Abstract
Objective
To synthesize the evidence of the effectiveness of self-management interventions during the peri-hospitalization period.
Data sources
Three databases (i.e. PubMed, Web of Science, and Scopus) were systematically searched.
Review methods
Full-text randomized controlled studies that assessed the effects of self-management interventions initiated during the peri-hospitalization period in patients with stroke were included. Two independent reviewers performed data extraction. A third reviewer was available for discrepancies. The methodological quality was evaluated using version 2 of the Cochrane risk-of-bias tool for randomized trials (RoB-2). Data were pooled and a meta-analysis was performed.
Results
Eight studies comprising 1030 participants were included. The self-management interventions showed considerable heterogeneity in their protocols, although most of them included an individualized plan based on the patient's needs. The meta-analysis was performed with data from the self-efficacy domains. The pooled results showed a trend towards the self-management intervention on quality of life (1.07, 95% confidence interval [CI] 0.52 to 1.63; P = 0.0002) but neither in dependence (0.80, 95% CI −0.14 to 1.74; P = 0.10) nor in self-efficacy (0.77, 95% CI −0.44 to 1.98; P = 0.21).
Conclusion
Most of the studies reviewed suggest that self-management interventions had an impact on dependency, quality of life and self-efficacy when compared with usual care, written materials about stroke, or post-discharge rehabilitation recommended by a physician. However, the evidence in this review neither supports nor refutes self-management interventions used in addition to usual care, or other interventions, to improve dependency, quality of life and/or self-efficacy in patients’ post-stroke.
Introduction
Stroke is the second largest cause of disability worldwide with 14 million new strokes each year and a clear trend toward increasing stroke incidence and prevalence rates.1,2 Stroke acute care, long-term sequelae, and the corresponding costs are expected to increase, with a burden on stroke survivors’ quality of life and health systems.1,3
Stroke usually leads to functional impairments, and spontaneous recovery is limited, being a leading source of disability in patients. 4 Specifically, only 65% of stroke patients return to full functional independence and more than 26% of stroke survivors are dependent on basic activities of daily living. 5 Additionally, the psychosocial disabilities arise independent of the degree of physical disabilities, these problems use to become chronic, and they hinder 52% of patients permanently. 6
Different authors have suggested a relationship between early impairments after stroke and long-term disability, highlighting the importance of proposing therapeutic interventions during the early acute stroke.7,8 In this line, the recognized window of enhanced neuroplasticity early after stroke has been the main argument for developing early rehabilitation, 9 but with some controversial results when applied in the first 2 weeks. 10
The relevance of early and chronic disability of stroke survivors, with special emphasis in familiar and social repercussions,11,12 has led to numerous self-management oriented proposals. These interventions are based on facilitating behavior change or teaching compliance with specific treatment recommendations and focused on encouraging people with chronic diseases to take an active part in the management of their own condition. Different reviews have been developed on stroke survivors demonstrating that self-management interventions can improve the management of the chronic illness and optimize the perceived health and well-being.13–16
While different reviews have been performed about efficacy of self-management interventions on stroke, no one has analyzed the effectiveness of early developed programs. The theory of illness suggests that the risks in the critical 30-day period after discharge might derive as much, or more, from the allostatic stress that patients experience in the hospital as they do from the lingering effects of the acute illness that precipitated the hospitalization. 17 In this line, the therapeutic opportunity of programs developed during this time frame can lead to different levels of effectiveness.
Thus, this systematic review and meta-analysis aims to synthesize the evidence of the effectiveness of self-management interventions during the peri-hospitalization period.
Methods
This systematic review and meta-analysis were conducted following the preferred reporting items for systematic reviews and meta-analyses guidelines (PRISMA) to search, extract, and evaluate the interventions. 18 The review was previously registered at the International Prospective Register of Systematic Review (PROSPERO) with registration number CRD42021292143.
An extensive electronic search was conducted using the following databases: PubMed, Web of Science, and Scopus. This review began in November 2021 and included all articles that existed in the database until that date, with the final search complete in May 2023. A search strategy in MEDLINE was developed using the following steps: (1) a thorough examination of the MeSH Database, (2) development of keywords by examining relevant key terms used in existing systematic reviews, and (3) expert guidance and review by a specialist. This search strategy was tested and refined to claim it was the most effective strategy for this systematic review. Then, this strategy was adapted to the other screened databases. Additionally, the references of relevant reviews were also screened for additional studies that may be potentially included in this review.
To define the research question, the PICOS (P: population; I: intervention; C: comparison; O: outcomes; and S: study design) model was applied. Studies were included based on the following criteria: (1) participants of the selected studies had to be patients with stroke over 18 years old; (2) the experimental group received an intervention focused efficacy of self-management behaviors, according to the definition of Chodosh et cols, 19 alone or combined with other interventions and initiated during the peri-hospitalization period (from admission to first 2 week post-discharge); (3) the comparator received a control intervention or no treatment; (4) the main outcome measures included dependency and/or quality of life variables; secondary outcomes included self-efficacy and impact on caregiver domains; and (5) randomized clinical trials were included.
The exclusion criteria were: (1) studies that included a mixed population of chronic diseases; (2) articles not published in English, French, Italian or Spanish languages; and (3) no full-text access.
After the records were obtained from the different databases, duplicates were removed.
When the articles were selected, the data extraction was performed by two independent researchers. A data extraction table was created, summarizing the most relevant information. The following data were extracted for each study: first author, year of publication, study design and number of groups, sample (number of participants, age, and gender), interventions, primary and secondary outcomes measures, and findings. It also included the taxonomy of everyday self-management strategies (TEDDS), which is made up for five goal-oriented domains (internal, social interaction, activities, health behavior and disease controlling), and two additional support-oriented domains (process and resource), thus creating a unified framework for understanding how people with neurological diseases self-manage all aspects of daily life. 20
The studies included were assessed independently by two reviewers. They performed the evaluations of the titles and abstracts of all obtained manuscripts and further reviewed the studies to ensure eligibility concerning inclusion and exclusion criteria. Of the selected articles, full texts were reviewed to verify that they met the inclusion criteria. All disagreements or differences between the two reviewers were resolved by a third reviewer.
The methodological quality of the included studies was assessed using version 2 of the Cochrane risk-of-bias tool (RoB-2). 21 This tool consists of five domains focusing on the randomization process, deviations from the intended interventions, missing outcome data, measurement of the outcome, and the selection of the reported result. The studies were interpreted as having a high, low, or unclear risk of bias. Two reviewers independently assessed the risk of bias in the included studies and any disagreement was resolved after discussion with a third reviewer.
Data analysis
Where appropriate, study results with respect to the quality of life, dependency, and self-efficacy were pooled and a meta-analysis was undertaken using Review Manager software (Rev-Man version 5.1, updated March 2011) and the Cochrane Collaboration guidelines for reviewing interventions. 22
Post-intervention means and standard deviations were used for conducting the meta-analysis. In cases where data were insufficient for the purpose of meta-analyses (e.g. lack of means or standard deviations), we made efforts to contact the authors of the trials. When standard deviations were unavailable, but P-values or 95% confidence intervals were provided, they were computed using the embedded Review Manager calculator. If different intervention arms were compared within a trial, they were included separately in the meta-analysis dataset.
For continuous outcomes, weighted mean differences were employed when all studies assessed outcomes using the same measurement scale. In cases where different scales were used to measure the same underlying symptom or condition across studies, standardized mean differences were used and 50% confidence intervals were calculated for all outcomes.
The overall mean effect sizes were estimated using either random effect models or fixed effect models based on the results of statistical heterogeneity tests (I2). A meta-analysis with an I2 value greater than 50% was considered heterogeneous, and a random-effects model was employed. Forest plots were visually inspected to identify any outlier studies. Possible sources of heterogeneity were explored, and sensitivity analyses were conducted by excluding trials at high risk of detection or attrition bias.
The data provided for caregiver assessments were not sufficient to perform a meta-analysis. A forest plot was generated to illustrate the overall effect of interventions on quality of life, dependency and self-efficacy.
Results
The PRISMA flow diagram of the search, the screening, and the study process is shown in Figure 1. A total of 7581 records were identified from the search in the electronic databases. After removing duplicates, 7029 titles were screened, of which eight articles were included in the systematic review.23–30 Finally, five studies were included in the quantitative analysis.24,27–30
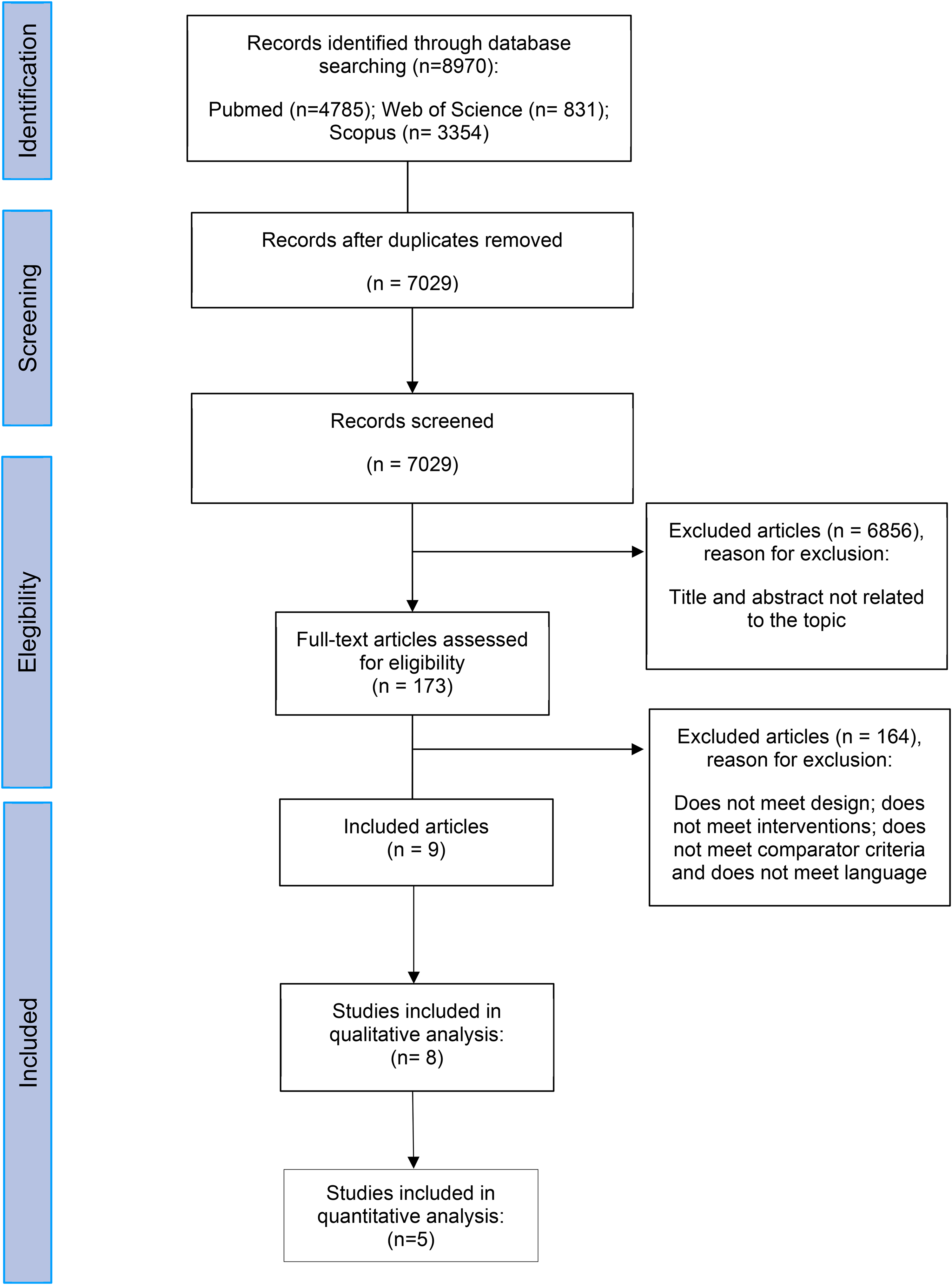
Flow diagram.
Table 1 summarizes the participants’ characteristics (n = 1030), and study details of the studies included such as the sample size, design, country, or the number of groups. All the articles had two groups,23–28,30 except the manuscript of Baykal et al. 29 which had four groups. The participants were aged between 55 and 69 in the self-management group and 58 and 72 in the control group.14–22
Characteristics of the included studies.
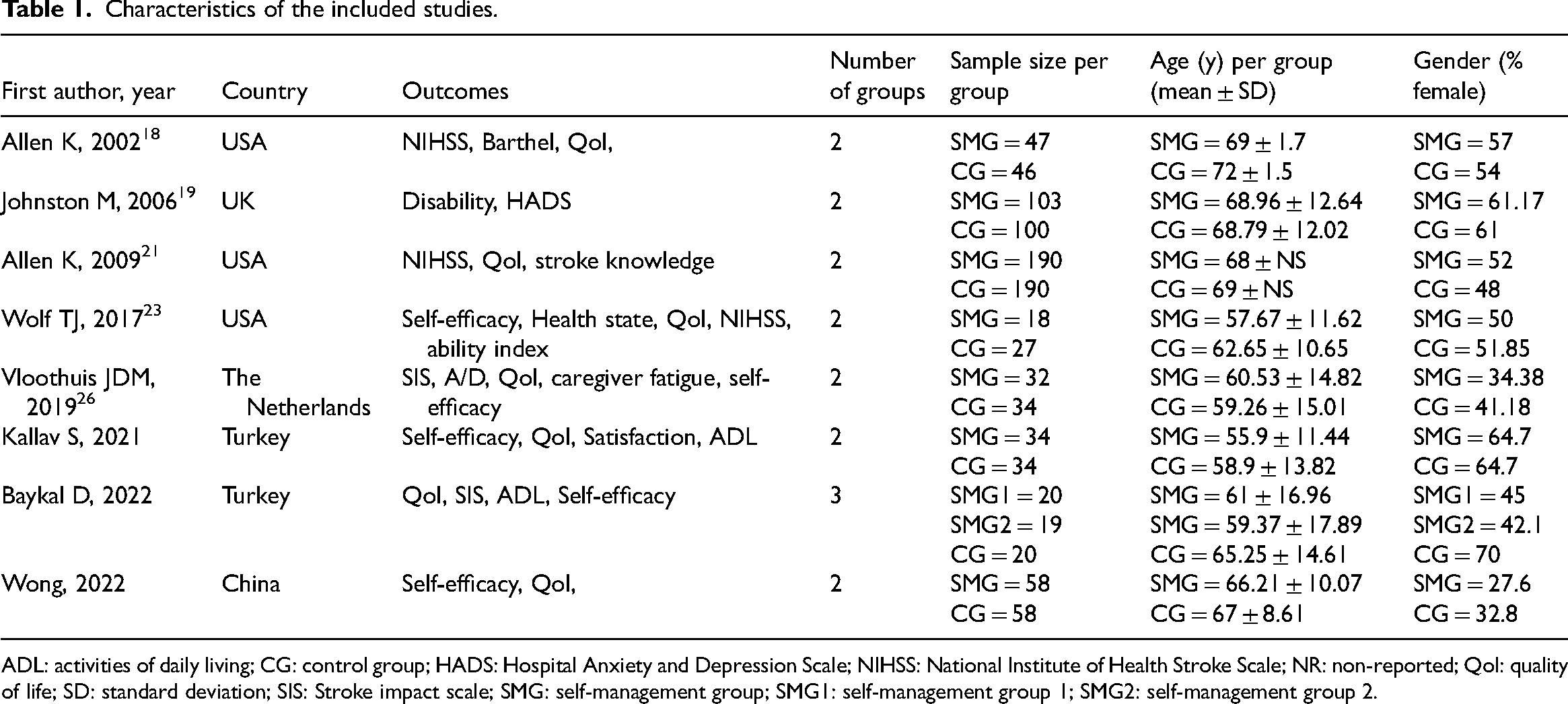
ADL: activities of daily living; CG: control group; HADS: Hospital Anxiety and Depression Scale; NIHSS: National Institute of Health Stroke Scale; NR: non-reported; Qol: quality of life; SD: standard deviation; SIS: Stroke impact scale; SMG: self-management group; SMG1: self-management group 1; SMG2: self-management group 2.
Table 2 shows the main characteristics of the interventions proposed, the main and secondary outcomes for this review, and the main results obtained after the interventions. The protocol used in the studies was heterogeneous. Most studies assessed whether the effects of the interventions persisted over time.26,27,30 The follow-up period ranged from 3 27 to 12 months. 26
Characteristics of the interventions, outcomes and findings.
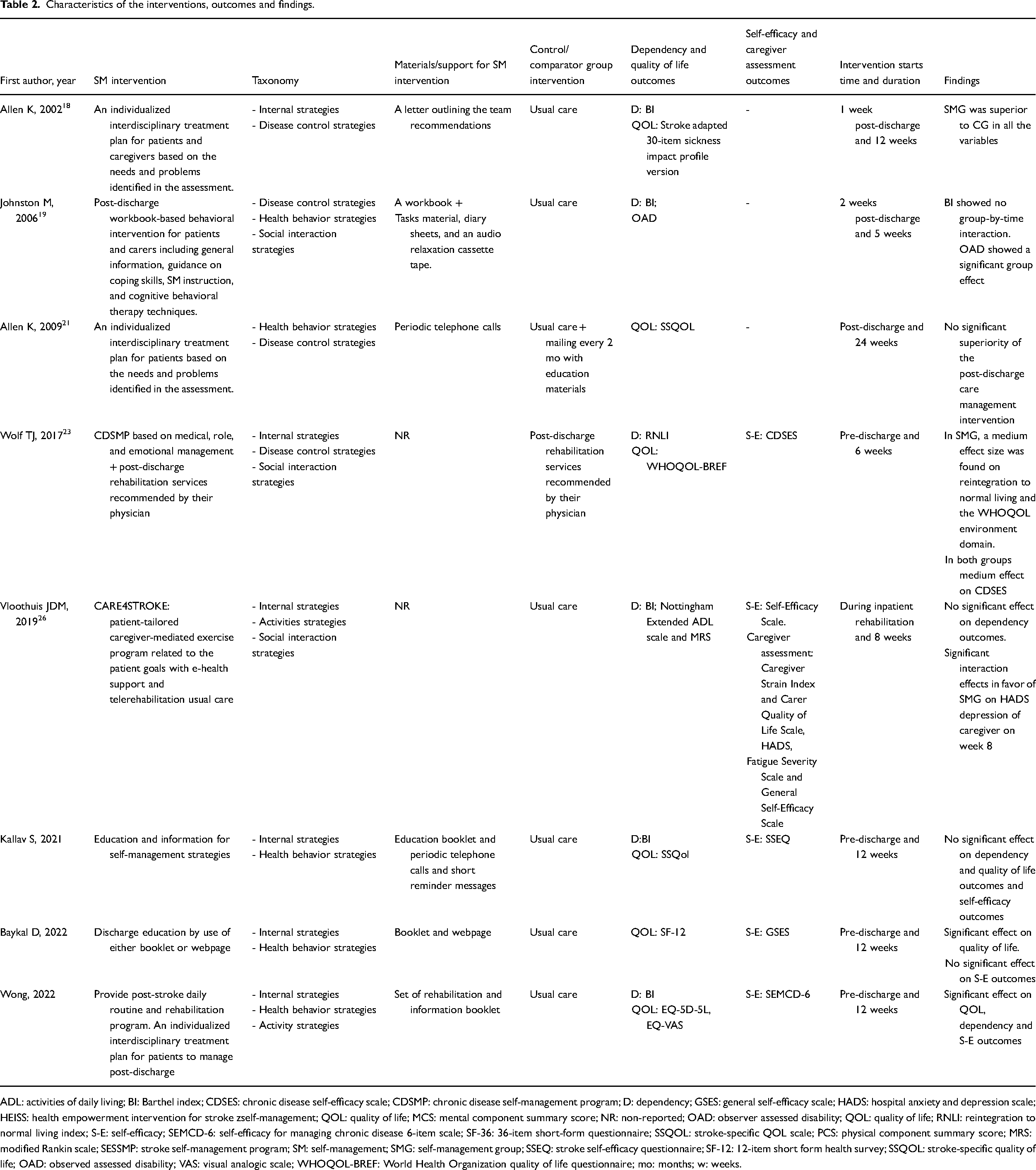
ADL: activities of daily living; BI: Barthel index; CDSES: chronic disease self-efficacy scale; CDSMP: chronic disease self-management program; D: dependency; GSES: general self-efficacy scale; HADS: hospital anxiety and depression scale; HEISS: health empowerment intervention for stroke zself-management; QOL: quality of life; MCS: mental component summary score; NR: non-reported; OAD: observer assessed disability; QOL: quality of life; RNLI: reintegration to normal living index; S-E: self-efficacy; SEMCD-6: self-efficacy for managing chronic disease 6-item scale; SF-36: 36-item short-form questionnaire; SSQOL: stroke-specific QOL scale; PCS: physical component summary score; MRS: modified Rankin scale; SESSMP: stroke self-management program; SM: self-management; SMG: self-management group; SSEQ: stroke self-efficacy questionnaire; SF-12: 12-item short form health survey; SSQOL: stroke-specific quality of life; OAD: observed assessed disability; VAS: visual analogic scale; WHOQOL-BREF: World Health Organization quality of life questionnaire; mo: months; w: weeks.
All studies received a self-management intervention. In two studies, the caregivers were part of the intervention.23,27 The characteristics of interventions and the protocol used in the studies were heterogeneous. However, all of the studies included, the treatment plan was based on the specific goals and needs of the patients.23–30 In most of the studies, internal strategies (managing emotions, proactive orientation, etc.),23,26–30 disease control (using medication, participation in rehabilitation, etc.),23–26 health behavior strategies (adopting healthy behaviors, exercising, etc.)24,25,28–30 and social interaction strategies (self-advocacy, social participation, etc.)24,26,27 were considered according to the TEDDS. 20 The comparator group included usual care,23,24,27–30 mailing with education materials about stroke, 25 or post-discharge rehabilitation recommended by the physician. 26 Dependency, quality of life, self-efficacy, and the impact on caregiver outcomes included a variety of validated assessment tools. Six of the eight articles in this review included dependency as one of the domains evaluated in their programs being the Barthel index the most reported outcome for this domain.23,24,26,28,30 The findings show that dependency significantly improved in three of the studies after the self-management interventions.23,26,30 Although the pooled analysis showed no significant differences when self-management alone or in combination with other interventions was compared with control interventions (SMD 0.80, 95% confidence interval [CI] −0.14 to 1.74), there is a trend that favors self-management interventions.24,27,28,30 Heterogeneity was high (I2 = 95%) and the overall effect of the intervention was not significant (Z = 1.66, P = 0.10) (Figure 2).
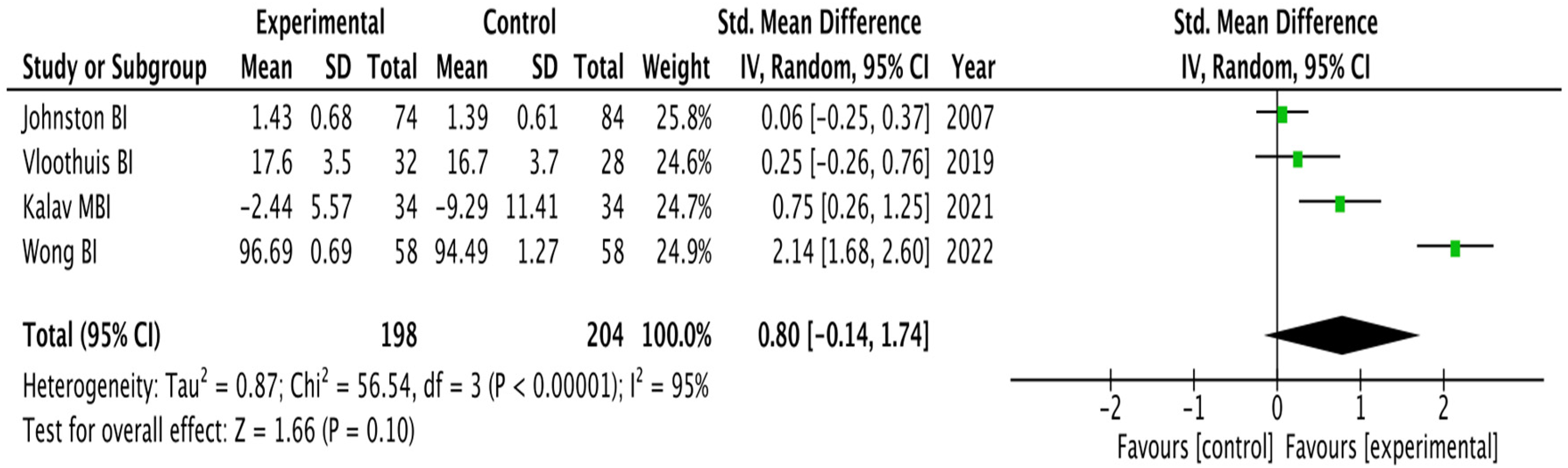
Effect of self-management interventions in patients with stroke for dependency. BI: Barthel index; CI: confidence interval; MBI: Modified Barthel Index; SD: standard deviation.
Six of the studies included measures about quality of life such as the Stroke adapted 30-item sickness impact profile version, 23 stroke-specific quality of life scale,25,28 World Health Organization quality of life questionnaire, 26 physical component summary score, and mental component summary score of the 36-item short-form questionnaire, 29 and the EQ-5D-5L with EQ.VAS. 30 The pooled analysis showed significant improvements in favor of self-management interventions when compared to the control interventions (SMD 1.07, 95% CI 0.52–1.63), heterogeneity was high (I2 = 80%) the overall effect of the intervention was not significant (Z = 3.78, P = 0.0002) (Figure 3)
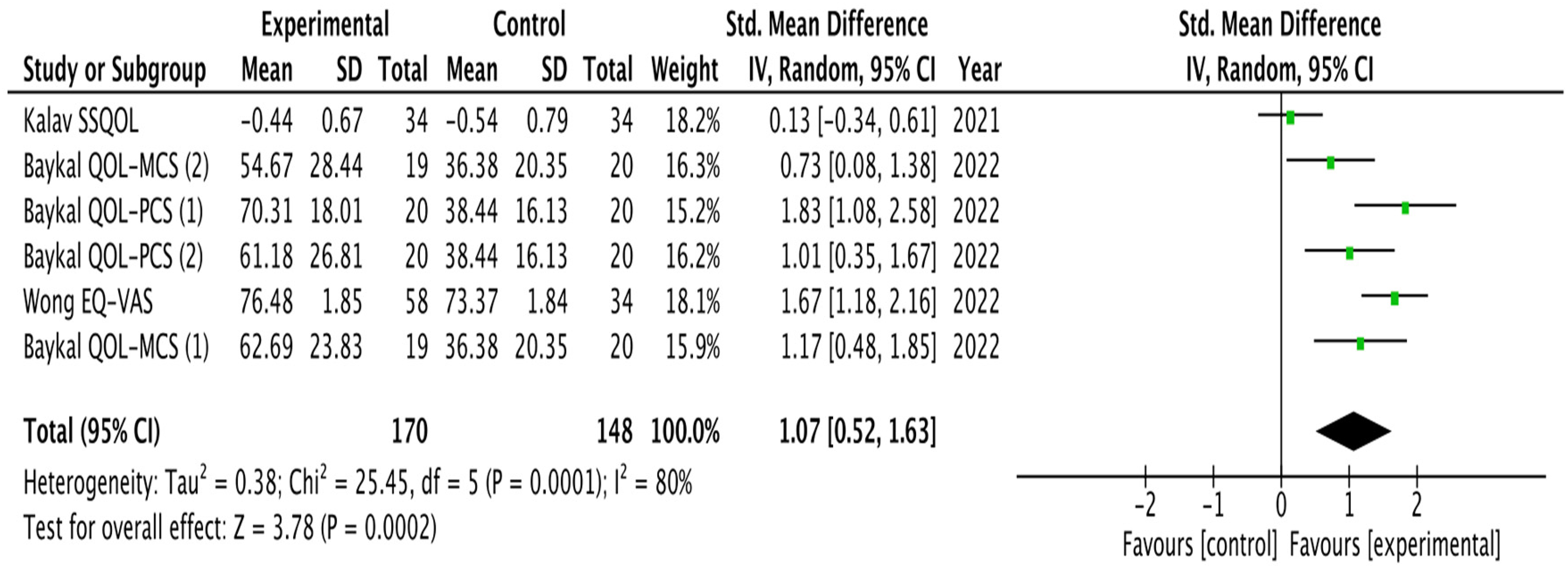
Effect of self-management interventions in patients with stroke for quality of life. CI: confidence interval; QOL: quality of life; MCS: mental component summary score; PCS: physical component summary score; SD: standard deviation; SSQOL: stroke-specific QOL scale; self-management group 1; 2: self-management group 2.
Five studies in this review included self-efficacy outcome measures,26–30 of which two studies reported significant improvement in self-efficacy variables in comparison with the comparator group.26,30 Four studies provide appropriate data to be included in a meta-analysis.27–30 The pooled analysis showed no significant differences when self-management alone or in combination with other interventions was compared with control interventions (SMD 0.77, 95% CI −0.44 to 1.98). Heterogeneity was high (I2 = 96%) and the overall effect of the intervention was not significant (Z = 1.25, P = 0.21) (Figure 4).16,21,22
Only one study evaluated the impact of self-management on the caregiver, including variables such as the carer strain index and the carer quality of life scale, hospital anxiety and depression scale, fatigue severity scale, and the general self-efficacy scale. 27 The study of Vloothuis et al. showed a positive impact on the caregiver profile. 27 However, meta-analysis was not possible due to the heterogeneity of outcomes and the lack of a sufficient number of studies (Figure 4).
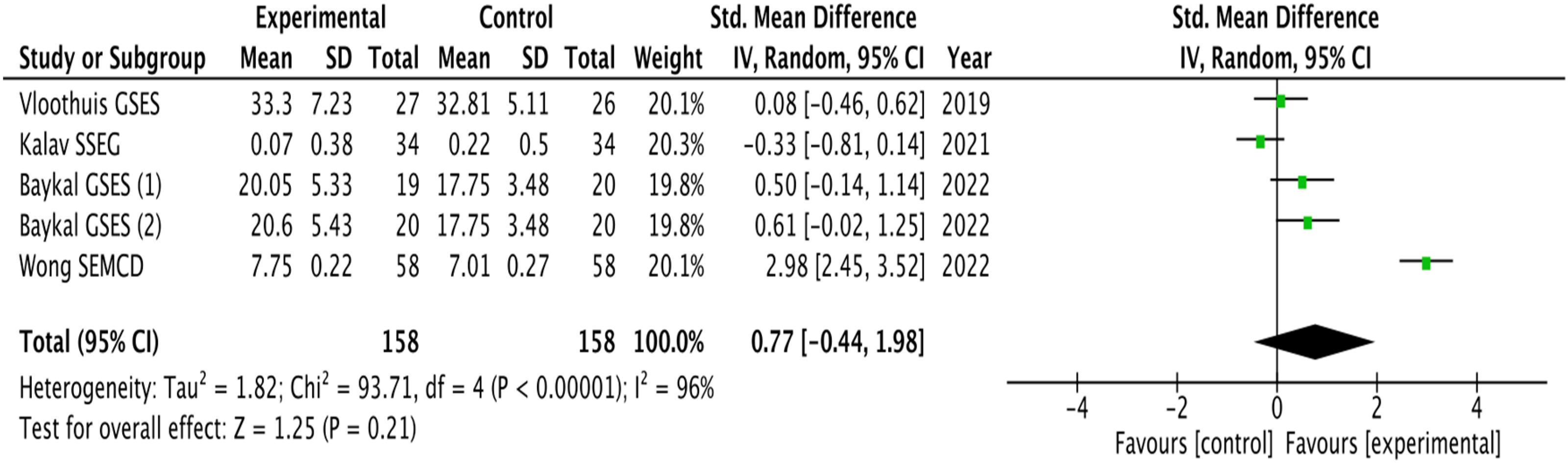
Effect of self-management interventions in patients with stroke for self-efficacy. CI: confidence interval; GSES: global self-efficacy scale; SD: standard deviation; SEMCD: self-efficacy for managing chronic disease; SSEQ: stroke self-efficacy questionnaire.
The methodological quality shows a low risk for four of the eight studies included,24,26–28 some concerns for one of them 25 and high risk in three of them (Supplementary material).23,29,30 The most frequent domains showing a high risk of bias were the randomization process,23,29,30 some concerns in the domains of measurement of the outcome.23,30 All studies show a low risk of bias in the deviations from the intended interventions, missing outcome data and selection of the reported result.23–30
Discussion
The purpose of this systematic review was to assess the effects of self-management interventions initiated during the peri-hospitalization period for patients with stroke. The results clarified the main characteristics and effects of self-management interventions on dependency and quality of life. Most of the studies developed an interdisciplinary individualized approach based on individual needs. The meta-analysis focused on dependency and self-efficacy showed that although there is a trend that favors self-management interventions, they were not superior to usual care, written materials about stroke, or post-discharge rehabilitation recommended by the physician. In relation to quality of life variables, self-management interventions were shown to be superior to usual care and statistically significant improvements were observed in favor of the experimental group.
The cost related to management of patients after a stroke is high considering the hospital and post-discharge care. 31 Nursiswati et al. 32 showed that it is important to consider the degree of care dependency at discharge to plan a rehabilitation program. Additionally, their findings highlight that care dependency items should be prioritized when designing and applying discharge planning. Six of the nine articles in this review included dependency as one of the domains evaluated in their programs.23,24,26–28,30 The findings show that dependency significantly improved in three of the studies after the self-management interventions.23,26,30 However, although there is a positive trend towards the efficacy of self-management interventions, the pooled results neither supports nor refutes self-management interventions used in addition to usual care, or other interventions, to improve dependency.
Results of this study support the importance of internal, disease control and social interaction strategies in the development of self-management programs. Lorig and Holman proposed that interventions to promote self-management should incorporate education to increase the patient's knowledge of their disease, their understanding of the health care system and supports available to them, and training to acquire problem-solving and decision-making skills. 33 In all of the studies included, the treatment plan was based on the specific goals and needs of the patients.23–30 In this sense, self-management interventions in patients after a stroke should consider the changing needs that differ depending on everyone's life situation and condition.20,34
The presence of disability was shown to be an independent determinant of poor health-related quality of life, being important to be assessed in patients after a stroke. Kirschner previously stated that biases in clinical decision-making affecting persons with disability include ineffectual bias, that is, the tendency to underestimate the competence and quality of life of persons with disability. 35 Quality of life was included as an outcome measure in six studies which showed benefits associated with the self-management program.23,24,26,28–30 Quality of life and activities of daily living are associated with self-efficacy. 13 Two studies reported significant improvement in self-efficacy variables in comparison with usual care or post-discharge rehabilitation services recommended by the physician.26,30 Although some benefits have been reported, the pooled results neither supports nor refutes self-management interventions used in addition to usual care, or other interventions, to improve self-efficacy. Previous studies have reported that self-management for patients with chronic conditions may improve clinical outcomes and self-efficacy.13,36 Korpershoek reported that the performance of activities of daily living in patients with stroke is related to higher levels of self-efficacy. 37
Some previously published reviews and meta-analyses also suggest benefits to be gained from programs that target self-management based on self-efficacy principles; however, the results related to time frame, specifically in peri-hospitalization in stroke survivors have not been explored. This review evaluates the feasibility and efficacy of self-management programs designed specifically during peri-hospitalization for stroke populations. That permits us to answer timing-related questions post-stroke in detail. In this line, there are still questions regarding involvement of caregivers, a more detailed description of components, format and professionals involved.13–16,34
The conclusions of this review have been drawn from a limited number of heterogeneous studies. Several of the studies included present a high risk of bias, including randomization process and inadequate blinding. In addition, heterogeneity regarding the interventions and procedure was present, often with minimal detail in descriptions of the programs and timing. Future studies are needed including well-designed randomized controlled trials. These studies should be well-powered and include validated measures and blinding procedures.
Most of the studies reviewed suggest that self-management interventions have a significant improvement on quality of life and may have an impact on dependency when compared with usual care, written materials about stroke, or post-discharge rehabilitation recommended by a physician. However, more research is needed to identify the optimal frequency, duration, and components of self-management interventions for maximizing improvements in dependency and quality of life.
We would have liked to have been able to perform a quantitative analysis of the impact of self-management on the caregiver, but we did not obtain sufficient data. Likewise, it would have been of great interest to see if the effects of these self-management interventions were sustained over time, so it would be necessary for future studies to analyze the long-term effects of these interventions.
Self-management intervention during the peri-hospitalization period after a stroke may have an impact on dependency and quality of life. The most reported interventions involved an interdisciplinary individualized approach based on individual needs. More research is needed in the development of self-management intervention early after stroke.
Supplemental Material
sj-docx-1-cre-10.1177_02692155231193563 - Supplemental material for Effectiveness of self-management interventions during the peri-hospitalization period in patients with stroke: A systematic review and meta-analysis
Supplemental material, sj-docx-1-cre-10.1177_02692155231193563 for Effectiveness of self-management interventions during the peri-hospitalization period in patients with stroke: A systematic review and meta-analysis by Esther Prados-Román, Irene Cabrera-Martos, Javier Martín-Nuñez, Geraldine Valenza-Peña, María Granados-Santiago and Marie Carmen Valenza in Clinical Rehabilitation
Supplemental Material
sj-docx-2-cre-10.1177_02692155231193563 - Supplemental material for Effectiveness of self-management interventions during the peri-hospitalization period in patients with stroke: A systematic review and meta-analysis
Supplemental material, sj-docx-2-cre-10.1177_02692155231193563 for Effectiveness of self-management interventions during the peri-hospitalization period in patients with stroke: A systematic review and meta-analysis by Esther Prados-Román, Irene Cabrera-Martos, Javier Martín-Nuñez, Geraldine Valenza-Peña, María Granados-Santiago and Marie Carmen Valenza in Clinical Rehabilitation
Footnotes
Author contribution
ICM, MCV: Conceptualization, Supervision, Writing; EPR, MCV: Reviewing and editing; JMN: Software, Formal analysis; EPR: Manuscripts selection and analysis; EPR, MGS: Writing first version of the manuscript.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
