Abstract
Background:
South Asia generally reports low levels of amphetamine-type stimulant (ATS) use, with few studies on the pattern of ATS use. We assessed the pattern of ATS use and associated high-risk behavior in Manipur, a north-eastern state of India.
Methods:
209 adult male ATS users (mean age 28.8 years) from three districts of Manipur were interviewed. Data were collected on the patterns of high-risk behavior with ATS use, health consequences, and help-seeking. The severity of use with various substances was assessed using the Alcohol, Smoking, and Substance Involvement Screening Test (ASSIST). Depression and anxiety were assessed by the Patient Health Questionnaire (PHQ-9) and Generalized Anxiety Disorder (GAD-7) scale, respectively.
Results:
The mean duration of ATS use was 3.7 years (SD 2.3). The majority used ATS almost daily (88%) and depended on ATS (77%). Methamphetamine (99.5%) was the most used ATS orally. Around 87% also suffered from opioid dependence. About 76% injected drugs, most commonly heroin. Almost three-fourths (78%) used ATS before their sexual intercourse, 31% of whom did not use condoms. Most reported physical problems with ATS and had above-cut-off scores on PHQ-9 and GAD-7. The majority (95%) reported that they could procure ATS easily. Also, the majority (93%) had thought of quitting ATS use.
Conclusions:
Most ATS users start using ATS at a young age and have comorbid other drug use, including heroin. ATS use is associated with various physical and psychological problems. Focusing on ATS use in India and developing strategies to address this problem is essential.
Through the collection of data from over 200 users from three districts, the study highlights the problems ATS users face in Manipur. The study highlights that methamphetamine tablet smoking is the choice of ATS. Almost all the participants reported concomitant use of other substances along with the ATS use. Most participants reported physical and mental health problems due to ATS use.Key Messages:
Amphetamine-type stimulants (ATSs) are used worldwide, with approximately 0.7% of the world’s population aged 15–64 reported to have used amphetamines and 0.4% having used ecstasy in the past year. 1 There are signs of growing use of ATSs, and this is reflected in the increasing number of individuals seeking treatment for ATS addiction, which corresponds to the rise in ATS seizures. 1 Studies have shown increased use of ATSs in various parts of the world, such as North America,2,3, Australia 4 , and Iran. 5 The past-year use of amphetamines in persons aged 15–64 years was the highest in North America (3.9%), followed by Australia and New Zealand (1.3%) in 2020. Numerically, the largest population with amphetamine use is in North America (12.5 million), followed by the East and Southeast Asia regions (10 million). 1 ATS use is associated with a wide range of adverse effects, including physical, psychological, and increased risk of high-risk behaviors.6,7 Treatment for ATS use reduces substance use and decreases HIV-related risk-taking behavior. 8
India is one of the most frequently mentioned countries involving the seizure of illicit shipments of ephedrine and pseudoephedrine, the precursors for producing ATSs. 9 Despite various reports on ATS use, there are few reliable epidemiological data concerning the prevalence and patterns of ATS usage in India. A nationwide survey assessing the magnitude of substance use in India reported that ATSs are used by 0.2% of the country’s population aged 10–75 years, of which 0.02% suffer from dependence on ATSs. 10 However, this survey did not provide detailed insights into the specific patterns of ATS use in India. Another qualitative study conducted across five Indian states with a limited sample of 100 ATS users found that ecstasy and methamphetamine pills were the most commonly used ATSs. 11 It is essential to assess the pattern and trends of ATS use to effectively design and implement appropriate interventions that reduce the adverse consequences of the emerging use of this drug.
Manipur, located in the north-eastern region of India, shares international borders with Myanmar, one of the world’s largest producers of heroin. 12 The North-eastern states, including Manipur, have been witness to drug use problems in their region. The recent national survey on the magnitude of substance use in India also records a high prevalence of significant substances in north-eastern states. All the north-eastern states recorded a prevalence of opioid use and dependence higher than the national average (2.1% opioid use and 0.26% opioid dependence). Some states, such as Manipur (14%), Nagaland (25%), Mizoram (26%), Arunachal Pradesh (22%), and Sikkim (19%), have a prevalence of opioid use in double digits. The north-eastern region, especially Manipur, Nagaland, and Mizoram, also has numerous people who inject drugs (PWID), and the HIV epidemic in these states is fueled by drug use, mostly injection of heroin. 13 Anecdotal reports from interactions with service providers working with people who use drugs (PWUD) suggested that methamphetamine has become common in Manipur and is increasingly used by PWID, commensurate with the increasing production of methamphetamine in Myanmar and other countries in Southeast Asia. 14 Hence, the present study was planned to assess the pattern of ATS use in Manipur, high-risk behaviors, adverse consequences associated with ATS use, and the treatment experience and needs of ATS users.
Methods
The study was conducted in three districts of Manipur—Imphal, Churachandpur, and Thoubal—after approval from the institutional ethics committee of the corresponding author (IEC-1159/06/11/2020). The data were collected from November 2020 to January 2021. A team of data collectors who had prior experience working with PWUD collected data from the selected districts. They underwent training on study methods and data collection tools before beginning the data collection. The participants were recruited through snowball sampling. Initially, ATS-using individuals known to the data collectors were recruited. These recruited participants were further asked to refer other ATS-using individuals from their network for study participation. To be eligible for participation, the ATS users had to be males aged 18 years who had used ATS at least once in the past three months. We excluded those unwilling or unable to participate in the interview. The interview was conducted face-to-face at a mutually convenient place in a single session after getting informed consent from the participants. Each interview lasted for 30–45 minutes. The data were collected on a mobile device (smartphone or tablet) using the RedCap software.
Data Collection Instruments
The study participants were assessed using the following data collection instruments:
Survey questionnaire: A questionnaire was prepared to collect information from the participants regarding their socio-demographic characteristics, the pattern of ATS and other substance use, injecting drug use, adverse health consequences, and help-seeking behavior. Alcohol, Smoking, and Substance Involvement Screening Test (ASSIST) was used to screen for the use of substances, including tobacco products, alcohol, cannabis, cocaine, ATSs, sedatives, and sleeping pills (benzodiazepines), hallucinogens, inhalants, opioids, and “other” drugs.
15
ASSIST determines a risk score for each substance that falls into a “low-,” “moderate-,” or “high-”risk category. Scores in the high-risk category reflect dependence on a particular substance. Patient Health Questionnaire (PHQ-9) and Generalized Anxiety Disorder Assessment (GAD-7): PHQ-9 consists of nine items used to screen for depression in the community setting. Each item can be scored from 0 (not at all) to 3 (nearly every day). The PHQ-9 score can range from 0 to 27.
16
Similarly, GAD-7 is a seven-item scale used to screen for generalized anxiety disorder in the community setting. The cut of 5, 10, and 15 points indicates mild, moderate, and severe anxiety levels of GAD-7, respectively.
17
Statistical Analysis
The quantitative data were managed through RedCap software and analyzed statistically through licensed SPSS 21.0 version software (IBM Corp. 2012, Armonk, NY, USA). The quantitative variables were summarized as mean (SD) and median (interquartile range [IQR]) as appropriate, while the categorical variables were summarized as frequencies and percentages.
Results
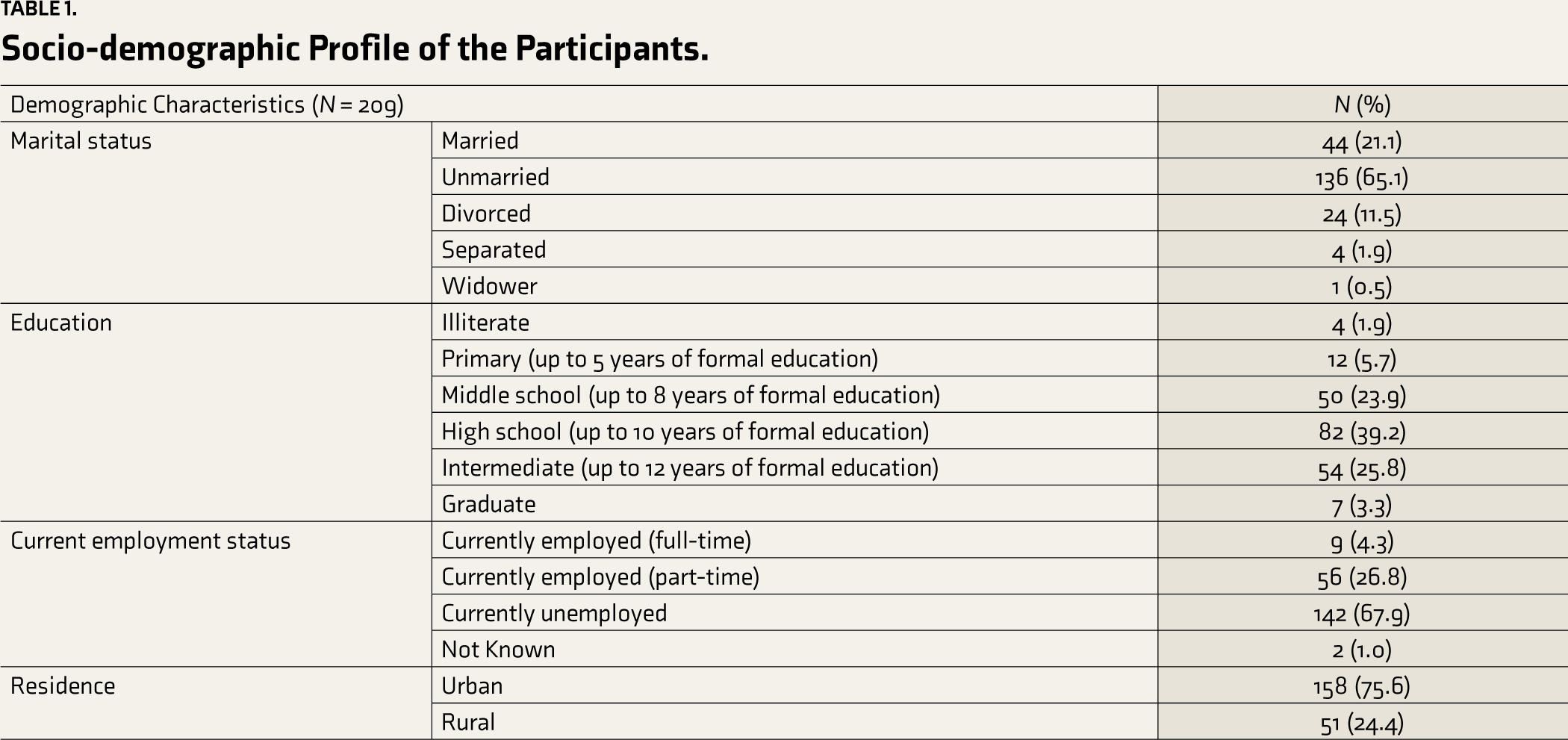
The study recruited 209 participants within the designated data collection timeframe. About 58.9% (n = 123) of the participants were from Imphal, 31.6% (n = 66) were from Churachandpur, and 9.6% (n = 20) were from Thoubal. The socio-demographic characteristics of the participants are shown in Table 1. The average age of the participants was 28.8 years (SD 6.5). The median family income was ₹20,000 per month (IQR 15,000, 35,000). Almost all participants reported tobacco use in their lifetime (97.1%, n = 203). The majority of the participants also reported the use of opioids (96.2%, n = 201). ASSIST scores indicated opioid dependence in 87.1% of the participants (n = 182), alcohol dependence in 23.4% of the participants (n = 49), and sedative dependence in 12.9% of the participants (n = 27). Table 2 shows the substance use–related characteristics.
Socio-demographic Profile of the Participants.

Details of the Use of Other Substances by the Participants (N = 209).
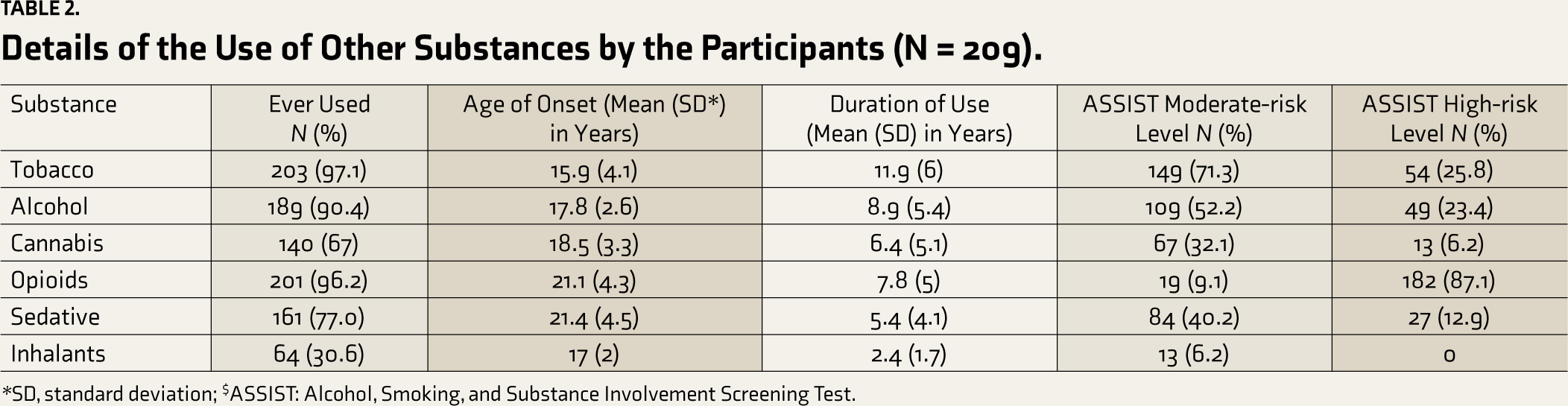
*SD, standard deviation; $ASSIST: Alcohol, Smoking, and Substance Involvement Screening Test.
ATS-related Characteristics
The average age of onset of ATS use was 25.1 years (SD 5.9), and the mean duration of ATS use was 3.7 years (SD 2.3). Most participants used ATSs daily or near-daily (88.5%, n = 185) in the past three months. Methamphetamine tablet (referred to as “WY,” short form for World Is Yours, locally) was the most common ATS used by the participants (99.5%, n = 208) in their lifetime. The other ATSs used by the participants in their lifetime included methamphetamine crystals (“ice”) in 1.9% (n = 4) and MDMA (“Ecstasy”) in 1.4% (n = 3). The most common route of ATS use was inhalation or smoking (99.5%, n = 208). Only one participant reported using ATS by injection. Most participants (76.6%, n = 160) scored in the “high-risk” category of ASSIST for ATS use, indicating dependence. The remaining 23.4% (n = 49) participants scored in the “moderate-risk” category, indicating hazardous or harmful use of ATSs.
The most common reason for starting ATSs was the “curiosity to experience its effect” (96%, n = 201), followed by “peer influence” (89%, n = 186). Other reasons for initiating ATS included “peer pressure” (31.6%, n = 66), “improving low mood or anxiety” (12.9%, n = 27), or “improving sexual performance” or “enjoying sex” (21.1%, n = 44). About 4.8% (n = 10) resorted to illegal activities to procure ATSs. The majority (95.3%, n = 199) reported that it was pretty easy for them to procure ATSs. Most participants consumed ATSs with their peers (69.4%, n = 145), while 30% (n = 64) reported that they took ATS alone. The familiar places of ATS consumption were the drug dealer’s place (39.7%, n = 83), friend’s house (29.7%, n = 62), or any other secluded area (21.1%, n = 44).
Health and Socioeconomic Problems Due to ATS Use
The majority of the participants (86.6%, n = 181) reported that they experienced physical problems due to ATSs. The most common physical problems reported by the participants were weight loss (84.2%, n = 176) followed by loss of appetite (86.6%, n = 181), respiratory problems (42.1%, n = 88), cardiovascular issues (29.2%, n = 61), injuries due to road traffic accidents (21.1%, n = 44), injection-related complications (0.5%, n = 1), and overdose (0.5%, n = 1). Around 10.5% (n = 22) of the participants reported that they had mental health problems before ATS use. Assessment with PHQ-9 showed 20.6% (n = 43), 35.9% (n = 75), 13.9% (n = 29), and 22% (n = 46) ATS users had mild, moderate, moderately severe, and severe depression, respectively. Similarly, assessment with GAD-7 revealed mild, moderate, and severe levels of anxiety in 27.8% (n = 58), 34.9% (n = 73), and 5.7% (n = 12) ATS users, respectively. About 52% (n = 23) of married participants (n = 44) reported separation or divorce from their spouses, while families disowned 2% (n = 4) of the participants due to their ATS use. About 15% (n = 31) lost their job, and 42% (n = 88) dropped out of studies due to ATS use. Most participants (73%, n = 153) reported a loss of standing/respect in society due to their ATS use. Also, most participants (86%, n = 179) were financially dependent on their family members due to ATS use. About 26% (n = 54) of the participants had committed illegal acts, including selling drugs, to support their substance use. More than half of the participants (54.5%, n = 114) reported being caught by police when procuring or consuming ATSs. One participant reported that he was jailed under the narcotic law for possessing or selling ATSs. Two participants were incarcerated in their lifetime. Table 3 describes the psychological and socio-occupational problems experienced by the ATS users.
Psychological and Socio-occupational Problems Related to ATS Use.
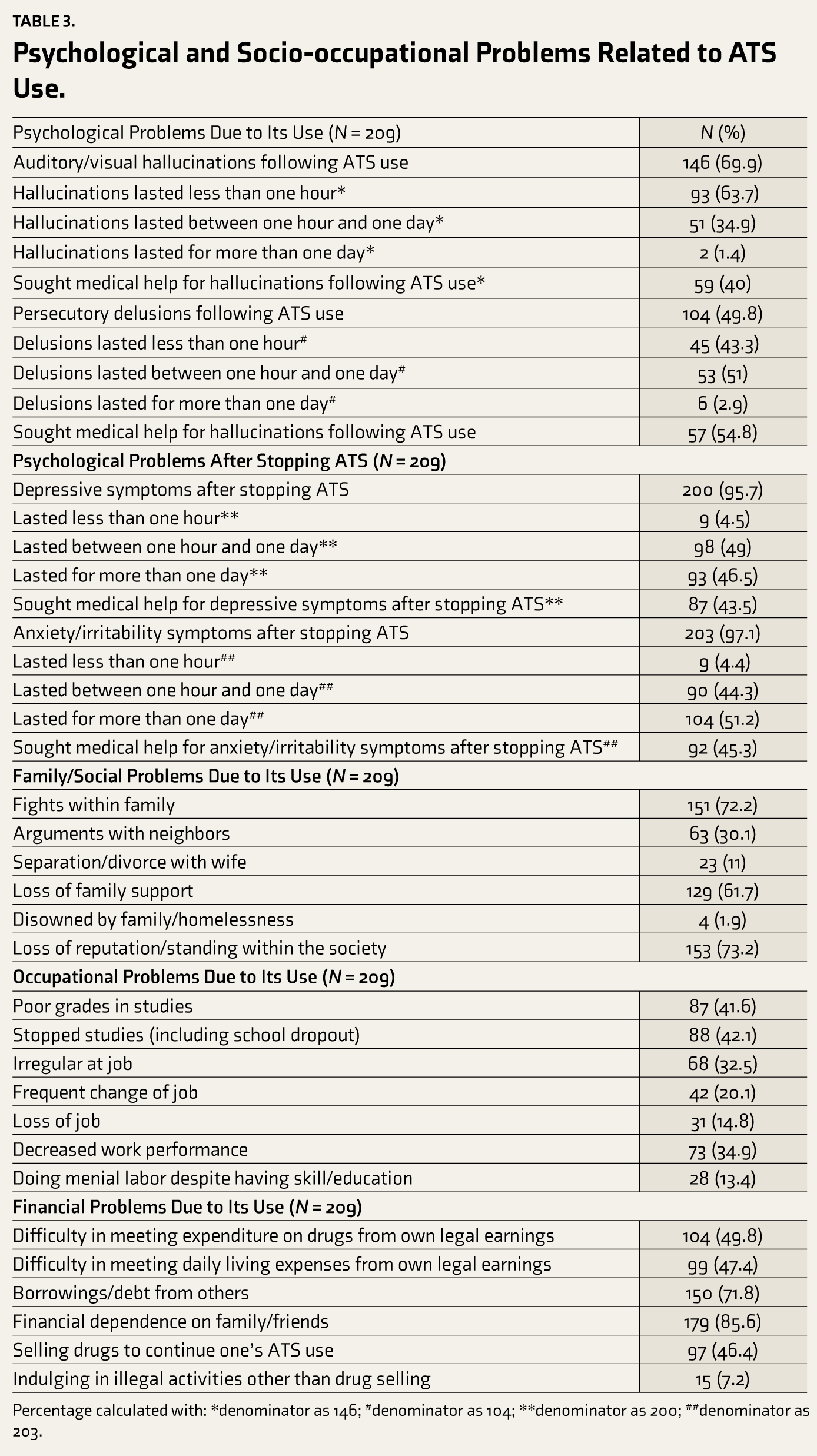
Percentage calculated with: *denominator as 146; #denominator as 104; **denominator as 200; ##denominator as 203.
High-risk Behavior with ATS Use
About 78% (n = 163) of the participants reported using ATSs before sexual intercourse, and 69% (n = 113) reported using condoms during sexual intercourse under the influence of ATSs. Only one participant agreed to using ATSs along with his sex partner. About 25.4% (n = 53) of the participants reported having sexual intercourse with female sex workers (FSW) under the influence of ATSs in their lifetime. Around 2.4% (n = 5) of theparticipants reported having sexual intercourse with a same-sex partner under the influence of ATSs, of which two reported ATS use together with their partner during sexual intercourse. Almost three-fourths (76.1%,n = 159) of the participants reported injecting drugs for non-medical or recreational purposes in their lifetime. Of these, most participants (71.7%, n = 114) reported heroin as the predominant drug for injection in the past three months. Only one participant reported injecting ATS in his lifetime and had shared injecting equipment when injecting ATS. Around 6.2% (n = 13) of the participants reported that they tested positive for HIV, and 19.6% (n = 41) tested positive for hepatitis C virus.
Treatment-seeking Efforts to Quit ATS Use
Most participants (93.3%, n = 195) reported that they had contemplated quitting ATS use at some point. However, only approximately 56.9% (n = 119) of the participants had sought treatment. Around 19.6% (n = 41) had sought treatment within the past three months. The primary motivations for seeking treatment in the past included addressing ATS withdrawal symptoms (56.9%, n = 119) and discontinuing ATS use altogether (56.0%, n = 117). The most frequented treatment facilities were government healthcare facilities (31.1%, n = 65) and private rehabilitation centers (31.1%, n = 65).
Discussion
The use of stimulants, including ATSs, is sporadically found in the country. 10 The present study highlights the pattern of ATS use in the north-eastern state of Manipur, India, by assessing 209 ATS users for their pattern of ATS use, comorbid substance use and psychiatric illness, problems faced in various domains, and treatment-seeking efforts. This study assumes importance in the absence of extensive data from India.
The overwhelming choice of ATSs in the study participants was methamphetamine tablets locally called WY, which is smoked. The use of crystalline methamphetamine or ecstasy was almost nil. This pattern of use is similar to that seen in other countries of Southeast Asia, including Myanmar, Thailand, and Malaysia, where methamphetamine tablets are the most common ATSs used. 18 The choice of a particular ATS for use may be governed by the availability of that product in the area. It is known that the region surrounding Manipur is a central hub for illicit methamphetamine production. The Golden Triangle (confluence area of Laos, Myanmar, and Thailand) is a significant source of methamphetamine tablets. 19 The type of ATS is also essential, as different ATS preparations are known to have different physical and psychological effects. ATS users often experience psychological effects such as euphoria, increased alertness, increased libido, confidence, and high energy levels. 20 ATS use can also lead to various cardiovascular effects, such as elevated heart rate, increased respiratory rate, and elevated blood pressure. Methamphetamine enhances cognitive and psychomotor performance, increases participants’ desire to retake the drug, and disrupts sleep. 21 It was also interesting to note that most participants felt it was easy to procure ATSs, as easy as cannabis or heroin. Procurement of methamphetamine tablets was not an issue for most participants in our study. It is of concern that easy availability may lead to large-scale use of ATSs in Manipur and can also spread to other parts of the country.
Most of the participants in our study were using ATSs daily in the past three months, and three-fourths were suffering from ATS dependence. A study from the USA reported that 27% of methamphetamine users had used ATSs for 200 days or more in the past year, and 53% of past-year methamphetamine users met the diagnostic criteria for methamphetamine use disorder. 22 Almost all of the participants in our study reported concomitant use of other substances and ATSs. The most common substance used along with ATSs was heroin, which 87% of the participants used. A majority of these individuals were also suffering from opioid dependence. The use of opioids and methamphetamine together is considered more risky than using either substance alone. Shearer et al. showed that the use of both opioids and methamphetamine is associated with a higher prevalence of injection needle use, consequent viral hepatitis, severe mental illness, and chronic physical conditions compared to either opioid or methamphetamine use alone. 23 Studies also show that the use of methamphetamine among treatment-seeking opioid users has increased worldwide.24,25 A previous study in the region reported that individuals preferred to use ATSs to increase productivity. 11 There could be various reasons for the concomitant use of ATSs and heroin. Some users report concomitant use to get an additive or synergistic high. In contrast, some others use ATSs to balance the effect of opioids, which might make them drowsy by taking ATSs as it might make them active so they can function normally. Some studies report users using methamphetamine to provide them energy to make money for purchasing heroin as well. 26
In this study, ATS users reported auditory or visual hallucinations and fear or suspicion of others after using ATSs. A study assessing methamphetamine users for six months found a twofold increase in the risk of psychotic symptoms in methamphetamine users, while a systematic review found that amphetamines doubled the odds of developing psychosis.27,28 However, ATS-induced acute psychosis has been shown to recover rapidly and appears to resolve with abstinence.29,30 Studies on rats exposed to amphetamine found changes in their prefrontal cortex, which is considered to be a precursor to psychosis. 31 A systematic review showed that the frequency of use and severity of methamphetamine dependence were associated with the occurrence of psychosis. 32 In the present study, 92% of ATS users had depressive symptoms, and 68% had anxiety symptoms. In a study conducted on the Chinese population, 42% of ATS users reported depressive symptoms. 33 Earlier studies on the Australian and U.S. population reported that 79% and 42% of ATS users, respectively, had depression.34,35 The odds of developing depression are doubled with the use of ATS. 28 Depression can lead to a vicious cycle of ATS use as a form of self-medication for their stimulant effect, which can, in turn, worsen depression. 36 The present study highlights the high prevalence of comorbid psychiatric symptoms in ATS users, which must be borne in mind during the treatment of ATS use disorder.
Most participants reported they thought of quitting ATS, and more than half sought treatment. A meta-analysis by Cumming et al. showed that embarrassment or stigma due to the use of ATS was considered the main psychosocial barrier to treatment access. It also showed the preference to quit alone without treatment and not addressing the need for treatment as other barriers to assessing ATS treatment. 37 Studies have shown that individuals with chronic methamphetamine use often encounter challenges in effectively focusing on their goals and intentions. The impairment in cognitive functions could affect their ability to maintain abstinence and seek treatment. 38 A sizeable proportion of participants in our study were vulnerable to high-risk behavior. Almost three-fourths of our participants were injecting drugs, especially heroin. Most participants also reported using ATS before their sexual intercourse.
Additionally, one-fourth of the participants reported having sexual intercourse without condoms under the influence of ATSs in the past month. ATSs were also used in a sexual context to enhance and prolong sexual pleasure and reduce sexual inhibition. 39 Studies have shown that methamphetamine use is associated with unprotected sexual intercourse, which increases the risk of sexually transmitted infections.40-43 This finding is of importance to the HIV prevention program in India as PWIDs in India have the highest rates of HIV. The rate of HIV among PWIDs in Manipur is 7.6%. While the rate of use of new needles and syringes is more than 80%, only half of the PWIDs in Manipur reported using condoms during sexual intercourse. 44 There is the likelihood of increasing HIV rates in PWIDs using ATSs due to risky sexual behavior, often not adequately targeted in needle syringe programs that focus more on injecting practices.
This study has its limitations. As the participants were selected by the snowballing method, the findings may be due to the initial sample chosen, which might only be generalizable to some ATS users in Manipur. Similarly, the study design did not allow an estimate of the prevalence of ATS use in Manipur. Nevertheless, this is one of the first studies on the pattern and profile of ATS use in Manipur, India, and the findings underscore the need to address this new and emerging psychoactive substance use in India.
Conclusions
Most ATS users start using ATSs at a young age and often use ATSs along with other drugs, such as heroin. ATS use is associated with various physical and psychological problems. There is an urgent need to estimate the extent of ATS use in India, develop strategies to address the issue of ATS use, and build the service providers’ capacity to manage ATS use disorders.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Declaration Regarding the Use of Generative AI
None used.
Ethical Approval
Ethical approval was obtained from the institutional ethics committee of the corresponding author (IEC-1159/06/11/2020).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was funded by Alliance India, New Delhi, India. The first author received financial support for the research. The authors did not receive funding for authorship and/ or publication of this article.
Patient Consent
Informed consent was obtained from the participants.
