Abstract

Background
In high-income countries, people from ethnic minority backgrounds are less likely to access specialist palliative care 1 and appropriate pain relief medication, 2 and use unplanned hospital care more in the last months of life. 3 Where people die depends on many social and clinical factors. 4 Most people prefer to avoid dying in hospital if possible, and yet hospital remains the most common place of death. 4
Historically, it has been challenging to explore ethnic inequality in place of death because ethnicity is not recorded on death certificates in most countries. 5 Census data contains self-reported ethnicity data considered the ‘gold-standard’ compared to the assigned ethnicity information common in clinical records. When linked to mortality records, Census data provides a valuable but underused resource for understanding ethnic inequalities in place of death. 6
We investigated the association between ethnicity and death in hospital (compared to all other locations) and examined how far this association is explained by geography, socioeconomic factors, and cause of death.
Methods
Census data linked to mortality records for a 1% sample of the population in England and Wales who died between 1st January 2011 and 31st December 2017, accessed through the Office for National Statistics Longitudinal Study (ONS LS). Death in hospital (vs home, hospice, and care home) was the outcome. Ethnicity was the main exposure coded in 11 categories. We ran Poisson models with robust standard errors, separately for men and women, adjusted for age, and cumulatively adjusted for other explanatory factors.
Analysis was carried out in Stata SE v17.0, with code available here: https://github.com/joannamariedavies/ONS_LS.
Results
After excluding 688 people who died in ‘other’ locations, and 17 with missing place of death, 34,230 decedents were included. Table 1 describes the sample.
Sample characteristics for decedents from the ONS Longitudinal Study (deaths between 2011 and 2017), by place of death.
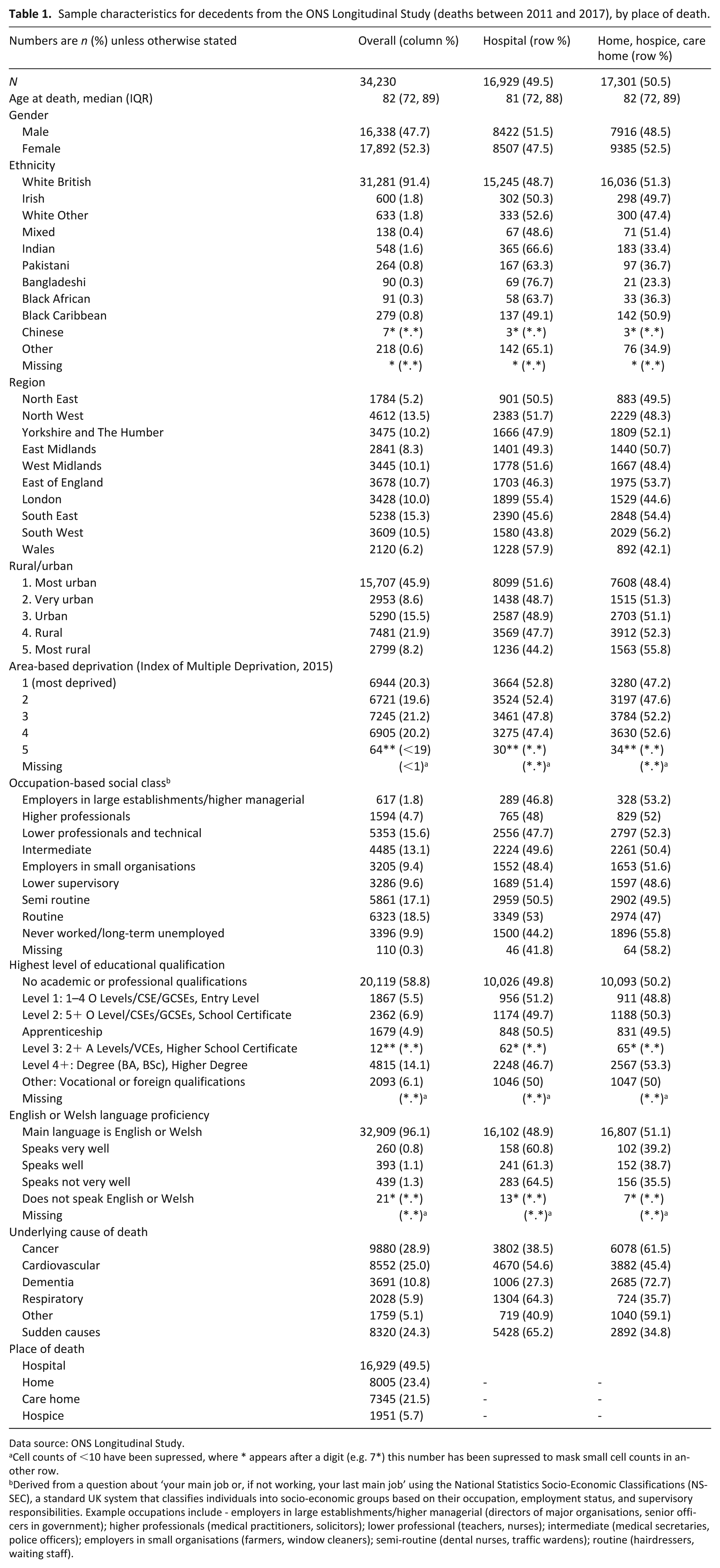
Data source: ONS Longitudinal Study.
Cell counts of <10 have been supressed, where * appears after a digit (e.g. 7*) this number has been supressed to mask small cell counts in another row.
Derived from a question about ‘your main job or, if not working, your last main job’ using the National Statistics Socio-Economic Classifications (NS-SEC), a standard UK system that classifies individuals into socio-economic groups based on their occupation, employment status, and supervisory responsibilities. Example occupations include - employers in large establishments/higher managerial (directors of major organisations, senior officers in government); higher professionals (medical practitioners, solicitors); lower professional (teachers, nurses); intermediate (medical secretaries, police officers); employers in small organisations (farmers, window cleaners); semi-routine (dental nurses, traffic wardens); routine (hairdressers, waiting staff).
After adjusting for age, geography, socioeconomic factors, and underlying cause of death, Bangladeshi men (PR 1.48; 95% CI 1.26-1.74), Pakistani men (1.19; 1.04–1.37), Indian men (1.18; 1.07–1.31) and women (1.17; 1.04–1.33), and men (1.19; 1.02–1.39) and women (1.21; 1.03–1.42) from ‘Other’ ethnic groups have statistically significantly higher rates of death in hospital, compared to White British men and women (Figure 1).
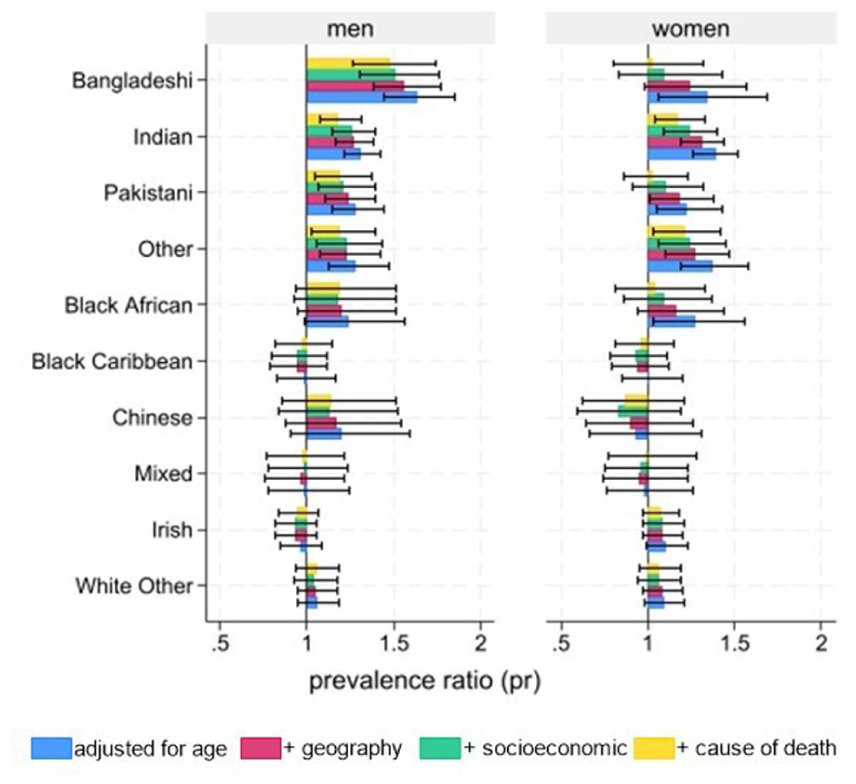
Adjusted prevalence ratio and 95% confidence intervals for death in hospital (compared to home, hospice or care home), by ethnic group and sex, compared to white British. Data source: ONS Longitudinal Study.
Discussion
In this representative sample of people who died in England and Wales, most ethnic minority groups have a higher proportion of deaths in hospital than White British people. For some groups, these differences are explained by differences in age and other factors. However, for Bangladeshi and Pakistani men, Indian men and women, and men and women from ‘Other’ ethnic groups, higher rates of death in hospital remain statistically significant after adjusting for differences in age, geography, socioeconomic factors, and underlying cause of death.
A strength of our analysis is that we used self-reported ethnicity data from the Census. Data linkage across primary and secondary health records can improve the quality of ethnicity information in routinely collected patient records. 7 However, there remain persistent inaccuracies in the ethnicity information recorded in health records and these inaccuracies are more common for minority groups. 8 For historical reasons associated with the Holocaust, in some countries, including France and Germany, the collection of ethnicity data is highly restricted, leading to ‘ethnic invisibility’ in administrative and survey data. In England and Wales, ethnicity has recently been introduced to death certificates, assigned by the attending practitioner based on the patient record. The usability of this data will depend on the quality and completeness of the patient record.8,9
Our sample size allowed us to use refined categories of ethnicity and sex, revealing important differences between subgroups, and we included good quality sociodemographic and geographical data. Potentially important unmeasured confounders include symptom burden, preferences, and access to community services. A limitation is that our data is relatively old (deaths between 2011 and 2017) but at the time of writing, the 2021 census was not available in the ONS Longitudinal Study. We used an area-based measure of socio-economic deprivation, which may not reflect individuals’ experience. Despite a large overall sample size, small numbers in some of the ethnic minority groups prevented further intersectional analysis. Analysis of census data linked to mortality data for the full population would offer more opportunities to explore interactions between ethnicity and deprivation, and geographical variation in ethnic inequalities in place of death.
This analysis highlights an ethnic inequality in place of death and differences between genders not previously described. Our findings are nuanced, illustrating how some ethnic differences in place of death are explained by differences in age and other factors, while others are not. Our findings align with recent analyses highlighting South Asian communities as being at higher risk of unplanned hospital-based care in the last months of life. 3 There is a lack of research on the reasons for these inequalities and whether they represent inequity in access to services. 10 Important first steps are to measure and monitor ethnic inequalities in palliative and end-of-life care, and to improve the quality of ethnicity information in routinely collected health records. 10 This should include public discussion on the purpose of collecting data on race and ethnicity. In addition, more work is needed to understand the experiences, needs and preferences of people from ethnic minority communities living with terminal illness to inform more equitable care.
Footnotes
Acknowledgements
The permission of the Office for National Statistics to use the Longitudinal Study (LS) is gratefully acknowledged, as is the help provided by staff of the Centre for Longitudinal Study information and User Support (CeLSIUS). CeLSIUS is funded by the ESRC under project ES/V003488/1. The authors alone are responsible for the interpretation of the data. This work contains statistical data from the ONS which is Crown Copyright. The use of the ONS statistical data in this work does not imply the endorsement of the ONS in relation to the interpretation or analysis of the statistical data. The work uses research datasets which may not exactly reproduce National Statistics aggregates. The Office for National Statistics Longitudinal Study (LS) uses information from the 1971, 1981, 1991, 2001, and 2011 censuses for England and Wales; individuals’ census forms are linked; data is also linked to some life events data (deaths, births and cancer registrations); individuals can enter the study by birth or immigration and being born on one of the four confidential LS birthdays, and leave the study through emigration or death; and the study contains data for over 1.1 million people. Find out more information about the LS here : doi: ![]()
Ethical statement
This study was given ethical approval by the curators of the data, the UK Office for National Statistics; study id: 2000705.
Author contributions
JD had full access to all the data in this study and had final responsibility for the decision to submit for publication. JD, KS, FM, KC, and MM contributed to the conception and design of the study. JD performed the statistical analyses and drafted the manuscript. All authors contributed to the acquisition, analysis, or interpretation of the data, and critically revised the manuscript for important intellectual content. JD and KS are guarantors. The corresponding author attests that all listed authors meet authorship criteria and that no others meeting the criteria have been omitted.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study is funded by Marie Curie (MC-21-816). KES is the Laing Galazka Chair in palliative care at King’s College London, funded by an endowment from Cicely Saunders International and the Kirby Laing Foundation. FEMM is a UK National Institute for Health and Care Research (NIHR) Senior Investigator. MM is supported by the NIHR Applied Research Collaboration (ARC) for South London. The views expressed in this paper are those of the authors and not necessarily those of the NIHR or the Department of Health and Social Care.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
