Abstract
Objective
This study aimed to evaluate the effectiveness of transcranial direct current stimulation associated with brain–computer interface in stroke patients.
Data sources
The PubMed, Central, PEDro, Web of Science, SCOPUS, PsycINFO Ovid, CINAHL EBSCO, EMBASE, and ScienceDirect databases were searched from inception to April 2023 for randomized controlled studies reporting the effects of active transcranial direct current stimulation associated with brain–computer interface to a transcranial direct current stimulation sham associated with brain–computer interface condition on the outcome measure (motor performance and functional independence).
Review methods
We searched for full-text articles which had investigated the effect of transcranial direct current stimulation associated with brain–computer interface on motor performance in the upper extremities in stroke patients. The standardized mean differences derived from the change in scores between pretreatment and post-treatment were adopted as the effect size measure, with a 95% confidence interval. Possible sources of heterogeneity were analyzed by performing subgroup analyses in order to examine the moderating effects for one variable: the level of injury severity.
Results
Nine studies were included in the qualitative synthesis and the meta-analysis. The findings of the conducted analyses indicated there is not enough evidence to suggest that active transcranial direct current stimulation associated with brain–computer interface is more efficient in motor performance and functional independence when compared to sham transcranial direct current stimulation associated with brain–computer interface or brain–computer interface alone. In addition, the quality of evidence was rated very low. A subgroup analysis was performed for the motor performance outcome considering the injury severity level.
Conclusion
We found evidence that transcranial direct current stimulation associated with brain–computer interface was not more beneficial than sham transcranial direct current stimulation associated with brain–computer interface or brain–computer interface alone.
Keywords
Introduction
Stroke is a leading cause of disability and mortality in the United States and other industrialized countries. 1 Motor impairments after a stroke can lead to activity limitations. These impairments interact to affect the function and can lead to a decreased quality of life. 2 Current rehabilitation approaches have focused on impairment reduction, recovery of functional skills, and quality of life improvement. 3
Conventional rehabilitation has been shown to have limited effectiveness on performance in activities of daily living, function, muscle strength, and cognitive abilities. In this scenario, transcranial direct current stimulation can modulate cortical excitability and improve the performance of activities of daily life. 4
Patients showed improvements when combined with other therapies in stroke treatment, and transcranial direct current stimulation enhanced the effects of the adjuvant therapy. 5 One technique that can be associated with transcranial direct current stimulation is robotic therapy, which is a type of brain–computer interface. Brain–computer interfaces acquire brain signals and translate them into commands that are relayed to output devices that carry out desired actions. 6 The main goal of brain–computer interface is to promote the recruitment of brain areas involved and to facilitate neural plasticity, beyond replacing or restoring function in neuromuscular disorders, such as stroke. 7
A preliminary study supports the feasibility of using transcranial direct current stimulation in conjunction with other approaches, such as robotic orthosis to facilitate gait recovery in subjects post-stroke. 8 In this context, using transcranial direct current stimulation and brain–computer interface can promote promising clinical results due to the potential to induce brain plasticity. Therefore, greater knowledge about the association of these resources is necessary. However, an investigation into the clinical efficacy of post-stroke motor rehabilitation based on transcranial direct current stimulation and brain–computer interface has not been explored through a meta-analysis. To fill this gap and consolidate existing knowledge, this systematic review with meta-analysis aimed to evaluate the effectiveness of transcranial direct current stimulation associated with brain–computer interface in stroke patients, with motor performance in the upper extremities as the primary outcome and the functional independence level as a secondary outcome, emphasizing the injury severity level in the subgroup analysis.
Methods
A systematic review and meta-analysis were performed according to the recommendations of the Cochrane group and this report follows PRISMA guidelines. The systematic review protocol was registered on the International prospective register of systematic reviews (CRD42022306959). The search was carried out in the PubMed, Central (Cochrane Library), PEDro (Physiotherapy Evidence Database), Web of Science, SCOPUS, PsycINFO Ovid, CINAHL EBSCO (Cumulative Index to Nursing and Allied Health Literature), EMBASE and ScienceDirect databases in April 2023.
The search terms were adapted to each database. Articles obtained by concatenating terms were stroke and transcranial direct current stimulation and brain–computer interfaces. In addition, further searches were performed in the reference list of literature reviews, and we also searched ongoing trials and research registers (http://clinicaltrials.gov) and google scholar (http://scholar.google.com/).
We conducted a comprehensive search for full-text articles, without imposing any language restrictions or limitations on the publication year. The included articles needed to meet the following criteria: investigated the effect of transcranial direct current stimulation associated with brain–computer interfaces in motor performance in the upper extremities in stroke patients; any type of active transcranial direct current stimulation (anodic, cathodic, or bihemispheric) associated with brain–computer interface versus sham transcranial direct current stimulation associated with brain–computer interface or only brain–computer interface; randomized controlled trials; parallel or crossover studies; adult patients; and stimulation over the primary motor cortex. In the context of this study, a stroke is defined as the manifestation of rapidly developing clinical signs of focal or overall disturbance in cerebral function, lasting more than 24 h, with no apparent cause other than of vascular origin. Furthermore, studies were excluded if they: included animals; included patients with other neurological or musculoskeletal disorders; or other types of noninvasive brain stimulation.
Two reviewers independently screened the title and abstract of each paper, considering eligibility criteria in Rayyan Systems Inc. Discrepancies were resolved by consensus, and if necessary, a third reviewer was included to make the decision. After the screening, full texts were evaluated. We extracted data regarding sample size, mean age, time post-stroke, level of severity, type of stroke, study design, stimulation parameters (electrode location, current intensity, duration, and the number of sessions), type of brain–computer interface and outcomes measures for each included article. Data were entered in Review Manager 5.4. The authors were contacted by e-mail in cases of studies with incomplete information or data.
The risk of bias for each individual study was assessed following the criteria proposed by Cochrane guidelines. This tool assesses the risk of bias based on the following domains: random sequence generation, allocation concealment, blinding of participants and personnel, blinding of outcome assessment, incomplete outcome data, and other biases. Each of these items was deemed as “low risk,” “high risk,” or “unclear risk.”
All analyses were performed using the Review Manager 5.4 program. Analyses were stratified by the outcome and individual studies were combined into a meta-analysis. The standardized mean differences (SMDs) derived from the change in scores between pretreatment and post-treatment between the active transcranial direct current stimulation with brain–computer interface and sham transcranial direct current stimulation with brain–computer interface groups were adopted as the effect size measure, with a 95% confidence interval (95% CI).
Heterogeneity was assessed using I2 (I2> 50% is considered substantial heterogeneity). Possible sources of heterogeneity were analyzed by performing subgroup analyses to examine the moderating effects for one variable: level of injury severity. The p-value <0.05 was considered in the statistical analyses.
Results
A total of 666 articles were screened and 14 full texts were assessed for eligibility. After reading these full-text articles, nine met the inclusion criteria (see Figure 1). A comprehensive summary of the characteristics of the included studies examining the effects of transcranial direct current stimulation associated with brain–computer interface on motor performance in the upper extremity can be found in Table 1. One study had patients in the subacute phase of stroke, 9 seven studies in the chronic phase,10–16 and one study in the subacute and chronic phase. 17 Regarding the type of stroke, one study included patients after ischemic stroke, 9 seven studies included patients with ischemic and hemorrhagic stroke,10–12,14–17 and one study did not specify this information. 13
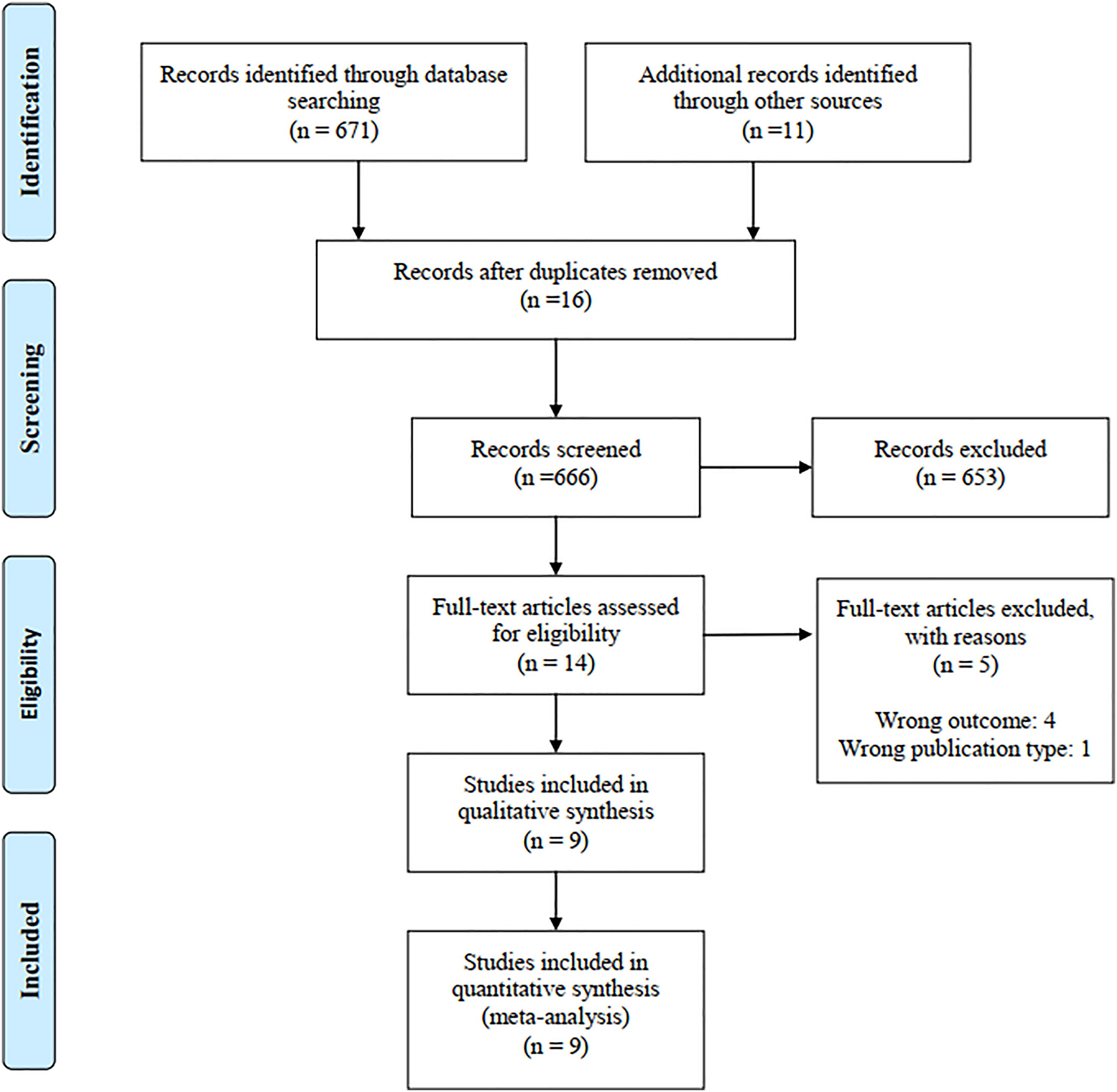
PRISMA flowchart of systematic review search process and meta-analysis.
Characteristics of included studies.
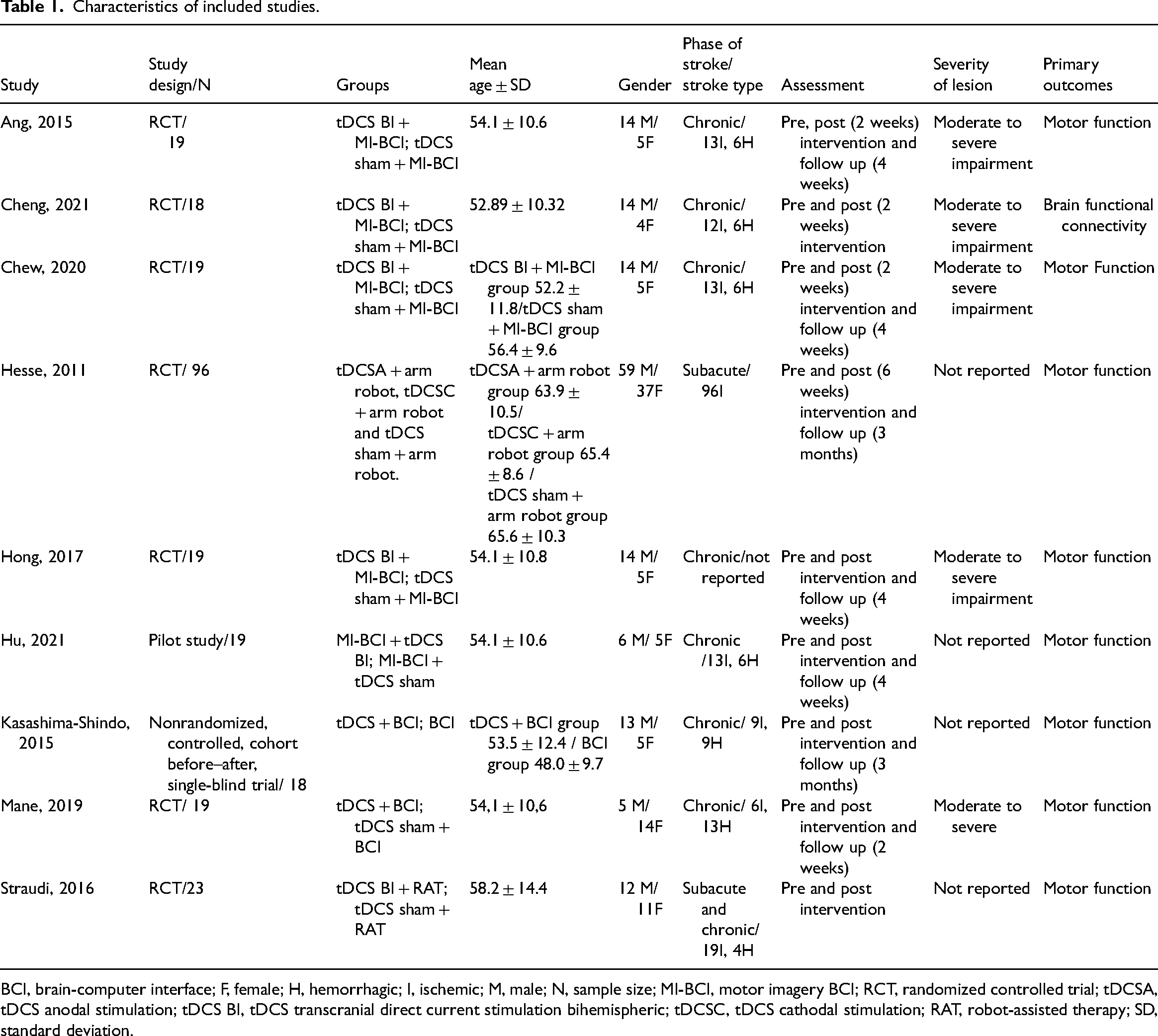
BCI, brain-computer interface; F, female; H, hemorrhagic; I, ischemic; M, male; N, sample size; MI-BCI, motor imagery BCI; RCT, randomized controlled trial; tDCSA, tDCS anodal stimulation; tDCS BI, tDCS transcranial direct current stimulation bihemispheric; tDCSC, tDCS cathodal stimulation; RAT, robot-assisted therapy; SD, standard deviation.
Six studies performed only bihemispheric transcranial direct current stimulation,10–15,17 one study applied both anodal and cathodal stimulation, 9 and one study only performed transcranial direct current stimulation anodally. 16 The current intensity applied in most studies was 1 mA,10–17 and the duration ranged from 10 to 30 minutes.
Regarding treatment duration, one study had a protocol with 30 sessions in 6 weeks of intervention. 9 However, most studies10–17 had a protocol with 10 sessions for 2 consecutive weeks. Concerning adverse effects, only one study 17 reported mild side effects after stimulation in 43% of patients. The effects related were: skin redness under the stimulation site, headache, sleepiness, and neck pain. Table 2 presents more information regarding the characteristics of treatment and the occurrence of adverse effects.
Characteristics of treatment and occurrence of adverse effects.
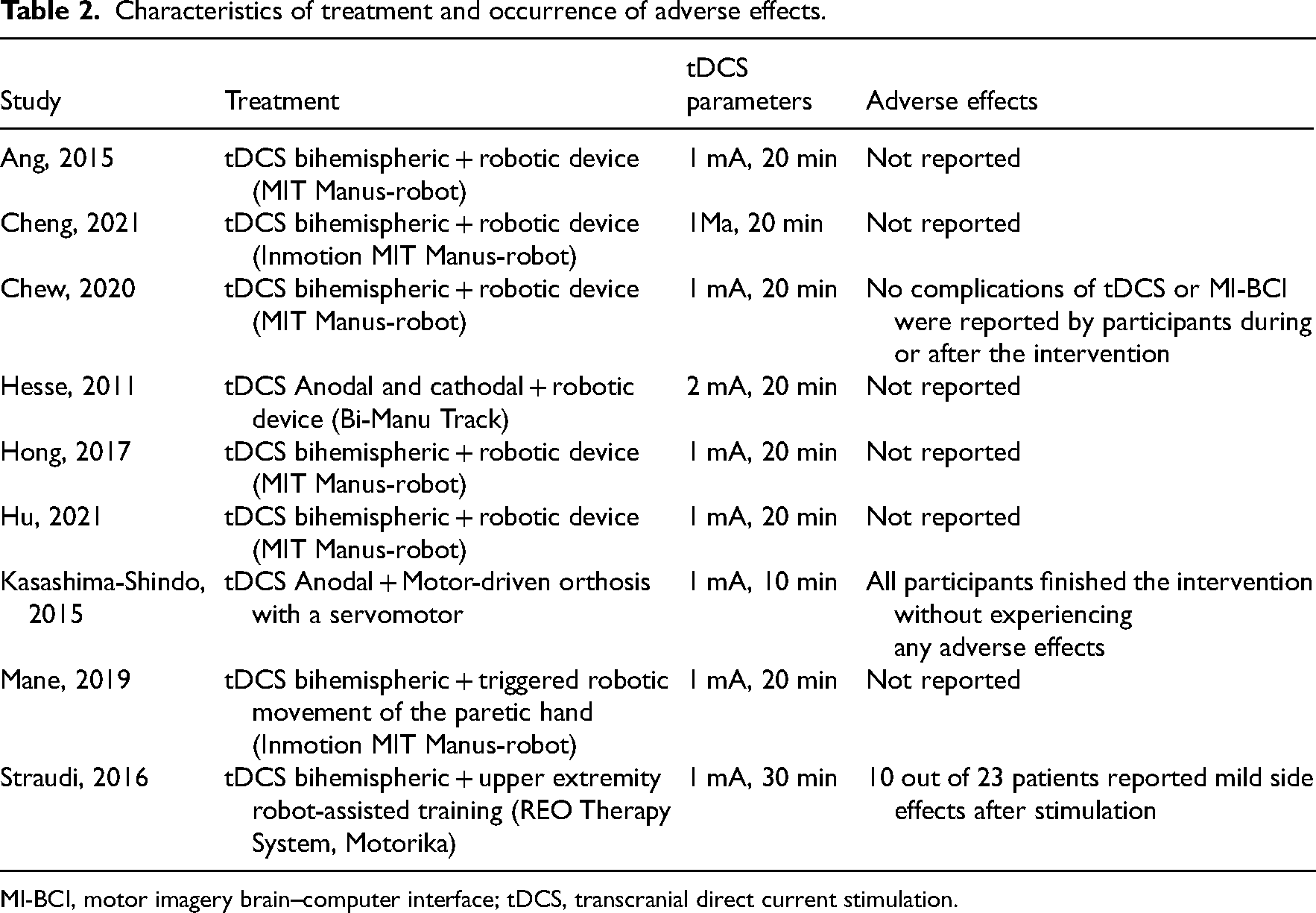
MI-BCI, motor imagery brain–computer interface; tDCS, transcranial direct current stimulation.
Regarding outcome measurements, seven studies performed the follow-up evaluation, two of them 2 weeks after the protocol was completed,11,15 three 4 weeks after the intervention protocol was completed,12–14 and two after 3 months.9,16 In addition, five studies performed the injury severity level measurement, which was verified using the Fugl-Meyer Motor Assessment. The patients in all of these studies had a moderate to severe injury level.10–13,15
All of the included studies used noninvasive interfaces for the brain–computer interface technology, specifically robotic equipment. Moreover, seven of the nine studies initially applied the transcranial direct current stimulation protocol followed by the brain–computer interface protocol,10–16 while two studies performed the application simultaneously.9,17
Included studies were of varying methodological quality. Trial populations were generally small (median sample size = 29, range 18–85), with many trials underpowered to demonstrate a difference between groups if one was present. In addition, two of the nine (22%) studies had adequate allocation concealment, six of the nine (67%) trials had a blinded outcome assessor, and one of the nine (%) trials described intention to treat analysis. The risk-of-bias graphs and summary are presented in Figure 2.
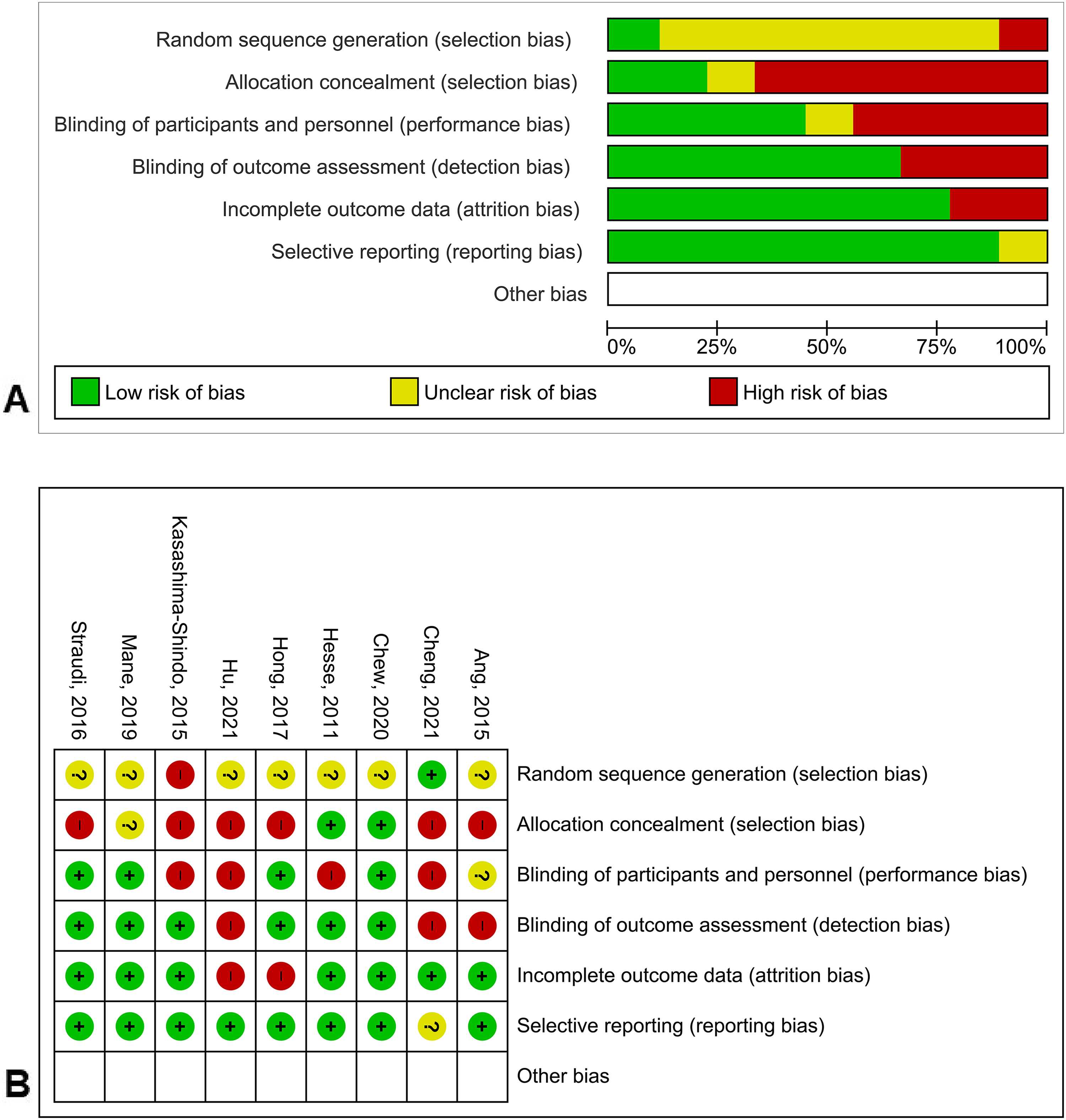
Risk-of-bias graph (A): review authors' judgments about each risk of bias item presented as percentages across all included studies; risk-of-bias summary (B): review authors' judgments about each risk of bias item for each included study.
All nine studies included in the quantitative analyzes evaluated the effect of transcranial direct current stimulation associated with brain–computer interface on upper limb motor performance using the Fugl-Meyer Motor Assessment. There was no significant effect of the transcranial direct current stimulation associated with the brain–computer interface favorable for the experimental group (SMD = 0.07 and 95% CI −0.16–0.31, I2=0%) (Figures 3 and 4).
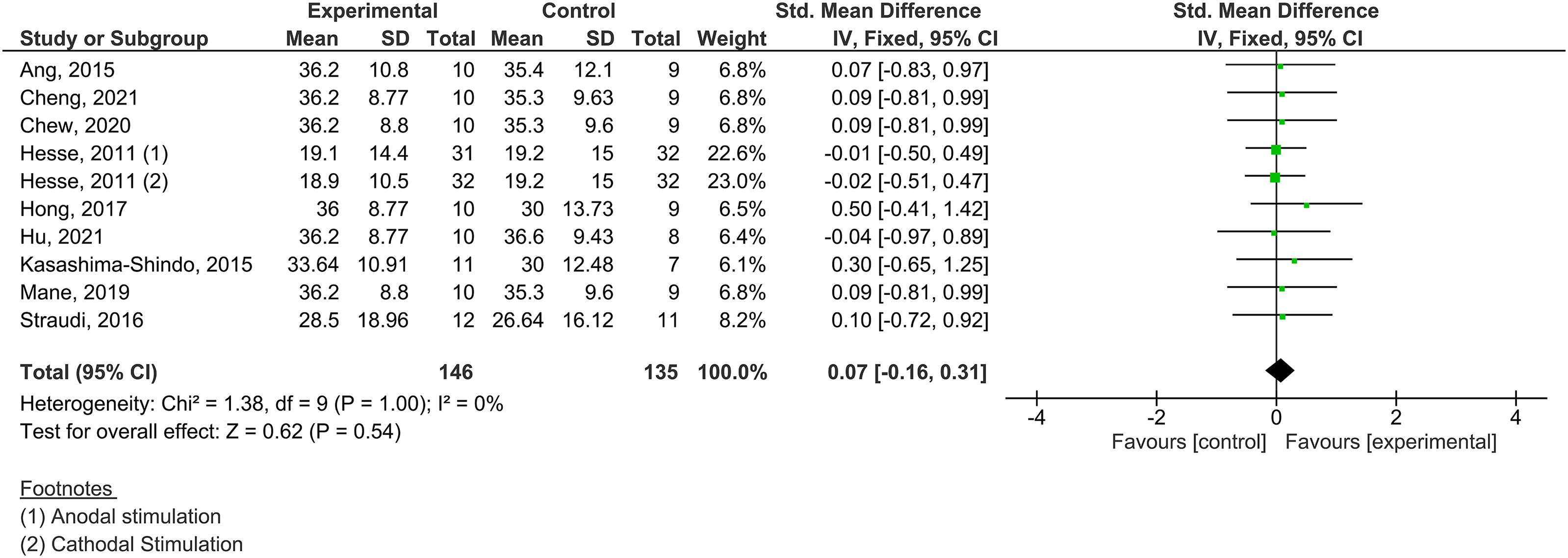
Meta-analysis for motor performance.
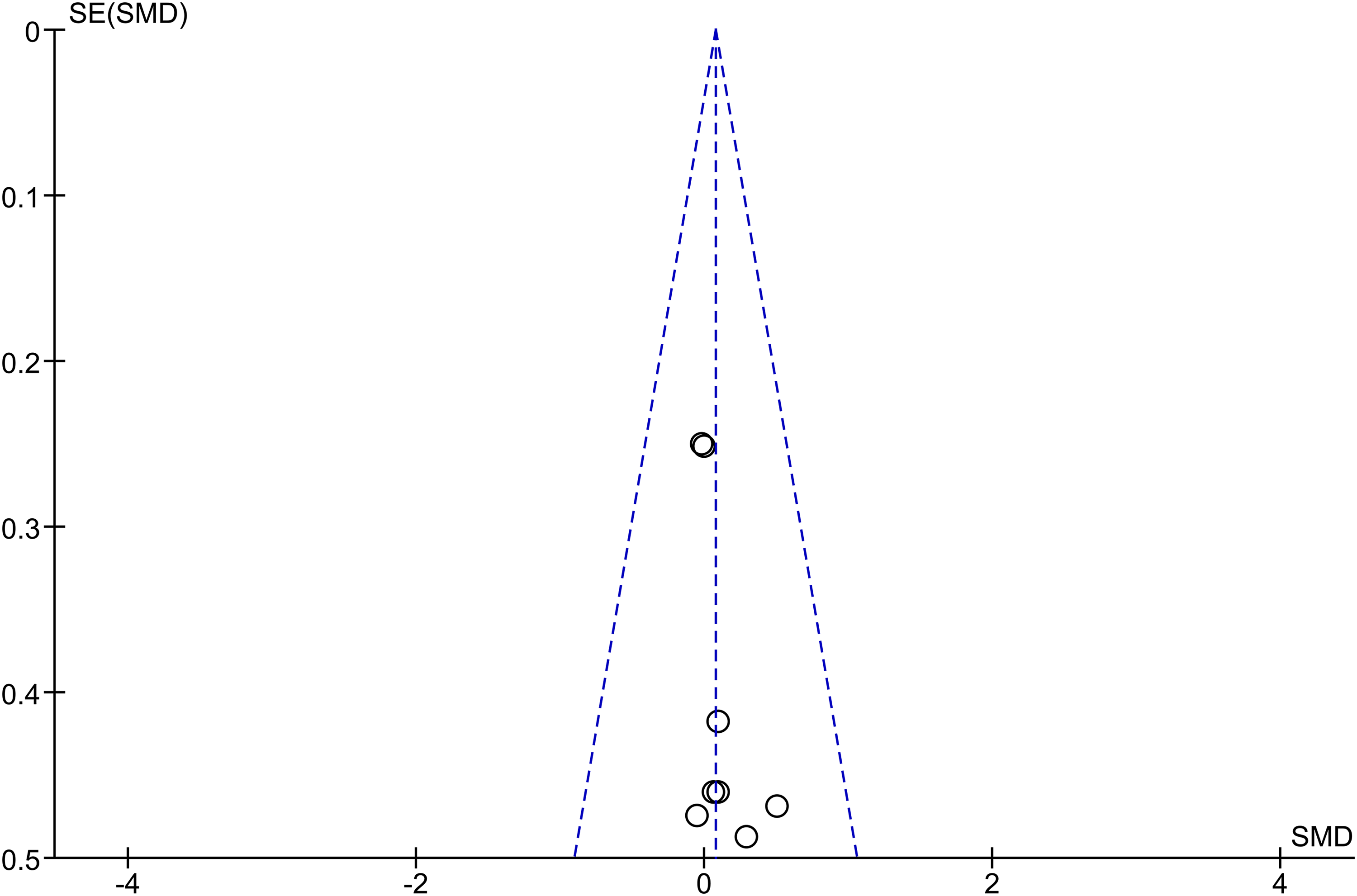
Funnel plot of the meta-analysis for motor performance.
Risk of bias assessments were integrated into the sensitivity analysis, in which a secondary data analysis only included studies considered to have “low risk” or “unclear risk” in the domains referring to random sequence generation, allocation concealment, and blinding of outcome assessment. Figure 5 shows that there was no significant difference in favor of the intervention on motor performance (SMD = 0.01; 95% CI −0.30–0.32, I2=0%).
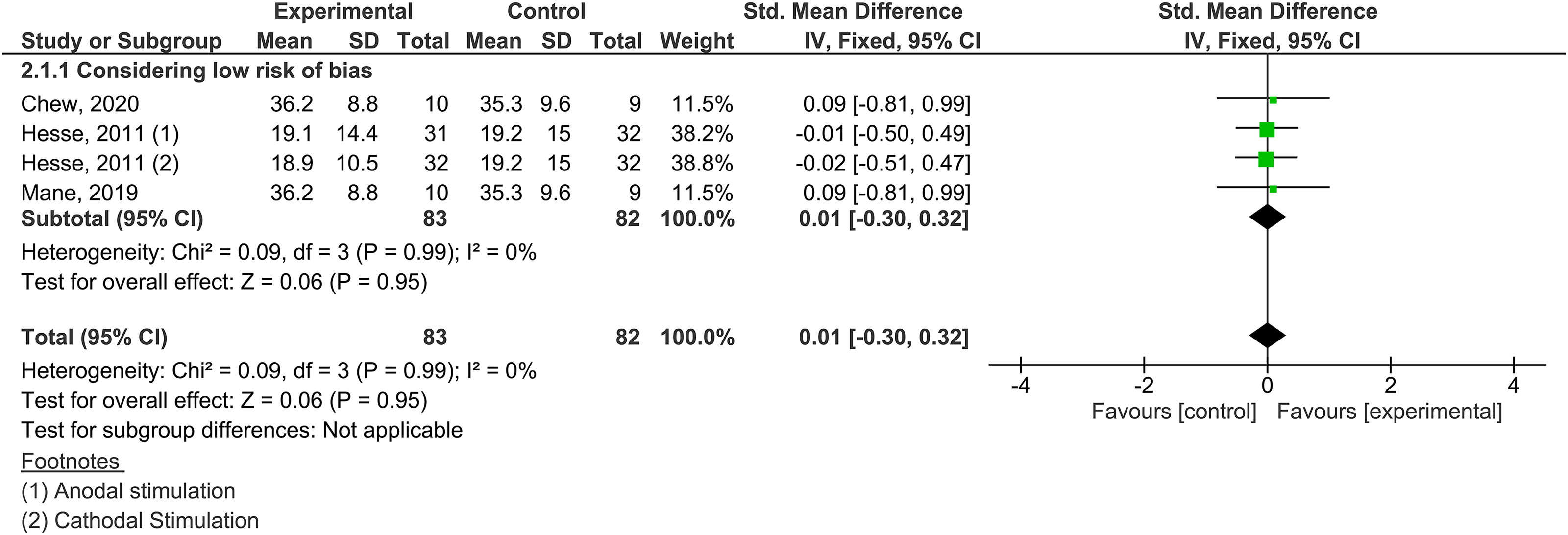
Outcome motor performance—sensitivity analysis.
Only the study by Hesse 9 measured functional independence using the Barthel index. The result of this meta-analysis showed that there was no significant difference favorable to the group that performed the intervention (transcranial direct current stimulation associated brain–computer interface) in relation to the functional independence outcome (SMD = 0.29; 95% CI −4.74–5.31; I2=16%) (Figure 6).
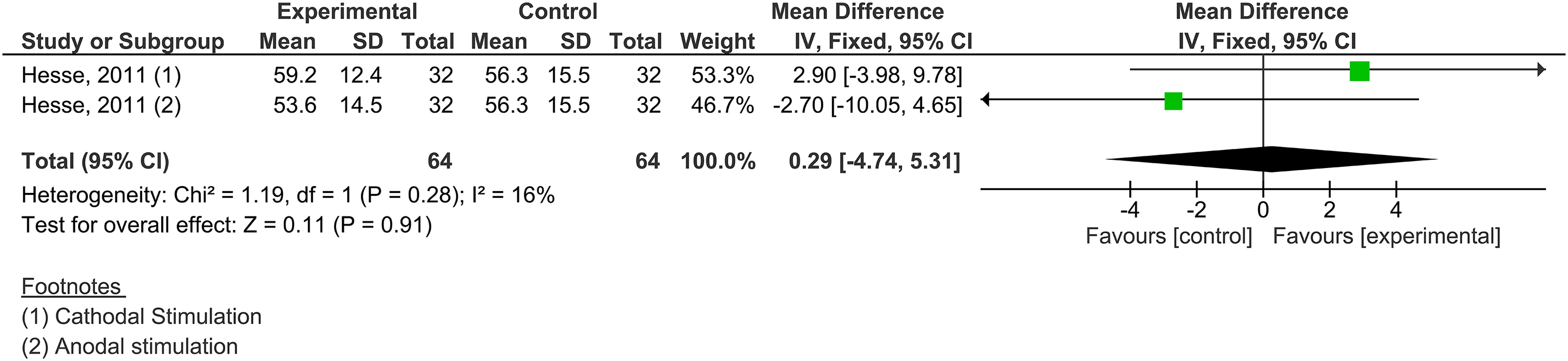
Meta-analysis for functional independence.
A subgroup analysis was conducted for the motor performance outcome considering the injury severity level (moderate to severe). The studies by Chew 12 and Mane 15 were inserted in this analysis. The meta-analysis revealed there was no significant favorable difference in the intervention group regarding the effect of transcranial direct current stimulation associated with brain–computer interface (SMD = 0.09; 95% CI −0.54–0.73; I2=0%).
We used the five “Grading of Recommendations, Assessment, Developing and Evaluation” (risk of bias, imprecision, inconsistency, indirectness, and publication bias) considerations to assess the quality of a body of evidence as it relates to the studies which contribute data to the meta-analyses. Thus, we found a low-quality evidence rating for the motor performance and functional independence outcome (see Figure 7).
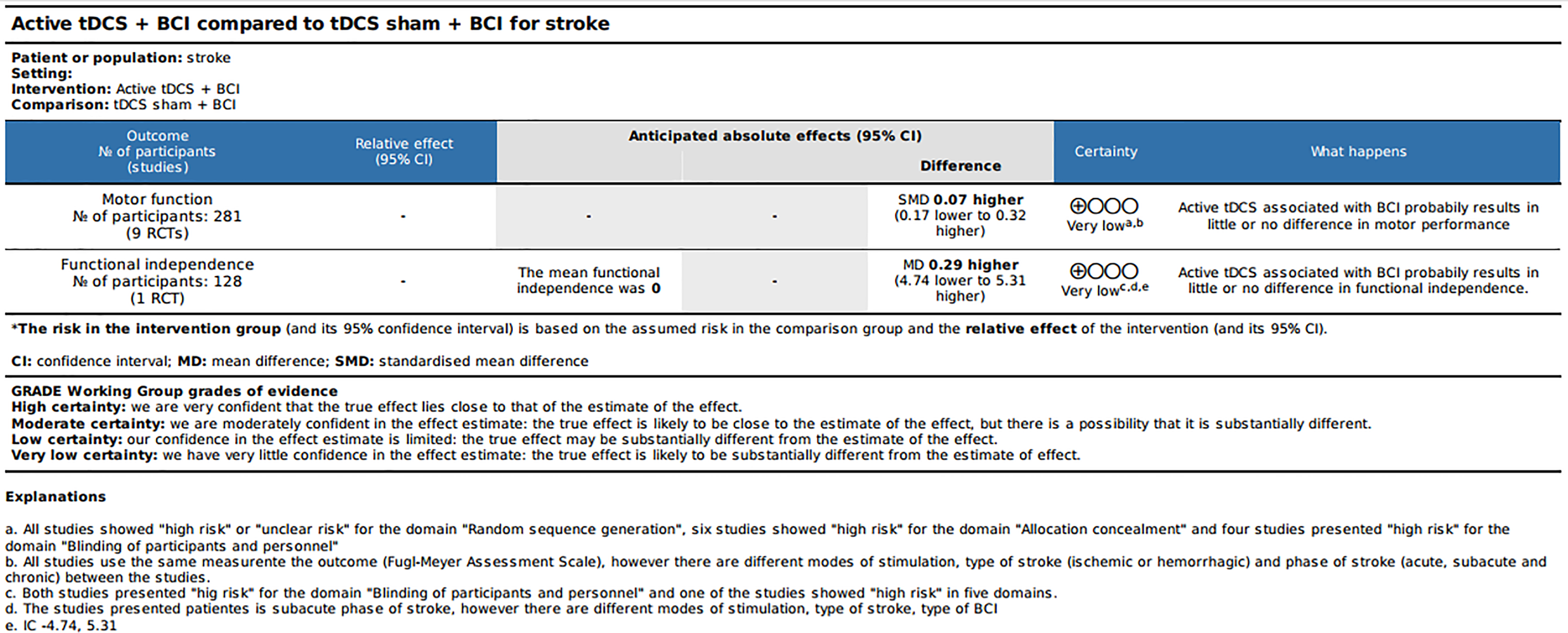
Summary of findings—quality of evidence by GRADE.
Discussion
This review focused on evaluating the effectiveness of transcranial direct current stimulation associated with a brain–computer interface for improving upper motor function and functional independence in people after stroke. We included 9 trials with a total of 262 participants. However, low-quality evidence suggests that there is no effect of transcranial direct current stimulation associated with a brain–computer interface in stroke recovery. In addition, there was no significant effect regarding the functional independence outcome in favor of transcranial direct current stimulation associated with the brain–computer interface and the quality of the evidence was considered very low. A small number of clinical trials investigated the effectiveness of the association of transcranial direct current stimulation and brain–computer interface in treating patients after stroke.
Furthermore, it is important to highlight that most of the studies presented great variations regarding the type and phase of the stroke and intervention protocols, which may influence the interpretation of the results. Moreover, there is racial bias in the patients included in this study, as most studies were exclusively conducted with Asians. The quality of the evidence for each outcome was limited due to small numbers of study participants and poor reporting of study details.
A review by the Cochrane group identified that transcranial direct current stimulation might improve activities of daily living after stroke, however the evidence had a low quality rating. Furthermore, evidence of low quality suggests that there is no effect of transcranial direct current stimulation on arm and leg function, muscle strength, or cognitive abilities. 4
Although another meta-analysis 18 suggests that the effects of transcranial direct current stimulation may be potentiated when associated with other therapies or interventions, in the present study it was not possible to verify its positive effect on motor function and functional disability when associated with a brain–computer interface. A number of studies have already shown that the responses to protocols involving noninvasive brain stimulation are variable, with a substantial number of subjects considered nonresponders. 19 Physiological, technical, and statistical factors may be responsible for intrasubject and intersubject variability. 20 These factors may impact the nonsignificant results of some studies involving transcranial direct current stimulation.
It is known that there are two ways in which the use of brain–computer interface technology in patients after stroke can contribute to rehabilitation. The first is the possibility of replacing the loss of neuromuscular functions by using brain signals to interact with the environment, such as controlling an external device. The second alternative would be the use of brain–computer interface for stroke rehabilitation in order to restore impaired motor function, inducing brain plasticity. 21
A recent meta-analysis showed that there are a substantial number of clinical studies that demonstrate the possibility of functional recovery associated with the use of a brain–computer interface. Significant immediate effects on paretic upper limb function were observed, however there are no data to support their long-term effects. In addition, the analysis suggests that its combined use with transcranial direct current stimulation, using a summary of the results of two studies, would not be able to potentiate the functional recovery of the upper limbs. However, the author states that the use of a brain–computer interface combined with functional electrical stimulation can produce positive effects. 22
Many of the trials included in this review were of poor methodological quality, with few concealing allocation or analyzing results using intention to treat principles, but there are many ongoing randomized trials on this topic which could change the quality of evidence in the future. Furthermore, high-quality trials which are more reflective of the current clinical practice using standardized methods of delivery and focus on the reduction of possible biases (such as type and phase of stroke) need to be conducted before we can draw conclusions regarding the benefits and optimal use of combined interventions in stroke treatment.
Clinical message
There is no evidence of the effect transcranial direct current stimulation associated with brain-computer interface in post-stroke recovery.
Transcranial direct current stimulation is of no additional benefit over brain–computer interface alone.
Future trials should address key methodological criteria such as allocation concealment and appropriate statistical reporting.
Footnotes
Author Contributions
EOL, LMS, ALVM, and JVTD conceived the study and designed experiments. EOL and MAA performed the data analysis. EOL, JMRSN, SMA, and EAO interpreted the data and drafted the manuscript. All authors critically revised and approved the final version of the manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
