Abstract
This article describes the occurrence of a bilaterally symmetrical encephalopathy in Sprague-Dawley rats, which occurred over the period 2005 to 2012 in our laboratory in both untreated control rats and rats treated with different pharmacologically active compounds. The acute brain lesions consisted of degeneration/necrosis in the ventral areas of the brain mostly with little inflammatory response; in the more rare chronic cases there were numerous lipid-laden macrophages. The areas most consistently affected were the crus cerebri, the ventral midbrain, the pyramids, and the internal capsule. Other areas less frequently affected were the mammillary bodies, the fimbria, the olfactory tubercles, the optic tracts, and the ventral hippocampus. All available data, including clinical signs, gross pathology, clinical pathology, diet, breeding, and housing were collected and are presented. Our investigations did not elucidate the pathogenesis of the lesions, although the infarction-type changes are suggestive of a vascular etiology. To our knowledge, this particular lesion with its consistent distribution pattern has not been reported in the rat literature and its publication is therefore important to the toxicological pathology community, because an unbalanced group distribution in a toxicology study could potentially confound the safety assessment of a compound.
Introduction
Over the past few years, a rather consistent lesion in the brain has been seen in several rat studies at the preclinical development and safety department, Beerse site of Janssen Research and Development. These brain lesions resulted in an acute deteriorating condition of the affected animals and subsequent euthanasia for the majority of rats. The lesion in its acute form consisted of infarction-type changes (areas with degeneration/necrosis) in the ventral areas of the brain mostly with little inflammatory response. In the more chronic cases, there remained areas with numerous lipid-laden macrophages. The lesions were bilateral and usually symmetrical. There was clearly no relationship to treatment. It was considered important to reevaluate all available data of the affected rats in an attempt to find a possible underlying etiology.
All available study-related and individual animal data (dose group and treatment duration, age, sex, body weight [gain], clinical observations, clinical pathology, and pathology) were captured and brain slides were reevaluated.
In the first study in which this entity was encountered, there was a confirmed (temporarily) dietary vitamin K (Vit K) deficiency. Although cases from all subsequent studies had much less hemorrhage associated with the lesions, analysis of Vit K in the diet of the most recently affected study was performed.
Thiamin (vitamin B1 [Vit B1]) deficiency is a well-known cause of degenerative brain changes in rats (Robertson et al. 1975). Thiamin deficiency can cause similar areas of complete necrosis and almost always affects the mammillary bodies (which were commonly affected in our rats). Vit B1 was therefore also analyzed in the diet of the most recently affected study.
We considered it important to publish these spontaneous brain lesions, because an unbalanced group distribution in a toxicology study could potentially confound the safety assessment of a compound.
Since this article was drafted, 3 additional cases were encountered in our test facility.
Materials and Methods
Statement of Ethical Approval
All animal experiments were performed in accordance with the European (ETS No. 123, 2007) and Belgian (1991) guidelines and with the principles of euthanasia as stated in the “AVMA Guidelines on Euthanasia” (American Veterinary Medical Association [AVMA] 2007). The experiments were approved by the Janssen Research and Development Ethical Committee and conducted in an Association for Assessment and Accreditation of Laboratory Animal Care International–approved facility.
Information on Affected Studies and Animals
Animals
Sprague-Dawley rats were supplied by Charles River Laboratories (Germany or France) and acclimatized for approximately 1 week before the start of the experiment. Animals were group housed (6 rats/cage) in polysulfone cages with a wire-mesh roof under routine conditions of temperature, relative humidity, ventilation, and illumination with the exception of the animals of study A that were single housed. A pelleted maintenance (Scientific Animal Food and Engineering [SAFE], France, for one study; Ssniff R/M-H, Germany, for other studies) or special diet (Harlan, the Netherlands) was available ad libitum with free and continuous access to drinking water.
Studies
Table 1 gives an overview of the affected studies, including (sometimes restricted) information on the compound, study type, animal details (sex, group size, housing, and origin), and diet.
General information (design, animals, compound, and diet) on affected studies.
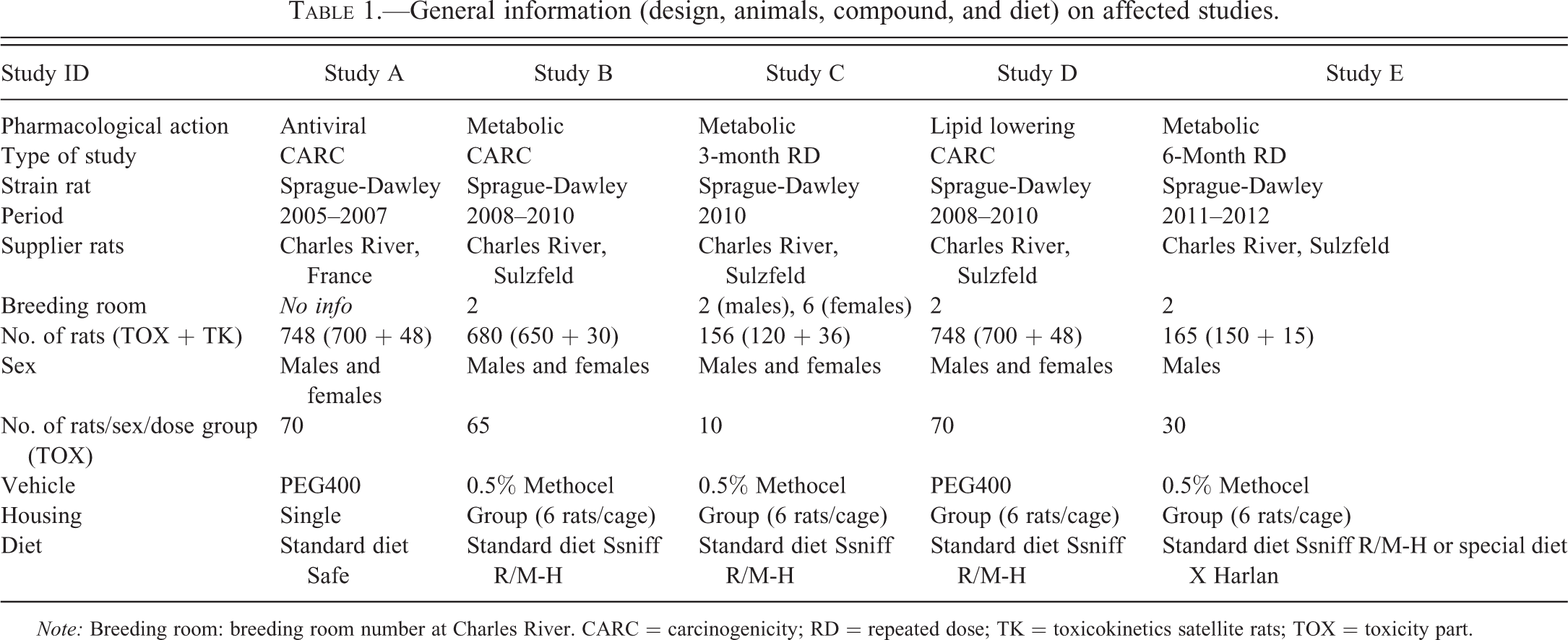
Note: Breeding room: breeding room number at Charles River. CARC = carcinogenicity; RD = repeated dose; TK = toxicokinetics satellite rats; TOX = toxicity part.
Affected studies were performed between 2005 and 2012 and included 3 carcinogenicity studies, one 6-month study (with a 1- and 3-month interim kill), and one 3-month study. In all studies, rats were dosed by oral gavage; approximately 70% of the studies performed at our test facility during this period were oral gavage studies.
In study A, increased mortality in male rats between the second and the fifth month was suspected and confirmed to result from Vit K deficiency, based on clinical observations (pale mucosae and blood loss), prolonged coagulation times, macroscopic hemorrhagic changes at necropsy and dietary Vit K levels. Rats were treated with Konakion (10 mg Vit K1/ml) in weeks 19 and 20, and the diet was enriched with Vit K from about week 20 onward, after which coagulation times normalized as well as mortality rate.
Clinical pathology
Except for study A, all animals were anesthetized with isoflurane before blood sampling. The majority of the affected animals were sacrificed preterminally. These moribund animals were in unfasted condition, and blood was collected from the carotid artery. In rats reaching the normal scheduled blood collection time point or necropsy time point, the animals were fasted overnight, and blood was collected from the orbital venous plexus (study A) or sublingual veins (other studies). Routine blood chemistry parameters were obtained utilizing a Hitachi-Modular automated clinical chemistry analyzer and Roche reagents (Roche Diagnostics, Switzerland). Hematological evaluations were performed on an Advia120 or Advia2120 instrument with multispecies software versions 3.1 and 5.9 (Siemens Diagnostics, Belgium). In the period of 2005 to 2007, the routine coagulation tests, prothrombin time, activated partial thromboplastin time, and fibrinogen were performed on an ACL Futura Plus analyzer, thereafter on a TOP500 instrument, both from Instrumentation Laboratory ([IL], Italy) using IL reagents.
Dietary analysis
Dietary analysis was performed, in particular for Vit K and Thiamin (Vit B1) levels. Samples of the 2 different diets of study E were sent to Ssniff, Soest (Germany) for analysis.
In study A, dietary analysis for Vit K had already been performed on samples of standard diet (SAFE, batch B) due to ongoing coagulation problems and independent of the diagnosis of encephalopathy.
For the standard diets and special diet X, the source of Vit K was menadione, which can also be referred to as Vit K3.
Pathology
Full necropsy was performed on all affected animals and macroscopic changes were recorded. Tissues were fixed in 10% phosphate-buffered formalin (except for eyes and testes in most studies, which are routinely fixed in Davidson’s fixative) and processed routinely; sections were stained with H&E. In studies A, B, and D (carcinogenicity studies), all tissues were examined histologically in all animals (complete tissue list as recommended by Committee for Proprietary Medicinal Products guidelines). In study C, all tissues were examined histologically in control and high-dosed rats with target tissues in intermediate groups. A limited tissue list (excluding brain) was evaluated in study E; all tissues (including brain) were evaluated in preterminally dead or euthanized rats. At the test site, it is a common standard procedure to evaluate all preserved tissues of preterminal dead or euthanized animals in toxicity studies to more accurately assess the cause of death. During the dosing phase of study E, it was decided to—due to unexpected mortality—also evaluate preterminally killed TK animals.
Routine histology of the brain included the following 3 transverse brain levels: at the level of optic chiasm, at the level of the pituitary gland, and a section through the cerebellum and medulla oblongata/pons.
From the single examined TK rat (TK203), additional sections (every 5 μm) were made of the embedded brain tissue and the remaining formalin-fixed brain tissue (from forebrain up to most distal part of medulla oblongata) was processed and evaluated. From all the affected studies, slides of rats with degenerative brain lesions were reevaluated for confirmation of the presence of the typical lesions. The anatomical localization of all the lesions was recorded.
Results
Individual Animal Data of Rats with Encephalopathy
General
In summary, 34 rats in 5 studies were affected (Table 2). Individual information on sex, time on study, treatment, and death status is included in pathology Table 3 (see further).
Number, sex, and dose group of affected rats per study.
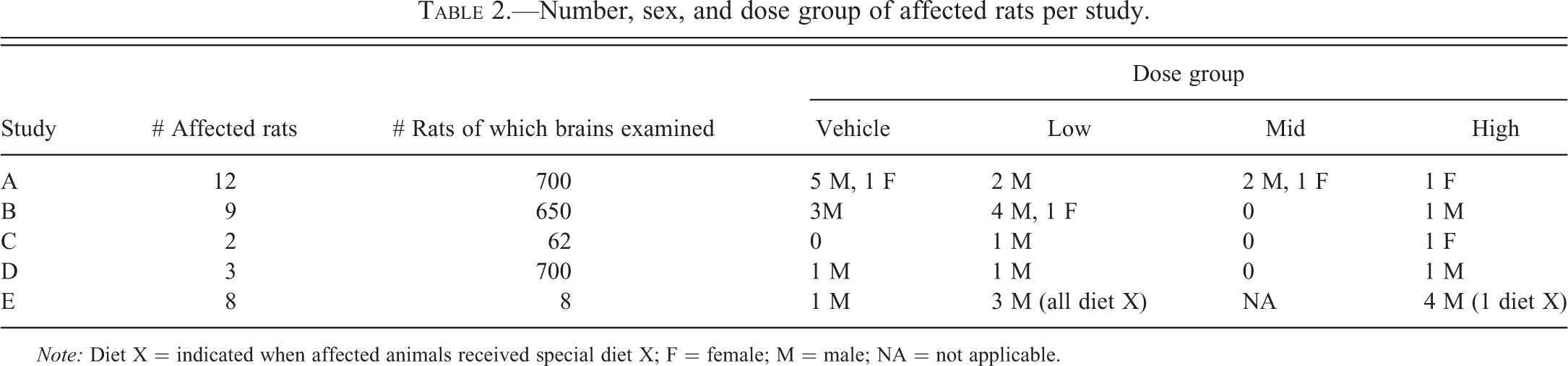
Note: Diet X = indicated when affected animals received special diet X; F = female; M = male; NA = not applicable.
Anatomical distribution of the lesions in the brain per study/animal.
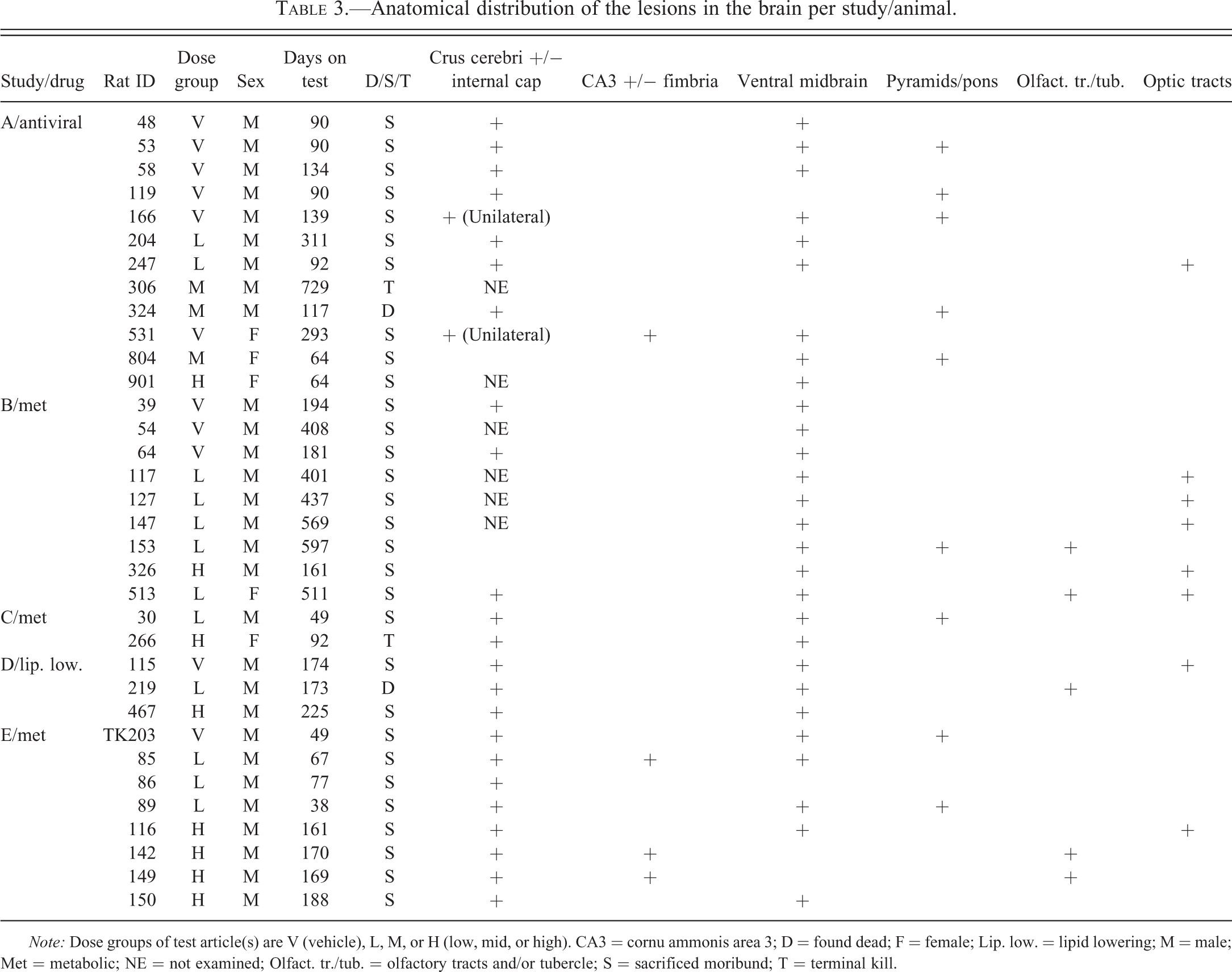
Note: Dose groups of test article(s) are V (vehicle), L, M, or H (low, mid, or high). CA3 = cornu ammonis area 3; D = found dead; F = female; Lip. low. = lipid lowering; M = male; Met = metabolic; NE = not examined; Olfact. tr./tub. = olfactory tracts and/or tubercle; S = sacrificed moribund; T = terminal kill.
Affected rats were killed between study day 39 and study day 729.
Most rats were sacrificed moribund due to their acute deteriorating condition. Only 2 animals were killed terminally and 1 animal was found dead. When considering all studies, there was clearly no relationship to treatment; overall 11 vehicle rats and 23 treated rats, receiving different compounds and dose levels were affected with no dose relationship. Males (29/34) were more commonly affected than females (5/34).
Body weight
All rats (for which data were available) showed prominent body weight loss when comparing their weight on the day of sacrifice to previously recorded weight(s). For several rats, the body weight loss was very acute, occurring during their last day on study. For only a few rats, the body weight loss started more than 1 week prior to death; for the remaining animals the onset of body weight loss occurred during their last week on study.
Clinical observations
The affected rats showed a poor general condition and/or decreased general activity on the day of sacrifice. In addition, about half of the animals had clinical observations that could be linked to the brain lesions, including narrowing of the palpebral fissures (12/34), circling (6/34), and/or ataxia and paresis (1/34). These findings usually occurred on the day of kill and in a minority of animals also on the day before kill, indicating the acute onset of this syndrome.
Clinical Pathology
The clinical pathology profile was not pathognomonic for any possible underlying condition (therefore details not shown). Several commonly affected parameters (e.g., increases in hematocrit, red blood cells, and hemoglobin) were indicative of hemoconcentration, related to anorexia/adipsy due to their poor condition. The majority of rats showed a decrease in lymphocytes, secondary to the animals, deteriorating condition/stress. Evaluation of clotting parameters is not routinely done in preterminally killed rats and—if scheduled—it was often not possible to withdraw sufficient blood or a good quality sample for coagulation assessment due to moribundancy. Some rats of study A showed significant prolongation of coagulation times, which was attributed to the temporarily low Vit K content in the diet; moreover, the compound dosed in this study was known to slightly increase coagulation times in rodents. Although limited in number of data, measured coagulation times were normal in rats of other studies.
Dietary analysis
Table 4 gives an overview of dietary levels of Vit K and B1. The dietary Vit K level of the standard (37 mg/kg) and special diet X (3 mg/kg) of study E exceeded the required level. As indicated before, the Vit K level of the initial standard diet of study A was below the required need.
Summary table dietary vitamin K and B1 levels.
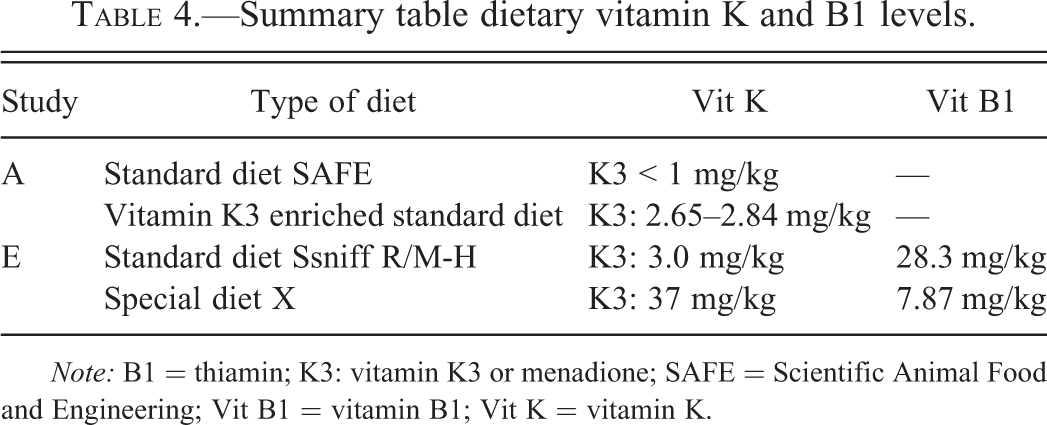
Note: B1 = thiamin; K3: vitamin K3 or menadione; SAFE = Scientific Animal Food and Engineering; Vit B1 = vitamin B1; Vit K = vitamin K.
For the diets examined, the Vit B1 level exceeded the required level (Institute for Laboratory Animal Research 1995).
The diets did not contain fish (communication with supplier), which can be a source of thiaminase.
Gross pathology
Gross brain lesions were noted in 3 animals. These were characterized by a red discolored focus in the brain of rat no. 247 of study A, red foci/areas in the medulla oblongata of rat no. 266 of study C, and dark discoloration of the cerebrum in TK203 of study E.
Histopathology
The brains of 34 affected rats were examined at the 3 routine levels and the brain of 1 rat was step sectioned from the olfactory bulb to the medulla oblongata (20 sections). The slides from this animal did not contribute any further relevant observations.
The areas most consistently affected were the crus cerebri (Figures 1 and 2), the ventral midbrain (Figure 3), the pyramids (Figure 4), and the internal capsule. Other areas less frequently affected were the mammillary bodies, the fimbria, the olfactory tubercles, the optic tracts, and the ventral hippocampus (cornu ammonis area 3 [CA3]). The lesions were bilateral and symmetrical for the most part and although principally affecting white matter tracts, gray matter was also involved, particularly in nuclei adjacent to the white matter lesions and in the ventral midbrain where the mammillary peduncle and nuclei, the nucleus interpeduncularis, and the medial portions of the substantia nigra were often affected.
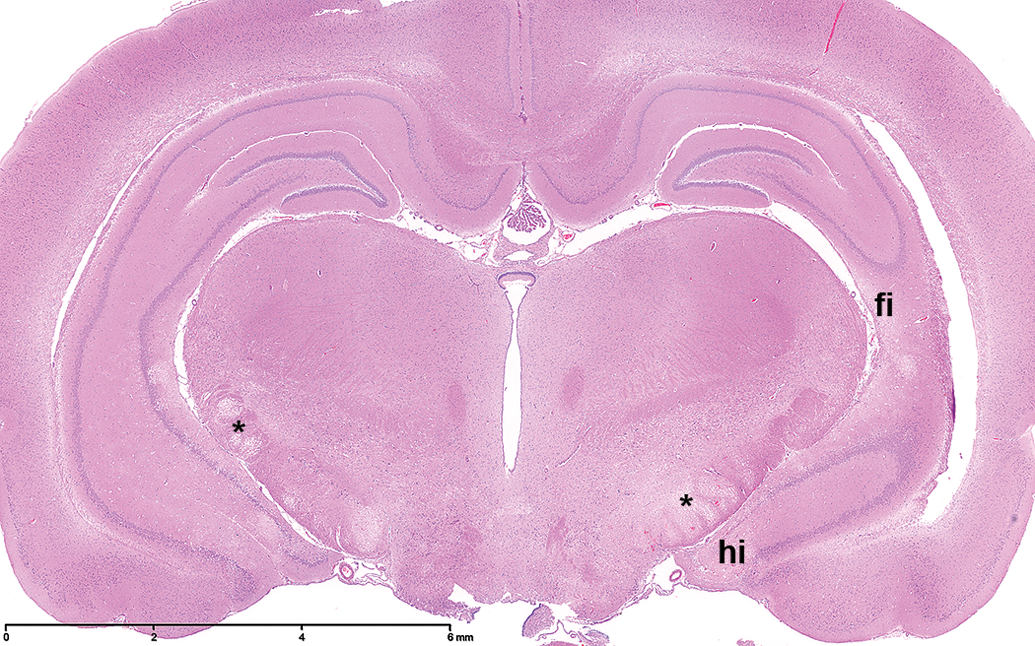
Full cross section of the brain at the level of the third ventricle, showing marked rarefaction of the crus cerebri (*) bilaterally. Also visible are small areas of rarefaction in the fimbria (fi) and the hippocampus (hi). H&E.
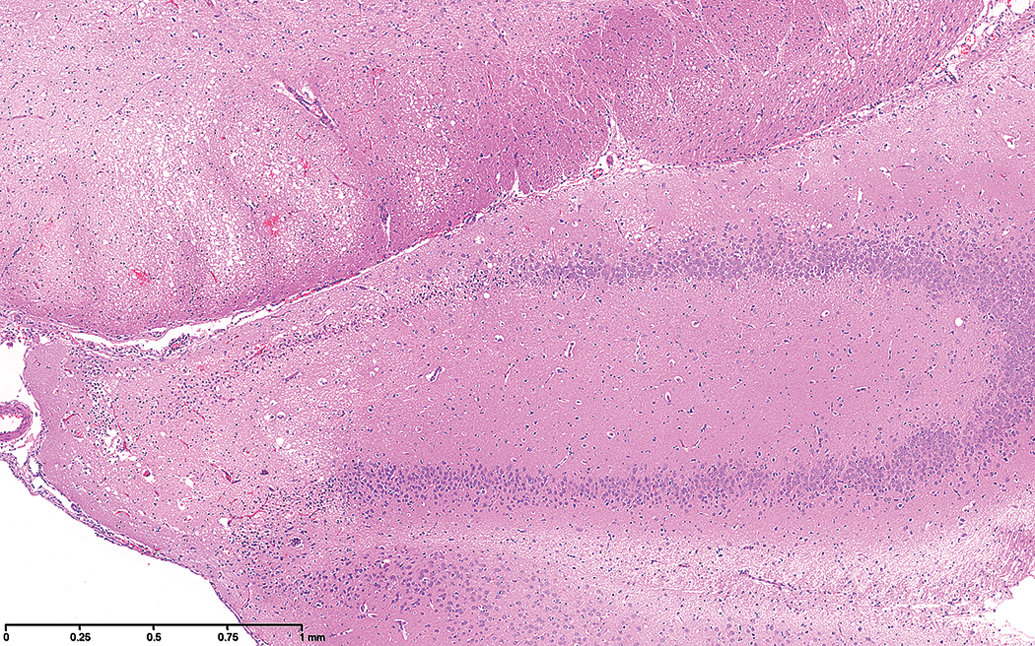
Higher power magnification of Figure 1 showing the vacuolar changes in the crus cerebri and the tip of the hippocampus.
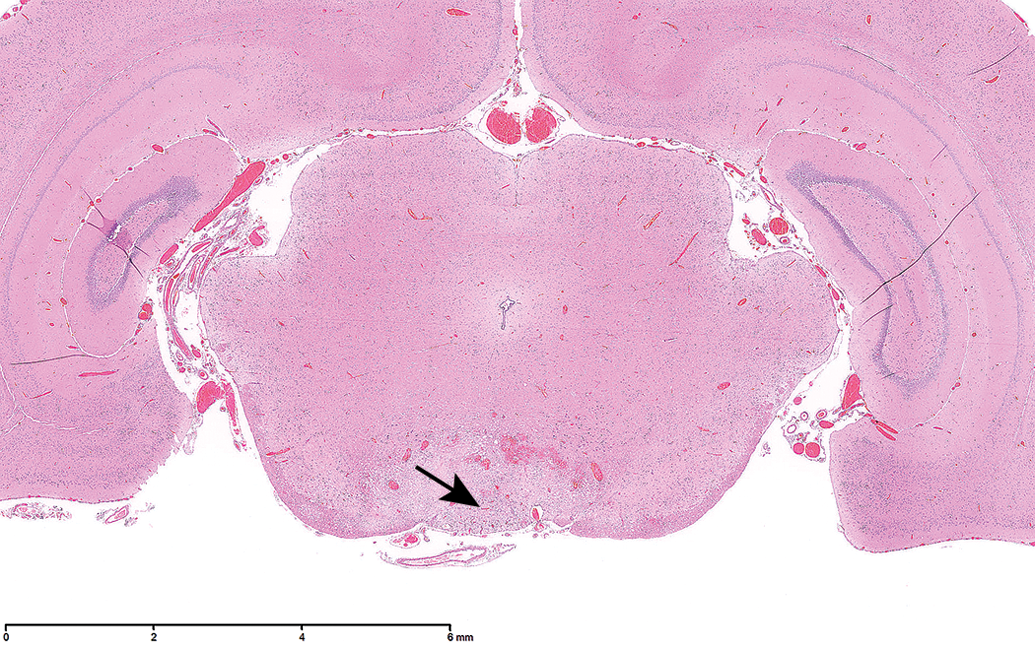
Midbrain at the level of the rostral colliculi, showing rarefaction in the ventral midline area involving the nucleus interpeduncularis (arrow) and surrounding structures.
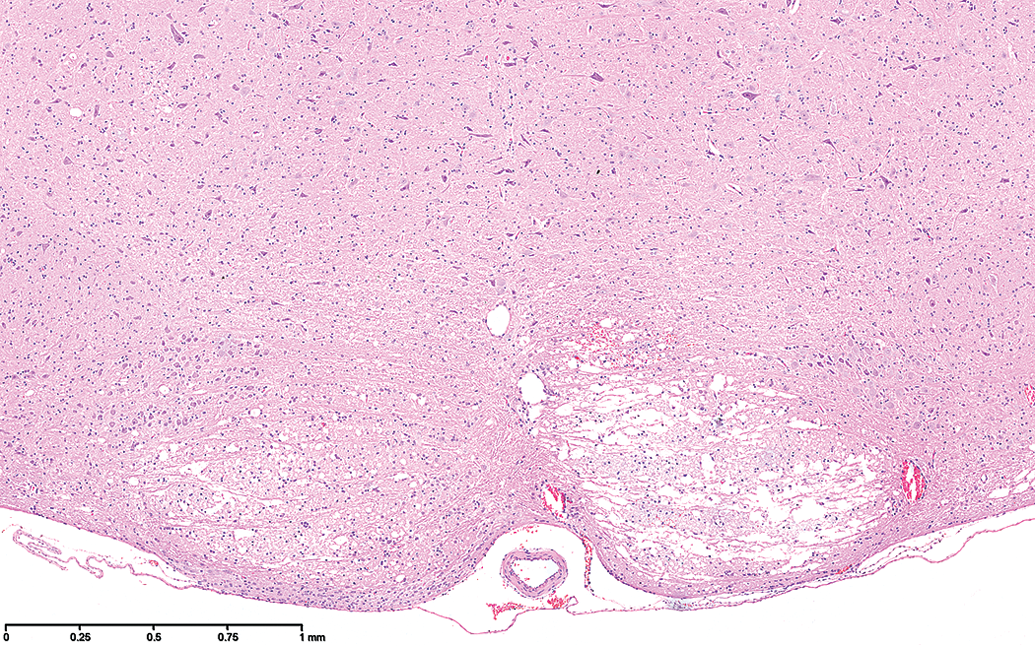
Section through the pyramid (corticospinal tracts) showing rarefaction of this structure, it being more severe on the right but present bilaterally.
The lesions were acute in the vast majority of cases and consisted of relatively well-defined areas of white matter vacuolation with pyknotic appearing glial cell nuclei and separation of fibers (edema; Figure 5), progressing to necrosis of neurons as well as glial cells. There was little inflammatory cell infiltrate apart from occasional neutrophils and monocytes and little blood vessel reaction was observed apart from occasional thin perivascular cuffs. In the more uncommon cases, where animals evidently had survived for a longer period of time, resulting in the development of more chronic lesions, lipid-laden macrophages filled the necrotic areas (Figure 6).
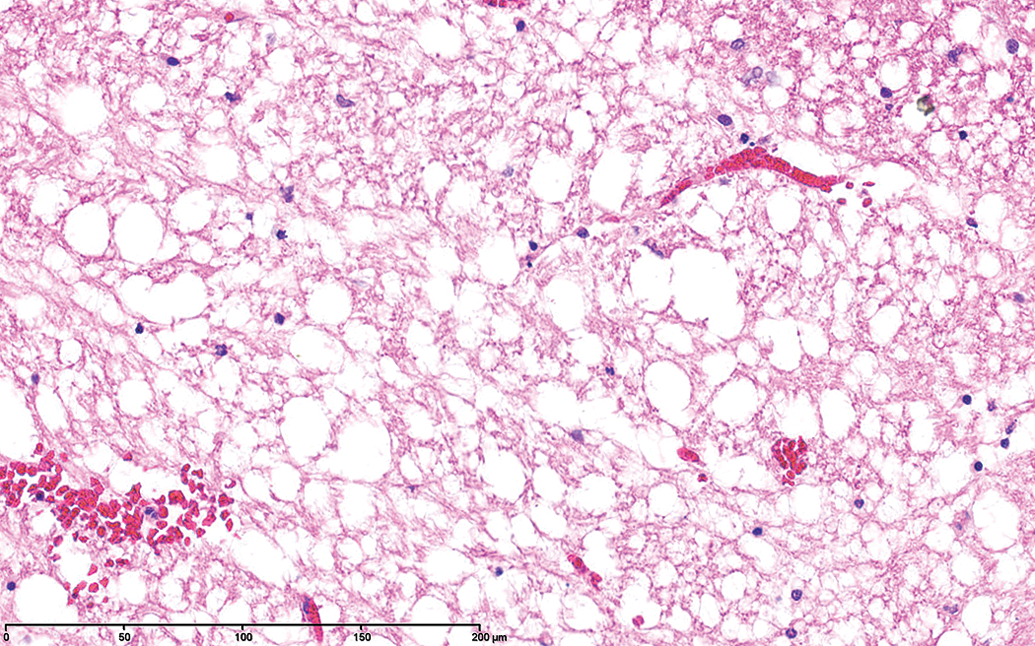
Higher power of acute lesion in the pyramidal area showing vacuolation of white matter, some glial cell pyknosis, and minor peracute hemorrhage.
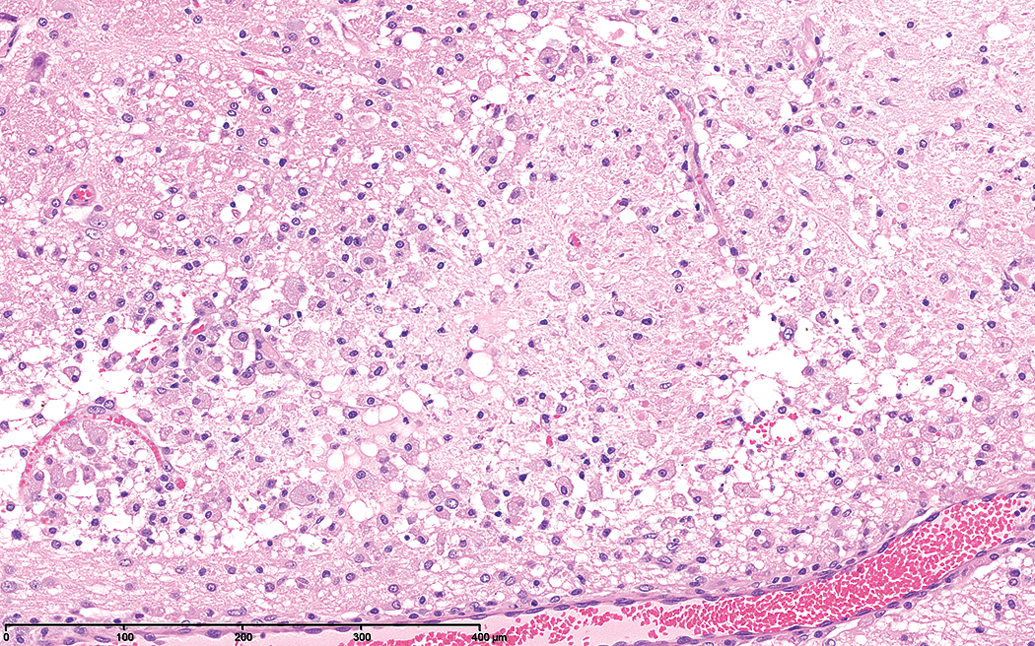
A more chronic lesion in the crus cerebri showing the formation of lipid-laden macrophages.
In one study (study A in Table 3) with a development compound, both vehicle control and treated animals had similar lesions as described above to which was added the presence of significant hemorrhage. The diet in this study was found to be deficient in Vit K.
Table 3 shows the distribution of the lesions in 5 separate studies with 3 pharmacologically unrelated compounds.
Discussion
A degenerative brain lesion called “bilateral symmetrical idiopathic necrotizing encephalopathy” has been observed in a total of 34 rats out of 2,120 rats divided over 5 studies at the preclinical development and safety facility, Beerse site of Janssen Research and Development, between 2005 and June 2012. Study details and individual animal data were analyzed and summarized, and in 2 studies the diet was analyzed for Vit K and Vit B1 levels.
Affected rats were between 39 and 729 days on study, which corresponds to an age range between almost 3 months and 2 years. Males were much more frequently affected (29/34). The onset of the disorder was acute: clinical observations (related to the general deteriorating condition or brain lesions, such as narrowing of the palpebral fissures and/or circling) usually occurred during the last 24 hr, and body weight loss was usually noted during the last day or week. Most rats had to be sacrificed preterminally in moribund condition.
The acute onset and type of clinical observations, the common presence of acute lymphoid atrophy, and the body weight loss in the affected rats indicate that this is an acute process that is stressful for the animals. Overall, there was clearly no relationship to treatment; 11/34 rats were negative controls, and the condition was encountered in studies with 3 different compound classes (antiviral, metabolic, and lipid lowering). In addition, the brain was unaffected in other repeated dose studies with the same compounds at similar or higher doses under similar conditions and in the same rat strain.
Changes in clinical pathology parameters were unspecific and largely associated with the animals’ general deteriorating condition. Coagulation times (if available) were known to be prolonged in study A, due to a temporarily Vit K–deficient diet but were normal in rats of other studies.
The acute brain lesions consisted of degeneration/necrosis in the ventral areas of the brain mostly with little inflammatory response (minor neutrophilic infiltration); in more chronic cases, there were numerous lipid-laden macrophages and there sometimes remained cystic areas. In these few chronic cases, the lesions can be considered ≥72–96 hr based on the prominent presence of macrophages. The areas most consistently affected were the crus cerebri (Figures 1 and 2), the ventral midbrain (Figure 3), the pyramids (Figure 4), and the internal capsule. Other areas less frequently affected were the mammillary bodies, the fimbria, the olfactory tubercles, the optic tracts, and the ventral hippocampus (CA3).
The combination of the lesions in the crus cerebri and the pyramids alone would suggest a primary lesion in the motor cortex, but lesions were not seen here in any of the animals. In addition, many other anatomical areas unconnected to the motor cortex were affected.
The lesions did not resemble those due to generalized cerebral hypoxia or hypoperfusion as these are generally more important in the hippocampus and cerebral cortex.
The topography and morphology of the lesions are suggestive of a vascular or metabolic origin. Thrombi or primary vascular lesions were not identified despite serial sectioning in one affected TK rat. Due to the occurrence with 3 pharmacologically and structurally unrelated compounds and its presence in untreated animals, it is considered as being unrelated to the compounds administered. In study A, where the diet was deficient in Vit K, hemorrhage was noted in addition to the other encephalopathic lesions. It seems possible that this hemorrhage occurred predominantly in the same areas due to the fragility of the vasculature within the lesions.
Because of the common presence of hemorrhage within the brain lesions of other studies and the high incidence in male rats, dietary Vit K levels were determined in recent affected studies. Males are more sensitive to develop coagulation disorders and hemorrhages related to Vit K deficiency, since estrogen has a protective effect (Matschiner and Willingham 1974).
Vit K deficiency could be excluded as the primary underlying etiology, based on normal coagulation times (except for study A) and the normal dietary Vit K contents (exceeding the recommended 1 mg Vit K/kg diet; Institute for Laboratory Animal Research 1995).
Thiamin (Vit B1) deficiency is a well-known cause of degenerative brain changes and can be associated with brain hemorrhages in rats (Robertson et al. 1975). Thiamin deficiency can cause similar areas of complete necrosis and therefore Vit B1 was also evaluated in the diet. The dietary Vit B1 level exceeded normal requirements. Rats require about 4 mg Vit B1/kg diet for growth and reproduction (Institute for Laboratory Animal Research 1995), and the diet did not contain fish meal; fish (especially raw) can contain high thiaminase levels. No further assessment of possible anti-thiamine factors was performed.
Arguments against thiamine deficiency were the hyperacute onset of clinical signs, the lack of neurological signs commonly seen with thiamine deficiency (e.g., ataxia and paresis, recumbency, opisthotonus, and extensor rigidity of the limbs), and the lack of a higher incidence of more subtle degenerative brain lesions in, for example, terminal rats at the test facility.
Rats from studies B, C, and D came from Charles River, Sulzfeld. Except for 1 female (no. 266 of study C), all affected rats in these 3 studies were confirmed to originate from the same breeding room (no. 2). This could be indicative of a common genetic susceptibility in these animals. For study A, rats came from Charles River, France. Charles River could not supply details on the breeding room of this older study. Since (breeding) rats are exchanged between Charles River Sulzfeld and France, a genetic susceptibility cannot be ruled out completely. Charles River was not aware of any cases from other companies.
Southard and Brayton (2011) recently described a new syndrome in Swiss mice termed spontaneous unilateral brain stem infarction, which closely resembles our cases in terms of the histological lesions of necrosis, degeneration, and variable amounts of hemorrhage, and, to a certain extent, in their distribution within the central nervous system (CNS).
However, important differences include the fact that their cases were all unilateral and many had neurological signs referable to vestibular disease, while the vast majority in our series was bilateral and symmetrical and lacked specific or neurological signs. It seems also that some of their cases appeared to be more chronic, while the lesions of the rats in the present series were mostly of an acute nature, without specific prodromal neurological signs. In one case, they describe and show a fibrin thrombus in a superficial branch artery, a feature we were not able to identify in any of our cases.
Brain infarcts have been produced experimentally in many species. In rabbits (Amiridze et al. 2009), they were produced by endovascular occlusion of the basilar artery, which caused bilateral ischemic lesions particularly in the pons and less consistently in the midbrain, medulla, and cerebellum. The authors ascribe this variability to the individual variation in the anatomic blood flow. Differences in blood flow within the brain have been also shown to occur between different strains of mice (Barone et al. 1993; Yang et al. 1997). In rats (Henninger et al. 2006), CNS infarcts were produced by the introduction of thrombi into the vertebral artery resulting in ischemic lesions in the pons, midbrain, and cerebellum.
The syndrome in Swiss mice resembles the Wallenberg lateral medullary syndrome, the most common form of brain stem infarct in man (Southard and Brayton 2011; Kim et al. 1994). Other less common causes of such lesions are abnormalities of the vertebral arteries in children (Ganesan, Cox, and Gunny 2011) and abnormalities of the cervical vertebrae such as subluxation (Ganesan et al. 2002).
Iatrogenic causes of vertebral artery injury are well described in man and include cervical spinal surgery and chiropractic manipulation (Inamasu and Guiot 2005) and, although uncommon, can have catastrophic consequences in terms of CNS degenerative lesions such as stroke.
A possible cause, although unpublished to our knowledge, of the type of lesions described in this article is cervical trauma due to manipulation during the gavage procedure. Although we cannot completely dismiss this possibility, we feel it is unlikely for several reasons, the foremost being that most of our technicians are well experienced with the technique, the majority being involved in all the gavage studies over the period concerned, and we performed a total of 130 oral gavage studies, in which we had affected rats in 6/130, and 0/18 by other routes.
In most species, rat included, paired vertebral arteries arise from the subclavian artery and course toward the brain between the transverse foramina of the cervical vertebrae from C6 to C1 and anastomose in the midline to form the basilar artery, in between here and the oculomotor nerve it gives off the inferior cerebellar artery and then the superior cerebellar artery (Zeman and Innes 1963; Noden and de Lahunta 1985). Blockage of the basilar artery would likely give rise to bilateral lesions, whereas blockage of the cerebellar arteries would be more likely to give unilateral lesions, depending on the presence of collateral circulations.
The similarities in the morphology of the lesions and their distribution between these experimental models, as well as the spontaneous syndrome reported by Southard and Brayton (2011) and our cases reinforce our conclusion that this is probably a vascular-related phenomenon, both strain and individual variations in anatomic blood supply explaining the differences in the distribution of the lesions between animals but the exact pathogenesis of such an ischemic lesion in our rats remains unknown.
To conclude, idiopathic “bilaterally symmetrical necrotizing encephalopathy” was observed in a total of 34 rats divided over 5 studies at the preclinical development and safety facility, Beerse site of Janssen Research and Development, between 2005 and June 2012. Study details and individual animal data were analyzed and summarized, and the diet was analyzed for Vit K and Vit B1 levels.
We considered it important to publish this previously undescribed entity, because an unbalanced group distribution in a toxicology study could potentially undermine safety assessment of a compound.
Footnotes
Acknowledgments
We are grateful to the biotechnicians and the laboratory staff of the Drug Safety Sciences department for excellent technical work over the years. We also wish to thank Erik Hansen for his technical help.
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Authors’ Contribution
Authors contributed to conception or design (SD and DA); data acquisition, analysis, or interpretation (EM, PV, BF, LL, AV, and AD); drafting the manuscript (SD and DA); and critically revising the manuscript (EM, PV, BF, LL, AV, and AD). All authors gave final approval and agreed to be accountable for all aspects of work in ensuring that questions relating to the accuracy or integrity of any part of the work are appropriately investigated and resolved. SD and DA contributed equally to this article.
