Abstract
Objective
To examine the feasibility and acceptability of Neuromuscular Bridges, a personalised self-management support intervention adapted for people with neuromuscular disorders, and to explore contextual factors influencing its implementation in specialist care.
Design
A hybrid type II feasibility study employing mixed methods to evaluate clinical and implementation feasibility, incorporating quantitative outcomes with qualitative process evaluation.
Setting
A specialist neuromuscular tertiary centre in the United Kingdom.
Participants
Thirty-three adults with diverse neuromuscular disorders and six trained clinicians (physiotherapists and clinical nurse specialists).
Intervention
NM-Bridges, a co-designed, person-centred self-management support intervention delivered in a single clinical consultation, underpinned by the Bridges approach and Social Cognitive Theory.
Main measures
Recruitment, retention, fidelity, and patient-reported outcomes were collected at baseline, post-intervention, and 3-month follow-up. Implementation was assessed using validated instruments and qualitative interviews.
Results
Of 106 eligible patients invited, 33 (31.1%) enrolled, with full retention and no missing data. Quantitative outcomes showed moderate pre- and post-improvements in patient-centred care, especially goal setting and activation. Small positive changes were noted in social participation, emotional well-being, mood, and self-efficacy, with effects generally sustained at follow-up. Fidelity was high, and implementation measures indicated strong clinician engagement. Qualitative data reinforced these findings, highlighting collaboration, relevance, and acceptability within routine care.
Conclusion
NM-Bridges was feasible and acceptable within specialist neuromuscular care. By integrating clinical outcomes with implementation learning, this hybrid feasibility study provides early evidence and a foundation for future evaluation of self-management support as a relational and sustainable component of neuromuscular rehabilitation.
Keywords
Introduction
Neuromuscular disorders are a diverse group of rare conditions affecting muscle and peripheral nerve function, leading to progressive weakness, fatigue, and, in many cases, multisystem involvement. 1 Though individually rare, neuromuscular disorders collectively impact approximately 110,000 people in the United Kingdom and ∼15 million people globally.2,3 These lifelong conditions carry considerable physical and psychological burden, and while advances in diagnostics and disease-modifying therapies offer new promise, most remain incurable.1,4 Care therefore focuses on symptom management, independence, and quality of life, requiring coordinated multidisciplinary support. Yet evidence-based interventions that address the broader impact of living with neuromuscular disease remain limited.
Self-management support has become integral to the management of long-term conditions such as stroke, diabetes, and arthritis, where relational and collaborative approaches have been shown to enhance confidence, engagement, and well-being. 5 Effective self-management is now understood as a partnership that strengthens shared decision-making and builds capability, rather than as an individual responsibility.6,7 However, programmes often remain constrained by limited personalisation, service pressures, and variability in clinician training. 6 Research in other progressive neurological conditions such as multiple sclerosis and Parkinson's disease has shown how self-management interventions can improve quality of life and psychological adjustment.8,9 Yet neuromuscular conditions differ in important respects: they are individually rare, heterogeneous, often of earlier onset, and require ongoing adaptation over many decades.1,10 People living with these conditions frequently face fluctuating function, uncertainty, and limited access to informed local care, demanding tailored approaches that are sensitive to both the clinical and psychosocial realities of rare disease.10–12
To date, self-management interventions for people with neuromuscular disorders remain extremely limited in both number and scope. While some programmes have been trialled, they are often small-scale, lack personalisation, or are not embedded into routine care.13,14 None have explicitly focused on tailoring delivery to the structure of specialist neuromuscular services or evaluating the implementation process in parallel with clinical outcomes. Addressing this gap, this study aims to evaluate the feasibility of delivering and implementing NM-Bridges, 15 a co-designed self-management support programme for people living with neuromuscular disorders, adapted from the established Bridges approach. 16
Methods
Ethical approval for this study was granted by Yorkshire & The Humber - Bradford Leeds Research Ethics Committee, reference 21/YH/0092. All participants (patients and clinicians) provided informed consent. This study was registered with the International Standard Randomised Controlled Trial Number (ISRCTN) registry (trial ID: ISRCTN14208138).
Participants and setting
This study was conducted at a specialist neuromuscular tertiary centre within a large NHS teaching hospital in London, which provides multidisciplinary care for individuals with a broad range of neuromuscular disorders. Participants included both patients and clinicians from the centre. Patients were eligible if they were aged 18 years or older, had a confirmed diagnosis, were currently receiving care at the service, and had the capacity to provide informed consent. Clinician eligibility criteria included being a health professional involved in the care of patients at the centre and a willingness to complete training and deliver the intervention. Eligible patients were identified through the clinical service database and invited to participate through one of three recruitment routes: during in-person clinic appointments, via the hospital's secure digital patient portal, or through postal invitation. Clinicians were recruited via internal email, with six training places available for participation in the NM-Bridges programme. These were allocated on a first-come, first-served basis, and all six places were filled without difficulty.
Study design
An embedded experimental mixed methods design was used, an approach commonly applied in health-services research. 17 A sequential two-phase structure combined quantitative and qualitative components: participant-reported outcome measures were collected at baseline (T1), immediately post-intervention (T2), and at 3-month follow-up (T3), with post-intervention qualitative interviews used to explore the experiences of patients and clinicians. 18
The feasibility of NM-Bridges was assessed using a single-arm pre- and post-design, selected to align with the study's feasibility focus and pragmatic constraints. To capture both intervention and implementation dimensions, the study was conducted within a hybrid type II framework, 19 enabling concurrent evaluation of intervention outcomes and implementation processes. 20 Full details of design decisions, including justification for the exclusion of a controlled design and specification of the implementation strategy package, are available in the published study protocol. 21
Theoretical framework
Normalisation Process Theory 22 was used to examine how NM-Bridges could be embedded and sustained in specialist neuromuscular care, providing a lens to explore the collective and individual work involved in implementing new practices. It informed the development of qualitative topic guides and analysis of implementation data. The Theoretical Domains Framework 23 was used to identify modifiable barriers and enablers to clinician behaviour change during the co-design phase, guiding the tailoring of implementation components such as training, prompts, and facilitation. Full details of the theoretical application and rationale are provided in the published protocol and Supplementary Table S1. 21
Stakeholder engagement
Stakeholder engagement was undertaken throughout the pre-implementation phase to inform intervention tailoring and strategy selection, consistent with updated MRC guidance on complex interventions. 24 Co-design workshops were conducted with clinicians (n = 10) and people living with neuromuscular disorders (n = 15), supported by scoping of service structures. These surfaced the need for flexible, person-centred support that could be delivered within the constraints of a single annual appointment. Clinicians identified challenges of time and fidelity processes but also strong alignment with their values, fostering ownership and credibility. Insights informed the design of the training package, adaptation of digital and paper tools, and identification of local implementation champions.
The NM-Bridges intervention
Bridges is a relational, theory-informed approach to supported self-management, underpinned by Social Cognitive Theory, that promotes self-efficacy through reflection, problem solving, and the achievement of small, meaningful goals.25,26 It has been applied in other long-term conditions by embedding self-management support into routine clinical encounters rather than as a separate programme.16,27
NM-Bridges was co-designed alongside people living with neuromuscular disorders, producing population-specific adaptations to both clinician training and patient materials. Clinicians took part in interdisciplinary training workshops tailored to the context of neuromuscular care, while patients received paper and digital workbooks featuring condition-specific vignettes, reflective prompts, and space to record meaningful activities and goals. 15
In this study, NM-Bridges was delivered during a single routine consultation. Clinicians incorporated the approach into their usual practice by using open, reflective questions and language modifications to elicit patients’ priorities and values. Workbook vignettes were drawn on to normalise challenges and stimulate discussion, while conversations emphasised existing coping strategies and supported the setting of small, achievable steps toward meaningful goals. Clinicians reinforced confidence by reinforcing existing skills, progress, and mastery experiences. The workbook was actively used during the consultation to capture reflections and priorities, with patients encouraged to continue using it afterwards on a self-directed basis, and to revisit it in future clinical encounters if they wished.
Implementation strategies
To support integration of NM-Bridges into routine practice, a package of strategies was tailored to the specialist neuromuscular service. These included early engagement of local opinion leaders, co-designed educational meetings to introduce and practise delivery, provision of clinician resources such as reference guides and patient workbooks, and integration of prompts into electronic records to reinforce fidelity. Individualised facilitation sessions were offered to address barriers and adapt the approach to existing workflows. Strategies were refined iteratively in response to clinician feedback to maximise acceptability and minimise additional burden. A full summary mapped to barriers, facilitators, and theoretical constructs is provided in Supplementary Table S2.
Outcomes
Patient-reported outcome measures were collected at baseline, immediately post-intervention, and 3-month follow-up. Selection was informed by patient and public involvement and published recommendations for self-management interventions. 28 To address intervention feasibility, outcomes included acceptability, demand, and suitability of measures, alongside patient-reported changes in person-centredness of care (Patient Assessment of Chronic Illness Care) 29 ; participation and activities (The Oxford Participation and Activities Questionnaire (Ox-PAQ)) 30 ; health-related quality of life (EQ-5D-5L) 31 ; self-efficacy (General Self-Efficacy Scale) 32 ; and mood (General Health Questionnaire-12). 33 Implementation feasibility was evaluated using the Acceptability of Intervention Measure, Intervention Appropriateness Measure, and Feasibility of Intervention Measure, together with the Normalisation Measure Development Questionnaire (NoMAD) scale to assess the extent to which clinicians perceived NM-Bridges as becoming embedded in practice.34–36 Study feasibility was assessed through recruitment and retention rates, completion of assessments, and participant characteristics. Fidelity was evaluated using a structured checklist adapted from earlier Bridges research, 16 completed during live observation of six sessions representing different clinicians and patient presentations.
Sample size and analyses
As this was a feasibility study, no formal power calculation was undertaken. A target sample of 60 people with NMD was initially proposed. A sample size of at least 30 is typically recommended for early feasibility studies, 37 but a higher target was set to account for potential attrition and to allow exploratory assessment of outcome measure performance. The mean recruitment rate was calculated. Descriptive statistics were used to summarise patient-reported outcome measures at baseline, immediately post-intervention, and at 3-month follow-up. For categorical or ordinal data, frequencies and percentages were reported. Exploratory within-group effects were examined using Hedges’ g effect size statistics for continuous and ordinal outcomes. 38 Effect sizes were categorised as large (>0.8), moderate (0.5–0.79), or small (0.2–0.49). Implementation outcomes were summarised using descriptive statistics. Fidelity data were reported as percentages indicating the frequency of application of core NM-Bridges components.
Qualitative interviews
Post-intervention semi-structured interviews with 12 patients were conducted remotely by the lead researcher, lasting 39–65 min (mean = 52). Interviews were audio-recorded, transcribed verbatim, and analysed thematically. The topic guide, informed by Social Cognitive Theory 25 and the Bridges self-management approach, 26 explored acceptability and potential mechanisms of change. Analysis combined inductive and deductive coding with an experiential orientation aligned to the study aims. All six clinicians trained in NM-Bridges also took part in semi-structured interviews after delivering the intervention. These were analysed using the same reflexive thematic approach, with inductive codes developed directly from transcripts and deductive mapping to Normalisation Process Theory. 22
Results
A total of 106 eligible patients were identified and invited to participate in the study. Of these, 56 were invited during clinic appointments, 31 were approached via the hospital's digital patient portal, and 19 received postal invitations. Forty-seven individuals were not contactable or did not respond to correspondence, and 24 declined to participate. Reasons for declining included being too busy (n = 10), not interested in the research (n = 6), perceiving the time commitment to be too large (n = 4), and no reason given (n = 4). Two individuals did not meet inclusion criteria. In total, 33 participants (31.13% of all eligible patients) were enrolled over a 14-month period (February 2022 to March 2023), with a mean recruitment rate of 2.36 participants per month. All 33 enrolled participants completed the study and were included in the evaluation.
The sample was 63.64% male, with a mean age of 51.9 years (SD = 15.64; range = 18–77). Participants presented with a wide range of neuromuscular disorders, including Charcot–Marie–Tooth disease (n = 11), facioscapulohumeral muscular dystrophy (n = 5), mitochondrial cytopathy (n = 4), and myotonic dystrophy (n = 2). A further 11 conditions were each represented by a single participant, including Lambert–Eaton myasthenic syndrome, distal muscular dystrophy, inclusion body myositis, Andersen–Tawil syndrome, periodic paralysis, congenital muscular dystrophy, distal hereditary motor neuropathy, chronic inflammatory demyelinating polyradiculoneuropathy, hereditary spastic paraplegia, and limb girdle muscular dystrophy. Demographic information is provided in Table 1.
Demographic information of patient participants in the ADAPT-NMD study.

Six clinicians were trained to deliver NM-Bridges (five female, one male), comprising four physiotherapists and two specialist nurses, all in senior NHS roles. Ethnic backgrounds included white British (n = 4), Filipino (n = 1), and mixed white and Asian heritage (n = 1). One clinician was unable to deliver the intervention due to staffing pressures. Among the remaining five, session delivery varied: one physiotherapist delivered 15 sessions, another delivered seven, one delivered three, and each specialist nurse delivered four.
Patient-reported outcome measures
Complete data were returned for all patient-reported outcomes across the three timepoints. Descriptive statistics (means and standard deviations) are presented in Table 2. Exploratory effect sizes (Hedges’ g) are shown in Table 3, comparing pre- to post-intervention (T1–T2), pre-intervention to 3-month follow-up (T1–T3), and post-intervention to follow-up (T2–T3). Mean Patient Assessment of Chronic Illness Care scores increased from baseline to post-intervention and were maintained at follow-up, while Ox-PAQ scores suggested slight reductions in participation, particularly in the social and emotional domains. EQ-5D-5L and General Self-Efficacy Scale scores remained broadly stable, while General Health Questionnaire-12 scores indicated a small reduction in psychological distress immediately post-intervention.
Descriptive statistics for patient-reported outcome measures. Values are presented as mean (SD). T1 = baseline, T2 = post-intervention, T3 = 3-month follow-up.
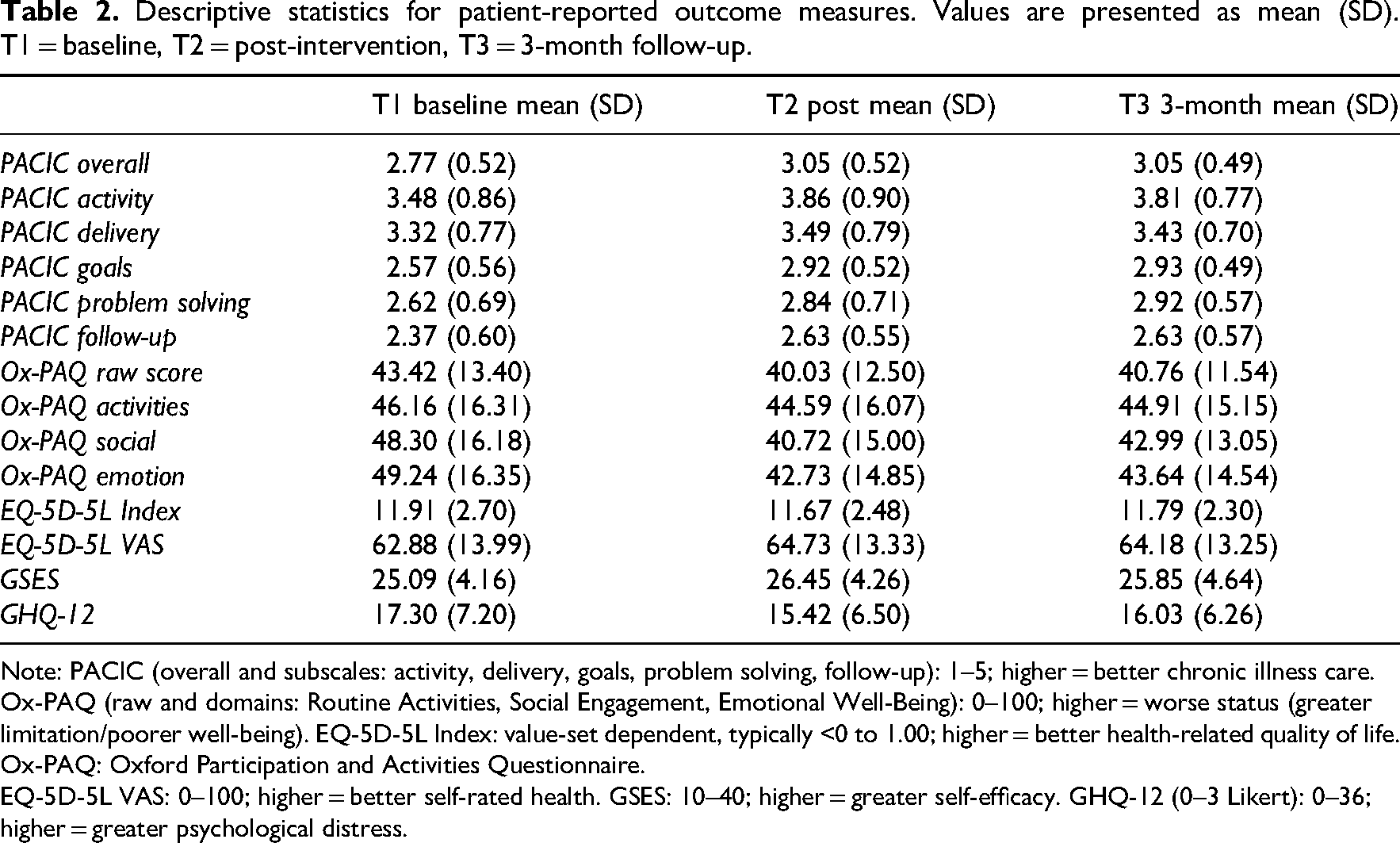
Note: PACIC (overall and subscales: activity, delivery, goals, problem solving, follow-up): 1–5; higher = better chronic illness care. Ox-PAQ (raw and domains: Routine Activities, Social Engagement, Emotional Well-Being): 0–100; higher = worse status (greater limitation/poorer well-being). EQ-5D-5L Index: value-set dependent, typically <0 to 1.00; higher = better health-related quality of life. Ox-PAQ: Oxford Participation and Activities Questionnaire.
EQ-5D-5L VAS: 0–100; higher = better self-rated health. GSES: 10–40; higher = greater self-efficacy. GHQ-12 (0–3 Likert): 0–36; higher = greater psychological distress.
Effect sizes for the patient-reported outcomes comparing pre-intervention (T1) to post-intervention (T2), pre-intervention (T1) to 3 months (T3), post-intervention (T2) to 3 months (T3). Hedge's G effect size statistic is reported. Effect sizes: large *(>0.8), medium + (>0.5), small • (>0.2).
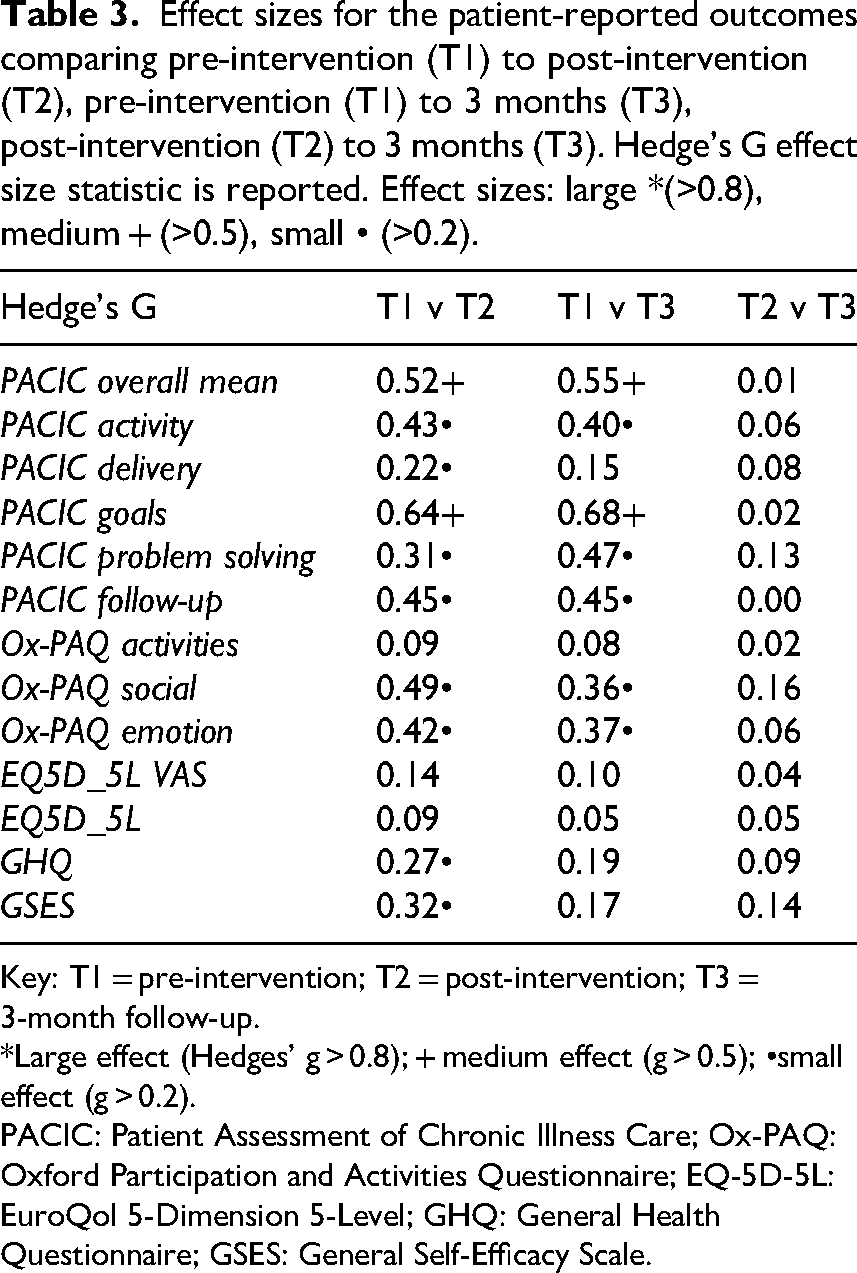
Key: T1 = pre-intervention; T2 = post-intervention; T3 = 3-month follow-up.
*Large effect (Hedges’ g > 0.8); + medium effect (g > 0.5); •small effect (g > 0.2).
PACIC: Patient Assessment of Chronic Illness Care; Ox-PAQ: Oxford Participation and Activities Questionnaire; EQ-5D-5L: EuroQol 5-Dimension 5-Level; GHQ: General Health Questionnaire; GSES: General Self-Efficacy Scale.
Qualitative interviews (patients receiving nm-bridges): summary of themes
A full analysis of patient interviews will be published separately; a brief summary is included here to contextualise the quantitative findings, with supporting quotes provided in Supplementary Table S3. Semi-structured interviews with 12 participants brought three interrelated themes into focus: feeling heard, feeling supported, and feeling success.
Feeling heard: Patients valued the opportunity to share their own stories and priorities, describing consultations as more collaborative and less transactional. Feeling supported: The intervention was experienced as building trust and shared understanding, with many reporting that this relational support motivated engagement with self-management. Feeling success: Patients described improved mood, optimism, and a sense of control through setting small, achievable goals, which were viewed as meaningful markers of progress.
Together, these findings suggest that NM-Bridges was acceptable and beneficial for patients, supporting person-centred dialogue and engagement in self-management.
Implementation findings
All six clinicians completed the NoMAD following delivery of the NM-Bridges intervention. Global normalisation scores indicated high familiarity with NM-Bridges (Mean = 8.0, SD = 1.26), a sense that it had become part of routine practice (Mean = 7.2, SD = 1.16), and strong intentions to continue using it (Mean = 8.0, SD = 0.63). Across the four core constructs of Normalisation Process Theory, clinicians reported high levels of coherence (Mean = 4.29, SD = 0.75), cognitive participation (Mean = 4.62, SD = 0.49), and reflexive monitoring (Mean = 4.30, SD = 0.53), with slightly lower ratings for collective action (Mean = 3.71, SD = 0.45). Within subconstructs, the strongest contributors to implementation were internalisation (Mean = 5.00), activation (Mean = 4.83), and enrolment (Mean = 4.83), while lower scores for contextual integration and skill-set workability (Mean = 3.50) suggested minor barriers related to resource availability and role clarity (Figure 1).
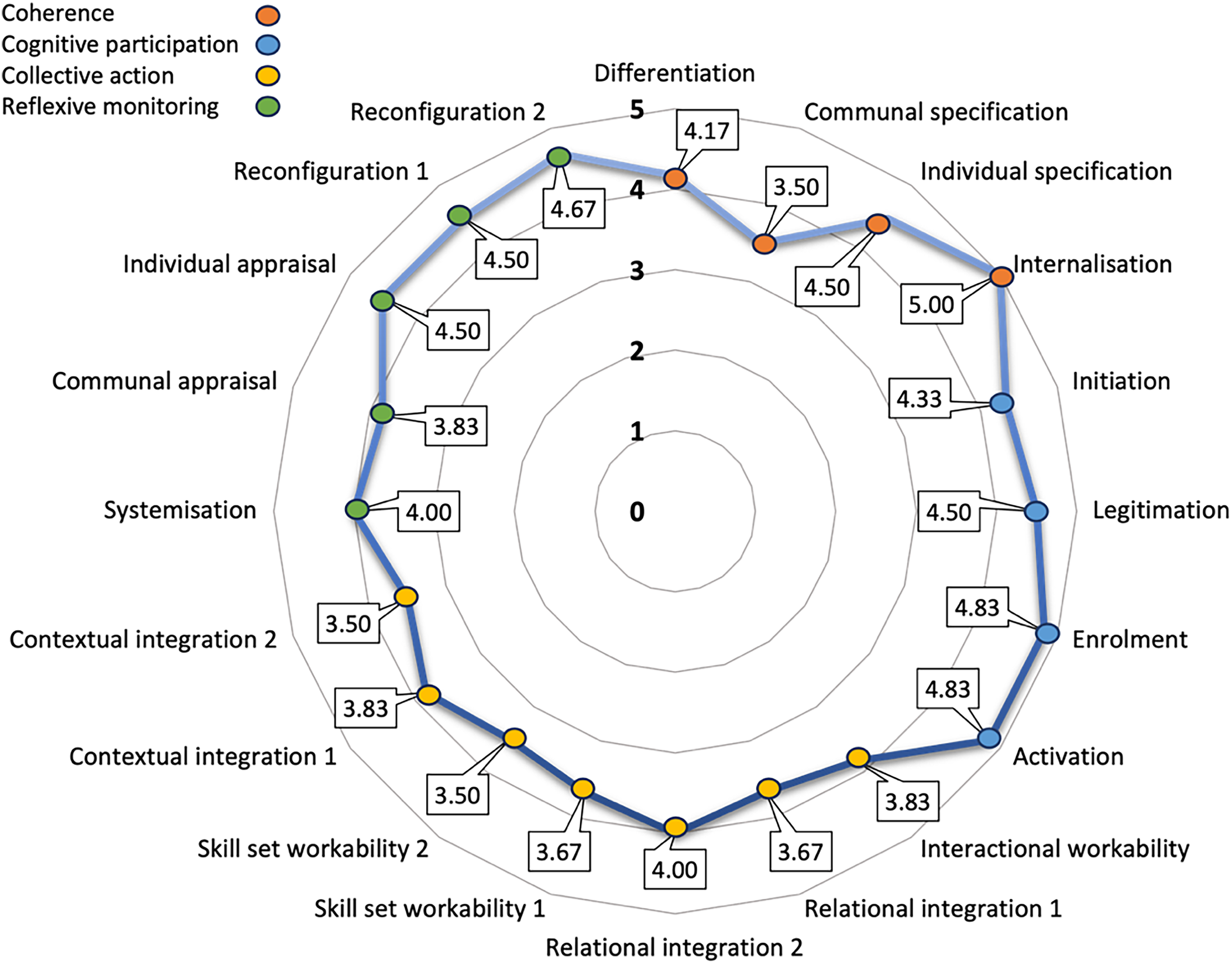
Radar chart showing mean scores for the 16 normalisation process theory subconstructs. Likert scale of 1 (strongly disagree) to 5 (strongly agree).
Quantitative implementation measures revealed that clinicians rated the intervention as highly appropriate, feasible, and acceptable. All clinicians agreed or strongly agreed with each item, with median scores of 18/20 (appropriateness), 16.5/20 (feasibility), and 19/20 (acceptability). NM-Bridges was perceived as fitting, suitable, and applicable to the clinical context, and was described as implementable and easy to use.
Fidelity was assessed using a self-report checklist completed after each intervention session. Across the 33 completed checklists, clinicians most frequently reported encouraging reflection (Mean = 90.00%), participation in meaningful activity (Mean = 83.14%), and development of knowledge (Mean = 78.95%). Use of the paper workbook (Mean = 27.52%) and digital workbook (Mean = 28.86%) was relatively low. Observations of six sessions mirrored these findings: reflection was observed in all sessions (100%), participation and knowledge development in 83.33%, and workbook use in 33.33% of cases. Overall, fidelity data indicated that core NM-Bridges principles were consistently applied, though flexibility was evident in how specific tools were used.
Qualitative interviews (clinicians delivering nm-bridges): Summary of themes
A full analysis of clinician interview data will be reported separately; a brief summary is provided here to contextualise the quantitative findings. Interviews highlighted processes of sense-making, engagement, and integration mapped to Normalisation Process Theory constructs.
Coherence: Clinicians described NM-Bridges as distinct from usual care, aligning with person-centred values and supporting more collaborative consultations. Early involvement in co-design fostered ownership and reinforced its perceived relevance. Cognitive participation: Engagement was evident, with clinicians initiating use and embedding elements into team practice. However, variation in training and role identity influenced confidence and consistency, particularly among newer staff. Collective action: NM-Bridges was viewed as adaptable and supported by training, but time pressures, variable use of materials, and limited medical staff engagement hindered routine uptake. Reflexive monitoring: Clinicians observed benefits in patient engagement and communication. They valued the toolkit as a practical scaffold. Sustained support and feedback mechanisms were seen as important for ongoing use.
These findings suggest clinicians found NM-Bridges acceptable and relevant, while drawing attention to contextual barriers that will require attention in future implementation.
Discussion
This study represents the first feasibility exploration of NM Bridges, a broad-based self-management support programme for people with neuromuscular disorders, using a hybrid methodology. 39 The Bridges approach, 16 already established as a flexible, relational model of self-management support, was newly adapted for this context and delivered within a single specialist consultation.
While there are parallels with other progressive neurological conditions, neuromuscular disorders differ in key respects: they are individually rare, often present earlier in life, follow highly variable trajectories, and lack disease-modifying therapies, leading to greater reliance on specialist centres and limited local expertise.1,11 People living with these conditions also face heightened uncertainty, stigma, and challenges to identity which shape both the lived experience and service context. 40 These factors contrast with more established illness narratives and support structures seen in conditions like multiple sclerosis or Parkinson's disease.8,9 Qualitative findings reinforced the value of tailored, condition-specific self-management support, highlighting the importance of validation and shared understanding. Despite such complexities, NM Bridges was feasible and acceptable, with high recruitment, strong retention, fidelity to core principles, and early signals of benefit across person-centred outcomes.
Implementation findings were encouraging. Clinicians reported strong alignment between NM Bridges and their practice values, particularly around relevance and legitimacy. 22 These findings echo broader literature on the importance of perceived ownership for successful implementation. 41 The co-design process, tailored training, and stakeholder engagement likely strengthened this alignment. However, challenges included lower scores for constructs such as skill-set workability and communal appraisal, suggesting limited peer reflection and shared learning opportunities. Minimal medical involvement also points to the importance of engaging a wider professional base for sustainable scale-up.
At the intervention level, NM-Bridges appeared to promote more collaborative, personalised care. Improvements in the Patient Assessment of Chronic Illness Care, especially in goal setting and activation domains, reflected stronger person-centredness and alignment with Bridges principles. 16 Improvements in the Ox-PAQ, particularly in emotional well-being and social engagement domains, echoed qualitative findings around connection, identity, and narrative agency. Given the high psychosocial burden of these conditions, these findings support the need for relational, holistic support rather than task-focused models. 12
Notably, meaningful gains in self-efficacy were achieved following a single session, suggesting a low-intensity, low-cost model with potential for scalability. Similar single-session interventions, such as in post-stroke self-management, have shown effectiveness in improving quality of life and engagement in rehabilitation. 42 The sustained changes at 3-month follow-up provide tentative evidence of durability, though the lack of control group and small sample preclude efficacy claims. Repeated sessions could yield greater benefits, depending on service models.
Fidelity data showed variation across professions: physiotherapists used goal setting more consistently than nurses, likely reflecting training backgrounds. This suggests that future roll-out may benefit from tailored support or calibration by discipline. While fidelity checklists gave useful data, a more detailed evaluation using video or multi-source methods could enhance understanding. The inclusion of a mixed diagnostic sample may be seen as a limitation, but was intentional and pragmatic, reflecting real-world specialist clinic caseloads. Rare disease trials increasingly adopt such inclusive approaches.13,43 The recurring psychosocial challenges across neuromuscular disorders resonate with the core principles of Bridges, which privilege individualised adaptation and narrative meaning-making above prescriptive disease-specific protocols. 26
Several limitations should be acknowledged. Implementation measures were cross-sectional, limiting understanding of change over time. Uneven delivery, with one physiotherapist leading almost half the sessions, may have introduced practitioner bias. Medical staff were under-represented, and future work should include broader disciplines such as psychology and occupational therapy to test integration and team-based delivery.16,26,27 The pre- and post-design was appropriate for feasibility, but lacks a control group, limiting causal inference. Change scores may be influenced by regression to the mean or confounding. Clinician gatekeeping may have favoured more engaged participants, suggesting a need for broader recruitment strategies in future trials.
Nonetheless, the study demonstrates feasibility of embedding person-centred self-management support into rare, complex conditions. Relational techniques, shared decision-making, and flexible delivery appeared to promote meaningful engagement across diverse patient profiles. Future work should refine implementation strategies and explore broader roll-out through controlled trials. Hybrid designs appear valuable at feasibility stage, offering insight into what works, for whom, and under what circumstances.
39
This study provides a foundation for large-scale evaluation of NM Bridges as a relational, sustainable model of self-management support within neuromuscular rehabilitation.
NM-Bridges was feasible and acceptable for people with neuromuscular disorders in a single outpatient consultation, with high engagement and low attrition. Clinicians valued it as a person-centred approach that supported more collaborative, reflective consultations. Patient-reported outcomes indicated potential improvements in quality of care, goal setting, well-being, and self-efficacy.Clinical messages
Supplemental Material
sj-docx-1-cre-10.1177_02692155251403989 - Supplemental material for ADAPT-NMD: A hybrid II feasibility study of a co-designed self-management support intervention for people living with neuromuscular disorders
Supplemental material, sj-docx-1-cre-10.1177_02692155251403989 for ADAPT-NMD: A hybrid II feasibility study of a co-designed self-management support intervention for people living with neuromuscular disorders by Laurence Edward Lee, Stefan Tino Kulnik, Annette Boaz and Gita M Ramdharry in Clinical Rehabilitation
Supplemental Material
sj-docx-2-cre-10.1177_02692155251403989 - Supplemental material for ADAPT-NMD: A hybrid II feasibility study of a co-designed self-management support intervention for people living with neuromuscular disorders
Supplemental material, sj-docx-2-cre-10.1177_02692155251403989 for ADAPT-NMD: A hybrid II feasibility study of a co-designed self-management support intervention for people living with neuromuscular disorders by Laurence Edward Lee, Stefan Tino Kulnik, Annette Boaz and Gita M Ramdharry in Clinical Rehabilitation
Supplemental Material
sj-docx-3-cre-10.1177_02692155251403989 - Supplemental material for ADAPT-NMD: A hybrid II feasibility study of a co-designed self-management support intervention for people living with neuromuscular disorders
Supplemental material, sj-docx-3-cre-10.1177_02692155251403989 for ADAPT-NMD: A hybrid II feasibility study of a co-designed self-management support intervention for people living with neuromuscular disorders by Laurence Edward Lee, Stefan Tino Kulnik, Annette Boaz and Gita M Ramdharry in Clinical Rehabilitation
Supplemental Material
sj-docx-4-cre-10.1177_02692155251403989 - Supplemental material for ADAPT-NMD: A hybrid II feasibility study of a co-designed self-management support intervention for people living with neuromuscular disorders
Supplemental material, sj-docx-4-cre-10.1177_02692155251403989 for ADAPT-NMD: A hybrid II feasibility study of a co-designed self-management support intervention for people living with neuromuscular disorders by Laurence Edward Lee, Stefan Tino Kulnik, Annette Boaz and Gita M Ramdharry in Clinical Rehabilitation
Footnotes
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Muscular Dystrophy UK, (grant number 18GRO-PS48-0122).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
