Abstract
Objective
To determine the characteristics of patients admitted to inpatient rehabilitation services for reconditioning to inform clinical care.
Design
An exploratory audit.
Setting
A major tertiary hospital service in Australia providing 48 inpatient beds across two facilities.
Participants
Patients admitted to a rehabilitation service over two years (2019–2020) and categorised under Australasian Rehabilitation Outcomes Centre impairment codes for reconditioning.
Main measures
Demographic and clinical service data.
Methods
Descriptive analysis of data from the hospital admissions data base.
Results
Of the 368 patients in the study sample (432 admissions), the age range was 22–100 years of age (mean = 75 years). Data on smoking, language and age groups was trended and identified a younger group of patients with 16% (58 of 368 patients) being aged 60 and under. The gender split was 54.2% male and 45.8% female. Admissions of Indigenous people was higher than the recorded population with females being disproportionately categorised as deconditioned, and an overall mean age 24 years younger than the sample mean. Identified for increased attention were nephology patients and a group of 58 people (15.7%) with two or more admissions for reconditioning rehabilitation in the two-year period. This group were older (aged over 80) and male.
Conclusion
Literature on reconditioning programs has a predominant focus on the older, more frail population. Patients admitted to inpatient rehabilitation for reconditioning are a diverse population and further study is required to determine effective interventions for specific groups of patients, particularly younger cohorts, and those with frequent readmissions.
Clinical messages
Patients requiring rehabilitation due to hospital-acquired deconditioning are a large and diverse population across all ages, and not just the elderly. This includes Indigenous Australians, renal patients, young and old.
Common definitions of what constitutes a clinical need for a rehabilitation reconditioning program are required.
Introduction
Deconditioning presents as a reduction in muscle mass and strength impacting ability to mobilise, carry out activities of daily living, and functional decline as a result of inactivity or bed rest. 1 When deconditioning occurs due to hospitalisation, it is referred to as hospital-associated deconditioning or hospital-acquired deconditioning (HAD). 2 HAD is largely preventable 3 and shares clinical features with frailty, including reduced muscle strength and mobility. However, frailty is a geriatric condition that has a slow onset and progression, whereas HAD affects any age group and has a more rapid onset occurring in as little as two days. 4 A pre-existing diagnosis of frailty can increase the likelihood of HAD 5 as can advanced age, extended bed rest, medical illness, disability, chronic disease, poor nutrition, inflammation, lower body weight, and hospitalisation.6–8 Ageing, and recently COVID-19 place an additional load on the system by increasing risk for deconditioning.9–11
Deconditioning impedes mobility and independence in activities of daily living, decreasing capacity to live independently at home. 12 It can have a detrimental effect on a person's cognition, 13 reducing occupational participation and posing a barrier to engagement in meaningful activities. 14 Hospital-acquired deconditioning results in increased system costs by delayed discharge, higher demand for discharge to community facilities, 12 heightened risk for falls and hospital readmission.2,513–15
Rehabilitation pathways for reconditioning are predominantly based on a geriatric rehabilitation model, however, the literature reveals a paucity of research defining the characteristics of patients who require reconditioning. A literature review by Chen et al. 16 identified deconditioning studies in the elderly population (over 60s) but omitted younger groups. People requiring reconditioning perform well in rehabilitation; however, there is a lack of evidence describing the patient characteristics that benefited from rehabilitation. 1 For rehabilitation approaches to be effective and client centred, greater emphasis must be placed on identifying and defining the characteristics of this broad population. 8 The research question was the result of the lack of clear guidelines for managing patients admitted for rehabilitation for reconditioning, and the observed growth in numbers and complexity of these patients from a rehabilitation perspective.
The Australasian Rehabilitation Outcome Centre (AROC) provides a system for national benchmarking of rehabilitation services through the classification of patients into coded impairment groups. 17 This includes a breakdown of codes for patients admitted for reconditioning: medical (code 16.1), surgical (code 16.2), and cancer related (code 16.3). 18 As patients were admitted under these codes, a readily available data bank was available to examine. This led to the design of an exploratory audit to answer the research question:
‘What are the characteristics of patients requiring reconditioning admitted to tertiary care inpatient rehabilitation services?’
Methods
This research is reported using STROBE. 19 The study site is a major tertiary hospital service operating 48 inpatient beds across two inpatient rehabilitation facilities. Twenty-eight beds are dedicated to a neuroscience rehabilitation unit, and twenty beds to a medical rehabilitation unit. A retrospective exploratory audit of deidentified data of patients over the age of 18, admitted from hospital wards to these rehabilitation services for reconditioning over a 24-month period between 1 January 2019 and 31 December 2020 was conducted. Data were requested from the Hospital Based Corporate Information System (HBCIS) using reconditioning codes. This included three codes, assigned to medical (code 16.1), surgical (code 16.2) and cancer (code 16.3) related deconditioning. Patients admitted for reconditioning under medical or surgical reconditioning impairment codes have experienced an aetiological diagnosis of one or more of the following: muscular wastage and disuse atrophy, an unspecified disorder of muscle, ligament, and fascia, chronic fatigue syndrome, and other malaise and fatigue which are unattributable to other impairment codes. Patients admitted under impairment code 16.3 have experienced hospital-acquired deconditioning due to a cancer diagnosis or cancer treatment. 18 This study had full ethical and site-specific approvals (reference HREC/2021/QGC/80463).
Data requested from the health informatic system included demographic and clinical information for patients admitted to the hospital under another specialty (not rehabilitation) and transferred to the inpatient rehabilitation unit for reconditioning. These fields included: age at admission, gender, Indigenous status, country of birth, language spoken, interpreter required, smoking status, facility, admission date, admission source, admission ward, admission specialty, discharge description, discharge date, discharge ward, discharge specialty, length of stay, first admission date, diagnosis related group (DRG) code and description, principal diagnosis, funding source, hospital stay admission date, hospital stay discharge date, rehabilitation start date, rehabilitation end date, and impairment code.
Original estimates by the medical director of the unit indicated a sample of approximately 30–50 a year. Data were requested for a 2-year period to allow for seasonal variations between admissions and enable a larger sample for analysis. The period was purposeful as the pandemic lead to a substantial change in case mix in 2021 when the state borders were opened with numerous ‘overflow’ wards and disrupted patient pathways potentially impacting the accuracy of data.
Deidentified data were received in excel format, with no personal identifiers (i.e., medical record number) to ensure full confidentiality. Data were stored in accordance with the university's data storage policy in a password protected cloud to protect patient confidentiality.
All data were cleaned and assessed for completion and then uploaded into IBM SPSS statistics for analysis. Descriptive data were assessed and analysed. For continuous variables, data are presented using mean and standard deviation (SD) or median and range and categorical data are presented as proportions (%). As an exploratory study our goal was to describe the sample based on descriptive statistics. Data were analysed in the broad groups of age, gender, and rehabilitation codes of surgical, medical and cancer. The unit prior to admission for rehabilitation reconditioning program was also explored to try and understand the source of the patient groups. A decision was made to analyse data by admissions for the time as this represented the case mix and workload of the population under study. As this resulted in duplicate demographic data because of readmissions, subsequent analysis included the first admission only. Using common demographic identifiers (e.g., date of birth, gender and place of birth, language spoken, etc.) patients admitted more than once were identified and analysed as a discrete data set. While this complicated the analysis, we believe it provides a more accurate picture of the characteristics of patients admitted to a rehabilitation unit for reconditioning programs.
Results
The total number of patient admissions for reconditioning over this period was n = 432. Closer inspection identified a high number of repeat patients or readmissions n = 368 individual patients. Due to the large number of variables, the data were split into categories for analysis;, admissions by gender (Table 1), admissions by age group, (Table 2), readmissions by single patient admissions over the 2 year period (Table 3), admissions by impairment code (Table 4) and referring speciality unit (Table 5). Of the 368 patients in the study sample, the age range was 22–100 years of age (mean = 75 years, median = 77 years). The data showed a broad age range of patients with 16% (58 of 368 patients) being aged 60 and under. This was unexpectedly high considering the scarcity of research on younger patients and hospital-acquired deconditioning. Seasonal (Australian) variance for admissions showed 150 admissions in spring, 73 in summer, 94 in autumn, and 115 in winter.
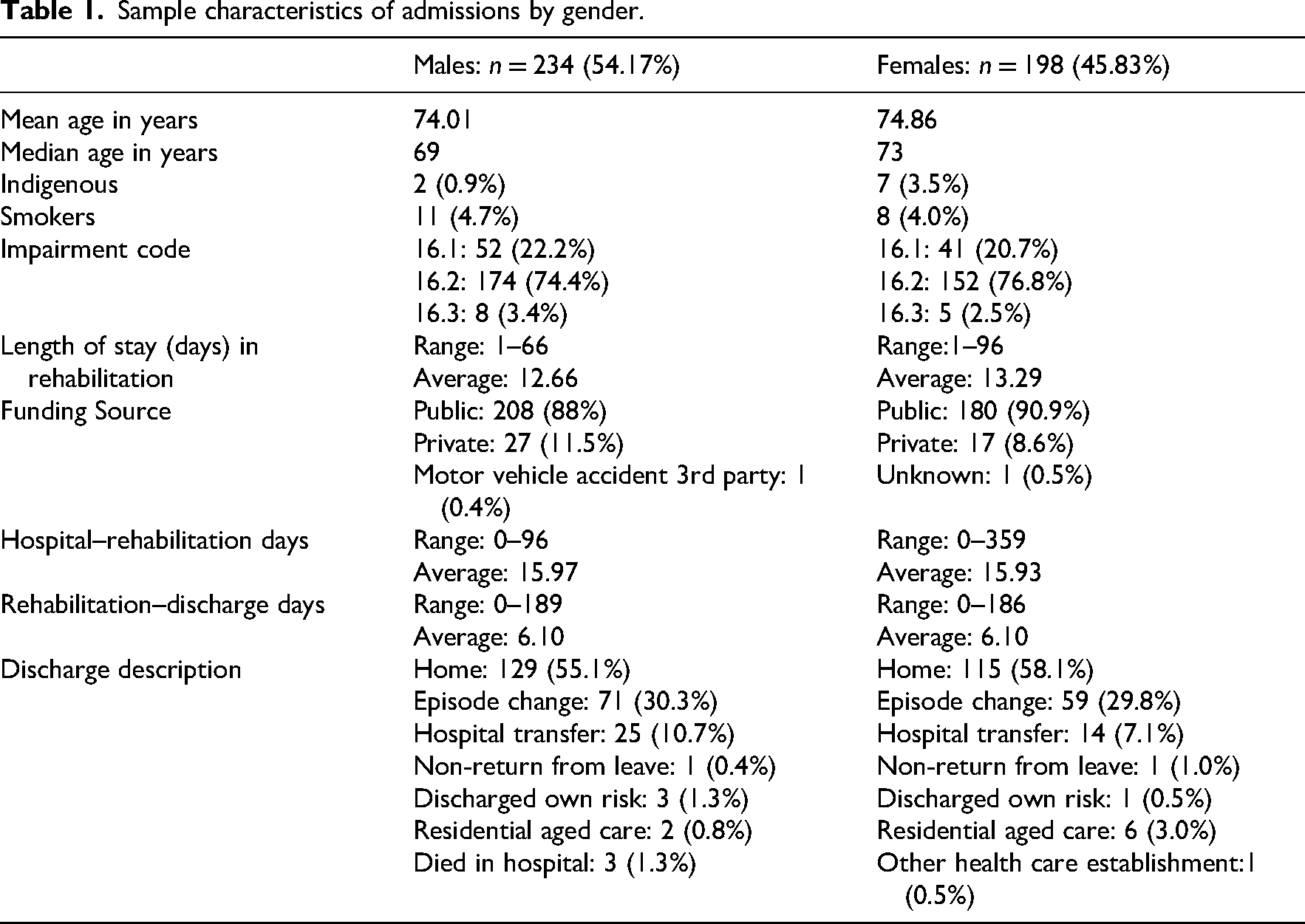
Sample characteristics of admissions by gender.
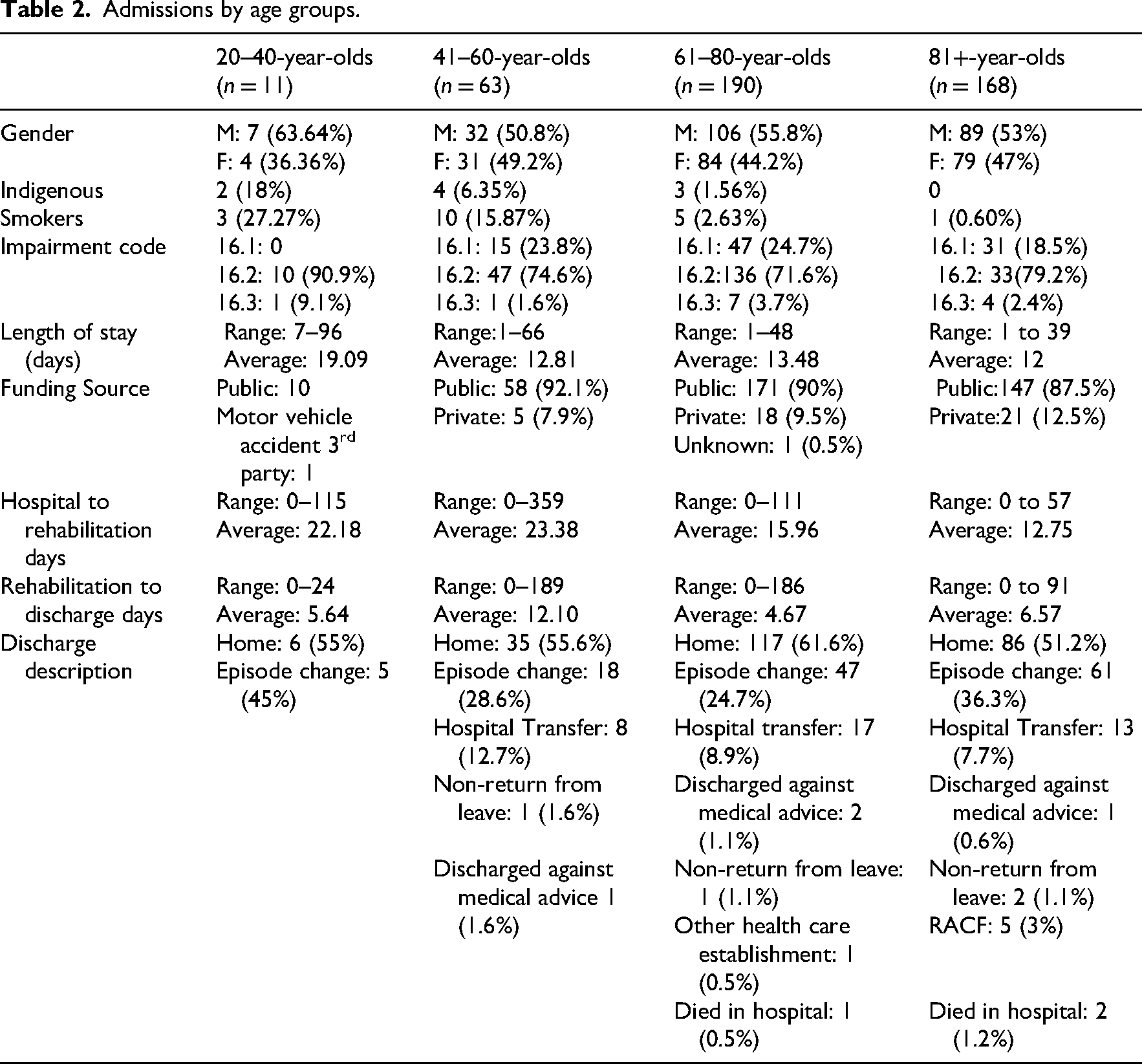
Admissions by age groups.

Readmissions by single patients over the 2-year period.
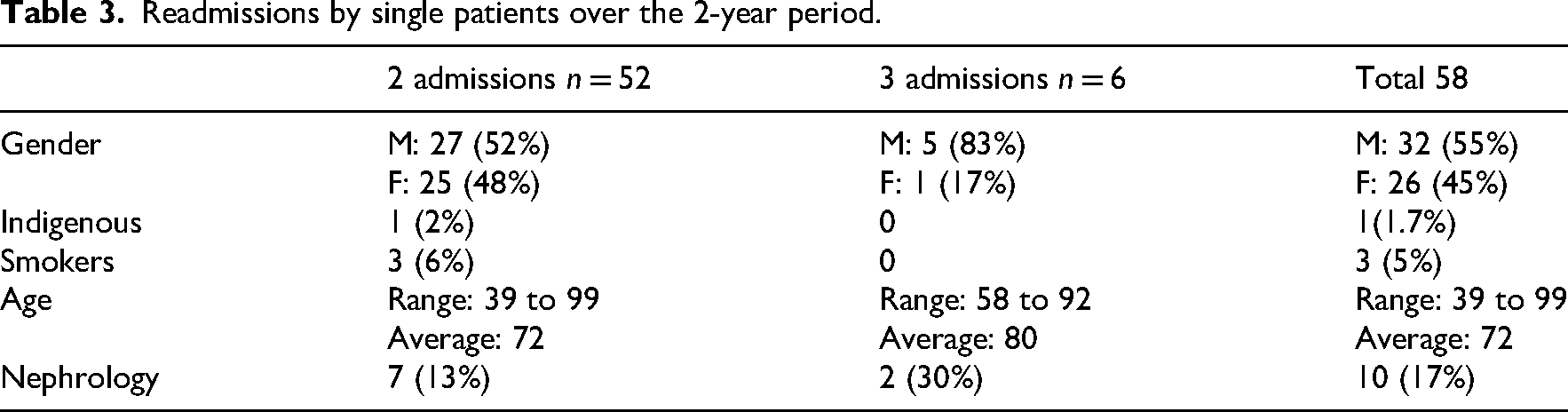
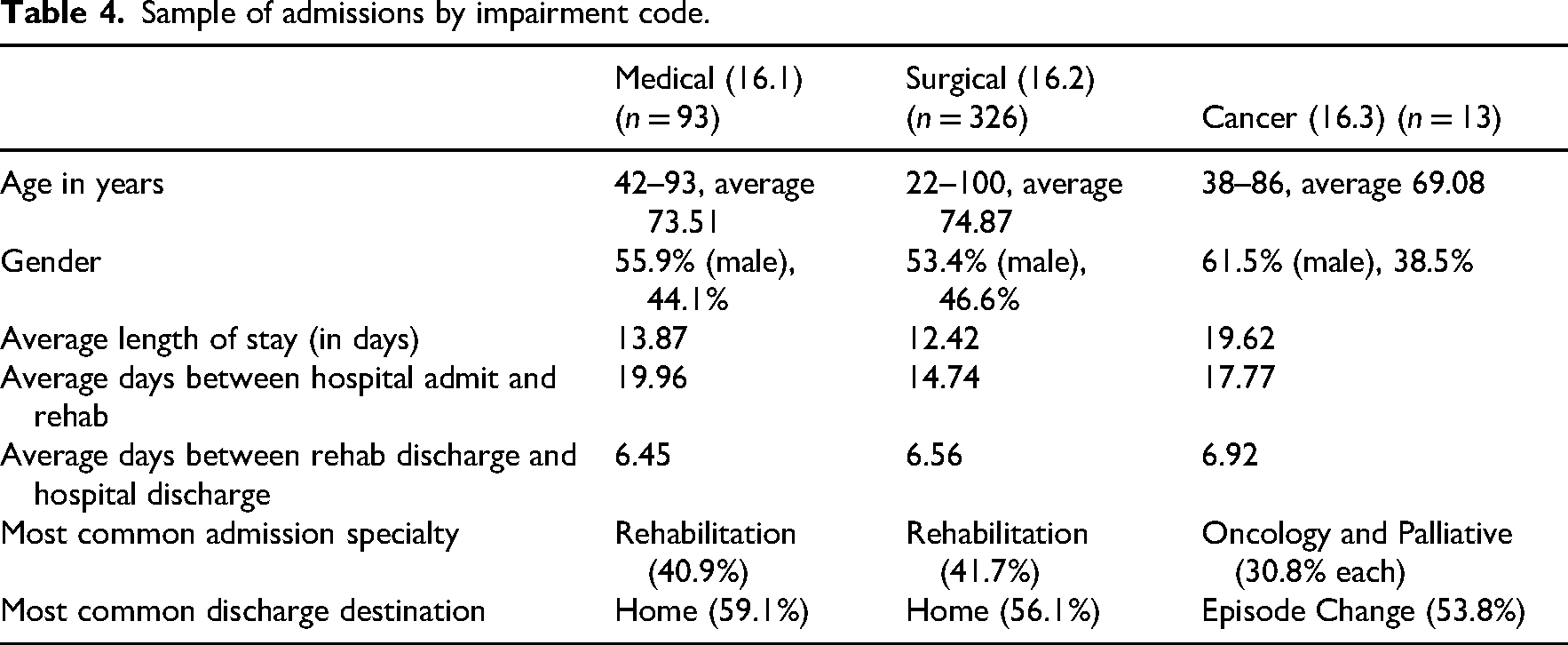
Sample of admissions by impairment code.
Hospital specialty prior to being coded as reconditioning program.
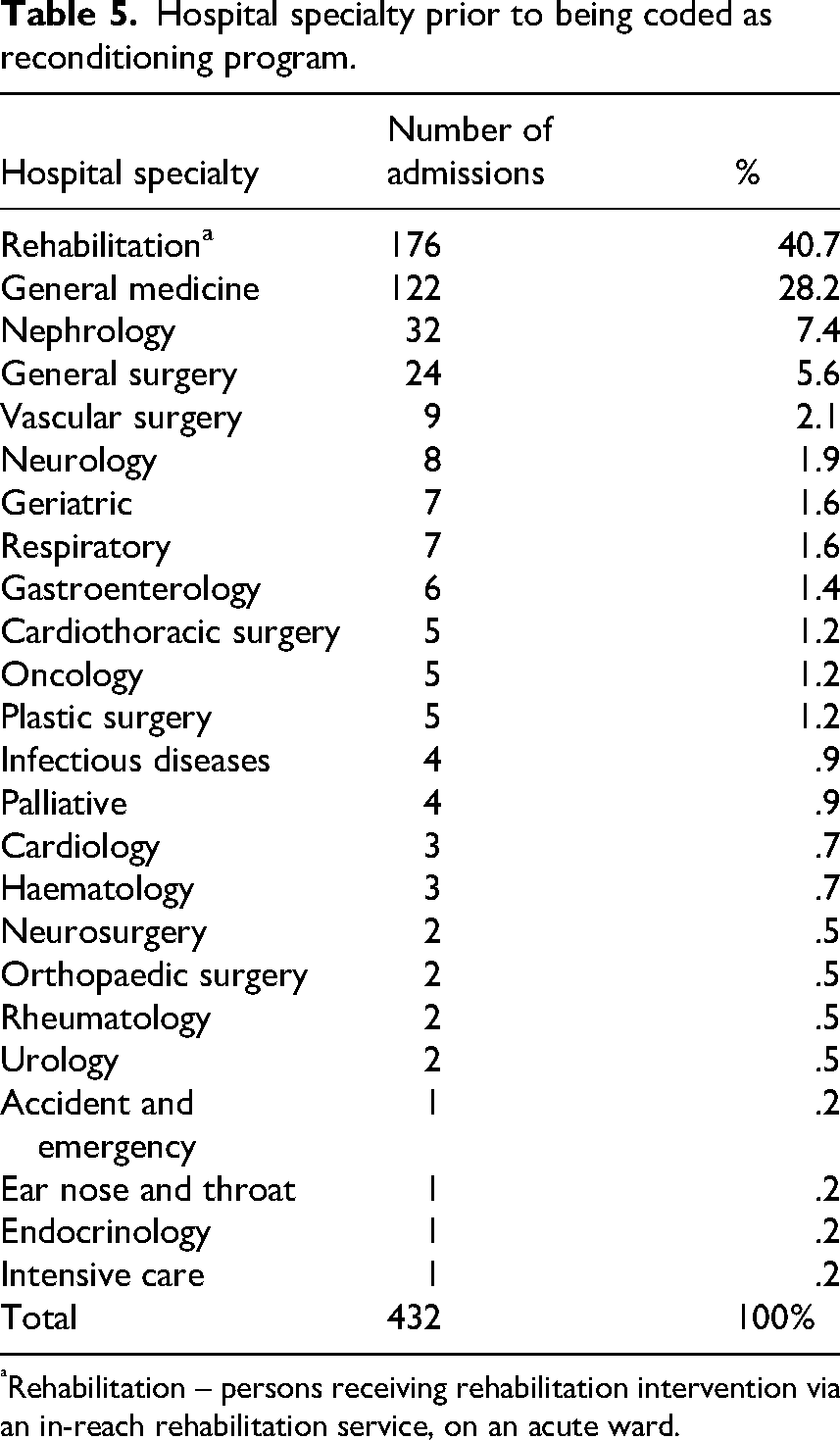
Rehabilitation – persons receiving rehabilitation intervention via an in-reach rehabilitation service, on an acute ward.
One patient (38-year-old female with breast cancer) spent 96 days coded as cancer reconditioning. Another patient recorded 359 days between admission to hospital and admission to rehabilitation, with a stroke classified as ‘of major complexity’. While these are outliers, it is important to consider that these patient's needs for rehabilitation interventions will differ, being more severely deconditioned and with complex medical conditions hence were included.
Gender was split into 54.2% male and 45.8% female (see Table 1), with males overrepresented compared to demographic data from the Australian Bureau of Statistics for the area. 20 Those under 40 were most likely to be male, and men were more likely to be smokers. Days between hospital admission to rehabilitation admission was similar for all genders as was days between discharge from rehabilitation ward to hospital discharge. Females were more likely to go home or to residential aged care and had a longer mean stay in rehabilitation than males. Males were more likely to discharge against medical advice.
Those born in Australia accounted for 255 (59%) of the sample, six spoke a language other than English at home, five people required an interpreter. Persons identifying as Aboriginal or Torres Strait Islander accounted for 2.1% 12 of the total number of admissions, which accounts for 2.08% of the total population admitted, and 3.53% of those in our sample born in Australia (see Table 2). While this is a small percentage of overall admissions, this is an important consideration as Aboriginal and Torres Strait Islanders historically have poorer health outcomes than non-indigenous persons, and require a level of cultural sensitivity to inform intervention. Over 90% of patients under 40 requiring reconditioning were coded under surgicial, with the remainder attributed to cancer, Nil were attributable to surgical reconditioning. This infers that patients under 40 are far less likely to require rehabilitation for deconditioning post-surgery and interventions should be greater focused towards medical. In addition, patients under 40 had the longest length of stay.
Overall age ranges, the largest source of deconditioning was attributable to medical conditions.
Cleaning the data exposed a group of admissions with the same demographic profile, suggesting these were the same patients with multiple admissions. Closer inspection of admission and discharge dates indicated that these were a subgroup of the total sample who had been coded as requiring reconditioning. It is of relevance to our research question, as there were 58 people (15.7%) of the total number of people who had two or more episodes of care categorised under the codes of interest (see Table 3). Those with three admissions were much older and male.
The spread of admissions across surgical, medical and cancer impairment codes is shown in Table 4. Length of stay varied from 1 to 95 days with a mean of 12.95 days. A higher percentage of younger people were recorded under the surgical code (i.e., orthopaedics, neurosurgery). A more detailed analysis of the sample by impairment codes by admissions is also presented in Table 4. The episode changes in patients with cancer were for readmission to an acute ward or palliative care.
The range between admission to hospital and admission to rehabilitation for reconditioning was reported as 0 to 359 days with a mean of 15.95 days, with 87.7% of admissions to rehabilitation within 31 days of the initial hospital admission date. Most admissions (341, 78.9%) were admitted from elsewhere in the hospital via an ‘episode change’. Other admission sources included ‘transfer from another hospital’ (n = 77, 17.8%), ‘outpatient department’ (n = 7, 1.6%), ‘community service’ (n = 3, 0.7%), ‘accident and emergency’ (n = 2, 0.5%), and ‘residential aged care facility’ (n = 2, 0.5%).
It was found that 244 (56.48%) of discharges were to home after the rehabilitation episode of care, increasing to 303 (70.14%) when including those discharged within 1 day of leaving rehabilitation. The second most common discharge reason was episode change which accounted for 130 patients, followed by hospital transfer (n = 39), discharge to residential aged care facility (n = 8), discharged at own risk (n = 4), non-return from leave (n = 3), and died in hospital (n = 3). For those that did not discharge home following their rehabilitation stay, the mean length of stay was 6.51 days post rehabilitation admission with the longest stay being 189 days. Data revealed that the reason for episode changes was variable and confusing. Reasons included changes from private to public, transfer from one hospital to another within the health services, and transfer from one ward to another.
Table 5 provides a breakdown of referring speciality units, which is the unit the patient was transferred from for a reconditioning program. The specialties that were attributed to the most admissions were rehabilitation with n = 176 (40.7%) and general medicine with n = 122 (28.2%). An unexpectedly high admission source was nephrology, with this specialty accounting for 7.4% of the single patient admissions. This is partly explained by the higher number of nephrology patients identified in the readmission subset shown in Table 3. Please note that Table 5 refers to admissions (not patients) hence these data are to be interpreted with caution as it includes readmissions and episode changes.
Discussion
This study aimed to identify the characteristics of patients admitted to inpatient rehabilitation for ‘reconditioning’. A sample of 30–50 patients a year was predicted; however, the data set included 368 people with 432 admissions over a 2-year period.
An unexpected finding was the age range of patients with 17% being aged 60 and under. As shown in Table 2, 90% of the 20–40 years age group were admitted under the surgical code 16.2, had the longest mean length of stay (19.09 days) and predominantly male (63.64%). There were none in the medical subgroup, and only one in the cancer subgroup. In the absence of additional data, we can only infer that this may have been orthopaedic, neurosurgery or trauma related which align with high risk behaviours in this demographic. 21 Most of the research into hospital-acquired deconditioning has focused on geriatric populations with an absence of information on younger people. Those in the 61–80-year-old category were most likely to go home, whereas those under 40 tended to be discharged from rehabilitation under ‘episode change’; however, no data are available for which service they were discharged to. This potentially reflects a greater clinical complexity for this patient group. Another unanticipated finding was the substantial number of patients (58 or 16%) with more than one admission for reconditioning over the 2-year period. A pattern of episode changes from sub-acute services (rehabilitation) to acute services (e.g., general medical and nephology) followed by a return to rehabilitation for reconditioning was identified. While we can speculate that changes in health status are common in this patient cohort, it highlights the lack of continuity of care for this vulnerable group. Consistent with the literature, patients aged over 80 had less time between admissions to hospital and to rehabilitation, with a high incidence of multiple admissions confirming that older adults are more susceptible to hospital-acquired deconditioning.22,23 The number discharged to residential aged care was low (n = 8), possibly linked to an episode of care change such as to maintenance care, transition care, or an Aged Care Assessment Team approval. 23
When compared to data from the Australian Bureau of Statistics 20 there was a higher proportion of males in our sample; with men were more likely to be smokers and to discharge at own risk. This could be attributable to the differences in risk-taking behaviours between genders. When compared to males, females spent more time in rehabilitation and were more likely to go home or to residential aged care. It would be beneficial for future studies to consider social situation as this was not included in our data set.
There were nine admissions of eight people who identified as Indigenous, with a mean age of 51. Acknowledging the small number, this is a 24-year age difference from the mean age of 75 for the entire sample. This is consistent with national data and inequities in health outcomes when comparing Indigenous people to non-Indigenous people. 24 Further research into why Indigenous people are experiencing hospital-acquired deconditioning at a younger age is warranted, along with developing culturally sensitive reconditioning programs. 24
Similarly, the high number of admissions from nephrology prompts investigations into why this cohort is becoming deconditioned so to develop preventative strategies. Patients undergoing dialysis are likely to be sedentary and exhibit physical decline with associated frailty, experiencing multiple changes in wards and fragmented care. 25 People with chronic kidney disease are a fast-growing group that require bespoke service pathways to manage future pressures on health services. 26
The most admissions were listed under rehabilitation (n = 176) which was an unexpected finding as it seemed unlikely that a patient would require reconditioning when they were already undergoing rehabilitation. Further investigations showed a pattern of episode changes, moves from one hospital facility to another with the health service. This was a limitation within our study as there was no definitive method to delineate which wards patients were coming from within the hospital. The hospital staff suggested that these patients may have been receiving rehabilitation while still classified as acute under the ‘Rehabilitation Response Team’ and admitted to inpatient rehabilitation through this pathway. Admission source was further complicated as wards closed and reclassified to COVID wards in late 2020, with lack of clarity regarding the dates of these changes.
Deconditioning in an inpatient hospital setting is managed by a multidisciplinary team involving medical, nursing, and allied health staff..7,27,28 The occupational therapist's role within the team is to promote independence by engaging patients in activities meaningful to them, adapting or modifying tasks, and recommending aids, equipment, education, and home modifications to support discharge.29,30 This study was driven by occupational therapists, and adds to the understanding of the client group which to date have been viewed in the literature as a homogenous group of predominantly older people. Hospital-acquired deconditioning reduces independence and impacts a person's ability to conduct their activities of daily living at any age. Occupational deprivation for the patient results in mental decline, loss of sense of self, boredom, and feelings of alienation from past roles. 31 This reduced functioning impacts the patients’ quality of life and increases the burden of care. 32 To date, there has been few studies focused on occupational therapy interventions for reconditioning albeit limited to older adults.33,34 While the findings of this current study enhance the understanding of the broader patient group to inform clinical practice, there are some clear limitations.
Auditing existing hospital information systems, enabled access to a large amount of data, and a larger sample size allows for greater significance and generalisability. 35 Retrospective studies rely on the accuracy of those who recorded the data and there is no option to seek clarification. Hence there were many factors which lacked clarity, such as admission source and episode change. Definitions of what constitutes hospital – acquired deconditioning are a key limitation may lead to inconsistent referral patterns. 8 This research used a snapshot of 2 years with the risk that data may be skewed by local biases and unknown factors.36,37 In addition, we have only conducted a descriptive analysis. Notably, our study included data from the pre-pandemic period to get an uninterrupted picture of hospital-acquired deconditioning.
In conclusion, this study found that hospital-acquired deconditioning affects many patients each year, diverse both in age and aetiology. The clinical implications are that a one-size fits all approach to rehabilitation of patients requiring reconditioning is likely to be ineffective and further study is required to contribute to the evidence. Triaging groups with clearer definition may assist to ensure that meaningful interventions are being identified, for example smoking cessation pathways for younger males, or culturally appropriate interventions for Indigenous people. Further investigations are warranted to understand how deconditioning can be prevented, and to identify clinical areas to target (such as nephology) and varying age groups. Using the characteristics to identify population specific rehabilitation approaches has promise as meaningful goals to a 45-year-old may differ greatly to that of an 85-year-old. Finally, creation of clinical guidelines, such as the ones for stroke or pressure injuries with clear definitions to ensure an evidence based, person centred approach is received by all persons requiring reconditioning services is recommended.
Footnotes
Acknowledgements
Appreciation to the support of Dr Ben Chen, Director of Rehabilitation, Gold Coast Health. Additionally, we acknowledge the generous assistance of the data custodians in medical records for deidentifying and supplying the final data set.
Ethical approval
Health research ethics committee approval reference: LNR/2021/QGC/80463.
Authors’ contributions
Alison Willis conducted this research as a component of her master's in occupational therapy including data analysis, literature review and preparation of final manuscript. Chloe Henly and Aleksandra Ballingall are occupational therapists employed at the rehabilitation service and assisted with data analysis, clinical interpretation of results and relevance to practice. Professor Susan Brandis, primary investigator and research supervisor, is responsible for project inception, design, ethics and oversight including data analysis, presentation and preparation of final manuscript.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
