Abstract
Background:
India’s landscape of sub/super-specialization courses is expanding rapidly. Numerous courses spanning various domains of psychiatry exist, and this trend is poised to continue its upward trajectory. We aimed to assess the need for sub/super-specialization courses in psychiatry in India and explore the structural components of the courses.
Methods:
This was a cross-sectional study. A total of 142 psychiatrists/psychiatry residents from India were surveyed using an online questionnaire after approval from the Institutional Ethics Committee.
Results:
“Good” and “intense” need for specialization courses was reported to be highest for child and adolescent psychiatry (68.3%), followed by addiction psychiatry (56.4%) and psychotherapy (55.6%). A 1-year post-doctoral fellowship was reported to be the most preferred course format. Practical examination was suggested to be the preferred summative assessment method for different course formats.
Conclusion:
The availability of sub/super-specialization courses presents an opportunity to enhance psychiatrists’ training in specific areas of interest. Offering a variety of course options enables psychiatrists to select the most suitable program based on their individual requirements and career goals.
There is a perceived need for specialty courses among psychiatrists/psychiatry trainee residents in India. Child and adolescent psychiatry, addiction psychiatry, and psychotherapy specialization courses were the most desired ones. One-year post-doctoral fellowship was reported to be the most preferred course format.Key Messages:
Medicine is an ever-evolving field. Over the years, psychiatry as a field of medicine has also evolved, and new advancements in understanding and practice have occurred. Hence, higher specialty training programs in psychiatry were introduced in various countries, including the United Kingdom (UK), the United States (US), Australia, and India, to keep the students up to date with the advancements in the respective fields. In the UK, specialty training options are general psychiatry, old age psychiatry, forensic psychiatry, child and adolescent psychiatry, psychiatry of learning disability, and medical psychotherapy. 1 In the US, after the 4-year General Psychiatry Residency program, one can opt for various subspecialty fellowships, many of which are accredited by the Accreditation Council for Graduate Medical Education (ACGME). 2 Similarly, Australia has advanced training in the final 24 months of the psychiatry fellowship training program in special areas, including addiction psychiatry, adult psychiatry, child and adolescent psychiatry, consultation-liaison psychiatry, forensic psychiatry, psychiatry of old age, and psychotherapies. 3
India has also observed a surge in the sub/super-specialization courses concerned with different domains of psychiatry in the past two decades. Several 3-year specialization courses (awarding a Doctor of Medicine, DM) are in place, including addiction psychiatry, child and adolescent psychiatry, geriatric psychiatry, and forensic psychiatry. Also, there are post-doctoral fellowship courses in more than 15 areas of psychiatry. 4 These courses were envisaged to help build capacity in specific areas of psychiatry through specialized training of psychiatrists. However, some concerns were raised regarding a rise in specialization courses. 5 In India, there needs to be a better match between the current number of psychiatrists available and those required per the population norms. 6 Thus, it has been argued that specialization courses may limit the psychiatrist’s expertise to the fields they are trained and may result in a reduction in the overall number of psychiatrists managing all kinds of psychiatric disorders. It has also been commented that starting a new course is a “trend” that psychiatry teaching centers are indiscriminately following. Also, there needs to be more consensus regarding the course durations, their pattern, the curriculum, undertaking mandatory research, and holding exit examinations.
Rationale for the Study
There is no published Indian research that explores the perceived need for sub/super-specialization courses in psychiatry. However, it is important to understand its need, the choice of courses, and their structure in the current Indian context. Thus, we conducted this survey to understand the perspectives of psychiatry students and psychiatrists from India on the need for sub/super-specialization courses in psychiatry and to explore the structural components of the curriculum for sub/super-specialization courses in India.
Methodology
This study involved a cross-sectional survey of psychiatrists and students pursuing psychiatry as a career. The estimated sample size was 148 (with the total number of psychiatrists being 10000, 95% confidence level, and 8% margin of error). The survey was administered online through Google Forms. Convenience and snowball sampling methods were used to recruit the participants.
All psychiatrists and students pursuing psychiatry as a specialty or super-specialty course who were aged 18 years or more and willing to provide consent to participate in the study were included in the study. The participant responses were excluded if they were practicing or pursuing psychiatry as a specialty or super-specialty course outside India. The institute ethics committee approved the study (approval number: 117th ECM IIA/P29). The data collection was done between September 2022 and August 2023.
The investigators circulated this survey using their contacts and personal and professional networks. Interested participants were required to consent to participate in the study and provide details regarding their academic profile, work profile, and experience. Their opinion and suggestions were sought on various aspects of sub/super-specialization courses in psychiatry, including exposure to different domains in psychiatry, the need for further training, appropriate duration of courses, methods of training, and evaluation. Responses regarding the perceived need for further exposure to different domains in psychiatry and the need for further training were collected on a 5-item Likert scale from “minimal” to “intense.” It would take about 10 minutes to complete the survey. Informed consent was sought during the introduction of the survey, and completion of the survey was considered consent for participation. The survey did not use any personal identifiers.
Statistical Analysis
Descriptive statistics for the continuous variables are expressed as mean (Standard Deviation, SD) or median (Inter Quartile Range, IQR), while the categorical variables are expressed as frequency (percentage). Statistical analyses were conducted using licensed SPSS for Windows, version 25.0. 7
Results
The total number of participants in the survey was 142. The median age was 34 (30, 40). Males constituted 64.1% of participants and females 35.2%. Of the total participants, 52.1% (n = 74) were MD in psychiatry, 16.9% (n = 24) were DM, and 22.5% (n = 32) were pursuing any of the postgraduate and above courses in psychiatry. 43.7% (n = 62) had up to 5 years of experience, 42.3% (n = 60) had between 6 and 15 years of experience, and 14% (n = 20) had more than 15 years of experience working in the field of psychiatry. 42.3% (n = 60) participants were teachers or faculty in medical institutions, 33.1% (n = 47) participants were students pursuing DPM/MD/DNB/DM/Fellowship courses in psychiatry, while 24.6% (n = 35) participants were working in private institutions/non-governmental organizations (NGOs) or doing private practice. 54 (38%) participants worked in institutions running sub/super-specialty courses in psychiatry, of which 16 were involved in running the course as course coordinators/faculty/senior residents.
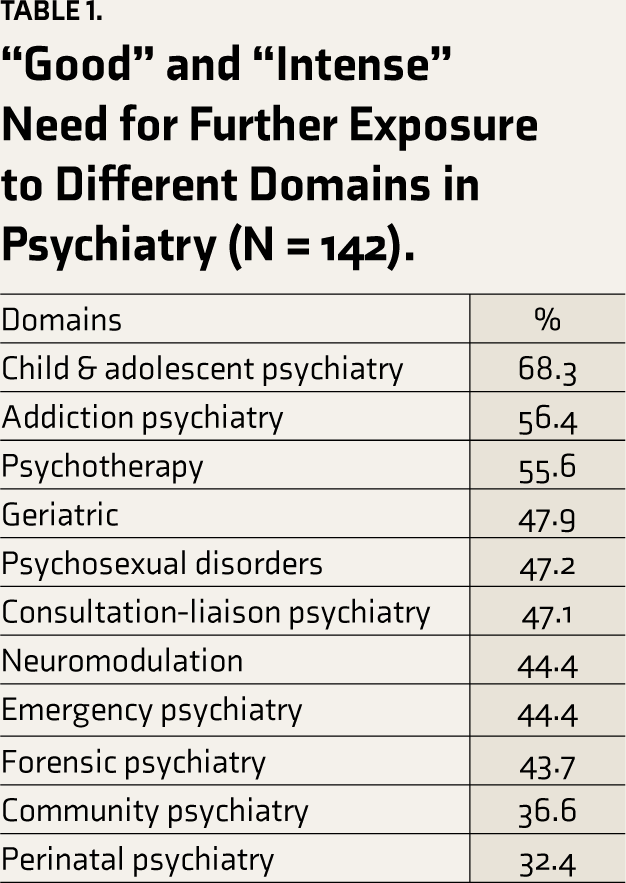
Regarding the perceived need for further exposure to different domains in psychiatry, the “Good” and “Intense” need was reported to be highest for child and adolescent psychiatry (68.3%), followed by addiction psychiatry (56.4%) and psychotherapy (55.6%) (Table 1).
“Good” and “Intense” Need for Further Exposure to Different Domains in Psychiatry (N = 142).
Most participants preferred a 1-year post-doctoral fellowship and a 6-month onsite certificate course (Table 2). Multiple participants also suggested other super-specialty courses in psychiatry, including those focused on neuropsychiatry (n = 6), psychotherapy (n = 4), psychopharmacology (n = 3), rehabilitation psychiatry (n = 2), psychiatry research (n = 2), and personality disorder (n = 2).
Course Formats Suggested to be Appropriate for Subspecialties.
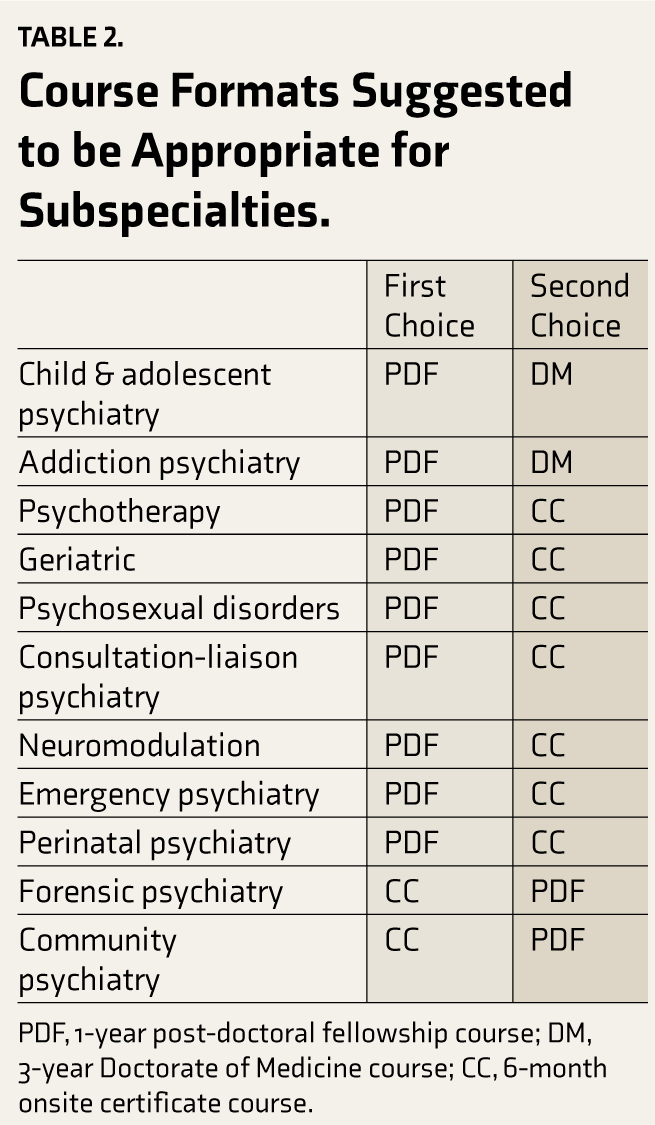
PDF, 1-year post-doctoral fellowship course; DM, 3-year Doctorate of Medicine course; CC, 6-month onsite certificate course.
The majority of the participants suggested clinical exposure (91.5%), case presentations (87.2%), bedside clinics (85.8%), focused group discussions (70.2%), demonstrations (68.8%), seminars (66%), journal clubs (59.6%), and tutorials (53.9%) to be integral teaching-learning methods in sub/super-specialization courses in psychiatry.
There were fewer suggestions for formative assessment methods. However, multiple participants suggested practical assessment/case-based viva (n = 9), demonstration of skills learned (n = 8), periodic MCQ-based exam (n = 5), case-based discussions (n = 4), regular tests and quizzes (n = 3), written exam (n = 2), patient satisfaction feedback form (n = 2), clinical case presentation (n = 2), E-portfolio (n = 2), and Mini CEX (n = 2) for formative assessment.
For summative assessment in DM courses (Table 3), the preferred methods suggested were practical examination (n = 106), written theory examination (n = 96), and thesis/research (n = 88). For PDF courses, practical examination (n = 102), written theory examination (n = 83), and internal assessment (n = 76), while for 6-month certificate courses, practical examination (n = 75), multiple-choice questions (n = 70), and internal assessment (n = 62) were suggested.
Summative Evaluation Methods for the Super-specialty Course.
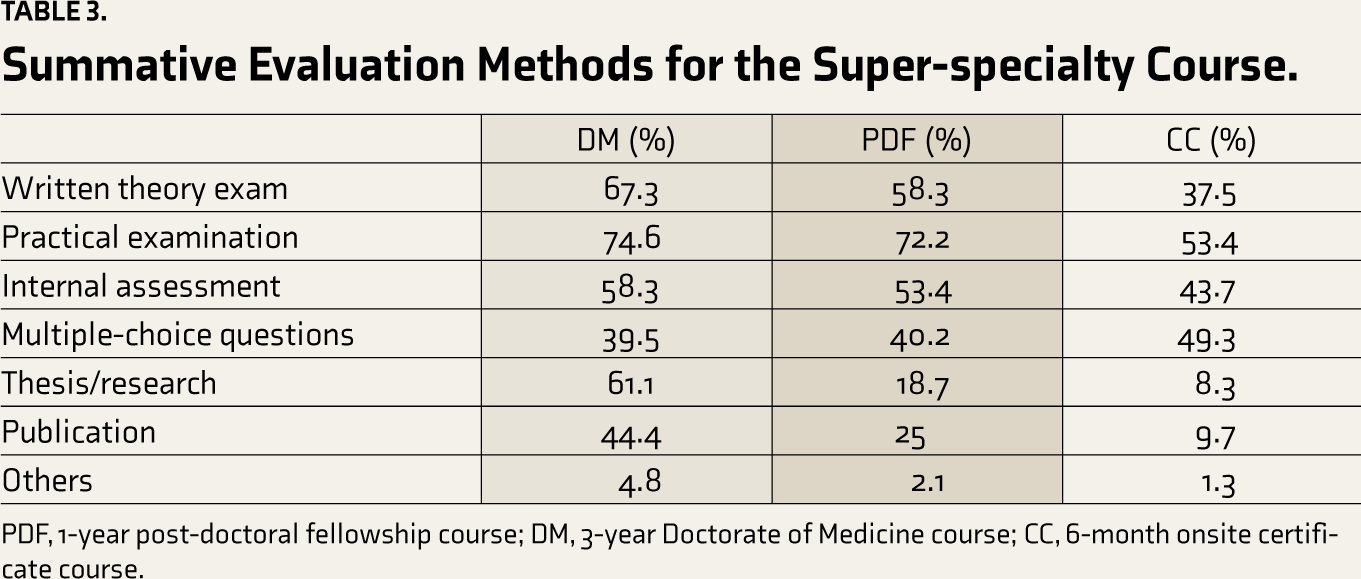
PDF, 1-year post-doctoral fellowship course; DM, 3-year Doctorate of Medicine course; CC, 6-month onsite certificate course.
Discussion
In India, several sub/super-specialization courses in psychiatry have emerged in recent decades. However, questions were raised regarding their need, structure, and usefulness. This survey served to answer some of these queries. It revealed that a significant proportion of psychiatrists and trainee residents feel the need for avenues to gain further training and expertise in diverse specialties within the field of psychiatry. The participants selected all the specialty course options and suggested many more, indicating diversity in the area of interest. More than half the participants desired further training in child and adolescent psychiatry and addiction psychiatry. This may be due to their personal interest or the profession’s demands.8,9 Also, being sensitized by peers might have led them to think of refining their skills and knowledge related to these subdomains, as several DM and PDF courses are ongoing in these fields. Interestingly, over half of the participants also desired additional training in psychotherapy. Clinical psychologists in India predominantly address this particular area. However, many psychiatry departments and institutes in the country need more skilled clinical psychologists; thus, residents’ training in psychotherapeutic skills needs to be better. Similar challenges regarding the shortage of skilled psychotherapists capable of providing training to psychiatrists were also highlighted in other studies. 8 Meanwhile, young psychiatrists increasingly acknowledge the significance of psychotherapy and actively seek opportunities to enhance and refine their psychotherapy skills. Earlier, Grover et al. also reported a major variation in the quality of training at different teaching institutions in diverse domains of psychiatry. 10
One-year PDF courses were the most preferred ones in most of the specialties. A preference for 6-month onsite certificate courses followed it. PDF and certificate courses may be perceived as adequate, especially from the clinical standpoint, to learn and master some key skills quickly and were thus the preferred choice. Moreover, individuals might be reluctant to confine their skills to specific subdomains of psychiatry, which can occur after extensive training in DM courses. In the US, a variety of courses accredited by the ACGME are indeed 12-month fellowship courses. These include fellowships in consultation-liaison psychiatry, forensic psychiatry, geriatric psychiatry, sleep medicine, and addiction psychiatry/addiction medicine. 2 However, the course duration is determined by the objectives and complexity of the domain. The 3-year-long DM courses in India appeal to those aiming to gain comprehensive knowledge and understanding in a specialized domain. In Western countries, several specialty courses in psychiatry extend over multiple years. The US child and adolescent psychiatry fellowship is a 2-year course. 2 In the UK, the higher specialty training program comprises at least 36 months of advanced training. 1
Regarding teaching-learning methods, the participants particularly endorsed various pedagogical approaches, including clinical exposure, case presentations, bedside clinics, and journal clubs. Only a few pedagogical approaches were suggested, including tutorials.
There were a relatively limited number of suggestions concerning formative assessment. This could be attributed to a lower level of awareness among participants regarding formative assessment, which was recently brought into focus by the National Medical Commission (NMC). 11 For summative assessment, while practical examination was commonly recommended for all the courses, written theory examination and thesis/research were also commonly suggested in this survey in DM courses. As getting various research approvals may cost some time, it is understandable why the participants did not commonly recommend thesis/research for the short-term PDF and certificate courses. Internal assessment was commonly suggested for the PDF and certificate courses, suggesting a larger role of internal assessment in evaluation in short-term courses. In Australia, for the Certificate of Advanced Training in specialty courses, one is required to complete the assessments and other defined requirements that include accomplishing entrustable professional activities (EPAs), observed clinical activity, formative and summative In-training assessments (ITAs), written long case history, written case summaries, a final qualitative report and psychotherapy record, and case formulations. In the US, the ACBME-accredited psychiatry subspecialty courses and both the formative and summative assessments are integral to the evaluation procedure. In India, recently, the NMC introduced competency-based medical education (CBME) for medical undergraduates and postgraduates. However, the competencies for sub/ super-specialization courses still need to be properly laid out. Developing competencies and framing curricula for the specialization courses will effectively guide the institutions in running the courses across the country.
Limitations of the Study
This study is subject to several limitations that warrant consideration. Foremost is the relatively small sample size, which limits the generalizability of the findings. Also, this need assessment exercise should have considered stakeholders’ perspectives other than those of psychiatrists and psychiatry residents. Additionally, a limitation stems from the restricted participation of individuals directly engaged in the administration of sub/super-specialization courses. Furthermore, several key areas and methodologies highlighted in the current NMC curricula, such as formative assessment, needed to elicit more responses from participants. This could be attributed to the novelty of these concepts concerning medical education, thus resulting in limited feedback from survey respondents.
Conclusion
This survey provided crucial insights into the need for specialization courses in psychiatry. It shed light on several key aspects, including the necessity of such courses, their ideal duration, and the structural components necessary for an effective curriculum. This research provides a framework for institutions to tailor their sub/super-specialization programs to better align with the evolving demands in psychiatry. The provision of sub/super-specialization courses provides an opportunity for psychiatrists to further their studies in specific areas of interest. However, to enhance psychiatric education in India and produce well-trained psychiatrists, it is essential to standardize specialty courses.
Footnotes
Data Availability Statement
The data that support the findings of this study will be provided on request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Declaration Regarding Use of Generative AI
AI was not used in writing this manuscript.
Ethical Approval
The study received approval from the Institutional Ethics Committee.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors acknowledge the grant provided by Indian Teachers of Psychiatry (IToP) and Minds United for Health Sciences and Humanity Trust for carrying out this work.
Informed Consent
Informed consent has been obtained from all the participants, prior to inclusion in the study.
Prior Presentation
Findings of the study were presented as a webinar at the Indian Teachers of Psychiatry (IToP) forum in 2023.
