Abstract
Background:
The need for palliative care is rising rapidly, but meeting global demand is falling behind. Telepalliative care offers a potential solution, though its implementation requires careful ethical evaluation.
Aim:
To provide an overview of the ethical concepts and arguments related to telepalliative care as presented in the argument-based literature.
Design:
We conducted a systematic review of argument-based literature following PRISMA-guidelines (PROSPERO: CRD42024533732). Data extraction and synthesis followed the Qualitative Analysis Guide of Leuven.
Data sources:
We searched 12 databases covering medical, ethical, and technological disciplines using broad, unfiltered terms. Publications in English, French, German, or Dutch on telehealth, palliative care, and ethics were considered. Two researchers independently screened publications, using peer review as a quality proxy due to the lack of standards for argument-based literature.
Results:
Twenty-six publications were included. Two main ethical approaches emerged: one related to the four principles of biomedical ethics and the other to care. Regarding respect for autonomy, telepalliative care may both promote and limit autonomy, with concerns raised about informed consent, privacy, and confidentiality. Regarding beneficence, potential improvements in symptom management and quality of life were identified. Regarding non-maleficence, risks such as replacing in-person care and medicalizing the home environment were highlighted. Regarding justice, issues of access, equity, distributive justice, and environmental issues were addressed. Concerns about the patient-provider relationship and holistic care were central to care-related arguments.
Conclusions:
Telehealth’s benefits challenge its incompatibility with palliative care, however, significant risks threaten core palliative care values. Thus, careful implementation must prioritize ethical considerations.
Keywords
Global demand for palliative care is growing, yet access to palliative care services remains limited.
Telehealth in palliative care is gaining attention and has the potential to improve access to palliative care services.
Current telepalliative care literature focuses on practices, efficacy, stakeholder perspectives, and outcomes, while ethical considerations are underexplored.
This paper provides a comprehensive overview of the ethical concepts and arguments related to telepalliative care as discussed in the argument-based literature.
Two main ethical frameworks emerge in the literature on telepalliative care: one related to the four principles of biomedical ethics and the other related to care.
Telepalliative care is shown to be a complex phenomenon, carrying both positive and negative ethical implications for patient care.
Implementation of telepalliative care should prioritize ethical considerations, as telepalliative care comes with risks, some of which challenge core palliative care values.
Further in-depth ethical analysis is needed, preferably guided by a care-ethics approach that also considers societal values.
Background
An urgent need for palliative care interventions is rapidly emerging around the world. By 2060, serious health-related suffering is anticipated to increase 87% worldwide.
1
Despite playing a critical role in improving patients’ quality of life, the highest standard of palliative care is currently accessible to only 14% of the global population, exposing a significant gap between the growing need for this kind of care and available resources.
2
Telehealth is one approach that may help fill this gap. Telehealth systems are defined as: . . .electronic information and telecommunication technologies that support long-distance clinical health care, patient and professional health-related education, public health and health administration. They are intended to allow monitoring and/or delivery of healthcare to patients at locations remote from where the healthcare professional is located.
3
Telehealth could make palliative care more accessible as a standard component of patient care. Despite popular beliefs, palliative care is not limited to the terminal phase of illnesses, as it can complement curative treatments. 4 Together, these considerations suggest that it will become increasingly imperative to integrate palliative care across healthcare settings, going beyond dedicated palliative care units. 5 Doing so could elevate quality of life for many patients. For instance, providing palliative care in the intensive care unit (ICU) is associated with improved decision-making when considering withdrawing or withholding life-sustaining treatments. 6 Telehealth can potentially support these efforts and the ICU team by facilitating access to palliative care experts.
The growing focus on telehealth in palliative care—also called telepalliative care—is reflected in the expanding literature on this topic. This literature mainly evaluates current practices,7–11 efficacy,12,13 stakeholder perspectives,14–16 and outcomes such as patient satisfaction, symptom management, quality of life, caregiver impact and cost.9,10,17–20 A glaring absence is a consideration of the ethics of telepalliative care. Gordon et al. 17 identified a notable lack of research addressing the ethical aspects of telepalliative care, underscoring the need for further exploration. Integrating telehealth into palliative care in itself raises ethical questions. This is particularly the case given the apparent tension between the concepts of proximity and human contact—often associated with palliative care—and the concept of distance implied by the Greek root of “tele” in telehealth. To promote a clearer understanding of the ethical issues surrounding telepalliative care, this review aims to provide an overview of the ethical concepts and arguments presented in the argument-based literature (for its definition see Table 1).
Eligibility criteria for selection of publications.
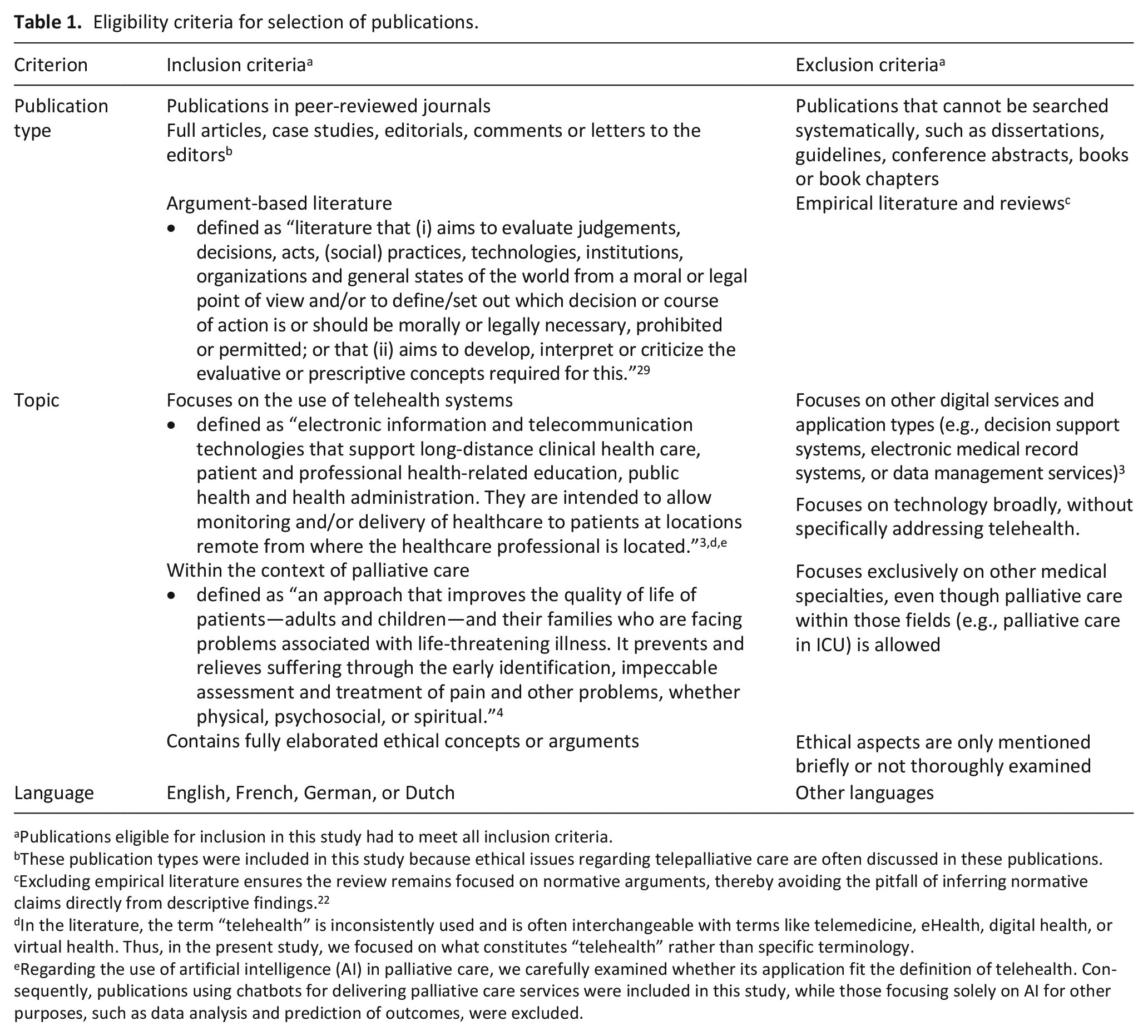
Publications eligible for inclusion in this study had to meet all inclusion criteria.
These publication types were included in this study because ethical issues regarding telepalliative care are often discussed in these publications.
Excluding empirical literature ensures the review remains focused on normative arguments, thereby avoiding the pitfall of inferring normative claims directly from descriptive findings. 22
In the literature, the term “telehealth” is inconsistently used and is often interchangeable with terms like telemedicine, eHealth, digital health, or virtual health. Thus, in the present study, we focused on what constitutes “telehealth” rather than specific terminology.
Regarding the use of artificial intelligence (AI) in palliative care, we carefully examined whether its application fit the definition of telehealth. Consequently, publications using chatbots for delivering palliative care services were included in this study, while those focusing solely on AI for other purposes, such as data analysis and prediction of outcomes, were excluded.
Methods
Design
We conducted a systematic review of argument-based literature.21,22 This design enabled us to identify and synthesize existing ethical literature on telepalliative care, 23 which could be valuable for informing healthcare policy and decision-making.24,25 The review protocol was preregistered with the International prospective register of systematic reviews (PROSPERO ID: CRD42024533732). Reporting followed the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) guidelines for systematic reviews 26 and the REporting of SystEmatic ReViews in Ethics (RESERVE) guidelines. 27
Research questions
The review addressed two research questions:
(1) What are the main ethical concepts involved in telepalliative care?
(2) What ethical arguments have been formulated based on these concepts?
Literature search
The search strategy was constructed around three concepts: telehealth, palliative care, and ethics. Additionally, terms (e.g., telepalliative) that combined the first two concepts (e.g., telehealth and palliative care) were included. Given the inconsistent use of the term “telehealth” in the literature, we used a broad search approach that included a wide range of related terms (e.g., virtual care, health technology, and medical informatics) to ensure thorough coverage. The first author (LK) created the initial search string for Medline in collaboration with the last author (CG; Supplemental Material—Additional File 1). This search string was later modified for use with other databases. All search terms were in English. A biomedical reference librarian at KU Leuven helped optimize the search. Figure 1 presents an overview of the process for identifying relevant publications.
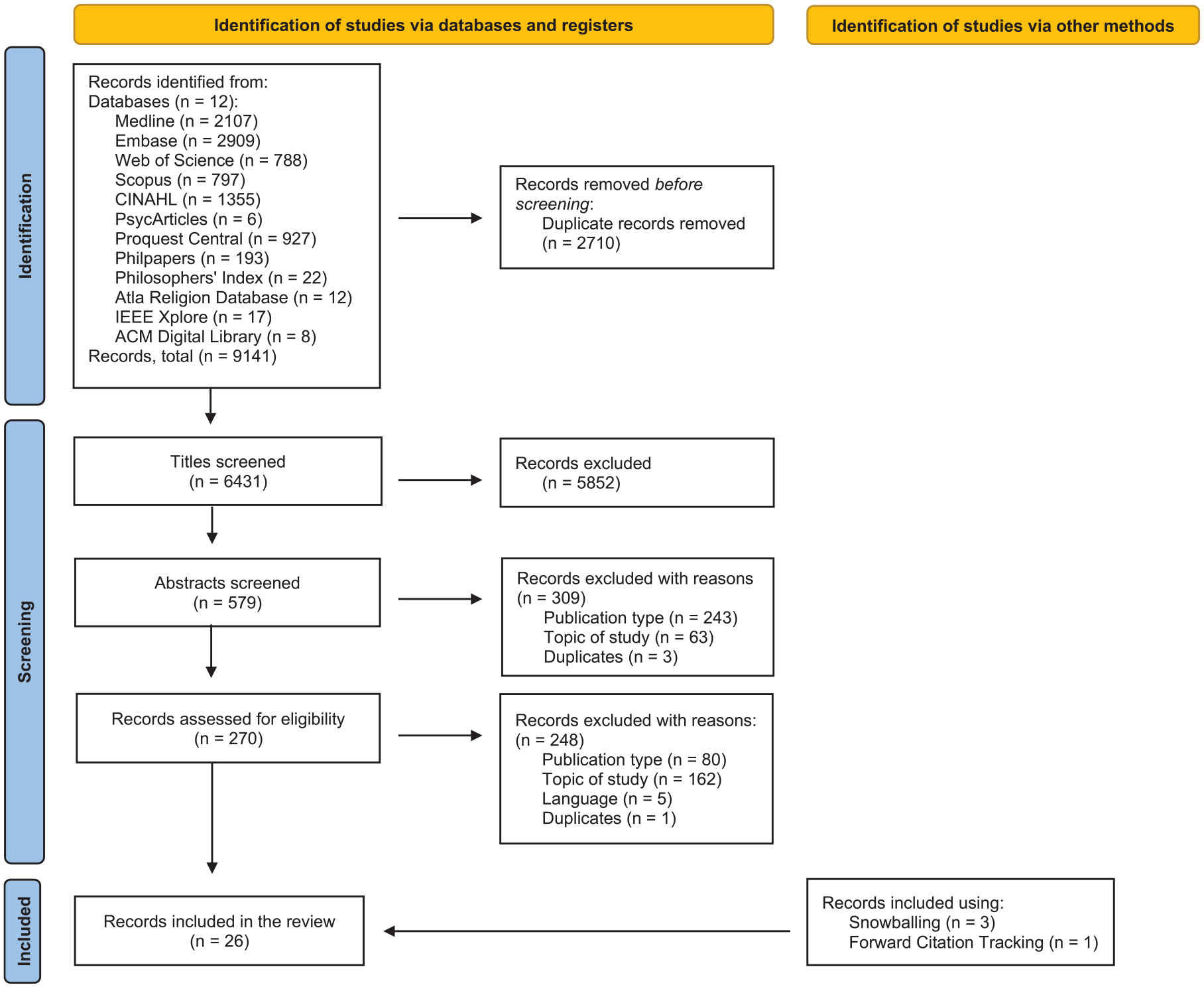
PRISMA 2020 flow diagram illustrating the process for identifying relevant articles. 26
On April 2, 2024, LK executed search queries in 12 online databases: Medline, Embase, Web of Science, Scopus, CINAHL, APA PsycArticles, ProQuest Central, PhilPapers, Philosopher’s Index, Atla Religion Database, IEEE Xplore, and ACM Digital Library. These databases were chosen to ensure comprehensive coverage of the medical, ethical, and technological fields. No filters or restrictions were imposed. References for the identified publications were managed using EndNote 21. 28 Duplicate references were identified and removed using EndNote’s duplicate detection function and checked manually by LK.
LK and CG independently screened the titles and abstracts of candidate articles according to predefined eligibility criteria (Table 1). Title screening achieved 96% inter-rater agreement (6152/6431), while abstract screening resulted in 82% (476/579). If at least one author included a title or abstract, it was included in the next round of screening. LK then conducted full-text screening of each candidate article to determine final eligibility. Uncertainties were addressed through discussions between LK and CG until consensus was reached. Additionally, snowballing and forward citation tracking were used. As there is no established standard for quality appraisal of argument-based literature, we relied on the peer-review process of the journals in which articles appeared as a proxy measure for article quality. 29
Data extraction and synthesis
Data extraction and synthesis followed the inductive approach of the five preparatory steps of the Qualitative Analysis Guide of Leuven (QUAGOL). 30 This process was primarily conducted by LK in collaboration with CG. First, we sought to gain a holistic understanding of the texts and identify ethical sections by thoroughly reading and rereading the included publications. Second, we created summary reports for each publication by outlining their ethical content, retaining as much of the original wording as possible. Third, from these summary reports, we developed more abstract conceptual schemes by translating each report’s content into its underlying concepts and arguments (Supplemental Material—Additional File 2). Fourth, we refined the conceptual schemes through a forward-backward, reading-checking process. The schemes were repeatedly checked against the ideas presented in the original publications to ensure the publications were relevant to our two research questions. Fifth, using an iterative process, we further developed and refined the conceptual schemes by comparing them with the schemes of other publications. This process objectively aided our search for common themes, which were then synthesized into a general conceptual framework.
Results
We identified 26 eligible publications whose key characteristics are described in Table 2 (Supplemental Material—Additional File 3). Publication years spanned from 2001 to 2024, with nearly 70% published between 2020 and 2024. Approximately 60% of first authors were affiliated with institutions in the United States; 50% of all first authors had medical backgrounds. Our analysis identified two main approaches within the ethical concepts and arguments discussed in the included publications: one related to principles, and the second to care.
Characteristics of included publications.
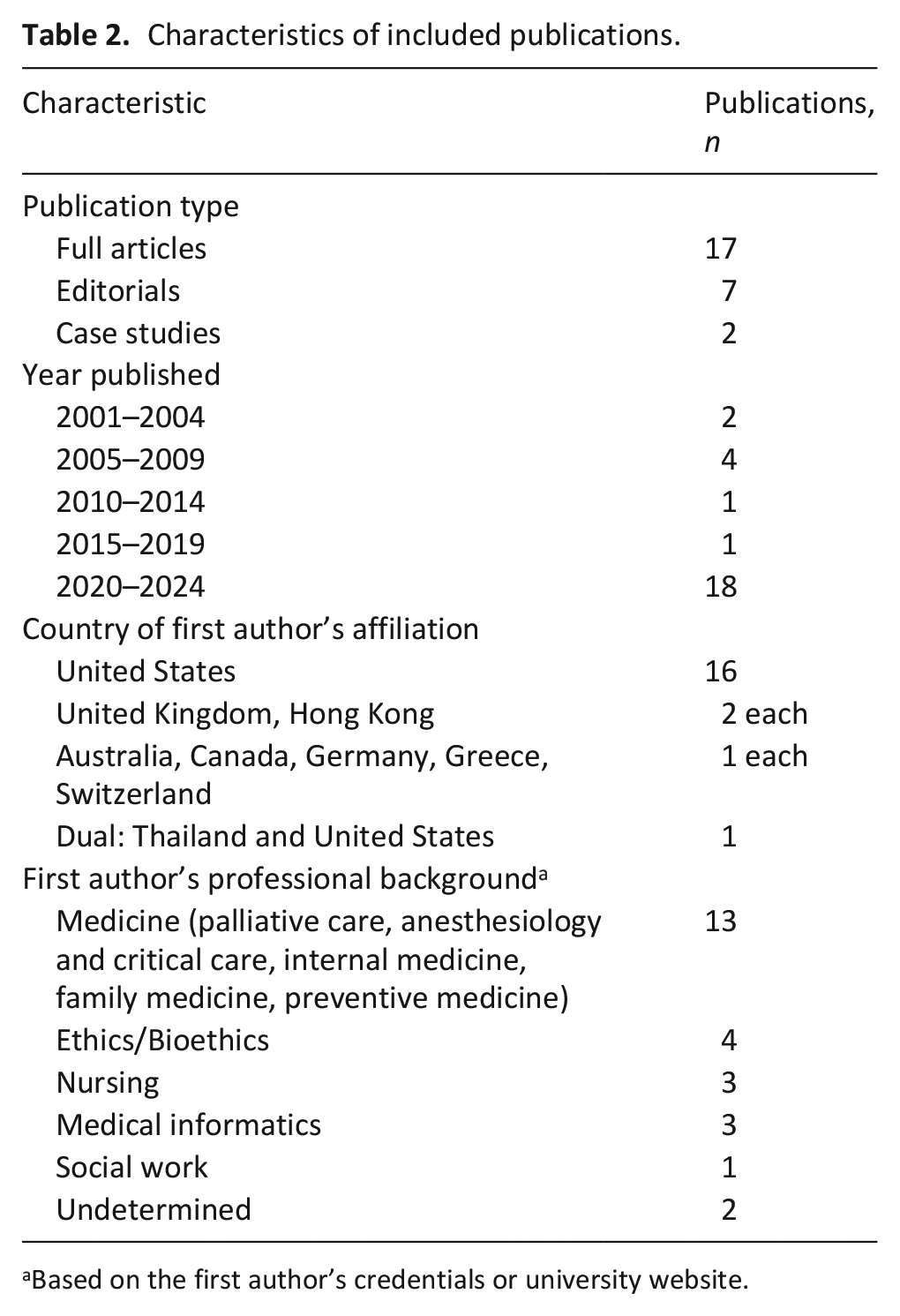

Based on the first author’s credentials or university website.
Ethical concepts and arguments related to principles
The included publications extensively covered concepts and arguments related to the principles of respect for autonomy, beneficence, non-maleficence, and justice—principles that align with those outlined by Beauchamp and Childress. 31
Respect for autonomy
The principle of respect for autonomy centers on the concept of self-determination, emphasizing individuals’ right to make informed decisions. 31 Our analysis revealed that telehealth can have a potential dual impact on autonomy. We also found that the publications considered concepts related to autonomy, such as informed consent, privacy, and confidentiality.
A dual impact on autonomy
Empowering patients by promoting autonomy may be especially important in palliative care, because patients often sense a loss of control when dealing with severe illnesses. 32 However, the included publications reported that telehealth can actually enhance patient autonomy in some situations but in others, restrict it. Thus, several points of tension emerge.
A first point of tension is telepalliative care’s potential to both expand and limit a patient’s choice. Telehealth can enhance autonomy by increasing the range of treatment options possible, such as more home care opportunities. 33 This situation allows care to better align with a patient’s preferences, thereby enabling person-centered care. 33 However, the possibility also exists for telehealth to replace traditional care services,34–36 and in doing so, it would limit a patient’s choice. Telehealth can limit autonomy further if it is implemented without considering the patient’s preferences, for example, how they view technology fitting into their daily lives.32,36,37
A second point of tension related to autonomy involves how patient health data can be used both to empower and disempower patient perspectives, affecting autonomy in opposite ways. Palliative care applications containing data from electronic patient-reported outcomes can promote autonomy by validating patient perspectives and contribute to person-centered care.38–40 However, if data from remote monitoring devices are used in isolation or to override the patient’s wishes, the patient’s perspective is diminished.36,41,42 Thus, under the assumption that data are infallible, these apps can lead to paternalism and limit autonomy.36,41,42
A third point of tension related to autonomy involves how telehealth can, at the same time, both promote independence and create dependence. On the positive side, telehealth can promote self-management32,40,41 and create a supportive environment,32,35–37 thus encouraging independence. However, telehealth can also cause dependence or over-reliance on technology,34,35,37 a risk that becomes particularly evident during technology failures. 37 For instance, reliance on automated monitoring might cause informal caregiver to “become less vigilant in monitoring health changes in their loved one (and patients themselves may become less vigilant in health self-monitoring or self-management)” 37 (p. 114).
Informed consent
Informed consent is essential to the principle of respect for autonomy, and the patient is most often recognized as the central figure from whom it must be obtained.34–36,40,43–46 Several publications underscored the need to obtain informed consent prior to implementing telehealth.34–37,40,42–46 Nevertheless, some authors also acknowledge the importance of securing informed consent from informal caregivers,34,37,42 as they may be involved indirectly in telepalliative care. For example, informal caregivers may assist the patient during virtual visits, and by doing so they also encounter risks to their own privacy.
The included studies mentioned two obstacles to obtaining proper informed consent when using telehealth. First, the risks and benefits of new technologies, or existing technologies applied in new contexts, are often unknown, making it challenging to adequately inform patients.34,36,37 Second, patients may struggle to comprehend risks related to technologies they are unfamiliar with, even when these risks are explained, thereby hindering valid informed consent.34,35,37 Patients may not recognize risks until they actively engage with the technology. For instance, without a foundational understanding of a smartphone, some patients may find it difficult to understand data security risks. To address this kind of risk, several authors proposed using a dynamic consent model that allows patients to adjust their preferences as they become more familiar with the technology and its associated risks.34,36,37,44
Privacy and confidentiality
The right to privacy aligns with respect for autonomy, because ensuring privacy and confidentiality safeguard an individual’s ability to control and protect their personal information. Respecting patients’ privacy and confidentiality was a recurring topic in many publications.34,35,37,40–42,44,45,47–51 Some authors emphasized its particular importance in palliative care settings,37,45,49 because of the intimate nature of the dying process, 37 or because confidentiality plays a crucial role in bereavement care. 45
Telehealth poses the risk of privacy breaches at multiple levels. The most frequently discussed privacy breaches are those involving storage and transmission of digital data.34–37,40–42,44,45,51 To mitigate these risks, telehealth platforms must comply with regulations, like the Health Insurance Portability and Accountability Act in the United States and the General Data Protection Regulation in Europe.44,45,51
A second privacy risk involves third parties and their presence as telehealth is being conducted.34,35,45,47,48,50,51 For example, third-party individuals living with the patient or providing tech support might overhear sensitive information, potentially undermining physician-patient confidentiality. At the same time, the privacy of third-party individuals is also at risk because they are included in these interactions.34,37,42
A third privacy concern is the inadvertent disclosure of the patient’s home environment. 49 Even though telehealth may offer more privacy than home visits, 50 inadvertent disclosure of the home environment remains a legitimate concern. Nonetheless, details about the patient’s home environment can have positive consequences. For example, interactions with healthcare providers may become more meaningful when they have details of living circumstances, and meetings between healthcare providers and the patient’s loved ones may be facilitated,38,47,52 providing insight into the patient’s social situation.38,48
Beneficence
Regarding the principle of beneficence, the included publications described potential benefits for patients, informal caregivers, and healthcare providers.
Beneficence at the level of the patient
At the patient level, we identified two main benefits of telepalliative care as discussed in the included articles. The first benefit was the potential for improved symptom management.32,33,38–40,42,44,49,52,53 Telehealth may offer better identification of symptoms, for example through remote monitoring.36,40–42,44 This is particularly important since patients often underreport their symptoms. 42 Telehealth technologies can also offer increased opportunities for self-reporting, such as through apps or chatbots, enabling patients to disclose symptoms that are most significant to them. 42 Additionally, telehealth supports symptom management through improved timing of care. Symptom changes can be detected sooner through telemonitoring,40,41,44 and interventions can be organized more promptly through telehealth platforms.32,33,41,47,50,52 This makes telehealth well-suited for urgent situations,38,50 potentially reducing emergency room visits and hospital stays.41,47,49 Furthermore, telehealth can further improve symptom management by offering patients self-management tools32,40,41 and facilitating access to multidisciplinary care teams47,52 and complementary therapies. 50
A second key benefit of telepalliative care is its potential to enhance patients’ quality of life.37,40,44,47,49,52 Telepalliative care enables patients to remain in the comfort of their homes,38,41,47,52and reduces the travel burden of patients who often experience a high symptom burden.38,47,49,51–53
Beneficence at the level of informal caregivers
At the level of informal caregivers, the most often discussed benefit of telehealth is its ability to provide increased emotional and social support, for example, through online counseling or peer support groups.33,35,38,39,44,49 This kind of support is valuable throughout both the caregiving and bereavement periods,35,39,45 as it may help alleviate feelings of isolation.35,38 Telehealth allows caregivers to receive support without leaving their loved ones or arranging additional help. 38 Another benefit is telehealth’s ability to facilitate virtual family visits,39,46,48 enabling family connections when in-person visits are not possible. Additionally, telehealth can alleviate caregiver burden.35,49 Telepalliative care can provide support by giving caregivers the reassurance of readily available support in case of emergencies33,35 and by enhancing caregiver education.35,38,39,41
Beneficence at the level of the healthcare provider
At the level of the healthcare provider, telepalliative care can enhance collaboration and communication.35,38,52 For example, it enables “a more experienced palliative care clinician to coach and support a less experienced provider who is with a patient in their home or a clinic” (p. 982) 38 and fosters integration of palliative care with local primary care. 52 Additionally, telehealth is frequently noted for its role in supporting advance care planning and goals of care conversations by enabling housebound patients, informal caregivers, family members, and various specialists to connect with each other in a timely fashion.35,36,39,47,50,51,54
Non-maleficence
The principle of non-maleficence is closely linked with the concept of risk. 31 In terms of non-maleficence, the included publications discussed multiple risks for patients and healthcare providers.
Non-maleficence at the patient level
A major concern for telehealth is its potential to replace face-to-face contact32,34–36,38–41,43,44,46,50 and thus cause harm. The unique value of in-person interactions could be lost if telepalliative care is used as a substitute. Rather than replacing traditional care, telehealth should be viewed as a complement.32,34,36,39–41,43,44,46 Multiple authors warned against imposing telehealth on patients through a rigid rule-based approach, treating it as a universal remedy.36,38–40,50 Instead, telehealth should be implemented with sensitivity to individual needs, avoiding a “one-size-fits-all” approach.36,38–40,50
Another risk is that telehealth can medicalize the home environment, transforming it into an extension of the clinic.34,36,37 This may undermine the benefit of receiving care in the comfort of one’s own home, as discussed above. Additionally, telehealth equipment might stigmatize patients by over-portraying them as ill and dependent,34,37 and it can serve as a constant reminder of declining health.36,37
Non-maleficence at the level of the healthcare provider
At the level of the healthcare provider, a primary concern with telehealth is the inability to perform physical examinations.38,43,47–50 This can complicate the gathering of relevant information,38,43,47–50 and thus harm the patient. Certain symptoms, such as new onset or severe pain, may require in-person evaluations to avoid overlooking serious complications.38,47 Nevertheless, some simple examinations, such as measuring vital signs or conducting skin assessments, might still be effectively performed through telehealth. 49
Justice
In the included publications, the principle of justice is discussed in terms of fair access, equity, and distributive justice.
Fair access and equity
Central to the principle of justice are considerations of equity and fair access to healthcare resources. Our analysis showed that telehealth could have dual impact: while it can promote equity, it also carries the risk of worsening inequities in certain situations.
Promoting equity is discussed in terms of improving access for patients facing geographical barriers in reaching palliative care services.32–35,37–39,41,45–50,52–54 Telehealth eliminates the need for travel, also removing associated costs.46–48,52,54 It also improves access for patients with high symptom burden or mobility limitations, which are common in palliative care.38,47,49,51–53 Additionally, it extends access to underserved populations, including those in rural and alternate care settings.32,34,35,38,41,43,45,47–49,52,53
While telehealth can enhance access to palliative care, it may also contribute to inequity by introducing technology-related access barriers.36,40,46,48,52,54,55 A frequently mentioned issue is the “digital divide,”34–36,45,46,48,51–55 defined by Demiris et al. 34 as the gap in computer and internet access that exists among groups differing by income, age, educational level, or other parameters. This digital divide restricts access to palliative care for patients lacking digital infrastructure.34–36,45,46,48,51–55 Similarly, because of limited digital literacy, some patients may be unable to access telehealth services.34,36,46,50–55 Also, functional limitations,34,35,40,46,50,54 or language barriers36,40,45,48,54,55 may inhibit access. To address these barriers and ensure access across diverse patient populations, multiple publications emphasized the need for usability testing.34,35,40,54
Distributive justice
Distributive justice focuses on the fair allocation of resources and is closely linked to matters of cost-effectiveness, reimbursement policies, and regulatory frameworks. Telehealth may offer advantages on multiple levels.
On an organizational and societal level, several publications suggest that telehealth can enhance cost-effectiveness.35,36,38,41,44,47–51,53 This can be achieved through cost-saving benefits,35,47–49,51,52 such as a potentially lower cost of telehealth consultations compared to in-person consultations. 35 Telehealth may also reduce no-shows and cancellations.47,48,51 Additionally, telehealth may increase efficiency,38,41,44,48,50,51,53 for instance by enabling providers to see more patients per timeframe,51,53 or by eliminating travel for home visits. 38 Moreover, it optimizes the utilization of in-person visits, reserving them for clearly necessary situations. 41 These cost-effectiveness benefits are particularly relevant given the persistent under-resourcing in palliative care, characterized by shortages of specialists and nurses.33,36,41,50,56
On the level of healthcare providers, telehealth presents “opportunities to turn previously unbillable work (i.e., phone calls) into billable work” 38 (p. 983). However, concerns are raised about liability insurance, as web-based activities may not be covered. 35 Additionally, healthcare providers may encounter licensure complications, as their licenses might not be valid outside their home regions.35,52
Sustainability and environmental impact
Matters regarding the sustainability and environmental impact of healthcare practices also align with the principle of justice. One publication discussed how telehealth may offer environmental benefits through “reducing patient travel time on the roads, decreasing fuel emission.” 48 (p. 233).
Ethical concepts and arguments related to care
Although concepts and arguments related to principles are more common in the included publications, a care approach is also represented. While some publications primarily focus on a care approach,36,39,42 others discussed concepts and arguments closely related to it.32,34,37,38,40,41,43,46–48,50–53,55–57 Fundamentally, care is about responding to vulnerability while upholding dignity. 58 Palliative care specifically addresses the needs of patients in vulnerable situations. 40 Ironically, incorporating technology in palliative care may obscure vulnerability by virtue of technology’s distractive nature, allowing caregivers “to avoid listening to that which is painful and unresolvable.” 57 (p. 292). Multiple authors agreed that telehealth should be used in a way that promotes dignity.37,40,41
The patient-provider relationship
In a care approach, there is a strong focus on relationships.58,59 In palliative care, the relationship between healthcare providers and patients is particularly important, as patients often encounter fear and uncertainty.41,56 Telehealth may enhance trust and rapport by allowing providers to interact with patients in their home environment, whereas care provided in a clinical setting may hinder this because the emphasis is on the clinician’s authority and the illness.38,47 However, in some situations, telehealth could hinder the development of therapeutic presence, trust, and rapport.46,50,55–57 In this case, risks of impersonal care41,53 and even dehumanization36,56 can occur.
One primary concern in the patient-provider relationship is that telehealth may undermine providers’ ability to recognize emotional cues and hinder empathy.43,47,50–53,55,57 This is particularly problematic in palliative care, where sensitive conversations are common.47,52 By its nature, telehealth limits nonverbal communication.38,43,48,51 To address this issue, adaptations may be necessary to compensate for this.38,45,52 Difficulties in reading emotional cues and providing empathy could explain concerns about discussing sensitive topics via video visits.38,50 On the other hand, some patients may find online environments more comforting, perceiving them as less intimidating.45,48
Another concern is that telehealth interactions lack human touch,32,34,37,38,43,46,48,50,57 depriving patients of a crucial aspect of palliative care.37,57 This lack of touch is another factor that may negatively affect the patient-provider relationship.37,38,48 However, framing the issue as a false dichotomy between high-tech and low-touch, or between cold technology and warm care, is seen as overly simplistic by some authors.33,36,39,42 Instead, they advocate for adopting a different perspective: a “high-tech, high-touch” model.33,36,39,42 This approach seeks to integrate technology while preserving human touch, making technology and personal interaction complementary rather than mutually exclusive. It agrees with the idea that telepalliative care should complement rather than replace traditional care,32,34,36,39–41,43,44,46 as discussed under the principle of non-maleficence.
A holistic approach
Another aspect of a care approach is viewing people holistically.58,59 Telepalliative care, however, may compromise this by prioritizing quantifiable aspects of care, neglecting non-physical dimensions such as existential, spiritual, and emotional concerns.36,41,42,57 For instance, telehealth might favor visible aspects like wound management over the psychosocial and spiritual aspects of palliative care.41,42 This could result in patients to be “merely treated as bodies to be measured and virtually represented” (p. 468), 36 rather than as whole persons with complex needs, and shift focus away from their personal narratives. 57
Discussion
Main findings
The present review provides an overview of the ethical concepts and arguments found in the argument-based literature on telepalliative care. Our findings support the notion that telepalliative care is not ethically neutral. In fact, the implementation of telehealth raises ethical issues that affect the core identity of palliative care in both positive and negative ways, and therefore deserve careful consideration.
On the negative side, potential disruptions to the patient-provider relationship are prominent. For example, telehealth presents difficulties such as challenges with empathy43,47,50–53,55,57 or the absence of physical touch.32,34,37,38,43,46,48,50,57 Issues like these warrant attention, as trust and rapport are fundamental to palliative care. 60 Additionally, because palliative care is inherently holistic—addressing physical, relational, psychosocial, and spiritual needs 4 —prioritizing easily measurable physical aspects over psychosocial or spiritual care,36,41,42,57 risks undermining its core principles. On the positive side, aligned with the principle of beneficence, several publications highlight benefits just as integral to palliative care. For instance, our review identified potential improvements in quality of life,37,40,44,47,49,52 a key goal of palliative care. 4 These potential benefits are supported by emerging evidence. For example, Dolan et al. 10 found that telehealth can achieve similar or improved quality of life outcomes in palliative care compared to in-person care, particularly when complementing face-to-face visits. Nevertheless, further research is needed to fully understand these effects.9,18
Reflecting on the ethical considerations surrounding telepalliative care also helps to make explicit the fundamental values we hold as a society on how serious illness and end-of-life vulnerability should be dealt with. Telehealth can either help realize these values—enabling humans to flourish—or undermine them, causing harm. 61 Consequently, telepalliative care should be implemented so that it aligns with these societal values.61,62 This can be achieved through continual discussion of, and respect for these societal values.61,62
By highlighting both positive and negative impacts, our results reveal the nuances in ethical reflections on telepalliative care. These nuances become even more evident by examining the ethical tension points identified in our review. For instance, telehealth can have dual effects on autonomy, both promoting32,33,36–41 and limiting it.32,34–36,36,37,41,42 Similarly, while telehealth may improve access to care,32–35,37–39,41,43,45–54 it can also reinforce existing inequities due to technology-related barriers.36,40,46,48,52,54,55 Additionally, while telehealth emphasizes the benefits of receiving care in the home environment,38,41,47,52 it simultaneously risks medicalizing this space.34,36,37 Finally, telehealth’s impact can vary significantly, depending on the individual. Some may find the online setting less conducive to sensitive conversations,38,50 while others may feel more at ease.45,48 These tension points illustrate that telepalliative care can be a double-edged sword, capable of both enhancing and hindering good care. Acknowledging these dual impacts does not imply that anything goes; rather, it underscores the importance of considering each patient’s specific care context to help clarify these impacts and leverage benefits while minimizing risks. Although a principlist approach provides a valuable framework for addressing broad ethical issues from an external point of view, it tends to overlook the ethical nuances that arise from the uniqueness of each telepalliative care environment.31,63 Given the sensitive nature of the dying process, providing person-centered and contextualized care is essential. Therefore, we advocate for further development of the ethics of care approach in telepalliative care, as it offers an internal perspective.59,63 This perspective incorporates individual circumstances and can therefore better accommodate the ethical nuances inherent in these particular contexts.59,63
An ethics of care approach also offers a conceptual basis for addressing open questions about telepalliative care implementation. Much of the ethical dialogue to date has focused on whether high-tech solutions are suitable for a high-touch environment.33,36,39,42 While we agree with various authors that the “high-tech, high-touch” model shows promise,33,36,39,42 a critical question remains: how can high-tech telehealth be ethically integrated into this high-touch context without undermining palliative care’s core values? Similarly, while multiple authors warn against a “one-size-fits-all” approach,36,38–40,50 they fail to provide guidance on how these technologies can be integrated ethically. To explore how telehealth can be ethically implemented to support good palliative care practices, we believe the work of Jeanette Pols offers valuable insights.64–66 Her work criticizes oversimplified binaries, such as “warm care” versus “cold technology” in the ethical evaluation of innovative health technologies,64,66 aligning with several authors in our review.33,36,39,42 Instead, she advocates for an “aesthetics of fit.” This approach posits that optimal care is contingent upon a good fit between technology and the specific context in which it is applied, 64 reinforcing our earlier point that paying attention to the particular context is imperative. In line with Pols, we believe modesty is essential in any ethical considerations regarding telepalliative care. 64 Policymakers and healthcare professionals must acknowledge technology’s unpredictable impact and remain open to the unique dynamics that arise from implementing these technologies in specific care contexts. 64 To better understand these dynamics, we agree with Pols that qualitative research methods, such as ethnographic studies, should be used to thoroughly examine how technologies function in specific care contexts. 65
Moreover, specific care contexts, along with the technologies and ethical considerations involved, are embedded in a broader socio-historical context. This is clearly explained by Vandemeulebroucke et al., 62 who stated that an ethical framework should be informed by the ethical values that are shared within this socio-historical context. Consequently, they argued that developing an ethical framework requires the integration of theoretical reflection with empirical research that captures the ethical intuitions of stakeholders concerning these technologies, as such intuitions are shaped by their specific contexts. 62 Employing qualitative research methods can serve as a platform for capturing the voices of patients, informal caregivers, or even the general public, fostering a democratic and pluralist dialogue on technological implementation. This involvement also ensures that ethical considerations are rooted in real-world lived experiences of relevant stakeholders. Moreover, further qualitative research is needed to explore citizens’ ethical intuitions concerning telepalliative care. Engaging the public from the outset can help them adapt more easily to new technologies61,62 and ensures that innovations are introduced in a manner that respects their perspectives.
Implications for policy and practice
Although this review maps the ethical considerations surrounding telepalliative care as presented in the argument-based literature to date, it does not yet take a position on which arguments are the most compelling or which ethical concepts should carry the most weight. Rather than providing direct guidance for practice or policy, the review offers a foundation for further reflection and research. 22 Nonetheless, the review identifies several potential starting points. To optimize telehealth in palliative care, a patient-centered approach appears essential, with interventions ideally tailored to the individual needs and preferences of each patient. Healthcare organizations might benefit from maintaining flexibility in offering both telehealth and in-person care, and from exploring hybrid models that combine virtual and face-to-face consultations. There also seems to be a need for more targeted training for healthcare providers—not only in the use of telehealth technologies, but also in communication strategies that could help address the limitations in physical presence, emotional cues, and empathy in virtual interactions.
Strengths and limitations
Although there are many reviews of the empirical literature on telepalliative care,7–11,14–20 to our knowledge, the present study is the first systematic review of argument-based literature on the ethics of telepalliative care. Our use of established PRISMA, 26 QUAGOL, 30 and RESERVE 27 protocols ensure that methodological rigor was at the core of our study throughout data collection, synthesis, and reporting. However, there were several limitations to our study. The use of English-language search terms may have limited the inclusion of non-English publications. Tempering this limitation, however, are estimates that of all indexed journals, 85%–94% publish exclusively or mostly in English.67,68 Another limitation is that we did not consider gray literature in our analysis, which could have provided additional insights; however, to maintain a systematic search strategy, we opted to exclude it. Additionally, many included publications were authored by researchers based in the United States and/or had medical professional backgrounds. This could have introduced some bias toward medical perspectives specific to that region. This last observation highlights a significant gap in the existing literature that future research should aim to address.
Conclusions
Recently, increased focus on telepalliative care may be explained by the growing recognition of its potential benefits. The benefits that we identified in our review include improved access to palliative care, enhanced communication, and increased cost-effectiveness, all of which challenge the idea that telehealth and palliative care are inherently incompatible. However, telepalliative care also comes with significant risks and tension points, some of which challenge core palliative care values. This latter point underscores the need for a thoughtful and cautious approach to its implementation that prioritizes ethical considerations. Overall, this review represents a new step in providing building blocks for developing an ethical framework that positively contributes to the development and evaluation of telepalliative care. Undoubtedly, further in-depth ethical analysis will be needed, preferably guided by a care-ethics approach that also considers societal values. Such an approach will ensure that telepalliative care aligns well with values specific to both particular patient contexts and socio-historical contexts.
Supplemental Material
sj-docx-1-pmj-10.1177_02692163251360115 – Supplemental material for Telehealth in palliative care settings: A systematic review of argument-based ethics literature
Supplemental material, sj-docx-1-pmj-10.1177_02692163251360115 for Telehealth in palliative care settings: A systematic review of argument-based ethics literature by Leen Krieckemans, Alice Cavolo, Michael Casaer and Chris Gastmans in Palliative Medicine
Supplemental Material
sj-docx-2-pmj-10.1177_02692163251360115 – Supplemental material for Telehealth in palliative care settings: A systematic review of argument-based ethics literature
Supplemental material, sj-docx-2-pmj-10.1177_02692163251360115 for Telehealth in palliative care settings: A systematic review of argument-based ethics literature by Leen Krieckemans, Alice Cavolo, Michael Casaer and Chris Gastmans in Palliative Medicine
Supplemental Material
sj-docx-3-pmj-10.1177_02692163251360115 – Supplemental material for Telehealth in palliative care settings: A systematic review of argument-based ethics literature
Supplemental material, sj-docx-3-pmj-10.1177_02692163251360115 for Telehealth in palliative care settings: A systematic review of argument-based ethics literature by Leen Krieckemans, Alice Cavolo, Michael Casaer and Chris Gastmans in Palliative Medicine
Footnotes
Author contributions
LK and CG were responsible for conceptualization and design, literature search, screening and selection, and data extraction and synthesis. The manuscript was drafted by LK and edited by LK, CG, AC, and MC.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The project is funded by the European Union’s HORIZON Europe research and innovation programme under Grant number: 101137221, by the Swiss State Secretariat for Education, Research and Innovation (SERI) under contract number 24.00021 (EPIC) and by the UKRI grant number 10115894. Neither the European Commission or other funding authorities nor any person acting behalf of the Commission or any funding authority is responsible for the use which might be made of the information provided on this publication.
Data management and sharing
All data generated or analyzed during this study are included in this published article and its supplementary information files.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
