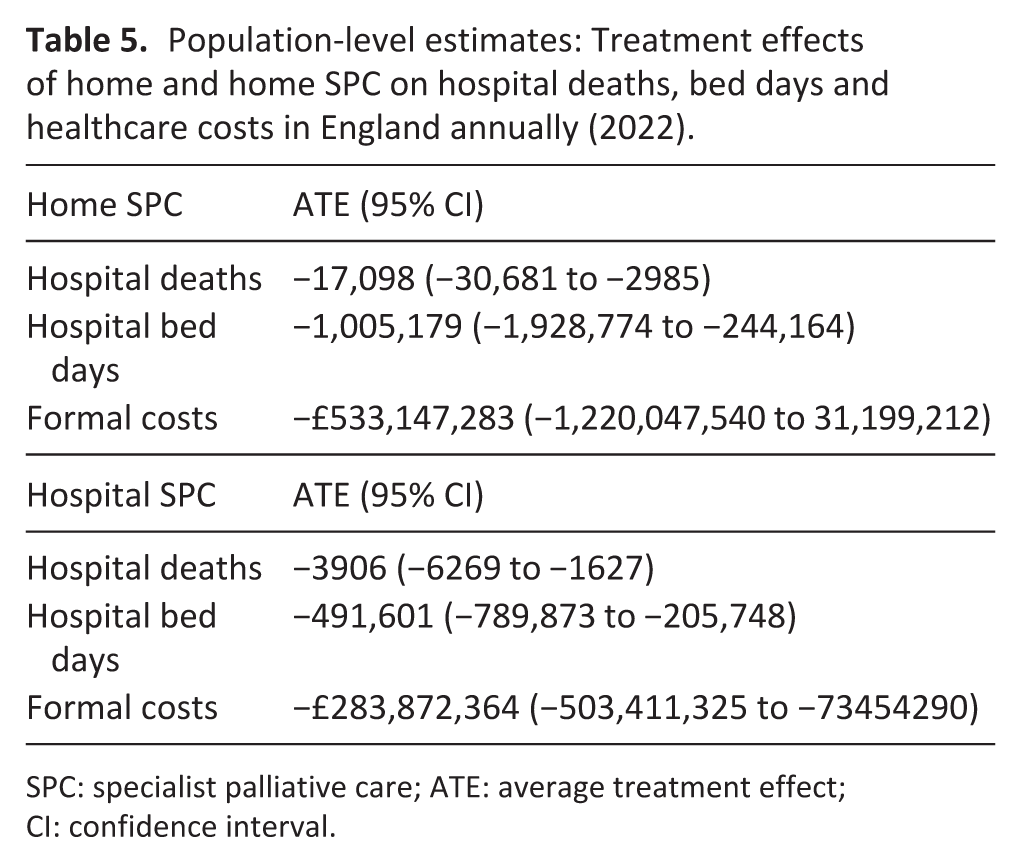
SPC: specialist palliative care; ATE: average treatment effect; CI: confidence interval.
Discussion
Key findings
This economic modelling exercise to estimate cost-effectiveness of home- and hospital-based care found that in both cases specialist palliative care represents very good value for patients and decision-makers. Observed cost-effects were realised primarily by reduced days in acute hospital. QALY improvements arose both from palliative care improving this outcome and by higher QALYs associated with places other than hospital. Including informal care costs reduced the estimated cost-effectiveness ratio as caregiver hours increase with time spent at home, but key conclusions were substantively unaffected. Combining our primary analysis with population-level estimates of palliative care need and receipt suggests that each year in England these two models of palliative care support over 20,000 people to die outside of hospital, save approximately 1.5 million NHS bed days and reduce system expenditures by £817 million.
What this study adds
Causal evidence of effects on place of death and quality of life is long established,8,9 but – to the best of our knowledge – this study is the first to examine the economic implications. 10 This paper therefore represents the best available evidence of the cost-effectiveness of specialist palliative care for adults in England, and quantifies for the first time the improvements in care and associated cost-savings. At a time when there is widespread unmet need, 37 and growing needs due to population ageing, 38 this evidence can inform planning to meet needs, curb cost growth and promote good-value care.
Since a minority of people who might benefit currently receive specialist palliative care, it is likely that in the short term expanding access would yield further cost-savings and quality improvements. However, given well-established inequities in access and outcomes, 39 meeting current needs also requires new approaches to identifying, engaging and meeting the needs of underserved groups. 40 In the long term, as the population ages, meeting needs will require significant expansion of the specialist workforce. It is important to consider delivery of palliative and end-of-life care by primary or ‘core’ teams, and how the range of intersecting primary and specialist providers can work most effectively together.
The challenges of providing good end-of-life care during a century of demographic ageing are not unique to England,41,42 and other countries can adapt and extend our approach to their own contexts and data. To this end, all modelling materials are provided in the Supplemental Appendix.
Strengths and limitations of the study
The strength of this study is that it combines high-quality data from multiple sources to derive credible evidence of cost-effectiveness on interventions that previously have not been subject to widespread economic evaluation. This method harnesses the best available data on specialist palliative care through Cochrane reviews while eliding limitations of other approaches to economic evaluation such as within a clinical trial (when sample size and time horizon are typically insufficient 11 ), or observational data (which face challenges of bias 43 and prospective identification of a sample44,45). Hospital palliative care dominated the usual care comparator in primary analysis. In the home-based evaluation, in the most pessimistic scenario from the formal cost perspective, expenditures increased slightly but the corresponding ICER (£12,151 per QALY) was well inside the threshold for funding.
The most important limitation is that we used aggregate, population-level data in a cohort model. 16 There is good evidence that patient quality of life, 46 care costs, 47 intervention costs, 26 patient preferences, 5 and treatment effects on outcomes18,48 all vary by myriad factors including diagnosis, phase of illness, beliefs, household conditions, palliative care dose and supply-side factors. In particular, the timing of palliative care and related dose effects are central to cost-effectiveness and clinical efficacy,49,50 and we lack a clear relationship between timing and treatment effect estimates to model that more precisely. A second key assumption is that Cochrane evidence on place-of-death effects is ‘true’ for our population; trial evidence is noted for internal validity but not always generalisability. We modelled effects on NHS costs with a sensitivity analysis incorporating informal costs, but some costs in the model are borne by third sector providers – particularly hospice and care home days.
It follows that this study should be the start and not the end of decision models that identify how and for whom specialist palliative care makes the biggest difference, addressing ex ante specific decision problems for policy, both so that services can optimise allocation of current limited capacity and plan for meeting future needs. Such analyses will optimally use individual-level data and dynamic modelling that allow for more thorough exploration of the demand- and supply-side heterogeneity. While we tested results to key hypothesised parameter uncertainties, we identified other potential uncertainties beyond the scope of our exercise that could be addressed with individual-level data (e.g. survival curves by age and sex; differences in quality-of-life trajectories by location, independent of treatment; unit costs associated with proximity to death or death in an institution; diminishing cost-effectiveness of the intervention as some people prefer not to leave hospital for home; relationship between proximity to death and treatment effect on place of death). Incorporating these uncertainties into future work is essential to appropriately meeting the needs of the more-than-half of people in England who might benefit from specialist palliative care but currently do not receive it.
Conclusion
This economic modelling study found that specialist palliative care reduces hospital bed days, deaths in hospital and healthcare costs, as well as improving quality of life, among adults in England. Future research should adapt and extend these findings to other countries and settings. Using individual-level data will allow for incorporation of demand- and supply-side heterogeneity, addressing specific decision problems for policy.
Supplemental Material
sj-docx-1-pmj-10.1177_02692163261423755 – Supplemental material for Specialist palliative care improves patient experience, reduces bed days and saves money: An economic modelling study of home- and hospital-based care
Supplemental material, sj-docx-1-pmj-10.1177_02692163261423755 for Specialist palliative care improves patient experience, reduces bed days and saves money: An economic modelling study of home- and hospital-based care by Peter May, Elham Nikram, Therese Johansson, Gemma Clarke, Sarah Mitchell, Irene J. Higginson, Katherine E. Sleeman and Fliss E. M. Murtagh in Palliative Medicine
Footnotes
ORCID iDs
Ethical considerations
This study uses only published literature and aggregate data, and as such ethics approval was not required.
Consent to participate
There were no participants in this study, which uses only published literature and aggregate data.
Author contributions
PM, KES and FEMM conceived and designed the study. PM, TJ, GC and FEMM acquired the data. PM and EN analysed the data. PM, SM, IJH, KES and FEMM interpreted the data. PM drafted the initial paper; all other authors revised the draft critically for important intellectual content and approved the version to be published. All authors have participated sufficiently in the work to take public responsibility for appropriate portions of the content.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work is funded through the National Institute for Health and Care Research (NIHR) Policy Research Unit in Palliative and end of life care [reference NIHR206122]. The views expressed are those of the author(s) and not necessarily those of the NIHR or the Department of Health and Social Care. Fliss EM Murtagh is a NIHR Senior Investigator. Katherine E Sleeman is the Laing Galazka Chair in palliative care at King’s College London, funded by an endowment from Cicely Saunders International and the Kirby Laing Foundation.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Methodological detail is provided in the accompanying Appendix, and all underlying data have been made publicly available on Open Science Framework (osf.io/knw9v).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
