Abstract
Background:
Deaths in the community are increasing. However, community palliative care out-of-hours is variable. We lack detailed understanding of how care is provided out-of-hours and the associated outcomes.
Aim:
To review systematically the components, outcomes and economic evaluation of community-based ‘out-of-hours’ care for patients near the end of life and their families.
Design:
Mixed method systematic narrative review. Narrative synthesis, development and application of a typology to categorise out-of-hours provision. Qualitative data were synthesised thematically and integrated at the level of interpretation and reporting.
Data sources:
Systematic review searching; MEDLINE, EMBASE, PsycINFO, CINAHL from January 1990 to 1st August 2022.
Results:
About 64 publications from 54 studies were synthesised (from 9259 retrieved). Two main themes were identified: (1) importance of being known to a service and (2) high-quality coordination of care. A typology of out-of-hours service provision was constructed using three overarching dimensions (service times, focus of team delivering the care and type of care delivered) resulting in 15 categories of care. Only nine papers were randomised control trials or controlled cohorts reporting outcomes. Evidence on effectiveness was apparent for providing 24/7 specialist palliative care with both hands-on clinical care and advisory care. Only nine publications reported economic evaluation.
Conclusions:
The typological framework allows models of out-of-hours care to be systematically defined and compared. We highlight the models of out-of-hours care which are linked with improvement of patient outcomes. There is a need for effectiveness and cost effectiveness studies which define and categorise out-of-hours care to allow thorough evaluation of services.
Keywords
Research on out-of-hours care to improve provision is a priority for patients and families
Out-of-hours palliative care provision is highly variable.
Systematic reviews on ‘out-of-hours’ palliative care have struggled to identify evidence on effectiveness
We provide a detailed understanding of how out-of-hours palliative care is provided, for patients with advanced illness near the end of life and their families. We define 15 categories of out-of-hours community care that detail three overarching dimensions (service times, focus of team delivering the care and type of care delivered).
We identify the improvement of patient outcomes with the provision of 24/7 specialist palliative care which provides both specialist advise and hands on clinical care.
We provide standardised categories of out-of-hours palliative care provision, and associated outcomes that can inform evidence-based commissioning of services.
We highlight the priority for future research on the effectiveness and cost effectiveness of the different categories of out-of-hours service provision identified
Background
The global demand for palliative care in the community is rising.1,2 This predicted rise is due to an ageing society, and the increasing prevalence of multi morbidity and chronic life limiting illness.2 –5 The Covid-19 pandemic accentuated this demand with a 41% increase in deaths across conditions in the community. 6
Patients and their families receiving palliative care in the community frequently rely on ‘out-of-hours’ services.7 –9 ‘Out-of-hours’ healthcare is defined as healthcare provided outside of core working hours, including; evenings, nights, weekends and public holidays. 10 The out-of-hours period constitutes 76% of any given week. 11 Internationally, community out-of-hours care is often provided by a variety of services including; family physicians, community nursing teams and specialist palliative care teams. 12 Family physicians and other services provided by generalists are key providers of care out of hours for patients and families receiving palliative care and are an integral part of out-of-hours palliative care8,12 –14
Patients with advanced disease experience a range of distressing symptoms that typically increase with disease progression and nearness of end of life. 15 The clinical priority is optimal management of symptoms and concerns to minimise distress as quickly as possible for the patient and the family. The provision of palliative care is required 24 h a day 7 days a week (24/7) to respond to distressing symptoms and ensure the person and the family receive sufficient resource to remain in their preferred place in the community at the end of life.16 –21 However, provision of community palliative care out-of-hours is highly variable, including the hours a service is available, the mode of service delivery (telephone or face to face), the composition/configuration of staff providing care, and the types of intervention available.22 –25 If a patient or family member is unable to obtain adequate and timely palliative care in the community, they will often be required to seek care from an emergency department. 15
Enabling palliative care patients and their families to feel safe and secure and remain in their preferred place of care requires care that is responsive to increasing needs, is delivered by skilled practitioners and is available at all times. 15 Access for patients and their families to specialist palliative care increases the chance of dying at home and reduces symptom distress. 18 However, access to specialist palliative care out-of-hours is highly variable.24,26,27 Bainbridge et al. in a systematic review of models of specialist palliative care, identified that access to 24/7 specialist palliative care was a component in 50% of specialist palliative care programmes considered efficacious and which resulted in a significant reduction in healthcare costs. 25
An understanding of the different models of out-of-hours palliative care is imperative to enable good quality care that supports patients to remain in their preferred place of care. Systematic reviews have identified that under-reporting of the components of intervention and comparator models are major barriers to the evaluation and implementation of models of palliative care. 19 However, reviews to date have not specifically considered the components which make up ‘out-of-hours’ community-based palliative care. The large variation in out-of-hours palliative care means it is essential to understand the models and components of ‘out-of-hours’ care, and what works best for patients and families, including considerations of cost-effectiveness.
This systematic review aims to identify and synthesise the published evidence on the components of community-based ‘out-of-hours’ palliative care for patients in the last year of life and their families and report outcomes and economic evaluation of these services.
Methods
Study design
A mixed method systematic narrative review registered on PROSPERO (CRD42019134939) and reported following Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines.28,29 A mixed method review of qualitative and quantitative research studies intended to deepen understanding of the published evidence with, for example, qualitative research studies generating new insights and knowledge from the perspective of patients and families which quantitative evidence alone could not provide 29 Narrative synthesis was used in the development and application of a typological framework. The construction of the typology drew on Guidance on the Conduct of Narrative Synthesis in Systematic Review to analyse disparate data from qualitative and quantitative studies, 30 and adaptation of Fischer et al.’s work on constructing typologies 31 The review was underpinned by Pask et al.’s adaptation for palliative care of Bronfenbrenner’s Ecological Systems Theory. 32 Drawing on this theory sought to strengthen exploration of patient and families perspectives . This adapted theory highlights the many layers that build complexity for patients and families living with advanced illness, including linkage with individual context and environmental factors, such as service-/system-level provision of palliative care.
Search strategy
We used a two-stage search strategy to optimise the balance between sensitivity and specificity of the electronic searches. Previous systematic reviews have struggled to identify evidence on out-of-hours palliative care, with for example, NICE 33 and Johnston et al. 34 Studies of home-based palliative care often do not state or describe the out-of-hours component in the title and/or abstract with detail confined to the full text. This impedes identification using only search filters and terms for ‘out-of-hours’. The two-stage search strategy intended to address this and identify the breadth of published evidence, previously little considered. The two-stage search strategy was supplemented through reference chaining of included publications and key reviews/guidance (Luckett et al. 23 and NICE 33 ), and citation searching all included papers using Scopus.
The two-stage search strategy included:
Stage one: Search strategy for electronic databases
Search strategy one involved electronic data base searches using a combination of MeSH and keyword terms identified from previous systematic reviews18,19 and piloted using scoping searches. The search strategy was refined until high numbers of eligible papers were being identified and we were able to capture the breadth of evidence and ensure a sensitive search. Four electronic databases MEDLINE, EMBASE, PsycINFO, CINAHL were searched from 1st January 1990 to 1st August 2022. The 1st January 1990 start date for searches enabled contemporary evidence to be included and innovations and changes to models of care over time to be captured. The keyword strings and full search strategy are provided in Additional File 1.
Stage two: Search strategy for trials on home-based palliative care
Search strategy two involved identification of trials on home-based palliative care, and specifically trials that included out-of-hours palliative care. The search strategy comprised hand-searching the trial publications included in the Gomes et al. 18 Cochrane Review of home-based palliative care to identify trials that included out-of-hours component. Then, updating the Cochrane search in MEDLINE from 1st January 1990 to 1st August 2022 to identify eligible trials on home-based palliative care reporting out of hours (see Additional File 1). Using and updating the Gomes et al. 18 Cochrane review enabled identification of studies on the effectiveness and cost-effectiveness of homes based palliative care with an out-of-hours component. A Cochrane review was used as the review methods are well established and considered robust, and the results detail explicitly the intervention components for home-based palliative care, including out of hours.
Eligibility criteria
We included evidence relating to adults (over 18 years) with advanced illness from malignant or non-malignant disease in the last year of life or their family caregivers receiving out-of-hours palliative care intervention or service.
A study of a palliative care intervention or service was included if community-based and included out-of-hours care, provided care outside hospital and other institutional settings as far as possible. Out-of-hours care could be described as one component of a model of care or the main component of the model of care. Provision included by primary or secondary care and by private, public or voluntary sectors. There is no internationally recognised term used for ‘out-of-hours’ provision and is variably referred to as ‘after hours’, ‘on call’, ‘outside of normal working hours’ or ‘weekend’ care. Evaluations of interventions delivering only one element of palliative care alone (e.g. medication, physiotherapy or bereavement support only), were excluded as they did not encompass the holistic nature of palliative care.
Clinical outcomes included any patient or carer centred outcomes reported and due to the limited data published on economic outcomes in this area, we were inclusive of any relevant economic outcomes.
Studies were identified for inclusion if they were in the English language. Systematic reviews and case studies were excluded but all other original research studies were included. Further details of eligibility criteria can be found in Additional Material 2.
Study selection
One investigator (AF) reviewed titles and abstracts and excluded all those clearly irrelevant. Full text review was then conducted by (AF, CPL, IG and DB) to exclude studies not meeting the inclusion criteria. Studies with uncertain eligibility were reviewed by a second reviewer (AF or CPL) and the final inclusion of studies was agreed by discussion and consensus with CE.
Data extraction and quality assessment
Data was extracted from each included study into a standardised data extraction template by AF or CPL. 50% of data was double extracted independently by AF and CPL. Data extraction included: study details (country, study stetting, study design, participant characteristics) and the components of the model of out-of-hours care. Identification and extraction of the model components were informed by the Template for Intervention Description and Replication (TIDier) guidelines 25 and Firth et al.’s specific criteria on model components for specialist palliative care.27,35 For qualitative data from qualitative and mixed method studies, the extracted data included the reported themes, illustrative quotes, and summary of the stated key findings. In line with our theoretical underpinning for this study the extraction of themes included individual context and environmental factors as well as system level descriptions of the service. The extraction of data reporting economic evaluation, was informed by the Consolidated Health Economic Evaluation Reporting Standards (CHEERS) 36 and included formal and informal service use and service outcomes (e.g. unplanned hospitalisation).
Qualitative and quantitative research studies were assessed using the validated tool, Quality Assessment Criteria for Evaluating Primary Research Papers (QualSyst), using respective the checklists for quantitative or qualitative studies, 37 or in mixed method studies, using both checklists. The checklists each state 14 items scored from 0 to 2. The percentage of the total possible score indicates quality grade. Percentage of the total possible score indicates quality grade: <50% low; ⩾50 and <70% medium; and ⩾70% high. For quality improvement studies we used the Quality Improvement Minimum Quality Criteria Set (QI-MQCS) that details 16 domains for quality assessment. 38 Assessment of quality did not inform the development of the typological framework as this is a tool for systematic categorisation of described/used models of care, however quality assessment did inform the understanding on the quality of evidence when considering the linkages with outcomes reported by RCT’s and controlled cohorts (Table 2).
Data synthesis
The data synthesis sought to construct a typology of out-of-hours care. We argue that the application of a typological framework is helpful for comparatively analysing the complex variety of out-of-hours services and to assess advantages and disadvantages of certain health care systems. A typology is a conceptual framework for sorting instances of a phenomenon according to (dis)similarities on various attributes into different categories. 39 Well-constructed typologies are a useful way to order and reduce empirical complexity, systematically assess diversity and detect patterns,39,40 used for example to describe the multi-faceted dimensions of systems for long term care.31,41
A narrative synthesis was used to analyse the breadth and heterogeneity of the evidence included from quantitative and qualitative studies to answer the stated aims on what were the components of out-of-hours service provision and the reported outcomes. 30 The steps for narrative synthesis involved: a preliminary synthesis of extracted data using textual description and tabulation of the identified components of the models of care for all included studies. The initial construction of the typology was informed by Fischer et al.’s work on the formation of dimensions. 31 Box 1 defines the terms used in the typological framework. 30 The components and themes identified in the narrative synthesis were examined and grouped into overarching dimensions. Dimensions were refined to strengthen coherence with existing evidence.42,43 The overarching dimensions and initial typological framework was then discussed and agreed with stakeholders including family carers as Patient and Public Involvement (PPI) representatives, and the project steering group comprising clinical-academics and researchers from primary care, community care and palliative care. The outcomes (RCT and controlled cohort study outcomes, economic/service utilisation) and perceived benefit (qualitative themes), were then mapped onto each category formed by the typological framework (Figure 2).
Definitions of terms used in the typological framework for out-of-hours care for patients with advanced illness.

Results
After deduplication 9259 titles and abstracts were screened (Figure 1: PRISMA 2020 flow diagram adaptation) and 64 papers reporting 54 different services were included (see Table 1). The 64 papers included 38 quantitative studies (6 RCT’s, 5 controlled cohort, 24 observational and 3 pilot studies), 14 qualitative studies, 4 mixed methods, and 8 service development papers (see Additional File 3 and Additional File 4 for further detail). The 18 studies reporting qualitative findings included perspectives of the patient (n = 3), family (n = 2), both patient and family (n = 4), a combination of patients, family, and healthcare professionals (n = 4) or healthcare professionals only (n = 5). The studies were mainly reported from the UK (n = 24), Australia (n = 11) Sweden (n = 7), USA (n = 7), and the Netherlands (n = 7) (see Additional File 4). Description of a theoretical underpinning in a study was generally limited to defining palliative care with no indication of any further theoretical basis. We now present the identified components of services that make up the models of care described in all included papers. We present the newly developed typological framework followed by a narrative synthesis of the qualitative and quantitative results for each identified category of care. We then present outcomes data including considerations of effectiveness and service utilisation/ economic evaluation.
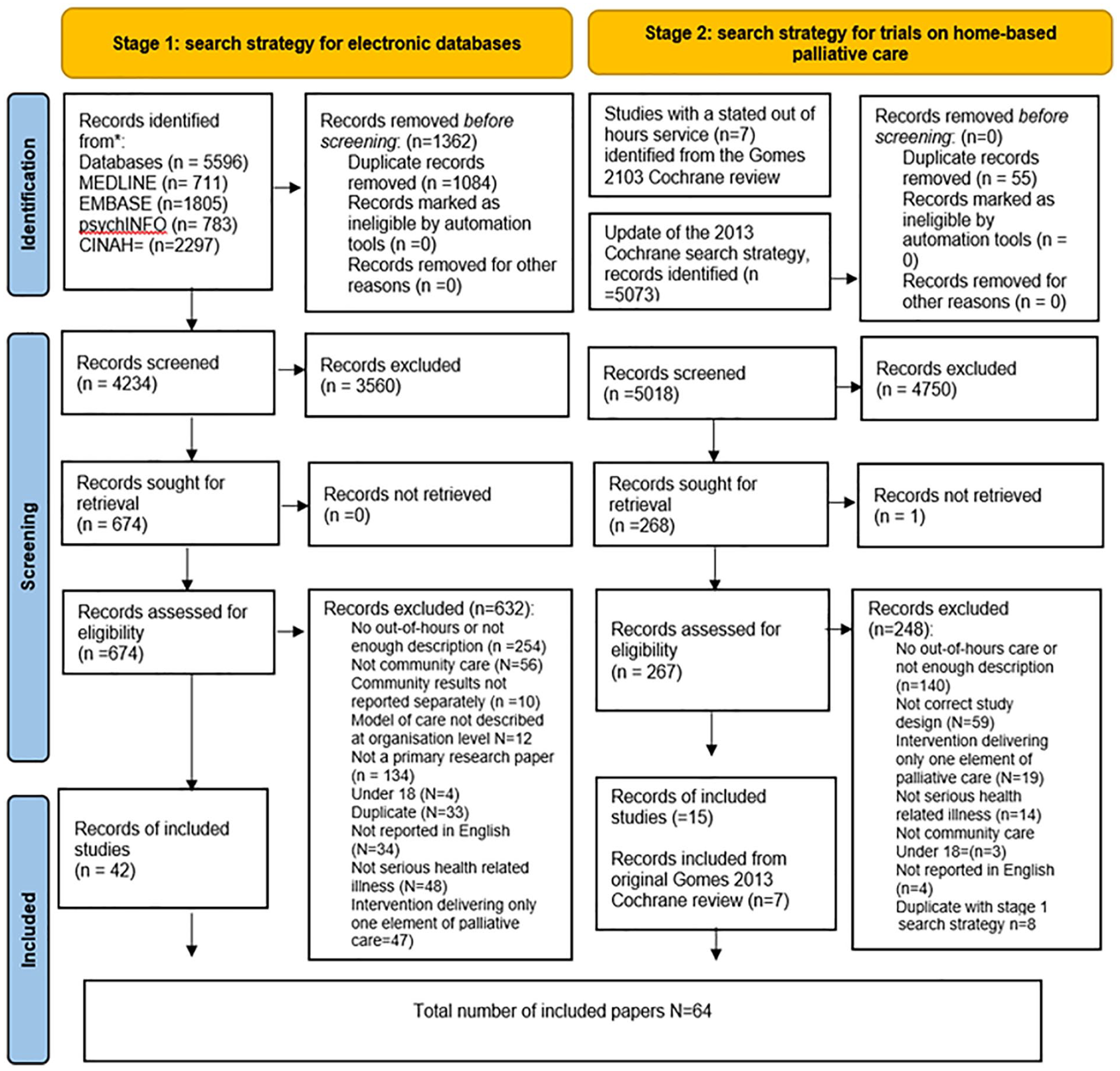
PRISMA 2020 flow diagram adaptation. 28
Components of the identified models of care.
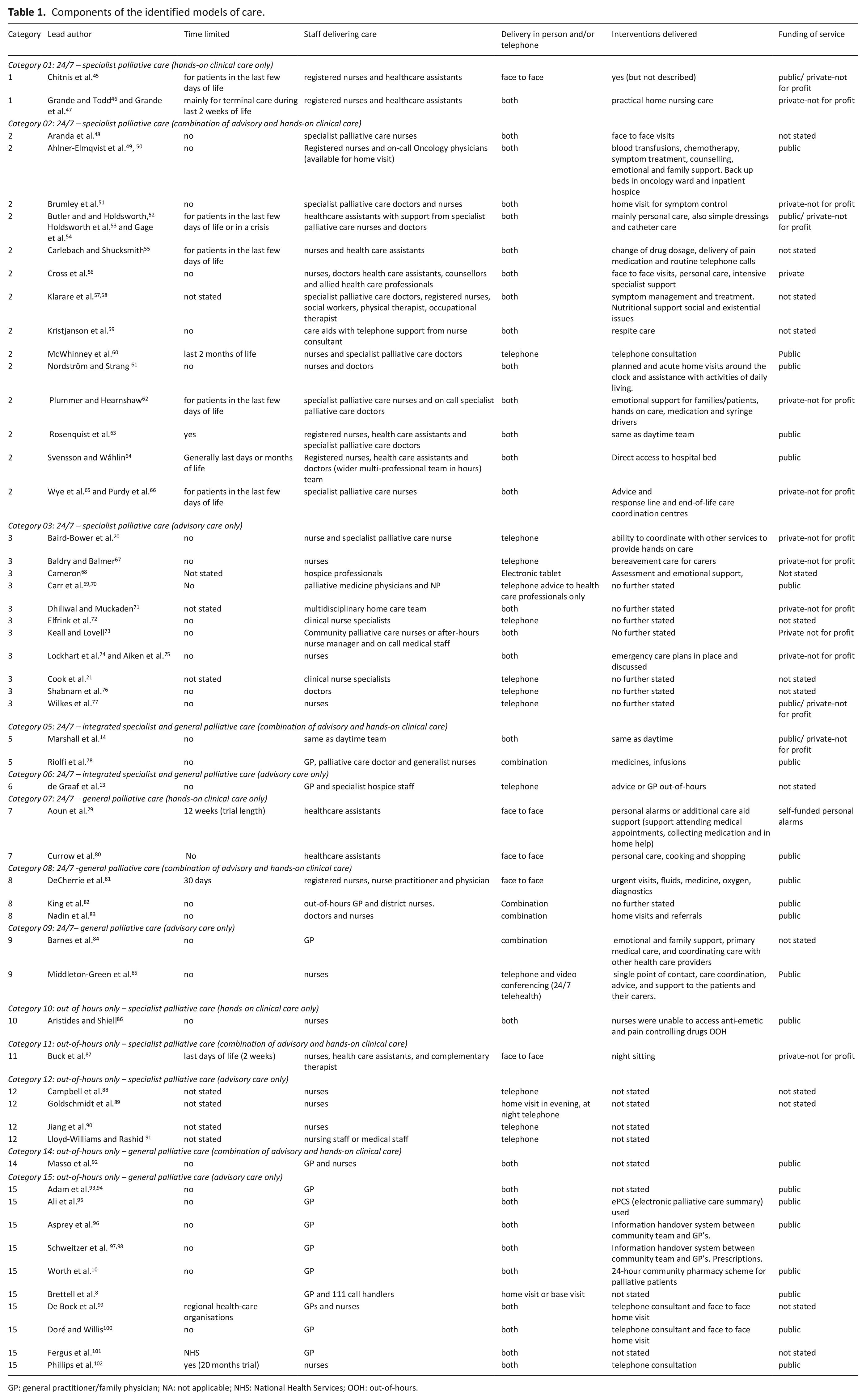
GP: general practitioner/family physician; NA: not applicable; NHS: National Health Services; OOH: out-of-hours.
Components of care and the dimensions of out-of-hours care
Table 1 details components of out-of-hours care reported in the studies. Studies differed substantially in their level of detail in the description of the out-of-hours components. From the components we constructed 3 overarching dimensions of out-of-hours care, comprising: (1) service times (if a service was provided during both daytime and out-of-hours or if it was only an out-of-hours service); (2) the focus of the team delivering the care (specialist palliative care/dedicated palliative care, general palliative care or integrated specialist and general palliative care) and; (3) the type of care delivered (if it was advisory only and/or hands-on clinical care). These three dimensions were defined (Additional File 5), applied (Additional File 3) and used to construct the typology formed from 15 multi-dimensional categories as shown in Figure 2.
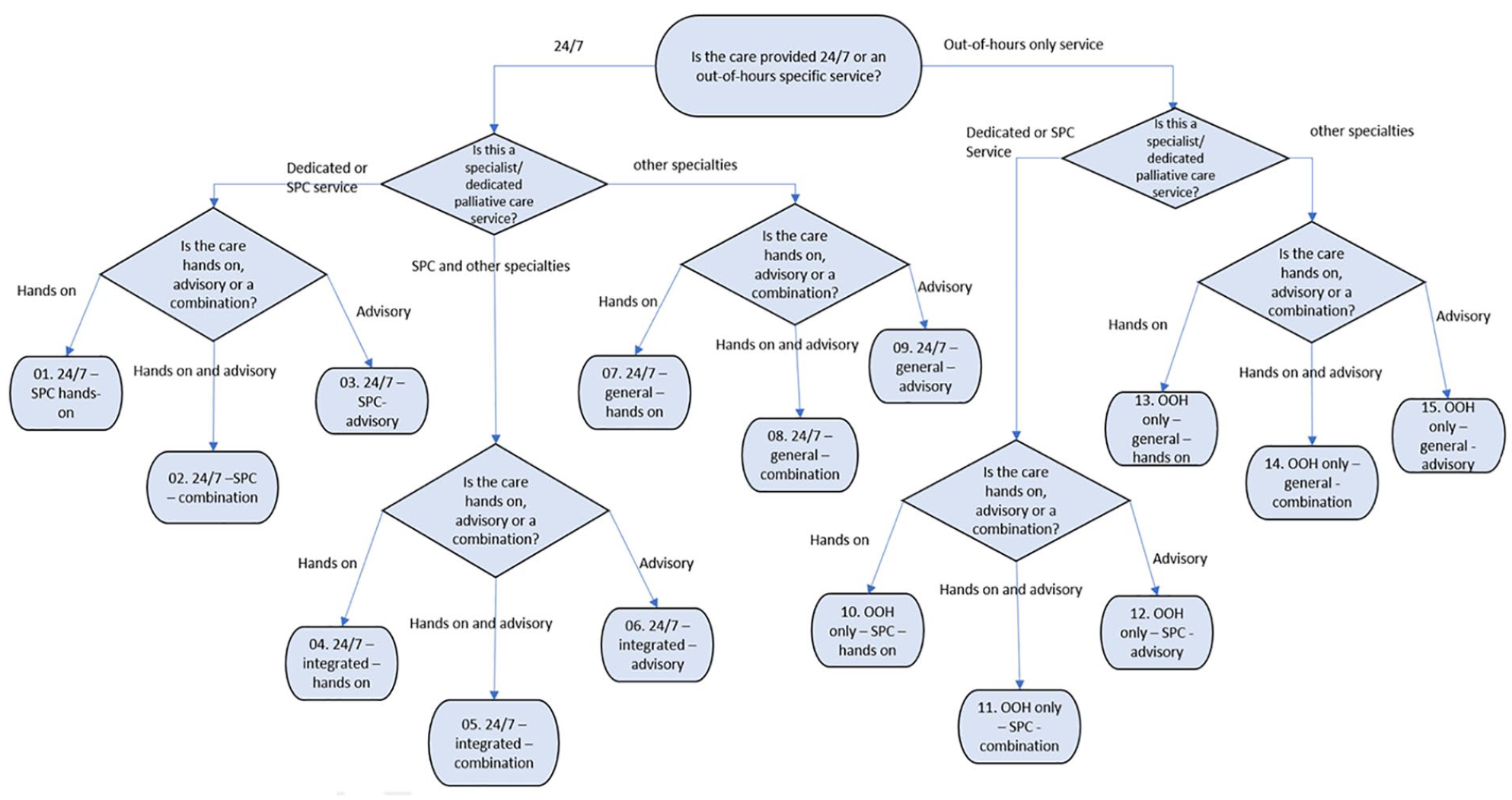
Flow diagram of the service characteristics and components to form a typological framework of out-of-hours service provision.
Similarities and differences between the identified categories of care
No eligible published papers were identified for category 4 (integrated specialist and general palliative care, hands-on clinical care only) or category 13 (out-of-hours only-general palliative care, hands-on clinical care only). These categories are detailed in the typology as we are aware of examples of clinical practice that echo these categories and anticipated that future research and clinical care is likely for these categories with increasing emphasis on integration between services. The below text reports a synthesis of the published evidence from the qualitative and quantitative data for each identified category of care from the typological framework.
Category 01: 24/7 – specialist palliative care (hands-on clinical care only)
Care was provided mainly for patients in the last few days of life.45 –47 The delivery of care was mainly uni-disciplinary by specialist palliative care nurses and/or health care assistants. No detail is given on the wider involvement of a specialist palliative care multi-disciplinary team.
Category 02: 24/7 – specialist palliative care (combination of advisory and hands-on clinical care)
All papers reporting category 2 care employed nurses to deliver the services, with 10 of the services (14 papers) having access to a specialist palliative care medical doctor out-of-hours.49 –54,56 –58,60 –64 Three services (four papers) were specifically to care for patients in the dying phase.55,62,65,66 Two key themes were identified of sense of security and high-quality coordination of services. Patients and families knowing they could contact the palliative care service 24/7 provided a sense of security 64 ; ‘And then I have a phone number and say my name. I don’t need to say more . . . they know immediately what it’s about. I’ve admired that many times’. (P3). 64 Patients/families viewed proactive routine telephone calls out-of-hours as helpful 55 as convened sense of not feeling forgotten55,57 and of being known to the service 57 ‘I don’t know if I could have managed . . . it was so helpful for someone to ring me up every night [to ask] if I needed any help’. (Patient 5). 55 High quality coordination of services enabled patients to receive appropriate care and feel comforted 65 with support and reassurance being quickly avalible64,66,‘It was absolutely fantastic that everything was linked together so that there wasn’t any more . . . if it hadn’t been linked it would’ve worked, I suppose, like everything else in healthcare with referrals here and there’ (P14). 64
Category 03: 24/7 – specialist palliative care (advisory care only)
This category reported providing a 24/7 specialist palliative care service with advisory care. These services were available to all patients receiving palliative care, and not limited to the dying phase. One service reported only being available for health care professional’s advice. 70 Services were generally provided over the phone with three services also offering home visits.71,73,74 One service used only an electronic tablet to provide 24/7 access to hospice staff for patients at home. 68 Some services reported the ability to coordinate with other services to provide hands on care in the patient’s home. Most services were delivered by registered nurses. Cameron identified a sense of ‘comfort’ for patients/families by always knowing care was available, 68 but integration and continuity were impeded with lack of access to shared patient records out of hours, ‘I don’t have the profile of the patient in front of me when I receive calls at home . . . the one who is calling, may not even know the diagnosis . . .’ (N) 76 .
Category 05: 24/7 – integrated specialist and general palliative care (combination of advisory and hands-on clinical care)
Both papers reporting 24/7 integrated care between specialist palliative care and generalist services detailed providing advisory and hands on clinical care. Care was delivered by multidisciplinary teams. This enabled the services to provide numerous interventions to patients and families out-of-hours.14,78
Category 06: 24/7 – integrated specialist and general palliative care (advisory care only)
De Graaf et al. reported a service providing 24/7 advisory care from an integrated multidisciplinary team (GP and hospice service). 13 De Graaf et al.′s retrospective cross-sectional evaluation reports a positive experience of integrated service and team work between specialist and general teams which supports patients to die in their preferred place of death. 13 However, there were no eligible qualitative papers to give patients and families perspectives on this model of care.
Category 07: 24/7 – general palliative care (hands-on clinical care only)
Studies by Aoun et al. 79 and Currow et al. 80 reported services that provided extended visits by care aids (healthcare assistants), including a sitting service, and personal and supportive care. These services were uni-disciplinary with care delivery by unregistered care aids with a specific focus on meeting activities of daily living, such as personal care needs ac Care aids were provided for patients who lived alone to support personal care.
Category 08: 24/7 – general palliative care (combination of advisory and hands-on clinical care)
Services reported in this category were provided by generalist services and comprising multi-disciplinary teams. In King et al. family members generally reported care as high quality and supportive; ‘“Are you alright?. . . and if you think you need us again, ring us up, we’ll be straight here, no problem”, and I thought that was very good of them because they were really fantastic nurses’. (Thelma, wife and carer). 82 However, family carers reported concerns of not feeling listened to and out-of-hours family physicians being little informed about the patient, 82 for example, ‘Well they came and they said “we’re going to turn him on to his side”, and I said “he can’t breathe on that side” and I was getting a bit worked up I think about it. I said “he can’t breathe on that side” . . .and she said “well I’ve had my instructions that he has to be turned over”’ (Phyllis, wife and carer).
Category 09: 24/7 – general palliative care (advisory care only)
Both services described providing care coordination. Barnes et al.’s study described a service led by family physicians providing out-of-hours care to patients registered with their practice. 84 This contrasts to category 15, were family physicians provided a specific out-of-hours service only.
Category 10: out-of-hours only – specialist palliative care (hands-on clinical care only)
Aristides and Shiell’s study from 1993 details provision of out-of-hours specialist palliative care hands on care, but highlighted challenges of accessing to prescriptions for medication for symptom management out-of-hours. 86
Category 11: out-of-hours only – specialist palliative care (combination of advisory and hands-on clinical care)
Buck reported a night sitting service which provided patients and families with both advisory and hands on clinical care by a multidisciplinary team and described demand outstripping supply by twice as many night care episodes requested than could be provided.
Category 12: out-of-hours only – specialist palliative care (advisory care only)
All four services in this category were provided by nurses,88 –91 with one service also supported by medical staff 91 Three out of four services provided only telephone advice.88,90,91 Lloyd-Williams and Rashid’s study using a telephone line was only for health care professionals. 91 None of the services stated providing any additional interventions other than advise.
Category 14: out-of-hours only – general palliative care (combination of advisory and hands-on clinical care)
Masso et al. details a service provided by a generalist multi-disciplinary team that provided both advisory and hands on clinical care.92,103
Category 15: out-of-hours only – general palliative care (advisory care only)
This category was provided by generalist out-of-hours services and offered advisory care. Eight of the services (10 papers) were provided by GP’s/family physicians,8,10,93 –98,100,101 with only one service provided by nurses, 102 and one provided by nurses and family physicians. 99 One service provided only face to face care, 8 with the remainder offering both telephone and face to face services. Six qualitative papers reporting interview findings (n = 1 patient/family only, n = 2 staff only, 3 = patients/family and staff). The key theme identified in this category was the importance of continuity of care.10,94,99,101 Including the preference of seeing own patients/ family physicians,94,99,101 and the challenges both family physicians and patients faced in difficulty of accessing patients notes,10,94,99,101 reluctance of patients and families to contact out-of-hours services due to lack of continuity of care and needing to re-tell their story and feeling unknown10,94,101 ‘I just had all this hassle . . . and I was reduced to tears. If you could get a bit more help when you phone without all the questionnaire things, you know.’ (Wife of patient 6). 101 The importance of family physicians having easy access to specialist palliative care for advice was also highlighted.98,101
Effectiveness on the stated outcomes
Eight Randomised Control Trials or controlled cohort studies (nine papers) evaluated the effectiveness of the out-of-hours service model on the stated outcomes (Table 2). Most studies reported service outcomes, of place of death and service use. Only one study reported patient health -related outcomes of physical and mental functioning. 75 No studies reported family caregiver outcomes. Five studies reported randomised control trial/quasi-experimental design.
Outcomes reported by RCT’s and controlled cohorts.
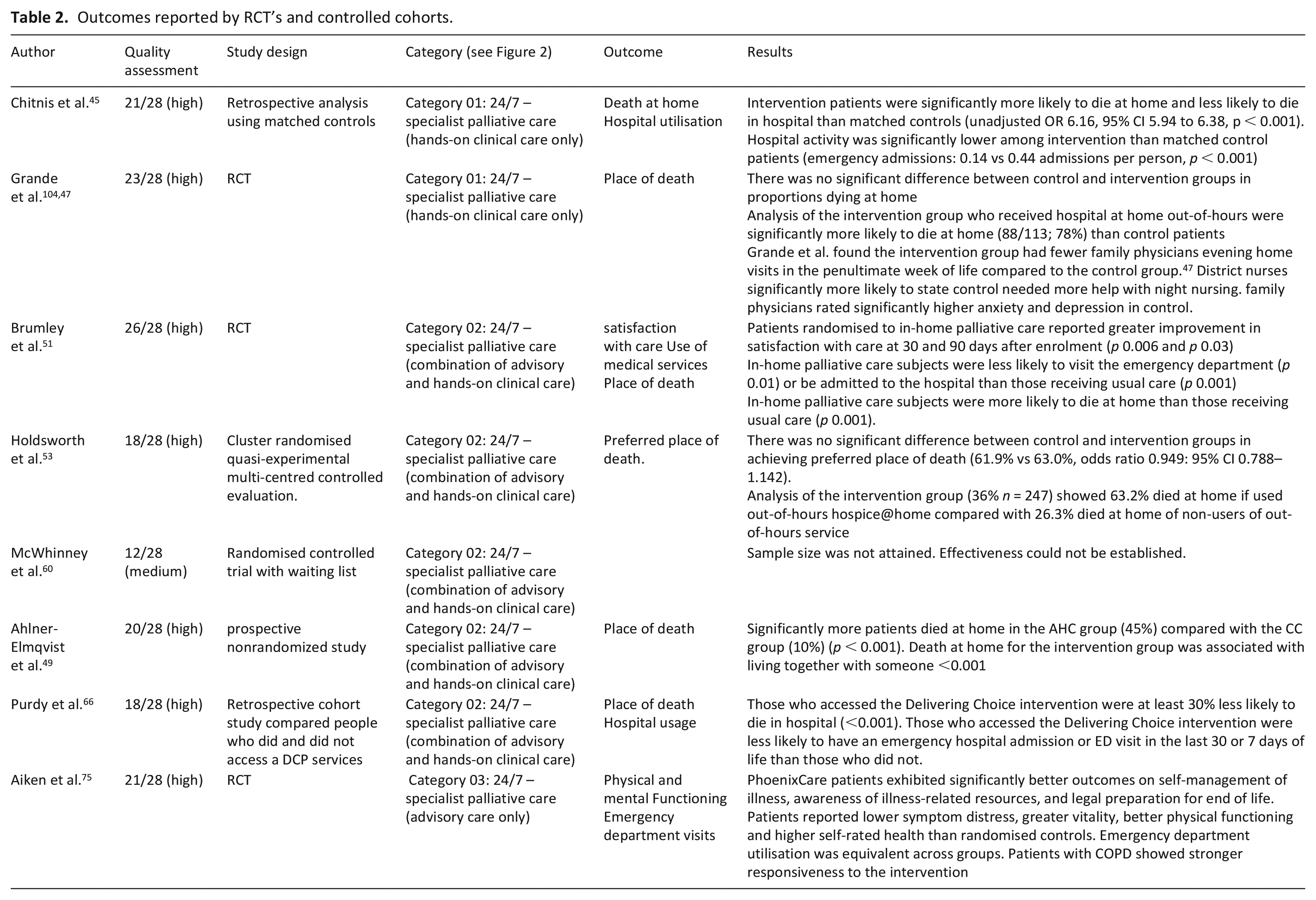
All of the services reporting effectiveness reported provision of 24-h care provided by specialist palliative care with the most evidence of effectiveness provided for category 2: where the services are provided 24/7 by specialist palliative care and are able to provide both hands on clinical care, alongside advisory care. Five papers reported a significant effect on the stated outcomes.45,49,51,66,75 Six services provided category 2 care (24/7 – specialist palliative care – combination), one failed to reach sample size, 60 three demonstrated effectiveness on the stated outcomes.49,51,66 Holdsworth et al. failed to detect change at level of significance on the stated primary outcome of (preferred) place of death. 53 However, Holdsworth’s analysis of the intervention arm, showed that patients who accessed the out-of-services has a higher attainment of preferred place of death compared to non-users (63.2% vs 26.3%). Purdy et al. also reported those who accessed the intervention were 30% less likely to die in hospital. 66 Two papers reported category 1 care, but only one demonstrated effectiveness on the stated outcomes. 45 Grande et al. failed to detect change at a level of significance on the stated primary outcome of (preferred) place of death. 104 However, further analysis of the intervention arm showed that patients able to access the hospital at home intervention were more likely to die at home compared with the control group (88/113; 78%, control: 25/43 (58%). Aiken et al.’s trial reported category 3 care: 24/7-specialist palliative care-advisory only. The results indicate lower symptom distress and better functioning for patients in the intervention group compared to the control. However, emergency department usage was equivalent between the two groups.
Economic evaluation and eservice utilisation
Nine studies provided a form of economic evaluation of out-of-hours services with advanced illness in the last year of life (see Table 3). Overall, the quality of economic methodology adopted was poor (see Additional File 6 for CHEERS Checklist). However, cost implications from two studies with relatively rigorous economic approaches were mixed.45,54 Hospital costs were lower (£1111, 95% CI 1071–1155) among people who received home-based nursing care at the end of life than matched control group who did not. 54 There was no difference between users and non-users of the Hospice Rapid Response Service except that users who were referred to the service near death had higher costs. 45 Although methodologically challengeable, Currow et al. estimated that potential cost saving would be AUS$11,379/year when a specialised palliative care service (free-of-charge, around-the-clock, live-in-support person) was provided. 80
Service utilisation and economic evaluation.
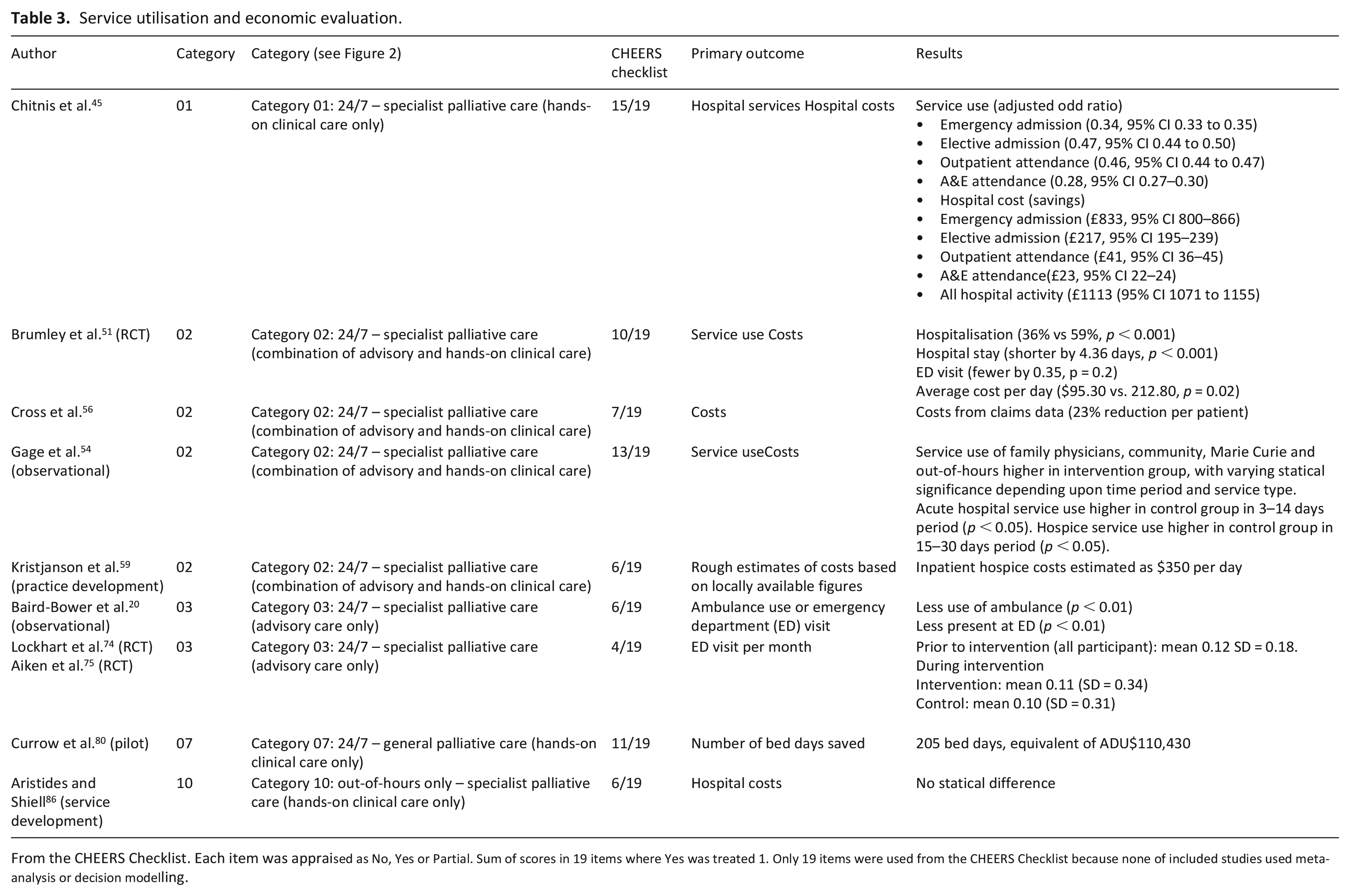
From the CHEERS Checklist. Each item was appraised as No, Yes or Partial. Sum of scores in 19 items where Yes was treated 1. Only 19 items were used from the CHEERS Checklist because none of included studies used meta-analysis or decision modelling.
Quality of reporting of economic evaluation improved in more recent studies compared with earlier studies. Recent studies provided more rigour in the reporting, detailed: greater breadth of service use and associated costs (primary or community care, and hospital care); sources of unit costs and year of costs and time and duration of the study. We intended to consider either unpaid informal care provided by family/friends or out of pocket payment or lost productivity, because the perspective of economic evaluation was not determined at the beginning, to ensure all studies including a form of economic evaluation could be included. Only one study included caregiver costs as assumed average weekly wage and probabilities of continuing to work. 80 No study conducted cost-effectiveness analysis with primary outcomes in the study and costs, or calculated impact on health-related quality of life such as quality adjusted life years. A decision analytic model was not applied by any studied included (CHEERS Checklist was accordingly amended).
Discussion
This review has systematically identified and synthesised the components used to provide out-of-hours community care for patients with advanced illness. The identified components have been translated into three overarching dimensions to construct a typology. The typology provides a unique template to define and categorise services available out-of-hours to patients with advanced illness and their families. This template enables service delivery models to be clearly described and understood, allowing for comparison and evaluation between models of patient and family outcomes and cost-effectiveness.
This typological framework allows identification and delineation of different service delivery models for out-of-hours care. This delineation is vital to define, test and compare different service types in experimental studies. Studies consistently identify the wide heterogeneity in service provision out-of-hours.24,27,105 The developed typology enables an evidence base to be built for different types of service provision. Brereton et al. assert that models of palliative care are first defined and then tested. 19 This typology provides the framework to define different models of service provision and test effectiveness and cost-effectiveness.
Although current evidence of effectiveness around out-of-hours care for this population is limited, we were able to identify several randomised controlled trials and controlled cohorts reporting effectiveness. All of the studies reporting effectiveness reported provision of 24-h care provided by specialist palliative care, with the most evidence of effectiveness provided for category 2: where the services are provided 24/7 by specialist palliative care and are able to provide both hands on clinical care, alongside advisory care. Unfortunately, evidence from economic evaluations and service utilisation for out-of-hours services was inconclusive due to limited number of studies and poor quality. Previous research has highlighted the importance and need of high quality economic evaluation of community palliative care provision.34,106
The typology was constructed from Three overarching dimensions comprising: (1) Service times (if a service was provided 24/7 or if it was only an out-of-hours service); (2) the focus of staff delivering the care (specialist palliative care/ dedicated palliative care, general palliative care or integrated) and (3) the type of care delivered (if it was hands-on clinical care or advisory).
Dimension one) Service times
24/7 access to care for palliative patients has previously been reported as a component of home care that results in significant cost reduction. 25 Our review reiterates the importance of 24/7 care for this population. Our qualitative synthesis has also highlighted the importance of patients and families feeling known to a service providing out-of-hours care. Our findings echo those in Sarmento et al.’s meta-ethnography 42 and a recent Delphi study. 107 Feeling known out-of-hours meant, patients and families didn’t need to retell their ‘story’ to different service providers and care was well coordinated between services providing out-of-hours care. Shared patient records were deemed important, as were services giving consistent information to patients and families, and patients receiving responsive and appropriate care aligned with their priorities and preferences.
Dimension two) Focus of staff delivering the care
There is rising demand for community healthcare with ageing populations globally and increasing proportion of people dying at home and in care homes.4,5 This requires provision of specialist/dedicated palliative care services for patients with complex needs, and services providing general out-of-hours palliative community services that are able to improve outcomes for patients and their families. 8 This review has identified many papers which detail both general and specialist/dedicated services providing palliative care. Although more research is specifically needed on effectiveness of the different categories of general palliative care identified in this review. A recent review has highlighted the importance of a capable workforce that works collaboratively across disciplinary boundaries, to provide comprehensive and ongoing multidimensional assessment. 108 Further research is also needed on models of integrated working out-of-hours between specialist and general services for palliative care, to ensure care provided is well coordinated.
Dimension 3) Type of care delivered
Most evidence on improved outcomes for patients was for category 2 services, which provided a combination of both hands-on clinical care and advisory care. This finding aligns with a recent Delphi study where patients, family members and healthcare professionals highly ranked the importance of hands-on clinical nursing care by community and district nurses highly. 107 This also echoes patients and families assertion for high quality coordinated care that meets their needs (whether this be advisory or hands on clinical care) and ensure sense of comfort and safety.65,66
A strength of this work is the extensive systematic search strategies used to identify evidence and the inclusion of the many types of out-of-hours services provided across the world in the community to patients and families with advanced illness in the last year of life, including primary c services as a vital resource in the last year of life. 12 This review included a range of study designs to ensure a synthesis that captures the breadth of published literature on models of service provision. This breadth enabled identification and delineation of out-of-hours service delivery models, and consideration of outcomes. Previous reviews have struggled to identify evidence on effectiveness.33,34 Randomised trials have proved to be difficult to undertake with success in this population. 46 It is postulated that the challenges of randomised trials (including recruitment, attrition, ethics, and heterogeneity) lead to a lack of clear evidence, and requirement to include and undertake well-conducted observational studies that provide useful evaluation data. 109
Some limitations to this study should be highlighted. Firstly, our methods were limited by two reviewers independently reviewing a sub-set of articles to calibrate the eligibility criteria and agree consensus. Although efforts were made to ensure consistent agreement between reviewers by cross-checking a subset of papers at each stage and discussing with a third reviewer disagreements, it is possible that reviewers differed slightly in their interpretation of the inclusion and exclusion criteria. Secondly our search strategy did not include unpublished literature or full reference checking.
In addition, this review was only able to synthesise information reported in the included papers. Information describing the service was at times poorly described, with few papers reporting using the TiDIER guidance for complex interventions. 35 This means If a paper has not reported providing a component of care it does not mean that it is not provided, simply it was not reported. One component we were consistently unable to capture was the complexity of integration between different service providers. Patients and family members often receive multiple services at one time. However, this was rarely described or with little detail. Further research is needed to understand these complex relationships and the impact they have on service delivery for patients and family members. Integration needs to be more widely reported and understood when describing a services model of care, especially in the context of upcoming legislative proposals focusing on integration. 110
This review has provided a typology which provides a framework to define and categorise services. More high-quality qualitative research investigating how patient and family experiences are related to the models of care of care they receive is needed. Further research is also needed to explore the integration of specialist and general palliative care and how this impacts the care patients and families receive out-of-hours. Furthermore, effectiveness and cost effectiveness studies are needed for our identified categories of service provision to ensure the funding of services that are effective and provide cost-effective care.
The development and application of our categories of service provision will enable policy makers, commissioners, and service providers to understand, identify and compare existing models of service provision. Defining and comparing service provision and considering effectiveness and cost effectiveness is a vital step to address inequalities in access to palliative care out-of-hours.
Footnotes
Acknowledgements
With thanks to our Patient and Public involvement group for their review and feedback during the development of the typology and to Dot Brown, research associate, for her help with the review searches.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study forms part of the ‘Understanding and improving community-based palliative care outside of normal working hours’ project funded by Marie Curie Research Grants scheme MCRGS-20171219-8011. This study is also supported by the National Institute for Health and Care Research (NIHR) Applied Research Collaboration South London (NIHR ARC South London) at King’s College Hospital NHS Foundation Trust. Fliss Murtagh is a National Institute for Health and care Research (NIHR) Senior Investigator. Catherine Evans is funded by Health Education England/NIHR Senior Clinical Lectureship. The views expressed are those of the author(s) and not necessarily those of the NIHR or the Department of Health and Social Care.
