Abstract
Background:
In the context of limited resources, evidence on costs and cost-effectiveness of alternative methods of delivering health-care services is increasingly important to facilitate appropriate resource allocation. Palliative care services have been expanding worldwide with the aim of improving the experience of patients with terminal illness at the end of life through better symptom control, coordination of care and improved communication between professionals and the patient and family.
Aim:
To present results from a comprehensive literature review of available international evidence on the costs and cost-effectiveness of palliative care interventions in any setting (e.g. hospital-based, home-based and hospice care) over the period 2002–2011.
Design:
Key bibliographic and review databases were searched. Quality of retrieved papers was assessed against a set of 31 indicators developed for this review.
Data Sources:
PubMed, EURONHEED, the Applied Social Sciences Index and the Cochrane library of databases.
Results:
A total of 46 papers met the criteria for inclusion in the review, examining the cost and/or utilisation implications of a palliative care intervention with some form of comparator. The main focus of these studies was on direct costs with little focus on informal care or out-of-pocket costs. The overall quality of the studies is mixed, although a number of cohort studies do undertake multivariate regression analysis.
Conclusion:
Despite wide variation in study type, characteristic and study quality, there are consistent patterns in the results. Palliative care is most frequently found to be less costly relative to comparator groups, and in most cases, the difference in cost is statistically significant.
Introduction
In the context of limited resources, evidence on costs and cost-effectiveness of alternative methods of delivering health-care services is increasingly important to facilitate appropriate resource allocation decisions. Care at the end of life is known to account for a large proportion of health-care resources. Estimates from the United States indicate that 25% of health-care expenditure is related to patients in their last year of life. 1 In the United Kingdom, it is estimated that approximately 20% of hospital bed days are taken up by end-of-life care. 2 Palliative care services have been expanding worldwide with the aim of improving the experience of patients with terminal illness at the end of life through better symptom control, coordination of care and improved communication between professionals and the patient and family.3,4
However, the application of economic evaluation to palliative care has been slow to develop, and the evidence base remains small. While available studies indicate that palliative care is cost-saving, the results should be treated with caution (e.g. heterogeneous methods, poor quality of evaluation 5 ). There are challenges in applying standard economic evaluation techniques to palliative care, some of which relate to difficulties in capturing all relevant data (e.g. informal care costs), while others refer to conceptual issues of valuing benefits. There are concerns that the full impacts of the interventions are not being captured. For example, the appropriateness of applying standard economic evaluation techniques (e.g. the Quality Adjusted Life Year (QALY)) to measuring outcomes in palliative care has been questioned. 5 The duration of effect is inevitably limited in many palliative interventions, but a short good experience may be given a high value and this is not captured in the standard approach of adding up QALYs.4,6
Thus, there are reasons why studies in this area do not undertake formal cost-effectiveness analyses, but rather assess implications of palliative care interventions on costs separately from outcomes. As a result, methodological approaches are varied and often rely on relatively small observational studies. 3 It is important to keep these challenges in mind when reviewing economic studies in this field, looking for consistent patterns across study results rather than undertaking formal meta-analyses. Existing systematic reviews have assessed some of the evidence on costs and cost-effectiveness of palliative care,3,4,7 but the focus and the extent to which the quality of the cost analyses is assessed has varied.
This article presents results from a comprehensive literature review of available international evidence on the costs and cost-effectiveness of palliative care interventions in any setting (e.g. hospital-based, home-based (see the ‘Methods’ section for discussion of terminology)) over the period 2002–2011. Given the linkages between health-care utilisation and costs, evidence on service utilisation is also assessed. While we follow standard methods for conducting a systematic review and assess the quality of the evidence against a set of criteria drawn from the evaluation literature, we take a deliberately inclusive approach and no study is omitted from the summary findings on the basis of poor quality. This reflects our focus on identifying consistent patterns in results within a small field of evidence.
The ‘Methods’ section outlines the research question for the review and presents the methods. Quality assessment and key findings of the included studies are presented and discussed in the ‘Results for literature review (2002–2011)’ section, while the ‘Conclusion’ section concludes the article.
Methods
Terminology and objectives
The terms ‘palliative’ and ‘hospice’ have not been used consistently in the literature. Given the aim to capture a comprehensive review of studies in this area, this review avoids making strict delineations between hospice and palliative care. In outlining key findings, we adopt the same terminology as applied in the source literature. The general term ‘palliative care intervention’ used in this article is intended to cover interventions that specify a palliative care focus and/or hospice-related care. The term ‘end-of-life’ was kept deliberately vague so as to include as many studies as possible, for example, studies that focus on the last 7 days, last month, last 3 months and so on.
The specific objectives of the review were to
Identify studies that investigate the cost or resource use implications of a ‘palliative care intervention’ relative to some type of comparator or control.
Identify studies that investigate the cost-effectiveness of a ‘palliative care intervention’ relative to some type of comparator or control.
Search strategy
Key bibliographic and review databases were searched including PubMed (including MEDLINE), EURONHEED, the Applied Social Sciences Index (ASSIA) and the Cochrane library of databases (including the National Health Service Economic Evaluation Database, the Database of Systematic Reviews, the Health Technology Assessment Database and others).
The search strategy was initially limited to articles written in the English language, published in the period 1980–2011 and involving human subjects. The search was kept as broad as possible as there can be quite a lot of overlap between the palliative care and ‘end-of-life’ literatures. The strategy employed a list of terms grouped under three main headings intended to identify all publications relevant to the review question: life stage (e.g. end of life, last year of life, life-threatening and so on) OR type/location of care (e.g. palliative, hospice and so on) AND costs/cost-effectiveness (e.g. cost, economic, price and so on). The full list of search terms is available on request from the authors.
Applying these search criteria to the databases provided a list for title screening. Titles were excluded on the basis of six criteria: an exclusively non-Western focus, a pharmacological focus, editorials or other descriptive (e.g. historical discussion), literature reviews (systematic or otherwise), no specific focus on palliative or hospice care, or no specific focus on costs or health-care utilisation. Any citations that were ambiguous with regard to the exclusion criteria were retained for the next stage. Duplicates were identified and removed. Abstracts from the retained titles were reviewed and included for full text review unless any of the above exclusion criteria applied. If there were any ambiguity following the abstract review, the article moved to the next stage. The full text for those articles found to be potentially relevant from the abstract screening were reviewed in detail. Only those that met the criteria of examining the cost and/or utilisation implications of a palliative care intervention with some form of comparator were included in the final literature review. References of the retrieved articles were also hand-searched for further relevant studies. Data were extracted (onto an MS Access database) from the selected papers to record key study characteristics and to facilitate quality assessment.
Quality assessment
There is no single approach to assessing quality for a systematic review, and different elements of quality need to be considered for different study designs.8,9 For the purpose of this review, it was difficult to find an existing single set of criteria that could be applied given the diversity in the types of studies included and given the specific focus on cost analysis. Thus, this review compiled a set of 31 indicators suitable for evaluating a diverse set of papers, drawing on existing evaluation criteria (see Table 1).4,8,10–13 As a general guide, quality assessment of any study should consider risk of bias, statistical issues, quality of reporting and generalisability. 9 These factors informed the selection of indicators.
Quality indicators criteria.

The 31 indicators cover six core issues:
Study description (e.g. details on objectives, importance of the research question outlined, clear description of the alternatives being compared)
Sample selection and size (e.g. details on how the sample was selected, adequate sample size)
Measurement (e.g. clear description of outcome measures, viewpoint of analysis clearly stated)
Reporting (e.g. details on baseline demographic and outcome measures, details of currency and adjustments for inflation)
Analysis (e.g. clear description of statistical analytic methods, adequate controls for variations in individual characteristics and self-selection and other sources of bias)
Conclusions (e.g. statements of study limitations)
The quality of the papers was judged by a panel of three reviewers to ensure consistency. The reviewers discussed and agreed on a final mark for each indicator. Each indicator was allocated one of three possible marks: 0 (poor), 2 (incomplete or not clear) or 4 (good). In some cases, the indicator was not applicable for the paper and was marked as such. An overall mark, ranging from 0 (lowest quality) to 1 (highest quality), was then calculated for each of the six core issues (i.e. study description, sample selection and size, measurement and so on). For example, ‘study description’ covers three indicators. If a particular paper scored 4, 2 and 0 for indicators one, two and three respectively, the numerator for ‘study description’ would be 6 and the denominator would be 12 (4 being the maximum mark for each indicator), giving an overall score of 0.5. Where a particular indicator was not applicable, it was excluded from the calculation.
However, while quality scales and summary scores have been used in a number of palliative care reviews,3,4 it is important to note that their limitations and their use in general have been questioned. 9 As shown in the ‘Results for literature review (2002–2011)’ section, an overall score for each paper can be useful to classify papers into broad quality groupings, but this is more informative when combined with other factors, such as an assessment of the type of analytical methods employed by each paper. As in other literature reviews of palliative care,3,4 it was not possible to undertake formal meta-analysis of the cost findings, given the heterogeneity of the methods in the studies included in this review. As an alternative, the study findings are discussed broadly in order of general assessment of quality, drawing on the formal assessment ratings and also taking into account the sophistication of the statistical analysis undertaken.
Results for literature review (2002–2011)
Study selection
A total of 54,268 papers were returned from the initial bibliographic and review database search (Figure 1). Following the title screening, 53,041 papers were omitted as they clearly met the exclusion criteria. Of the 1227 papers that moved on to the abstract screening stage, 100 duplicates were omitted and 640 met the exclusion criteria. The full texts of the remaining 487 papers were retrieved. Focusing on the period 2002–2011, 285 papers were reviewed for potential inclusion in the literature review, of which 46 papers met the criteria of examining the cost and/or utilisation implications of a palliative care intervention with some form of comparator.
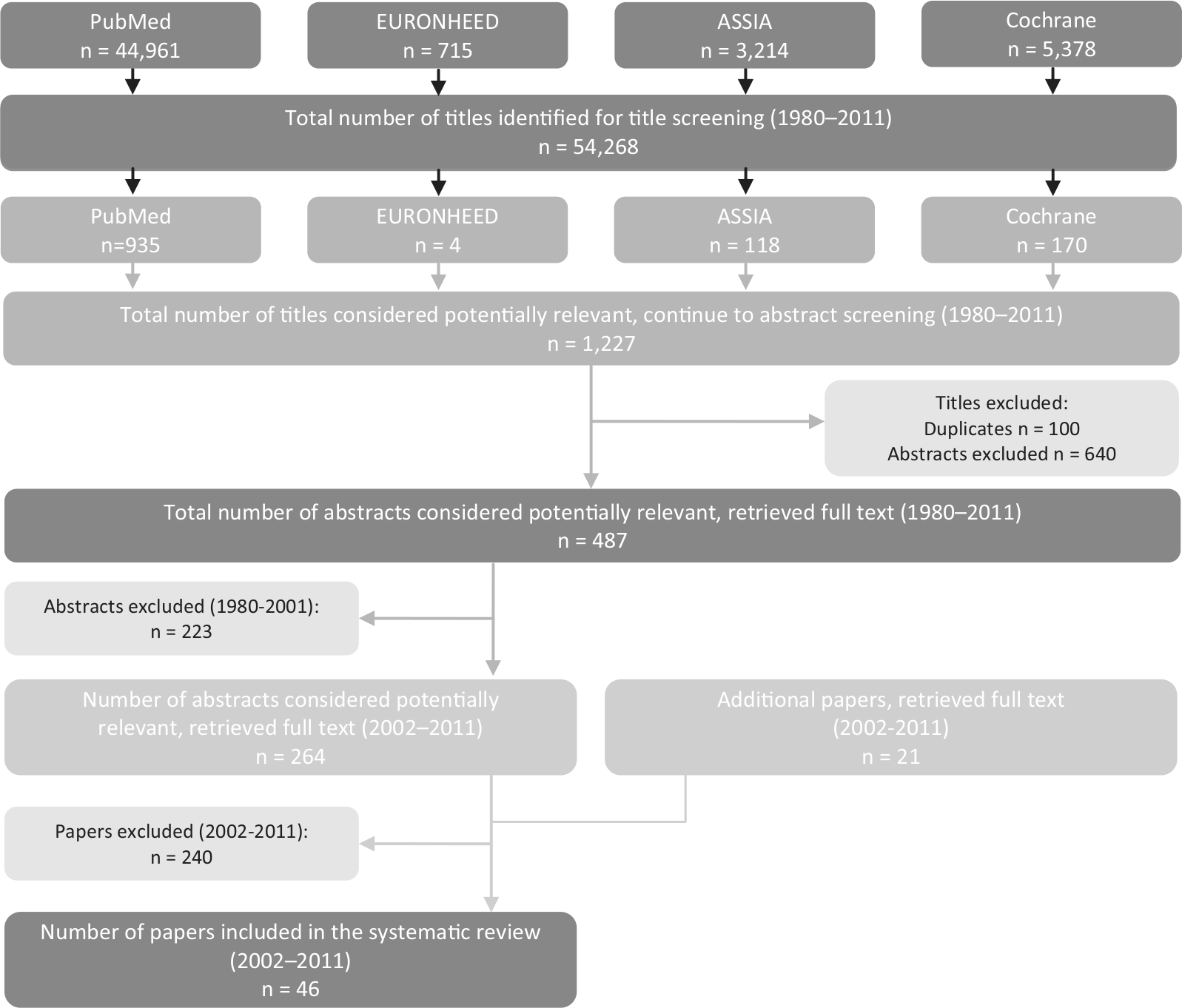
Flow Diagram of Study Selection Process 1
Study characteristics
Table 2 outlines the key characteristics of the 46 papers selected for inclusion in the review. Drawing on classifications outlined in the literature, 9 the papers fall into six main categories. There are 5 randomised controlled trials (RCTs), 2 non-RCTs, 34 cohort studies, 2 case studies, 2 before-and-after studies and 1 ‘other’ study.
Literature review paper characteristics (n = 46). a

PC: palliative care (non-specific use in this table to refer to the intervention being studied); ALOS: average length of stay; ED: emergency department; LYOL: last year of life; CI: confidence interval; LOS: length of stay; ICU: intensive care unit; sig.: significant (refers to statistical significance).
Some of the studies undertake additional analysis that is outside the focus of the central research question for the review. The results presented and discussed in sections ‘Results for literature review (2002–2011)’ and ‘Conclusion’ focus only on the analysis relevant to this review.
Focus on cost results only.
The included papers cover a range of different palliative care interventions including hospice care, hospital-based palliative care programmes, home-based palliative care programmes and others. As noted earlier, the definitions of palliative care interventions vary across studies, and in a number of cases, adequate descriptions of the intervention being studied were relatively limited, making international comparisons more difficult. Most of the papers analysed the impact of one specific palliative care intervention relative to a control, while three focused on comparisons across different types of palliative care or on palliative care in different locations.
The papers were also categorised according to whether they focused on costs, utilisation or both. Most of the studies focus on costs either with or without separate analysis of health-care utilisation. Of the five RCTs, 3 are ‘both cost and utilisation studies’, 1 is ‘cost only’ and 1 is ‘utilisation only’. The non-randomised controlled studies are all ‘both cost and utilisation papers’. The cohort studies comprise 15 ‘cost’ studies, 15 ‘both cost and utilisation’ studies and 4 ‘utilisation only’ studies. The before-and-after studies and one other study are ‘both cost and utilisation’ papers. Of the two case series papers, 1 is ‘cost only’ and 1 is ‘utilisation only’. Just one out of the 46 studies reports cost-effectiveness analysis, 14 illustrating the scarcity of this type of analysis in the palliative care field. Almost all of the cost studies focus on directly observable costs. Informal care costs are included in two studies,14,15 and out-of-pocket costs are the focus of one study, 15 although in some cases it is not clear whether out-of-pocket copayments have been included. As noted in other reviews, 7 there is variation in the cost data used with some studies relying on charges, others on observed expenditures and the remaining on detailed bottom-up estimates based on actual resource use.
In all, 31 of the papers are based on data from the United States and this is important when considering the generalisability of the findings to other health-care systems. The remaining studies are based on data from Belgium (1), Canada (2), France (2), Greece (1), Israel (2), Italy (2), Spain (1), Taiwan (1) and the United Kingdom (2).
Study quality
Figure 2 gives a graphical summary of the quality score results. The RCTs and non-RCTs perform well for all indicators with the exception of ‘reporting’ where there is some variation. The quality of the cohort studies (n = 34) varies across the indicators. Most perform well on study description, measurement and conclusions, but results are mixed for sample selection and size, reporting and analysis. The case studies perform well for all indicators. The quality score results for the remaining studies were mixed.
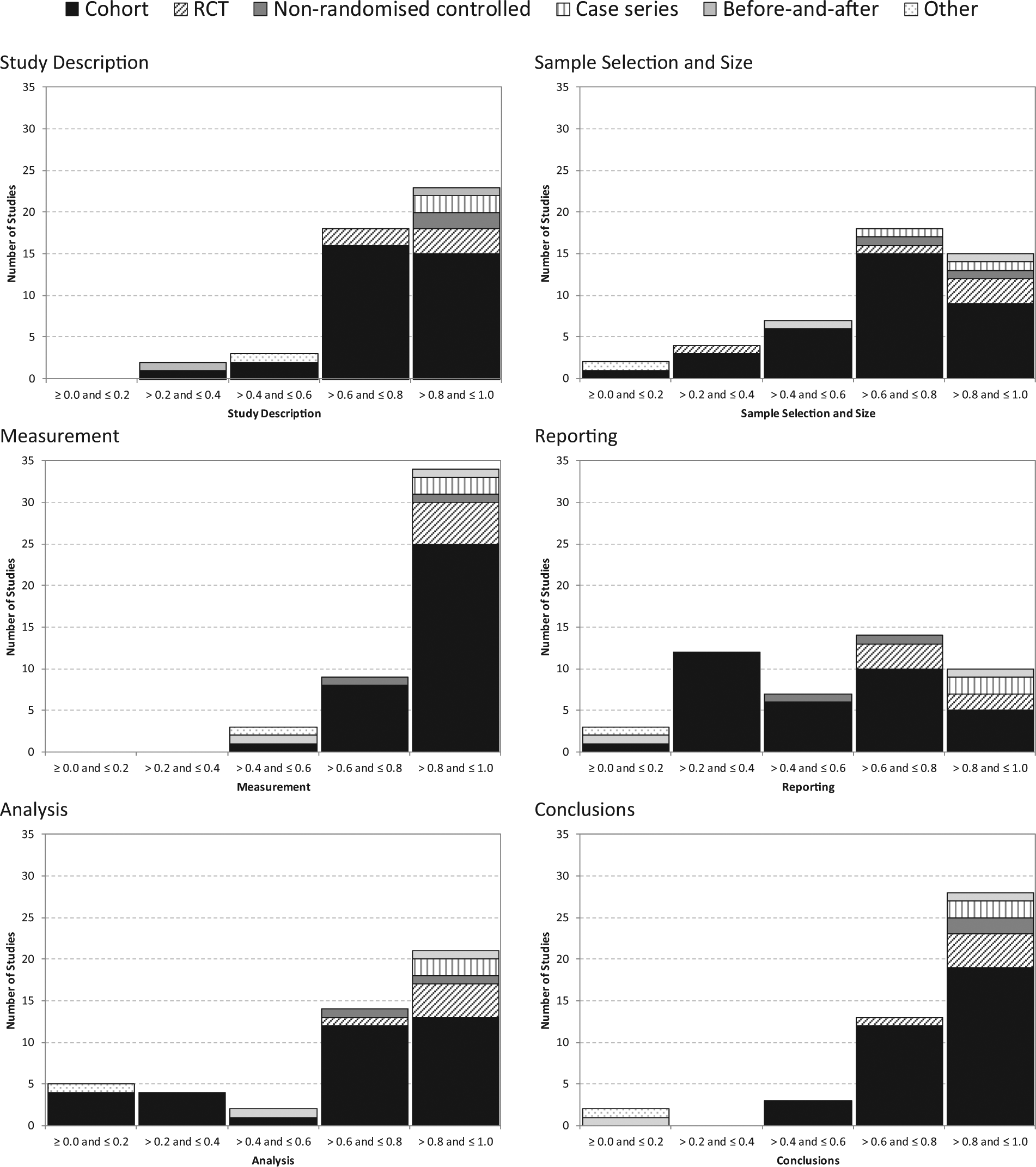
Study quality (n = 46).
It is useful to discuss the findings of the papers in some order of priority based on the quality assessment. Notwithstanding the caveats in generating summary quality scores for papers, there is scope for combining information on the scores with other factors to generate broad quality rankings. This review assigns papers into groups based on a joint assessment of the total quality scores and the type of analysis undertaken in each study.
RCTs are typically considered to be the gold standard for evaluating the effects of an intervention. An appropriately designed and implemented RCT allocates participants to the intervention and control groups using randomisation and concealment, which should ensure that the groups being compared are ‘similar in all respects other than the intervention’ (p. 34). 9 RCTs are typically assessed for risk of bias along key dimensions including sequence generation, allocation concealment, blinding (of participants and outcome assessors), outcome data, outcome reporting and other sources of bias. 8 Based on a brief assessment, the five RCTs14,16–19 perform relatively well along these dimensions although there is some lack of clarity in terms of blinding and allocation concealment. As noted, these studies perform well on the quality criteria compiled for this review and rank among papers of highest quality.
In non-RCTs, participants are allocated to the intervention and control groups using methods other than randomisation. 9 This increases the risk of selection bias, whereby individuals can be deliberately selected (or self-select) to the intervention or control group meaning that the results of the trial may be influenced by systematic differences between the study groups in terms of participant behaviours/prognosis. The two non-RCTs performed well against the quality criteria for this review.20,21 The first of these studies controlled for variations in individual characteristics across the groups using appropriate multivariate statistical techniques. 20 In the second study, although patients were not individually randomised to the intervention group, there was some randomisation at a higher level (i.e. two general medical practices operating alongside each other and a coin flip determined, which would form the intervention group and form the control). 21
Grouping the cohort studies according to whether multivariate i or univariate ii analysis was undertaken, the average total quality score is higher for the group of multivariate analysis studies (0.82 versus 0.68). Subdividing the ‘univariate’ group into studies that undertook formal statistical analysis and those that did not (e.g. no t-tests, chi-square tests and so on), there are differences in the average total quality score (0.70 versus 0.63). The variation in average quality among these three groups is even more distinct in terms of the average scores on the analytic dimension of quality: 0.85 for multivariate studies, 0.64 for univariate studies with formal statistical tests and 0.11 for studies with no formal statistical analysis.
Study findings on costs
In two out of six RCTs/non-RCTs that include cost data, the costs of the palliative care intervention were significantly lower than the costs for the control group.17,18 In three further studies, the costs were lower for the palliative care intervention although not significantly different,14,16 or no report of statistical significance. 20 In the remaining studies, costs were higher, but not significantly different, in the intervention group relative to the control group. 21 Throughout this review, the term ‘significant’ refers to statistical significance and the level of statistical significance (i.e. p value) is indicated where available.
Four of the RCTs included data on costs. One US study focused on a hospital-based palliative care programme. 17 Costs were computed for all health services used within 6 months following index hospitalisation discharge (e.g. hospital outpatient, home health visits, hospital readmissions and skilled nursing facility admissions). Univariate analysis found that total mean health costs per patient for the palliative care intervention group were significantly lower than the usual care control group (US$14,486 versus US$21,252, p = 0.001, year not stated although data were collected between 2002 and 2003). Cost savings were largely driven by a significant difference in hospital readmission costs (US$6421 per palliative care patient versus US$13,275 per usual care patient, p = 0.009). A second US study focused on an in-home palliative care programme and observed significantly lower costs for the palliative care group relative to the usual care control group. 18 Costs included acute inpatient, ambulatory, home health and palliative care costs. Total costs were on average US$7552 (at 2002 prices) lower for the in-home palliative care group over the study period (95% confidence interval (CI) = −US$12,730 to −US$2374, t = −3.63, p < 0.001), even after adjusting for a shorter survival period (i.e. from study enrolment to death) for the intervention group (196 days vs 242 days for the control group). The average cost of care per day was US$95.30 for the intervention group compared to US$212.80 for the control group, a significant difference (t = −2.417, p = 0.02).
The third RCT is a UK cost-effectiveness study of a new palliative care service for people with multiple sclerosis. The study found that total costs of care, including acute inpatient, ambulatory, other social/community care and informal care costs were £1789 (2005 prices) lower for the palliative care intervention group over a 12-week follow-up period (bootstrapped 95% CI = −£5224 to £1902). Excluding acute inpatient and informal care, mean service costs were £1195 lower for the intervention group (bootstrapped 95% CI = −£2916 to £178). 14
The fourth RCT is a US-based study of an advanced illness coordinated care programme designed to improve the care of people with serious illness to help them cope with advanced illness and with making end-of-life decisions. The study examined inpatient, outpatient, nursing home, inpatient hospice and other costs (e.g. diagnostic services) for participants and non-participants from 6 months prior to enrolment in the programme to 6 months post enrolment. Results found that total costs of care were lower for patients participating in the programme (US$12,123 per patient, year not stated, paper published in 2006) than for non-participants (US$16,295 per patient) at 6 months post enrolment. This difference in costs was not statistically significant (p = 0.18). 16
Two US studies undertook non-RCTs of palliative care.20,21 One focused on comparing an outpatient palliative medicine consultation intervention with usual primary care. Costs included physician office visits, emergency department visits and acute inpatient care. Results found that the mean charge for the palliative care patients over the study period was US$47,211 (year not stated, paper accepted for publication in 2003) compared with US$43,338 for the control group, and this difference was not statistically significant (p = 0.8). 21 The second study focused on a home-based palliative care programme, comparing this with standard home health services. Costs analysed referred to staffing costs only. Results found that the mean cost of care for the palliative care group was US$6580 (1999 prices) lower than the mean cost for the control group, after controlling for variation in the number of days receiving the service, severity of illness and having a congestive heart failure diagnosis (p values not reported). 20
In the cohort studies that undertook multivariate analysis of costs, 9 out of 11 studies found evidence of significantly lower costs in the palliative care intervention relative to the control group.22–30 The remaining two studies, both based in the United States, identified a more complex picture when disaggregating by age, cancer and length of nursing home enrolment.31,32
Five studies analysed the impact of hospice care on health-care expenditure. Three of these were US studies that investigated the impact of hospice care on Medicare (and in one case Medicaid also) expenditure during the last year of life. One study 25 used propensity score matching to control for variation in demographic and clinical characteristics of individuals across the hospice and non-hospice control groups. Results showed that hospice use reduced Medicare expenditures by an average of US$2309 (2003 prices) in the time period between initiation of hospice care and death relative to the same period for the matched control group (p < 0.001). The impact of hospice use on government expenditures was found by the other two studies to vary according to age, patient diagnosis and/or nursing home status.31,32 One study based in Taiwan 22 also undertook multivariate regression analysis, controlling for self-selection, demographic and clinical factors, examining the impact of hospital-based and home-based hospice on health-care expenditures per patient in the week before death. Results indicate that hospice has a negative impact on total expenditure in the last week of life relative to conventional care (p < 0.01), controlling for other factors. A study in Israel focused on the impact of home hospice on health-care expenditures in the last 2 months of life relative to conventional care. 26 Multivariate regression analysis found that controlling for gender, age and the number of treatment items per patient, the cost of care in the intervention group was significantly lower than in the control group (p < 0.01).
Five US studies examined the impact of hospital-based palliative care on health-care expenditure.24,27–30 Results were consistent across these studies, each finding palliative care to be associated with significantly lower inpatient costs. Three of these studies used propensity score matching to control for variation in demographic and clinical characteristics of individuals across the palliative care intervention and usual care groups.24,27,29 For example, in one study, for patients discharged alive from hospital, direct costs for the palliative care group were on average US$1696 (2004 prices) lower per admission relative to the control group (p = 0.004, or US$174 lower per day, p < 0.001). For patients who died in hospital, palliative care consultation was associated with mean savings of US$4908 in direct costs per admission relative to the control group (p = 0.003, or savings of US$374 per day, p < 0.001). 27
One US study undertook multivariate analysis of the impact of a palliative care home-based programme on staff costs relative to usual home health care. 23 Results showed that cancer patients enrolled in the palliative care group spent US$5936 (1999 prices) less on average compared to those in usual care (p = 0.001) over the last year of life, controlling for severity of illness and the number of days on service.
In the cohort studies that undertook univariate statistical analysis, 5 out of 13 studies found evidence of significantly lower costs in the palliative care intervention group compared with the control group,33–37 and a sixth study found evidence of lower costs without reporting statistical significance. 38 Five others found some evidence for significantly lower costs in the palliative care intervention group, but not consistently so, and variations were observed over a number of different factors including diagnosis, nursing home length of stay, daily cost versus total admission cost, type of ward on which palliative care was provided and time period studied.39–43 One study found evidence of significantly higher costs in a home-care scheme relative to conventional hospital care, although these results require careful interpretation because of the additional number of blood tests intentionally provided under the home-care scheme. 44 One study focusing on out-of-pocket expenses found no significant differences between the intervention and control groups, while finding informal care costs significantly higher in the intervention group, 15 underlining the importance of paying more attention to the indirect cost in palliative care.
The five cohort studies that did not undertake formal statistical analysis observed patterns of lower expenditures related to palliative care45–48 or no difference in costs between palliative care and non-palliative-care patients. 49
Three cohort studies compared palliative care costs across different types of palliative care.22,50,51 A study based in Taiwan observed no significant differences between home-based and hospital-based hospice expenditures per patient in the week before death, controlling for other factors. 22 One US study examined utilisation differences in hospice care between the institutional and home setting. 50 Multivariate analysis of utilisation over a 30-day period, adjusting for patient characteristics and length of enrolment, found institutional hospice users were significantly more likely to receive several types of services including physician services (odds ratio (OR) = 2.55, 95% CI = 1.68–3.87), prescription medicines (OR = 1.6, 95% CI = 1.16–2.2) and others. Average length of enrolment was significantly shorter for institutional hospice users than for home hospice users (p < 0.001). A study based in France examined variations in hospital-based palliative care costs across different types of hospitals (hospitals providing medical, surgical and obstetric care versus hospitals offering extended care and rehabilitation). 51 Univariate analysis found that the cost per patient per day was significantly lower in the hospitals focused on extended care and rehabilitation (p < 0.05), driven by differences in personnel and medications costs.
Case studies, before-and-after, other studies
Of the five studies that investigated the impact of palliative care on health-care costs using alternative methods to including a formal comparison group, four found evidence of significantly lower costs related to the palliative care intervention.52–55 The fifth found evidence of higher charges for palliative care relative to a national average charge. 56 For example, one of the case studies, based in France, compared the cost of hospital at home services with the estimated cost of treating the same patients in a standard hospital setting. 53 Univariate analysis found that for patients considered to be at the palliative care stage, the average cost per patient of hospital-at-home over a 2-week observation period was €1202 (2001 prices) compared with the estimated cost of inpatient hospital care of €3490, a significant difference (p < 0.0001).
Study findings on health-care utilisation
In general, the impact of palliative care on resource utilisation is mixed as illustrated by one of the highest quality ranking cohort studies, which focused solely on the use of services (i.e. no cost data 57 ). This US study used multivariate analysis to compare resource use by cancer decedents who received hospital-based palliative care with those who received usual care. Results indicated that patients in the palliative care group who were enrolled for longer than 113 days were less likely than the control group to have an acute care admission during the last 60 days of life (OR = 0.306, 95% CI = 0.117–0.802). The average length of stay per acute care admission was significantly shorter for palliative care patients relative to the control group (p < 0.05). Results on the total number of acute care days within the last 60 days of life depended on the length of palliative care enrolment. Palliative care patients who were enrolled in palliative care for less than 60 days were more likely to have a greater number of total acute care bed days relative to the control group (p < 0.05). Palliative care patients who were enrolled for more than 60 days were more likely to have a smaller number of total acute care bed days relative to the control group (p < 0.05).
The mixed results apply to all of the study categories included in the review. Of the six RCTs/non-RCTs with utilisation data, three studies found evidence of lower use of some hospital services,17,18,20 while three found no significant differences in others.17,19,21 Of the cohort studies that report specific results on health-care utilisation, the same mixed pattern is observed,24,28–30,33,35,37–39,42,44,46,48,49,58,59 while detailed analysis by two studies33,57 illustrate the varied impacts of palliative care on utilisation (e.g. depending on time period studied, length of enrolment).
Study findings on cost-effectiveness
Only one of the studies met the criteria for a cost-effectiveness study. 14 Patient outcomes were measured on the Palliative Care Outcome Scale (POS-8) iii and caregivers’ burden was measured using the Zarit Carer Burden Inventory (ZBI). There was no significant difference in the POS-8 measure over the trial, while ZBI scores improved for the intervention group and worsened for the control group. The point estimates indicate that the intervention is cost-saving with equivalent outcomes on the POS-8 scale and improved outcomes on the ZBI. Sensitivity analysis examined uncertainty around those point estimates. For the POS-8 measure, the cost-effectiveness plane shows the intervention group had lower costs and better outcomes than the control group 33.8% of the time, and lower costs and worse outcomes 54.9% of the time. When the cost-effectiveness analysis is based on the ZBI measure, the intervention group shows lower costs and better outcomes 47.3% of the time, and higher costs and better outcomes 48% of the time.
Conclusion
Overall, the review presents an up-to-date picture of the most recent analysis being undertaken on the cost (and resource use) implications of palliative care interventions over the period 2002–2011. The main focus of these studies is on direct costs, from the provider or third-party payer perspective, with little focus on informal care or out-of-pocket costs. While a small number of studies follow an RCT or non-RCT format, the majority of studies are described as cohort studies and therefore need measures to control for confounding factors and selection bias in the analysis. The overall quality of the studies is mixed, although a number of cohort studies do undertake multivariate regression analysis and include measures to control for selection bias.
The evaluation criteria, combined with information on the type of statistical analysis undertaken, have provided a useful overview of the overall quality of the papers. The absence of randomisation in most of the studies highlights the importance of controlling for confounding factors and selection bias when analysing the impact of a palliative care intervention on the outcome of interest. A number of the cohort studies have undertaken multivariate regression analysis, and many of these have also used propensity score matching techniques to control for selection into the intervention and control groups. In general, the RCT papers, the non-RCTs and the cohort and case studies that undertook multivariate analysis are at the higher end of the quality scale.
In terms of generalisability, a couple of points should be considered. The models of care and reimbursement for palliative care pursued across different countries can vary widely, which is particularly relevant here as a large proportion of the 46 studies examined here are based on United States. In addition, while the included studies focus on both malignant and non-malignant conditions, it is recognised that conditions may follow different trajectories.
However, despite the wide variation in study type, characteristic and study quality, there are consistent patterns in the results. Palliative care is most frequently found to be less costly relative to comparator groups, and in most cases, the difference in cost is statistically significant. It is also worth noting that there may be complex interactions between costs of care and diagnosis (e.g. cancer/non-cancer distinctions), age groups and other factors (e.g. length of nursing home enrolment in US studies) that require further investigation and in particular the role played by informal care needs to be analysed in more detail.
Footnotes
Acknowledgements
The authors would like to thank Dr Karen Ryan for valuable comments on an early draft of this review.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This review was conducted as part of a larger project on palliative care in Ireland funded by The Atlantic Philanthropies (Grant No. 18744). The funding body was not involved in the conduct of the review or in the development of this article.
i
Multivariate analysis involves analysing the impact of a particular variable on an outcome of interest, while taking into account (i.e. controlling for) the effects of all other variables that may influence the outcome of interest (e.g. regression analysis).
ii
Univariate analysis examines the association between a particular variable and an outcome of interest, without controlling for any other factors that may influence the outcome of interest. The association can be tested for statistical significance using a range of statistical tests (e.g. t-tests, chi-square tests) depending on the type of variables involved (continuous, categorical).
iii
Eight questions on anxiety, patient and carer concerns and practical needs.
