Abstract
The International Conference on Harmonization (ICH; S1B of 1997) allows a second species carcinogenicity study to be an alternative to one of the traditional 2-year studies. In the past 17 years, the FDA’s Center for Drug Evaluation and Research’s (CDER) Executive Carcinogenicity Assessment Committee received 269 alternative carcinogenicity assay protocols for review. This committee’s recommendations regarding choice of animal model and dose selection are generally followed by sponsors conducting these studies to increase the acceptability of such studies. The P53+/− assay is generally considered appropriate for genotoxic products, and the TgRasH2 assay is appropriate for non-genotoxic or genotoxic drugs. In the United States, the TgAC assay is not used any more and the animals are no longer available. The TgAC assay can detect both tumor promoters and complete carcinogens, and consequently more than half of the dermal TgAC assays resulted in a positive assessment. Currently, more than 75% of mouse carcinogenicity studies are conducted in TgRasH2 mice. Behavior of genotoxic and non-genotoxic drugs in the various assays is reviewed.
Introduction
Assessment of the carcinogenic potential of small-molecule pharmaceuticals has generally been conducted in 2 species, most often rats and mice. International Conference on Harmonization (ICH; S1B of 1997) allows a second species carcinogenicity study to be an alternative to a 2-year study. Rats are preferred for the traditional 2-year assay at present, in the absence of clear evidence favoring a study in mice. Several alternative models have been used and are generally conducted in mice. In the United States, the CDER Executive Carcinogenicity Committee considers proposals and justification for the particular alternative animal model from drug sponsors. This article reviews the number of alternative protocols and final studies received by CDER. We discuss the results of these studies and the overall performance of the assays.
Consideration for Assay Selection, Protocols Received, and Results Received
Carcinogenicity study results with phenolphthalein in 1997 triggered greater interest in the P53+/− assay (Dunnick et al. 1997). The p53-deficient (+/−) mouse model responded to phenolphthalein treatment with a carcinogenic response of thymic lymphomas after only 4 months of dosing. Previously, phenolphthalein had resulted in thymic lymphomas in male and female B6C3F1 mice in 2-year studies (NTP 1996). These findings resulted in removal of phenolphthalein from the over-the-counter (OTC) market in 1999 (FDA 1999). By 1998, protocols for alternative assays in greater numbers started to be submitted to CDER/FDA. Initially, most alternative carcinogenicity protocols were for the P53+/− assay. The P53+/− assay was accepted if the drug was clearly or equivocally genotoxic; later, only if the drug was clearly genotoxic. The P53+/− assay has been accepted even if the drug was only positive for inducing chromosomal aberrations (CAs) as long as the signal was clear. The neonatal model was accepted if the drug was clearly or equivocally genotoxic. The TgAC model was accepted for dermally applied products and for the testing of active ingredients administered to humans by any route, but administered to the TgAC animals dermally. Use of the TgAC model has declined and the animals are no longer available in the United States. The TgRasH2 model was accepted for genotoxic or non-genotoxic products, but not by the dermal route of administration. Currently, most carcinogenicity testing is conducted using a 6-month transgenic mouse model paired with a standard 2-year rat study. Details of the alternative models are given in multiple articles in the January 2001 supplement to Toxicology Pathology (Tox Path 2001) and in Sistare and Jacobs (2003).
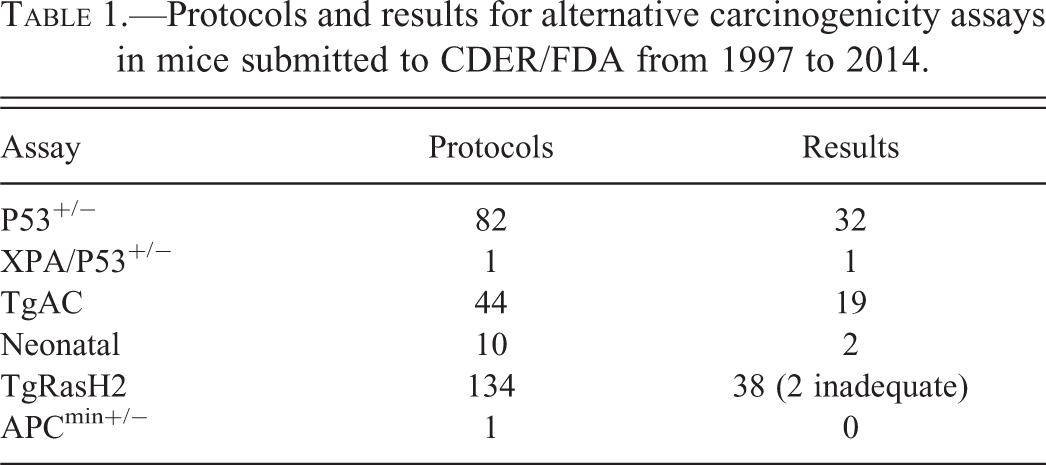
See Table 1 for protocols and results received by CDER for various alternative carcinogenicity assays from 1997 to 2014.
Protocols and results for alternative carcinogenicity assays in mice submitted to CDER/FDA from 1997 to 2014.
P53+/− Assay
As of June 10, 2014, 2 of the 32 submitted final P53+/− studies were positive. Another 2 studies were positive, but were also positive in wild-type animals; therefore, carcinogenicity was not considered related to the enhanced sensitivity of the animals due to the deletion of one allele of P53.
Performance of positive controls
It is generally recommended that positive control compounds be used in all transgenic alternative animal carcinogenicity studies. Benzene, methyl nitrosourea (MNU), and p-cresidine have been used as positive controls in the P53+/− assay. All the studies discussed in this article included a positive control. Of the 3 benzene controls, 2 gave expected neoplasm results and 1 failed. Of the first 5 studies with MNU, 4 produced the expected neoplasms and 1 failed. Of the studies with p-cresidine, performance was very variable as illustrated in Figure 1, which shows the variation of urinary tract neoplasm incidence in positive control animals. The source of the variation is unknown.
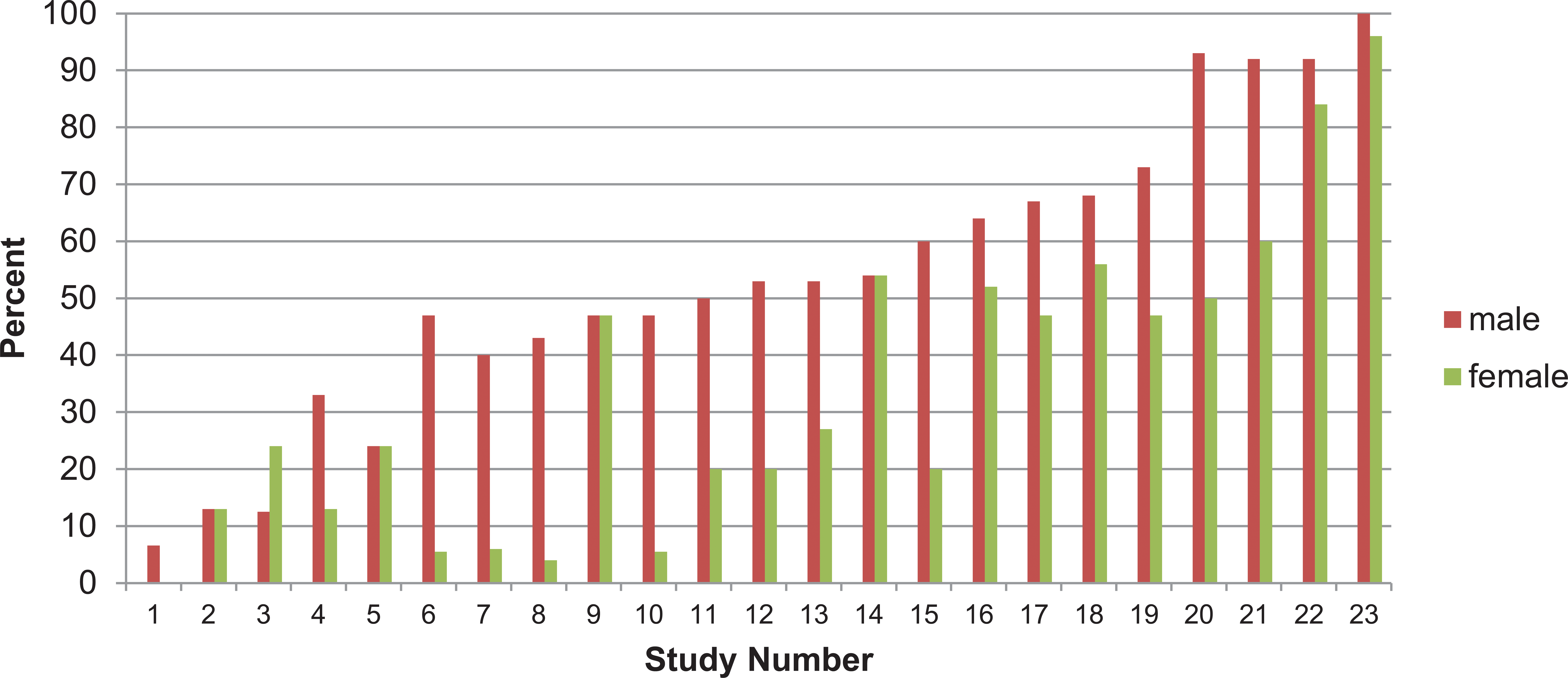
Urinary tract neoplasm incidence (%) for p-cresidine (400 mg/kg per day) in the P53+/− assay.
The incidence of urinary bladder neoplasms in the p-cresidine positive controls increased as the age of the animals increased at study initiation. Initially, 15 animals per group were used, but the number was increased to 25 animals by CDER/FDA to improve the statistical power. The drugs tested in the P53+/− studies exhibited a variety of genotoxicity profiles. The 2 positives in the P53+/− assay were both genotoxic. Phenolphthalein was genotoxic in vitro in Chinese hamster ovary (CHO) cells and in the in vivo micronucleus test. The second chemical that was positive in the P53+/− assay (a drug degradant) was positive in the mouse lymphoma assay.
Genotoxicity results for those drugs that were negative in the P53+/− assay are shown in Table 2.
Distribution of genotoxicity findings for compounds that were negative in the P53+/− assay.
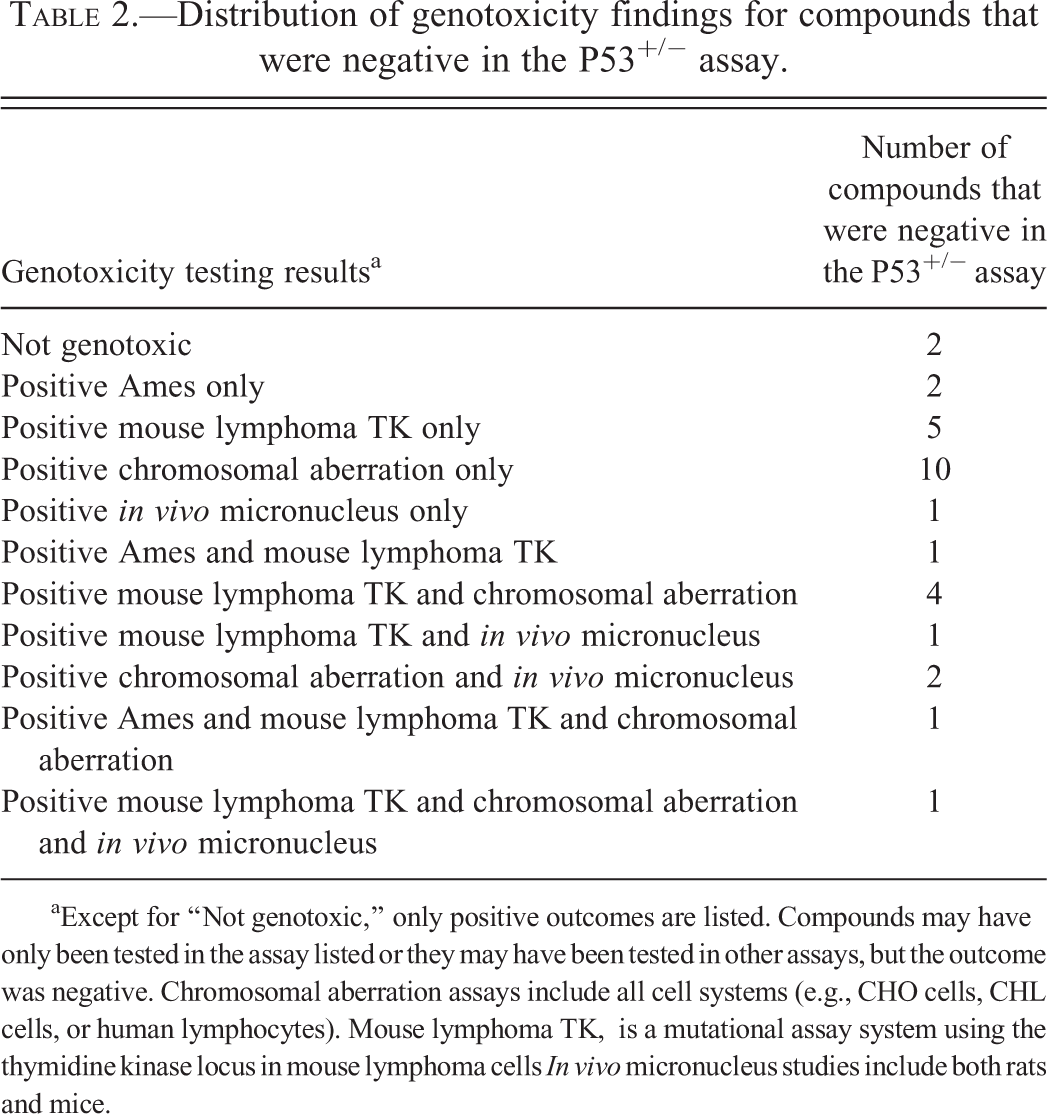
aExcept for “Not genotoxic,” only positive outcomes are listed. Compounds may have only been tested in the assay listed or they may have been tested in other assays, but the outcome was negative. Chromosomal aberration assays include all cell systems (e.g., CHO cells, CHL cells, or human lymphocytes). Mouse lymphoma TK, is a mutational assay system using the thymidine kinase locus in mouse lymphoma cells In vivo micronucleus studies include both rats and mice.
Some of the drugs that were negative in the P53+/− assay produced neoplastic findings when tested in 2-year rat assays. Carcinogenicity findings in rats for drugs that were negative in the P53+/− assay included brown fat hibernomas, urinary bladder carcinomas, stomach enterochromaffin-like cell neoplasm, lymphoma, thyroid follicular cell neoplasms, mammary neoplasms, adrenal (cortical adenomas and pheochromocytomas), lung neoplasms, and skin neoplasms. Some findings in rats were attributed to non-genotoxic mechanisms, and some studies in rats had no drug-related neoplastic findings.
Eleven of the drugs tested in P53+/− mouse studies also had 2-year studies conducted in the mouse. Six of those eleven 2-year mouse studies had no drug-related neoplastic findings. Five of those studies had drug-related liver neoplasms only or liver plus lung (one study) or rete testes neoplasms (1 study).
Possible Conclusions Regarding Negative P53+/ − Findings
Several conclusions could be possible based on the results of the P53+/− assays observed by CDER over the past several years. Most of the studies were negative for carcinogenicity despite the drugs having some positive genotoxicity signal. A positive result in an in vitro CA assay did not necessarily predict a carcinogenic result in a P53+/− study. The P53+/− assay may be generally insensitive to drugs causing CA. Of the 19 drugs with positive CA findings, 18 were negative for neoplastic findings in the P53+/− assay. Alternative explanations could be that the recommended protocol for the P53+/− assay is generally insensitive, or alternatively, an indirect mechanism was responsible for the signal detected in an assay in the genotoxicity battery. In this latter case, the P53+/− assay may have been inappropriate because of a false positive genotoxicity signal. It is not known what is more predictive of human effects, the P53+/− findings or 2-year studies in mice. However, the 2-year findings in mice (e.g., liver neoplasms) were not necessarily relevant to humans.
Potential Issues with the P53+/− Protocol
The variable performance of the positive control chemicals in the P53+/− assay is very notable. The effects of age at study initiation could be better understood, as this appears to have an impact on susceptibility of the mice to tumor formation. There appears to be a higher background of bone formation and osteosarcoma in P53+/− mice if 10- to 12-week-old animals are used at the start of the study rather than 6- to 8-week-old animals. Perhaps the age at study initiation should be standardized. Some have wondered whether increasing the study duration to 9 months would increase the power of and confidence in the test. This is based on the assumption that treating the animals for a longer duration would increase their response to a carcinogen, while the background tumor rate remained sufficiently low so as to preserve the ability to detect a true increase in drug-induced tumors. The proposal to extend the studies to 9 months duration has not been implemented.
Because fewer and fewer genotoxic drugs are submitted for regulatory study, the P53+/− assay has been used less and less, especially since the TgrasH2 animals became available. The discordant results between the rat 2-year studies and the mouse P53+/− results could be interpreted to mean that the rat findings may not be a result of P53 effects.
TgAC Assay
Of the 17 final TgAC studies submitted to CDER by June 10, 2014, 9 had a positive tumor signal. One study was negative at the application site but positive in untreated skin. One study was uninterpretable due to conduct and may have been positive. This assay appears to be sensitive to vehicle effect, especially dermatologic vehicles. Originally, the TgAC assay was thought to be useful for testing entire dermal formulations of non-genotoxic products.
Only dermal application studies have been considered acceptable in Tg.AC (v-Ha-ras) transgenic mice (TgAC mice). In these studies, application is to a shaved area on the animal’s back. In the evaluation of study results, papillomas at distal sites (e.g., urogenital) were not considered. Dermal formulations were not diluted, but could be enriched with drug substance. As with other topical carcinogenicity studies, high dose selection was based on the maximum tolerated dose (MTD) or maximum feasible dose (MFD). The MFD was generally defined as application of the largest possible volume of the formulation containing the highest possible concentration of the active ingredient that did not change the physical properties of the formulation.
12-O-tetradecanoyl-phorbol-13-acetate (TPA, 2.5 µg, 3 times per week) is routinely used in the TgAC assay as a positive control. Acetone was often used as the vehicle for TPA. However, it was noted that TPA potency was not the same in all vehicles. For example, TPA failed to induce papillomas or gave a lower response when formulated in dimethyl sulfoxide (DMSO). TPA failed in ethanol diluted below 85%. TPA gave a lower response in acetone/olive oil than in acetone alone. The positive control, TPA, thus needed to be checked in the clinical vehicle so as to confirm that the vehicle did not interfere with the assay. This could have been done in preliminary studies or may have been assessed as an additional arm of the carcinogenicity assay.
The dermal MTD should not be exceeded when selecting the high dose for the TgAC assay. Indication of achieving the dermal MTD has included moderate erythema, scaling, slight edema, alopecia, and thickening, as well as epidermal hyperplasia, fibrosis, minimal–mild epidermal edema, minimal–moderate dermal edema, and moderate inflammation.
In 1 TgAC study, the drug substance in a clinical vehicle was positive in both males and females, but the same drug substance in 85% ethanol was negative in both males and females. In another case, the drug vehicle alone was positive in males and females. Overall, the relevance of results of the TgAC assay to humans has been unclear.
Examples of Non-neoplastic Skin Effects but No Skin Neoplasms in the TgAC Assay
We have noted that chronic inflammation or irritation of skin does not necessarily lead to skin neoplasms in TgAC mice. Some examples are considered below.
For drug A, which was considered positive for papilloma formation in the TgAC mice, the incidence of skin neoplasms did not correlate with the incidence of hyperkeratosis or inflammation. Squamous cell papillomas occurred in 19/20 male and 17/20 female low-dose animals in the absence of inflammation, and the incidence of hyperkeratosis was less than in control: 2/20 low dose versus 8/20 control. No irritation, erythema, edema, hardening, or desquamation was observed in the 4-week dose-ranging study for drug A.
For drug B, which was considered positive, inflammation, hyperkeratosis, and acanthosis in the skin of the mid- and high-dose groups were similar to that for the positive control, TPA.
For drug C, which was considered positive, no inflammation, hyperkeratosis, or acanthosis was seen.
For drug D, which was not considered positive, there was drug-related epidermal hyperplasia, but the site of application papilloma incidence was minimal (males: 0/15, 0/15, 0/14, 0/15, 2/15; and females 0/15 [control], 0/15, 2/15, 2/15, 2/15; with a positive control incidence of 14/15 in males and 14/15 in females).
Excipient A was negative in the TgAC assay, at a dose that caused acanthosis in 10/10 and skin ulcers in 2/10 B6C3F1 mice at 13 weeks. A much lower dose of excipient A in 2-year dermal National Toxicology Program (NTP) studies caused hyperkeratosis.
Correlation of the TgAC Mouse Assays with Standard 2-year Rat Studies
Thirteen drugs tested in the TgAC assay also had results from the traditional 2-year rat assays. Eight of these 13 studies with positive TgAC results had negative results in traditional rat carcinogenicity assays. No traditional studies were conducted for 3 other products. Two rat studies have not yet been received by the agency.
Although the TgAC assay was evaluated by International Life Sciences Institute (ILSI) (Toxicol Path 2001) and considered by ICH as a stand-alone alternative to a traditional mouse assay, it is not clear that the assay distinguishes promoters from complete carcinogens. Although assessment of promoting potential alone has not been routine for drug development, one could consider that this is more representative of products applied to sun-exposed skin, since sun-exposed human skin has already been modified by ultraviolet exposure.
TgRasH2
Carcinogenicity assays in TgRasH2 mice have become the most common type of alternative protocol submitted to CDER for both genotoxic and non-genotoxic drugs. This is probably because the TgAC assay has fallen out of favor because it has occasionally been difficult to interpret. In addition, the TgRasH2 assay is considered acceptable for both genotoxic and non-genotoxic drugs, whereas the P53+/− assay is considered appropriate only for clearly genotoxic drugs, of which there are few. As of June 10, 2014, 134 protocols and 38 final results have been received by CDER/FDA for studies in TgRasH2 mice.
Study Design Details
Twenty-five animals per group is desirable. There is a variable high background of pulmonary neoplasms (up to 6/25 = 24%) and of hemangiosarcomas (generally 5–8% but up to 3/15 = 20% in males and females) at 6 months. An MTD, saturation of exposure, or a limit dose (but not AUC ratios over the clinical exposure) is used for dose selection. For the TgRasH2 assay, as for all the 6-month transgenic studies, exposure margins are not considered with either dose selection or when interpreting drug-related results.
Results
Of the 36 adequate studies submitted to CDER, 4 had clear positive results: (1) ovarian granulosa cell neoplasms, also seen in the 2-year rat study, with incidences of 32% in the TgRasH2 animals and 44% in the rats; (2) endometrial stromal polyps in TgRasH2 animals with rare mesovarian neoplasms seen in the 2-year rat study; (3) gastroduodenum papillomas and carcinomas with similar large incidences (about 90%) seen in the 2-year rat study; and (4) squamous cell papilloma of the tail. In this last study in which squamous cell papillomas of the tail were observed, an increase in hemangiosarcomas of the mesentery was observed in rats but the hemangiosarcomas were not increased when all organs and tissues were considered together. The gastroduodenum neoplasms in TgRasH2 mice and rats mentioned earlier were seen in both males and females and the lowest effect dose was a low multiple (1–3×) of the human exposure in mice and rats. The 6-month TgRasH2 studies are usually conducted at higher doses than are the 2-year rat studies, because the tolerated dose for 6 months is higher than that for a 2-year study. The doses at which drug-related neoplasms occur at 6 months in more susceptible animals are often different from the doses at which neoplasms occur in a 2-year lifetime study. In general, it is difficult to make any conclusion about the relationship between the exposures at which neoplasms were observed in the TgRasH2 studies and the exposures at which neoplasms were observed in 2-year rat studies.
Seventeen of the 36 studies with negative TgRasH2 results also had negative results in rats. Several drugs still have 2-year studies in rats ongoing, and 4 do not have any 2-year rat studies. Of the 36 adequate studies, (1) one TgRasH2 negative had liver and thyroid follicular-cell neoplasms secondary to liver enzyme induction in rats; (2) one negative had Leydig-cell tumors in male rats, and (3) one negative had increased C-cells in the thyroid but not C-cell neoplasms, as seen in rats; (4) another that was positive in rats, but negative in the TgRasH2 assay was a fusion protein connected to an immunoglobulin G (IgG).
Four of the negatives in the TgRasH2 assay had positive genotoxicity findings: (1) one was positive in the mouse lymphoma assay and for CAs in Chinese hamster lung (CHL) cells, (2) one was positive in the mouse lymphoma assay and for CA in human lymphocytes, (3) one was positive for CA in human lymphocytes and in CHO cells, and (4) one was equivocal for CA in human lymphocytes.
Three of the 4 positives in the TgrasH2 mice were negative in the genotoxicity battery and 1 was positive in CHO cells.
A limitation of the TgRasH2 assay is that it is generally insensitive to effects on hemangiosarcomas or alveolar/bronchiolar pulmonary neoplasms, because of the high variable (up to 20%) background of these neoplasms. As a consequence of the background strains, this model seems relatively insensitive to the mouse-specific liver neoplasms seen in many 2-year studies. Some might consider this insensitivity an advantage because the relevance of these mouse liver neoplasms to humans is often questioned.
Neonatal Mice
Only 2 completed carcinogenicity studies using neonatal mice have been submitted to CDER so far; only 1 in the past 6 years. Neonatal mouse carcinogenicity studies are conducted by oral or intraperitoneal administration of the drug to neonatal mice on days 8 and 15 of age with analysis after 1 year. Three dose groups have been used in this assay. The model is considered appropriate for genotoxic compounds. One study was equivocal for lung neoplasms (2/25 in the high-dose group vs. 0/25 in control) and the other study was negative.
XPA/P53+/−
The use of DNA repair-deficient XPA−/−/P53+/− knockout mice in carcinogenicity evaluations has been uncommon. Only 1 study (negative) was submitted to CDER, and none were submitted in the past 10 years.
APCmin+/− for Colon Polyps
Mice carrying a mutation in the Apc gene (APCmin+/−) have rarely been used for carcinogenicity assessment of drugs in a regulatory setting. One such study, which indicates promotion effects on colon polyps, was submitted and reviewed. There is limited information in the literature for pharmaceuticals in this model. For 1 IND product, promotion results were observed in a feed study in this model, but inhibition of polyps by the same drug was observed in a drinking water study. This model has not been recommended by CDER.
Overall Use of Alternative Assays
The use of carcinogenicity study designs other than 2-year assays has grown considerably over the last several years. The TgRasH2 studies are rapidly replacing the 2-year mouse studies although an acceptable alternative for dermal products is still lacking. Sponsors seeking to use an alternative study should still request concurrence from the appropriate CDER review division that use of an alternative model is appropriate, because not all models are appropriate for all drugs. The CDER Executive Carcinogenicity Assessment Committee concurs as to whether an alternative study is appropriate, reviews proposed protocols, and concurs as to whether a completed study is positive or negative.
Use of alternative carcinogenicity study models has produced a range of impacts in particular drug development programs. In some cases, continued development of the drug has been allowed even when the drug was clearly genotoxic but was also negative in a P53+/− assay. As with results from standard carcinogenicity assays, product labeling describes results of the alternative studies but does not explicitly label a product as carcinogenic. Although systemic exposure in animals relative to maximum human exposure is provided in labeling for 2-year studies, exposure multiples are not provided for results of alternative carcinogenicity studies. This is because the transgenic mice have a greater susceptibility to tumorigenesis and the duration of exposure in the alternative assays is much less than lifetime, whereas human exposure could be for a lifetime. Consequently, the models are suitable for hazard identification but not for direct comparisons of the exposures at which tumors occur in animals to the exposures achieved in humans.
The CDER Executive Carcinogenicity Assessment Committee concurs as to whether a study is positive or negative for drug-related neoplastic findings. However, each human drug review division in the FDA integrates all nonclinical and clinical data into a risk/benefit determination for humans under conditions of use. The carcinogenicity assessment is only 1 component of that assessment. The product indication, patient population, and relevance of findings to humans are important factors in determining whether positive results will be an acceptable risk.
Overall, the alternative assays use less drug and fewer animals, and also save development time, although an alternative carcinogenicity study model for dermal products is still lacking. We anticipate that the use of alternative carcinogenicity studies with pharmaceuticals will continue to grow.
Footnotes
Author Contribution
All authors (PB, AJ) contributed to conception or design; data acquisition, analysis, or interpretation; drafting the manuscript; and critically revised the manuscript. All authors gave final approval, and agreed to be accountable for all aspects of work in ensuring that questions relating to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
*This is an opinion article submitted to the Regulatory Forum and does not constitute an official position of the Society of Toxicologic Pathology or the journal Toxicologic Pathology. The views expressed in this article are those of the authors and do not necessarily represent the policies, positions, or opinions of their respective agencies and organizations. The Regulatory Forum is designed to stimulate broad discussion of topics relevant to regulatory issues in toxicologic pathology. Readers of Toxicologic Pathology are encouraged to send their thoughts on these articles or ideas for new topics to
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The author(s) received no financial support for the research, authorship, and/or publication of this article.
