Abstract
Background:
Suicide is common among persons with physical disabilities as they face several physical, social, psychological, and economic problems. They are at risk for suicidal thoughts, behaviors, and death by suicide. We aimed to systematically review empirically published articles and identify the associated factors of suicidal ideation and suicide attempts in persons with physical disabilities.
Methods:
A systematic search was carried out on the literature published from January 1, 2000 to January 19, 2023 in PubMed, Cochrane, Web of Science, Google Scholar, Shodh Ganga, and so on. All the synonyms of keywords or MeSH terms for suicidal ideation, suicide attempt, and physical disability were used. Two hundred thirty-six articles were found, and after following inclusion and exclusion criteria, 12 remained.
Result:
The associated factors of suicidal behavior were disability status (11/12 studies), burdensomeness (8/12 studies), felt stigma (4/12 studies), depressive symptoms (6/12 studies), loneliness (2/12 studies), lack of social and emotional connectedness (2/12 studies), long-term physical or mental disability (2/12 studies), congenital disability (1/12 studies), and aggression (1/12 studies).
Conclusion:
Timely, evidence-based, low-cost interventions can provide great assistance and address the specific needs of this vulnerable population as they have higher risk for suicidal behavior.
Suicide is a serious public health issue. Worldwide, suicide is a leading cause of death among disabled people. According to Diagnostic and Statistical Manual for Mental Disorder, 5th edition (DSM-5), Suicidal Behavior Disorder (SBD) is defined as a self-initiated sequence of behaviors by an individual who, at the time of initiation, expects that the set of actions will lead to their own death. 1 Suicidal ideation is a tendency toward thoughts, ideas, or ruminations about ending one’s life, ranging from thinking that one would be better off dead to implementing elaborate plans. 2 Suicide attempts can be defined as a specific episode of self-harming behavior, undertaken with the conscious desire to end one’s life. 2 “Suicide acceptability” isa personal assessment of whether, in a certain setting or community, dying of suicide is a reasonable course of action. 3
Disability is an umbrella term covering impairments, activity limitations, and participation restrictions. Impairment means functional or structural problems in the body; activity limitation means difficulty encountered by an individual in executing a task or action; and participation restriction means problem experienced by an individual in involvement in their life situations. 4 Thus, disability is quite complex as it is an interplay between an individual’s physique and the community. In India, out of 121 crore population, 2.68 crores have a disability, of which 1.5 crore are males and 1.18 crore are females. 5 The 2011 census reported that in India, 20% of disabled persons have a physical disability. Physical disability is a condition of decadent motor functions, loss of physical capacity, and inability and impairment to perform bodily activities that include walking, moving hands and arms, sitting and standing, and regulating muscles. 6
In Iranian disabled males, the prevalence of suicidal ideation, and single and multiple attempts of suicide were 27.7%, 16.9%, and 18.1% respectively, and the corresponding rates in disabled females were 72.3%, 83.1%, and 80.4% 7 Moreover, it had been reported that 71% of those who attempted suicide had severe mental disability, whereas only 31% had physical disability. 8 People with various types of functional disabilities are at elevated risk for suicide-related outcomes compared to people without disabilities. Moreover, severe disability, odd physical health, and complex activity disability have been associated with suicide attempts.7,9
Physically disabled persons have normal intellectual and cognitive abilities, but the disabled status is an obstacle to achievement in their lives. This leads to self-blame, self-harm, and psychopathology such as anxiety, stress, and depression, and finally, suicidal ideation.10–12 Against this background, the present study aimed to systematically review empirically published articles and identify the associated factors of suicidal ideation and suicide attempts in them.
Methods
Design and Registration
The study followed the Preferred Report Items for Systematic Review and Meta-Analysis (PRISMA) checklist for selecting and screening the articles. 13 It was also registered on the International Prospective Register of Systematic Reviews (PROSPERO), and the registration number is CRD42023402121. 14
Search Strategy
A systematic search was carried out on the literature published from January 1, 2000 to January 19, 2023 in PubMed, Web of Science, Google Scholar, Cochrane, and Shodh Ganga (Figure 1). In the first step, the free text was searched via keywords such as ((suicide attempts) AND (suicidal ideation) AND (physical disability) AND (locomotor disability)), and the detailed search strategy is explained in Table 1. All the possible synonyms of keywords were included in the free text search. Database-specific subject headings and detailed search strategies were constructed using appropriate Boolean operators. Appropriate filters were used. Only electronic and manual searches (in the departmental library of the university) were performed to collect the articles in the systematic review.
Search Strategy.

Flowchart of the Selection Process and Distribution of Selected Articles.
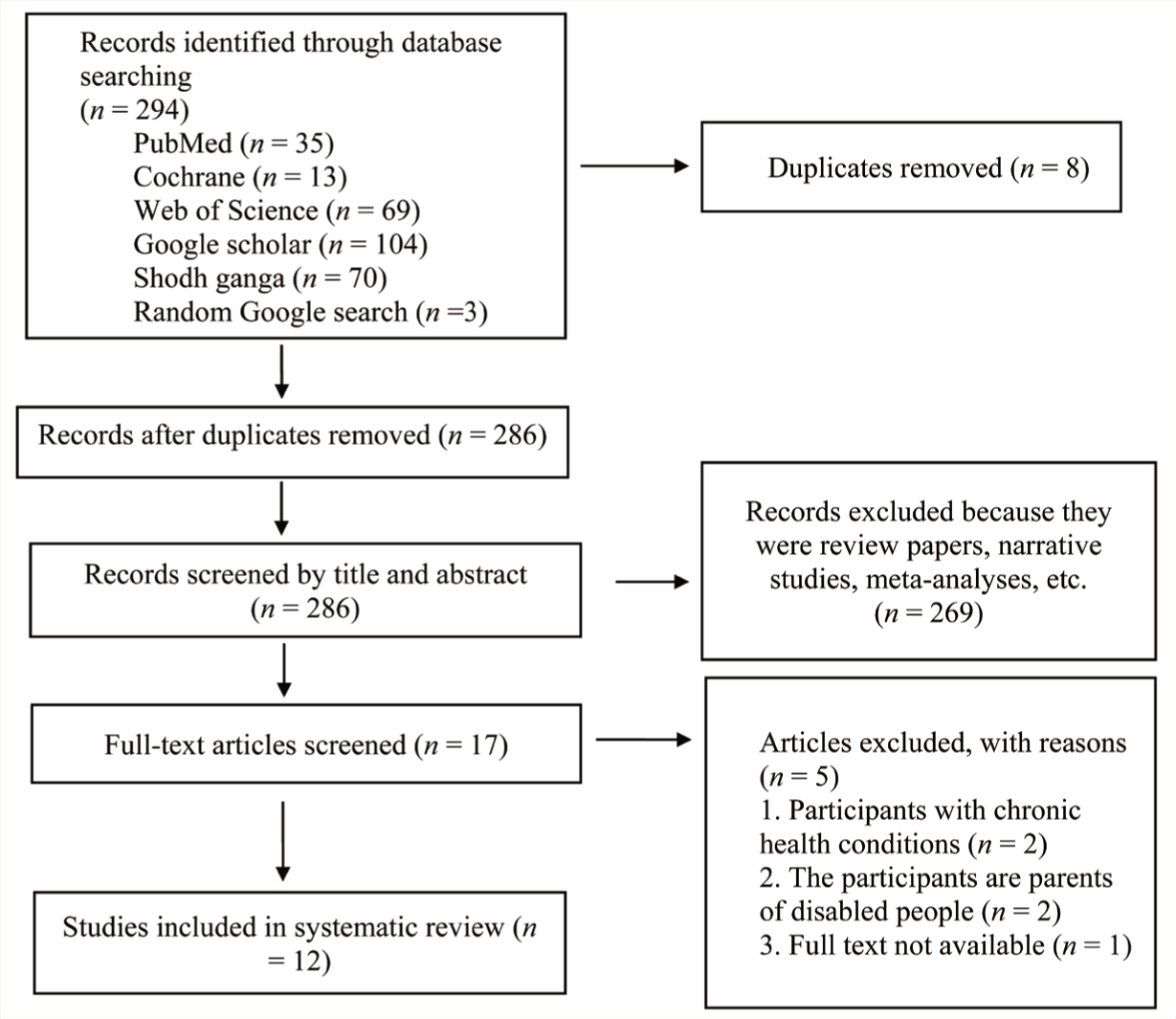
Inclusion and Exclusion Criteria
Primary correlational studies that evaluated suicidal ideation and attempts in adult samples of people with physical disabilities aged above 15, published in English, between January 1, 2000 and January 19, 2023 were included. Research on children below 15 and on people with sensory impairment, multiple disabilities, or psychiatric disorders, review articles, and meta-analyses were excluded.
Risk of Bias (Quality) Assessment
The methodological quality of the included studies was evaluated for each individual element of the study, including participant selection, outcome evaluation, sufficiency of follow-up, and data completeness. The Newcastle-Ottawa Scale (NOS) was used to assess the quality of evidence. 15 The quality of studies was then graded on a scale of “lowest” to “highest” possible quality, with the highest quality deemed the greatest possible degree of proof for an association.
Results
The 12 studies incorporated in the review had the highest quality. They are summarized in Table 2.
Studies Assessing Suicidal Ideation and Suicide Attempts Among Persons with Physical Disability.
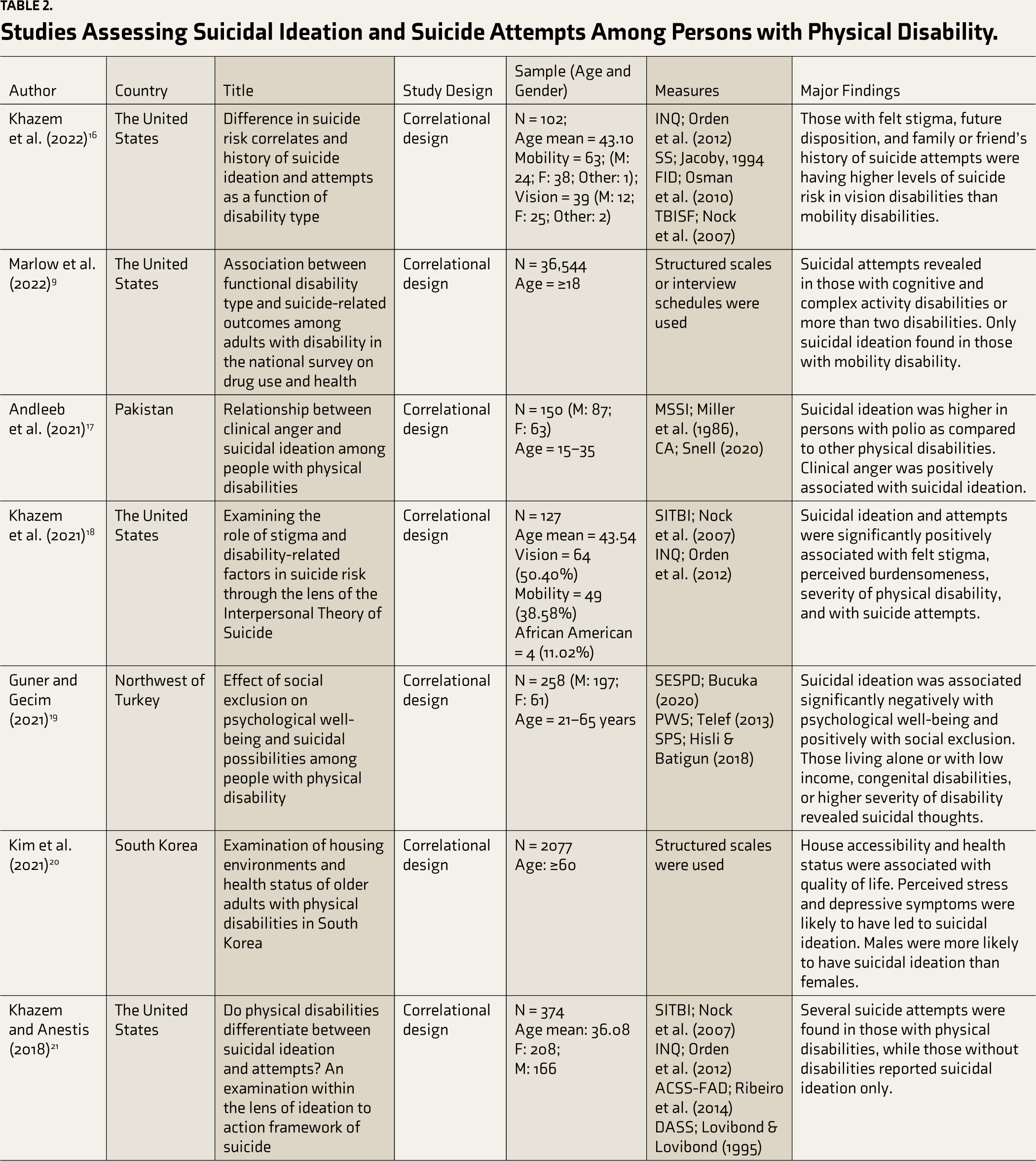
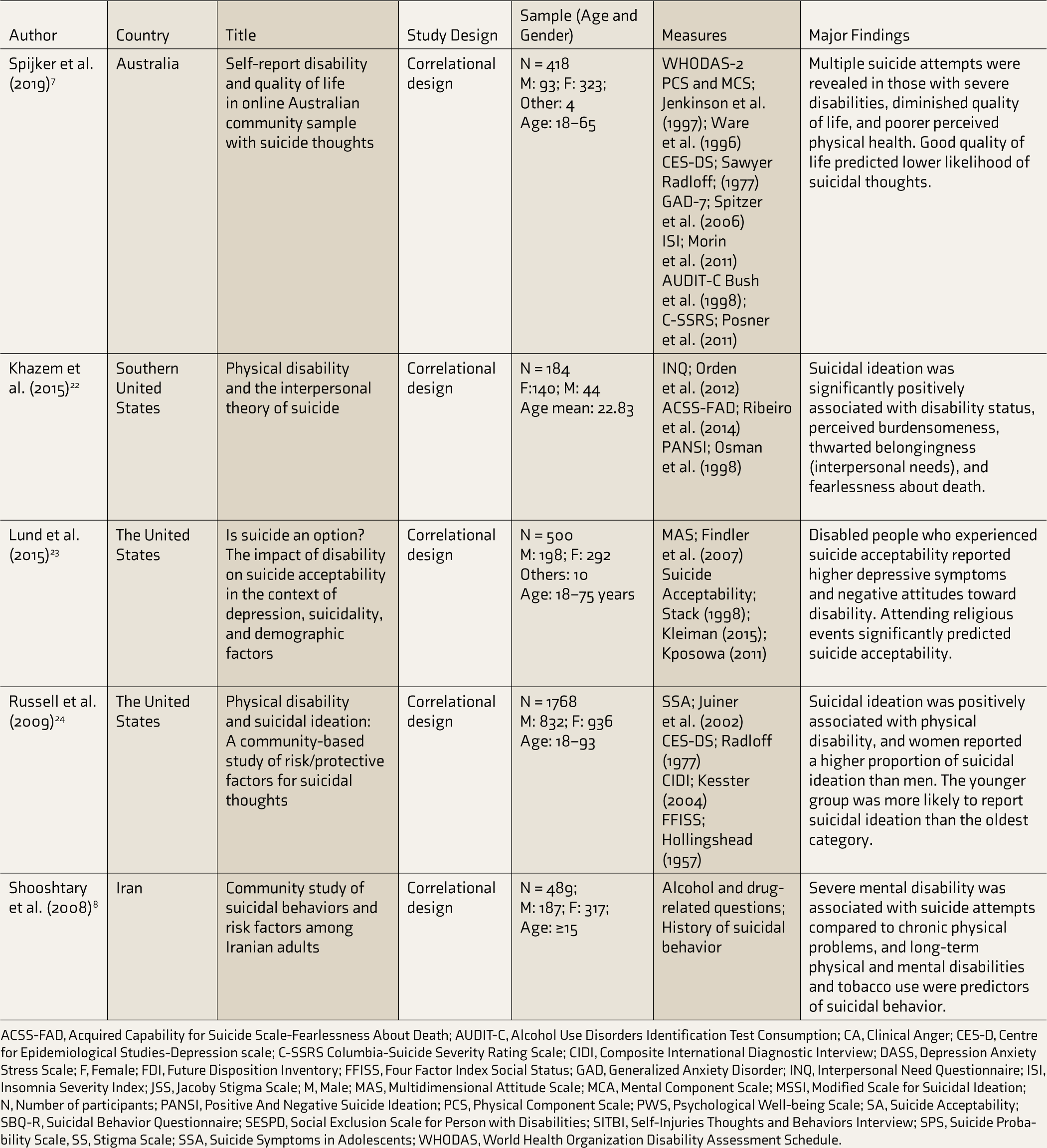
ACSS-FAD, Acquired Capability for Suicide Scale-Fearlessness About Death; AUDIT-C, Alcohol Use Disorders Identification Test Consumption; CA, Clinical Anger; CES-D, Centre for Epidemiological Studies-Depression scale; C-SSRS Columbia-Suicide Severity Rating Scale; CIDI, Composite International Diagnostic Interview; DASS, Depression Anxiety Stress Scale; F, Female; FDI, Future Disposition Inventory; FFISS, Four Factor Index Social Status; GAD, Generalized Anxiety Disorder; INQ, Interpersonal Need Questionnaire; ISI, Insomnia Severity Index; JSS, Jacoby Stigma Scale; M, Male; MAS, Multidimensional Attitude Scale; MCA, Mental Component Scale; MSSI, Modified Scale for Suicidal Ideation; N, Number of participants; PANSI, Positive And Negative Suicide Ideation; PCS, Physical Component Scale; PWS, Psychological Well-being Scale; SA, Suicide Acceptability; SBQ-R, Suicidal Behavior Questionnaire; SESPD, Social Exclusion Scale for Person with Disabilities; SITBI, Self-Injuries Thoughts and Behaviors Interview; SPS, Suicide Probability Scale, SS, Stigma Scale; SSA, Suicide Symptoms in Adolescents; WHODAS, World Health Organization Disability Assessment Schedule.
The factors associated with suicide ideation and attempts were extracted from the studies and arranged based on how many studies detected them.
Associated Factors of Suicidal Ideation
Disability status (11 studies),7–9,16–19,21–24 perceived burdensomeness (6 studies),9,16,18,21,22,24 depressive symptoms (6 studies )7,9,20,21,23,24 felt stigma (5 studies),8,9,16,18,19 thwarted belongingness (4 studies),16,18,21,23 severity of physical disability (3 studies),18,19,23 fearlessness about death (2 studies),22,23 low income (2 studies),19,20 lower levels of social support (2 studies),9,24 congenital disabilities (1 study), 19 mobility disability (1 study), 9 long-term physical disability (1 study), 8 mental disability (1 study), 8 tobacco use (1 study), 8 social exclusion (1 study), 19 suicidal thoughts while living alone (1 study), 19 higher levels of social stress (1 study), 20 emotional reliance (1 study), 20 mastery (1 study), 20 self-esteem (1 study), 20 and clinical anger (1 study) 17 were the associated factors of suicidal ideation.
Outcomes of Suicidal Ideation
Suicide attempts (1 study), 18 and diminished psychological well-being (1 study), 19 were the outcomes of suicidal ideation.
Sex and Suicidal Ideation and Attempt
Suicidal ideation,7,17 suicide attempts, multiple attempts, 7 clinical anger, 17 and physical disability status 24 were more in females. Males were more likely to report lower levels of stress and higher levels of depressive symptoms and suicidal ideation. 20 Females were more likely to have suicidal behaviour. 8
Types of Disability and Suicidal Ideation
Those with complex activity disabilities, more than two disabilities, 17 long-term mental disabilities, 16 or physical disability conditions had more probability of suicidal ideation, suicide plan, and suicide attempts than those without them.
Associated Factors of Suicide Attempts
Perceived burdensomeness (6 studies),9,16,18,21,22,24 physical disability (6 studies),17,19–22,24 felt stigma (4 studies),8,9,16,18 severity of physical disability (2 studies),18,23 poor perceived physical health (1 study), 7 diminished quality of life (1 study), 7 complex activity disabilities (1 study) 9 more than two disabilities (1 study), 9 and severe mental disabilities (1 study) 8 were associated factors of suicide attempts.
Associated Factors of Suicide Acceptability
Suicide acceptability was associated with a higher risk of suicidal ideation and attempts. 3 Depression (6 studies)7,9,20,21,23,24 negative attitudes toward disability (1 study), 19 acceptance of disability conditions (1 study), 19 and disability status of family member (1 study) 19 were significant risk factors of suicide acceptability.
Association of Sociodemographic Variables
Tobacco abuse, 8 drug addiction, and aggression were related with suicidal ideation. 17 Anxiety, alcohol, opioids, or sedatives were not significantly associated with suicide attempts. 8 House accessibility and perceived health were associated with lower levels of suicidal ideation among older adults; however, home ownership or household quality was not correlated with suicidal ideation. 20
Discussion and Conclusion
Published articles were reviewed to understand the associated factors of suicidal behavior, suicide ideation, and attempts among people with physical disability. Based on the included studies, many associated factors have been identified. The biological factors include disability status, the severity of physical disability, long-term physical disability, congenital disabilities, complex disability, and multiple disabilities.
Disability status and severity of physical disability prevent participation in group and social activities, making the individual prone to unhealthy lifestyles. It lowers their self-esteem, self-image, and self-efficacy. They become hopeless and pessimistic and experience poor quality of life. The level of disability and severity affect mobility and hence their educational endeavors. Limited educational institutes and lack of career options lead to resentment regarding academic and educational choices. Mobility is the biggest issue for severely disabled people because they require an escort for movement, which makes them feel pathetic and burdened. Long-term physical disability and congenital disabilities lead to burdensomeness and susceptibility throughout life, which is very baleful to them and makes them helpless. Those with long-term physical disability reported higher levels of mental health problems and had more probability to report suicidal ideation, suicide plans, and suicide attempts than those without them. 8 Complex disability and multiple disabilities make life worse. Those with them become slack and heedless, and they are always dependent on others for completing tasks, promptness, and mobility. They become dependent on people’s support, and their life becomes monotonous, anxious, and humdrum, inducing suicidal ideation. 9 It threatens their mental health and causes frustration, which leads to decadence, psychosocial distortion, loss of temper and perseverance, and finally suicidal ideation.
The psychosocial factors include perceived burdensomeness, social stigma, aggression, substance use, loneliness, and social exclusion. Perceived burdensomeness is a perception of being a burden on the family and society. Thwarted belongingness is a psychologically unpleasant mental condition that occurs when the basic urge for connectivity is unmet.25,26 People with disabilities may struggle with feelings of burdensomeness and thwarted belongingness due to the lack of accessibility, adverse personal experiences, and lack of received support and assistance.16,23 They experience challenges and limitations that affect their daily lives and achievements, which is an escalator of mental health issues such as depression, anxiety, stress, and eventually suicidal ideation. They feel stigmatized in the community based on their physical appearance, body image, and disability. Body dissatisfaction has been highly associated with quality of life and mental health problems. It directly influences individuals’ perceptions and facilitates negative beliefs and lower self-esteem and self-concept. 21 Difficulty in making friends and socializing leads to isolation, and negative schemas lead to suicidal behavior. Experiencing unique challenges and emotional burdens, such as dealing with pain, mobility, dependence, social isolation, and negative societal attitudes, threatens their mental health. They cannot balance their body and mind and experience higher levels of anger due to several psychosocial problems such as stigmatization, acceptance, displeasure, wrath, annoyance, and irritability. These factors and other personal circumstances and mental health issues contribute to aggression and promote suicidal ideation. Some also indulge in substance use to cope with physical, emotional, or social difficulties, which can provide temporary relief or escape, but it can also exacerbate mental health problems and increase the risk of suicidal thoughts or behaviors. Social exclusion is a major concern leading to loneliness, lack of social and emotional connectedness, low self-esteem, and social stress. Most physically disabled people do not want to participate in social activities because they cannot join the group or company owing to their disability status. Most of the time, people are also excluded from society due to accessibility barriers, limited opportunities, and discrimination. 19 Negative attitudes and societal barriers can contribute to a lack of social integration and opportunities for meaningful social connections. These effects can further perpetuate the cycle of exclusion, limit their overall well-being, and lead to suicidal ideation or attempts.
Suicidal behavior is a common issue and not limited to persons with a physical disability. It is not a characteristic problem of people with disabilities only. According to WHO estimations, India has the world’s 41st-highest suicide rate as of 2019. 27 The difficulties disabled people face in adjusting themselves to their disability and accepting it stand different from the problems people without disabilities face. Our findings highlight felt stigma, exclusion, discrimination, burdensomeness, dependence, and lack of mobility due to disability as the factors responsible for suicidal ideation and attempts in disabled persons. People with disabilities have poorer health outcomes, poor quality of health and health care received, and less social and economic participations than people without disabilities. 28
Suicide rates among physically disabled people can be reduced by providing them with the best, most advanced, free-of-cost treatment and medical support in institutions, hospitals, and rehabilitation centers to lower the level and severity of disability and help them stay active and become a part of the community. Social support and acceptance by the family, friends, and community can be an enormous resource to meet their expectations. This can help increase their confidence, enhance their quality of life and well-being, and reduce the probability of suicidal ideation. Arrangement of ramps, elevators, accessible restrooms, appropriate signage, and accessible schools and workplaces, coupled with welcome attitudes and acceptance, can promote access to quality education and suitable employment. This can lead to economic advantages and their inclusion in the workforce. Social inclusion can have significant psychological impacts, enhance their self-esteem, and lower their mental health problems and suicidal ideation or attempts.
This review was limited only to associated factors of suicidal behavior, such as suicidal ideation and suicide attempts among people with a physical disability. It focused on correlational studies exploring the associated for suicide. Other study designs such as cohort and case-control must be incorporated into future reviews.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
