Abstract
Objective
This study aimed to explore the acceptability and factors that influenced implementation of a multidomain, home-based fall prevention programme (
Design
Qualitative, inductive thematic analysis of semi-structured interviews.
Setting
Homes of
Participants
Eighteen interviews with people with Parkinson's disease and/or their care-partner who were purposively sampled after completing
Intervention
Results
Five themes were identified: (a) the importance of personalisation, (b) a collaborative effort, (c) capacity building, (d) navigating fall risk with Parkinson's is complex and (e) the ease (or not) of making changes. Participants and their care-partners appreciated the personalised, home-based programme that involved shared decision-making and was delivered by expert therapists. They developed increased safety awareness and problem-solving skills. Making improvements, receiving ongoing support from therapists and care-partners and making change easier promoted sustained engagement. However, some participants faced emotional and psychological barriers to engagement including fatalistic beliefs about disease progression and a desire to avoid appearing ‘disabled’. The reality of Parkinson's disease motivated participants to make changes but Parkinson's-related impairments such as apathy and motor fluctuations hindered this.
Conclusions
People with Parkinson's disease who are recurrent fallers, and their care-partners, found the
Introduction
Parkinson's disease is the fastest growing neurodegenerative disease, with the number of people with Parkinson's disease globally expected to double between 2020 and 2040, exceeding 12 million people. 1 Falls increase as the disease advances, and around two-thirds of those who fall do so recurrently. 2 These falls are personally and financially costly.3,4 Fall prevention strategies that are effective across the disease spectrum are therefore urgently needed to reduce the fall-related healthcare needs of this growing population.
Fall prevention exercise programmes reduce falls in people with mild to moderate Parkinson's disease by around 26%, 5 leaving an unacceptably high fall rate. The World Guidelines for Falls Prevention 6 recommends personalised multidomain interventions be delivered by multidisciplinary teams including occupational therapists and physiotherapists. This includes a conditional recommendation that people with Parkinson's disease specifically be offered multidomain interventions, with further research required. 6
Our research team recently designed and tested the
Methods
Semi-structured interviews conducted between July 2021 and February 2024 were used to explore participants’ views in depth. Interviews were analysed with reflexive, inductive thematic analysis, using an interpretivist paradigm8,9 that enabled subjective interpretations of experiences without preconceived hypotheses. Ethical approval was granted by the University's Human Research Ethics Committee (2019/034) prior to commencing recruitment. All participants with Parkinson's disease and any participating care-partners provided written informed consent. This study is reported using the Standards for Reporting Qualitative Research. 10
Eighteen interviews were analysed: ten dyads (people with Parkinson's disease and their care-partner), two interviews with only the care-partner and six with only the person with Parkinson's disease. Eligibility for the
Details of the
Semi-structured interviews lasting up to 60 minutes were conducted with the participant at home, over the phone or via video call based on participant preference. Interviews were conducted 1 to 2 weeks after the post-intervention assessment. Participating care-partners were interviewed alongside the person with Parkinson's disease. The female interviewer (RS) was an experienced research physiotherapist; she had previously conducted research interviews and received training and guidance from researchers with qualitative experience (NEA and CGC). Participants were aware that the interviewer was a physiotherapist as she completed the post-intervention assessments, but participants had no other relationship with her. The interviewer was not involved in delivering the intervention, thereby minimising potential bias in her approach or in participant responses. An interview guide with prompts was used to ensure consistency while allowing flexibility to probe responses as needed (see Online Supplementary Material 1). The interviewer recorded field notes at the end of each interview. Interview audio was digitally recorded and transcribed verbatim by a transcription service. Member checking was not used to avoid overburdening participants. 13 Instead, the interviewer summarised and checked the key points with the participants at the end of each section of the interview.
Data was analysed thematically 8 by a team of physiotherapy researchers with qualitative research experience (NEA, LG, SSP), physiotherapy honours students (AD, ST) and a medical student who was also an occupational therapist (CK). Analysis was facilitated by NVivo 14 (Lumivero, Denver, CO). All transcripts and field notes were read multiple times and coded line by line by one researcher (NEA) and by at least one other researcher to achieve researcher triangulation. Codes reflecting similar ideas were grouped into themes and subthemes through an iterative process of discussions amongst the team until consensus was reached. Final themes were agreed upon by all authors. To protect participant privacy quotes have been anonymised.
Results
Participant characteristics are presented in Table 1. Overall, participants were a mean (SD) of 14 (7) years since diagnosis, had moderate to advanced Parkinson's disease and fell recurrently, with a median of 22 falls per person in the year prior to commencing the
Characteristics of the participants with Parkinson's disease.
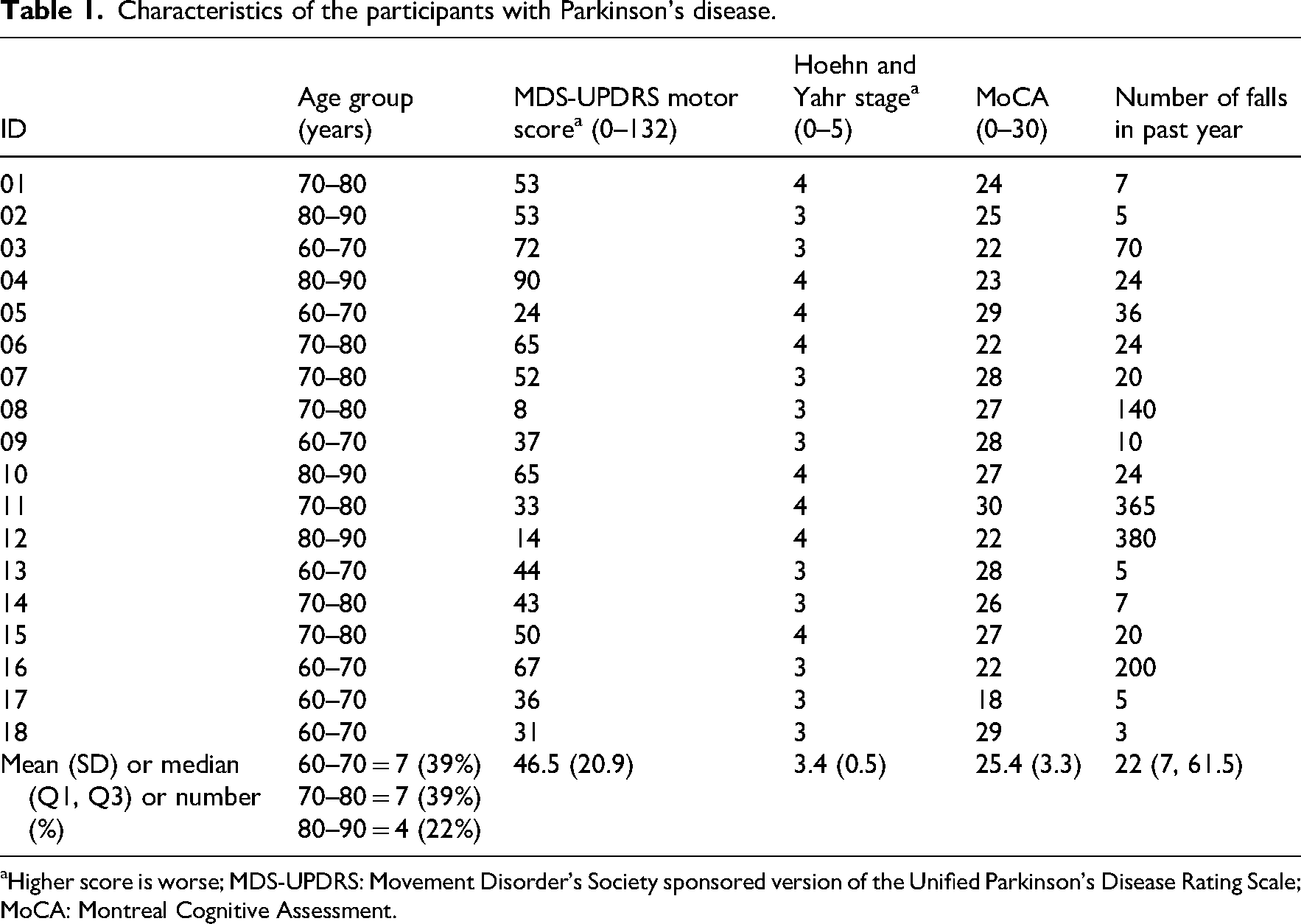
Higher score is worse; MDS-UPDRS: Movement Disorder's Society sponsored version of the Unified Parkinson's Disease Rating Scale; MoCA: Montreal Cognitive Assessment.
Five main themes with associated subthemes were elucidated from the experiences of people with Parkinson's disease and care-partners regarding the
The importance of personalisation
Tailor-made for one
Participants appreciated the programme was individualised to address their personal Parkinson's disease impairments (e.g. freezing of gait) and activity limitations. They described previous experiences in ‘one size fits all’ group programmes as not entirely meeting their complex needs. The delivery of the programme in the home environment was a key part of the tailoring process, as therapists could contextualise the individual's mobility problems. Being at home allowed ‘
The programme was flexible to meet needs
In addition to the programme being personally tailored, participants appreciated that it could be adapted to accommodate unexpected or additional constraints, such as busyness, fatigue or pain.
A collaborative effort
Involvement in decision making
Participants reported they were able to have a ‘
The value of expert knowledge
Participants valued therapists’ extensive knowledge about Parkinson's disease and intervention that specifically accounted for their problems. Some explained that they had not made home safety changes earlier as they did not know what changes to make. Several noted that they now had strategies that helped them to manage their freezing of gait and therefore walk more safely.
However, one participant felt the programme did not add to their knowledge about safer mobility due to previous health professional input.
Support and accountability
Regular discussions with the therapists provided support and positive reinforcement that helped participants to adhere to the programme and continually adapt it to their needs. One participant described the therapist as ‘
For most participants, care-partners played an important supportive role, providing encouragement and prompts to exercise and use safer mobility strategies. Active care-partner involvement also ensured participants completed the intervention optimally and remained committed to the programme.
Care-partners also expressed that they felt reassured and supported by the therapists. This support was enhanced when participant dyads shared mutual beliefs about the benefit of the intervention. However, when beliefs were conflicting, the care-partner was less able to encourage positive change and at times tension arose in the relationship. Person with Parkinson's disease: Care-partner:
Capacity building
Planning to be safe
Some participants chose to avoid activities they felt they were unable to complete safely. In contrast, one spoke of increased confidence in his abilities after completing the programme but reflected that at times this led to carelessness.
Despite the ability to identify risky activities, a few participants noted that the desire or need to undertake the activity superseded any concern about falling. One described needing to leave his walker behind when working in his garage as the space was not conducive to using a mobility aid. Another felt compelled to climb a stepladder to reach an item as there was no-one else to do it. Participants described how they were careful when doing these activities. While participants noted that increased safety awareness helped to reduce falls, some found the extra vigilance difficult to maintain.
Adapting and equipping for the future
Participants were able to extrapolate from their prescribed home hazard reduction recommendations and safer movement strategies and develop their own strategies in different and novel situations. One participant described how she implemented her own movement strategy to make golfing safer.
Participants also described how their new awareness, knowledge and skills in planning to be safe would equip them to solve mobility safety issues into the future. They described improved awareness of when to seek help and would likely seek expert advice before making any significant changes in relation to home hazard reduction.
Navigating fall risk with Parkinson’s is complex
The reality of Parkinson's as motivation
Having a progressive condition motivated participants to complete the
For some, the realisation that they had already experienced deterioration underscored the necessity of the intervention, prompting them to take action to reduce their fall risk.
Participants often described how education and support from the therapists helped them reframe Parkinson's disease as a manageable condition
Some participants were reluctant to implement home hazard reduction measures due to concerns about aesthetics and the emotional impact of acknowledging functional decline, viewing it as ‘
A few wanted to continue undertaking certain high-risk activities, as they did not want to admit they were not able to do them safely anymore.
Parkinson's takes control
Some people with Parkinson's disease expressed frustration with their impairments interfering with their ability to engage with the programme. They spoke of challenges due to poor memory, fatigue, apathy, anxiety and motor fluctuations.
The ease (or not) of making changes
System barriers
For larger home fall-hazard reduction changes such as installation of ramps and rails which required external service providers, participants often cited barriers and lengthy delays related to government means testing and approval processes. The occupational therapist was able to guide people through the process and expedite it when necessary.
Competing priorities
Competing priorities affecting time, energy and money influenced programme adherence. Most participants reported they had plenty of time to undertake the program, as they were retired and the COVID-19 pandemic restricted their social life. Others described difficulty finding time to exercise or preferring to do exercises and physical activity different to ones prescribed. Additionally, participants spoke of having a finite amount of physical and cognitive energy with which to achieve their daily tasks and explained that completing the programme was not always their highest priority. Participants also spoke of competing financial priorities preventing them from making some of the home fall-hazard reduction changes.
Making new habits is hard (but possible)
Participants spoke of difficulties establishing new habits for exercise or using safer mobility strategies. They described that a regular exercise habit was made easier by therapists assisting them to determine how they could build the exercise into their daily routines. The provision of a simple instruction booklet with pictures also helped, with some using the booklet as a prompt to exercise. Therapists promoted the use of safer mobility strategies through repetition, mantras (e.g. stop, think, be safe), and signs and notes placed strategically in the environment as reminders.
Care-partners often provided prompts for completing the exercises and using the safer mobility strategies. Notably, some care-partners expressed that they would regularly prompt the safer mobility strategies, but preferred not to prompt the exercise too often as they felt it was bad for their relationship.
Participants also described the environment itself became a cue to use a safer movement strategy, as they had repeatedly practiced the strategy in that area. They became better at recognising near falls or precursors to falls, such as gait festination, and used these as prompts to implement their safer mobility strategy. Many participants reported that at least some of their strategies were becoming a habit, though often they could not say how the habit formation had occurred.
Discussion
This study found the
This study builds on previous fall prevention and exercise-based research, including the PDSAFE trial,14,15 which offered a personalised, home-based programme consisting of fall prevention exercise and strategies delivered by physiotherapists. Like
The acceptability of home fall-hazard reduction for people with Parkinson's disease has been underexplored. This study identified factors influencing adherence that align with findings in the general older population, including greater willingness to modify the home when the need and benefits were clearly understood.19,20 Shared decision making with expert therapists improved tailoring and acceptance of recommendations.20,21 Barriers mirrored those in previous research, including competing priorities (financial and time),22,23 stigma around aesthetics19,20 and system challenges20,23 such as navigating processes and delays in subsidised modifications. Support from healthcare providers (e.g. occupational therapists), particularly in coordinating with external agencies, can improve implementation. 24
Little is known about the acceptability of safer mobility strategies. Previous research with older adults 25 and people with Parkinson's disease26,27 described how people balanced the risk of falling with their desire to engage in enjoyable activities, maintain independence and live a ‘normal’ life. In this study, most participants were motivated to use safer mobility strategies to reduce their risk of falling, with greater movement awareness and planning for safety during risky activities. Reminders from care-partners, signs, notes, mantras and practice in the appropriate environment encouraged use of these strategies. However, making new safer mobility strategies a habitual part of daily routines was challenging. Habit formation involves cue-association mechanisms learned through repetition in specific contexts. 28 People with Parkinson's disease may struggle to establish new habits due to deficits in automaticity and motor learning. 29 Nonetheless, some participants in this study developed habits through intentional and context-driven practice over 6 months. Research is required to further explore strategies to optimally promote habit formation in people with Parkinson's disease, including those with cognitive decline.
Several clinical implications for fall prevention in people with moderate to advanced Parkinson's disease are highlighted by this study. Multidomain interventions are complex, therefore care-partners play an important role by supporting, encouraging and prompting participants. This was particularly important for those with impaired cognition. Care-partners therefore require appropriate training and support to fulfil their role safely and effectively without adding to their burden of care. Health professionals should also consider any potential psychological and emotional barriers to adopting fall prevention programmes, including difficulty accepting change, fear of appearing ‘disabled’ and fatalistic beliefs. Empathy and support from therapists can help people adjust to changes as their needs evolve over time.
Health professionals should also uphold the principle of dignity of risk, 30 allowing people with Parkinson's disease autonomy to choose which recommendations to follow. Some participants chose to undertake certain high-risk activities as the desire or need to undertake the activity outweighed the risk of falls. Further research is required to explore optimal implementation of this principle in clinical practice and the role of behaviour change techniques to address barriers to fall prevention, 31 such as social support and reframing perspectives on change. Such research may provide additional insights into increasing acceptance and adherence to fall prevention strategies.
This study also underscores the importance of involving people with Parkinson's disease and their care-partners in shared problem solving and collaborative goal setting. Participants valued being involved in individualising their fall prevention programme, which increased engagement. Equipping people with Parkinson's disease and their care-partners with fall-prevention knowledge and skills will help build their capacity to manage falls now and into the future when circumstances change.
This study had several limitations. The sample consisted of volunteers, who were possibly more motivated than the general Parkinson's population. Insights from less interested individuals may be lacking. Furthermore, although the study included participants with impaired cognition, those with severe cognitive impairments were excluded, meaning their perspectives and those of their care-partners were not represented. Despite encouragement for honest feedback, participants may have given positive responses to please the interviewer or avoid seeming critical.
In conclusion, this study provides new insights into how people with Parkinson's disease and their care-partners engage with a multidomain fall prevention intervention. Engagement was enhanced by the personalised and collaborative approach between participants and therapists. Participants felt empowered and better equipped to identify and address mobility safety-related problems and were motivated by their own improvements and their desire to remain independent. Conversely, engagement was hindered by fatalistic beliefs, emotional and psychological readiness for change, Parkinson's disease impairments, competing priorities and system-related barriers. Future research should address these barriers and further investigate the benefits of tailored, multidomain interventions on reducing falls in people with Parkinson's disease.
People with Parkinson's disease who have recurrent falls plus care-partners found a home-based multidomain fall prevention programme acceptable. Participants valued individualised programmes, shared decision-making, therapist expertise and increased their safety awareness during movement. Emotional and psychological barriers, such as fear of appearing disabled, need to be addressed.Clinical messages
Supplemental Material
sj-docx-1-cre-10.1177_02692155251365151 - Supplemental material for Acceptability of a programme for safer mobility (INTEGRATE): Perspectives of people with Parkinson’s disease and their care-partners
Supplemental material, sj-docx-1-cre-10.1177_02692155251365151 for Acceptability of a programme for safer mobility (INTEGRATE): Perspectives of people with Parkinson’s disease and their care-partners by Natalie E Allen, Annabel Darmali, Cecelia Koch, Sammi Tran, Serene S Paul, Colleen G Canning, Simone Edwards, Susan Harkness, Roslyn Savage, Lyndell Webster, Genevieve Zelma and Lina Goh in Clinical Rehabilitation
Supplemental Material
sj-docx-2-cre-10.1177_02692155251365151 - Supplemental material for Acceptability of a programme for safer mobility (INTEGRATE): Perspectives of people with Parkinson’s disease and their care-partners
Supplemental material, sj-docx-2-cre-10.1177_02692155251365151 for Acceptability of a programme for safer mobility (INTEGRATE): Perspectives of people with Parkinson’s disease and their care-partners by Natalie E Allen, Annabel Darmali, Cecelia Koch, Sammi Tran, Serene S Paul, Colleen G Canning, Simone Edwards, Susan Harkness, Roslyn Savage, Lyndell Webster, Genevieve Zelma and Lina Goh in Clinical Rehabilitation
Footnotes
Acknowledgements
The authors would like to thank the participants in this study.
Author contributions
NEA, SSP, CGC, contributed to the concept and design of the study, NEA, SSP, SH, RS, LG organised the study, NEA, SE, SH, RS, LW, GZ, LG provided the intervention and collected the data, NEA, AD, CK, ST, SSP, LG completed the analysis and interpretation of the results, NEA, AD, CK, ST, SSP, CGC, SE, SH, RS, LW, GZ, LG contributed to the writing of the manuscript.
Ethical considerations
This project received ethical approval from The University of Sydney's Human Research Ethics Committee (ref: 2019/034).
Consent to participate
All participants provided written informed consent prior to enrolment.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This study was funded by a Parkinson's NSW Research Grant, a University of Sydney Laffan Equity Prize and The University of Sydney DVCR Support Fund for COVID-19 impacted research.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Data availability
The data supporting the findings of this study are available within the article. Individual transcripts cannot be provided as participants did not provide consent for that.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
