Abstract
Objective
The Take Charge intervention, delivered early after hospital discharge following acute stroke, is effective at improving 12-month health status, independence and advanced activities of daily living. This study aims to provide a deeper understanding of the experiences of receiving Take Charge.
Design
This was a qualitative study nested within a large randomised control trial, the Taking Charge After Stroke (TaCAS) study. Data were analysed using thematic analysis, and we describe our findings using interpretive description.
Participants
People with stroke aged over 18 years, who were participants in the TaCAS study conducted in Aotearoa New Zealand.
Intervention
Take Charge, a person-centred conversation delivered face-to-face, designed to explore a person's identity and priorities, conducted by a trained facilitator and guided by a workbook.
Results
We interviewed nine participants, three from each of the three arms of the TaCAS trial – each would have received one, two, or zero Take Charge sessions (the control group). The overall theme of ‘Doing things my way/coming to know my own wisdom and expertise’ was enabled by ‘being listened to and feeling heard’ and ‘focusing on the goals which were important to me’, both strongly expressed by people who received the Take Charge intervention, and hindered by ‘medical paternalism’ and ‘loss of sense of self/“not me”’ most commonly expressed by people in the control arm.
Conclusions
The Take Charge intervention empowers people with stroke by enhancing intrinsic motivation. A trusting, therapeutic relationship and non-judgemental facilitation are essential to ensure that the person feels heard.
Introduction
Stroke affects approximately 12.2 million people worldwide each year, with over 101 million people currently living who have experienced stroke. 1 In high-income countries, therapist-led rehabilitation is the mainstay of subacute care, particularly aimed at physical impairments following stroke. However, many people with stroke and their families continue to live with ongoing impacts of stroke that affect their quality of life, well-being, and psychosocial health, which are often poorly addressed in routine care.2,3
Take Charge is a novel rehabilitation intervention. Designed to be provided in the first few weeks after discharge home, it has been shown to be effective in improving 12-month health-related quality of life, advanced activities of daily living and independence in two randomised controlled trials when delivered face-to-face.4,5 These tested Take Charge in Indigenous and non-Indigenous people with stroke in Aotearoa New Zealand and are referred to as the Māori and Pacific Stroke Study (MAPSS) 4 and the Taking Charge After Stroke (TaCAS) 5 trial. The intervention's design was informed by Self Determination Theory which purports that the needs for competence, connectedness, and autonomy are essential for personal growth, integration, intrinsic motivation, and well-being. 6 It is proposed that the Take Charge intervention produces positive outcomes by encouraging self-confidence and intrinsic motivation and providing permission and support for people to ‘take charge’ of their own lives after stroke. 7 Prior work has shown ‘taking charge’ as an important positive step in rehabilitation for any person after stroke and for other disabling conditions. 8
The aim of this research was to understand how the TaCAS intervention appeared to impact on people's recovery, by contrasting the experiences of those who did and did not receive Take Charge.
Method
Taking Charge after stroke intervention
The TaCAS randomised controlled trial 5 that this qualitative study is nested within was conducted between 2016 and 2019 in seven New Zealand centres. Four hundred people discharged to community living after acute stroke (ischaemic stroke or intracerebral haemorrhage) were randomised to one of three groups, all of whom received usual care including community rehabilitation where clinically appropriate. The control group received a brief educational intervention, at a single visit, focused on future stroke prevention. The other two groups received either a single Take Charge session (TCS) or two Take Charge sessions, six weeks apart. The Take Charge intervention is described fully elsewhere 9 but briefly, is a time-unlimited (usually 45–60 min on average) session in the person's home with a trained facilitator using a short, illustrated booklet. 10 The facilitator is trained to listen and reflect rather than talk and asks the person with stroke to describe ‘who they really are’ as a person, separate from their stroke, what their hopes and fears are for the next 12 months and beyond, and what steps they may take to achieve those hopes. The person is encouraged to write in the booklet which they keep. Family members may or may not be present and can be encouraged to support the person with stroke.
Ethics approval was obtained from the NZ Health and Disability Ethics Committee (ref. 15/CEN/115). All participants provided written informed consent. The trial was registered with the Australia and New Zealand Clinical Trials Registry (ACTRN12615001163594) and funded by the Health Research Council of New Zealand (15/297).
Methodology
This nested study used Interpretive Description methodology. 11 It was initiated after the TaCAS trial's 12-month follow-ups began, when it became apparent that rich insights into participants’ recovery experiences were not fully captured in quantitative outcome measures. We sought to generate an interpretive description of people's experiences of ‘taking charge’, reflecting the methodological intent of producing clinically relevant knowledge that could inform future practice. 11 We reported our findings using the COREQ framework. 12
Participant recruitment and data analysis
Potential participants were identified by the blinded assessor who completed the 12-month outcome assessments for the TaCAS trial. After these data were locked, the assessor initiated a conversation with the participant about their life after stroke, and unblinded themself to the participant's allocation. This conversation was the first step in our purposive sampling approach, which focused on intensity sampling. 13 This approach enabled us to select a small number of cases that would be more likely to have in-depth knowledge and experience about taking charge of their lives after stroke, i.e., those who appeared to experience the concept of ‘taking charge’. Participant selection was led by the assessor in consultation with study team members
The key inclusion criterion for this study was participants who spontaneously spoke about ‘taking charge’ after their stroke, how the stroke impacted them, and how they overcame these consequences. Of those who met this criterion, we selected participants who recalled receiving Take Charge and details of the intervention visit(s), and for the sake of comparison, we also sought control participants who had not received Take Charge but who also spontaneously spoke of their experiences of ‘taking charge’, to determine if, and how, their experiences were different. Other inclusion criteria included: participants residing within the greater Wellington region (urban and rural settings), could communicate sufficiently in English, and able to provide informed consent. People with cognitive impairment or aphasia were included, as long as they were capable of indicating informed consent.
We sought equal representation across the three groups of participants with three participants from each arm of the TaCAS trial (control vs. one TC session vs. 2 TC sessions). The semi-structured interviews explored peoples’ perspective on their own recovery (see Supplementary material) and lasted 30‒45 min. They took place in the participants’ homes between 13 and 16 months after stroke, and between 14 and 20 months after receiving the intervention or active control visit. The interviewer (KMF) was an experienced community nurse who had no prior relationship to the participants. She had previously been a Take Charge facilitator, but not with any of the interview subjects, and had not met them before the interview. Interviews were audiotaped and transcribed. After transcription, the interviews were sent back to the participants who validated their content.
We carried out data collection and analysis simultaneously and modified the interview questions during the process to extend our analysis. The team analysing the data included: the nurse-researcher conducting the interviews who was a trained Take Charge facilitator; and a physician-researcher who was the blinded outcomes assessor, who had not delivered a Take Charge session in the trial. We coded the interviews individually at first, and then met frequently to review our findings. We used NVivo software (Lumivero) to manage data analysis.
We used a general inductive approach to analysis. 14 In initial coding, we particularly attuned to how people described taking charge after stroke and what appeared to influence this. For those who received the intervention, we focused on their experience and whether (and how) they felt Take Charge may have helped. From this, we developed categories and proposed themes representing their perspectives and experiences.
Results
Nine participants were recruited. Equal numbers were in each arm of the TaCAS trial. Five participants were women, and four were men. The mean age of participants was 67 years (range 50‒84 years). All participants were Caucasian (NZ European/Pākehā).
Key themes
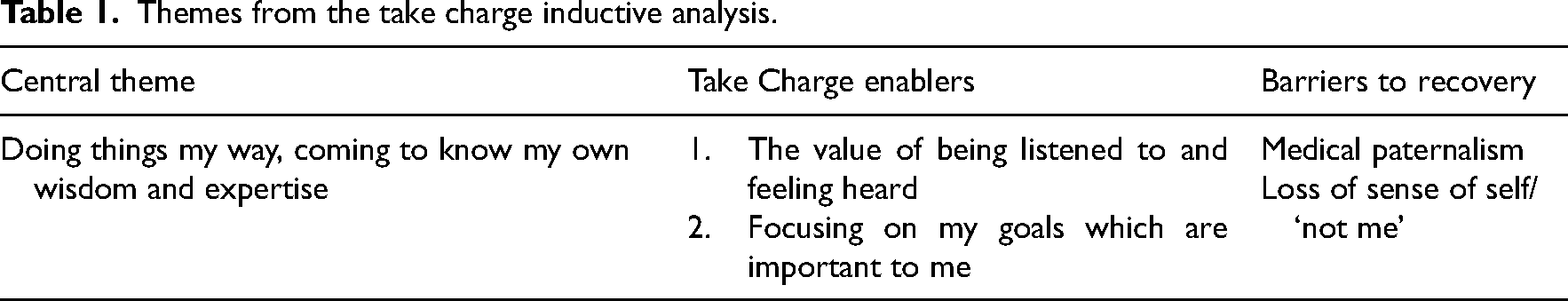
We identified one overarching theme from all the interviews: ‘Doing things my way, coming to my own wisdom and expertise’. This expressed the participants’ primary message for recovery. The main sub-themes reflect two key features of Take Charge that supported recovery: (a) being listened to and feeling heard; and (b) focusing on my goals, which are important to me. These themes are presented in Table 1.
Themes from the take charge inductive analysis.
Being listened to and feeling heard
Participants who received the Take Charge intervention valued feeling heard. Active listening is a vital part of the intervention; in feeling heard, participants felt that their opinions mattered and held value. ‘Being listened to’ appeared an important first step toward empowerment and exercising their autonomy and agency to ‘do things my way’.
It was quite a psychological thing for me. [The opportunity to talk] was very significant … I was in tears actually towards the end. I felt it was just good because I could talk to somebody about it. It did me a world of good.
(Participant 2, 50M, two TCS)
Being listened to contrasted with common experiences in stroke services. Participants described feelings of depersonalisation when being categorised by age, or their stroke deficits, rather than being seen as a whole person. One participant said it felt like being ‘put in a box’ (Participant 6, 84F, two TCS). Connected with this was a feeling that much of the advice from therapists was ‘scripted’ (Participant 1, 66M, one TCS) and inflexible and would have been the same for any person with similar stroke deficits, but that this was ‘not me’.
Others were clear that as the person with stroke, their perspectives were not sought and they were not involved in decision-making: ‘They [health care professionals] have their own fixed … you know … this is where you are, this is what you should be doing, you know. So … that's very fixed. There's about five or six people involved in this thing, making decisions about me. Every time I see someone they give you a form and tick, tick, tick … no you’re not depressed. I say I know I’m not depressed … why did you give me the bloody form then? But you know it's standard procedure.’
(Participant 7, 57M, control)
Focusing on my goals which are important to me
The Take Charge intervention helped participants to identify and focus on what they wanted to achieve. The conversations prompted them to re-connect with the person they are, and to think widely about what was important to them, beyond impairments or lower-level goals commonly set in stroke services. ‘It [Take Charge] was the most helpful thing out of everything that was going on … people have to latch on to something that is important to them because I think that that is something that can pull them through. They have to think about what works for them, I guess … I really sort of think that everybody must surely have something that they love, they used to love doing..’
(Participant 4, 53F, one TCS)
Being able to describe higher-level goals and not just small goals was important for some. Participant 3 (72F, one TCS) spoke about how having such a big goal ‘seemed to be way out there’, but she believed that having it enhanced her recovery. Initially, she was overwhelmed and unsure, recalling that the stroke had caused significant anxiety and fear. By setting personalised goals during Take Charge, she was able to break down her higher-level goals into smaller, doable steps that were acceptable to her, which helped her to look beyond her fears and persevere. By 12 months after stroke, she had made plans to return for short periods to the classroom as a relief teacher. ‘I thought, that was one of my goals and I need to achieve it and I put it off and I put it off and I thought, Ok I’ll do that before she comes, … I didn’t want to do it but I did do it … in trepidation I would take my steps and I’d walk up to the bus stop then back again, it's only a little way and I thought that's pathetic but it was big for me, and sometimes I’d do it twice, and then I went a bit further up to the school and back and then a little bit further past the school and then I thought I think I can tackle going around this way … but I had to work up to it.’
(Participant 3, 72F, one TCS)
Of note, when the Take Charge participants were interviewed 14 to 20 months after the intervention, most had achieved the goals that they set during the Take Charge session despite initially considering some goals to be unattainable.
Many participants who received Take Charge commented on the value of writing goals down in the booklet. Doing so helped them see the reality of their goals and provided them with structure and a pathway forward. Used within the context of the Take Charge session, the written record enabled people to focus, to avoid being distracted or dominated by fears (of inadvertently harming themselves) and enabled them to visualise, and chart, a way forward toward goal attainment, and to keep track of progress. ‘That booklet thing made me just sort of … put things in check a wee bit and I made sure of it, of doing what we wrote down and said and talked about … and actually doing them and achieving them and just putting other things … I’m not going to do other things until I’ve done that.’
(Participant 2, 50M, two TCS)
The process of writing down personal goals was also important in the context of post-stroke challenges such as changes in executive function. ‘I think if I probably didn’t have them written down, I would have been too busy jumping from one thing to another and I wouldn’t have improved on any, but because I had written it down, I would do that…’
(Participant 6, 86F, two TCS)
Conflict with others over ‘appropriate’ goals was a particular issue. One participant believed that being able to dress herself was an important goal and that she had the common sense to work towards achieving it, but her family doctor disapproved of her goals under the guise of safety concerns. ‘I’d put down balancing on one leg to get my knickers and jeans on … she asked me what they were and inwardly I laughed because I told her what they were, and her eyes shut up, and she said, “Oh … you must sit down when you put your knickers on … you’re too old, you might fall”, and then she … proceeded to show me this demonstration … but once again, I don’t put them on standing in the middle of nowhere! I’m standing by my bed with the dressing table so I can put my hand there or fall on the bed … I’m taking precautions!’
(Participant 6, 86F, two TCS)
This was an example of the person with stroke facing a barrier of medical paternalism. For this participant, the paternalism may have been an additional, paradoxical, motivating factor to overcome. For others, the judgment and projection of paternalistic attitudes by medical professionals, friends, and family had a significant disempowering effect. Participants described feeling overprotected and being frustrated with health professionals’ tendency to be risk averse. They sensed that health professionals had an attitude that they knew better than the participant about what was good for them. ‘Doctors are very, very cautious and that's my experience with the whole thing. They’re risk averse. Oh, don’t do that, you might fall. Well, I haven’t fallen!’
(Participant 7, 57M, control)
The maintenance of listening without judgment, criticism, or warning throughout the Take Charge intervention created space for people to have control and provided recognition of a person's expertise in themselves. Thus, the person with stroke had the freedom, autonomy, and support to work on the goal-setting component of the Take Charge session: identifying, writing down, and breaking down personally meaningful and important goals into smaller steps. This promoted self-determination and motivation during stroke recovery.
Doing things my way and coming to my own wisdom
A recurrent theme from all interviews was the importance of the need to ‘understand myself’ and ‘do things my way’. Participants talked about coming to their own understanding of who they are, what was important to them, what motivated them, what personal characteristics or strengths they had which could help them in their rehabilitation, knowing their own needs, and working out their own ways of managing new challenges they faced. Box 1 lists the different concepts that were described as self-actualised by participants. ‘You do have to take what you have, what in life you have, and run with it or enjoy it or whatever … whatever capacity you have to live life … I’ve got to live life as best I can. It's got to come from your heart.’
(Participant 3, 72F, one TCS)
List of concepts about which recipients of Take Charge came to their own wisdom.
Who I am
What is important to me
What motivates me
What personal characteristics/strengths I have, that can help me in my rehabilitation
What my needs are
How to manage new challenges
Take Charge provided people with a sense of supported autonomy – through being listened to and heard, through identifying and working toward goals that mattered, and over time they came to have confidence in themselves their expertise and their wisdom. They knew what was important, they knew what they needed to focus on, they figured out what worked for them, and they came to have a strong sense of knowing and valuing themselves.
One participant described how engaging in Take Charge helped build self-confidence. Doing things ‘her way’ on this occasion changed her outlook: ‘That [Take Charge] gave me confidence to realise … I had always been very much in awe of doctors, my generation were, doctors were God, you know…and but this gave me confidence to follow my own instincts a little bit and push myself because I felt like I had it up here (taps head) … I felt my reasoning wasn’t too bad and I was still thinking logically how to protect myself if I was going to do something, and so that made me motivated…’
(Participant 6, 86F, two TCS)
She was able to set aside the recommendations put to her by others who were trying to keep her safe, and to start to do things which stretched her. She chose to follow her own instincts and push herself. She refuted the overprotective approach of the health professionals because it was their duty to improve a person's well-being, and that would not be achieved by limiting what they could do.
Having confidence in oneself was seen as important. This encompassed a positive outlook, the idea that ‘I can do this’; often a degree of stubbornness was important for many. ‘I’m stubborn that way … you can’t walk? Well, who said I can’t walk! Well, I’m a doctor, I say you can’t walk. Oh, I’ll prove them wrong. I’ve always been that way. There's only so much the health system can do.’
(Participant 7, 57M, control)
Other participants spoke of the importance of self-belief accompanied by action, with some reporting a sense of personal responsibility for their own improvement. Regardless of participation in the Take Charge intervention, participants who would do what they wanted no matter what health professionals told them appeared to know within themselves that they were the experts. For others, this self-belief required the crucial element of time and came later.
All participants described variations of coming to their own wisdom as a gradual process of learning to listen to their bodies, adapting, practising, or approaching their recovery with a sense of humour. However, there were key differences between control and intervention participants: first, the theme of ‘feeling heard’ was absent from the control participants’ interviews; second, the Take Charge participants spoke of their self-realisation with confidence and hope. This self-assuredness was absent from the interviews with control participants, who spoke about learning to live with the consequences of stroke, but their tone and choice of words were resigned in comparison. They spoke more about realising their limitations. ‘A lot of things I’ve been doing I’m trying to do now to a limited extent, but … it just takes me that much longer to do. They did warn me that doing that sort of thing is not a good idea … so I’ve taken that on board, but it is one of the frustrations of … I can’t really do that sort of thing, working off a ladder. I’m not doing quite as much, but I’m still doing most of the things I want to. I suppose it's really at the point where I know I can’t do it that I’ve got to say, ok, well, that is completely beyond me, and that's something I recognise. There was no way I was going to be able to tackle that, but before the stroke I’m sure I would’ve done that myself.’
(Participant 8, 72M, control)
In contrast, participants who received Take Charge reflected on the insight, skills, and support which enabled them to take charge. ‘I … thought, ‘You know what, I’m just going to throw myself in’ and so I did. I threw myself in a dive sort of way and then realised I can dive in from here on in … so you’ve just got to test yourself all the time, I think. See what you can achieve… I think being you is important.’
(Participant 4, 53F, 1 TCS)
This suggests that the benefits of Take Charge extended beyond the goals set in the intervention, and the process of identifying what matters and working out how to do those things was transferrable to other contexts.
Discussion
The purpose of this study was to understand how Take Charge impacts people's recovery, and which components were most significant. We suggest that Take Charge systematically provides the tools of self-determination, allowing people to come to their own wisdom, contributing to higher self-confidence and better quality of life. Key components include a therapeutic relationship built on trust, where the person with stroke is comfortable to share their views, feels heard, and is supported to focus on meaningful aspects in their life.
The theme of ‘being heard’ was strikingly absent in control group interviews, suggesting that it is a unique, necessary characteristic of the Take Charge intervention. Our findings indicated that paternalistic attitudes, risk-averse behaviour, and depersonalised care by health professionals may inhibit recovery and contribute to not feeling heard. These results are consistent with other research which shows how powerlessness and paternalism are barriers to taking charge,15,16 and conflicts between areas of personal meaning and therapist-derived goals can result in not feeling heard. 16 We suggest that Take Charge sessions must provide for forming a connection, building trust, open and active participation, and maintaining a psychologically safe, therapeutic relationship; all conditions that make it more possible for the person with stroke to express themselves freely. 17 Prescriptive education or advice from the facilitator may limit their effectiveness or may even be detrimental if the participant feels uncomfortable expressing differing viewpoints. This is embedded in Take Charge facilitator training which emphasises encouraging ideas without judgment, criticism, or advice. 10
While all participants demonstrated aspects of ‘taking charge’ of their recovery, those in the intervention groups appeared more confident in themselves. Narratives reflected possibility and hope. For some, this may even reflect a process of post-traumatic growth. 18 These characteristics also align with supported self-management and supported efficacy, which are important after stroke.19,20 Supported self-management involves a supportive therapeutic relationship and partnership, a focus on meaningful goals, and building self-confidence, 21 while supported efficacy suggests that the clinician's belief in the person can help the person with stroke have more belief in themselves. Our research, and that from supported self-management 22 and self-efficacy, all highlight the facilitators’ engagement with the person with stroke is critical in creating conditions for people to take charge. In fact, we suggest that the facilitator and their way of working may have a potentiating effect, enabling greater confidence and independence than what the person may be able to achieve alone. This is reflected in the narrative differences between control and intervention groups and improved independence, daily activities, and quality of life in Take Charge participants. 5
Take Charge seeks to empower people to recognise, develop and use the ‘tools’ of self-determination: autonomy, mastery, and purpose. 6 Participants suggested that even those with a latent mindset to ‘take charge’ benefited from the intervention, with more focused goals and ownership of their goals. Facilitators encouraged them to dream big, not confining goals to what they considered achievable, as is common in rehabilitation. 23 Other authors have proposed that meaningful and aspirational goals, broken into actionable steps, build self-regulatory capacity. 24 The Take Charge booklet, which helps people reflect on their hopes and dreams, focus goals, and break them into tangible steps, may be key to helping these people succeed. While all participants reported a sense of taking charge, the specific mechanisms of the intervention, including the facilitated conversations and a guided process to exploring and articulating hopes and goals, may have strengthened people's sense of self-determination and self-efficacy and may explain why Take Charge participants appeared more confident in taking charge.
The Take Charge intervention, its intents and proposed mechanisms are illustrated in Figure 1. Our data suggest that the benefits of Take Charge occur when the person with stroke is outside the ‘tent’ of stroke care, which is often characterised by a focus on stroke-related impairments, progress toward discharge,25,26 and medical paternalism. 27 The therapeutic space is depicted in the Figure by the warmth and light of the open fire. This environment allows for free expression in a psychologically safe space and feeling truly heard. Take Charge provides the tools to enable autonomy, mastery, and connectedness, through listening, non-judgemental enquiry, and exploring personally meaningful goals. This can result in people feeling ‘the sky's the limit’ – the essence at the heart of the Take Charge intervention, depicted in the final panel of the Figure.

A summary illustration of how the Take Charge intervention enables the process of ‘taking charge’ for the individual (artwork by C. Kearns, Artibiotics).
Our study suggests areas for future development of the Take Charge. For example, earlier intervention might allow some people to ‘leave the tent’ earlier. However, this would likely require substantial change to current rehabilitation approaches as core elements of Take Charge may be in conflict with dominant practices in stroke rehabilitation. 28 Other possibilities include intervention provision via phone, video call or use of conversational agents (avatars). Further research is exploring these options and whether they maintain the sense of ‘being heard’ without human and/or face-to-face contact.
Several limitations need to be considered. Participants were selected from those available 12 months post-stroke, who were able and willing to share their experiences. Possibly these people had a more positive outlook, although many also shared negative experiences. We may have excluded less forthcoming participants who could have contributed valuable data. Recall bias is possible as not all participants in the main trial could recall Take Charge intervention visits. We mitigated this by selecting participants who spoke about the initial study visits at their 12-month outcome visit and encouraged the use of the study booklet as a prompt where available. Participants were all Caucasian (NZ European/Pākehā – a function of the inclusion criteria of the main study which had to exclude Māori and Pacific people who were the subject of a previous positive randomised trial 4 of Take Charge after stroke). Resource limitations restricted us to participants within greater Wellington region; the interviewer was also a Take Charge facilitator but not known to any of the participants. Our small sample size reflected limited time and resources, but our approach to sample specificity, high quality dialogue, and analysis of the data by experienced researchers and clinicians provided valuable insights. 29 Participants were younger and more likely to have been working than those in the parent study, limiting transferability to other contexts.
Overall, our findings support the idea that the Take Charge intervention empowers people with stroke, enhancing intrinsic motivation for people who already have a mindset that encourages ‘taking charge’ and encouraging ‘taking charge’ for people who wouldn’t otherwise have done so. For people to ‘come to their own wisdom’, the first necessary step is to provide a psychologically safe, listening environment that allows the person with stroke to feel they have ‘been heard’ and honoured as an individual.
Clinical messages
The Take Charge intervention is a systematic way of delivering person-centred care.
People who received Take Charge reported that it helped them feel heard and to focus on things that were uniquely important to them, which enabled them to ‘do things my way’.
Take Charge improves hope, confidence, and quality of life (taking charge and thriving, rather than surviving) which supports the quantitative TaCAS trial results.
Supplemental Material
sj-docx-1-cre-10.1177_02692155241310770 - Supplemental material for Coming to my own wisdom: A qualitative study exploring the role of the Take Charge intervention in stroke recovery
Supplemental material, sj-docx-1-cre-10.1177_02692155241310770 for Coming to my own wisdom: A qualitative study exploring the role of the Take Charge intervention in stroke recovery by Vivian Fu, Kathryn Mary Fernando, Felicity Bright, Judith Riley, Kathryn McPherson, Harry McNaughton and in Clinical Rehabilitation
Supplemental Material
sj-docx-2-cre-10.1177_02692155241310770 - Supplemental material for Coming to my own wisdom: A qualitative study exploring the role of the Take Charge intervention in stroke recovery
Supplemental material, sj-docx-2-cre-10.1177_02692155241310770 for Coming to my own wisdom: A qualitative study exploring the role of the Take Charge intervention in stroke recovery by Vivian Fu, Kathryn Mary Fernando, Felicity Bright, Judith Riley, Kathryn McPherson, Harry McNaughton and in Clinical Rehabilitation
Footnotes
Acknowledgements
The authors would like to thank the participants and their whānau for their manaaki.
This research was conducted by Tangata Tiriti in Aotearoa New Zealand. As clinician-researchers of health care systems, we recognise that we have the responsibility and power to create culturally safe and appropriate environments of care for all.
Author contributions
VF contributed to conceptualisation, funding acquisition, methodology, formal analysis, writing and validation. KMF contributed to conceptualisation, data collection and curation, methodology, formal analysis, writing and validation. FB contributed to validation and writing–review and editing. JR contributed to conceptualisation, data curation, formal analysis and writing–review and editing. KM contributed to validation and writing–review and editing. HM contributed to conceptualisation, funding acquisition, validation and writing–review and editing.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The main TaCAS trial was funded by the Health Research Council of New Zealand (grant number: 15/297).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
