Abstract
Objective
To explore the short- and long-term effects of lower-limb endurance training on chronic obstructive pulmonary disease outpatients.
Design
Prospective quasi-experimental study.
Setting
1383-bed teaching hospital in Taiwan.
Participants
Overall, 69 outpatients diagnosed with chronic obstructive pulmonary disease were enrolled. A total of 60 patients completed the study.
Intervention
Training group: Lower-limb endurance training; control group: Education only.
Main measures
The modified medical research council score, chronic obstructive pulmonary disease assessment test score, pulmonary function test, and number of acute exacerbation within a year.
Results
The training group showed significant improvement in the chronic obstructive pulmonary disease assessment test total score, modified medical research council score (both P < 0.001) at third month sustaining to 12th month (P < 0.001) and presented less events of acute exacerbation (P = 0.011) at 12th month. The chronic obstructive pulmonary disease assessment test decreased by 8 points sustaining to 12th month. The training group presented significant post-training functional capacity improvements in 6-min walking distance, lowest oxygen saturation during 6-min walking test, peak workload, maximum inspiratory/ expiratory pressures, and calf circumference.
Conclusions
The lower-limb endurance training improved perceived dyspnea in daily activity and health status after completion of training and sustaining for a year. The lower-limb endurance training alleviated disease impacted on reduced acute exacerbations.
Keywords
Introduction
Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory disease causing airway obstruction. Patients with COPD may suffer from loss of ability and worse quality of life due to symptoms. Repeated hospitalization for acute exacerbation would lead to further deconditioning, causing physical and financial burdens on the families and society. COPD has become the third leading cause of death around the world, 1 and the seventh in Taiwan. 2 As COPD progresses, breathlessness resulting in lower activity levels can further impact the health-related quality of life (HRQoL). 3 According to the global initiative for chronic obstructive lung disease guideline, COPD patients can be classified into three groups and those patients classified B and E are encouraged to enroll in a pulmonary rehabilitation program, 4 including exercise training, breathing control, patient education, and self-management. Pulmonary rehabilitation is strongly recommended as one of the most effective methods and is routinely executed for COPD patients to restore physical conditions. Previous meta-analysis indicated that pulmonary rehabilitation programs including lower limb endurance training are important for patients with stable COPD to improve dyspnea, HRQoL, and exercise capacity. 5
Dyspnea as the most common reason for a patient visit has been associated with the limitation of exercise performance. 6 The lower limb endurance training has demonstrated improvements in cardiopulmonary fitness by increasing exercise capacity, and thus attenuating dyspnea sensation. 7 The COPD assessment test (CAT), modified medical research council (mMRC), and the 6-min walking distance are positively correlated with patient's HRQoL. The CAT is one of the main predictors of the HRQoL for COPD patients as well as a strong indicator on the response to pulmonary rehabilitation.8,9 Recently, clinicians have broadened treatment goals for COPD beyond improving lung function and symptoms by addressing the importance of preventing and reducing acute exacerbations. 10 However, the correlations between the improvements on CAT and 6-min walking distance on acute exacerbation has not been well explored.
This study aims to explore the short- and long-term effects of lower limb endurance training for COPD outpatients using mMRC, CAT, and acute exacerbation as main outcomes.
Methods
This prospective quasi-experimental study was conducted in a 1383-bed teaching hospital in Taiwan and approved by the Ethics committee of Chang Gung Medical Foundation (approval number: 102-4163B). Informed consent was obtained from all participants.
According to a study by Dodd et al., 9 the critical sample size was calculated with the mean CAT score > 20 and then being reduced to 18 after completion of the exercise training program. The sample size was estimated by the G-power software. To reach 80% power required to detect significance at the 5% level, the estimated sample size was 30 participants, with an expected dropout rate of 20% and an allocation ratio of 1:1 for the minimum difference in the change of CAT score between the two groups.
COPD patients were referred to the lower limb endurance training program from the pulmonary outpatient clinics at Chiayi Chang Gung Memorial hospital between November 2014 and November 2016. Patients were diagnosed with COPD according to the criteria of the global Initiative for chronic obstructive lung disease report, post-bronchodilator forced expiratory volume in 1 s (FEV1)/forced vital capacity (FVC) ratio < 70%. 11 The inclusive criteria were COPD patients classified as groups B, C, and D. The exclusion criteria were patients with comorbidities such as instable cardiovascular disease, neurological or musculoskeletal conditions, which were likely to adversely affect performance during assessments or exercise training. Participants who were willing to participate in the exercise training program twice a week for 3 months, were assigned to the training group¸ receiving education and exercise, whereas participants who could attend outpatient clinic regularly for drugs and education, were assigned to the control group only receiving education about the disease and self- management.
The exercise training program consisted of education and lower limb endurance training. The education of the program included the pathophysiology of the disease, accurate medication usage, breath control, energy conservation strategies, bronchial hygiene, nutrition, and management for acute exacerbation.
The participants received 24 exercise sessions, each session for 40 min, 2 sessions per week for 3 months. The exercise training program was designed according to the recommendation from the American College of Sports Medicine. 12 A paddling ergometer (Ergoline200, Ergoline GmbH, Germany) was used as lower-limb endurance training modalities. The target training intensity was 60%–80% of the age-predicted maximal heart rate or at the level of symptom limitation based on a modified Borg scale score rating of 4–6. The procedures were as follows: Warm-up exercise (0 watts) for 5 min, then incrementally increasing watts within 5–10 min till reaching 60%–80% of maximum heart rate for at least 20 min, then ending with cool-down exercise (10 W) for 5 min. In order to maintain a prescribed exercise dose, twenty-four patients were supplemented with oxygen via nasal cannula, titrated to maintain pulse oxygen saturation (SpO2) > 90% throughout the exercise training. 13 Participants were monitored on heart rate, blood pressure, modified Borg scale score, mMRC dyspnea score, and end-tidal carbon dioxide.
The demographics (age, gender, height, weight), body mass index (BMI), global initiative for chronic obstructive lung disease grade, COPD group, comorbidities, and smoking status of referred patients were systematically recorded. All patients underwent a routine baseline and primary outcome assessment in which the following variables were obtained by mMRC, CAT, post-bronchodilator spirometry FEV in the first second and FVC (FEV1/FVC), and acute exacerbation at the time of referral to start the exercise training program at baseline, mMRC and CAT were repeatedly measured upon the completion of the end of 3-month exercise training and at 12th month, while pulmonary function tests were measured at 12th month only. The history of acute exacerbations in the previous 12 months and following one year was recorded when the patients participated the study. For the training group, participants received 6-min walking test, maximum inspiratory pressure, maximum expiratory pressure, and calf circumference measurements before and after lower-limb endurance training.
The CAT involves 8 dimensions for assessing the impact of COPD patients on the HRQoL, and the reliability of the Chinese version Cronbach's alpha is 0.805. 14 The assessment test includes cough (CAT-1), phlegm (CAT-2), chest tightness (CAT-3), breathlessness (CAT-4), limited activity (CAT-5), confidence leaving home (CAT-6), sleeplessness (CAT-7), and energy (CAT-8). Each item scores 0–5 points, with a total score of 40. Dyspnea in daily living was evaluated by the mMRC scale consisting of five statements describing almost the entire range of dyspnea from none (Grade 0) to almost complete incapacity (Grade 4). Acute exacerbation is defined as “an acute event characterized by a worsening of the patient's respiratory symptoms that is beyond normal day-to-day variations and leads to a change in medication,” and severe of severity when required hospitalization. 11 Acute exacerbation number indicates the occurrence before 1 year of the study, while acute exacerbation change describes the number of acute exacerbations after 1 year of the study subtracting the number 1 year prior to the enrollment.
The 6-min walking test as a common tool for assessing exercise capacity was performed at baseline and third month. During the 6-min walking test, the patients were encouraged to use their maximum ability to walk briskly. 15 Oxygen saturation was measured using a pulse oximeter and heart rate, and CAT scale score were recorded throughout the test. The CAT scale score was utilized for the degrees of dyspnea by rating in a range between 0 for none and 10 for maximal sensation. The maximum inspiratory pressure and maximum expiratory pressure were measured using a pressure-monometer (Galemed Inc., Taiwan). The maximum inspiratory pressure was measured at the mouth during maximum inspiratory strength for at least 1.5 s, while the maximum expiratory pressure was measured by FEV1. The measurement was repeated three times with 1-min break, and the best result was recorded. 16
Calf circumference was monitored in the standing position using a non-elastic tape. The tape was placed around the calf without compressing the subcutaneous tissue and was moved along the length of the calf to obtain the maximal circumference. 17
Statistical Analysis
Shapiro-Wilk tests were conducted to assess the normality of the data. Continuous variables and categorical variables are represented as median (interquartile range, IQR) and numbers, respectively. Analyses were performed with Mann–Whitney U tests for continuous unpaired variables, Wilcoxon signed-rank tests for paired variables, and chi-square or Fisher's Exact tests for categorical variables.
Correlations among outcomes in the training group were tested by Spearman's correlations and Friedman tests were conducted to compare repeated measures outcomes at baseline, the end of third month and12th month. All p-values were two-tailed and a P-value <0.05 was considered statistically significant. Statistical analyses were performed using the statistical package for the social sciences version 26.0 (SSPS Inc., Chicago, IL, USA).
Result
One hundred and thirty-eight patients were referred to the training program for screening, and 69 patients were included. Figure 1 illustrates the flowchart of the study and lists reasons for exclusions.
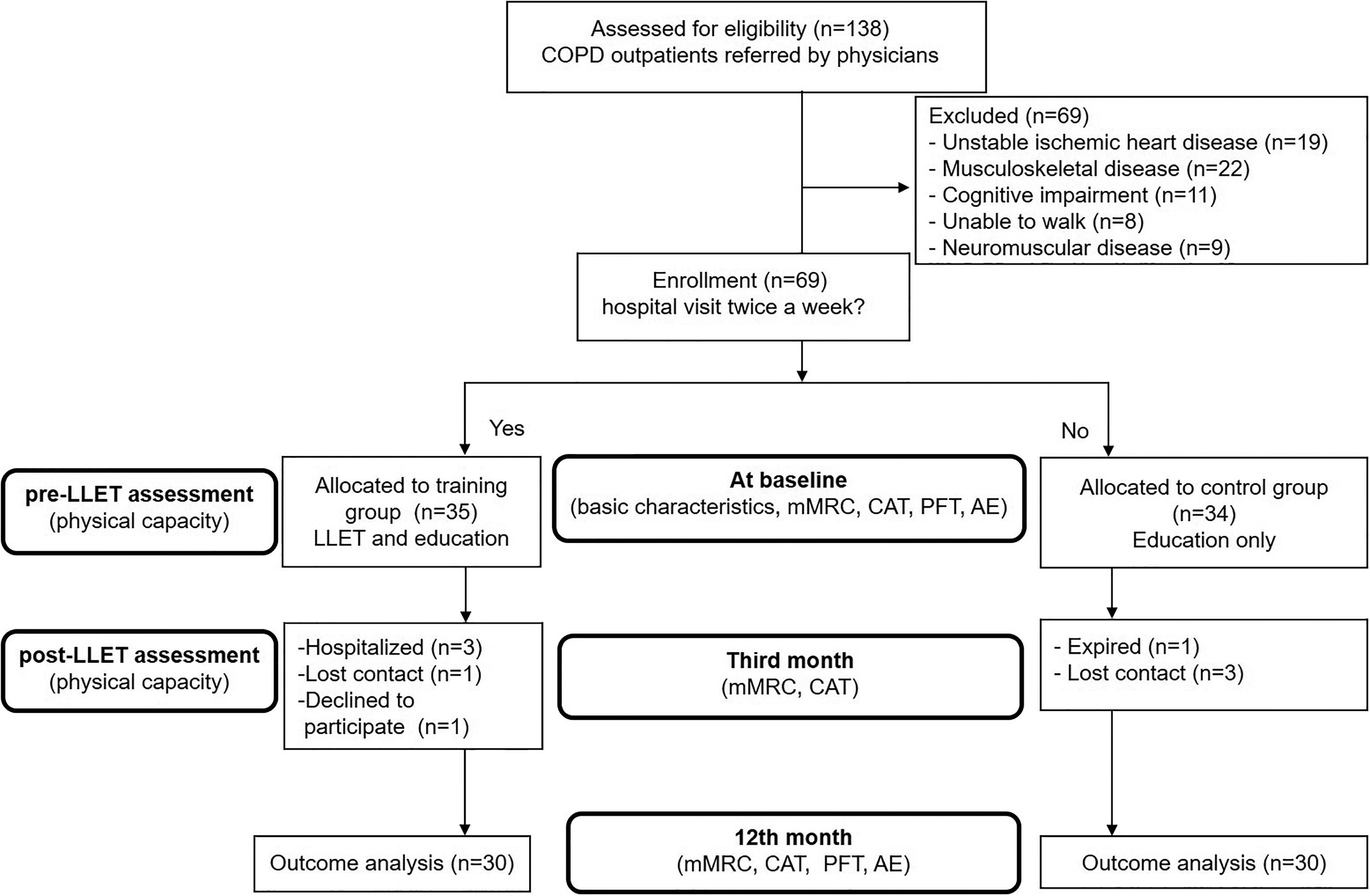
Flowchart for the study protocol. COPD: chronic obstructive pulmonary disease; LLET: lower-limb endurance training; mMRC: modified medical research council dyspnea score; CAT: chronic obstructive pulmonary disease assessment test; PFT: pulmonary function test; AE: acute exacerbation.
The baseline characteristics expressed as median and IQR were similar between the 2 groups (Table 1). The median ages were 66 years and 69 years for the training group and control group, respectively, and 58 out of 60 participants were male. The majority of participants in both groups were diagnosed with global Initiative for chronic obstructive lung disease grade 3; however, training group had more than 60% of participants classified as COPD group D. Most of the participants had more than one comorbidity (67.6%), with cardiovascular disease, bronchiectasis, anxiety, and cancer.
Characteristics of participants.
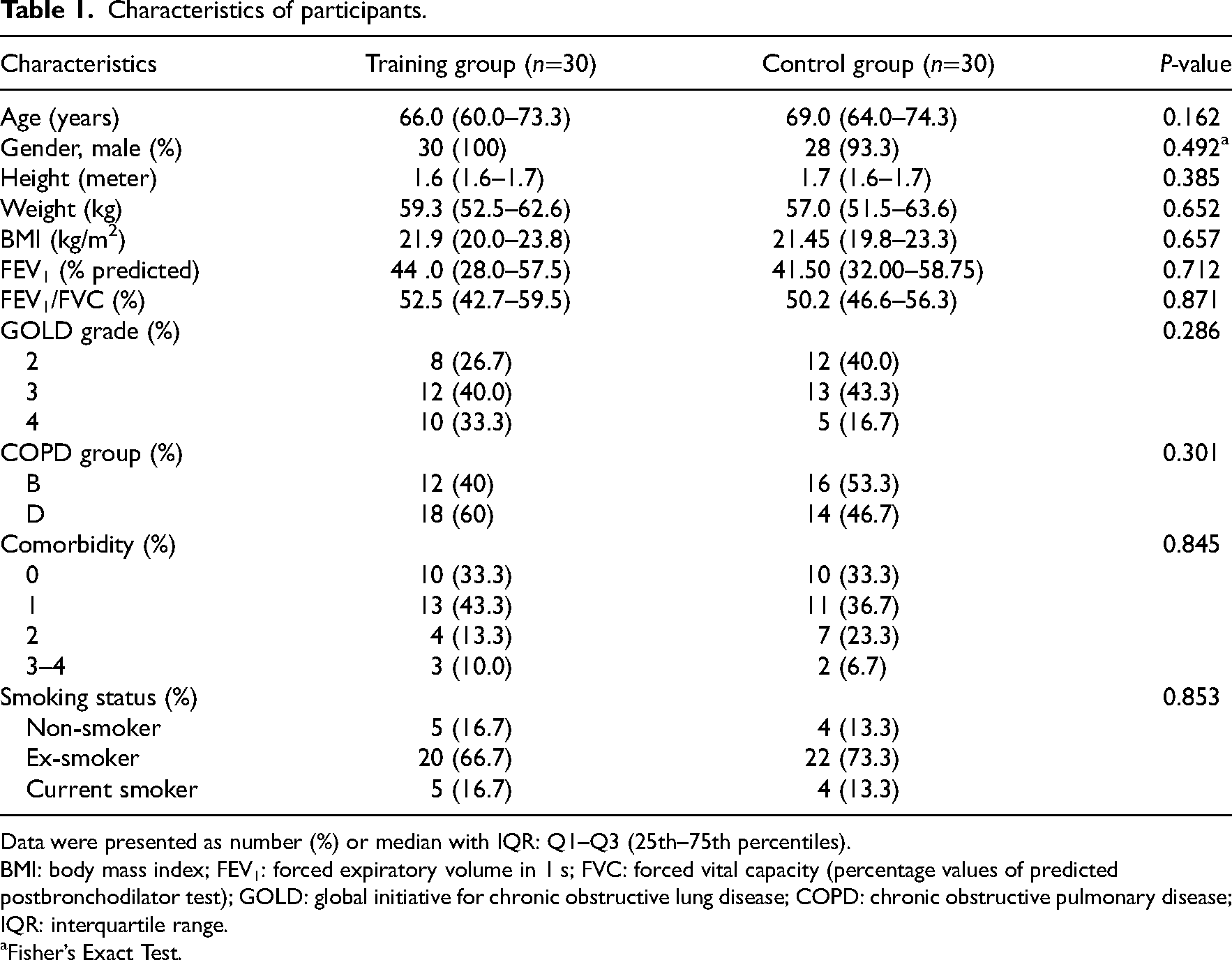
Data were presented as number (%) or median with IQR: Q1–Q3 (25th–75th percentiles).
BMI: body mass index; FEV1: forced expiratory volume in 1 s; FVC: forced vital capacity (percentage values of predicted postbronchodilator test); GOLD: global initiative for chronic obstructive lung disease; COPD: chronic obstructive pulmonary disease; IQR: interquartile range. aFisher’s Exact Test.
Table 2 illustrates comparisons of outcomes at the at baseline, third month, and 12th month. Participants had similar status on mMRC, CAT score, pulmonary function test results, and acute exacerbation one-year prior to participation of the study. The mMRC scores from 3 to 2 points and the CAT score from 18.5 to 10 points, were significantly much lower in the training group at the third month (P < 0.001) and remained lower when comparing the control group at the 12th month (P < 0.001). The number of acute exacerbations in the previous year was similar (0 for training group versus 1 for the control group), but the number of change from a previous year was significantly lower in the training group (−1 for training group versus 1 for control group; P = 0.011). Additionally, acute exacerbation was significantly less within the training group (P = 0.018). No difference was noted in pulmonary functions between groups. The CAT score total score and scores of each domain were compared (Figure 2). All scores were similar between the two groups at the baseline, but significantly reduced after 3 months of training, except the “chest tightness” score.
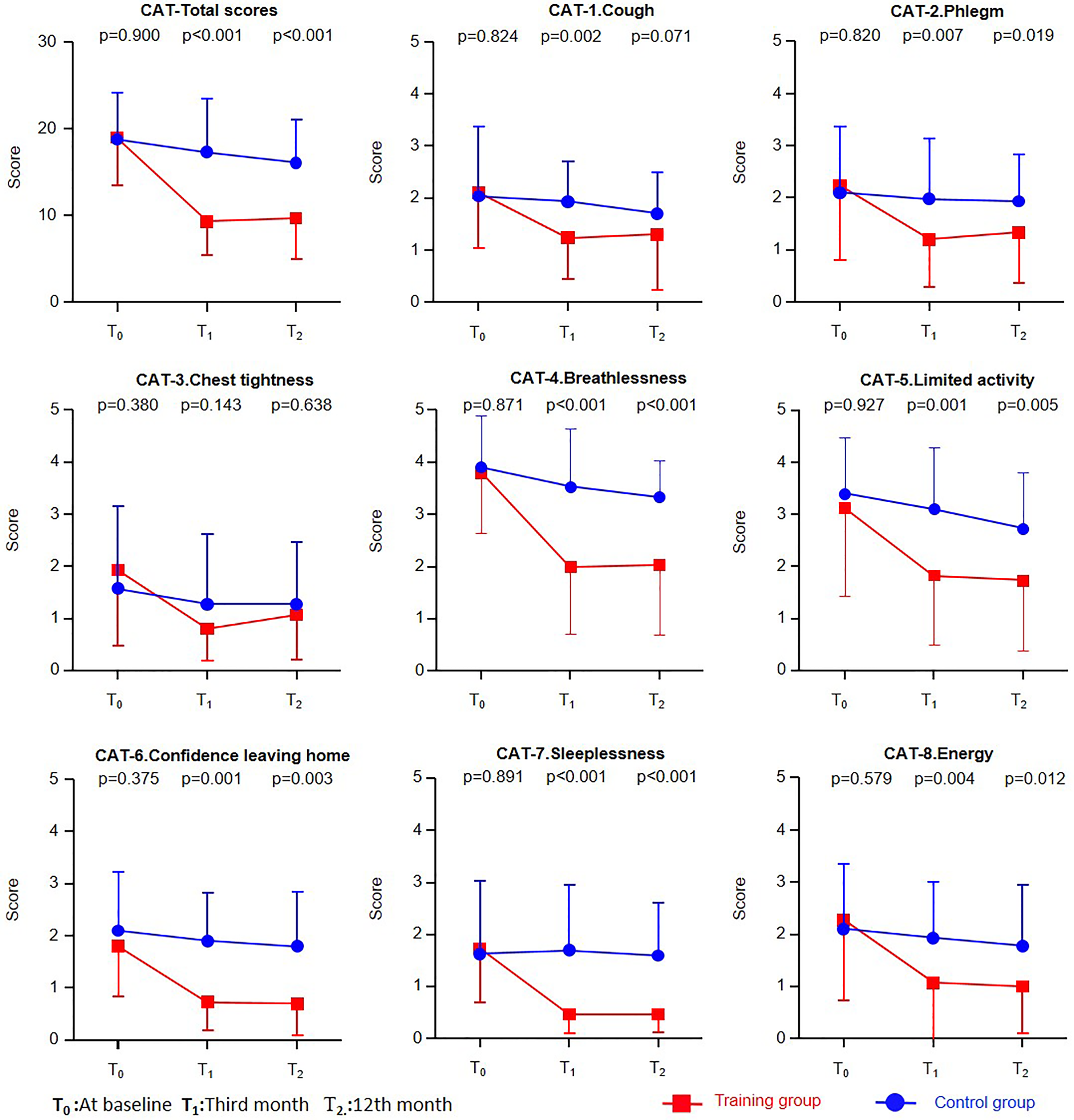
Comparisons of chronic obstructive pulmonary disease assessment test total scores and sub-scores of each domain data were presented as mean and SD within groups for repeated measurement at T1 (third month) or T2 (12th month) comparing with T0 (at baseline). CAT-total: chronic obstructive pulmonary disease assessment test total scores; SD: standard deviation; CAT-1: cough; CAT-2: phlegm; CAT-3: chest tightness; CAT-4: breathlessness; CAT-5: limited activity; CAT-6: confidence leaving home; CAT-7: sleeplessness; CAT-8: energy.
Comparisons of primary outcomes (training group n=30; control group n=30).
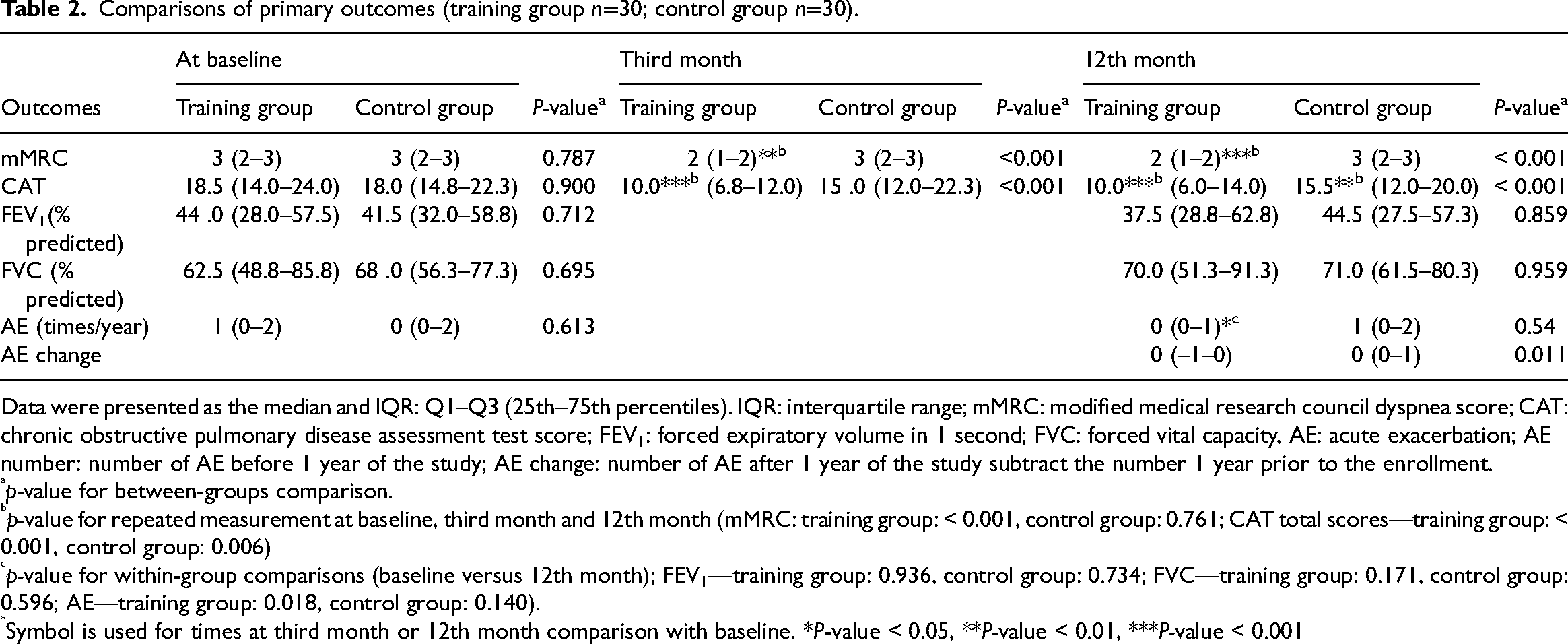
Data were presented as the median and IQR: Q1–Q3 (25th–75th percentiles). IQR: interquartile range; mMRC: modified medical research council dyspnea score; CAT: chronic obstructive pulmonary disease assessment test score; FEV1: forced expiratory volume in 1 second; FVC: forced vital capacity, AE: acute exacerbation; AE number: number of AE before 1 year of the study; AE change: number of AE after 1 year of the study subtract the number 1 year prior to the enrollment.
p-value for between-groups comparison.
p-value for repeated measurement at baseline, third month and 12th month (mMRC: training group: < 0.001, control group: 0.761; CAT total scores—training group: < 0.001, control group: 0.006)
p-value for within-group comparisons (baseline versus 12th month); FEV1—training group: 0.936, control group: 0.734; FVC—training group: 0.171, control group: 0.596; AE—training group: 0.018, control group: 0.140).
Symbol is used for times at third month or 12th month comparison with baseline. *P-value < 0.05, **P-value < 0.01, ***P-value < 0.001
The variable measurements of physical capacity in the training group are presented in Table 3, and Supplemental material 1 shows changes in exercise intensity at the first and 24th sessions of training. Comparing to the baseline, lower-limb endurance training significantly improved on the 6-min walking distance by 37 m (P < 0.001), peak exercise working load by 10 W (P < 0.001), maximum inspiratory pressure by 8 cmH2O (P = 0.003), maximum expiratory pressure by 6 cmH2O (P = 0.002), and calf circumference by 1 cm (P = 0.001). Furthermore, significantly higher oxygen saturation was presented during 6-min walking test after lower-limb endurance training.
Physical capacity before and after training in the training group (n=30).
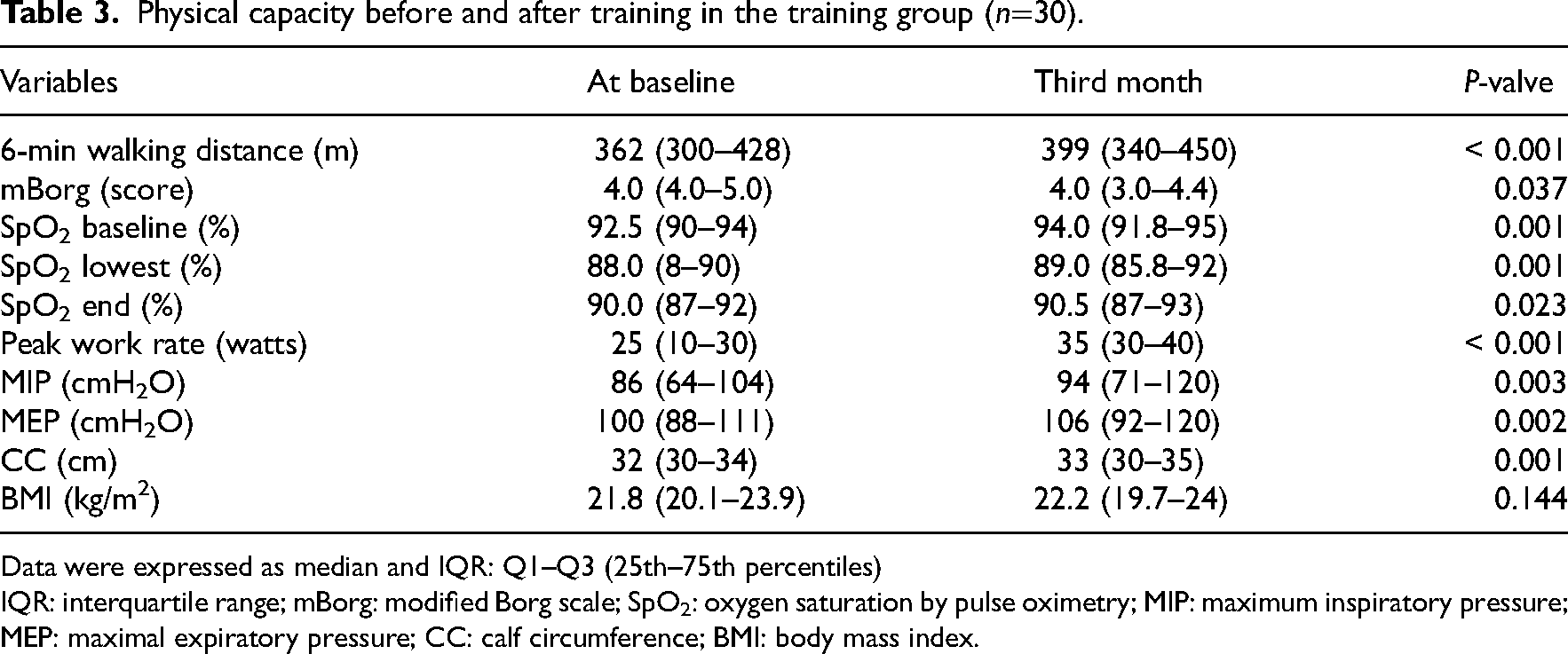
Data were expressed as median and IQR: Q1–Q3 (25th–75th percentiles)
IQR: interquartile range; mBorg: modified Borg scale; SpO2: oxygen saturation by pulse oximetry; MIP: maximum inspiratory pressure; MEP: maximal expiratory pressure; CC: calf circumference; BMI: body mass index.
Table 4 illustrates the correlations of major outcomes in training group, and Supplemental material 2 presents correlations among each domain and outcome at the baseline and end of training. The major findings of correlations were illustrated as follows:
A strong correlation was found between mMRC and CAT score at 12th month (r2 = 0.81). Moderate correlations were found between CAT score and acute exacerbation at 12th month (r2 = −0.56), and 6-min walking distances and mMRC both at third month and 12th month.
Correlations among outcomes in the training group (n=30).
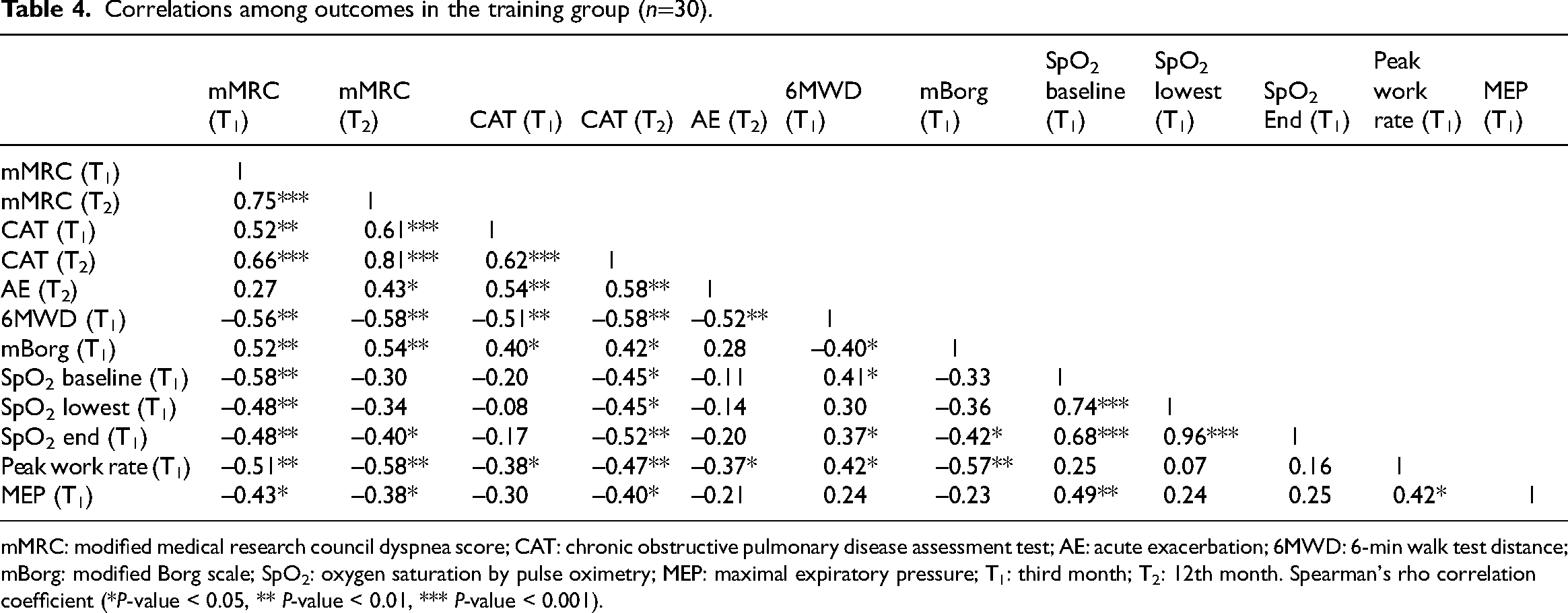
mMRC: modified medical research council dyspnea score; CAT: chronic obstructive pulmonary disease assessment test; AE: acute exacerbation; 6MWD: 6-min walk test distance; mBorg: modified Borg scale; SpO2: oxygen saturation by pulse oximetry; MEP: maximal expiratory pressure; T1: third month; T2: 12th month. Spearman's rho correlation coefficient (*P-value < 0.05, ** P-value < 0.01, *** P-value < 0.001).
Discussion
This study has demonstrated that three months lower-limb endurance training reduced the mMRC and CAT scores, increased physical capacity, and lowered the rate of hospital readmission for acute exacerbation.
Our findings are consistent with previous studies which revealed that activity-related symptoms and functional status of COPD outpatients were improved through the effect of lower-limb endurance training.5,7 In a meta-analysis of lower-limb endurance training in stable COPD patients, the training improved the mMRC, CAT score during exercise and increased 6-min walking distance. 5 Our study has shown that supervised training significantly decreased the mMRC median scores by 1 point (Table 2), compared to control group with no change. We strongly suggest that individually supervised lower-limb endurance training could be beneficial to those who do not exercise at home or require frequent monitoring during exercise. Additionally, the mMRC moderately correlated with CAT score dyspnea sensation during 6-min walking test in the training group, indicating the benefits of lower-limb endurance training on dyspnea sensation for COPD patients.
A previous study has shown a reduction of CAT total score by 2 points is considered as clinically significant improvement. 18 Dodd et al. 9 reported that the mean change of CAT score following exercise training decreased by 2.9 points, and > 3.8 points was considered as a great improvement after exercise training. In our study, the CAT total scores in training group decreased by 8 points with a dramatic drop in most of CAT score domains, except “chest tightness.” The median CAT total score of training group decreased 8.5 points and the greatest improvement in training group was “breathlessness” with a reduced mean score by 1.8 points, sustaining for 9 months. The decreased CAT score in training group has improved symptom burden on COPD outpatients. Moreover, a parallel finding was presented on mMRC in training group with a strong correlation to “breathless” (r2 = 0.72, in Supplemental material 2).
In a one-year prospective study, Monteagudo and colleagues demonstrated that worsening quality of life was associated with deterioration of respiratory symptoms, and increased hospitalization. 19 Our study has presented that lower-limb endurance training might contribute less acute exacerbation and was correlated with CAT score reduction. Furthermore, previous studies have shown that respiratory symptoms impaired daily activities, morning activities, and sleep quality. 20 To prevent from dyspnea, COPD patients become physically inactive, resulting in deconditioning vicious cycle. 21 Breathlessness and desaturation are the main symptoms occurring during exercise, CAT and mMRC scores were inversely related to the maximal oxygen uptake and workload. 22 We found that the mMRC, “breathlessness” and “limited activity” were negatively correlated with 6-min walking distance and cycling peak work rate which might indicate that the training significantly improved dyspnea sensation with increasing physical activities, and then broke the deconditioning vicious cycle (Table 4 and Supplemental material 2).
Respiratory and peripheral muscle dysfunction in COPD patients worsen physical conditions and quality of life. Lower limb muscle dysfunction plays a key role in muscle deconditioning and the reduction of physical activity.23–25 Additionally, dynamic hyper-inflation and loss of elastic recoil may flatten and shorten the diaphragm, which increases the workload of breathing resulting in dyspnea. 26 Studies have revealed that lower-limb endurance training, such as walking and cycling, ameliorates exercise-induced hyperinflation, exertional dyspnea, and offsetting muscle dysfunction in COPD. 27 In our study, the training improved patients’ functional capacity and peak workload confirmed by the improvement of 6-min walking distance greater than the minimal clinically important difference of 30 m. 28
Increasing inspiratory muscle strength is associated with improvement in exercise capacity, quality of life, and dyspnea sensation, 29 and maximum inspiratory pressure is associated with the severity of acute exacerbation and stability of COPD. 30 Previous studies showed core muscle were strengthened while providing leg training, as well as improvement on maximum inspiratory/expiratory presssures.31,32 The improved expiratory muscle function generates an increase in expiratory flow, eventually leading to sufficient expiration as well as reduction of air-trapping and dynamic hyperinflation. 33 The reduced dynamic hyperinflation leads to increasing inspiratory volume, associated with the reduction in exercise intolerance and breathlessness. 34 Expiratory muscle strength is responded for airway clearance and coughing, and an improvement in the maximum expiratory pressure may contribute to an amelioration of the “cough” score and reduction of acute exacerbation. The maximum expiratory pressure was associated with “breathlessness,” mMRC, baseline pulse oxygen saturation, and peak work rate in our study. The effect of a long-term maintenance program is necessary for future studies.
The limitation of this study lies in three parts. First, the sample size was small because this study was conducted at a single center in a rural area. Second, this was not a randomized study design, which may have underlying bias. The participants of the control group were those who were unable to get to the hospital due to the inconvenience of transportation and no caregiver support, which may affect the accessibility to exercise training. Third, a physical capacity assessment was not performed for the control group at baseline and third month, thus, the physical capacity was not compared at the end of the study period. The global initiation of chronic obstructive lung disease report recommends physical activity to all groups of COPD patients; however, we only included patients diagnosed with great than group B, while the lower limb endurance training was considered as part of pulmonary rehabilitation.
In conclusion, 3-month lower limb endurance taring was associated with lower dyspnea during the activity of daily living, improvement of health status, physical capacity, and respiratory muscle strength at the completion of 3 months of training, and the benefits are maintained for additionally 9 months with a lower occurrence of hospital readmission for acute exacerbation.
The lower-limb endurance training enhanced the functional capacity confirmed by an increased 6-min walking distance with a better oxygen saturation and larger exercise peak workload. The training improved health status and symptoms with a lower occurrence of acute exacerbation within a year among COPD outpatients.Clinical messages
Footnotes
Acknowledgments
The authors thank colleagues from Health Information and Epidemiology Laboratory at Chiayi Chang Gung Memorial Hospital and Dr Chia-Hao Chang, Associate Professor of Nursing Department at Chang Gung University of Science and Technology, Chiayi campus, who provided expertise on statistical analysis. We would also like to show our gratitude to Dr Hsiu-Lien Chu, Assistant Professor of General Education at Chang Gung University of Science and Technology, Chiayi campus, who gave comments on the English version of the manuscript.
Author contributions
Conceptualization was done by An-Chi Chung, Chun-Jung Chang, Jui-Fang Liu, Ming-Szu Hung, and Tien-Pei Fang. Methodology was designed by An-Chi Chung and Tien-Pei Fang. Investigation was done by An-Chi Chung and Chun-Jung Chang. Formal analysis was done by Jui-Fang Liu, Tien-Pei Fang and Hui-Ling Lin. Writing was done by Hui-Ling Lin, Chun-Jung Chang, and Tien-Pei Fang. Project administration and supervision were carried out by Tien-Pei Fang and Hui-Ling Lin.
An Authorship Statement
All authors listed meet the authorship criteria according to the latest guidelines of the International Committee of Medical Journal Editors and that all authors are in agreement with the manuscript.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Chang Gung Mermorial Funaiton (Grant number: CMRPG6C0541).
Ethical approval
This study was approved by the Ethics committee of Chang Gung Medical Foundation (approval number: 102-4163B).
Informed consent
Informed consent was obtained from all participants
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
