Abstract
Newer urinary protein kidney safety biomarkers can outperform the conventional kidney functional biomarkers blood urea nitrogen (BUN) and serum creatinine (SCr) in rats. However, there is far less experience with the relative performance of these biomarkers in dogs and nonhuman primates. Here, we report urine protein biomarker performance in tenofovir-treated cynomolgus monkeys and beagle dogs. Tenofovir intravenous daily dosing in monkeys for 2 or 4 weeks at 30 mg/kg/day resulted in minimal to moderate tubular degeneration and regeneration, and tenofovir disoproxil fumarate oral dosing in dogs for 10 days at 45 mg/kg/day resulted in mild to marked tubular degeneration, necrosis, and regeneration. Among biomarkers tested, kidney injury molecule 1 (Kim-1) and clusterin (CLU) clearly outperformed BUN and SCr and were the most reliable in detecting the onset and progression of tenofovir-induced tubular injury. Cystatin C, retinol binding protein 4, β2-microglobulin, neutrophil gelatinase–associated lipocalin, albumin, and total protein also performed better than BUN and SCr and added value when considered together with Kim-1 and CLU. These findings demonstrate the promising utility of these urinary safety biomarkers in monkeys and dogs and support their further evaluation in human to improve early detection of renal tubular injury.
Tenofovir disoproxil fumarate (TDF), a prodrug of tenofovir (TFV), is a nucleotide reverse transcriptase inhibitor widely used as an effective therapeutic treatment of HIV infection. TDF, when administered orally, is absorbed from the gut and taken from the plasma by leukocytes where it can be quickly converted to tenofovir (or (R)-9-(2-phosphonoylmethoxypropyl)adenine [PMPA]), which in turn is phosphorylated intracellularly to become the active antiviral metabolite PMPA diphosphate (PMPApp) by adenylate kinase. PMPApp competitively inhibits viral reverse transcriptase activity by competing with deoxyadenosine triphosphate and causing premature chain termination during DNA elongation, thereby inhibiting HIV RNA conversion to DNA and subsequent virus replication (Fung, Stone, and Piacenti 2002). Alternatively, a significant portion of TDF following oral administration is converted in plasma to tenofovir and eliminated in a transporter-dependent manner by proximal tubule cells of the kidney. While effective for its intended use, TDF is associated with drug-induced kidney injury (DIKI) and bone injury, with renal cases of acute renal failure and Fanconi syndrome seen in approximately 1% of patients treated at the approved daily dose of 300 mg (Fernandez-Fernandez et al. 2011). This toxicity is reported to be mitochondrial in origin, likely due to the inhibition of mitochondrial DNA polymerase and subsequent disruption of nucleic acid processing (Fernandez-Fernandez et al. 2011; Lebrecht et al. 2009).
In preclinical studies conducted to support development and marketing of TDF, the major target toxicity organs identified were kidney, gastrointestinal tract, and bone, with nephrotoxicity seen as the most clinically concerning toxicity (FDA 2001). Renal tubular epithelium toxicity was observed in all preclinical species tested and is the primary dose-limiting toxicity associated with oral administration of TDF in nonrodent species (FDA 2001). Since tenofovir and its prodrug have been shown to cause dose-dependent kidney toxicity in both monkey and dog, these compounds are attractive candidates to investigate the relative performance of the novel urinary biomarkers in these species as compared to conventional serum parameters.
DIKI is still a common hindrance in drug development, and there is a need for improved ability for monitoring kidney toxicity due to the insensitivity of conventional biomarkers blood urea nitrogen (BUN) and serum creatinine (SCr; Bonventre et al. 2010). Elevations in BUN and SCr may not be seen until the kidneys lose 50% to 75% functional capacity. In preclinical toxicity studies, the occurrence of low-grade DIKI confirmed histologically without concurrent BUN or SCr increases is not unusual (Bonventre et al. 2010; Dieterle et al. 2010a; Vlasakova et al. 2014). When it happens, it can be difficult to advance the development of compounds into clinical trials due to the lack of a means to monitor and ensure patient safety. On the other hand, there are situations, such as prerenal azotemia, in which BUN and SCr levels may increase without intrarenal histomorphologic changes, further limiting the utility of these serum biomarkers in kidney safety monitoring. Efforts have been launched to identify, evaluate, and qualify more sensitive and more specific accessible translational kidney safety biomarkers (Amin et al. 2004; Ennulat and Adler 2015). As a result, a set of urinary translational kidney safety protein biomarkers has been shown to outperform serum biomarkers in rats and has received regulatory endorsement for their use in demonstrating monitorability of DIKI in rats as well as for application in human clinical trials on a case-by-case basis (Dieterle et al. 2010a; Dieterle et al. 2010b; Phillips et al. 2016; Sistare et al. 2010; Vlasakova et al. 2014). While this is an important step in advancing the application of these biomarkers in the clinic, the performance of these biomarkers in tenofovir-treated monkeys and dogs has not been assessed, and few studies have assessed the performance of these safety biomarkers in nonrodent preclinical animal species in general. A demonstration of superior performance of these new translational kidney safety biomarkers in nonrodent animal studies helps to establish their utility in drug development for compounds with kidney toxicity liability seen in animals but with uncertain relevance in humans. Furthermore, these data support application of these biomarkers for identifying particularly susceptible individuals or synergistic deleterious risk factors underlying the low incidence (∼1%) but significant renal toxicity that can be seen in the clinic with tenofovir.
We report here an evaluation of the performance of a set of urinary protein kidney safety biomarkers kidney injury molecule 1 (Kim-1), clusterin (CLU), neutrophil gelatinase–associated lipocalin (NGAL), N-acetyl-β-D-glucosaminidase (NAG), osteopontin (OPN), albumin (ALB), total protein, cystatin C (CysC), β2-microglobulin (B2M), and retinol binding protein (RBP4) in comparison with conventional serum biomarkers BUN and SCr in tenofovir-treated beagle dogs or cynomolgus monkeys. We demonstrate that several of these novel urinary renal tubular safety biomarkers outperform BUN and SCr in detecting tenofovir-induced renal tubular injury. These findings therefore provide evidence to justify further exploration of the utility of these biomarkers in clinical studies with TDF and related compounds.
Materials and Method
In vivo Studies
TDF and PMPA were obtained from Pharmaron Inc. (Irving, CA). TDF was dosed orally to dogs, while PMPA was administered intravenously to cynomolgus monkeys due to the known poor oral bioavailability of TDF in monkeys. These exploratory studies were approved by the Merck Institutional Animal Care and Use Committee and conducted in an Association for Assessment and Accreditation of Laboratory Animal Care International–accredited facility in compliance with the National Institutes of Health (NIH) Guide for the Care and Use of Laboratory Animals and the Animal Welfare Act. The animals were acclimated and randomized into treatment and control groups.
Cynomolgus monkeys aged 3 to 4 years weighing 2.5 to 4.5 kg were obtained from Noveprim Europe Ltd (Ebene, Mauritius). Ten monkeys were divided into a 2-week arm and a 4-week arm with 5 monkeys each. Within each study arm, 2 control monkeys were treated with vehicle (0.9% sodium chloride) and 3 monkeys were treated daily with 30 mg/kg/day PMPA, which would result in approximately 14-fold of human plasma exposure at the recommended daily clinical dose of 300 mg (FDA 2001). The route of drug administration was intravenous via the saphenous vein with the day of first dosing noted as study day 1. Serum and urine were collected at predose, study days 3, 9, and 15 for the 2-week study arm with necropsy at day 15; and at predose, study days 3, 9, 15, 22, and 29 for the 4-week study arm with necropsy at day 29 (Table 1). The dose level and the treatment duration were chosen to result in minimal renal tubular injury based on prior tenofovir studies conducted by the drug sponsor in which only low-grade degenerative changes in kidney were observed in both male and female cynomolgus monkeys treated with PMPA at 25 mg/kg/day for 14 days (FDA 2001).
Treatment Regimen and Test Article–related Histomorphologic Findings in Cynomolgus Monkeys.
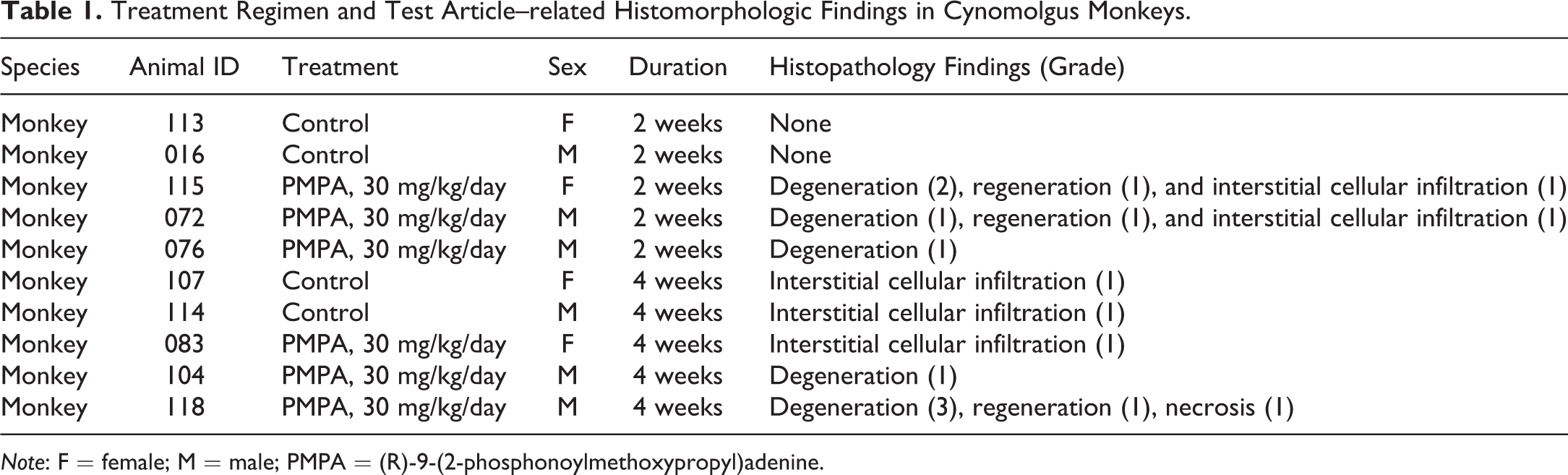
Note: F = female; M = male; PMPA = (R)-9-(2-phosphonoylmethoxypropyl)adenine.
Beagle dogs aged 1 to 3 years weighing 7 to 12 kg were obtained from Marshall BioResources (North Rose, New York). A total of 4 dogs were treated with vehicle (deionized water) and 4 dogs with 45 mg/kg/day TDF daily, which would also result in approximately 14-fold of human exposure of PMPA at the recommended daily clinical dose of 300 mg (FDA 2001). The route of drug administration was via oral gavage (Table 2). The duration of the treatment was shortened to 10 days instead of the planned 14 days with necropsy at day 11 due to clinical signs observed. Serum and urine were collected at predose, study days 4, 8, and 11. The dose level and the treatment duration were chosen to result in minimal renal tubular injury based on prior TDF studies in which only minimal renal tubular degeneration with individual epithelial cell necrosis was observed in 2 of the 2 male beagle dogs treated with TDF at 45 mg/kg/day for 5 days (FDA 2001).
Treatment Regimen and Test Article–related Histomorphologic Findings in Beagle Dogs.
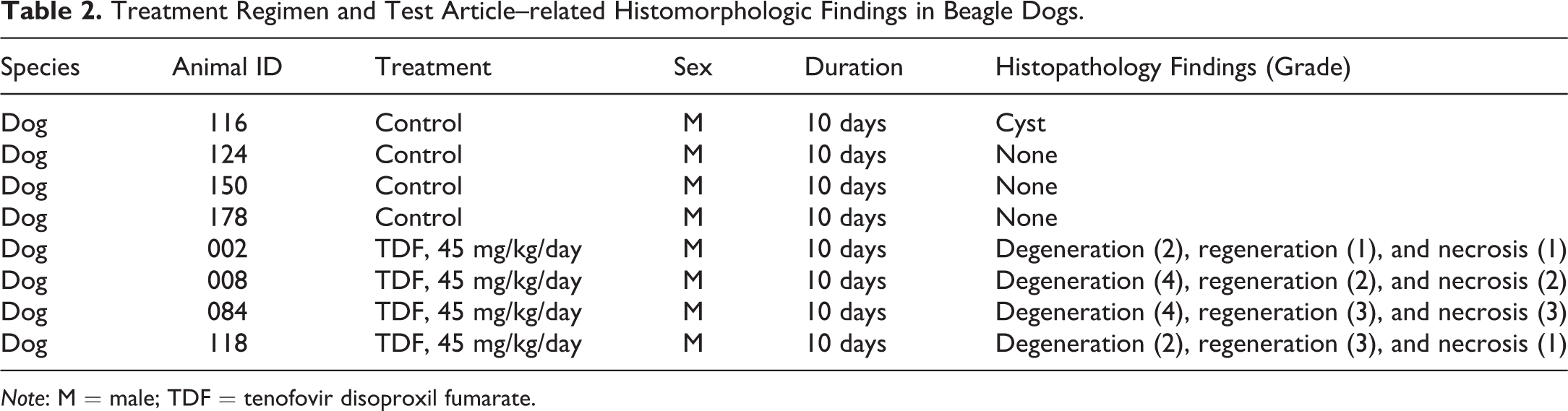
Note: M = male; TDF = tenofovir disoproxil fumarate.
All animals were fasted during overnight urine collection and before necropsy. Urine was collected overnight (16–20 hr) on wet ice, samples were either immediately used for urinalysis parameters including urinary creatinine measurements or centrifuged and aliquoted and stored at −70°C until subsequent biomarker measurements.
Histopathology
Microscopic histomorphologic examinations were limited to kidney, liver, heart, skeletal muscle (rectus femoris), and bone. Hematoxylin and eosin (H&E)-stained tissue sections were examined, and grades were assigned in a five-point grading scale with 0 being no observable pathology, 1 being minimal, 2 being mild, 3 being moderate, 4 being marked, and 5 being severe.
Serum Chemistry and Urine Protein Biomarker Analysis
Serum parameters BUN and SCr, as well as urinary protein analytes ALB, total protein, and NAG in both monkey and dog studies, were determined by routine clinical pathology procedures using a Beckman AU5800 Chemistry Analyzer. The other urinary biomarkers Kim-1, CLU, NGAL, OPN, CysC, B2M, and RBP4 were determined using ELISA kits according to the manufacturer’s instructions (Table 3). Assays are chosen based on their relevance to kidney toxicity and availability at the time of the study. Urinary Kim-1 was measured only in monkeys and not in dogs due to the lack of assay availability for dog Kim-1. The lower limits of quantitation (LLOQ) of the assays used are also listed in Table 3. The analyte concentration in the urine was normalized against the urine creatinine concentration. For the purpose of calculating fold changes and for graphing, 50% of the LLOQ value was used when the analyte concentrations fell below the LLOQ of the assay, which was the case for a number of samples especially at the baseline levels for Kim-1, ALB, B2M, and total protein in monkeys as well as CLU and ALB in dogs.
Urinary Renal Safety Biomarker Assays.
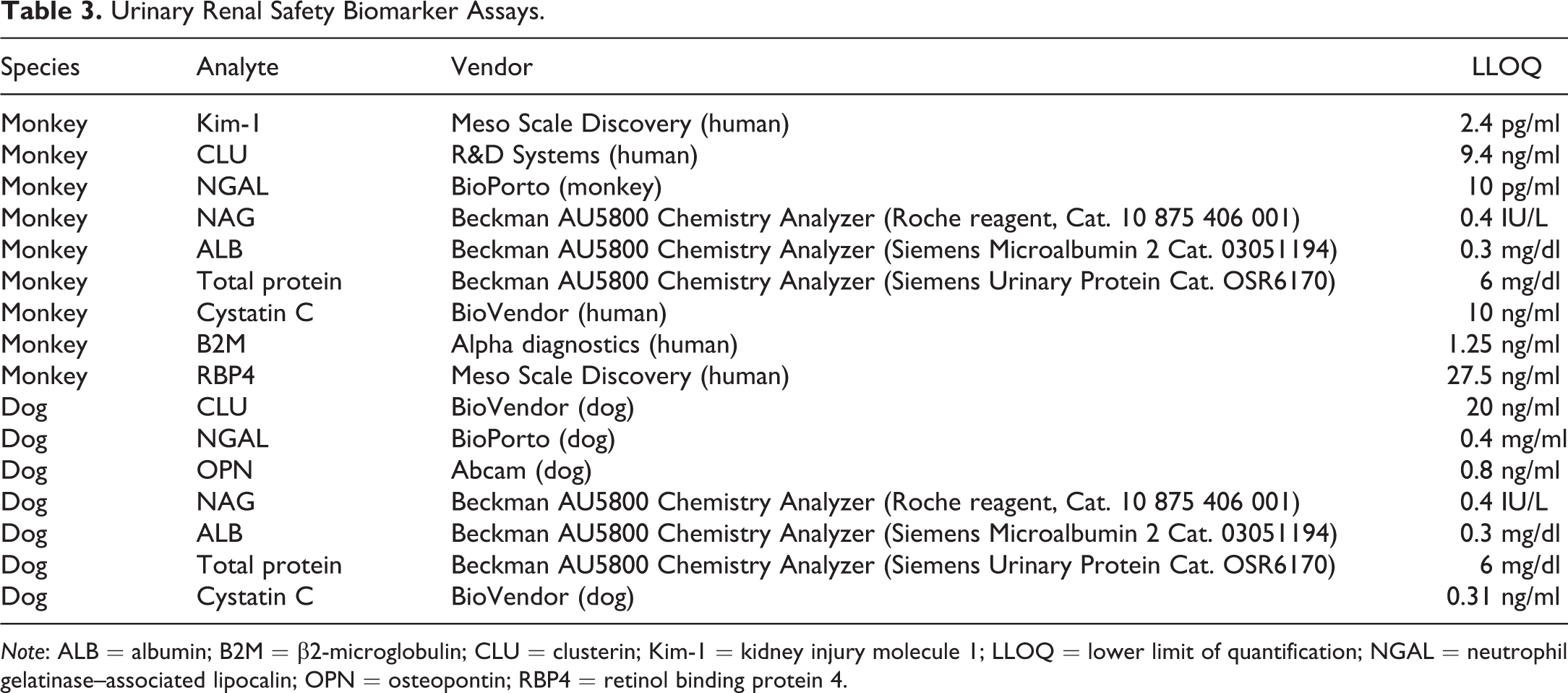
Note: ALB = albumin; B2M = β2-microglobulin; CLU = clusterin; Kim-1 = kidney injury molecule 1; LLOQ = lower limit of quantification; NGAL = neutrophil gelatinase–associated lipocalin; OPN = osteopontin; RBP4 = retinol binding protein 4.
The mean study baseline levels of each analyte for each species used for calculating fold changes were determined as the average of the normalized analyte concentrations of all time points of the control group animals together with the predose normalized analyte concentrations of the treatment group animals. Urinary biomarkers were considered to be increased by TDF or tenofovir if the normalized urinary level of the analyte at any time point following treatment exceeded 3-fold above the mean study baseline level for that analyte for each species. BUN and SCr were considered elevated if increases above 1.5-fold of each individual animal’s baseline value was achieved.
Results
Histopathology
The histomorphologic renal findings observed in the cynomolgus monkey and beagle dog are summarized in Tables 1 and 2, with representative histomorphologic changes shown in Figure 1. In the 2-week arm of the cynomolgus monkey study, all (3/3) tenofovir-treated animals showed low-grade proximal tubular degeneration with concurrent regeneration (2/3) in the cortex of the kidney. Distal tubules were largely unaffected aside from occasional minimal dilatation, and there was no involvement of glomeruli or other tubular elements. Degeneration in the monkey was often characterized by cytoplasmic swelling and disorganization of epithelium and karyomegaly. Areas of interstitial cellular infiltrates were occasionally observed adjacent to areas of tubular degeneration; however, given the presence of similar levels of cellular infiltrates in the concurrent control animals, the relationship to treatment could not be determined. The histomorphologic changes in the kidney were similar following 4 weeks of treatment, with minimal to moderate tubular degeneration/necrosis and regeneration observed in 2 of 3 monkeys. No treatment-related liver, heart, skeletal muscle, or bone findings were observed in these short-duration monkey studies.
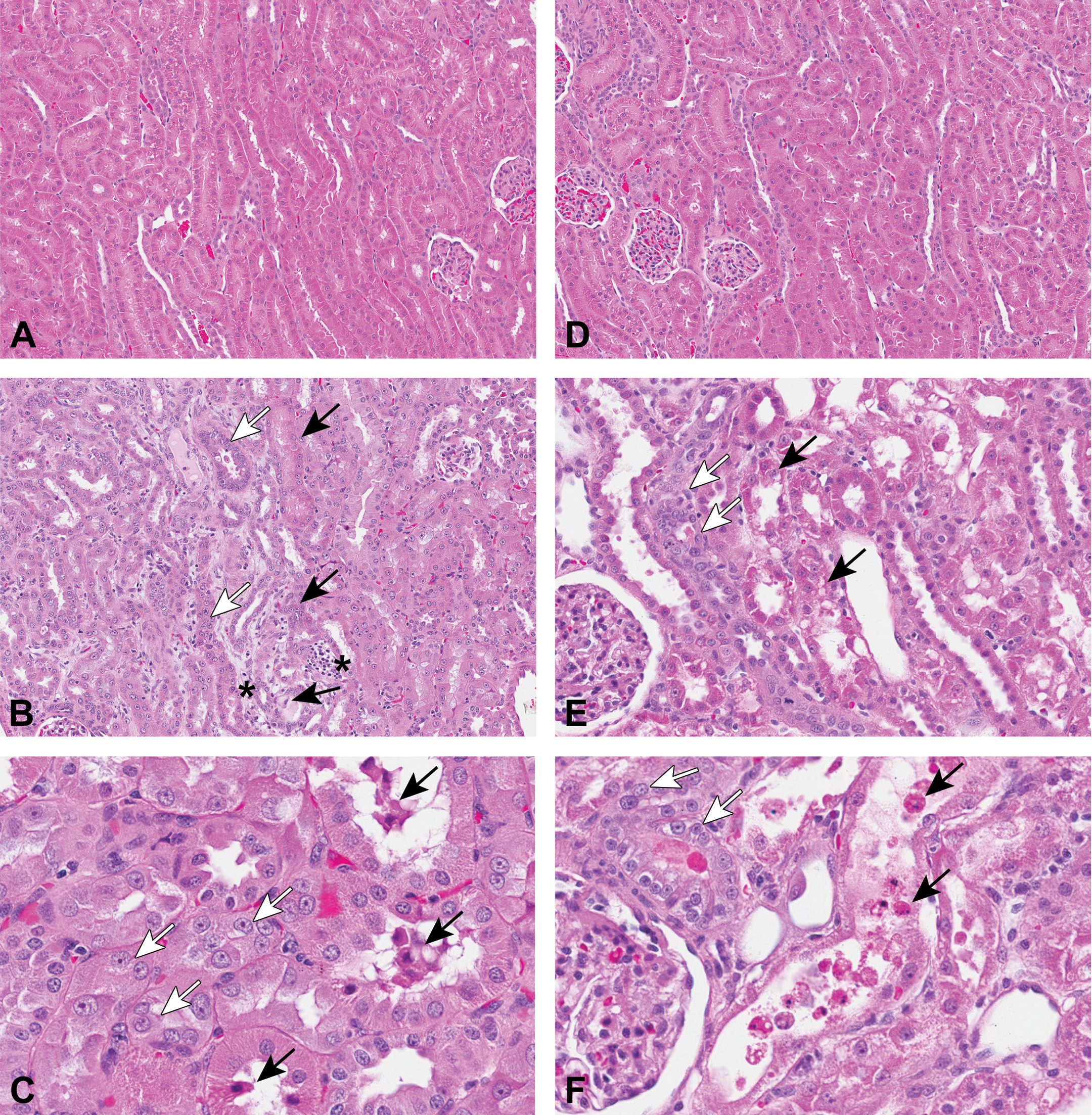
Histomorphologic findings in kidneys of monkey and dog tenofovir studies. Tenofovir-treated monkeys showed low-grade proximal tubular degeneration with concurrent regeneration in the cortex of the kidney. Distal tubules were largely unaffected aside from occasional minimal dilatation, and there was no involvement of glomeruli or other tubular elements. (A) Vehicle control–treated monkey; (B) Tenofovir-treated monkey at 30 mg/kg/day for 4 weeks; (C) Tenofovir-treated monkey at 30 mg/kg/day for 4 weeks (high magnification). TDF-treated dogs showed mild to marked tubular degeneration, necrosis, and regeneration predominantly focused on proximal tubules within the cortex with some extension to distal tubules most prominent in dogs with higher severity scores. There was no glomerular involvement and other tubular elements such as collecting ducts were largely unaffected aside from occasional luminal debris or casts. (D) Vehicle control–treated dog; (E) Tenofovir-treated dog at 45 mg/kg/day for 10 days; (F) Tenofovir-treated dog at 45 mg/kg/day for 10 days (high magnification). Black arrow = tubular degeneration and/or necrosis, white arrow = tubular regeneration/karyomegaly, star (*) = interstitial cellular infiltration, TDF = tenofovir disoproxil fumarate.
The TDF dog study was terminated on day 11 instead of planned day 15 due to decreased food consumption, body weight loss, and increase in SCr levels. All 4 tenofovir-treated dogs showed mild to marked tubular degeneration, necrosis, and regeneration predominantly focused on proximal tubules within the cortex with some extension to distal tubules most prominent in animals with higher severity scores. There was no glomerular involvement, and other tubular elements such as collecting ducts were largely unaffected aside from occasional luminal debris or casts. In addition, marked inflammation in the large intestine and minimal glycogen depletion in liver were observed. No other treatment-related histomorphologic changes were observed in heart, skeletal muscle, bone, and liver of dogs.
Biomarker Performance
Cynomolgus monkey study
The biomarker data from the cynomolgus monkey study are presented in Table 4. A transient BUN increase of more than 1.5-fold was seen in only 2 of 6 treated monkeys on day 3, which returned to baseline levels at the next collection time point (day 9) even with continuous daily tenofovir dosing. The two monkeys with these transient BUN increases were the 2 monkeys (animals #115 and #118) that presented with mild and moderate kidney lesions at necropsy. A similar transient increase was observed for SCr on day 3 but only in 1 of the 6 treated monkeys (animal #115), which was also the monkey presenting with mild kidney lesions at necropsy. For the 3 monkeys presenting with grade 1 kidney histopathology (animals #072, #076, and #104) and the one treated monkey with no histopathology (animal #083), there was not a concurrent 1.5-fold alteration in either BUN or SCr.
Fold Change of Renal Tubular Biomarkers Over Baseline (Mean of Biomarker Values of All Time Points of Control Animals and Baseline Values of Treated Animals) in Tenofovir Monkey Study.a
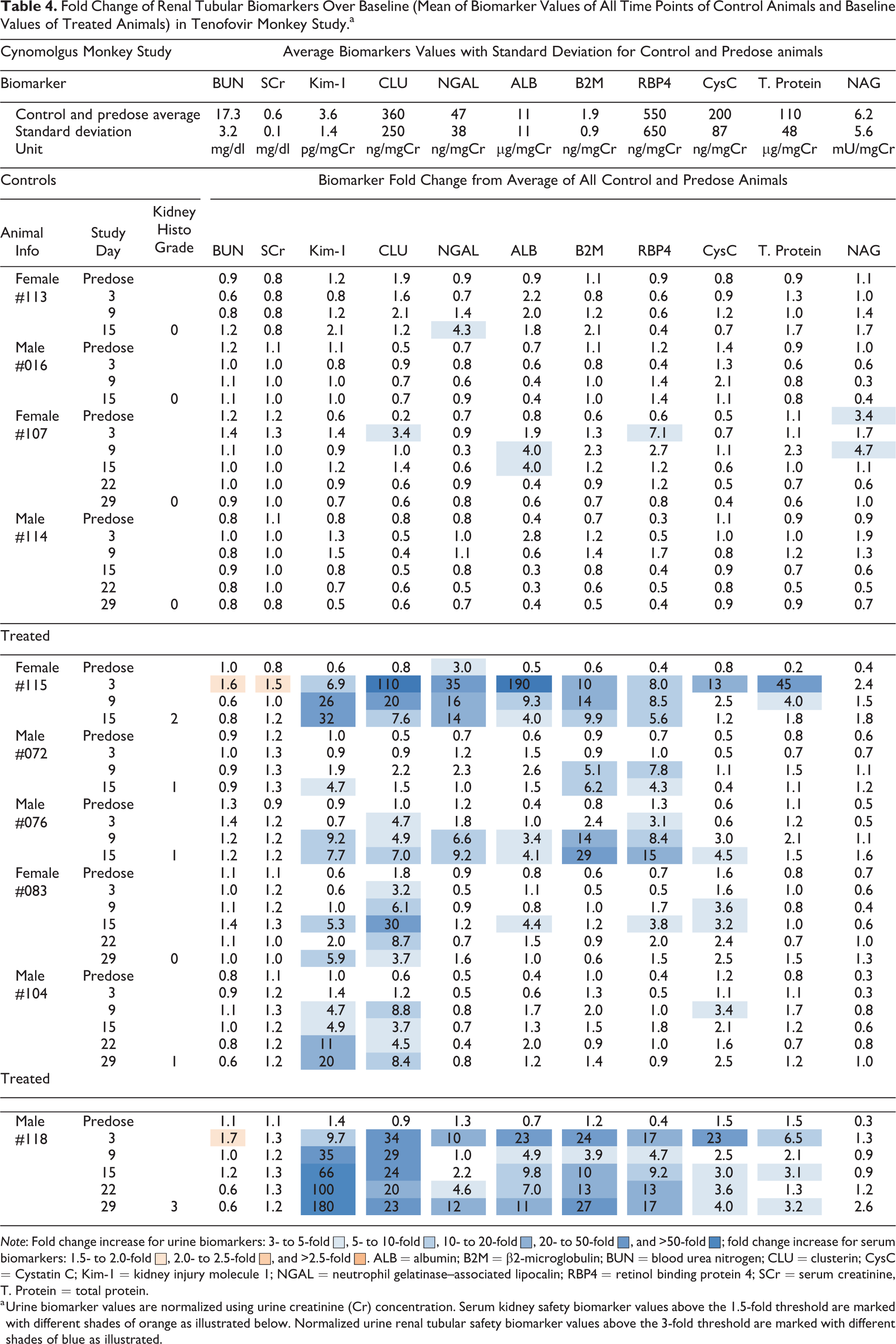
Note: Fold change increase for urine biomarkers: 3- to 5-fold ▪, 5- to 10-fold ▪, 10- to 20-fold ▪, 20- to 50-fold ▪, and >50-fold ▪; fold change increase for serum biomarkers: 1.5- to 2.0-fold ▪, 2.0- to 2.5-fold ▪, and >2.5-fold ▪. ALB = albumin; B2M = β2-microglobulin; BUN = blood urea nitrogen; CLU = clusterin; CysC = Cystatin C; Kim-1 = kidney injury molecule 1; NGAL = neutrophil gelatinase–associated lipocalin; RBP4 = retinol binding protein 4; SCr = serum creatinine, T. Protein = total protein.
a Urine biomarker values are normalized using urine creatinine (Cr) concentration. Serum kidney safety biomarker values above the 1.5-fold threshold are marked with different shades of orange as illustrated below. Normalized urine renal tubular safety biomarker values above the 3-fold threshold are marked with different shades of blue as illustrated.
With the threshold value set at 3-fold increase over the mean study baseline values, urinary protein Kim-1 levels were elevated in all 6 tenofovir-treated monkeys with peak changes of 5- to 180-fold, with no elevations seen among the control monkeys. Kim-1 levels first crossed the threshold in 2 of the 6 treated monkeys on day 3, followed by 4 of the 6 monkeys by day 9, and in all 6 monkeys by day 15. A marginal rise in urinary Kim-1 was observed in one tenofovir-treated female monkey on day 15 and day 29 that presented with no notable kidney histomorphologic changes at the time of necropsy (monkey #083). Kim-1 elevations were generally sustained over the time course once elevated, and levels generally continued to rise upon continuous daily dosing of tenofovir. This is especially evident in the 2 monkeys with grade 2 or 3 kidney injuries (monkey #115 and 118). The fold changes of Kim-1 over control at the time of their necropsy were generally proportional to the severity of histopathology observed.
The pattern of change in urinary CLU levels following tenofovir treatment in monkeys showed some differences compared with that of Kim-1. Urinary levels of CLU increased in 5 of the 6 tenofovir-treated monkeys with peak elevations ranging from 7- to 110-fold, with no change however in animal #072 that exhibited grade 1 kidney histopathology. A transient 3.4-fold rise was also seen on day 3 in one control monkey (#107). The elevations of CLU in treated animals began in 4 of the 6 treated monkeys on day 3, followed by an additional treated monkey by day 9. The peak magnitude and duration of CLU elevations observed generally correlated with the grade of kidney pathology observed in individual treated animals, but were not as concordant as seen for Kim-1. Examples include animal #072, which had grade 1 kidney pathology and a minimal rise of Kim-1 but no increases seen in CLU, and animal #083 with no notable kidney pathology but with up to 30-fold CLU increases. Furthermore, peak elevations of CLU were generally seen at earlier urine collection time points on days 3, 9, or 15 and subsided subsequently with continued treatment, while peak elevations were generally seen at the final collection time point for Kim-1.
Urinary RBP4 and CysC were elevated in 5 of the 6 treated monkeys seen as early as day 3 and with greater peak magnitude and generally more sustained changes in the 2 treated monkeys with mild and moderate kidney lesions (#115 and 118, respectively). RBP4 was elevated at a single time point in one control animal, while no elevation was seen for CysC in control animals.
Urinary B2M and ALB were elevated in 4 of the 6 treated monkeys. ALB was marginally increased in one control animal with 4-fold elevations on two consecutive time points and in 2 treated animals with minimal or no kidney pathology with similar unconvincing 3- to 4-fold single time point elevations. B2M on the other hand showed 6- to 29-fold peak elevations in treated monkeys with no elevations seen in control animals.
NGAL was increased in urine collections of 3 of the 6 treated monkeys, and total protein was elevated in urine samples of 2 of the 6 monkeys. Each of these 2 biomarkers showed highest elevations in the 2 monkeys, with the grade 2 and grade 3 kidney pathology findings also presenting with SCr and BUN changes. NGAL was elevated in one control animal, while total protein showed no urine elevations in control monkeys. NAG levels were not increased in urine of TFV-treated monkeys and appear not to be a useful indicator for tenofovir-induced renal tubular injury in monkey.
Beagle dog study
In this study, BUN increases of more than 1.5-fold were seen in 2 of the 4 treated dogs. SCr showed more than 1.5-fold increase in all 4 treated dogs starting with the first sample collection on day 4 and more than 2-fold increase in all 4 dogs by the time of necropsy (Table 5).
Fold Change of Renal Biomarkers over Baseline (Mean of Biomarker Values of All Time Points of Control Animals and Baseline Values of Treated Animals) in TDF Dog Study.a
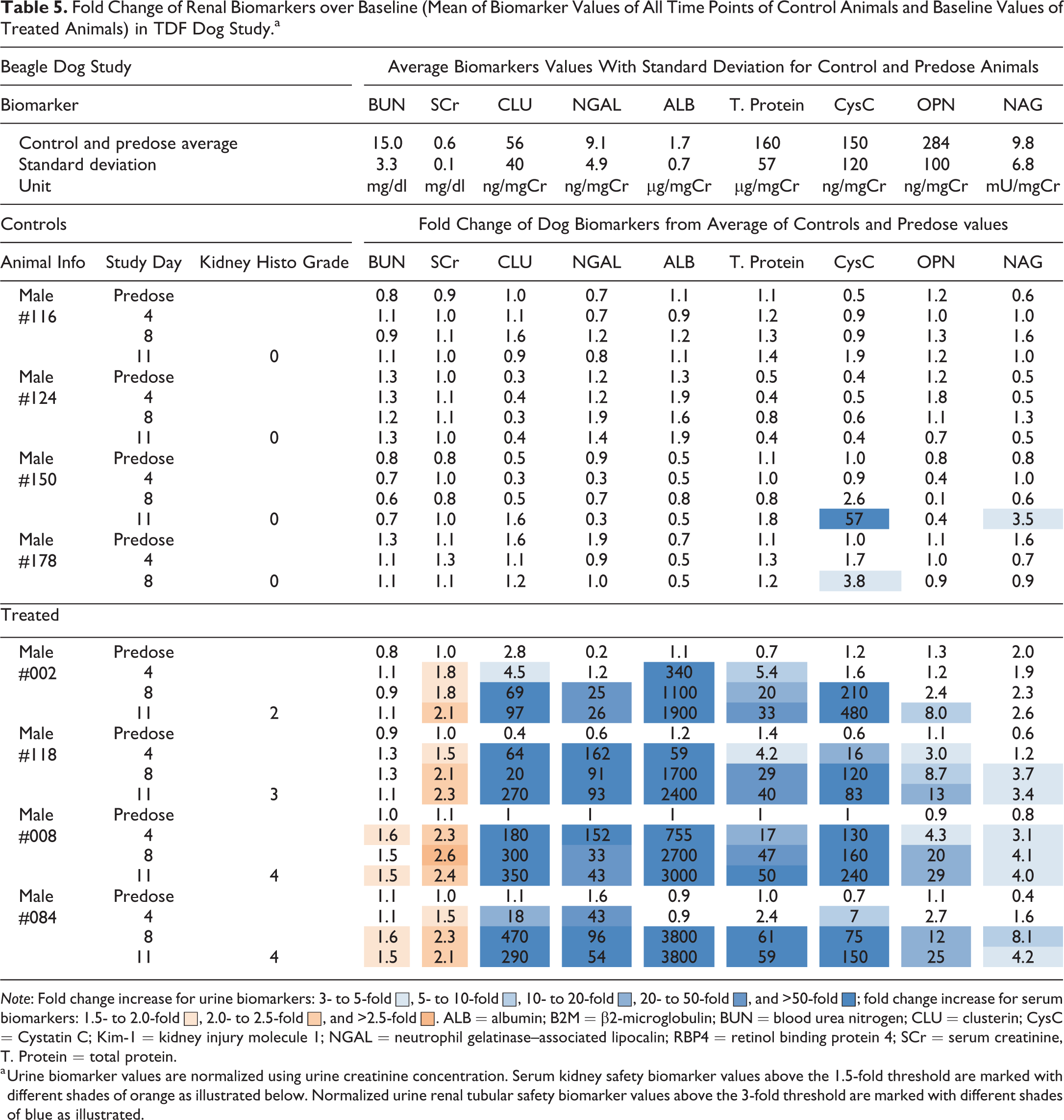
Note: Fold change increase for urine biomarkers: 3- to 5-fold ▪, 5- to 10-fold ▪, 10- to 20-fold ▪, 20- to 50-fold ▪, and >50-fold ▪; fold change increase for serum biomarkers: 1.5- to 2.0-fold ▪, 2.0- to 2.5-fold ▪, and >2.5-fold ▪. ALB = albumin; B2M = β2-microglobulin; BUN = blood urea nitrogen; CLU = clusterin; CysC = Cystatin C; Kim-1 = kidney injury molecule 1; NGAL = neutrophil gelatinase–associated lipocalin; RBP4 = retinol binding protein 4; SCr = serum creatinine, T. Protein = total protein.
a Urine biomarker values are normalized using urine creatinine concentration. Serum kidney safety biomarker values above the 1.5-fold threshold are marked with different shades of orange as illustrated below. Normalized urine renal tubular safety biomarker values above the 3-fold threshold are marked with different shades of blue as illustrated.
Of the urinary kidney safety biomarkers tested in dog, all except NAG were elevated in all TDF-treated animals. CLU levels crossed the 3-fold threshold (up to 180-fold) on day 4 in all 4 treated dogs and were not elevated in any of the controls. Increasing and sustained CLU levels in treated animals demonstrated good sensitivity and utility of CLU in TDF-treated dogs. NGAL increases of up to 162-fold were seen in 3 of the 4 treated dogs on day 4, 4 of the 4 treated dogs by day 8, and remained elevated in all 4 treated dogs until necropsy. OPN levels crossed the threshold starting on day 4 in 2 of the 4 treated dogs, followed by up to 20-fold increase in 3 of the 4 treated dogs on day 8, and all 4 treated dogs at necropsy, while no elevations were seen in control animals. ALB and total protein showed elevations in 3 of the 4 treated dogs on day 4 and all 4 treated dogs at later time points, while no elevations of either biomarkers were seen in control dogs. CysC elevations were seen in 3 of the 4 treated dogs on day 4 and all 4 treated dogs on days 8 and 11. Although large increases in urinary CysC were observed in all 4 treated dogs, a significant increase was also observed in a control dog (animal #150). NAG was only marginally elevated in 3 of the 4 treated dogs as well as in one control dog (Table 5).
Discussion
Histomorphologic findings described in these monkey and dog studies are consistent with the renal tubular injury previously observed in the monkey and dog studies used to support clinical development and marketing approval of tenofovir (FDA 2001). Although the plasma exposures of tenofovir were not measured in these studies, we targeted comparable compound exposures in these two species (about 14 times of the human exposure at the daily dose of 300 mg TDF) based on available toxicokinetic data in the literature. Histomorphologic examination reveals that the renal tubular injury was greater and more than expected in the dog compared with that of the monkey under these experimental conditions, suggesting higher exposures or increased sensitivity to tenofovir-induced renal toxicity in the dog.
In the monkey study, two predose urine samples were taken per animal. One of the two baseline urine samples in two female monkeys (#107 and 115) was visibly contaminated with blood due to these monkeys going through their menstrual cycles at the time of urine collection. The two samples were excluded from data analysis since the blood contamination resulted in high background levels for CLU, ALB, and total protein among the biomarkers analyzed, each of which are known to be present in the blood. This observation indicates the importance of examining multiple urine kidney safety biomarkers holistically and understanding limitations as well as interfering confounders for each biomarker.
The extent of renal tubular injury in the monkey study as reflected in the grades of histopathology is also observed in the magnitude of changes of the new kidney toxicity biomarkers. The conventional serum kidney biomarkers BUN and SCr showed only transient increases in 2 of the 6 treated monkeys, while 5 of the 6 treated monkeys exhibited tenofovir-related tubular degeneration, demonstrating that traditional biomarkers BUN and SCr were not sensitive indicators for the low-grade tenofovir-induced renal tubular injury elicited in this study. Importantly, these transient increases in conventional kidney biomarkers were seen only in the 2 monkeys with more severe kidney histomorphologic changes (grades 2 and 3). In contrast, the urinary kidney toxicity biomarkers Kim-1 and CLU demonstrated greatly improved monitoring of onset and progression of tenofovir-induced tubular changes compared to BUN and SCr and exhibited high sensitivity to low-grade kidney injuries. Although both Kim-1 and CLU exhibited high sensitivity in response to TFV-induced renal tubular injury in monkey, and for CLU the statement can be made for both species, the patterns of their responses over the tenofovir treatment time course were different in that Kim-1 levels generally kept rising throughout the time course, while CLU tended to peak at earlier time points, and sometimes declined over the study period even with continued dosing. This was most evident in the monkey study where the injury was milder in nature. Marginal rises in Kim-1 on days 15 and 29 were observed in one monkey with no notable kidney histomorphologic changes at the time of necropsy (monkey #083). One of the possible explanations as judged from changes of multiple biomarkers was that this monkey endured minimal renal tubular injury around day 15 but recovered at the time of necropsy.
These differing patterns of biomarker changes across time are consistent with the notion that the elevation of Kim-1 likely reflects a tissue reparative and regenerative proliferation response within the proximal tubule (Bonventre 2009; Bonventre et al. 2010; Ichimura et al. 2008). Tenofovir nephrotoxicity is known to be characterized by proximal tubular cell dysfunction, so the increase of Kim-1 urine concentration aligns well with the location of this pathology. CLU is a secretory heterodimeric glycoprotein involved in various biological processes including binding and trafficking of necrotic tissue debris (Humphreys et al. 1999; Poon et al. 2000; Shannan et al. 2006). It is transcriptionally induced in the tubular epithelium including both proximal and distal tubules upon kidney injury with increases in CLU protein concentrations seen in the urine (Bonventre et al. 2010; Dieterle et al. 2010a; Vlasakova et al. 2014). Elevation of kidney CLU expression reflects the presence of renal injury appearing following the initial insult (Wadey et al. 2014). The observation of CLU peaking early before Kim-1 peaked in the monkey study, and declining while Kim-1 may continue to rise, aligns well with purported physiological roles of these proteins following injury.
It is interesting to note that the measured baseline level of Kim-1 in normal cynomolgus monkeys seems low, which is reflected by a number of baseline measurement values in this study being below the assay LLOQ, and the average of Kim-1 baseline values was 3.6 pg/mgCr (Table 4), as compared with human baseline levels of Kim-1 being in the range of 50 to 540 pg/mgCr (Brott et al. 2014). This could be a reflection of either the different Kim-1 baseline levels of different species or the different assays used. But clearly the utility of Kim-1 as a kidney safety biomarker in monkeys is not impaired due to significant upregulation of urinary Kim-1 transcription and expression upon kidney injury (Brott et al. 2014; Liangos et al. 2007; Pavkovic et al. 2016). Although Kim-1 has been shown to be an excellent proximal tubule injury biomarker in rat, monkey, and human, Kim-1 was not evaluated in this dog study due to the lack of an available high-performing canine Kim-1 assay. The dog urine samples generated and retained from this study will be valuable to test emerging canine Kim-1 assays (Naboulsi et al. 2018). For CLU, the normalized urinary baseline concentration in monkeys and dogs are comparable with those seen in human (Brott et al. 2014).
While OPN was not measured in the monkey study, its performance in the dog study was encouraging. OPN was reported to be expressed and upregulated more distally in the nephron tubule and not in proximal tubule (Hudkins et al. 1999). We speculate that the delayed peak seen with OPN may be a reflection of a later occurring indirect damage response appearing downstream of the primary site of drug injury in the proximal tubule, and this view is consistent with the findings of distal tubule involvement observed upon histomorphologic examination.
Urinary B2M, RBP4, and CysC are functional biomarkers for glomerular/tubular injury (Bonventre et al. 2010; Vlasakova et al. 2014). B2M, RBP4 and CysC were elevated in 4 of the 6, 5 of the 6, and 5 of the 6 treated monkeys, respectively, agreeing well with each other and with Kim-1 and CLU data. Importantly, there were no increases among control monkeys for B2M and CysC, while a transient increase was seen in RBP4 in one control monkey. In the dog study, while CysC showed robust responses in treated animals, spurious elevations were also observed in 2 control animals. The performances of these functional glomerular/tubular injury biomarkers were within our expectation since tubular injury could lead to a reduction of tubular resorption of these biomarkers and result in increases of their urinary concentrations. CysC and B2M have been shown to outperform serum biomarkers BUN and SCr for detecting glomerular injury (Dieterle et al. 2010a), and they also perform well when tubular resorption is affected by renal tubular toxicants (Vlasakova et al. 2014). However, since glomerular toxicants often trigger downstream tubular injury, these biomarkers cannot by themselves readily distinguish tubular injury from glomerular injury or the likely consequences seen following the treatment with glomerular toxicants and the manifestation of both glomerular and tubular injury (Dieterle and Sistare 2010; Vlasakova et al. 2014). The smaller molecular weight–filtered functional biomarkers CysC, B2M, and RBP4 may provide added value on regional location only when the timing of their elevations is evaluated holistically along with the timing of elevations of tubular injury response biomarkers such as Kim-1 and CLU, and the larger molecular weight markers in measures of urinary total protein.
NGAL is an injury response biomarker for proximal and distal tubular injury (Bonventre et al. 2010). NGAL performed well in identifying mild-grade kidney lesions in both monkeys and dogs, while its sensitivity to identify minimal grade kidney damage was not as good as that of Kim-1 and CLU. The same can be said for ALB and total protein, two functional glomerular/tubular injury biomarkers in these studies (Vlasakova et al. 2014). While NGAL, ALB, and total protein were not as sensitive indicators of minimal kidney damage as were Kim-1 and CLU, the value of these biomarkers is apparent in their discrimination of the animals with only the higher grade kidney lesions when compared side by side with the levels of Kim-1 and CLU. NAG, a leakage biomarker for renal tubular injury, was not a useful or sensitive biomarker in TFV-treated monkeys or dogs, consistent with its performance in rat (Vlasakova et al. 2014).
In the dog study, the rise of serum biomarkers SCr and BUN in this study indicates early onset of the kidney injury and is consistent with the higher grade (grades 2–4) kidney pathology seen in dogs (Table 5). With such toxic effects being readily evident in the kidney with increases in SCr and BUN, this study is not a good test of comparative biomarker sensitivity. A study in dogs with a lower TDF dose resulting in milder kidney histomorphologic changes would be needed to test for comparative sensitivity of these urinary biomarkers in the dog. However, when comparing the dog with grade 2 kidney lesions (animal #002) with dogs with grade 4 kidney lesions (animals #008 and #084), we observed in general higher or much higher fold changes of urinary proteins (CLU, NGAL, ALB, total protein, and OPN) while fold changes of SCr were similar in all three dogs, suggesting potentially better monitoring capacity of urinary proteins. Marked inflammation was observed in the large intestine in 2 of the 4 treated dogs (animals #008 and #084). Urinary levels of several renal tubular toxicity biomarkers including Kim-1, NGAL, CLU, and OPN were shown to be upregulated upon the treatment of Lipopolysaccharide (LPS; Vlasakova et al. 2014). Therefore, we cannot exclude the possibility that the levels of urinary NGAL, CLU, and OPN measured in the dog study might be partially attributable to gastrointestinal inflammation observed in these two dogs.
Overall, the 3-fold threshold of treated values over the means of control and baseline levels worked well in this experiment, but it can be refined with further experience when assay standards are improved, historical baseline data from larger numbers of monkeys become available, and more rigorous statistical assessments of historical control values can be established.
The size of these nonrodent preclinical studies are deliberately kept small for animal welfare in accordance of the 3R’s guideline (replace, reduce, and refine). The performance of the urine renal tubular biomarkers tested in monkeys and dogs demonstrates high correlation with histomorphologic findings at the individual animal level supporting the usage of these biomarkers in monitoring kidney safety. The weight of evidence including the superior performance of these urine renal tubular safety biomarkers in rodents over serum biomarkers provides further support for the application of these biomarkers in toxicology studies conducted both in nonrodent species and in human. The urine samples collected and preserved from animals with documented histomorphologic anchoring in these studies also serve as a valuable resource for future testing of emerging newer urine biomarkers and new emerging assays for kidney safety.
The data presented here demonstrate the value of new urinary biomarkers in monitoring renal tubular toxicity in monkeys and dogs. It also opens the path for the investigation and application of these biomarkers in clinical settings to better monitor and understand kidney toxicities related to treatments of TDF, tenofovir alafenamide fumarate, and other nucleoside-based compounds especially in populations with potential for drug–drug interaction or other unrecognized underlying susceptibilities to kidney injury (Ray, Fordyce, and Hitchcock 2016). Furthermore, kidney lesions are observed sometimes in preclinical species without monitorable changes in BUN and SCr for various compounds in drug development, sometimes in a single test species, and sometimes with low-therapeutic exposure margins, establishing the further weight of evidence for monitoring kidney toxicity using such new kidney safety biomarkers helps advance biomarker acceptance and should open potential opportunities for various compounds to be tested in clinical trials without compromising patient safety.
In summary, we have demonstrated tenofovir-induced renal tubular injury in monkeys and dogs and for the first time systematically evaluated urinary kidney biomarker performance in these two species. We have shown that Kim-1 and CLU clearly outperformed BUN and SCr, while CysC, RBP4, B2M, NGAL, ALB, and total protein also performed better than BUN and SCr and added value when considered together with Kim-1 and CLU in the monkey study. Although higher severity of kidney injury observed in dog prevented a more critical comparison of relative performance of the biomarkers tested in that study, we showed that CLU, NGAL, CysC, OPN, ALB, and total protein performed comparably with SCr and better than BUN in the dog study. The superior sensitivity of urinary biomarkers such as Kim-1, CLU especially and also for NGAL, CysC, B2M, RBP4, OPN, ALB, and total protein provides rationale to further test their utility in the clinic not only with tenofovir prodrugs but also for maximizing drug development opportunities in general while ensuring patient safety.
Footnotes
Author Contributions
Authors contributed to conception or design (YG, KV, RP, HT, WG, FS); data acquisition, analysis, or interpretation (YG, KV, ST, HT, FP, FS); drafting the manuscript (YG); and critically revising the manuscript (KV, ST, RP, HT, FP, WG, FS). All authors gave final approval and agreed to be accountable for all aspects of work in ensuring that questions relating to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Declaration of Conflicting Interests
The authors declared no potential, real, or perceived conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
