Abstract
The World Health Organization’s (WHO) International Classification of Functioning, Disability, and Health (ICF) is a framework designed to describe and measure health and disability. It examines how a person’s health condition affects their daily life and overall functioning and considers not just the physical or mental limitations that may come from a condition but also how environmental factors (like accessibility and social support) influence a person’s ability to participate in life. An ICF Core Set is a short list of the most important factors to consider when looking at how a specific health condition affects a person’s life. These Core Sets are made to be practical tools for health care providers, researchers, and caregivers. Here we describe how this process was conducted for the development of the comprehensive Core Set for deafblindness. The four required studies included a systematic literature review, qualitative interviews with individuals living with deafblindness, an online expert survey, and a multi-centered clinical evaluation. All studies include data from each of the six regions of the WHO (Africa, the Americas, Europe, the Eastern Mediterranean, the Western Pacific, and South-East Asia). Data from 54 countries were linked using the ICF coding system, then merged, and presented at an international consensus conference in Spain in 2024. The process resulted in the first version of the comprehensive Core Set for deafblindness with 218 codes representing the most salient functional effects of deafblindness. This Core Set builds the foundation for an eventual brief Core Set (~30 codes), and allows us to begin the process of validation and implementation in policy, teaching, research, and service delivery environments.
The awareness of deafblindness by the public is historically influenced by the mainstream perception of individuals such as Hellen Keller, the first American with deafblindness to obtain a college degree in 1904 (Bjorling, 1981), or Hamen Girma, the first deafblind person to graduate from Harvard University with a law degree in 2013 (Girma, 2019). There are many similar role models in other countries around the world that have a strong influence on the perception (and pre-conceived ideas) of persons living with deafblindness (Wittich & Riggillo, 2025). The community of individuals living with deafblindness, however, is more diverse than what these role models may be able to represent, resulting in misconceptions about what it may be like to live with deafblindness. The variables that influence this diversity include the severity of each sensory impairment (ranging from residual low vision to no light perception; hard of hearing to no sound perception), the order of onset (vision loss first, hearing loss first, simultaneous onset), and the timing of the onset (congenital or pre-lingual, post-lingual, working-age adulthood, late life; Dammeyer, 2014). One key characteristic that makes deafblindness a unique disability lies in the inability to use one sense to compensate for the other, as would be the case for individuals living with uni-sensory loss.
Definitions of deafblindness
The term deafblindness describes the combination of vision and hearing difficulties, independent of their levels of severity, or order and time of onset (Dammeyer, 2014; Wittich et al., 2013). Within the medical model, the definition of deafblindness is primarily disease-based (Ask Larsen & Damen, 2014). Impairments of vision and hearing are generally assessed and quantified using behavioral measures such as high-contrast distance visual acuity, visual field diameter, signal-to-noise ratios in speech perception, or pure-tone audiometry to determine detection thresholds (Bright et al., 2023). These thresholds are then used in the context of eligibility criteria, for example, to establish whether an individual gains access to specific rehabilitation services, assistive devices, or other government benefits (Wittich et al., 2012). Within the psycho-social or rehabilitation model, the definition of deafblindness focuses on functional ability. The Nordic definition (Nordic Leadership Forum on Deafblindness, 2024) stipulates that deafblindness is a unique disability and should not be simply considered as the addition of visual and hearing disabilities. This unique characteristic is rooted in the inability to use one sense to compensate for the other, a feature that has been recognized by the European Parliament (2004). In addition, the World Federation of the Deafblind (2018) has adopted and endorsed the Nordic definition as their standard. The Nordic definition further proclaims that individuals living with deafblindness experience participation restrictions to a level where services, environmental adaptation, and assistive devices are required to facilitate engagement in society.
The Dutch Functional Definition of Deafblindness (Heppe et al., 2021) takes this description one step further, dividing the population of individuals living with deafblindness into three distinct subgroups. The first subgroup includes individuals with congenital sensory impairments where their deafblindness is present generally before the development of speech, possibly acquiring tactile sign language or pro-tactile as their principal communication modality later in life (Edwards, 2014). This type has also been termed pre-lingual deafblindness (Dammeyer, 2011). Individuals with post-lingual vision and hearing impairments develop their sensory difficulties after the acquisition of speech and may rely on a large variety of communication modalities, depending on the severity, time, and order of onset of the impairment combination. Finally, individuals with age-related dual sensory loss live with sensory conditions that are related to the aging process such as age-related macular degeneration and presbycusis. The use of these terminologies varies somewhat across professional groups (Wittich et al., 2013), and is further complicated by some overlap between, and exceptions within these three groups. Older adults with acquired impairments are unlikely to identify with the label deafblind, having lived most of their lives with functional sight and hearing, and being more comfortable with the term dual sensory impairment. Some individuals living with Usher syndrome are born deaf and often consider themselves part of the culturally Deaf community (D/deaf) because of their use of sign language; their vision impairment develops later and is perceived as an impairment, but not necessarily as part of their identity (Evans & Baillie, 2022).
These examples express some of the variability and heterogeneity in terms and definitions across invested parties in the field of deafblindness. Similarly, there is a range of terminologies being used to describe and identify individuals living with combined vision and hearing difficulties (Crowe & Wittich, 2024). For this chapter, we utilize the overarching term deafblindness to refer to all sub-populations; however, we acknowledge that multiple terminologies exist and that there are different preferences among subgroups of the population. While the terms deafblindness and dual sensory impairment are often used interchangeably, a preference has emerged for the use of dual sensory impairment when referring to older adults living with acquired sensory losses (Wittich et al., 2013).
The effect of deafblindness on functioning
The presence of deafblindness can have devastating effects on a multitude of aspects in an individual’s life, no matter when the onset of either impairment occurs, how severe they are, or whether they occur acutely or progressively. The main functional concerns can largely be divided according to the three groups defined by the Dutch Functional Definition (Heppe et al., 2021). For children who are born with deafblindness or develop the impairments before the development of language, the focus is on the acquisition of communication modalities (Bruce et al., 2016), as well as the facilitation of cognitive development (Larsen & Dammeyer, 2021; Nicholas, 2020). In addition, the development of independent mobility and access to education (Wolthuis et al., 2020) are significant concerns. Compensatory strategies often focus on the tactile modality (Brede & Souriau, 2016). For individuals who develop deafblindness after language acquisition, prominent effects can manifest in changes in how they identify as a person living with a disability (Wimberly, 2023), coping with the acquired sensory changes (Lehane et al., 2018; Wettstein et al., 2019), as well as employment (Scheffelin, 1981) and social participation (Jaiswal et al., 2018). For individuals who develop age-related deafblindness, the functional adjustments often focus on rehabilitation strategies to maximize residual vision and hearing (Saunders & Echt, 2007), as well as interventions to optimize independence while reducing social isolation (Hersh, 2013; Jaiswal et al., 2020).
In addition, there are individuals who fall between these three main groups, and whose unique functional needs add to the heterogeneity of this population. For example, individuals who live with one congenital impairment and who then develop a second impairment later in life face unique challenges. The experience of older adults with congenital deafblindness differs considerably from that of individuals who develop age-related deafblindness (Simcock et al., 2023; Wittich & Simcock, 2019). Members of the culturally Deaf community, for example, often view their hearing status as part of their identity without perceiving it as an impairment. The onset of visual impairment, however, can then threaten this identity if the vision changes manifest as a communication disability and interfere with the ability to utilize sign language. Similarly, congenitally blind individuals who have relied on their hearing all their life as their primary compensatory mechanism may suddenly experience difficulties using auditory cues during orientation and mobility tasks when they develop age-related hearing difficulties (Wiener et al., 2010). The need to develop a holistic understanding of the functional effects of deafblindness has been expressed previously, whereby the bio-psycho-social perspective of the International Classification of Functioning, Disability, and Health (ICF), proposed by the WHO, may hold the key (Möller, 2003). Such a perspective is a way of understanding how health and illness are influenced by a combination and interaction of biological, psychological, and social factors, that can then be used in clinical care and research to study human behavior and disorders with a more inclusive approach.
Description of ICF and its coding system
The International Classification of Diseases (ICD) focuses on diagnosing and classifying diseases (World Health Organization, 2019), while the ICF (see Figure 1) focuses on how health conditions affect an individual’s functioning and participation in daily life (World Health Organization, 2001). The ICD identifies what is wrong, while the ICF examines how it impacts a person’s ability to live. The ICF comprises contextual factors such as environmental factors (e.g., technology) and personal factors like age and wealth, though the latter are not coded. It also considers aspects of functioning, including body structures (e.g., eyes, ears), body functions (e.g., sensory functions and pain), and activities and participation (e.g., mobility, communication), and how all these interact within the context of a specific health condition.
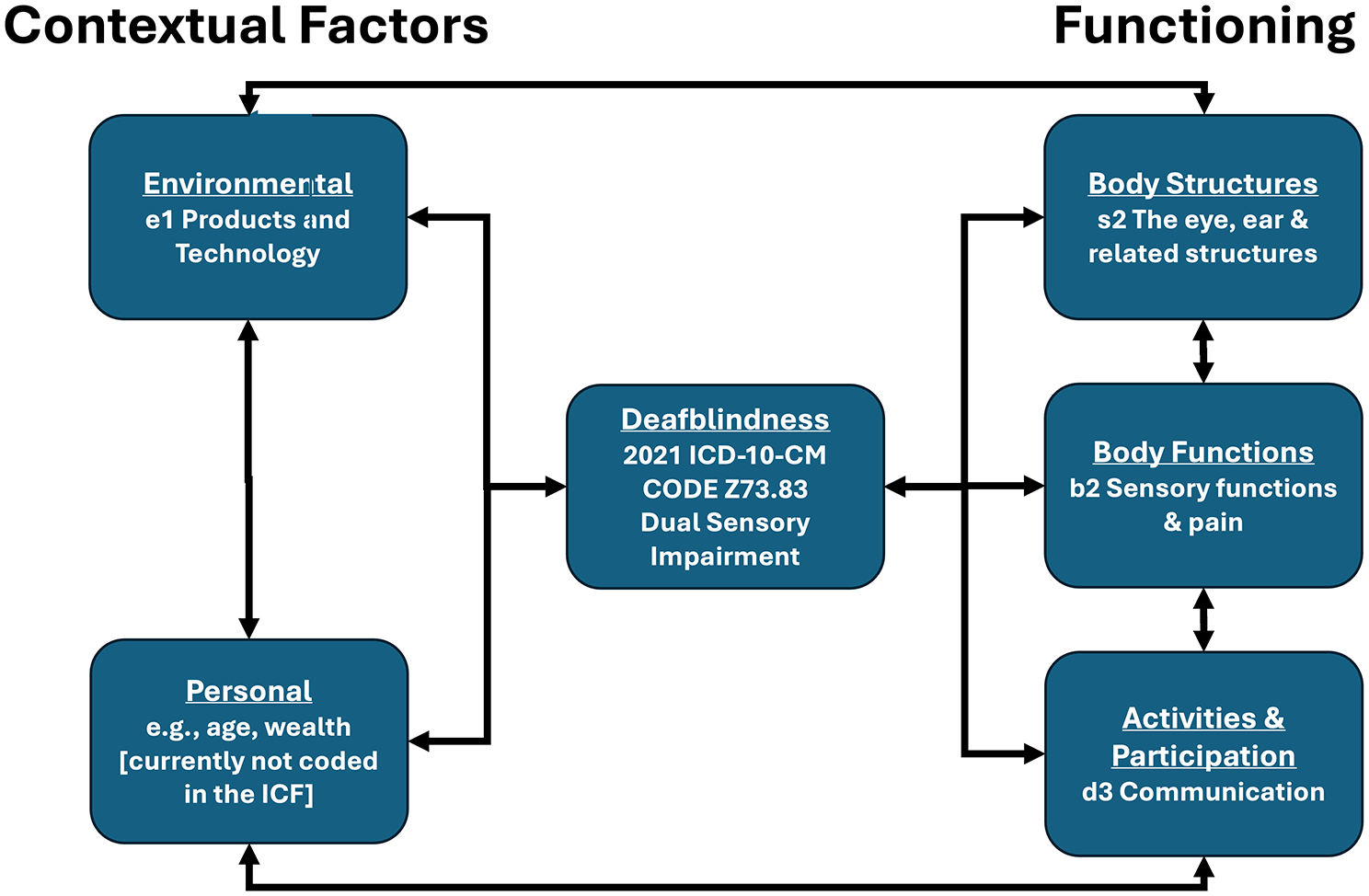
Overview of the World Health Organization’s (WHO) International Classification of Functioning, Disability, and Health (ICF), including examples of ICF categories as they apply to deafblindness as the focus of the presented Core Set development. This framework is designed to conceptualize health as impairments of physical body structures and their functions, as well as activity limitations and participation restrictions while considering contextual factors such as the environment and the person living with a specific health condition. The bidirectional arrows indicate the interactive nature of the components within this framework.
What are Core Sets?
The ICF framework includes over 1400 individual categories, and while extensive and comprehensive, it may not be practical for use in many contexts, such as clinical settings or policymaking. Therefore, subsets of categories relevant to a specific health condition, or Core Sets, have been developed that facilitate the use of the system. The development and identification of categories that then compose the Core Sets follows a process laid out by the ICF Research Branch, as displayed in Figure 2 (Selb et al., 2015). The Preparatory Phase requires four studies to be completed, including a systematic literature review, a survey with experts in the topic domain, qualitative interviews with individuals living with the condition of interest, and a clinical evaluation study that explores the use of standardized measures when evaluating individuals with lived experience. The data from each study are then coded, using a specified process of linking the outcome content to the ICF categories (Cieza et al., 2019). This process is not to be underestimated, because it requires specific training, and takes time as well as reflection and discussion among the team members to produce a high-quality result. In Phase 1, the data are then integrated and synthesized during a consensus conference at which all relevant parties and all regions of the WHO are represented. Core Sets exist in two main formats: Comprehensive Core Sets specifically try to contain all or nearly all elements that are relevant to the condition in question. Therefore, they can be quite long, depending on the complexity of the health condition. Brief Core Sets, in comparison, try to focus on the most essential aspects of a health condition, and generally are around 30 codes in length. Their condensed nature makes them more user-friendly and increases their chance of being implemented in practice. Both comprehensive and brief Core Sets are currently available on the ICF Research branch website (https://www.icf-core-sets.org/) for a variety of health conditions, including several musculoskeletal conditions (e.g., low back pain), cardiopulmonary conditions (e.g., ischemic heart disease), neurological conditions (e.g., multiple sclerosis) and neurodevelopmental and psychiatric conditions (e.g., autism or depression). In terms of sensory health, the Core Sets for hearing loss are already available, and studies to develop those for visual impairment are currently underway (Billiet et al., 2021, 2024).
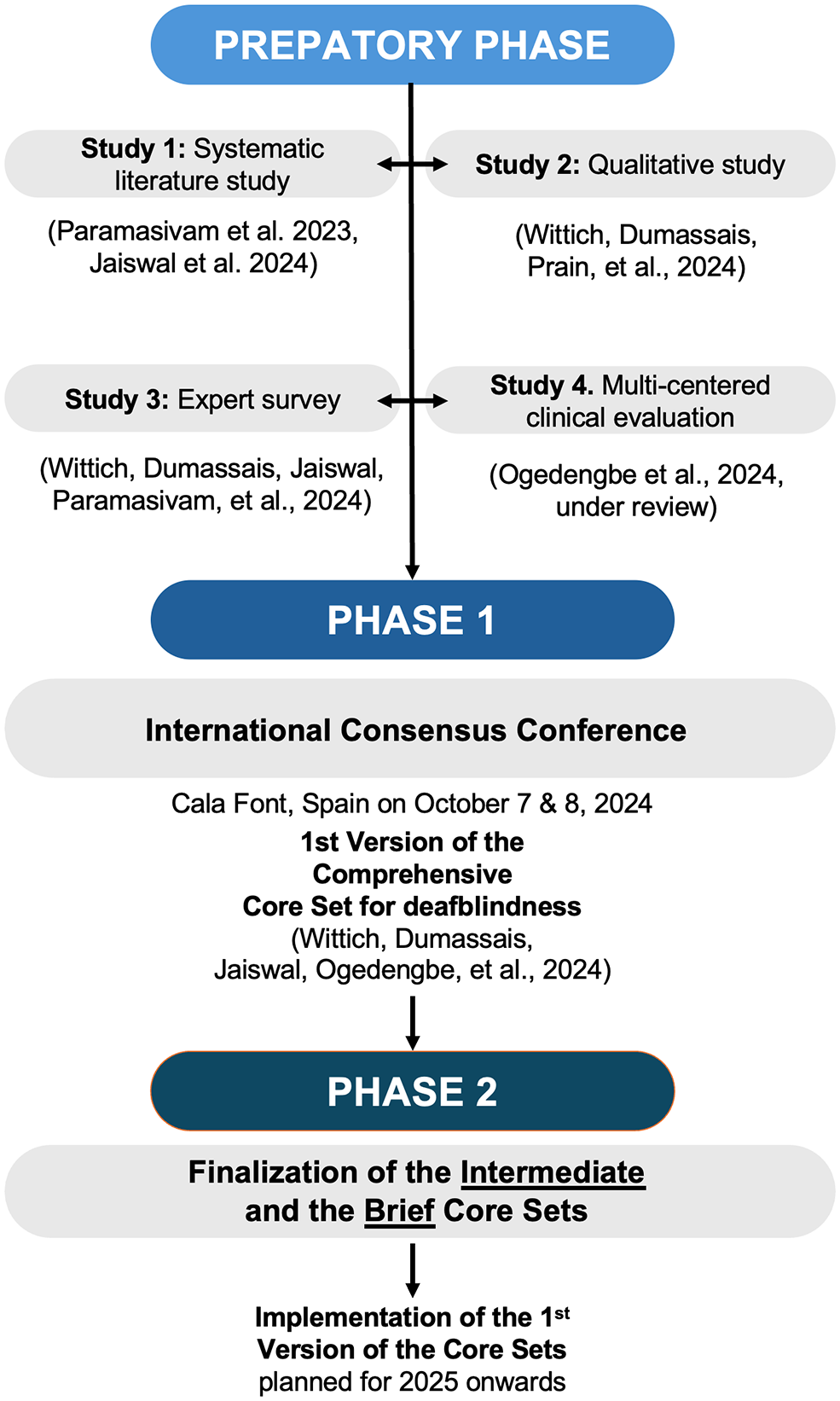
Flowchart displaying the development steps of the Core Sets for deafblindness, based on the phases laid out by Selb et al., 2015.
Why Core Sets for deafblindness?
At first glance, the implementation of a coding system based on a standardized set of terminologies may appear somewhat daunting, and its applied benefits may not be immediately apparent. Conceptually, Core Sets provide a standardized framework for assessing the functioning and disability of individuals for a specific health condition, and to capture the most relevant aspects, allowing for comprehensive evaluation and comparison of outcomes across populations, interventions, and settings. The standardized and universal terminology facilitates communication among health care professionals, researchers, policymakers, and individuals living with the condition. Given the breadth of the coding framework, the assessments are holistic, capturing not only medical aspects of health but also factors related to participation, environmental barriers, and personal factors, ultimately improving the quality of care, research, and policy development in health care. However, there are also additional uses of these Core Sets. Decision-makers often rely on standardized information when they need to regulate insurance coverage, education curricula, or policy guidelines. Documents like the Core Sets can be used in such situations, aligning decisions with global priorities. Given the specific expertise required to manage care needs for individuals with deafblindness, the Core Sets are available to guide and inform all stakeholders who can benefit from their representative content. In the case of the Core Sets for deafblindness, their relevance was initially identified by a father with lived experience of caring for a daughter with deafblindness (Lopez i Manzano et al., 2020), leading him to initiate the process described here.
Preparatory phase
The process of Core Set development requires global collaboration, given that the data need to be representative of all six regions of the WHO. The process is generally driven by stakeholders with vested interest in the condition at hand, in our case, policymakers, individuals with lived experience, and researchers (Lopez i Manzano et al., 2020). Previous teams initiated their work by inviting interested parties in the form of an invitation paper, as was the case for the vision and hearing Core Sets (Billiet et al., 2021; Danermark et al., 2010). In the case of deafblindness, the research community is much smaller and already well connected through existing networks. Therefore, there was no need for this step because the project was initiated by representatives of Deafblind International, its European Deafblind Network, and its Research Network. Instead, the team published a protocol paper, laying out the plan for the overall process (Paramasivam et al., 2021). As the project developed, the networking expanded to include the World Federation of the Deafblind as an additional partner to maximize the engagement of individuals with lived experience.
Study 1: the outcomes of the systematic literature review
The first step in Core Set development is a systematic literature review whose purpose is to represent the perspective of researchers and academics. For deafblindness, the publication of this step was divided into two parts. Part 1 presented an overview of the review outcomes focusing on the study characteristics and the extracted qualitative and quantitative outcome measures (Paramasivam et al., 2023). Part 2 provided a presentation of the linked data that showed the proportional distribution of unique ICF categories represented within these outcome measures (Jaiswal et al., 2024). The review included 147 studies, published between March 2011 and September 2022, all of which presented original qualitative and/or quantitative data, and included at least five adult (18+) participants living with any type of severity of deafblindness. The outcomes measures included 57 standardized measures such as audiometry, 59 patient-reported standardized measures such as the Centre for Epidemiological Studies Depression Scale (Radloff, 1977), 178 patient-reported non-standardized measures such as education level, and 11 measures that relied on standardized responses from health professionals such as the InterRAI Community Health Assessment (interRAI Instrument and Systems Development Committee, 2006), among others. Only three measures emerged that were specifically designed to assess individuals living with deafblindness: the deafblind supplement of the InterRAI Community Health Assessment (Hirdes et al., 2007), GOCC4All Survey which evaluated a specific assistive device (Rodríguez et al., 2022), and the Usher Lifestyle Survey (Damen et al., 2005).
In preparation for study 4, the multi-centered clinical evaluation, the Core Set development requires the identification of the three most frequently used patient-reported standardized measures that are available without cost. These measures are then included in study 4, in part to establish the feasibility of such assessments in the target population, and to provide additional contextual data during the consensus conference. In the present case, the three most often used and available measures were the Centre for Epidemiological Studies Depression Scale screening for depressive symptoms (Radloff, 1977), the Mini Mental State Exam screening cognitive abilities (Folstein et al., 1983), and the Lawton Brody Instrumental Activities of Daily Living scale (Lawton & Brody, 1969).
Study 2: the qualitative interviews
The qualitative study (Wittich, Dumassais, Prain, et al., 2024) was an important part in the development of the ICF Core Sets, as it is designed to gain insight into the experiences and challenges faced by individuals living with deafblindness and their informal caregivers (e.g., family members). Unlike the literature review, this study focused on firsthand accounts, providing a nuanced understanding of daily functioning and challenges. These insights were critical in ensuring the Core Sets reflected real-world experiences. We conducted 26 semi-structured interviews and nine focus groups with 72 individuals who participated in this initiative across the six WHO regions (African Region n = 9; Region of the Americas n = 20; South-East Asian Region n = 11; European Region n = 10; Eastern Mediterranean Region n = 9; Western Pacific Region n = 13; female n = 30; Mage = 41.69, SDage = 19.56, rangeage = 1–83). Over half of the participants had congenital etiology deafblindness such as Rubella, CHARGE syndrome, or Usher syndrome while around 10% had acquired cases of deafblindness (e.g., cataracts, presbycusis, viral infections, etc.). The discussions aimed to examine multiple facets of functioning, such as communication barriers, social interactions, independence in daily activities, and access to education. They were structured around the six following key questions, based on the guidelines for the development of ICF Core Sets, and specifically adapted to address the context of deafblindness (Selb et al., 2015):
How does your deafblindness affect the way your body and your mind work?
In which parts of your body does your deafblindness give you problems?
How does your deafblindness affect the things you can and cannot do in your everyday life?
What and/or who in the environment where you live and work/go to school is helpful and supportive in your everyday life with deafblindness?
What and/or who in the environment where you live and work/go to school makes everyday life with deafblindness difficult for you?
When you think about yourself and the person you are, what helps you to handle your everyday life with deafblindness?
The transcribed interviews and focus groups were systematically analyzed by first identifying key concepts from the analysis and then linking them to relevant categories from the ICF. To give a voice to individuals with lived experience of deafblindness, individual identified categories were not ranked in terms of the frequency of how many times they were identified by a participant in the focus groups or individual interviews. Every single inference of a meaningful concept that could be successfully linked to an ICF category was included in the analysis. However, all meaningful concepts were summed up to get a better idea of which ICF domains and categories were prevalent in the discussions.
Analyzed and linked data revealed several key challenges across different domains of functioning. In the domain of activities and participation, participants with lived experience identified a significant number of categories, with a particular focus on mobility (d4), interpersonal interactions and relationships (d7), and communication (d9). These results suggest that individuals with deafblindness experience the most significant barriers to full participation in society. For instance, activities such as mobility and communication are crucial for independence and social connection and, limitations affect their daily living. Within the environmental factors domain, the chapters on services, systems, and policies (e5), as well as products and technology (e1), were most prominent. The identified environmental factors highlight the importance of external support such as technology for individuals living with deafblindness to navigate life. However, access to these enabling technologies is often governed by existing policies, which may explain why services, systems, and policies were also frequently emphasized. In addition, in the body functions and body structures domains, mental functions (b1), sensory functions and pain (b2), alongside the eye, ear, and related structures (s2), were recurrently discussed. These categories stood out because they represent not just the physical challenges of sensory loss, but also the psychological and emotional burdens that come with it, which are often less visible but equally impactful on quality of life. These findings were further refined in the following study, through an expert survey.
Study 3: the expert survey
The third study, the international expert survey (Wittich, Dumassais, Jaiswal, Paramasivam, et al., 2024), focused on gathering the insights of professionals working with them or providing them with services. These services included but were not limited to health care delivery, education, as well as social support. An accessible online survey was distributed by invitation to professionals in these fields, asking participants to address the same questions posed in the qualitative study but from their professional perspective. The survey responses that were entered in the analyses were proportionally stratified to ensure diversity and representation across various fields, professions, and WHO regions. They included 105 professionals of various domains of work such as intervenors, various health care-related therapists, educators, and administrators (African Region n = 8; Region of the Americas n = 32; South-East Asian Region n = 22; European Region n = 26; Eastern Mediterranean Region n = 3; Western Pacific Region n = 14; women n = 74; Mage = 46.91, SDage = 13.5, rangeage = 22–74). The data analysis process for the qualitative responses followed the same approach as the qualitative study; however, in this study, the identified categories were ranked by the frequency of mention, and only categories cited by 5% or more of the experts made it through to the final analyses.
Analyses revealed notable differences between the input from individuals with lived experience of deafblindness and that of experts. In contrast to the lived experience group, the domain with the highest number of identified categories in the expert survey was environmental factors, followed by body functions, activities and participation, and, finally, body structures. Despite these differences, significant overlap was observed across various chapters, with mental functions (b1), communication (d3), and mobility (d4) emerging as prominent categories, suggesting a shared recognition of the core challenges that affect both the functional and psycho-social aspects of life for individuals with deafblindness. The expert survey complemented the qualitative study and literature review by providing a professional perspective that highlighted broader systemic factors, enriching the understanding of deafblindness beyond the direct functional challenges identified by individuals with lived experience.
Study 4: the multi-centered clinical evaluation
The purpose of the multi-centered clinical evaluation is to identify the most reported problems and difficulties experienced by persons living with deafblindness as they are described while undergoing a standardized clinical functional assessment by a professional trained in the use of the ICF coding system. This assessment was conducted using the ICF Check List, version 2.1a (World Health Organization, 2003), which consists of a socio-demographic questionnaire and 125 WHO ICF categories recognized in general clinical practice (Tomandl et al., 2018). It was supplemented by the three most used, and freely available measures that emerged during the systematic literature review: the Centre for Epidemiological Studies Depression Scale screening for depressive symptoms (Radloff, 1977), the Mini Mental State Examination screening cognitive abilities (Folstein et al., 1983), and the Lawton Brody Instrumental Activities of Daily Living scale (Lawton & Brody, 1969).
Recruitment was facilitated through the local rehabilitation partners of the investigator team, as well as mailing list outreach by Deafblind International and the World Federation of the Deafblind. The 29 participants with lived experience resided in Australia, Bangladesh, Canada, Egypt, India, Japan, Nepal, Netherlands, New Zealand, Niger, Rwanda, Spain, Tanzania, the United States, and Zambia. These 14 men and 15 women ranged in age from 20 to 74 with a mean (SD) age of 47.3 (16.3) years, and their representation across the six WHO regions included 17% from Africa, 24% from the Americas, 14% from South-East Asia, 17% from the European, 21% from the Western Pacific, and 7% from the Eastern Mediterranean Regions. Fourteen participants self-reported that their deafblindness was congenital, while 15 indicated acquired sensory impairments.
Their assessments were completed by an occupational therapist with extensive experience using the ICF coding system and its clinical assessment tool. For consistency in the administration across six regions of the WHO, we decided to conduct all assessments remotely, using the Zoom platform (Zoom Video Communications, Qumu Corporation, San Jose, CA). As in previous studies conducted by the research team (Wittich et al., 2023), consent and communication modalities were adapted to facilitate communication according to the individual needs of each participant. The occupational therapist rated each of the ICF categories within the checklist based on the extent to which the environmental factor was reported to be a barrier or a facilitator, using ICF qualifiers (Selb et al., 2015).
In line with the previous studies, the results of the checklist data indicated that the most reported categories of body structures were related to the eye and ear (s2), resulting in impairment of seeing (b210) and hearing (b230) functions. The categories related to listening (d115), communicating with receiving non-verbal messages (d315), and driving (d475) all indicated severe difficulty according to the participants. Some of the most relevant environmental facilitators included immediate family (e310), friends (e320), and the individual attitudes of immediate family members (e410). Environmental barriers included climate (e225) and housing services, systems, and policies (e525). Categories that were identified as both facilitators and barriers included people in position of authority (e330) and design, construction and building products, and technology of buildings for public use (e150) (Ogedengbe et al., 2025).
Phase 1: the process of the consensus conference
During Phase 1 of the ICF Core Sets development, as defined by the ICF Research Branch, an International Consensus Conference takes place (Selb et al., 2015). This crucial step ideally involves 20 to 30 participants who meet to synthesize and finalize findings from studies 1 through 4. Here, participants collaboratively determine which categories meet the required consensus for inclusion, marking the completion of the Core Sets.
Preparing the Consensus Conference
To prepare for the Consensus Conference, two committees were established: a scientific committee and a logistical committee. The logistical committee handled all conference-related arrangements, including inviting participants, assisting with travel visa applications, selecting and setting up the venue, and securing funding to support participants from low-income countries. The logistical committee comprised the scientific lead and research director of the initiative, a scientific co-lead with experience in Core Sets development for a related health condition (hearing loss), two project coordinators supporting the scientific lead, the project initiator who is a policymaker and director of a deafblindness advocacy organization, his project assistant/coordinator, and two additional co-organizers from various deafblindness organizations. This committee ensured a well-organized, accessible, and smoothly run conference. The scientific committee included the scientific lead and research director of the initiative, their research assistant and project coordinator (both graduate students in vision science), a postdoctoral fellow in vision science, and a scientific co-lead with experience in developing Core Sets for hearing loss.
In compiling the identified categories from the initial three studies of Core Set development, a total of 581 categories emerged: 251 in the activities and participation domain, 40 in body structures, 190 in body functions, and 100 in environmental factors. This extensive number of categories was far too much to create a practical and useable Core Set, necessitating a reduction process. To address this challenge, the scientific committee met virtually over ten 1 hr meetings to provide recommendations on the relevance of each category. These recommendations were made based on multiple factors: primarily, the expertise of committee members, but more importantly, the data gathered from previous studies, including the linked data collected from the three most used measures that emerged during the systematic literature review. Each category was ranked according to its frequency and significance across the systematic literature review and the international expert survey, as well as whether it had been mentioned at least once in the qualitative study. This ranking system allowed the committee to prioritize categories that showed strong, consistent relevance across the different research methods. Categories deemed highly relevant were recommended for direct inclusion, while those considered irrelevant or not specific to deafblindness were recommended for exclusion. Categories labeled as “other specified” or “unspecified” were automatically excluded, as they lacked specificity. For categories where there was uncertainty among the committee members, these were flagged for focused discussion at the consensus conference. This thorough procedure was intended to streamline conference discussions by narrowing the focus to the most critical categories.
Following the scientific committee’s recommendations, 30 experts in deafblindness—including individuals with lived experience and their intervenors/interpreters, family members, health and social service providers, and policy decision-makers—were invited to provide feedback. From May to August 2024, these experts were provided with the same information from all studies that the committee had used in making their recommendations (the identified categories and their rankings) as well as the committee’s recommendations. Through three online surveys, they were asked to indicate whether they agreed with the committee’s recommendations for each category. If they disagreed, they specified whether the category should be directly included, excluded, or discussed at the conference. Categories achieving 75% consensus were directly included or excluded from the Core Sets, while those that required further input were assigned for discussion at the conference.
The Consensus Conference
On October 7–8, 2024, 26 of the 30 experts who answered the three surveys met in Salou, Spain, to discuss the categories assigned for discussion as a result of the surveys (African Region n = 2; Region of the Americas n = 6; South-East Asian Region n = 3; European Region n = 9; Eastern Mediterranean Region n = 1; Western Pacific Region n = 5; women n = 20). The remaining four experts were unable to attend because of declined visas (3) or personal reasons (1). Observers with an interest in understanding the process were invited to attend the conference, allowing them to witness without actively participating in the discussions or voting. Over 2 days, participants engaged in structured plenary sessions where each unresolved category was reviewed. Using specially prepared voting paddles that included braille labels for accessibility, participants voted for each category’s inclusion or exclusion. Each paddle displayed a thumbs-up for “yes” (inclusion) on one side and a thumbs-down for “no” (exclusion) on the other side, with “in” and “out” braille labels to ensure accessibility for visually impaired participants. Following each discussion, two coordinators collected and recorded the votes to determine consensus. Categories with 75% or higher agreement were confirmed for the comprehensive Core Set, while those below this threshold were excluded, having not reached the required consensus. The process of now further reducing the comprehensive Core Set to its Brief version is currently ongoing. Once both documents have been completed, and the mandates studies have been published, the complete package will be submitted to the ICF Research Branch for ratification and inclusion on their website. The first version of the comprehensive Core Set for deafblindness was presented at a policy day in Barcelona, Spain, on October 9, 2024, and is now available online (Wittich, Dumassais, Jaiswal, Ogedengbe, et al., 2024).
Discussion
The experience of developing the Core Sets for deafblindness has been meaningful and fulfilling for many individuals who participated in this exercise. The initial motivation for this project came from a parent of a deafblind daughter who is professionally engaged in policy development (Lopez i Manzano et al., 2020). He decided to initiate this project, involve other individuals with complementary expertise (Paramasivam et al., 2021), and engage international partners. Throughout data collection, the research team and its network of international collaborators placed great emphasis on the representation, inclusion, and recruitment of individuals living with deafblindness from all regions of the WHO. Considerable resources were set aside to facilitate this representation, both through indemnities paid to participants, the cost coverage of professional sign language interpreters (see Acknowledgment section) and travel means. Interestingly, the logistics of recruitment in low- and middle-income countries were less complicated than initially anticipated; the community partners across all continents were extremely supportive and facilitated this step with outstanding efficiency and efficacy. What emerged as a much more labor-intensive barrier was the process of administering grant funds to pay participants and communication professionals across so many different countries. After several failed attempts to organize bank transfers, the most functional path for payments with minimal banking fees was translations made with Western Union.
The process of core set development is clearly defined (Selb et al., 2015); therefore, researchers are somewhat limited in their creativity within this process. There are, however, potential limitations that need to be considered when interpreting the data from the four studies that are laid out during the preparation phase. The priorities identified in the literature review likely over-represent high-income countries, given the publication bias toward more resources producing more research (Man et al., 2004). Similarly, the data from the expert survey contains more representation from countries that have more abundant numbers of professionals. The qualitative interviews and the multi-center clinical evaluation likely bring the largest bias to the data because of the need for access, expertise, funding, and other resources to facilitate data collection. Finally, it is easier for individuals with sufficient access to funding to participate in an in-person consensus conference that requires travel to Spain. The tendency to under-represent low- and middle-income countries has been shown in other core set developments (Billiet et al., 2024; Wildeboer et al., 2022), and we were acutely aware of these potential limitations, and took measures wherever possible to seek the necessary support; however, it is still likely that the Core Sets presented here are not fully representative of the needs of individuals living with deafblindness, and their allies.
Phase 2: implementation and next steps
The next step is the implementation of the Core Sets into practice, research, and policy development. The application of the Core Sets in the clinical context will depend on factors such as training of professionals in their use; however, our community partners have already taken a leadership role in raising awareness and clarifying the utility of the ICF in service delivery locally, nationally, and internationally. The use of social media for this purpose by our community partners has been specifically impressive and is further supported by the accessibility features that are available on platforms such as Facebook and X. Webinars and short videos made available through Deafblind International have had wide-reaching effects in making the community aware of the Core Sets for deafblindness. Comparison of the coding results among the different preparation phase studies has already pointed to research gaps, such as the lack of research on orientation and mobility, a clear priority for persons with lived experience (Wittich, Dumassais, Prain, et al., 2024). In addition, partners such as the European Deafblind Network have launched efforts to use the Core Sets in the context of policy through, for example, invitations of decision-makers to the launch event in Barcelona. In addition, the team has conducted a comparison analysis of data distributions from the preparation phase to further explore potential differences in categories that emerged in the Global North versus the Global South, or when comparing perspectives according to WHO regions, or by sex or gender (whenever these data are available). Given the large number of congenital diseases and syndromes that can cause deafblindness, the next priority is the development of Core Sets for children and youth with deafblindness, a process that is currently ongoing and supported by the same community partners.
Footnotes
Acknowledgements
We gratefully acknowledge the invaluable contributions of our collaborators and supporters whose involvement has been essential to the success of this project. We thank the European Deafblind Network, World Federation of the Deafblind, Deafblind Ontario Services, Canadian National Institute for the Blind, Canadian Helen Keller Center, Centre National de Ressources Handicaps Rares—Surdicécité, Deafblind Association Nepal, Society of Deafblind Parents Nepal, Sense India, Perkins School for the Blind (Egypt), and the DeafBlind Association of Zambia for their partnerships and assistance with recruitment. We further appreciate the financial support and collaboration provided by Statped Noruega, Royal Kentalis, Able Australia, Centre de réadaptation Lethbridge-Layton Mackay du CIUSSS du Centre-Ouest-de l’Ile-de-Montréal, Institut Nazareth et Louis-Braille du CISSS de la Montérégie-Centre, National Centre for Deafblindness, Federación Española de Sordoceguera, SensesWA, Deafblind Information Australia, and the University of Melbourne. Finally, we are deeply thankful to all those who were key contributors to the scientific portion of this project. Our recognition includes master’s students, PhD candidates, post-docs, and international research assistants, as well as the dedicated research coordinators, caregivers, intervenors, and interpreters who facilitated our work. We also wish to acknowledge the numerous research and health centers that supported us along the way.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: We extend our deepest gratitude to the Canadian Hearing Services, the Centre for Interdisciplinary Research in Rehabilitation of Greater Montreal, Diputació de Barcelona, Deafblind International, Deafblind Ontario Foundation, and the Vision Sciences Research Network funded by the Fonds de Recherche du Québec—Santé for their generous grant support.
