Abstract
This study was conducted to characterize lung microscopic lesions in control beagle dogs from inhalation and oral gavage toxicity studies, to determine differences associated with the route of administration, and to discuss distinguishing features from compound-induced lung lesions. Samples from 138 control dogs from oral gavage studies and 124 control dogs from inhalation (vehicle control) studies were evaluated microscopically. There was no significant sex-related difference in the incidence of all lesions. Perivascular mononuclear cell infiltration, centriacinar mixed cell infiltration, bronchopneumonia, subpleural septal fibrosis, and alveolar macrophage accumulation were the most common lesions. Aspiration pneumonia was more common in dogs from gavage studies, suggesting reflux after gavage dosing or accidental administration of test formulation as possible causes. Centriacinar mixed cell infiltration was more common in dogs from inhalation studies, suggesting mild irritation by the vehicles used. Vascular lesions, which included pulmonary arteriopathy and smooth muscle mineralization, were observed in a few animals. Some of the spontaneous lesions are similar to lesions induced by test compounds. Compared to spontaneous lesions, compound-induced lesions tend to be multifocal or diffuse, follow a pattern of distribution (e.g., centriacinar, perivascular, and interstitial), show a dose response in the incidence and severity, and may show cell-specific toxicity.
Although beagle dogs are commonly used as a nonrodent model for evaluating chemical toxicity (Gad 2009), there are limited data on spontaneous lung findings in these animals. Few published articles have reported the incidences of common spontaneous lesions in all organs in beagle dogs (Hottendorf and Hirth 1974; Oghiso, Fukuda, and Iida 1982; Morishima et al. 1990; Hahn and Dagle 2001; Sato et al. 2012; Barnes et al. 2016). However, in these reports, no detailed histopathological examination and description of the lung lesions was performed. In addition, no discussion was made on how these lesions can be differentiated from compound-induced lesions.
The development and severity of lung lesions in control animals can be associated with the route of administration of the control item. In gavage studies, lung lesions can be induced by accidental administration of test or control item into the lung, mechanical tissue damage, or accidental aspiration of test or control item as a result of reflux after gavage dosing. In inhalation studies, the test or control item may cause irritation resulting in lung lesions. Some of the spontaneous lesions may resemble or mask compound-induced lesions, and this could complicate the interpretation of pathology results in toxicology studies. Therefore, a thorough understanding of the morphologic differentiating features and distribution of these lung lesions is necessary for a correct and accurate diagnosis.
The aims of this study are (1) to characterize lung microscopic lesions in untreated control beagle dogs from oral gavage and inhalation toxicity studies, (2) to determine if there were any differences associated with the route of administration, and (3) to compare the spontaneous lesions to compound-induced lesions, and where possible, concisely document the differentiating features. Given the lack of significant information on lung lesions in young beagle dogs, these findings will serve as a useful addition to the literature and aid in the interpretation of lung lesions in gavage and inhalation studies.
Materials and Methods
Animals
This report is based on lung samples from a total of 262 beagle dogs (138 dogs from 20 oral gavage studies and 124 dogs from 18 inhalation studies) obtained from control groups of preclinical toxicological studies evaluated between 2009 and 2015 at Charles River Laboratories Edinburgh Ltd. Dogs were aged 10 to 20 months and were from studies with durations of 1 to 6 months. Control groups varied in size from 3 to 5 animals per group per sex. These dogs were dosed with commonly used vehicles by the oral gavage or inhalation route. All samples were from vehicle controls. For inhalation studies, no air-only controls were included in the study. All dogs were obtained from Harlan, United Kingdom. Dogs were housed in groups of 3 by sex in custom designed dog pens with an area of at least 2.25 m2 for each dog at a temperature of 15°C to 24°C and a minimum of 10 air changes per hour and a 12-hr light/dark cycle. Each dog was given 300 g/day of standard Certified Canine Diet No. 5007 (PMI Nutrition International, Inc.) and purified water ad libitum. The dogs were maintained in accordance with the U.K. Animals (Scientific Procedures) Act 1986, which conforms to the European Convention for the Protection of Vertebrate Animals Used for Experimental and Other Scientific Purposes (Strasbourg, Council of Europe).
Histologic Evaluation
Prior to necropsy, each dog was euthanized by intravenous injection of sodium pentobarbital followed by exsanguination. Lung tissues were inflated via the trachea with neutral buffered 10% formalin to approximate full volume by visual observation and fixed by immersion in 10% neutral buffered formalin. Following fixation, sections of the left caudal lobe and right middle lobe were embedded in paraffin, sectioned at 3 to 5 μm, stained with hematoxylin and eosin. Single longitudinal sections of the left caudal lobe and right middle lobe were evaluated by 1 pathologist (S.M.) using light microscopy. Occasionally, adjacent multiple serial sections were evaluated to further characterize the lesion.
Results
Spontaneous and Dosing Procedure–related Lung Lesions
The variety and incidence of the findings encountered in control beagle dogs from oral gavage and inhalation studies are presented in Table 1. In general, there was no significant difference in the incidence of all lesions between males and females, and most lesions were not associated with respiratory signs nor resulted in the death of the animals, with the exception of a few cases of extraintestinal pathogenic Escherichia coli (ExPEC)–induced necrotizing hemorrhagic pneumonia and some cases of aspiration pneumonia. A comparison of the range and incidences of lung lesions observed in this study with published data is presented in Table 2.
Microscopic Lung Lesions Observed in Control Beagle Dogs from Inhalation and Gavage Toxicity Studies.
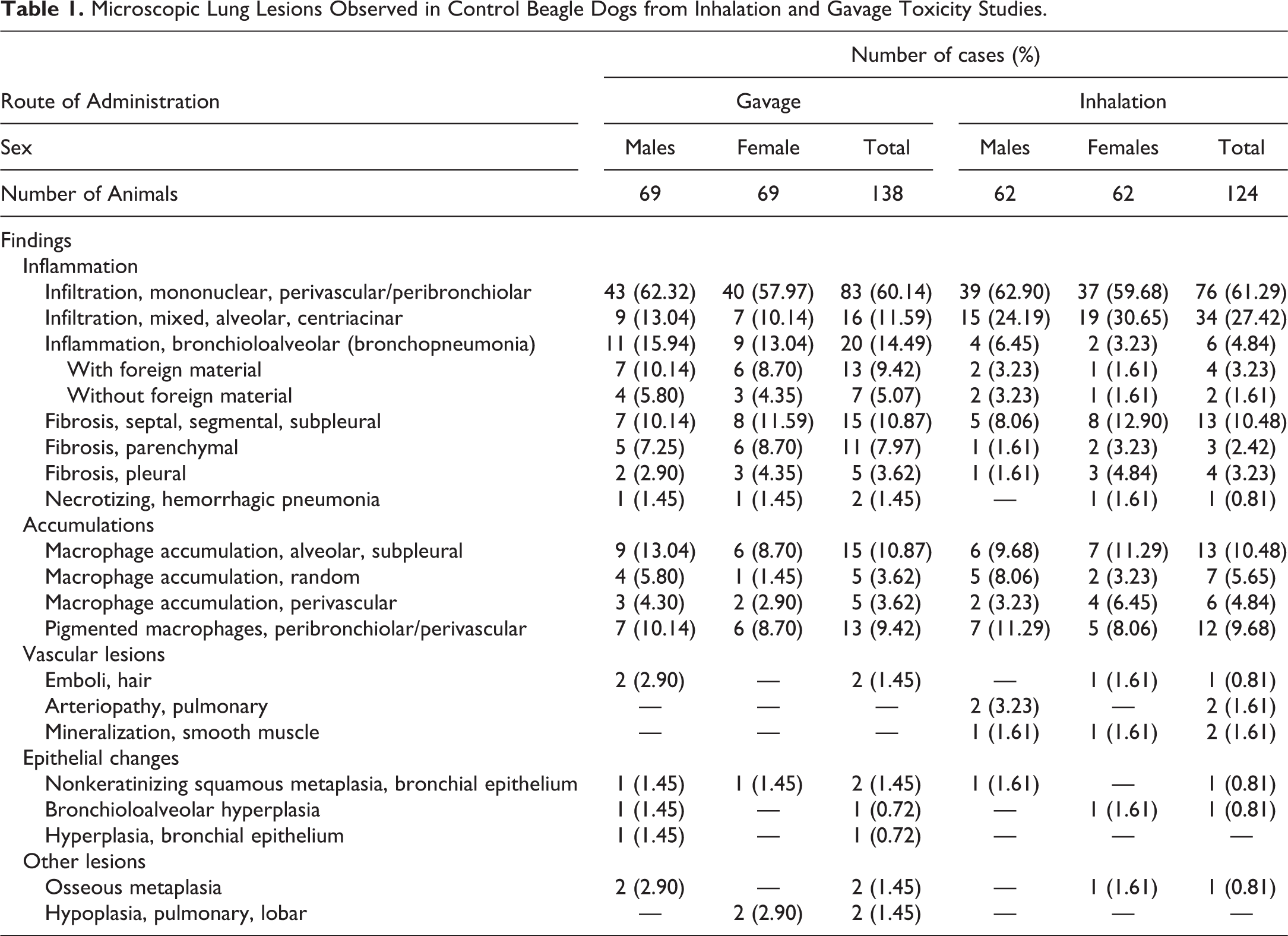
Microscopic Lung Lesions Observed in Control Beagle Dogs: Comparison with Published Reports.
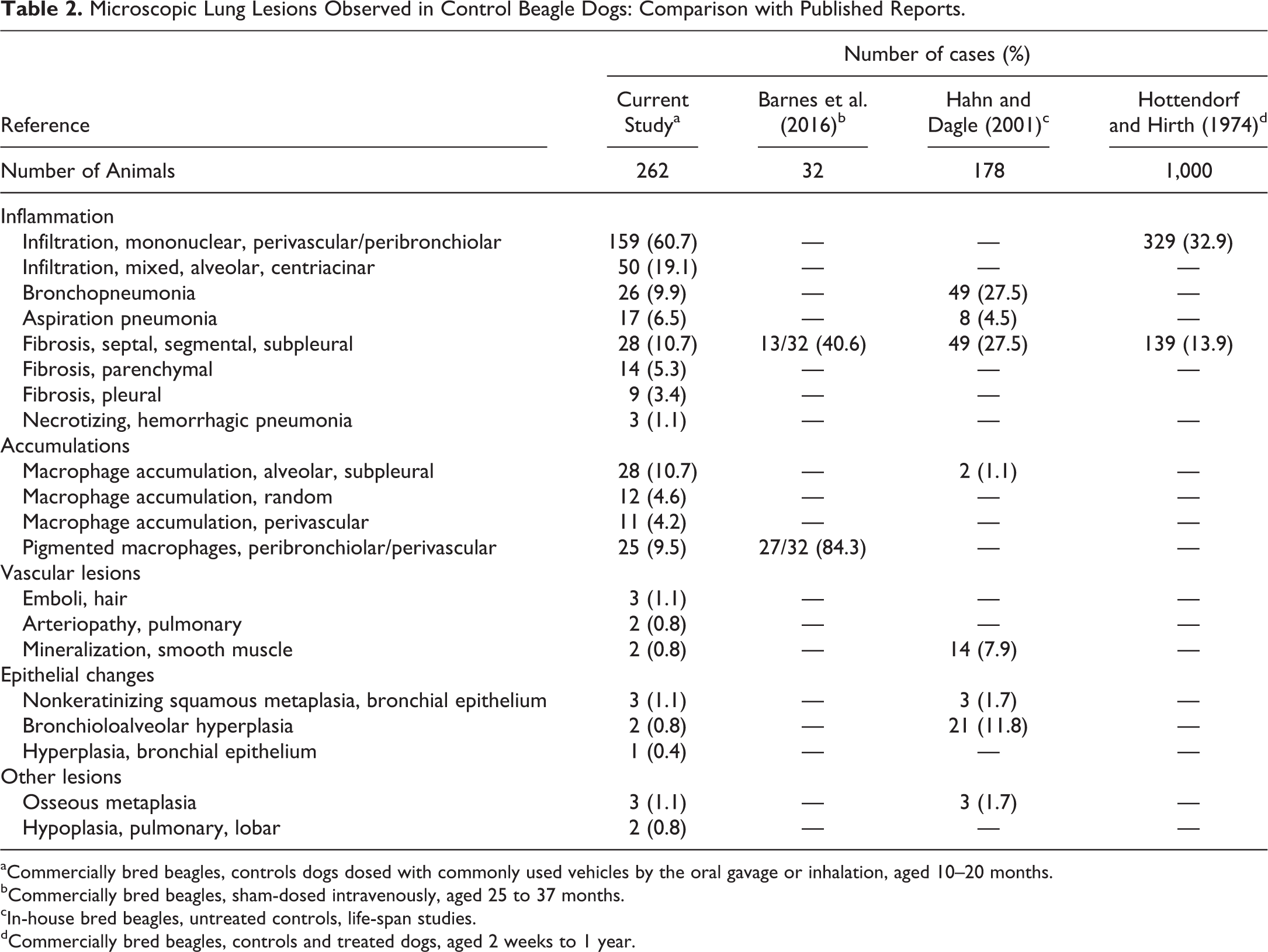
aCommercially bred beagles, controls dogs dosed with commonly used vehicles by the oral gavage or inhalation, aged 10–20 months.
bCommercially bred beagles, sham-dosed intravenously, aged 25 to 37 months.
cIn-house bred beagles, untreated controls, life-span studies.
dCommercially bred beagles, controls and treated dogs, aged 2 weeks to 1 year.
Inflammation
Regardless of the route of administration, inflammatory conditions were more common than other conditions. Perivascular mononuclear cell infiltration was the most common finding, occurring at similar incidences in gavage (60.14%) and inhalation (61.29%) studies. The lesion was characterized by perivascular and/or peribronchiolar infiltration by many lymphocytes and few plasma cells and macrophages (Figure 1). This finding was observed on its own or in association with other lung lesions such as acute or chronic bronchioloalveolar inflammation, fibrosis, and alveolar macrophage accumulation. The severity of perivascular/peribronchiolar mononuclear cell infiltration varied from minimal to moderate, and the severity was higher when found in association with other lung conditions.
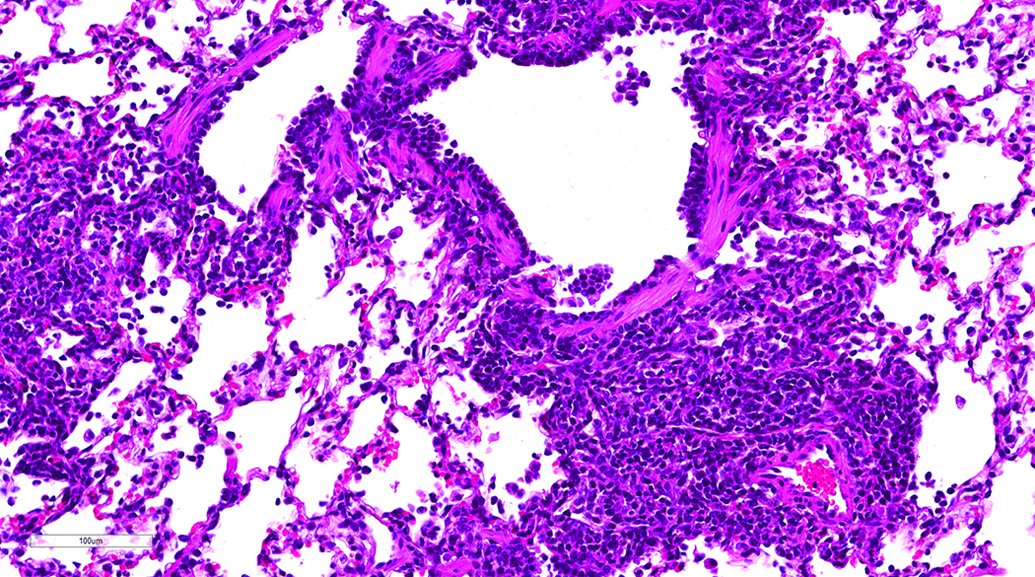
Lung, male beagle from gavage study (hematoxylin and eosin stain). Perivascular/peribronchiolar infiltration by lymphocytes, plasma cells, and macrophages. Original magnification 20×.
Centriacinar mixed cell infiltration was a common finding irrespective of administration route. However, dogs from the inhalation studies exhibited a higher incidence (27.42%) compared to dogs from the gavage studies (11.59%). The lesion was minimal to mild and was characterized by centriacinar (junction of respiratory bronchioles and alveolar ducts) accumulation of neutrophils and macrophages without associated lesions such as necrosis, type II pneumocyte proliferation, or epithelial hyperplasia of the respiratory bronchioles (Figure 2).
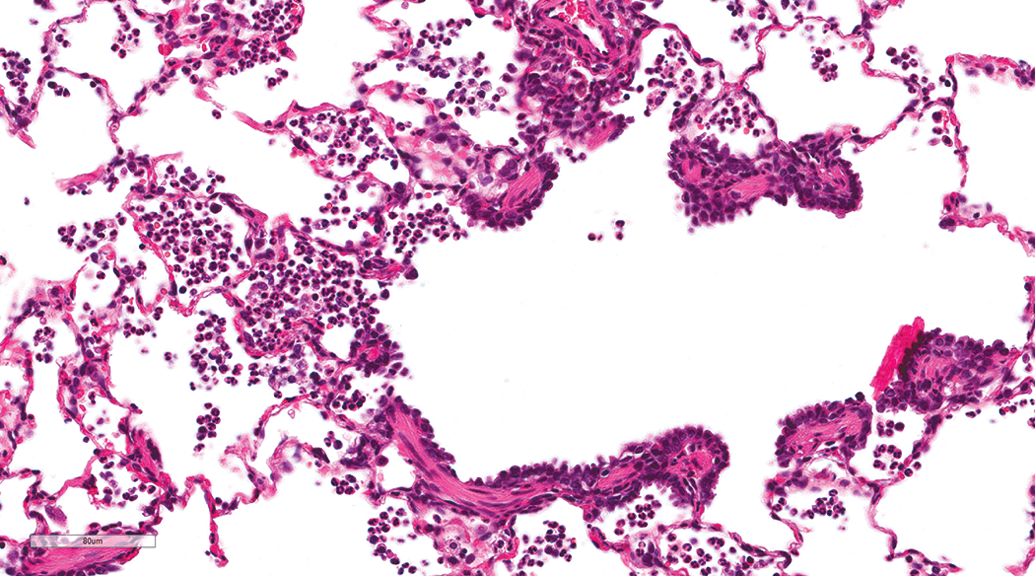
Lung, female beagle from inhalation study (hematoxylin and eosin stain). Centriacinar (junction of respiratory bronchioles and alveolar ducts) infiltration by neutrophils and macrophages. Original magnification 26.4×.
Mild to severe bronchioloalveolar mixed cell inflammation (bronchopneumonia) was observed in animals from both gavage and inhalation studies. However, dogs from the gavage studies exhibited a higher incidence (14.49%) and severity of this lesion compared to dogs from the inhalation studies (4.84%). Acute lesions were characterized by accumulation of neutrophils and macrophages in the airways (bronchi, bronchiole, and alveoli) with necrosis and hemorrhage (Figure 3). Chronic lesions were characterized as granulomatous foreign body reaction and fibrosis (Figure 4). In some cases, foreign materials (Figure 3) and/or bacterial colonies were observed in the airways. The severity of bronchopneumonia varied from mild to severe, and severe lesions were often associated with unscheduled euthanasia of the animal.
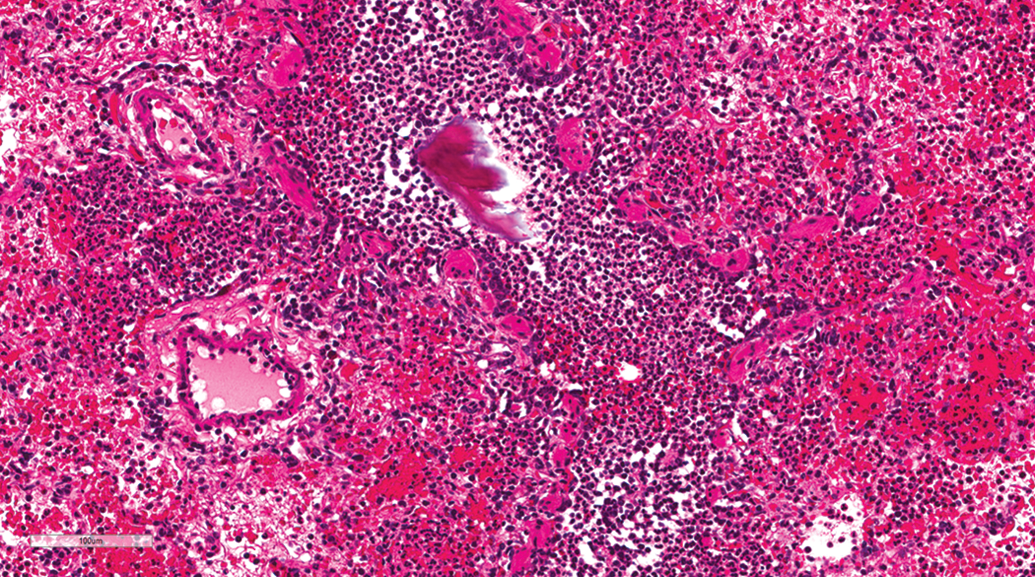
Lung, female beagle from gavage study (hematoxylin and eosin stain). Aspiration pneumonia characterized by hemorrhage, accumulation of neutrophils in the bronchiole and alveoli, and presence of foreign material in the bronchiole. Original magnification 20×.
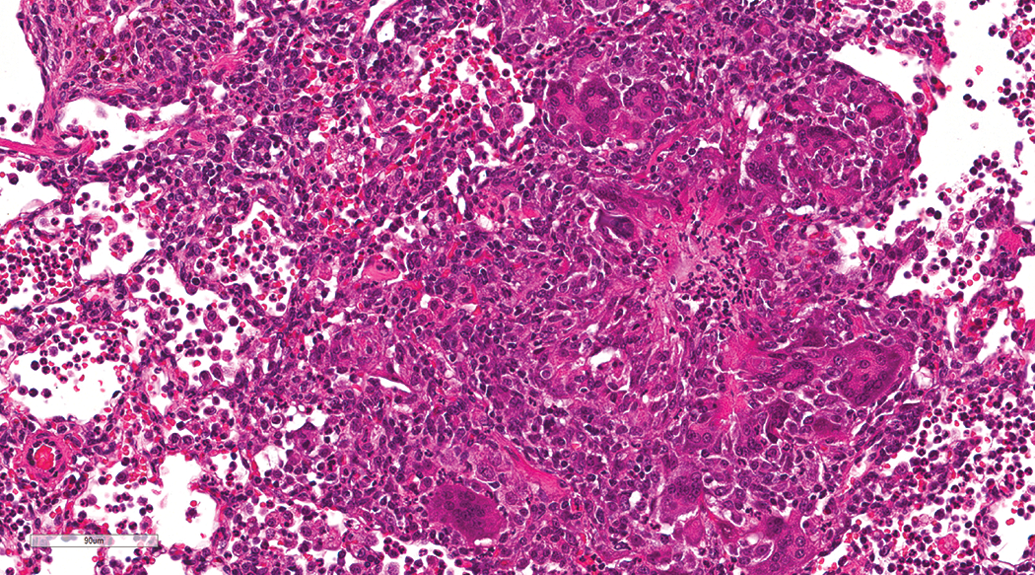
Lung, male beagle from gavage study (hematoxylin and eosin stain). Aspiration pneumonia characterized by a granulomatous foreign body reaction. Original magnification 23.2×.
Segmental subpleural septal fibrosis was observed in animals from both gavage and inhalation studies with similar incidences in gavage studies (10.87%) and in inhalation studies (10.48%). Grossly, this lesion was often observed as small, tan, or gray subpleural nodules in all lung lobes. Microscopically, the lesion was multifocal, segmental, and subpleural in distribution often wedge shaped extending from the pleura into to the parenchyma (Figure 5), and in some cases, fibrosis involved the entire tip of a lung lobe (Figure 6). The main characteristic of the lesion was septal fibrosis. Depending on the case, septal fibrosis was accompanied by bronchioloalveolar hyperplasia, nonkeratinizing squamous metaplasia (Figure 7), alveolar macrophage aggregation, and pleural fibrosis or hyperplasia of the mesothelium. No signs of respiratory distress were observed in dogs with this lesion. Pulmonary parenchymal fibrosis was observed in a few animals from both gavage (7.97%) and inhalation studies (2.42%). Pulmonary fibrosis was characterized by multifocal fibrosis of the lung parenchyma (alveoli and bronchioles) and occasionally intraluminal fibrosis was observed in the bronchioles (Figure 8). Pleural fibrosis was observed in a few animals, usually in association with subpleural segmental fibrosis or parenchyma fibrosis.
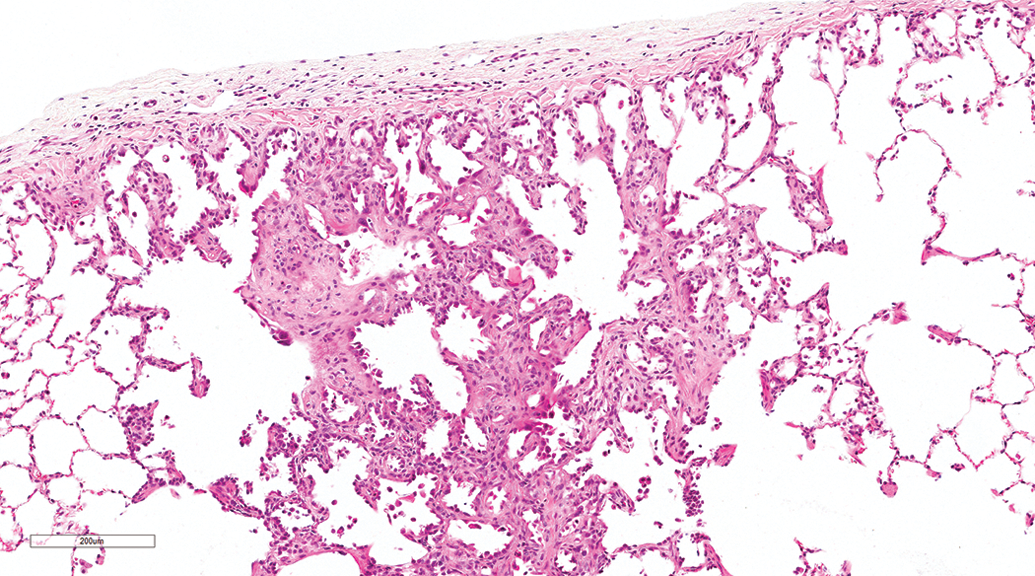
Lung, female beagle from inhalation study (hematoxylin and eosin stain). Segmental subpleural septal fibrosis with minimal type II pneumocyte proliferation. Original magnification 8.9×.
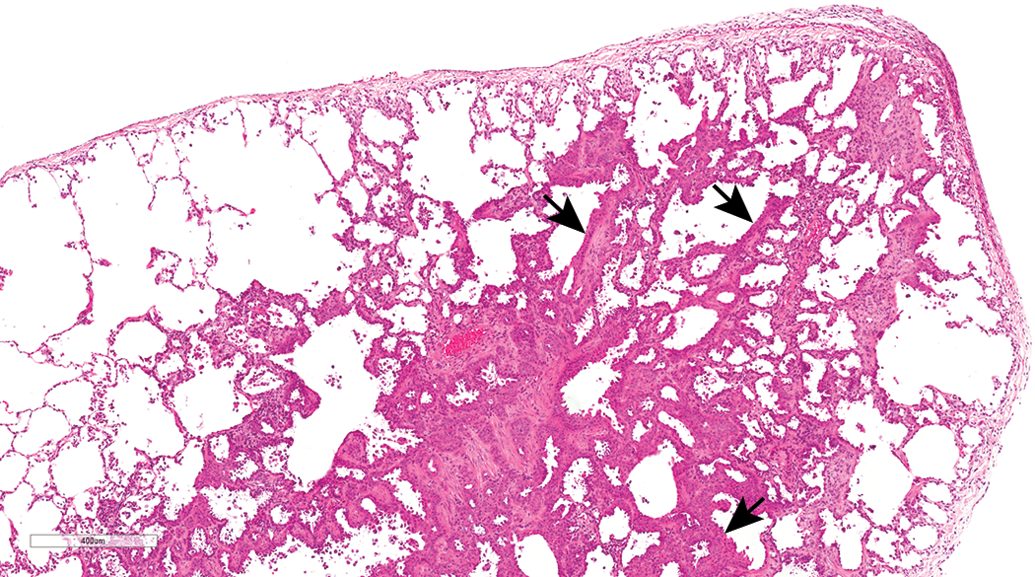
Lung, male beagle from gavage study (hematoxylin and eosin stain). Segmental subpleural septal fibrosis involving the tip of the lobe with moderate alveolar pneumocyte proliferation (arrows). Original magnification 20×.
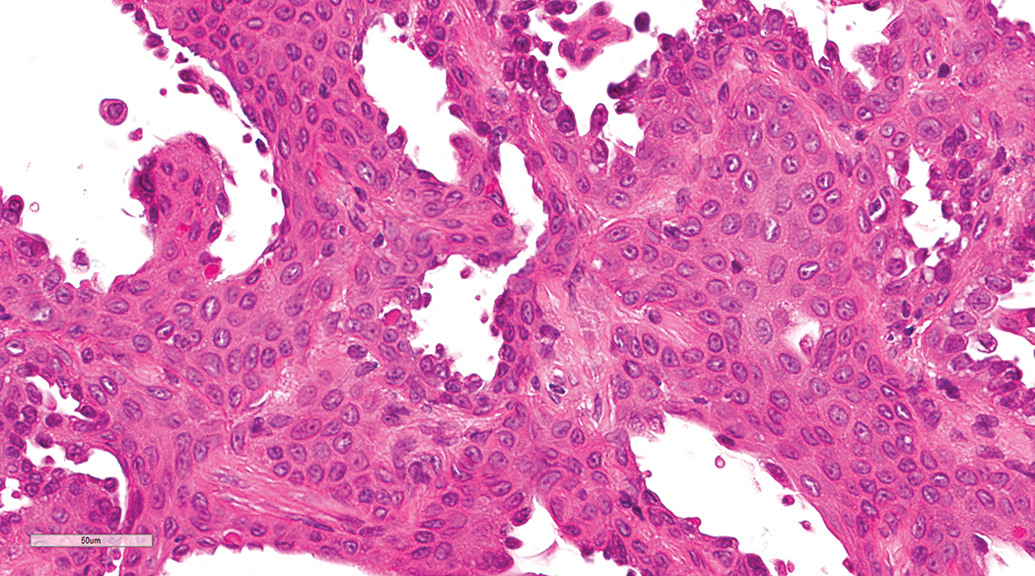
Lung, male beagle from gavage study (hematoxylin and eosin stain). Segmental interstitial fibrosis. Higher power of Figure 6 demonstrating nonkeratinizing squamous metaplasia of the alveolar and bronchiolar epithelium. Original magnification 40×.
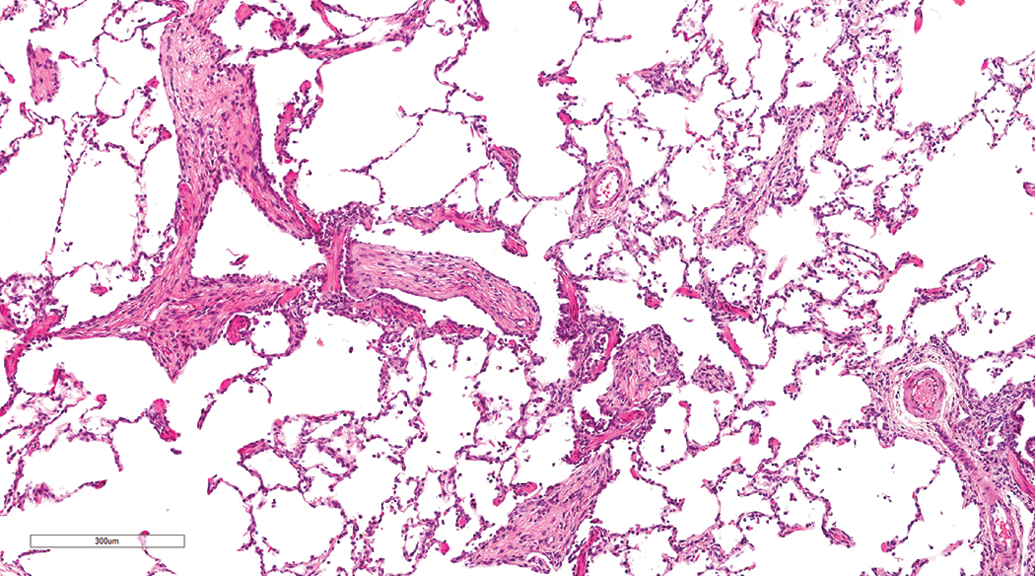
Lung, female beagle from gavage study (hematoxylin and eosin stain). Pulmonary parenchymal fibrosis characterized by multifocal fibrosis of the lung parenchyma (alveoli and bronchioles) and intraluminal fibrosis. Original magnification 20×.
Three cases of necrotizing hemorrhagic pneumonia were observed, 2 from gavage studies and 1 from an inhalation study. In all of the 3 cases, the lesion was characterized by coagulative necrosis of bronchiolar walls, alveolar septae, and pleural surfaces, with associated fibrinoid necrosis of vessel walls, hemorrhage, and congestion (Figure 9). Respiratory bronchiolar lumina and alveoli were frequently filled by proteinaceous fluid, fibrin, and degenerate neutrophils. Numerous gram-negative, rod-shaped bacteria were present in the airways, alveolar spaces, lining necrotic alveolar septae, and within necrotic pleura (Figure 10). In all 3 cases, pure lung cultures of hemolytic E. coli were isolated from the lung tissue.
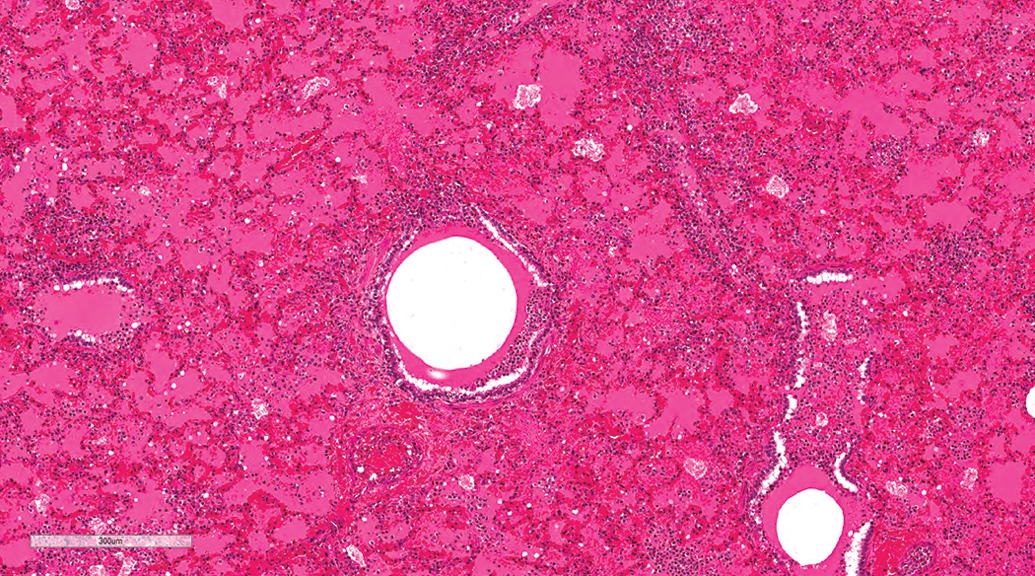
Lung, male beagle from inhalation study (hematoxylin and eosin stain). Extraintestinal pathogenic Escherichia coli–induced hemorrhagic pneumonia. Proteinaceous fluid with scattered macrophages and neutrophils within alveolar spaces. Original magnification 8.8×.
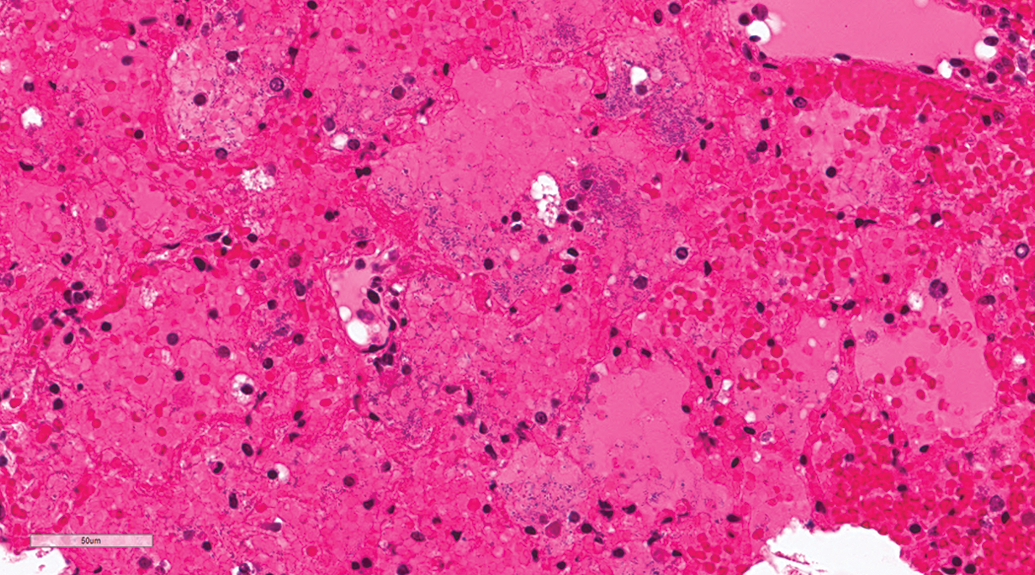
Lung, male beagle from inhalation study (hematoxylin & eosin stain). Extraintestinal pathogenic Escherichia coli–induced hemorrhagic pneumonia. Large numbers of rod-shaped bacteria in the alveoli. Original magnification 40×.
Accumulations
Subpleural alveolar macrophage aggregation occurred at similar incidences in gavage (10.87%) and inhalation studies (10.48%). The lesion was characterized by accumulation of foamy macrophages in the subpleural alveoli, and occasionally this was associated with infiltration by lymphocytes and plasma cells, cholesterol clefts formation (Figure 11), and/or type II pneumocyte proliferation (Figure 12). Within the foci, the macrophages were contiguous. Random alveolar macrophage aggregation was an occasional finding, occurring at similar incidences in gavage and inhalation studies. The lesion was characterized by focal or multifocal random accumulations of foamy macrophages without inflammation or other lung lesions. The accumulations were not subpleural or centriacinar. Perivascular macrophages aggregation was observed in a few dogs from both gavage and inhalation studies. Peribronchiolar (Figure 13) and/or perivascular pigmented macrophage aggregation was observed at similar incidences in gavage (9.42%) and inhalation studies (9.68%). The pigment was brown, yellow, or golden and occasionally was associated with other lesions such as hemorrhage and inflammation.
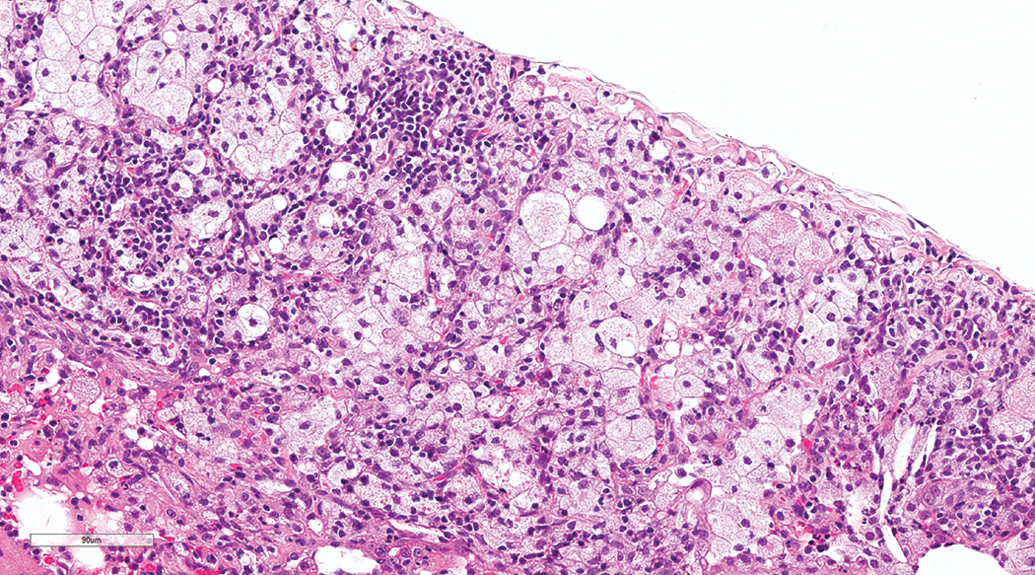
Lung, male beagle from gavage study (hematoxylin and eosin stain). Alveolar macrophage accumulation with inflammatory cell infiltration and cholesterol clefts. Original magnification 20×.
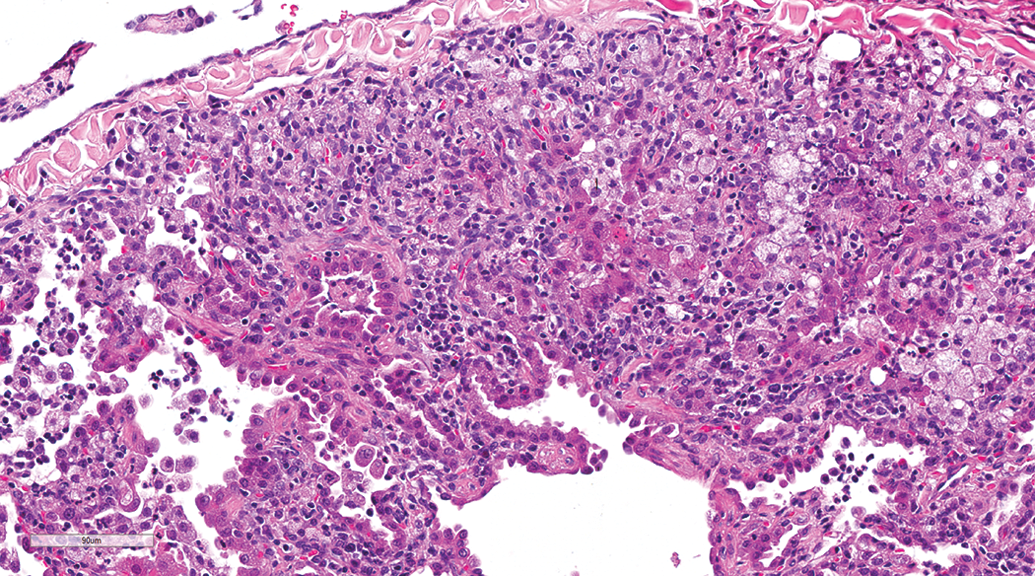
Lung, male beagle from inhalation study (hematoxylin and eosin stain). Alveolar macrophage accumulation with type II pneumocyte proliferation. Original magnification 22.4×.
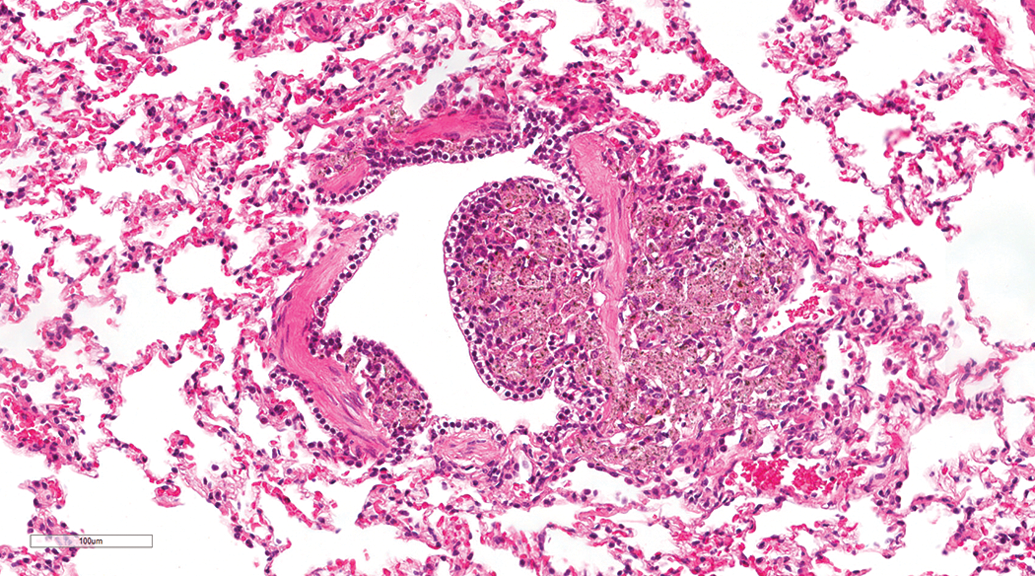
Lung, male beagle from inhalation (hematoxylin and eosin stain). Peribronchiolar pigmented macrophage accumulation. Original magnification 20×.
Vascular Lesions
Lesions involving pulmonary vessels were rare and occurred at similar incidences in gavage and inhalation studies. The following vascular lesions were observed in a few animals: hair emboli (Figure 14), pulmonary arteriopathy, arteritis, and smooth muscle mineralization. Two cases of pulmonary arteriopathy were observed. In both cases, arteriopathy was characterized by concentric medial hypertrophy and intimal thickening (Figure 15) and formation of plexiform lesions (Figure 16). In some arteries, there was necrosis and infiltration of the arterial wall by acute inflammatory cells (Figure 15). Medial hypertrophy and intimal thickening resulted in partial or complete occlusion of the vascular lumen. Plexiform lesions were characterized by proliferation of endothelial channels lined by myofibroblasts, smooth muscle cells, and connective tissue matrix (Figure 16). Examination of adjacent multiple serial sections revealed more plexiform lesions; however, no other lesions suggestive of loss of vascular supply were present.
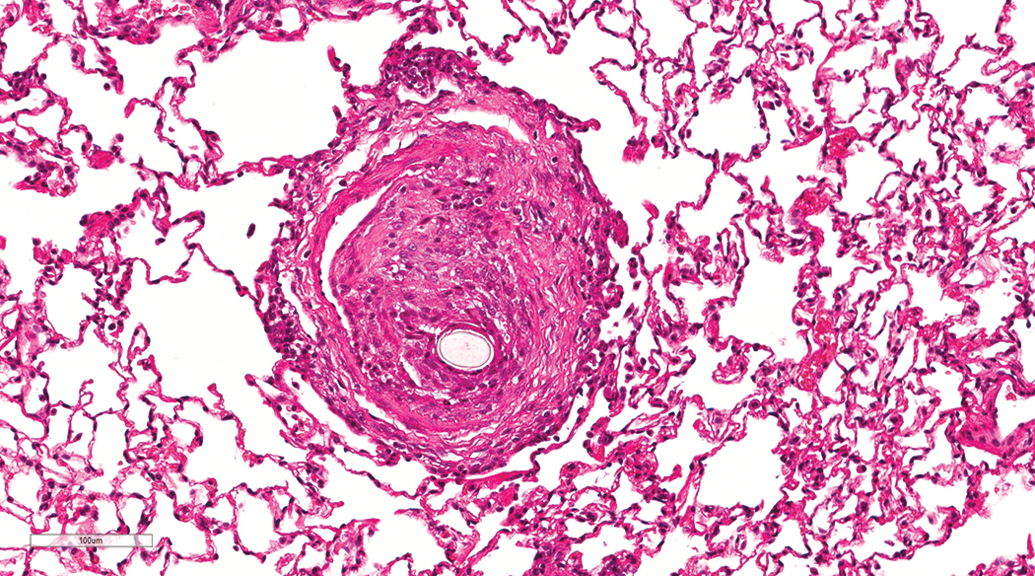
Lung, male beagle from gavage study (hematoxylin and eosin stain). Hair emboli in a pulmonary vessel. Original magnification 20×.
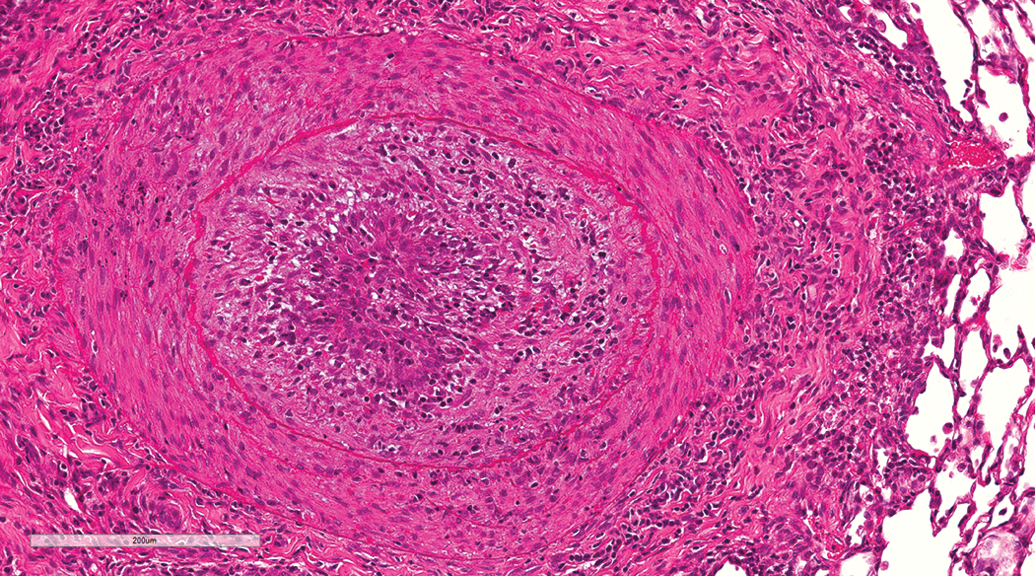
Lung, male beagle from inhalation study (hematoxylin and eosin stain). Pulmonary arteriopathy. Marked intimal and medial thickening of pulmonary artery with complete occlusion of the vascular lumen and necrosis and infiltration of the arterial wall by acute inflammatory cells. Original magnification 18.8×.
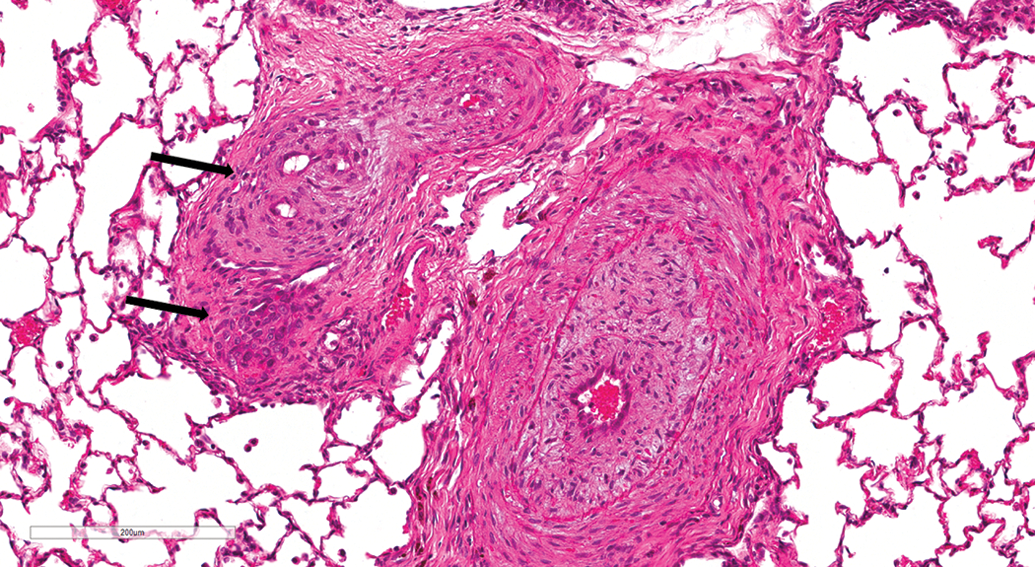
Lung, male beagle from inhalation (hematoxylin and eosin stain). Pulmonary arteriopathy. Plexiform lesions (arrows) characterized by proliferation of endothelial channels lined by myofibroblasts, smooth muscle cells, and connective tissue matrix. Original magnification 20×.
Pulmonary hemorrhage, edema, and thrombosis were occasionally found but were always associated with other lesions such as ExPEC-induced pneumonia and aspiration pneumonia.
Epithelial Changes
Epithelial changes were rare and included the following: nonkeratinizing squamous metaplasia of the bronchial epithelium, bronchioloalveolar hyperplasia, and hyperplasia of the bronchial epithelium. These lesions were mostly focal in distribution and minimal in severity. The bronchioloalveolar hyperplasia observed in the two dogs was not associated with septal fibrosis or other lung conditions (Figure 17).
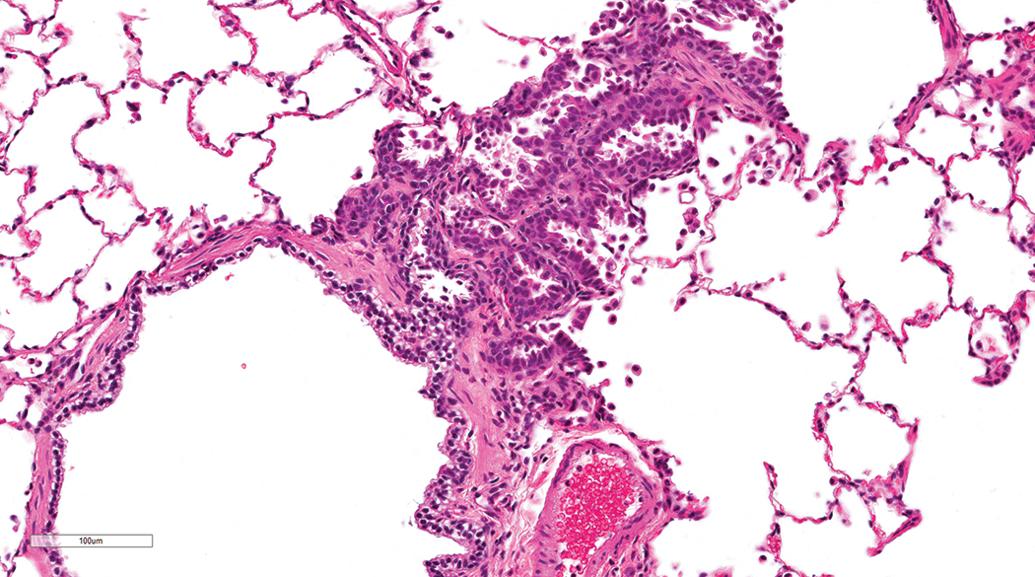
Lung, male beagle from gavage study (hematoxylin and eosin stain). Bronchioloalveolar hyperplasia without septal fibrosis. Original magnification 20×.
Other Lesions
Other lesions were rare. Osseous metaplasia and pulmonary lobar hypoplasia were observed in few animals. Pulmonary lobar hypoplasia was characterized by insufficient bronchiole and alveolar development (Figure 18). No neoplastic lesions were observed.
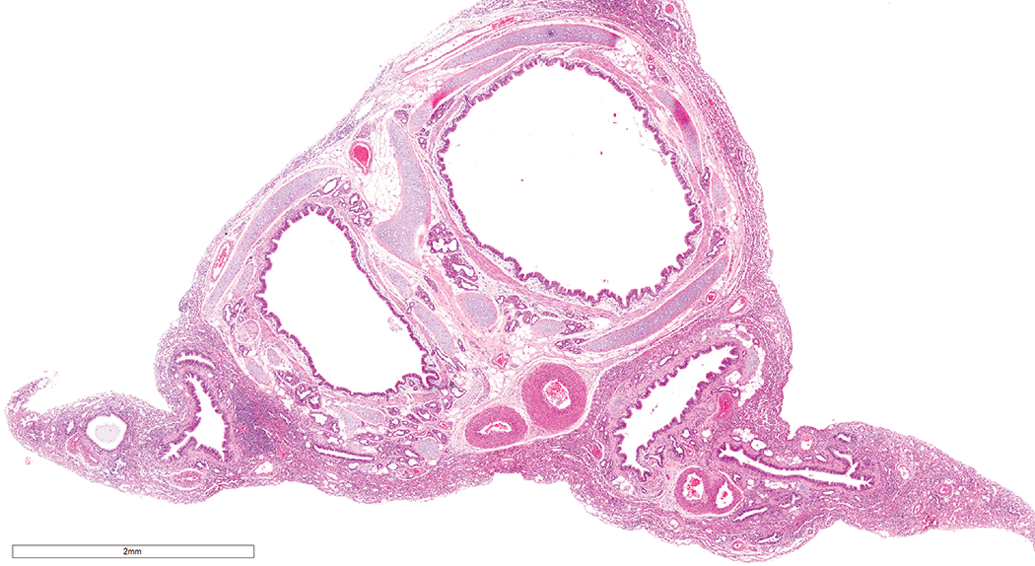
Lung, male beagle from gavage study (hematoxylin & eosin stain). Pulmonary lobar hypoplasia, characterized by insufficient bronchiole and alveolar development. Original magnification 4×.
Drug-induced Lesions
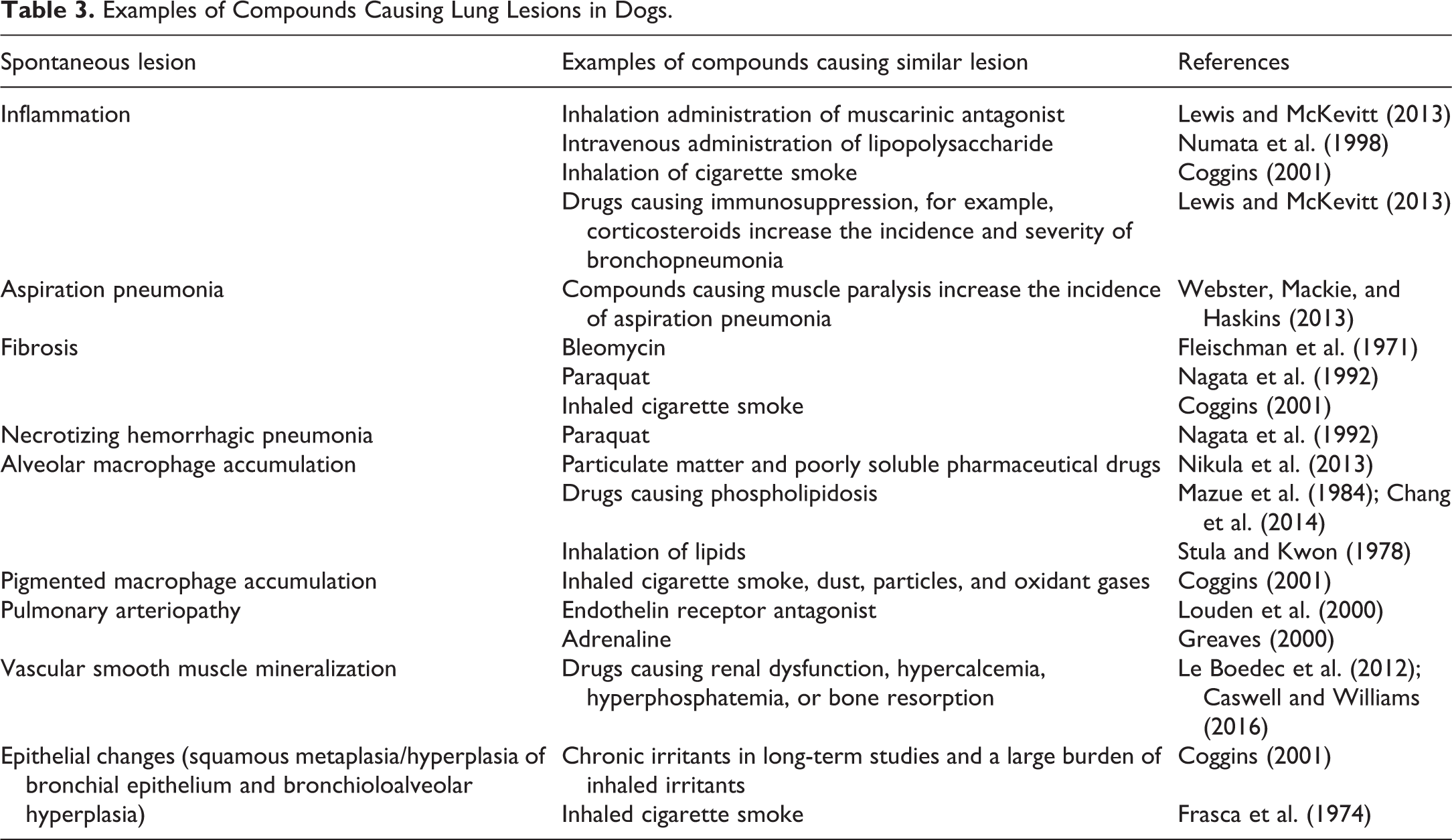
The lung can be a target of toxic injury by inhalation administration of test compounds that are directly toxic to epithelial or endothelial cells or by noninhalation administration of test compounds that are metabolized to reactive intermediates mainly by type II pneumocytes and club cells. In beagle dogs, a variety of chemicals and drugs administered by inhalation or noninhalation routes can elicit lesions in the lung which are histologically similar to the lesions described above. Table 3 lists some of the common chemicals and drugs that can induce these lesions.
Examples of Compounds Causing Lung Lesions in Dogs.
Discussion
The beagle dog is the most commonly used nonrodent species in preclinical toxicology studies (Gad 2009). Gross and histologic examination of the lung is essential in preclinical toxicology studies. Abnormal findings in the lungs can be attributed to spontaneous lesions, compound-related toxicity, technical gavage errors (i.e., accidental administration of test formulation into the lung and/or serious mechanical tissue damage), gavage-related reflux (accidental aspiration of dose formulation and stomach contents as a result of reflux after gavage dosing), and agonal changes and artifacts. In this study, a wide range of spontaneous or dosing route–associated lung lesions were observed compared to previously published literature (Table 2). Lesions that were not observed in previous studies include bacteria-induced necrotizing hemorrhagic pneumonia, pulmonary arteriopathy, and hyperplasia of bronchial epithelium. Vascular amyloidosis, hemosiderosis, hyalinosis, and mucous cell metaplasia have been observed in previous studies in aging dogs (Hahn and Dagle 2001) but not in this study. These lesions are most likely age-related changes.
Distinguishing test compound–related findings from spontaneous findings is critical for accurate risk assessment. There are no pathognomonic histologic features that differentiate spontaneous from compound-induced lung lesions. Table 4 shows some of the histopathological features that can be used to differentiate spontaneous from compound-induced lung lesions. In general, spontaneous lung lesions tend to be focal, affect one lobe, are less extensive, and show no dose response in incidence or severity. Compound-induced lesions tend to be multifocal or diffuse, follow a pattern of distribution (e.g., centriacinar, perivascular, and interstitial), show a dose response in the incidence and severity, and may show cell-specific toxicity (e.g., necrosis of club cells).
Histological Differentiation of Spontaneous and Compound-induced Lung Lesions in Beagle Dogs.

Perivascular/peribronchiolar mononuclear infiltration was the most common inflammatory condition. In some cases, the infiltration was associated with other lung lesions, suggesting that it is not a primary change. Systemic diseases, such as congestive heart failure, hyperadrenocorticism, and hepatitis (Hahn and Dagle 2001), and mild viral infections may induce perivascular mononuclear cell infiltration (Caswell and Williams 2016). The cause of spontaneous perivascular/peribronchiolar mononuclear infiltration is unknown and may be difficult to distinguish from a drug effect if there was increased incidence or severity in treated animals when compared with controls. However, minimal to mild perivascular/peribronchiolar mononuclear infiltration in the absence of other lung lesions is likely to be of no toxicological significance.
Centriacinar mixed cell infiltration was more common in dogs from inhalation studies than gavage studies. The centriacinar distribution suggests aerogenous route of entry of the causative agent. This type of reaction is considered to be nonspecific after inhalation of mild irritants (environmental toxicants or infectious agents). The higher incidence of this lesion in dogs from inhalation studies suggests that some of the vehicles used in these studies caused minimal irritation. Differentiating lesions induced by a novel vehicle from test compound–induced lesions might be difficult and this might warrant inclusion of air-only control group. Administration of test compounds by noninhalation routes, for example, lipopolysaccharides (Numata et al. 1998) and paraquat (Nagata et al. 1992), can also cause mixed cell infiltration. However, the distribution is usually interstitial and not centered on the airways.
Mixed cell bronchioloalveolar inflammation (bronchopneumonia) was more common in dogs from gavage than inhalation studies. The bronchioloalveolar distribution suggests aerogenous route of entry of the causative agent. The presence of foreign material and/or bacterial colonies in some cases suggests aspiration pneumonia. Aspiration pneumonia can be a result of aspiration of stomach contents, vomitus, or dry finely particulate food or bedding. In gavage studies, aspiration pneumonia can be a result of gavage-related reflux (accidental aspiration of dose formulation owing to reflux related to gavage dosing) or technical gavage error (accidental administration of test formulation into the lung and/or serious mechanical tissue damage during the gavage procedure). Test compounds that cause vomiting, nerve paralysis, and muscle atrophy can increase the incidence of aspiration pneumonia. Inhalation of muscarinic antagonists can induce mixed cell inflammatory lesions, bronchopneumonia, and granulomatous pneumonia consistent with inhalation of food particles (Lewis and McKevitt 2013). These lesions are considered to be related to the pharmacological properties of muscarinic agonists in dogs, such as diminished salivary flow/dry mouth and concomitant increase in the risk of oropharyngeal floral aspiration (Gibson and Barret 1992). In addition, muscarinic antagonists can increase the risk of spontaneous gastroesophageal reflux and aspiration of gastric contents (Wilson and Walshaw 2004).
We have recently observed an increase in the severity of aspiration pneumonia in dogs given immunosuppressive test compounds. Although, not common in beagle dogs, bronchopneumonia can also be caused by bacteria or viruses.
Segmental subpleural septal fibrosis with varying degrees of bronchioloalveolar hyperplasia, nonkeratinizing squamous metaplasia, alveolar macrophage aggregation, pleural fibrosis, and/or hyperplasia of the mesothelium was observed in both gavage and inhalation studies at similar incidences. This type of fibrosis has been reported at a higher incidence in aging beagle dogs (Hahn and Dagle 2001; Barnes et al. 2016). In some cases, there was exaggerated alveolar pneumocyte and bronchiolar epithelium hyperplasia and squamous metaplasia, and some authors regard it as a precursor of neoplasia (Hajdu and Rona 1965). The cause of this lesion is not documented, but the presence of fibrosis, epithelial cell proliferation, and alveolar macrophages suggests a reaction to some form of interstitial lung injury. Similar lesions have been reported to be caused by lungworms (Filaroides hirthi; Hirth and Hottendorf 1973). In this study, no lung worms were observed, and no eosinophilic granulomatous inflammation suggestive of parasite infestation was observed. Pulmonary fibrosis is a common sequel of parenchymal lung injury. In dogs, pulmonary injury and inflammation caused by anticancer drugs, such as bleomycin (Fleischman et al. 1971; Thompson et al. 1972), or by paraquat poisoning (Nagata et al. 1992) usually progress to fibrosis. Histologically, the lesions produced by bleomycin administration are located in the pleural and subpleural zones (Thompson et al. 1972) and resemble those described for segmental subpleural septal fibrosis observed in this study. However, the lesions induced by bleomycin and presumably other test compounds are more extensive and affect several lobes.
Necrotizing hemorrhagic pneumonia was observed in 3 dogs, 2 from gavage studies and 1 from an inhalation study, and pure hemolytic E. coli isolates were cultured from lung tissues of these dogs. E. coli, of the bacterial family Enterobacteriaceae, is a normal inhabitant of the lower intestinal tract of all warm-blooded animals. ExPEC strains express virulence factors that help the organism to overcome host defenses and infect organs other than the gastrointestinal tract. The ExPEC strains carry genes encoding for virulence attributes such as cytotoxic necrotizing factor (Cnf-1), type 1 fimbriae, and P fimbriae adhesion (Johnson et al. 2001). In dogs, ExPEC is most frequently implicated in urinary tract infections and has also been associated with mastitis, pyometra, otitis, prostatitis, skin disease, and cholecystitis (Timoney et al. 1988). E. coli has also been described as the cause of spontaneous fatal pneumonia in dogs, including purpose bred beagle dogs (Handt et al. 2003), cats (Highland et al. 2009), and in horses (DebRoy et al. 2008). Streptococcus equi subspecies zooepidemicus has been reported to cause outbreaks of necrotizing and/or hemorrhagic pneumonia in shelter dogs (Pesavento et al. 2008). The gross and microscopic appearance of S. equi subspecies zooepidemicus-induced pneumonia is similar to that of ExPEC-induced pneumonia. Bacterial culture, Gram stain, or polymerase chain reaction can easily confirm the causative agent. No cases of S. equi subspecies zooepidemicus-induced pneumonia have been reported in beagle dogs. Published reports of necrotizing hemorrhagic pneumonia following administration of test compounds are rare. Acute paraquat toxicity in beagle dogs can cause necrotizing hemorrhagic pneumonia (Nagata et al. 1992). The absence of intralesional bacteria differentiates compound-induced from bacteria-induced hemorrhagic pneumonia.
Subpleural macrophage accumulation was observed in animals from both gavage and inhalation studies. This condition was similar to that observed in rats (Dungworth et al. 1992). The specific cause and pathogenesis of this lesion is unknown and is probably multifactorial. In general, either bronchial obstruction or direct pneumocyte injury leads to overproduction of surfactant with high cholesterol content. Phagocytosis of this lipid leads to accumulations of foamy macrophages, which may subsequently incite other inflammatory responses. The subpleural location of this lesion and its occasional segmental appearance and, in some cases, the presence of pneumocyte hyperplasia suggest that this lesion might progress to the segmental fibrosis observed in some of the dogs evaluated in this study.
Centriacinar alveolar macrophage accumulation was observed in dogs from inhalation and gavage studies at similar incidences. The centriacinar distribution suggests aerogenous route of entry of the causative agent and is most likely a nonspecific response to inhalation of particulate matter such as dust particles. Inhalation of poorly soluble test compounds can also result in the same type of response (Nikula et al. 2013). Alveolar macrophage accumulation can also be induced by noninhalation administration of compounds which cause phospholipidosis (Mazue et al. 1984; Chang et al. 2014). In dog studies, interpretation of a marginal increase in the incidence and/or severity in dosed groups can be challenging because of the small group sizes used in toxicology studies. In inhalation studies, the macrophages accumulate around respiratory bronchioles, whereas in spontaneous lesions, macrophages tend to accumulate in the subpleural region or are randomly dispersed. In phospholipidosis, alveolar macrophage accumulation is usually multifocal or diffuse and foamy macrophages may accumulate in other organs.
Vascular lesions (hair emboli, pulmonary arteriopathy, and smooth muscle mineralization) were rare findings in this study. The morphological features of pulmonary arteriopathy (concentric medial hypertrophy and intimal thickening and formation of plexiform lesions) observed in the 2 dogs from this study are similar to those seen in human patients with pulmonary arterial hypertension (Tuder et al. 2013). To our knowledge, this lesion has not been reported in beagle dogs. However, similar lesions have been reported in 6 dogs with idiopathic pulmonary arterial hypertension (Zabka, Campbell, and Wilson 2006). Pulmonary arterial pressures were not measured in the 2 dogs from this study, therefore, it could not be determined whether these 2 dogs had pulmonary hypertension. Pulmonary arteriopathy observed in the 2 dogs in this study must be distinguished from lesions associated with idiopathic canine polyarteritis and compound-induced vascular toxicity. In idiopathic canine polyarteritis and compound-induced vascular toxicity, there is usually fibrinoid necrosis, intense periarterial/arterial infiltration by lymphoctes, and the lesions affect mostly the coronary and mesenteric arteries, although pulmonary arteries can be affected (Louden et al. 2000). Vasoactive drugs that induce these lesions in beagles include endothelin receptor antagonists (Louden et al. 2000) and adrenaline (Greaves 2000). The absence of a heavy mononuclear cell arteritis/periarteritis and presence of plexiform lesions can be used to distinguish this type of arteriopathy from test compound–induced vascular lesions or lesions associated with idiopathic canine polyarteritis.
Mineralization of vascular smooth muscle is a common feature of uremic pneumonopathy in dogs with acute or chronic nephropathy (Caswell and Williams 2016). However, in this study, neither of the 2 dogs with this lesion had nephropathy, and no other lesions suggestive of metastatic calcification were observed in these animals. This lesion has not been reported in young beagles (Hottendorf and Hirth 1974; Oghiso, Fukuda, and Iida 1982; Hahn and Dagle 2001; Barnes et al. 2016). However, a high incidence of vascular mineralization has been reported in aging beagle dogs (Hahn and Dagle 2001), most likely this is related to the high incidence of chronic nephropathy reported in these aging dogs. Similar lesions may result from the administration of compounds, which cause hypercalcemia, hyperphosphatemia, or increased bone absorption (Le Boedec et al. 2012; Caswell and Williams 2016).
Epithelial changes (nonkeratinizing squamous metaplasia of the bronchial epithelium, bronchioloalveolar hyperplasia, and hyperplasia of the bronchial epithelium) were observed in a few animals. Inhalation of irritant test compounds can also result in the same type of response. Although the bronchioloalveolar hyperplasia was not located subpleurally, the morphology was similar to the lesion observed in lungs with subpleural septal fibrosis and was most likely an extension of the subleural lesion. In long-term studies, similar epithelial changes can be induced by test compounds that cause irritation (Coggins 2001), and differentiating these from spontaneous lesions might be difficult, especially if few animals are affected. Spontaneous lesions are usually focal and of minimal severity. In some cases, the examination of multiple lung sections to determine the severity and distribution of epithelial lesions is recommended to differentiate compound-induced lesions from spontaneous lesions.
Congenital anomalies of the lungs are rare in animals and may reflect abnormal development of lung bud or pulmonary circulation (Lewis and McKevitt 2013). In this study, 2 cases of pulmonary hypoplasia were observed, and the cause of this lesion could not be determined. This lesion was not reported in most of the previous surveys of spontaneous lesions in beagles (Hottendorf and Hirth 1974; Oghiso, Fukuda, and Iida 1982; Hahn and Dagle 2001; Barnes et al. 2016).
In summary, various lesions including inflammatory conditions, macrophage accumulations, vascular lesions, and epithelial changes were observed in beagle dogs from oral gavage or inhalation studies. There were differential effects associated with the route of administration. Some of the spontaneous lesions are morphologically similar to lesions induced by test compounds, which could interfere with the interpretation of histopathology data. Careful evaluation of the lesion morphology, distribution, severity and the presence or absence of a dose response, and the use of historical control data will aid in differentiating these lesions from compound-induced lesions.
Footnotes
Authors’ Contribution
Authors contributed to conception or design (SM, BG, CP, AB, IK); data acquisition, analysis, or interpretation (SM, BG, CP, AB, IK); drafting the manuscript (SM); and critically revising the manuscript (BG, CP, AB, IK). All authors gave final approval and agreed to be accountable for all aspects of work in ensuring that questions relating to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
