Abstract
Inhibitors of Bruton’s tyrosine kinase (BTK) are under development as potential therapies for various autoimmune diseases. In repeat-dose toxicity studies, small-molecule BTK inhibitors (BTKi) have been reported to cause a constellation of histologic effects at the pancreatic endocrine–exocrine interface in male rats; however, similar findings were not reported in other species. Since the BTKi-induced pancreatic effect is morphologically similar to well-documented spontaneous changes (predominantly characterized by insular/peri-insular hemorrhage, pigment deposition, chronic inflammation, and fibrosis) that are known to vary by rat strain, we investigated potential strain-dependent differences in the pancreatic effects of a small-molecule BTKi, LY3337641. Following 13 weeks of LY3337641 treatment, Crl:CD(SD) rats were most sensitive, Crl:WI(Han) rats were of intermediate sensitivity, and Hsd:SD rats were least sensitive. These strain differences appear to be related to differences in rate of weight gain across strains and sexes; however, a definitive mechanism was not determined. This study demonstrated that BTKi-induced pancreatic effects were highly dependent on rat strain and correlated with differences in the incidence and severity of the spontaneous background change. When considered with the lack of pancreas effects in nonrat species, these changes in rats are unlikely predictive of similar changes in humans administered a BTK inhibitor.
Keywords
Introduction
Bruton’s tyrosine kinase (BTK) is a member of the TEC tyrosine kinase family of nonreceptor protein tyrosine kinases expressed in many hematopoietic cells including B cells, mast cells, and macrophages. BTK is essential for B-cell receptor signaling and acts as a crucial regulator of B-cell development, differentiation, activation, proliferation, migration, and signaling (Smith et al. 1994; Schwartzberg, Finkelstein, and Readinger 2005; Conley et al. 2009; Hendriks 2011; Vetrie et al. 1993). It is well established that B cells play a critical role in the development of a broad range of autoimmune diseases through secretion of autoantibodies, their antigen presenting functionality, and secretion of pro-inflammatory cytokines. Deficiency of BTK results in failure of B-cell maturation and failure to produce immunoglobulins, resulting in inadequate humoral immune responses. In addition, BTK is an essential mediator of both B-cell-dependent and myeloid cell–dependent inflammatory signals that facilitate the manifestation of rheumatoid arthritis (RA; Di Paolo et al. 2011; Chakravarty et al. 2013). Given the pleiotropic effects of BTK, its inhibition has a potential to improve the treatment of RA as well as other autoimmune diseases that involve lymphocyte and myeloid cell dysfunction such as Sjögren’s syndrome and systemic lupus erythematosus.
LY3337641 is an orally available small molecule that irreversibly binds and inhibits BTK. In nonclinical assessments to characterize its toxicity profile, LY3337641 was orally administered daily to Charles River Sprague-Dawley [Crl:CD(SD)] rats in 4-week, 13-week, and 26-week toxicity studies. These studies were conducted at doses that ranged from no observed adverse effect level (NOAEL) to maximum tolerated dose (MTD) and beyond. A major finding in these studies was a morphologically distinct complex of microscopic effects within and around pancreatic islets. These morphologic changes included islet and/or peri-islet hemorrhage, pigment (hemosiderin) deposition, chronic inflammation, and fibrosis that extended into the islet and/or adjacent exocrine tissue. Changes in the adjacent exocrine regions included exocrine lobular and acinar cell atrophy. These effects were almost exclusively present in male Crl:CD(SD) rats and only occurred in female Crl:CD(SD) rats at a low, non-dose-responsive incidence and severity in the 26-week study. The spectrum of these microscopic effects was consistent with spontaneous findings reported in control Crl:CD(SD) rats (Dillberger 1994; Imaoka, Jindo, and Takasaki 2013; Imaoka, Satoh, and Furuhama 2007; Chadwick et al. 2014; Hajdu and Rona 1967). Treatment with LY3337641 appeared to accelerate the onset of the spontaneous background finding, resulting in an increased incidence and severity over time. The findings involved a relatively low number of islets, were not associated with clinical chemistry changes suggestive of abnormal glucose regulation or exocrine pancreas injury, and were considered nonadverse in the context of the repeat-dose toxicology studies. These pancreas effects did not occur in cynomolgus monkey studies that ranged in duration from one month to nine months of treatment.
In assessing data from multiple repeat-dose toxicity studies using non-BTKi (BTKi, BTK inhibitors) molecules in rats that ranged from 3-month studies to 2-year carcinogenicity studies, the authors observed that the incidence and severity of the pancreatic islet finding were significantly higher in control male Crl:CD(SD) rats when compared to other rat strains (data not shown). Also, a recent report investigating the pancreatic effects of multiple reversible oral small-molecule BTKi showed that BTKi, regardless of BTK selectivity, induced effects similar to LY3337641 in Crl:CD(SD) rats (Erickson et al. 2017). Consistent with our observations, the pancreatic effects noted by Erickson et al. were also generally not dose-responsive and occurred predominantly in male rats. In addition, Erickson et al. observed in short-term (14-day) studies that Crl:CD(SD) rats were particularly susceptible to these effects when compared to Fischer 344 (F344 Fischer) and Charles River Wistar-Han [Crl:WI(Han)] rats.
To characterize further this apparent species/sex/strain-specific change, we conducted a 13-week repeat-dose investigative study in three different strains of rats [Crl:CD(SD), Crl:WI(Han), and Harlan Sprague-Dawley (Hsd: SD)] administered daily doses of LY3337641. Hsd: SD was selected to evaluate another strain with a Sprague-Dawley background since the spontaneous pancreatic findings and similar BTKi-related pancreatic effects are mostly reported in the Crl:CD(SD) strain. Aims of this study included (1) comparing the incidence and severity of these spontaneously occurring pancreatic findings across three rat strains, (2) comparing the effects of treatment with LY3337641 on these effects across these rat strains, and (3) determining whether these changes resulted in functional alteration in both endocrine (glucose homeostasis) and exocrine pancreas.
Materials and Method
Test Article
BTK small-molecule inhibitor, LY3337641 (HM71224), was synthesized as a dihydrochloride salt at Hanmi Fine Chemical Co., Ltd. (South Korea) and formulated for oral administration in the vehicle: 0.5% (w/v) 400 cP methyl cellulose (Sigma Aldrich, St. Louis, MO) in reverse osmosis water. The same vehicle served as the control article. LY3337641 dihydrochloride is referred to as LY3337641 throughout this article.
Experimental Models
The 4-week, 13-week, and 26-week rat studies with LY3337641 were conducted at Laboratory of Pharmacology and Toxicology (LPT; Hamburg, Germany), which is fully accredited by the German Good Laboratory Practice (GLP) authorities, and were performed in strict accordance with the guidelines in the European Animal Welfare Regulations (European Union [EU] Welfare Standards: Directive 2010/63/EU of the European Parliament and of the Council of September 22, 2010—Protection of animals used for scientific purposes—2010/EU, L276), which were identical to those of the Association for Assessment and Accreditation of Laboratory Animal Care (AAALAC).
The multistrain rat study was conducted at Covance Laboratories, which is fully accredited by the AAALAC, and was performed in strict accordance with the guidelines in the National Institutes of Health Guide for the Care and Use of Laboratory Animals.
All study designs considered the replacement, reduction, and refinement principals, and appropriate efforts were made to reduce animal suffering. All procedures in the protocol were approved by the local Institutional Animal Care and Use Committees.
The focus of this article is to discuss the novel findings of the investigative multistrain rat study. A high-level description of the preceding GLP repeat-dose studies with LY3337641 is below followed by a more detailed description of the multistrain study.
GLP Repeat-dose Toxicology Studies
Three repeat-dose toxicology studies of 4-week, 13-week, and 26-week duration were conducted at LPT (Hamburg, Germany) and had similar live phase study designs but differed in duration, Toxicokinetics sample collections, and pathological end points. All three studies were conducted in male and female Sprague-Dawley [Crl:CD(SD)] rats from Charles River Laboratories (Sulzfeld, Germany). The rats were 5 to 7 weeks of age at study start. Animals received once daily (QD) dosing by oral gavage using a dose volume of 10 ml/kg. Twice daily clinical observations and weekly body weights were collected for all animals. Table 1 contains a summary of the design of these toxicology studies and the investigative study discussed in the article.
Summary of Rat Study Designs.
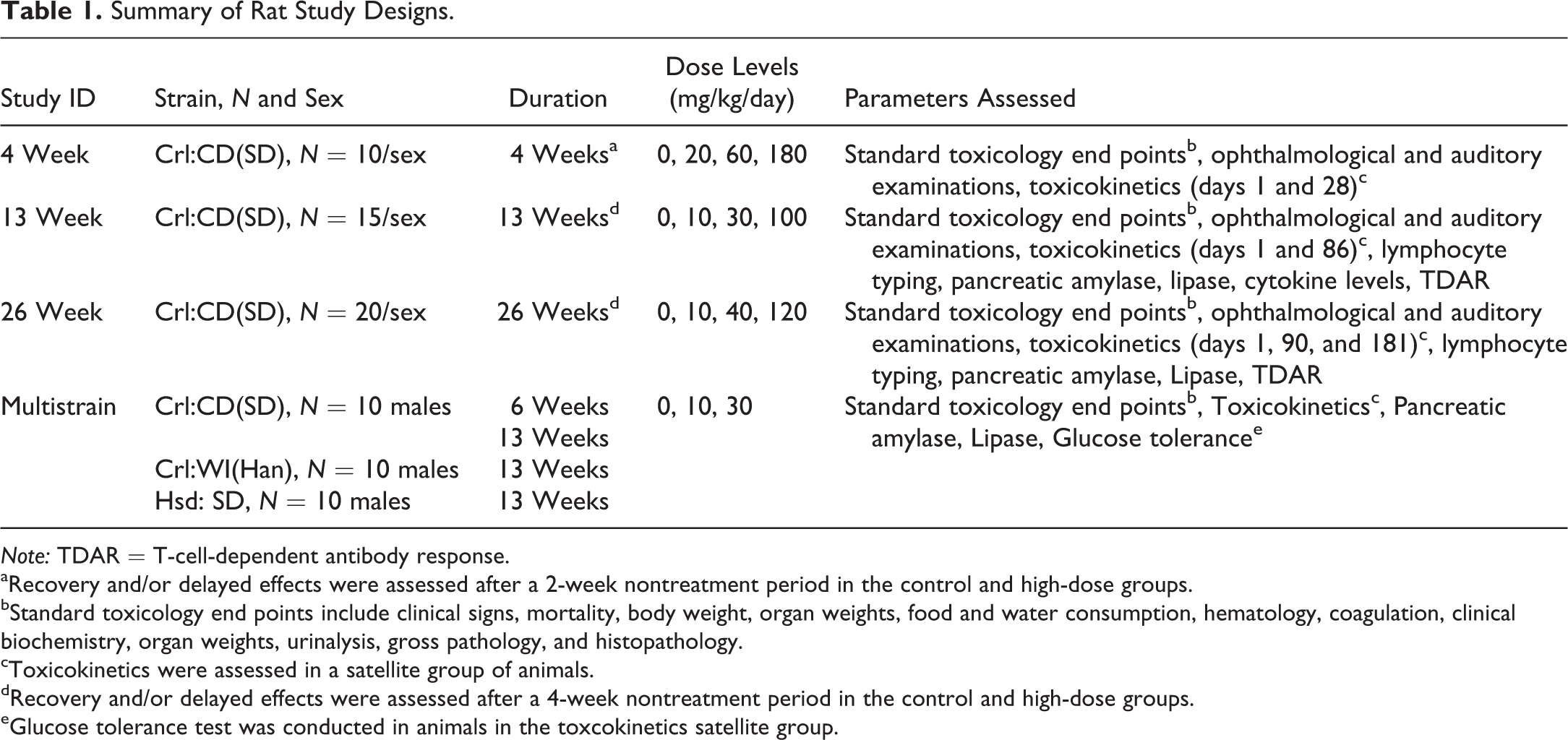
Note: TDAR = T-cell-dependent antibody response.
aRecovery and/or delayed effects were assessed after a 2-week nontreatment period in the control and high-dose groups.
bStandard toxicology end points include clinical signs, mortality, body weight, organ weights, food and water consumption, hematology, coagulation, clinical biochemistry, organ weights, urinalysis, gross pathology, and histopathology.
cToxicokinetics were assessed in a satellite group of animals.
dRecovery and/or delayed effects were assessed after a 4-week nontreatment period in the control and high-dose groups.
eGlucose tolerance test was conducted in animals in the toxcokinetics satellite group.
Rat Multistrain Investigative Study
An investigative repeat-dose toxicity and toxicokinetic study (hereinafter referred to as multistrain study) that focused on pancreatic changes in three strains of male rats administered LY3337641 QD by oral gavage for 13 weeks was conducted (Table 1). Only male rats were used because LY3337641-related effects were noted at a much higher incidence in male rats in the previous toxicology studies. In addition, spontaneous pancreatic changes of the nature described in this article occur predominantly in male rats. The three rat strains used were Sprague-Dawley [Crl:CD(SD), Hsd: Sprague-Dawley (Hsd: SD), and Wistar-Han (Crl:WI(Han)]. The Crl:CD(SD) and Crl:WI(Han) were purchased from Charles River Laboratories (Raleigh, NC). The Hsd: SD rats were purchased from Envigo RMS, Inc. (Indianapolis, IN). At study start the animals were 6 to 7 weeks old. Animals received QD dosing by oral gavage using a dose volume of 10 ml/kg at dose levels of 0 (vehicle control), 10, and 30 mg/kg. The two dose levels of LY3337641 were the same as the low- and mid-doses of the previous 13-week repeat-dose toxicity study. These dose levels and duration of treatment had the highest overall incidence and severity of changes across previous studies and hence provided the best doses to reproduce the pancreatic changes. Daily clinical observations and weekly body weights were collected for all animals. Toxicokinetics, glucose tolerance, clinical pathology, and histopathology (pancreas only, details below) were assessed at the end of the study (13 weeks) for all three strains and at an interim 6-week time point for the Crl:CD(SD). Body weight and weights of brain and pancreas were also recorded.
Clinical pathology
Rats were fasted overnight prior to blood sampling for hematology, coagulation, and clinical chemistry via jugular vein on the days of scheduled sacrifices. Samples intended for hematology tests and coagulation were collected using potassium EDTA and sodium citrate, respectively. Samples collected for clinical chemistry were without anticoagulant.
Glucose tolerance testing (GTT)
Ten LY3337641-treated and 3 control animals were used for this analysis from each of the three strains. Animals used for GTT were fasted overnight and orally administered one dose of dextrose (2,000 mg/kg) at a dose volume of 10 ml/kg on the last day of the dosing phase. Approximately, 0.2 ml of blood was collected from a jugular vein into a serum separator tube (SST; no additive) before the administration of dextrose and at approximately 0.25-, 0.5-, 1-, and 2-hr post-dextrose administration. The blood samples were centrifuged within 1 hr of collection, and serum was taken for analysis. The samples were analyzed using the hexokinase method on a Roche Diagnostic Modular P chemistry analyzer.
Histopathology
Necropsies were performed on the day following the last dose of the test article. Necropsy on a subgroup of Crl:CD(SD) rats was also performed at the interim time point of 6 weeks. All collected tissues were macroscopically examined, and any observations were recorded prior to fixation and processing. An expanded histologic survey of the pancreas was performed to increase the ability to detect small lesions. Specifically, six evenly spaced transverse sections of pancreas, two each from proximal and distal head, body, and tail were trimmed and placed into separate cassettes, fixed in 10% neutral-buffered formalin and paraffin embedded. From each block of pancreas (six total), one slide was prepared for routine hematoxylin and eosin staining and one slide was prepared for Perl’s Prussian blue staining. It should be noted that for all the other repeat-dose toxicity studies listed in Table 1, only one section of pancreas was collected and analyzed, and the region of pancreas sampled was not specified in these studies. The severity of the findings was graded on a scale of none (0), minimal (1), slight (2), moderate (3), marked (4), and severe (5). All the slides in all studies were evaluated by experienced toxicologic pathologists.
Statistics
For GTTs, analysis of variance and Dunnett’s t-test were used for pairwise comparisons between each treated and control group. Statistical analysis was not performed for semiquantitative analysis of histopathological changes in the pancreas because of the general consensus in the toxicologic pathology community that grading scales are often nonlinear, and the assigned number is only semiquantitative and is based on variable and subjective criteria (Mann et al. 2012).
Results
Single Rat Strain Repeat-dose Toxicology Studies
LY3337641 was generally well tolerated in rats at dose levels up to 100 mg/kg for 13 weeks and 40 mg/kg for 26 weeks. No effects on body weights occurred in the initial repeat-dose studies at dose levels up to 120 mg/kg in females (26-week study) and up to 100 mg/kg in males (13-week study). Slight body weight decreases were observed in males treated with 120 mg/kg (26-week study) and in males and females treated with 180 mg/kg (4-week study). Growth curves from the 26-week rat study (Figure 1) are representative of those in the 4- and 13-week studies. Mortality occurred at 180 mg/kg in one male in the 4-week study and in 5 animals in the 26-week study at 120 mg/kg. The NOAEL was 60, 30, and 40 mg/kg in the 4-, 13-, and 26-week studies, respectively. Plasma exposure levels were consistent across studies relative to the administered dose level.
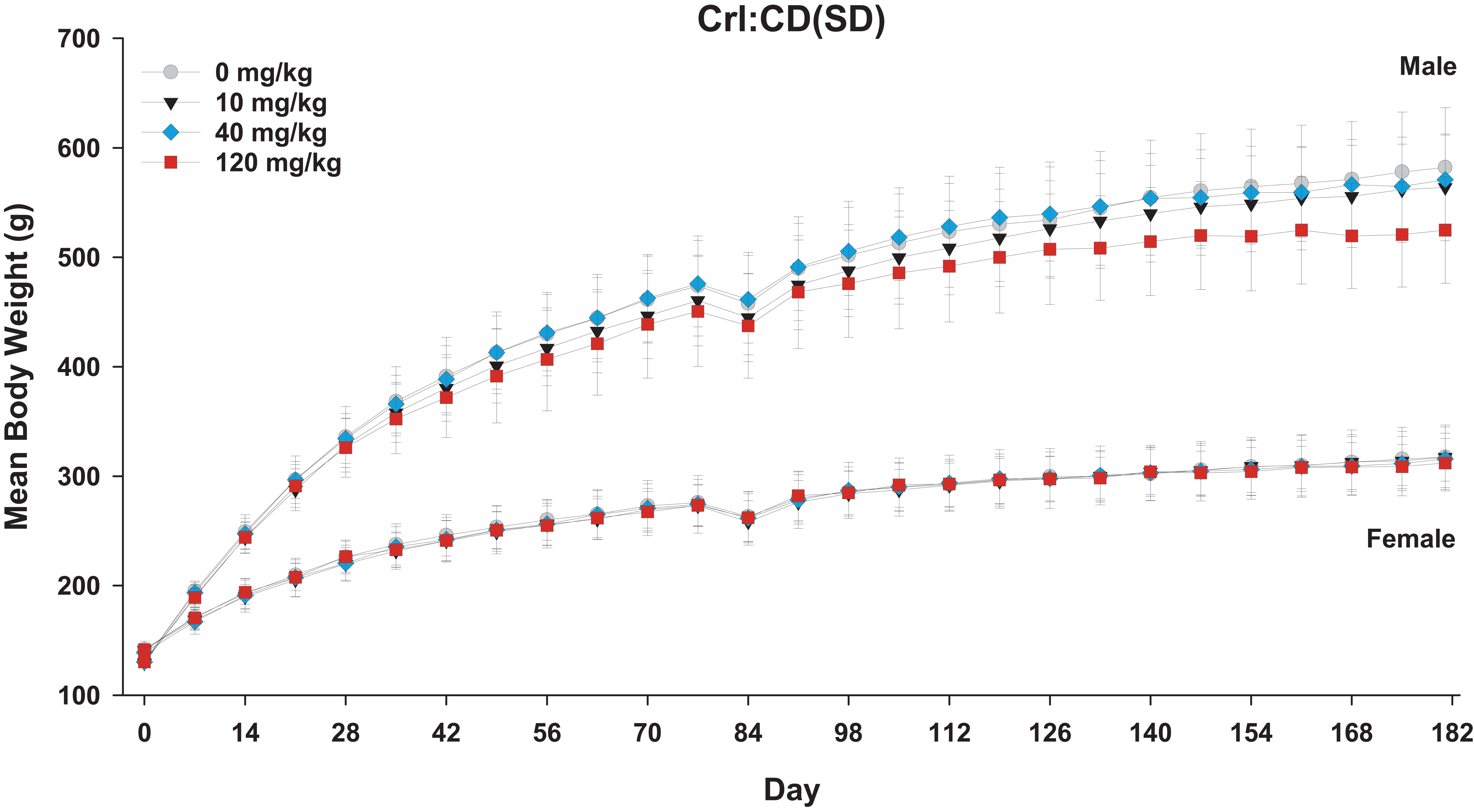
Mean body weights for male and female Crl:CD(SD) rats (±1 standard deviation, n = 20–25/sex) treated daily with vehicle or LY3337641 for 26 weeks. Body weights were measured once per week. Growth curves for rats treated for 4 weeks and 13 weeks were very similar (data not shown).
Pancreatic Effects in the Single Rat Strain Repeat-dose Toxicology Studies
Rat repeat-dose toxicity studies, in which daily doses of LY3337641 were administered orally, are summarized in Table 1. The duration of these studies ranged from 4 to 26 weeks. In all these studies, a morphologically distinct complex of LY3337641-related microscopic findings in the pancreas (predominantly characterized by insular/peri-insular hemorrhage, pigment deposition, chronic inflammation, and fibrosis) in males was non-dose-dependent and affected the islet and/or adjacent exocrine tissue, resulting in the disruption of the normal morphology. Majority of the islets within the pancreas section were not affected. For purpose of clarity, the morphologic findings listed above are defined in detail in the Investigative Study section.
The incidence and severity of the pancreatic effects in males from these studies are summarized in Table 2. Morphologic findings in the pancreas were present only in LY3337641-treated animals in the 4- and 13-week studies were consistent with spontaneous background changes that occur in the pancreas of slightly older male Crl:CD(SD) rats. By 26 weeks, these findings were also present in control males, although at a lower incidence and severity than observed in LY3337641-treated males. These microscopic findings involved a low number of islets, were non-dose-dependent, were present primarily in males, and were considered nonadverse in these studies. Reversibility was not assessed in the 4-week study as the pancreatic effects were not present in the control and high-dose group. Following a 4-week recovery phase in the studies of longer duration, the pancreatic effects were completely reversible in the 13-week study and showed partial reversibility in the 26-week study. At the end of the recovery period in both studies, these pancreas findings were also present in control animals. In females, pancreatic effects were absent in the 4-week studies and rare incidences of minimal inflammation and islet cell hyperplasia occurred in treated females from the 13-week study. The 26-week study had very low incidences of acinar cell atrophy, pigment deposition, and chronic inflammation of minimal to slight severity in females relative to controls.
Incidence and Severity of Selected Microscopic Pancreatic Findings in Male Crl:CD(SD) Rats Treated with LY3337641.
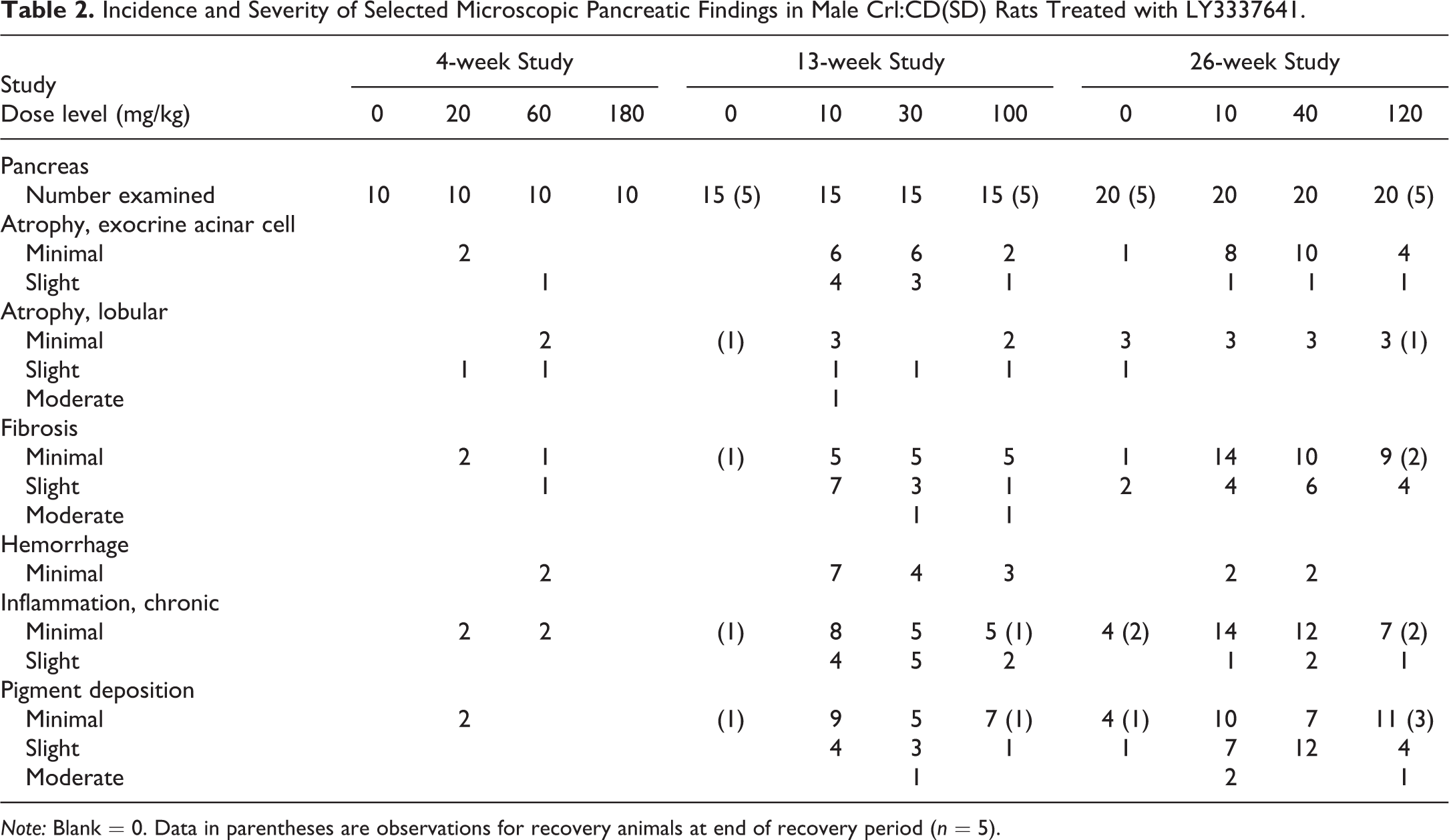
Note: Blank = 0. Data in parentheses are observations for recovery animals at end of recovery period (n = 5).
Fasting glucose levels were not affected by treatment in the 4-week study. Fasting glucose levels were decreased at the high dose (6–20%) in males and females (similar magnitude in both sexes) from the 13- and 26-week studies, despite the fact that morphological pancreatic effects were noted only in males. Amylase and lipase activities did not show treatment-related changes in these studies.
Multistrain Rat Study
An investigative multistrain study that focused of pancreatic changes in three strains of male rats administered LY3337641 QD by oral gavage for 13 weeks was conducted. Study design details are described in the Materials and Method section and in Table 1. No test article–related clinical observations, changes in food consumption, or changes in pancreas weights occurred in any of the three rat strains [Crl:CD(SD), Hsd: SD, and Crl:WI(Han)]. No macroscopic findings were observed at terminal necropsy. Systemic exposure to LY3337641 was consistent across the three strains.
Body weight changes
Treatment with LY3337641 had no effect on the growth curves within a particular strain of rats; however, the rate of weight gain in Crl:CD(SD) rats was significantly higher than that in the other two rat strains in this multistrain rat study (Figure 2). The mean body weights at the beginning of the study for Crl:CD(SD) rats were lower than the other two strains, but during the treatment period Crl:CD(SD) rats including those in the control group had a rapid body weight gain that resulted in higher body weights on day 15, had a clear separation from the body weights of other two strains by day 22 and was significantly higher by the end of the study. This observation highlighted the rapid and sustained growth (body weight gain) in this strain.
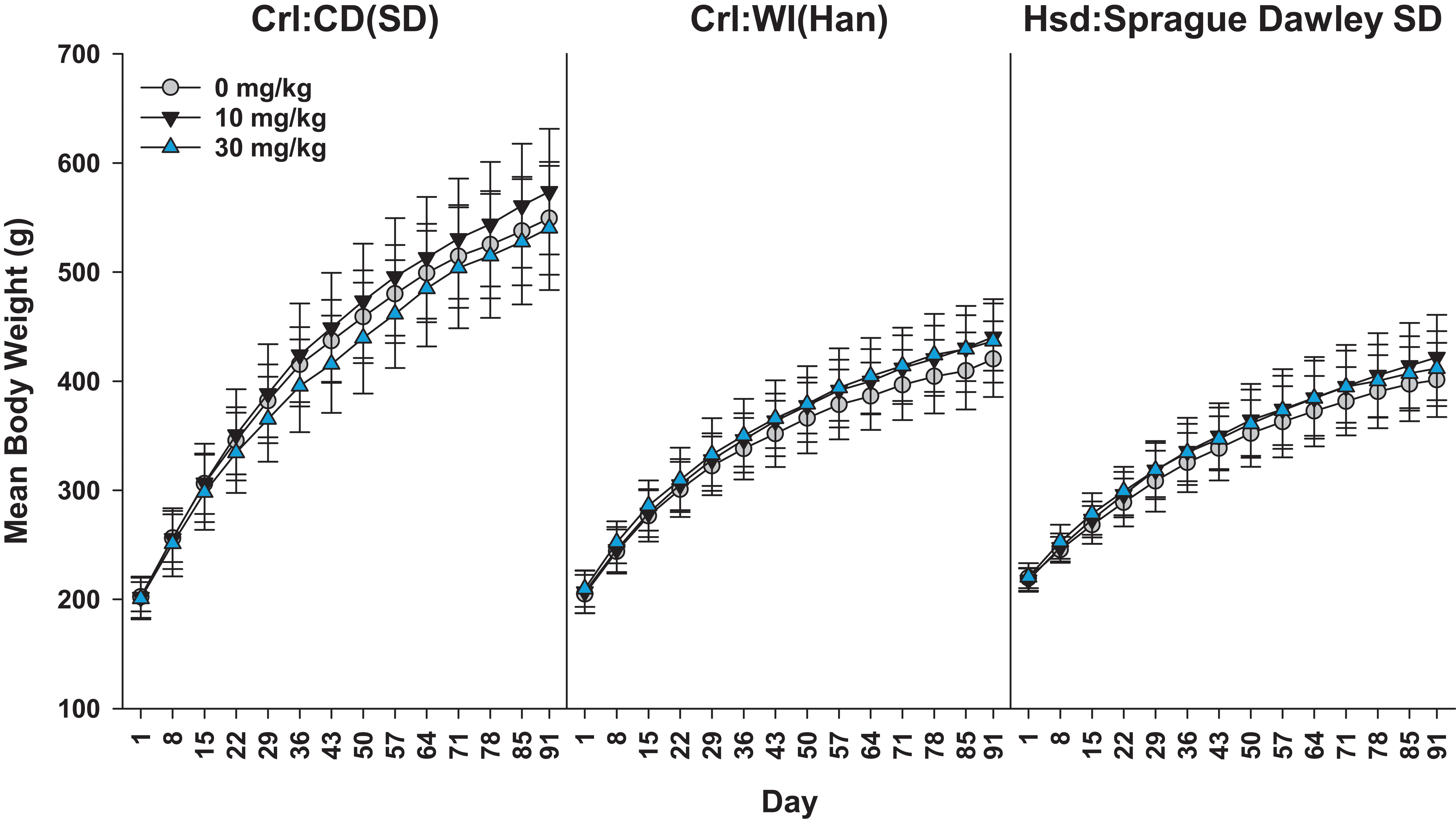
Mean body weights for male Crl:CD(SD), Crl:WI(Han), and Hsd: SD rats (±1 standard deviation, n = 10–20) treated daily with vehicle or LY3337641 for 13 weeks. Body weights were measured once per week.
Histological changes in the pancreas
Morphologic characterization
Across each time interval and strain, when an individual component of the pancreatic findings occurred the histologic features were similar. As such, the following section provides an overview of these morphologic features, and subsequent sections provide comparisons between the 6- and 13-week treatment durations in the Crl:CD(SD) as well as comparisons among the three rat strains. The findings described below primarily occurred within and around islets (insular/peri-insular) and often extended into the adjacent exocrine pancreas. This strain comparison (multistrain) study included examination of three regions of the pancreas (approximate head, body, and tail); pancreas findings were observed in all three regions suggesting no site predilection. In some cases, the findings were only present in one of the three regions of the pancreas, and within an individual region, not all of the islets were affected. The occurrence of both acute (hemorrhage) and chronic (fibrosis) findings, occasionally within different islets in the same animal, suggests a polyphasic development of these effects.
Hemorrhage was characterized by extravascular accumulations of erythrocytes and fibrin that were predominantly within and around islets (Figure 3A and B). Pigment deposition was characterized by infiltrates of macrophages with intracytoplasmic golden-brown pigment (sideromacrophages) and corresponded with the presence of Prussian blue–positive cells in the Perl’s Prussian blue –stained sections, consistent with identification of the pigment as hemosiderin (Figure 4A–F). Chronic inflammation was generally characterized by accumulations of lymphocytes, plasma cells, and macrophages and immature fibrous connective tissue within and around islets (Figure 3D–F); chronic inflammation often obscured or distorted the round to oval shape of the islets (Figure 3D and F). Fibrosis was generally characterized by the presence of variable amounts of collagen within and around islets (Figure 3C–F). Exocrine acinar cell atrophy was characterized by variable loss and atrophy of peri-insular acinar tissue. This was considered distinctly different from lobular atrophy, characterized by randomly distributed focal lobular areas of acinar atrophy.
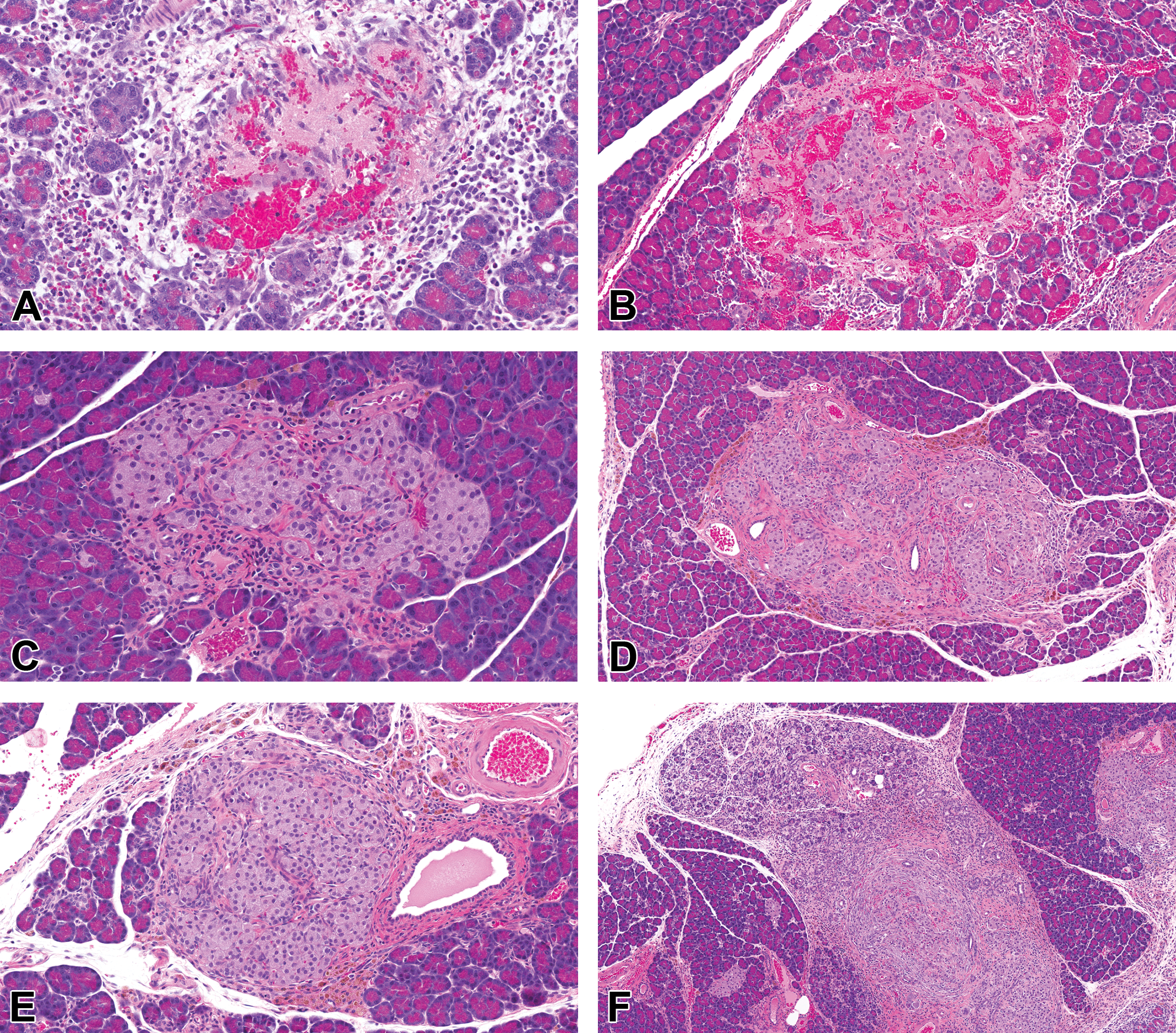
Pancreatic islets and adjacent exocrine pancreas of control (A, C, E) and LY3337641-treated (B, D, F) Crl:SD(SD) rats. In both control (A) and treated (B) rats, varying degrees of hemorrhage and fibrin exudation within and around islets were often accompanied by mononuclear cell infiltrates and minimal acinar cell atrophy of the adjacent exocrine pancreas. The morphologic appearance was similar at both the 6-week and 13-week time points. Fibrous connective tissue dissected some islets in both control (C, E) and treated (D, F) rats, and was accompanied by varying degrees of chronic insular and peri-insular inflammation, hemorrhage, and pigment deposition. In some cases, there was prominent distortion of islet architecture and acinar cell atrophy of the adjacent exocrine pancreas (F). (A) Control, 6 weeks. (B) LY3337641-treated, 13 weeks. (C) Control, 13 weeks. (D) LY3337641-treated (30 mg/kg), 13 weeks. (E) Control, 13 weeks. (F) LY3337641-treated (10 mg/kg), 13 weeks.
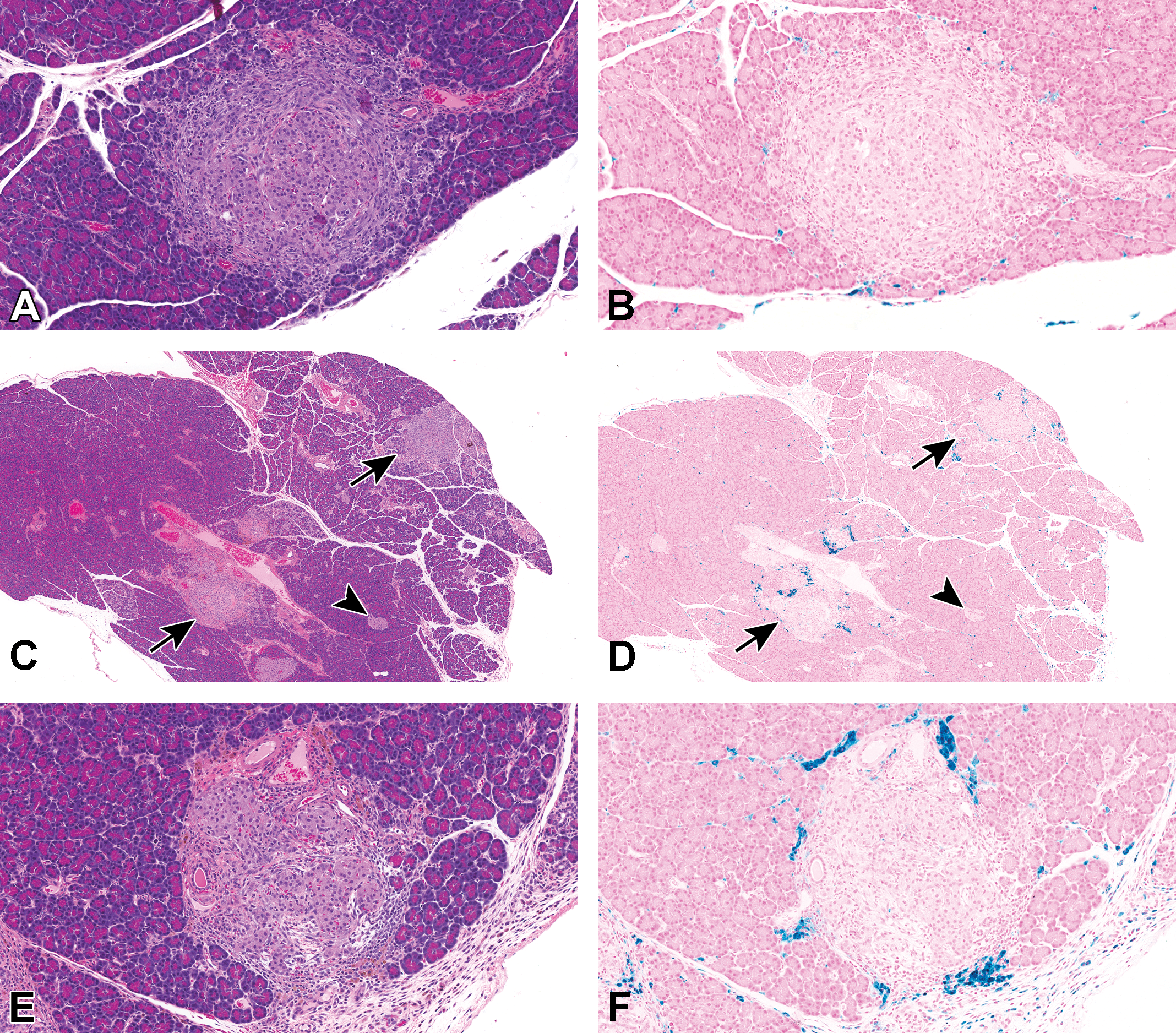
Hematoxylin and eosin (A, C, E) and Perl’s Prussian blue (B, D, F)–stained adjacent sections of pancreas from control (A, B) and LY3337641-treated (C-F) Crl:CD(SD) rats. In both control and treated rats, there were peri-insular aggregates of macrophages containing golden brown pigment that was positive (blue) for ferric iron (sideromacrophages). Note the presence of both unaffected (arrowheads) and affected (arrows) islets in the same section (C and D, Crl:CD(SD), 10 mg/kg, 13 week time point). (A, B) Control, 13 weeks. (C, D) LY3337641-treated (10 mg/kg), 13 weeks. (E, F) LY3337641-treated (10 mg/kg), 13 weeks.
Evaluation of the Crl:CD(SD) strain following 6 and 13 weeks of treatment
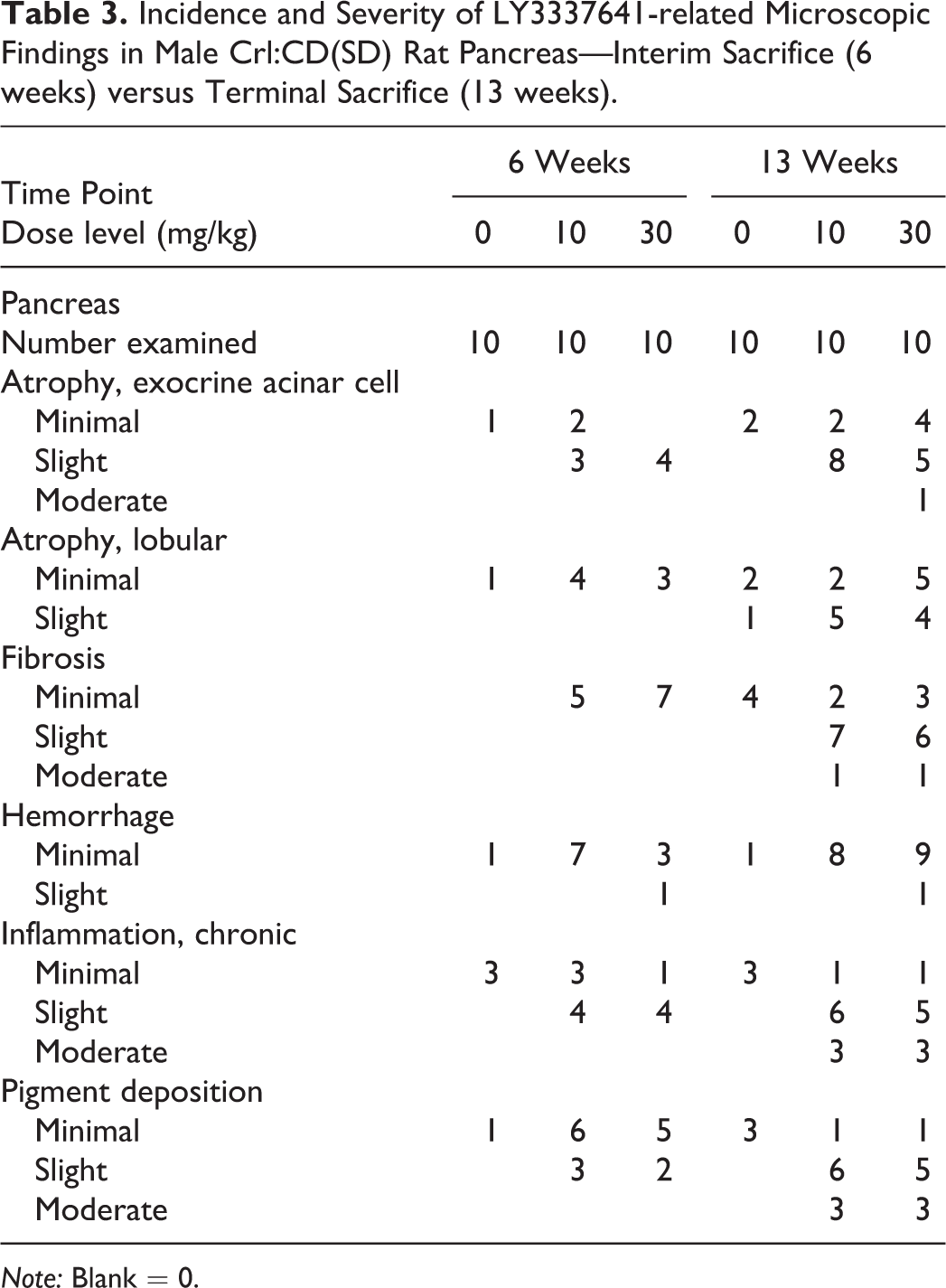
In an attempt to characterize the progression of pancreas effects over time, Crl:CD(SD) rats were examined following both 6 and 13 weeks of treatment (Table 3). At the 6-week time point, LY3337641-related effects were observed for each of the pancreatic findings described above. The incidence and severity of the findings were generally similar in rats administered either 10 or 30 mg/kg confirming prior observations that the occurrence of these findings is, generally, nondose responsive. Fibrosis was not observed in the pancreas of control rats; however, all other findings attributed to LY3337641 treatment represented an increase in the incidence and/or severity of changes that were observed in at least one control animal. At 6 weeks, these changes were graded as minimal or slight (grades 1 and 2 of a 5-point scale).
Incidence and Severity of LY3337641-related Microscopic Findings in Male Crl:CD(SD) Rat Pancreas—Interim Sacrifice (6 weeks) versus Terminal Sacrifice (13 weeks).
Note: Blank = 0.
At the 13-week interval, LY3337641-related microscopic findings in the pancreas occurred at a greater incidence and/or severity compared to the 6-week time point (Table 3). At 13 weeks, the severity grades ranged from minimal to moderate (grades 1–3 of a 5-point scale) with slight and moderate findings more frequent than at 6 weeks. Similar to the 6-week time interval, the findings were generally similar in rats administered 10 or 30 mg/kg. Although the incidence and severity increased from 6 to 13 weeks, the basic morphology of the finding was similar at each time point and there was no apparent difference in occurrence of findings that would be considered more acute (hemorrhage) to those considered more chronic (fibrosis). It is important to note that at the 13-week time point, all components of the pancreas findings were observed in at least one control animal and the overall incidence and severity of the lesion components in controls were greater at 13 weeks than at 6 weeks. The observations in control rats are consistent with prior observations of an increasing frequency of these changes with increasing age (Imaoka, Satoh, and Furuhama 2007).
Comparison of pancreas effects in Crl:CD(SD), Hsd: SD, and Crl:WI(Han) at 13 weeks
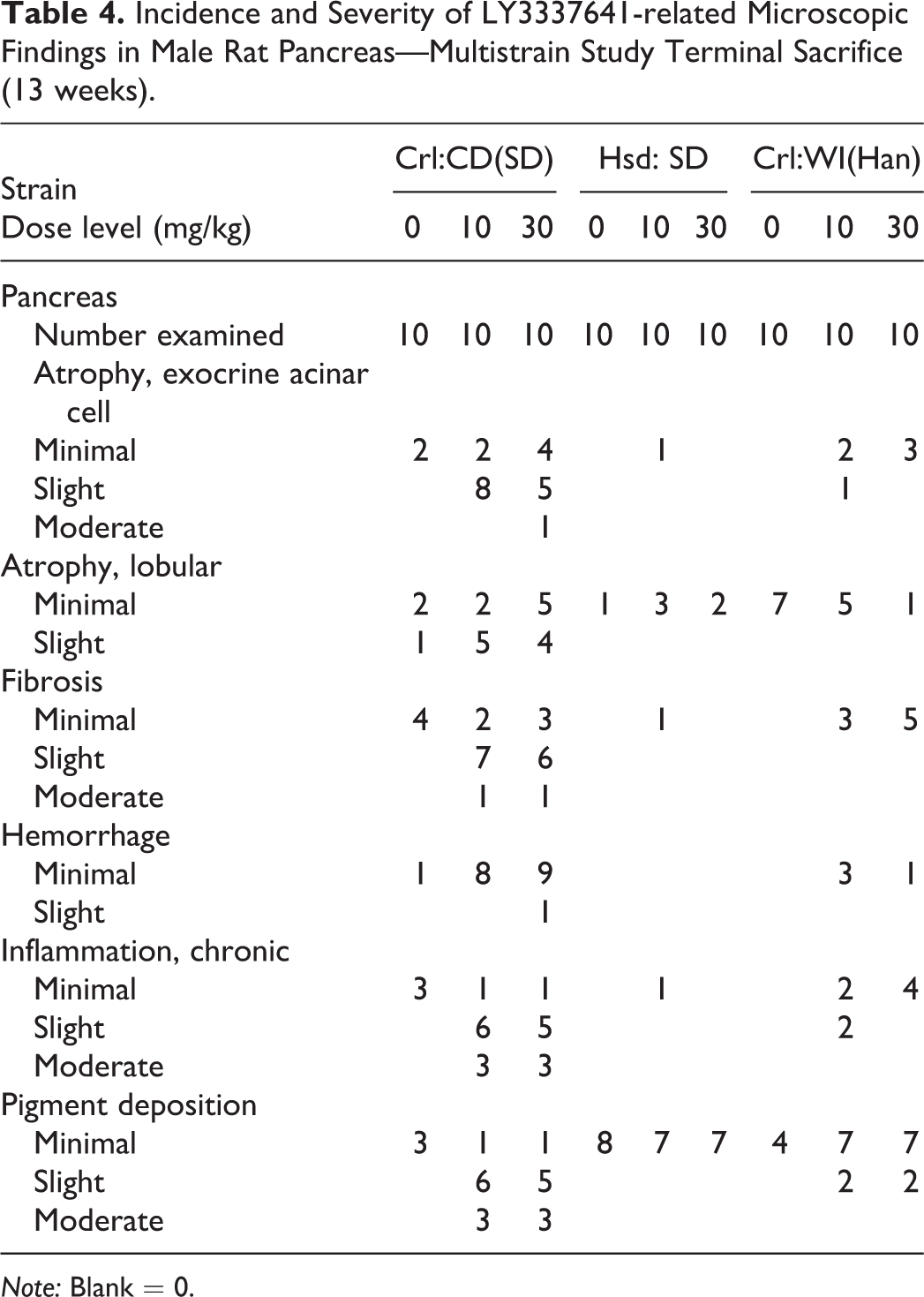
The incidence and severity of LY337641-related pancreas effects treatment were greatest in the Crl:CD(SD) strain (Table 4). In the other strain of Sprague-Dawley rat assessed (Hsd: SD), no LY3337641-related peri-islet effects occurred. The minimally increased incidence of lobular atrophy observed in LY3337641-treated Hsd: SD was suggestive of a test article effect but was difficult to interpret given the low incidence in both control and LY337641-related rats. In control Hsd: SD rats, the only relevant peri-islet finding was minimal pigment deposition (Figure 5A and B), whereas Crl:CD(SD) controls had a low incidence of all the peri-islet findings. The incidence/severity of pancreatic effects in the Han Wistar [Crl:WI(Han)] rats was intermediate between the two Sprague-Dawley rat strains. In terms of LY3337641-induced effects, Crl:WI(Han) rats developed the same spectrum of islet/peri-islet findings as the Crl:CD(SD) rats (Figure 5C–F); however, the overall incidence and severity of the effects were lower in the Crl:WI(Han) rats (Table 4). The control Crl:WI(Han) rats were similar to the Hsd: SD strain control rats in that pigment deposition was the only islet/peri-islet change present. The incidence of lobular atrophy was highest in control Crl:WI(Han) rats, and LY337641 treatment did not increase the incidence nor the severity of this change.
Incidence and Severity of LY3337641-related Microscopic Findings in Male Rat Pancreas—Multistrain Study Terminal Sacrifice (13 weeks).
Note: Blank = 0.
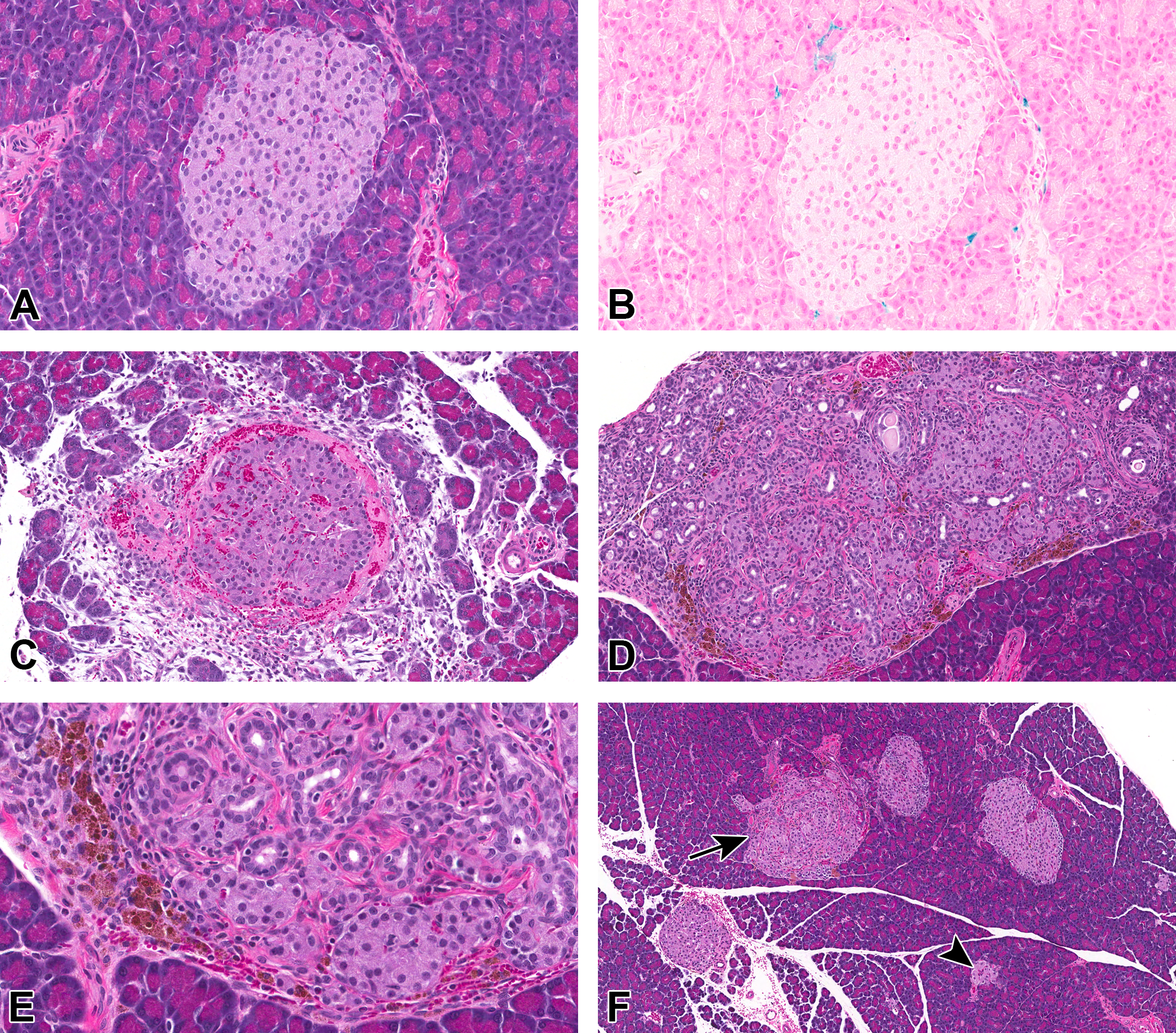
Findings in the pancreas of Hsd:(SD) (panels A and B) and Crl:WI(Han) (panels C–F) rats. In Hsd:(SD) control rats, islets were most often unremarkable (A) and the most common observation in controls were small peri-insular accumulations of sideromacrophages (B, Perl’s Prussian blue). In Crl:WI(Han) rats, the morphology of the islets in both controls and treated rats was similar to those observed in Crl:(CD) rats. Hemorrhage, fibrin, and peri-insular inflammation were frequently observed (C, Crl:WI(Han), 10 mg/kg, 13-week time point). Insular and peri-insular inflammation was often accompanied by pigment deposition in macrophages (D and E, Crl:WI(Han), 10 mg/kg, 13-week time point). In panel D, note the atrophy of the adjacent exocrine pancreas. As was the case for Crl:CD(SD) rats, both affected (arrows) and unaffected (arrowhead) islets were present in the same section (Panel F, Crl:WI(Han), 30 mg/kg, 13-week time point). (A) Control Hsd:(SD), 13 weeks. (B) Control Hsd:(SD), 13 weeks, Perl’s Prussian blue. (C) Crl:WI(Han), LY3337641-treated (10 mg/kg), 13 weeks. (D) Crl:WI(Han), LY3337641-treated (10 mg/kg), 13 weeks. (E) Crl:WI(Han), LY3337641-treated (10 mg/kg), 13 week. (F) Crl:WI(Han), LY3337641-treated (30 mg/kg), 13 weeks.
Oral glucose tolerance test and other clinical pathology parameters
In order to determine whether the histological finding in and around the islets translated into impairment of glucose homeostasis, oral GTT was performed on day 91 in all groups in the rat multistrain study. No obvious test article–related effects were observed in serum glucose concentration in any of the three strains at the end of 13 weeks. Inspection of individual animal glucose data identified marked individual animal variability in both the control and treated groups; however, no effects of the test article were detected. There were no treatment-related effects on fasting glucose levels, amylase activity, or lipase activity in this study.
Discussion
In toxicity studies in male and female rats conducted to support the clinical development of LY3337641, a complex set of microscopic findings centered on the pancreatic endocrine–exocrine interface were observed. The primary morphologic features included peri-islet hemorrhage, pigment deposition, chronic inflammation, and fibrosis; acinar cell atrophy also occurred in the adjacent exocrine tissue. The incidence of lobular atrophy, which was characterized by randomly distributed focal lobular areas of acinar atrophy, was not clearly atered by LY3336741 treatment in these single-strain studies as evidenced by the lack of meaningful difference from controls in the 26-week study (Table 2). In studies with durations ranging from 4 to 26 weeks, the effects were largely limited to male rats and were nondose-responsive. This is in contrast to the fact that there were no appreciable differences in systemic exposure between males and females and increases in systemic exposure were, generally, dose-proportional (data not shown). The morphology of these effects was very similar to the well-described spontaneously occurring background finding in the pancreas of the Crl:CD(SD) strain that have been shown to increase with age (Reaven and Reaven 1981; Dillberger 1994; Imaoka, Satoh, and Furuhama 2007; Hajdu and Rona 1967). Based on these similarities in morphologic appearance and the observations of the authors that different rat strains have differing background incidences of a variety of findings, including islet-centric lesions, we hypothesized that there may be strain-specific differences in susceptibility to LY337641-induced pancreatic effects and designed a study to compare this effect in three commonly used outbred rat strains.
The results of this strain-comparison study clearly demonstrate that individual rat strains vary significantly in their susceptibility to the pancreatic effects of the BTK inhibitor LY3337641. The incidence and severity of this effect were significantly higher in the Crl:CD(SD) strain when compared to Crl:WI(Han) and Hsd: SD. Surprisingly, the two Sprague-Dawley strains were the most divergent, with the Crl:CD(SD) being the most susceptible of the three strains tested and Hsd: SD displaying the least susceptibility. In Hsd: SD rats, there were no effects on islet-centric lesions. The only potential effect of LY3337641 was an equivocal increase in the incidence of lobular atrophy. The Crl:WI(Han) strain had an intermediate susceptibility to pancreatic effects. In the susceptible strains, there was very little difference between the low- (10 mg/kg) and high-dose (30 mg/kg) levels, but there was a clear difference in the severity of the effect in both treatment groups compared to the concurrent control groups. The highest background incidence of the similar, spontaneous pancreatic finding in controls was in the strain most susceptible to the LY3337641 effects, indicating that the LY337641 effect represents an earlier onset and exacerbation of the background finding that is prominent in this strain.
The current study is not the first to suggest that susceptibility to the pancreatic effects of a BTK inhibitor varies by rat strain. A recent report investigating the pancreatic effect of other small-molecule BTKi showed that that Crl:CD(SD) rats were the most susceptible to this pancreatic effect, F344 Fischer rats had intermediate (but minimal) susceptibility and Crl:WI(Han) rats had the lowest susceptibility that appeared only with longer treatment (Erickson et al. 2017). Based on the data presented in this article and in Erickson et al., the susceptibility of rat strains to these pancreatic effects would be ranked as follows: Crl:CD(SD) > F344 Fischer > Crl:WI(Han) > Hsd: SD. To our knowledge, the current study is the first to show that two different strains of Sprague-Dawley can have different incidences of the spontaneous background pancreas finding as well as differing susceptibility to BTK-induced pancreatic effects.
The studies described in this article also provided an understanding of the progression of the lesions with increased duration of dosing. In the multistrain rat study, the incidence and severity of pancreatic effects increased as dosing duration increased from 6 to 13 weeks (Table 3); however; this effect apparently reached a plateau as the data from the repeat-dose toxicity studies did not suggest a significant increase in the severity as treatment duration extended to 6 months (Table 2). The differences in the incidence and severity of the pancreatic effects following 13 weeks of treatment between the original 13-week study (Table 2) and the multistrain comparison study (Tables 3 and 4) are likely related to the increased sampling of the pancreas in the multistrain study (6 pancreas sections/animal) compared to 1 section/animal in the 13-week study. It is interesting to note that across both our investigations of LY3337641 and those reported by Erickson et al., at any given time point, the peri-islet findings range from those that would typically be considered more acute (hemorrhage) to those that require a longer period of time to develop (fibrosis). Furthermore, a single pancreas section may have unaffected islets, islets with hemorrhage as the only finding, and islets that have more chronic features consisting mainly of fibrosis.
An additional objective of the multistrain comparison study was to assess the potential impact of these pancreatic findings on either markers of exocrine cell injury (amylase and lipase) or islet cell function (oral GTT). In our study of LY3337641, these markers did not suggest exocrine pancreatic injury or functional impairment of the islet subsequent to these pancreatic changes. No changes attributable to LY3337641 were present in fasting glucose levels, the oral glucose tolerance test, or in amylase and lipase activities. On this basis, there is no clear evidence that these changes represent a test article–related adverse effect in rats. The lack of a functional effect may correlate to the observations that, even in the more severely affected animals, there are a proportion of islets that are not affected and there may be adequate islet cell reserve capacity. These findings are consistent with Erickson et al.’s observation that mild glucose dysregulation levels observed after treatment with GDC-0853 at 100 mg/kg/day for 28 consecutive days did not correlate to the pancreatic changes noted (Erickson et al. 2017).
Various theories have been put forward regarding the cause for the spontaneous pancreatic findings. Earlier studies that discuss these changes (Hajdu and Rona 1967; Reaven and Reaven 1981; Dillberger 1994; Shino et al. 1973) described β-cell hyperplasia that caused islet hypertrophy as an initiating cause that preceded fibrosis and hemosiderin deposition in SD rats. The authors suggested that the pathogenesis of the islet changes began with an increased demand for insulin, which caused compensatory β-cell hyperplasia and subsequent islet enlargement. Over time, the islets would be dissected by fibrous tissue into discrete nodules of proliferating β-cells. Similar changes were also noted in rat strains that were predisposed to obesity or impaired glucose homeostasis, including Zucker, eSS, LA/N, OLETF, WBN/KOB, WY/Kob, SDT, and Goto–Kakizaki rats (Gomez Dumm, Semino, and Gagliardino 1990; Ahuja et al. 1987; Mori et al. 1990; Shino et al. 1973; Lacraz et al. 2009; Jones, Nugent, and Jenkins 2010; Katsuda et al. 2014; Masuyama et al. 2004). However, later studies that tried to characterize this change in control Crl:CD(SD) rats did not report β-cell hyperplasia and subsequent islet enlargement nor any evidence of functional impairment of glucose homeostasis associated with these pancreatic changes (Imaoka et al. 2009; Imaoka, Satoh, and Furuhama 2007). Similar to the findings of Imaoka et al., β-cell hyperplasia and subsequent islet enlargement were not noted in Crl:CD(SD) rats in either the repeat-dose toxicity or multistrain studies when treated with LY3337641, despite analysis of time points as early as 4 weeks of treatment. Further, the full range of microscopic findings that were present at the end of 13 weeks in Crl:CD(SD) rats had also manifested at the 6-weeks interim time point, although at lower incidence and severity. This polyphasic nature of pancreatic findings along with the relatively small number of islets affected at both time points was suggestive of the absence of an initial inciting event that uniformly affected the majority of the islets. Pancreatic findings similar to those described in these studies were also reported as a drug-related effect in 7- to 14-day studies that used an undisclosed drug target in Crl:CD(SD) rats (Brenneman et al. 2014). A possible mechanism for these pancreatic effects included test article–mediated glucose/insulin dysregulation or hypertension, direct cytotoxicity, or a combination of one or more of these mechanisms to cause microvascular injury at the exocrine–endocrine interface. This, in turn, may have resulted in the peri-islet serum exudation, fibrin deposition, hemorrhage, inflammation, and secondary degeneration/necrosis of surrounding exocrine tissue along with lobular atrophy and islet fibrosis. In contrast to our study, a sex predisposition was not noted for these effects. Also, the effects were more frequently observed in the tail region of pancreas. These findings were present less frequently in two other rat strains (Piebald Virol Glaxo and Brown Norway) and were absent in the mouse, dog, and monkey. All these pancreas observations are consistent with Crl:CD(SD) rats, regardless of the exact mechanism, being predisposed to developing a group of microscopic findings at this site when treated with BTKi or other xenobiotics that are morphologically similar to the spontaneous pancreatic finding in this strain.
Rapid weight gain and higher body weight in Crl:CD(SD) rats compared to other strains or in other obesity/glucose impairment models is a common observation that may be related to these pancreatic findings, whether spontaneous or test article related. It was noted that these pancreatic findings were absent in the leaner counterparts of obese models, and dietary restriction that caused weight loss in obese rats partially (at least) reversed these changes (Dillberger 1994; Reaven and Reaven 1981). Erickson et al. have also discussed the possibility that there is a direct correlation between rate of weight gain in rats and the severity of rat-specific pancreatic changes in rats treated with GDC-0853, a BTK inhibitor. They observed that male Crl:CD(SD) rats had a significantly faster growth rate and were 30–70% larger when compared to Crl:WI(Han) by 12 weeks of age, attributed to higher daily food consumption. In our multistrain rat study, Crl:CD(SD) had the greatest rate of weight gain of the three strains assessed (Figure 1) and the highest incidence and severity of both spontaneous and treatment-related pancreatic findings. Hsd: SD rats were chosen in this study to see whether a Sprague-Dawley background had an effect on the development and progression of these findings, as spontaneous pancreatic changes and similar BTKi and other test article–related pancreatic findings have mostly been reported in Crl:CD(SD). We found that the Hsd: SD rat strain has very minimal findings in pancreas, and the pancreatic effects were less prominent than in the Crl:CD(SD) or Crl:WI(Han) strains. Analysis of the growth charts for the Crl:CD(SD) strain in our repeat-dose toxicology studies and from work done by others show that the growth rate of females correlates with a clear paucity of these pancreas findings. Female Crl:CD(SD) rats have growth curves similar to those for Hsd: SD and Crl:WI(Han) rats (Figures 1 and 2). Thus, the fewer pancreatic findings may be related to the lower growth rate (body weight gain). However, there was a clear increase in the treatment-related pancreatic effects in the Crl:WI(Han) in which body weight gains were lower than the Crl:CD(SD) but comparable to Hsd: SD strain. There are clearly other factors, besides the rate of weight gain, that may determine the susceptibility of rat strains to pancreatic background and treatment-related pancreatic effects. The inciting causes of the background pancreatic findings in Crl:CD(SD) rats and other rat strains with a genetic predisposition to obesity/diabetes have been attributed to increased metabolic demands that come from increased growth rates combined with the unique anatomic peculiarities of the microvasculature at the exocrine–endocrine interface in rats where, unlike other species, arterial blood supply to the capillary networks of the acinar lobules and the islets are separate resulting in an insulo-acinar portal system around the islet. This anatomic feature may pre-dispose this species to hemorrhage and subsequent inflammation and fibrosis that is initiated in the peri-islet regions (Greaves 2012; Brenneman et al. 2014). More work is needed to elucidate the exact mechanism of these changes that accounts for the nonuniformity of these changes across the pancreatic sections (not all islets are affected), the polyphasic nature of the changes, and the lack of complete correlation between rate of weight gain and incidence/severity of pancreatic effects in rats.
In addition to the pancreas effects observed in rodents administered BTKi, it is important to consider effects in other laboratory species in assessing the overall significance of these findings. For LY3337641, a full set of repeat-dose toxicity studies has been completed in cynomolgus macaques (data not shown), and these findings were absent in monkeys dosed daily for up to 39 weeks at dose levels near the MTD for that species. Erickson et al. reported that pancreatic findings similar to that observed in the rat were not observed in mice or dogs after daily dosing with their BTKi up to 9 months at much higher exposures. Our study results are consistent with the Erickson et al.’s observation that exacerbation of these islet centric pancreatic changes are most likely a class effect of BTKi that are exclusive to rats. The incidence and severity of these findings significantly vary across species and between rat strains, with Crl:CD(SD) rats being the most susceptible. When assessing the predictivity of animal findings for human toxicity, it has been established that there is a lower concordance between human outcomes and effects observed only in rodents as compared to effects observed in either the nonrodent species only or those observed in both the rodent and nonrodent species (Olson et al. 2000; Tamaki et al. 2013; Monticello et al. 2017).
BTKi inhibitors, and possibly other kinase inhibitors, induce a characteristic pancreatic finding in rats. This is observed primarily in male rats. Susceptibility to these effects varies widely across strains of rats from the highly susceptible CRL:CD(SD) strain to the Hsd: SD strain, which was virtually unaffected in a study with LY3337641. Susceptibility across rat strains appears to be roughly correlated with the background rate of a highly similar age-related pancreatic finding that has been well characterized. Although the mechanism for this finding has not been definitively determined, metabolic factors and growth rate may be contributing factors. These pancreatic effects appear to have little or no impact on the function of the pancreas, as measured by glucose metabolism and markers of pancreatic injury such as amylase and lipase. Based on the results from these comparative studies, these pancreatic effects should be considered not adverse in rats. There is no evidence that these effects translate to or are relevant to human risk assessment. Finally, researchers should consider the results described in this article when determining which strain of rat to use as there may be situations (e.g., expectation of a treatment-related pancreatic effects) where it would be advisable to use a strain that has a low incidence of this background pancreatic finding. As this finding may not be translatable to humans, the choice of a nonsusceptible strain would not compromise human safety assessment.
Footnotes
Acknowledgments
The authors would like to acknowledge the contributions of the study director and pathologist for the repeat-dose studies, J. Leuschner and Robertus J. M. M. Thoolen, respectively, and the study director for the multistrain study, Jonathan Van Dyke. In addition, the authors would like to acknowledge the members of the pathology working group that provided unified pathological assessment for the standard repeat-dose studies: Paul W. Snyder, Robertus J. M. M. Thoolen, Woo-Chan Son, Kathleen Ann Funk, Michael R. Elwell, Thomas J. Rosol, and Günter Klöppel. Finally, the authors would like to acknowledge Steve Van Adestine for digital image preparation.
Author Contributions
Authors contributed to conception or design (MB, PC, JV); data acquisition, analysis, or interpretation (MB, PC, SS, ME, NR, MP, JV); drafting the manuscript (MB, PC, ME, NR, JV); and critically revising the manuscript (MB, PC, SS, ME, MP, JV). All authors gave final approval, and agreed to be accountable for all aspects of work in ensuring that questions relating to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. ME and SS are employees of Covance Inc., which has a contractual relationship to Eli Lilly and Company.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
