Abstract

In a seminal study published in 1966, Werner K. Noell and associates reported that the “retina of laboratory rats is affected irreversibly by intense light applied for less than an hour or for up to 2 days depending on the experimental conditions.” (Noell et al. 1966). They found this effect when the retinas of “normal unanesthetized and unrestrained rats were maintained continuously for 24 hours in an environment illuminated by ordinary fluorescent light bulbs.” In an insightful introductory comment, the authors indicated that the “interest in this effect rests mainly on the assumption that any unusual vulnerability of the retina to physical or chemical agents may relate to the cellular abnormalities which lead to retinal degeneration on a hereditary basis.” This ushered in an era of intense investigation of the interactions between light and photoreceptor degeneration that has helped unravel the mechanisms of this effect, identify potential consequences to human patients, and develop therapies that could be translated to the clinic (e.g., studies on neuroprotection from light damage by ciliary neurotrophic factor and its eventual use in human clinical trials; LaVail et al. 1992; Tao et al. 2002; Sieving et al. 2006). From 1966 to August 2012, over 184 papers have been published on retinal light damage in rats. In mice, where the same finding was first reported in 1971 (Aoyagi 1971), there have been >134 publications (search: light damage/retina/rat and light damage/retina/mouse with manual review of the search results to eliminate references that are not pertinent).
Although light and light damage mechanisms have been extensively examined in basic retinal cell biology studies
Based on safety studies reviewed by one of the authors (G.D.A.) in recent years, it appears that retinal degeneration, putatively caused by light, has been a confounding factor in studies using albino rodents, and this appears to have increased in frequency. Differentiation of light induced from test article–related retinal damage has become a costly and effort-intensive undertaking in order to ensure that the observed findings have limited or no potential adverse effects on human patients (Figure 1). Part of this increase could be attributed to new caging methods for laboratory rodents that increase light fluxes within the cage. Instead of the traditional individual cages with solid metal back and sides, and a mesh front, many of the new caging systems are clear plastic. If ambient illumination is not precisely controlled in the animal rooms, the higher light fluxes within the new enclosures enhance cumulative light exposures and favor retinal light damage.
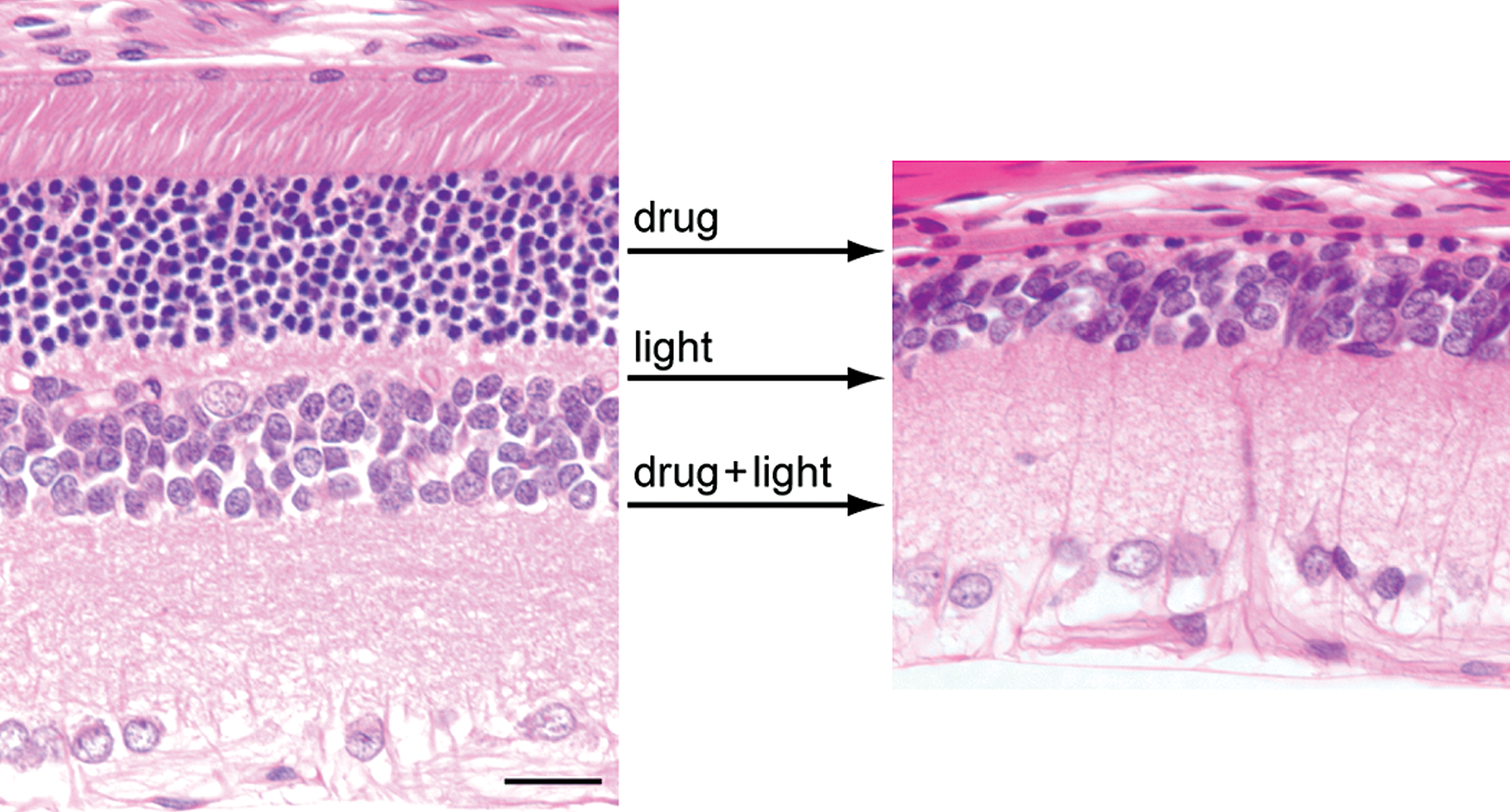
Photomicrograph of normal albino SD retina (left). In the context of safety studies, the change from normal to extensive photoreceptor degeneration (right) can result from the test article, phototoxic retinopathy, or a combination of both. In this example, the damage, regardless of cause, results in nearly complete loss of photoreceptor cells. Calibration bar = 40 µm.
In this review, we discuss concepts and mechanisms of light damage and indicate how these might relate to preclinical safety studies. As well, we provide recommendations for evaluating the retina and developing protocols for evaluating a potential light damage mechanism in studies where retinal degeneration is observed.
Retinal Light Damage: General Principles
The majority of light damage studies have been carried out in albino rodents because of their apparent “exquisite” sensitivity to light damage (O’Steen, Shear, and Anderson 1972; Organisciak et al. 1985; Wenzel et al. 2005; Organisciak and Vaughan 2010). On a quantal absorption basis, however, photoreceptors in albino animals are as sensitive to light damage as those of pigmented animals (Rapp and Williams 1980a; Penn and Williams 1986). Nonetheless, the pigment in the uveal tract (iris, ciliary body, choroid) and retinal pigment epithelium (RPE) of nonalbino animals serves as a protective screen that limits light fluxes in the retina and “prevents” light damage. This protection, however, can be abrogated in pigmented animals by pupillary dilatation (Williams, Howard, and Williams 1985).
Although the rat has been used for most biochemical studies of light-induced retinal degeneration, it is the albino mouse that has been used to define the molecular mechanisms and pathways involved in light damage (Wenzel et al. 2005). In general, damage is mediated by rhodopsin and is prevented by absence of vitamin A chromophore (Grimm et al. 2000). Based on studies in mice, there is a requirement for repetitive photon absorption to cause damage (Wenzel et al. 2005), and this is facilitated by having a more active form of the RPE65 gene, involved in the RPE retinoid cycle, to produce a faster turnover and greater availability of vitamin A (11-cis retinaldehyde) to the photoreceptors (Wenzel et al. 2001).
In addition to the abovedescribed modifying effect of pigmentation and RPE65 gene product activity, there are other parameters that can influence the damaging effect of light on the retina (Wenzel et al. 2005) such as:
Quality of light. It is assumed that fluorescent white light is more damaging as it has a spectrum similar to daylight. Broadband green and more narrow-spectrum blue and green lights also cause damage and are used to more precisely examine the damaging effects of light and the wavelength specificity.
Exposure duration and intensity. There is an interplay between duration, wavelength, and light intensity that affects the outcome; as well, the outcome depends on whether the study is carried out in mice or rats. Additionally, cyclic illumination, for example, 12-hr on/12-hr off, is less damaging to the retina than constant illumination, but that too is intensity dependent.
Age of the animal and temperature. Juvenile rats are more resistant to light damage than adults (Joly et al. 2006). Induced hyperthermia during light exposure accelerates damage (Organisciak et al. 1995). However, the timing of the increased body temperature is critical as transient hyperthermia prior to light exposure reduces the damaging effects of light by increasing production of heat shock proteins (Barbe et al. 1988).
Gender. Based on comparisons between ovariectomized and intact female rats in terms of light damage susceptibility, it appears that ovariectomy protects against light damage, and estrogen supplementation overcomes the protective effect of ovariectomy, suggesting that intact female rats are more sensitive to the damaging effects of light (Olafson and O’Steen 1976; O’Steen 1977). Furthermore, the pituitary through direct prolactin effects on the retina also modulates light damage, and hypophysectomized animals show protection from light damage which is abrogated by prolactin administration (O’Steen 1980). However, with few exceptions, direct male to female comparisons in terms of light damage sensitivity have not been published.
Topography of Retinal Light Damage
Prior studies have demonstrated that retinal light damage in albino rodents does not occur uniformly across the retina, at least in the early stages, but has a very specific topographic distribution. The superior retinal quadrants particularly above and near the optic disk are preferentially damaged, while the inferior and peripheral regions are spared (Organisciak et al. 1999; Figure 2). The distribution of damage across the retina can be quantified by making maps of outer nuclear layer (ONL) thickness at different retinal positions; these are commonly referred to as “spidergraphs” (Rapp 1985; Figure 3A). The increased susceptibility to retinal light damage by the central retina has been proposed to result from increased rod outer segment (ROS) lengths (Figure 3B) accompanied by increased rhodopsin packing density in the central photoreceptors (Rapp et al. 1985). Recent work now shows that it is the superior temporal region that shows the greatest sensitivity to light damage, and topographic maps of ONL thickness clearly demonstrate these findings (Tanito et al. 2008; Figure 3C and 3D).
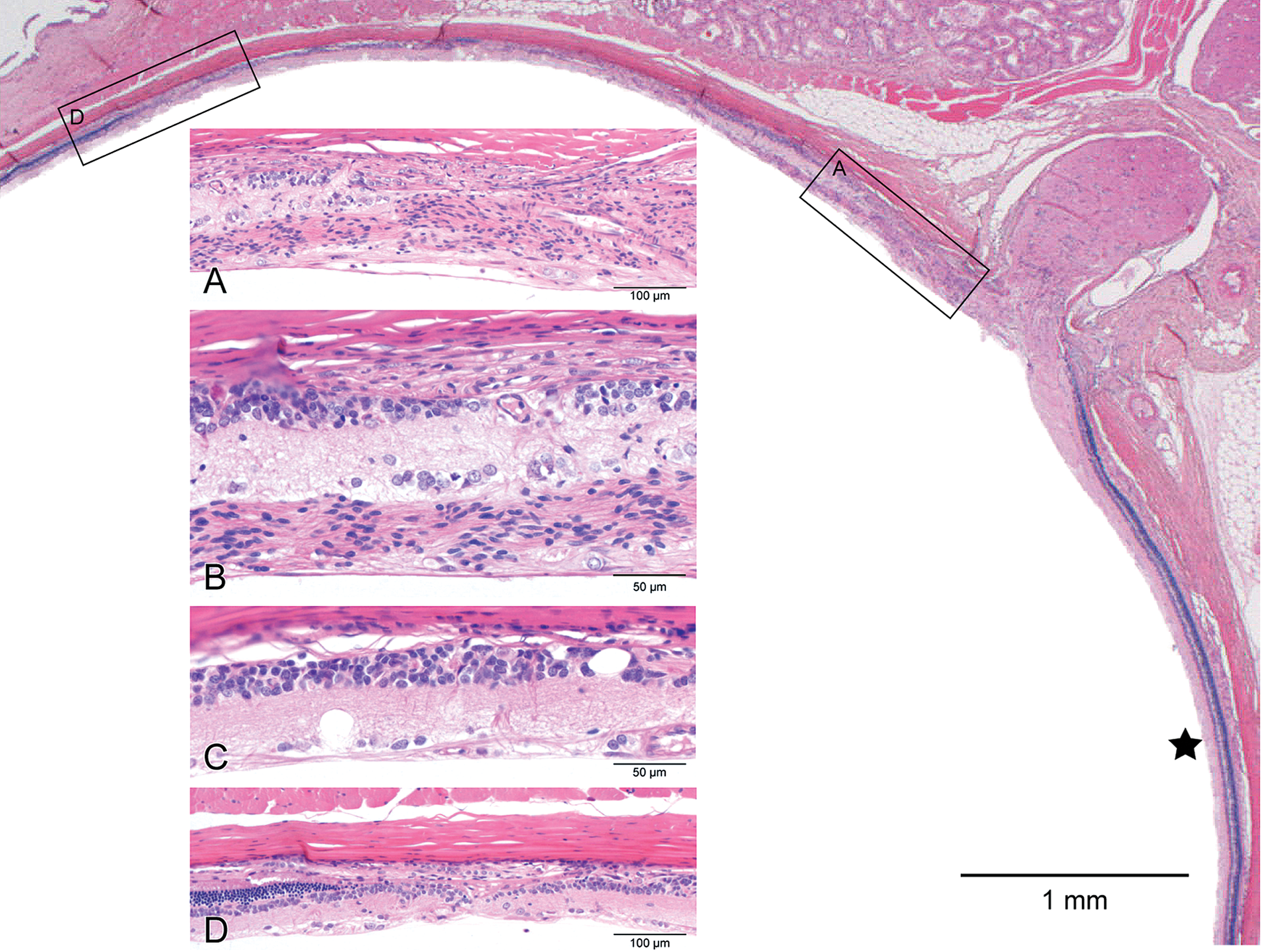
Light-induced retinal degeneration in an albino rat from a 2-year carcinogenicity study. There is a distinct difference in thickness of the retina on either side of the optic disk. The ↔ marks the relatively normal inferior retina. Approximately 50% of the superior retina is markedly reduced in thickness and shows different degrees of retinal atrophy. These begin adjacent to the disk (boxed area-A, Figure A) and extend to the midperiphery (boxed area-D, Figure D); intervening regions are illustrated in B and C. A. The retina nearest the optic disk shows full-thickness loss of retinal layer organization and fibrous connective tissue in the vitreal aspect of degenerating retina. B. The same tissue overlays the ganglion cell layer; the inner nuclear layer is moderately reduced and abuts the choroid and sclera. The outer retinal layers and retinal pigment eipthelium are absent. C. Microcystoid vacuoles are present within remnant inner retinal layers. D. There is an abrupt transition into less affected retina with preservation of retinal pigment epithelium, outer nuclear, and photoreceptor layers. H&E.
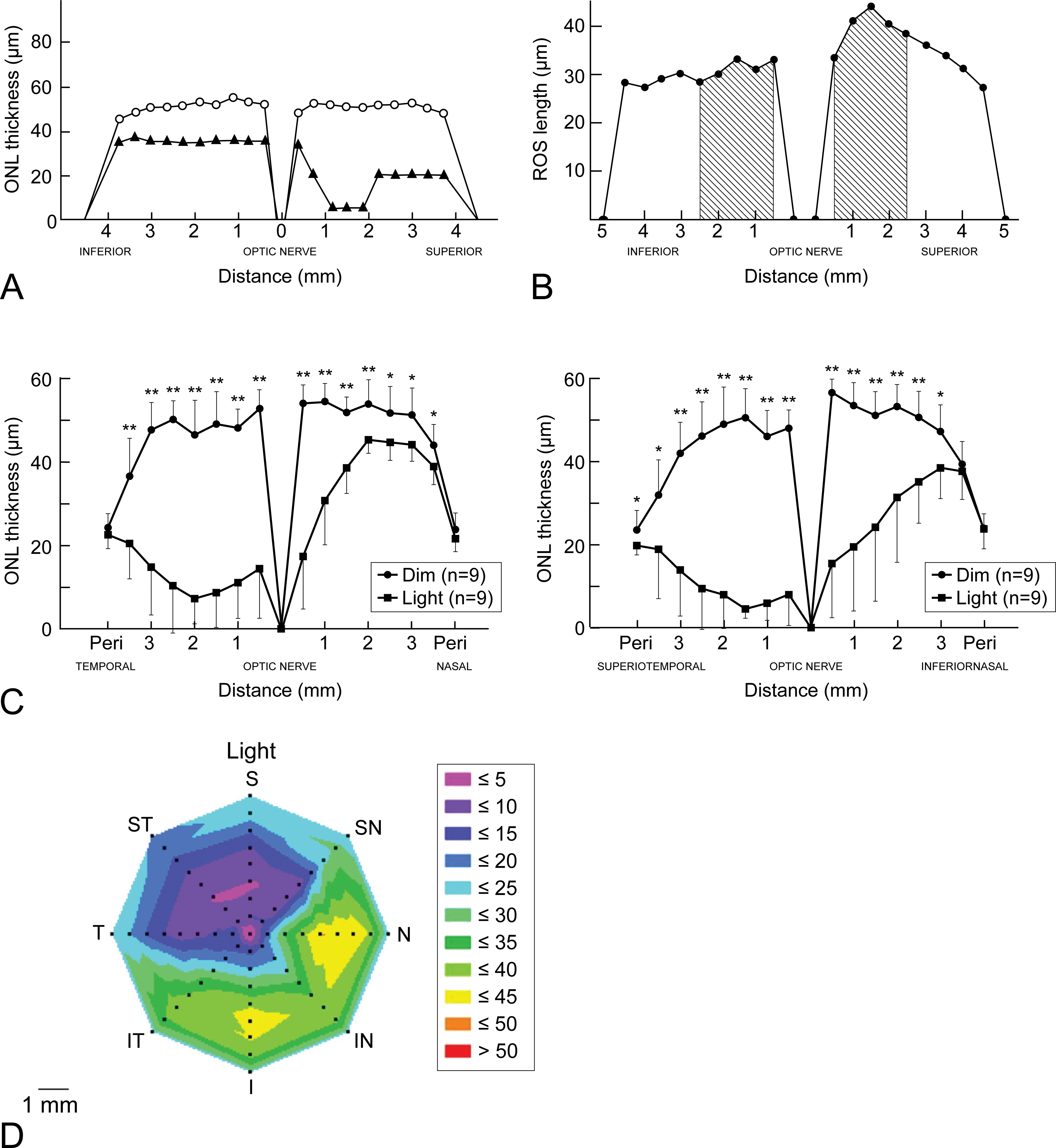
Topography of retinal light damage. A. Spidergraphs illustrating the exquisite sensitivity of the superior retina to light damage in an albino SD rat (black triangles) exposed to 4 days of continuous illumination at 40 lux compared to a cyclic light control (open circles). Loss of photoreceptor cells results in thinning of the outer nuclear layer (ONL) that is most severe above the optic nerve head. (Figure modified and reprinted with permission from Figure 2 of Rapp 1980b). B. Schematic representation of rod outer segment (ROS) length at different locations in the superior and inferior quadrants of the rat retina. ROS are longer at the site where the retina is most susceptible to light damage. (Figure modified and reprinted with permission from Figure 2 of Rapp et al. 1985). C. Intense short-term light exposure (Light, 5,000 lux for 6 hr) also results in a topographically distributed retinal lesion in comparison to dim light control (5 lux cyclic light). When the damage is evaluated across different retinal regions, the superiotemporal and temporal quadrants are most sensitive. D. The damage is best illustrated in color-coded maps of ONL thickness which illustrate that the ONL thickness has decreased to <15 µm; scale in right correlates color with ONL thickness in µm. (Reprinted with permission [C = Figure 2A; D = Figure 3B] from Tanito et al. 2008).
Differences in Light Damage Susceptibility in Albino Rats
In mice, light damage susceptibility is strain dependent (LaVail, Gorrin, and Repaci 1987; LaVail et al. 1987a), and recent studies have shown several genetic loci that determine this susceptibility (Danciger et al. 2004), of which the RPE65 locus appears to confer the most resistance (Wenzel et al. 2001). In rats, a light damage study by Borges et al. has shown that Wistar and Fischer (F344) strains are equally sensitive, but more resistant than Buffalo and Lewis strains (Borges, Edward, and Tso 1990). In addition, 2 other studies have compared albino rat strains, and these showed Sprague-Dawley (SD) rats to be more resistant than Wag/Rij (O’Steen and Donnelly 1982), and that Fischer (F344) rats are more resistant than Wag/Rij (LaVail et al. 1987b).
It is important to note that these evaluations, and most experimental light damage studies, use “acute” exposures with high-light intensities that last a few hours, or are constant for several days. These light intensities are far higher than routinely used in animal rooms during preclinical safety assessment, thus a direct comparison is not possible.
Age- and Light-dependent Retinal Changes in Albino Rats
A study by Weisse, Stotzer, and Seitz (1974) and associates examined age- and light-dependent retinal changes in albino Wistar rats. Age-related changes showed that females were preferentially affected. Light-related changes were similar in both sexes, with light intensity showing a significant relationship to the incidence of retinal damage. A more recent study using only male SD rats also found that older rats reared in dim cyclic light were more susceptible to light damage than young animals, while dark reared animals were equally susceptible at all ages (Organisciak et al. 1998).
Eye Pigmentation Protects from Light Damage
Constant light at a level that destroys almost all photoreceptors in albino rats and mice in 1 week has no effect on pigmented rat or mouse eyes exposed to light for almost a year. However, if the pupils are dilated in pigmented rat eyes, degeneration occurs. The protective effect of pigment is due to both RPE pigmentation and screening by melanin in the anterior and posterior uvea that limits light fluxes in the retina (Rapp 1980a; LaVail and Gorrin 1987; Sanyal and Zeilmaker 1988; Weisse 1995; Wasowicz et al. 2002).
RPE65 Gene and Differences Between Rats and Mice in Light Damage Susceptibility
Albino rats have been used most often to define the biochemical pathways involved in light damage because the experimental light damage paradigms result in more consistent outcomes that are subject to less variation than comparable studies in albino mice (Bicknell et al. 2002; Ablonczy et al. 2005; Tanito et al. 2005; Duncan et al. 2006). In contrast, the albino mouse has been the preferred species to dissect the molecular mechanisms and genetic determinants of light damage (Wenzel et al. 2005), and these studies have provided details on strain differences in light damage susceptibility in mice.
LaVail et al. (1987a) examined the sensitivity to light-induced photoreceptor degeneration in 7 different inbred albino mouse strains and compared the findings to the BALB/cByJ (BALB/c) albino mice (sensitive to light damage) and to C57BL/6J-c2J albino mice (resistant to light damage). Mice of the A/J, AKR/J, and NZW/LacJ strains were indistinguishable from BALB/c mice in light damage sensitivity. Mice of the Ma/MyJ and RF/J strains were somewhat more sensitive to light than BALB/c mice, and those of the RIIIs/J were far more sensitive than all of the other strains (LaVail, Gorrin, and Repaci 1987).
Subsequent quantitative genetic studies in the C57BL/6J-c2J albino mice mapped the locus for resistance to light damage to a genomic region that included the RPE65 gene, and this accounted for ∼50% of the protective effect. At this locus, a leucine 450 methionine (Leu450Met) amino acid substitution was found to cosegregate with the increased resistance to light damage (Danciger et al. 2000). This change has been examined in the 6J-c2J and other mouse strains and found to determine light damage resistance (Wenzel et al. 2001). Light sensitive strains, for example, BALB/c, B6CF1, and 129/Ola, have leucine at codon 450 and produce normal amounts of RPE65 protein. In contrast, the RPE65 450 methionine substitution found in light damage resistant strains, for example, 6J-c2J and B6;129S(N)2, shows markedly decreased amounts of RPE65 protein, and consequently lower amounts of rhodopsin following bleaching (less 11-cis retinaldehyde is produced).
In a safety context, there is little information about the light damage susceptibility of CD-1 outbred mice, or their status at the Leu450Met locus. As this is the most widely used mouse strain in chronic and carcinogenicity studies, the information is critical in order to separate adverse retinal changes secondary to the test article from light-/age-related findings; however, this information is not readily available.
To this end, we have sequenced the relevant portion of the RPE65 gene in outbred CD-1 mice surrounding the M/L 450 single nucleotide polymorphism (SNP) using gene-specific primers and genomic DNA from 6 CD-1 outbred male mice (Charles River Laboratories, Germany) as template (Figure 4; Dr, U. Certa, F. Hoffmann-La-Roche Ltd., Basel, Switzerland). A unique PCR product of 250 base pairs was obtained from all 6 animals which had the predicted size and is about 80 bases longer than the product obtained with cDNA because it includes intronic sequences (Figure 4A; Wenzel et al. 2001). Following AluI digestion of the genomic fragment the expected products appeared (Figure 4A). Sequence analysis showed that all animals carried the Leucine450 RPE65 allele, indicating that these mice do not have the protective polymorphism at this locus (Figure 4B).
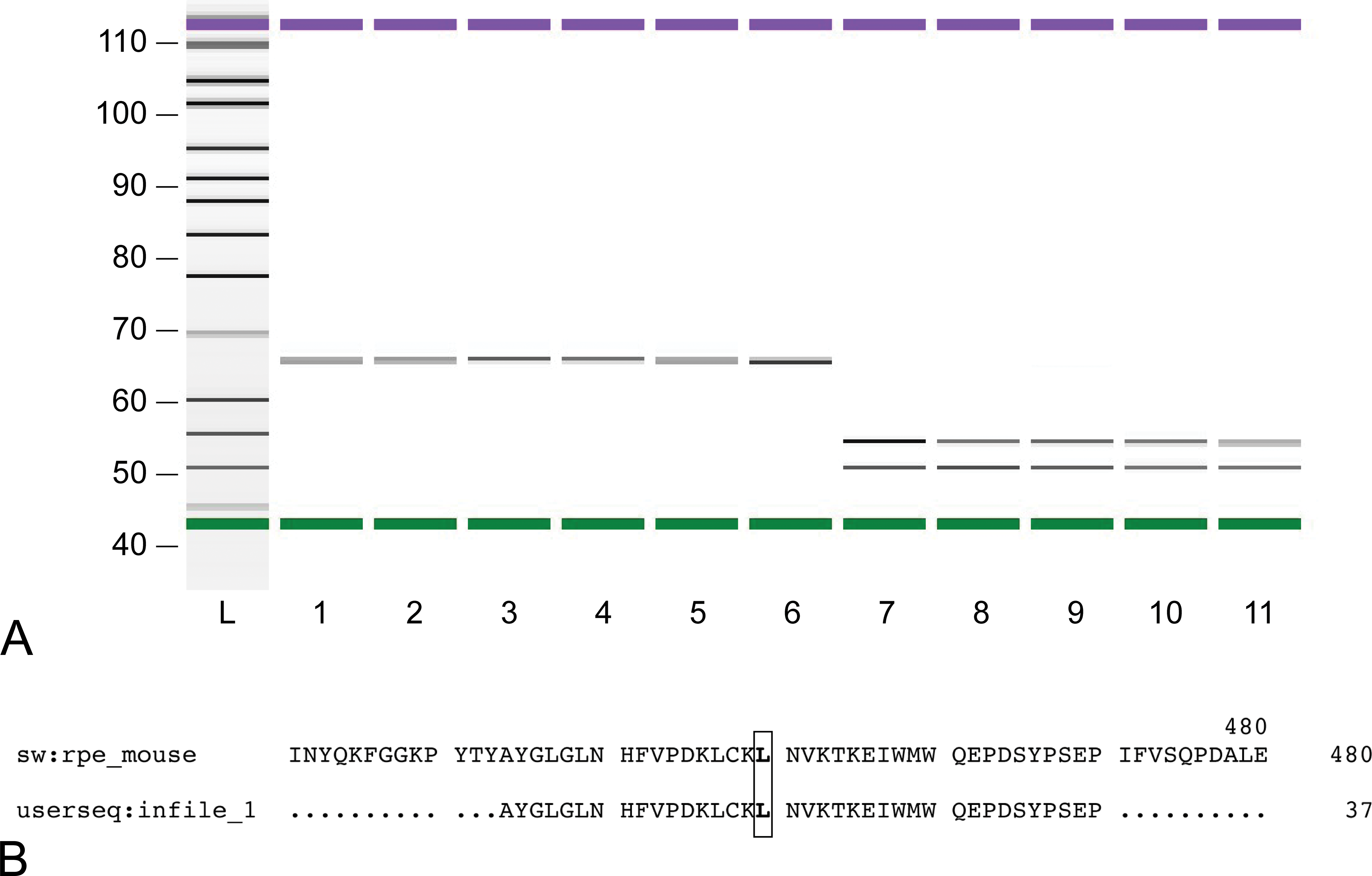
RPE65 genotype of CD-1 outbred mice. A. The amplicons generated by Rpe65 gene-specific primers (Rpe65_forward: CTGACAAGCTCTGTAAG; Rpe65_reverse: CATTACCATCATCTTCTTCCA) from genomic DNA are displayed by agarose electrophoresis for 6 CD-1 outbred male mice. The primers generated a single 250 bp band in all 6 mice (lanes 1–6 below) which is larger than that reported for cDNA in the literature because the amplicon included intronic sequences (Wenzel et al. 2001). Sequencing indicated that the 80 bp intronic sequence was present just before the AluI site (lanes 7–11). B. Sequence alignment of the relevant RPE65 coding region (Boulanger et al. 2001) from all 6 CD-1 outbred mice indicated Leucine at codon 450 (L, boxed region) indicating that they do not have the protective polymorphism at this locus.
The genetic contribution to light damage susceptibility is still far from completely defined. As noted above, the RPE65 locus only contributes ∼50% of the heritable component to this trait (Danciger et al. 2000). Even in mice that have the same RPE65 protective genotype and are light damage “resistant,” there are differences still in light damage susceptibility, and it takes 10-fold more photons to induce light damage in 6J-c2J than in B6;129S(N)2 (Wenzel et al. 2001). Furthermore, additional quantitative trait loci have been found that modify the light sensitive leucine450 variant of RPE65 (Danciger et al. 2004).
In contrast to mice, changes in RPE65 gene sequences have been excluded as modifiers of the light damage phenotype in rats (Iseli et al. 2002). Thus, this major modifier locus can be excluded when considering light damage susceptibility or resistance in different rat strains, and at present, pigmentation appears to be the main (Rapp 1980), but not the only light damage modifier.
Retinal Structure and Light Damage
Standard procedures for histopathological assessment of retinal findings in rodents typically involve evaluation of a cross section of each eye, pupil-lens-optic nerve, and, in general, the section plane is not considered. When retinal light damage is a concern, however, the lack of topographic information can be problematic in determining compound versus light damage findings.
Another issue that complicates assessment is that the threshold used to establish severity often favors overlooking significant abnormalities. Although grading scales may vary by pathologists, it is generally accepted to use a scale ranging from normal → minimal → slight → moderate → marked → severe (Figure 5). The less severe categories, that is, normal through slight, generally assess the entire retina and give considerable more weight to inner retinal preservation and absence of retinal layer disorganization or rosette formation. These lesions tend to be localized rather than diffuse, while the more advanced stages tend to be more widely distributed. Thus, in one author’s experience (G.D.A.), so-called normal retinas can have a 20 to 25% decrease in the ONL thickness (number of vertical rows of photoreceptor nuclei), a significant loss, indeed, of photoreceptor cells. Minimal and slight grades can represent decreases of 65 to 90%, respectively. In general, such grading system appears to be common, if not the industry standard, although we are not aware of publications that formally set out this classification.
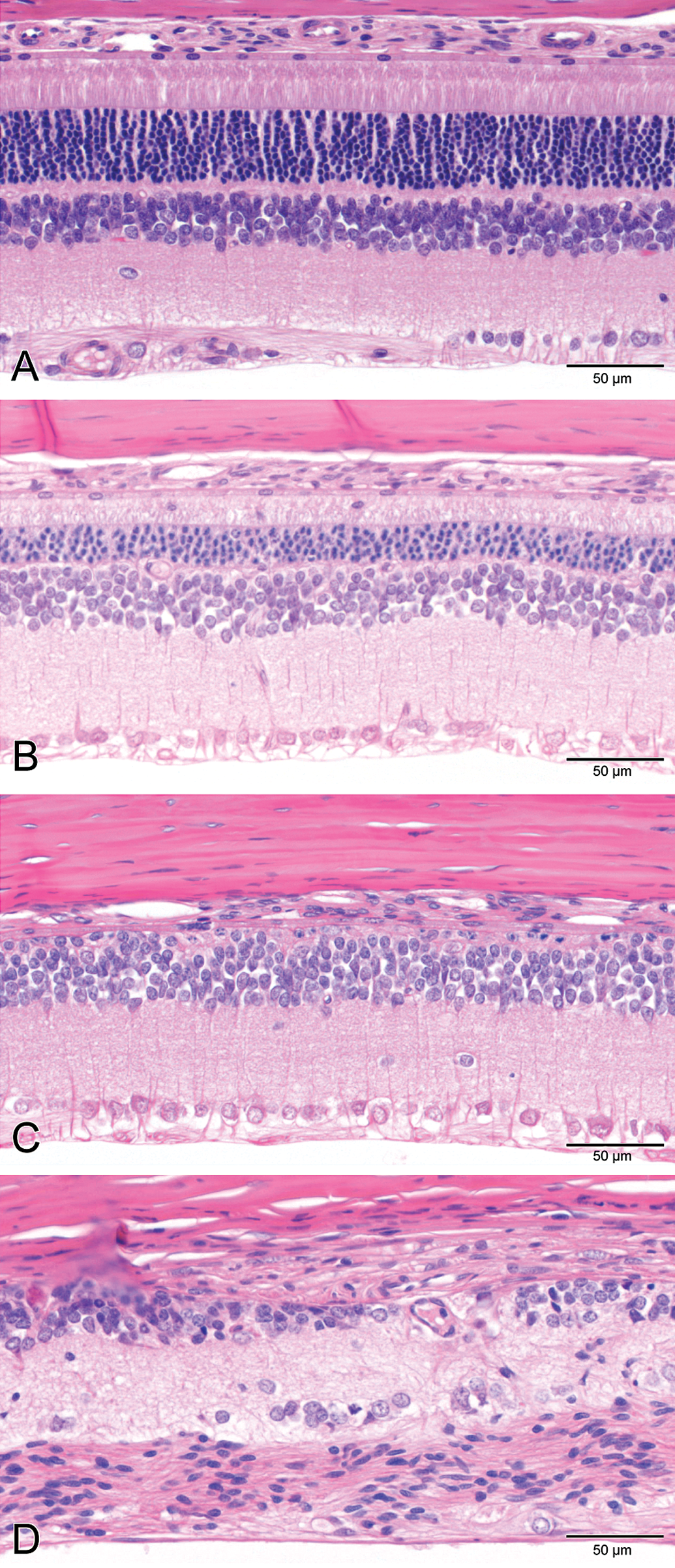
Example of a generally accepted grading scale (normal → minimal → slight → moderate → severe) to evaluate retinal atrophy in rat toxicity studies. A. Normal retina: the different retinal layers are distinct, photoreceptor inner and outer segments are elongated, outer nuclear layer is intact. B. Slight retinal atrophy: different layers remain distinct, but the outer nuclear layer is reduced in thickness, and macrophages are present in the photoreceptor layer. C. Moderate retinal atrophy: the retinal pigment epithelium, photoreceptors and most of the outer nuclear layer are lost; the outer plexiform layer is not present. The inner nuclear layer remains relatively intact albeit irregular. D. Severe retinal atrophy: There is marked disruption of the normal retinal architecture with loss of retinal layer organization. Remnants of inner nuclear and ganglion cells remain. H&E.
Given that long-term safety studies, 13 weeks or longer, have an “acceptable” level of outer retinal pathology that can be considered a “normal” aging change, evaluation of photoreceptor damage can be underestimated. This is illustrated in Figures 6 through 8 which illustrate retinal findings from typical 2-year carcinogenicity albino rat and mouse studies. Not only are the characteristic peripheral retinal changes present, but, in addition, the images clearly show that the ONL is thinned to focally absent with loss of photoreceptors, and the inner nuclear layer (INL) becomes attenuated. When such extensive retinal damage occurs in all treatment groups, it is not possible to assess whether the test article causes any incremental retinal damage.
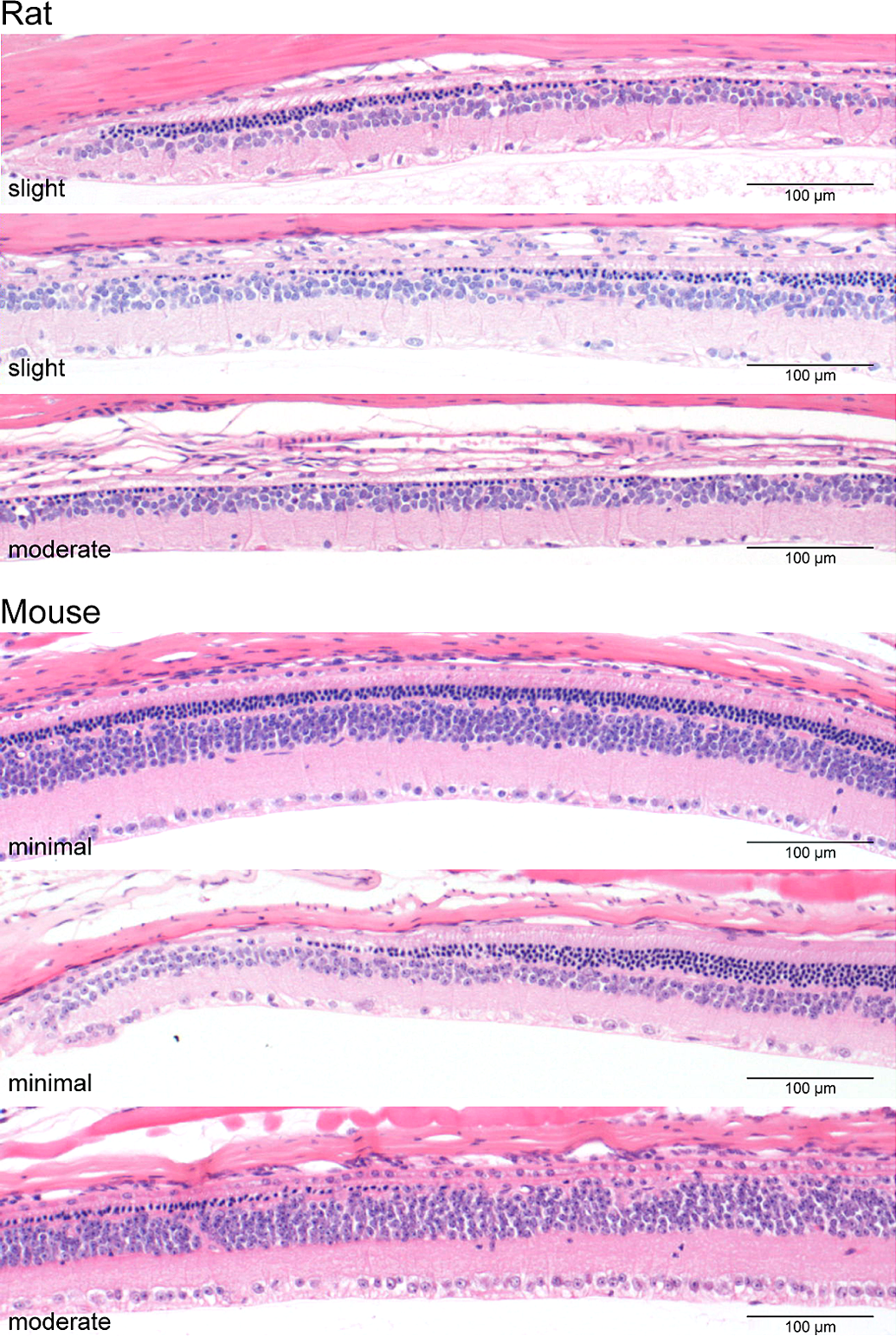
Examples of retinal atrophy findings in rat and mouse carcinogenicity studies illustrating the grading classification currently used. Peripheral retinal atrophy in control SD rats and CD-1 mice in 2-year carcinogenicity studies. H&E.
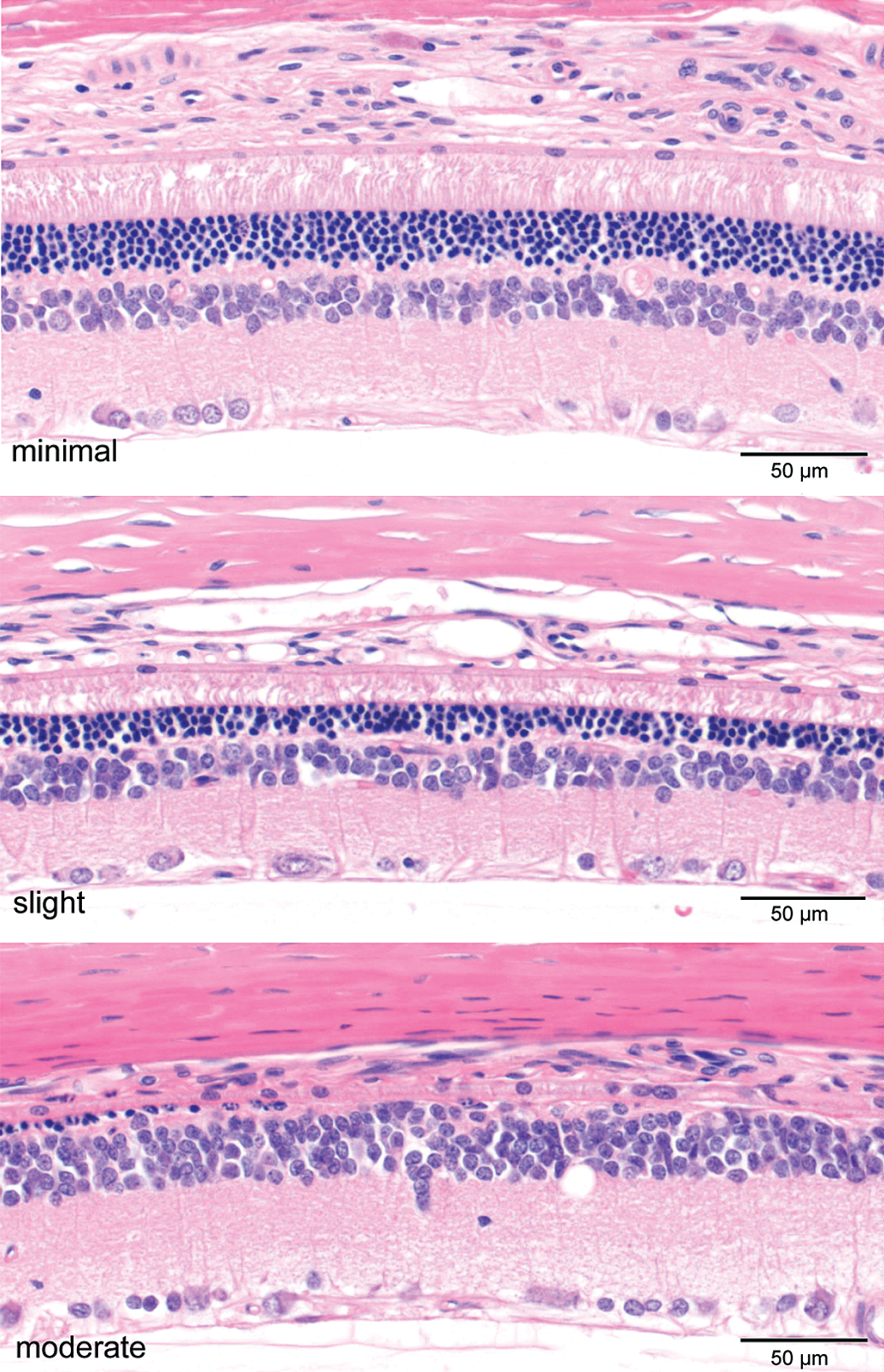
Examples of retinal atrophy findings in control Wistar rats in 2-year carcinogenicity studies. There is atrophy in the central and midpheripheral regions the retina. There is minimal to severe thinning of the outer nuclear layer, loss of photoreceptors, and occasional microcystoid vacuoles in the inner nuclear layer. Note that slight and minimal gradings still represent significant photoreceptor pathology. H&E.
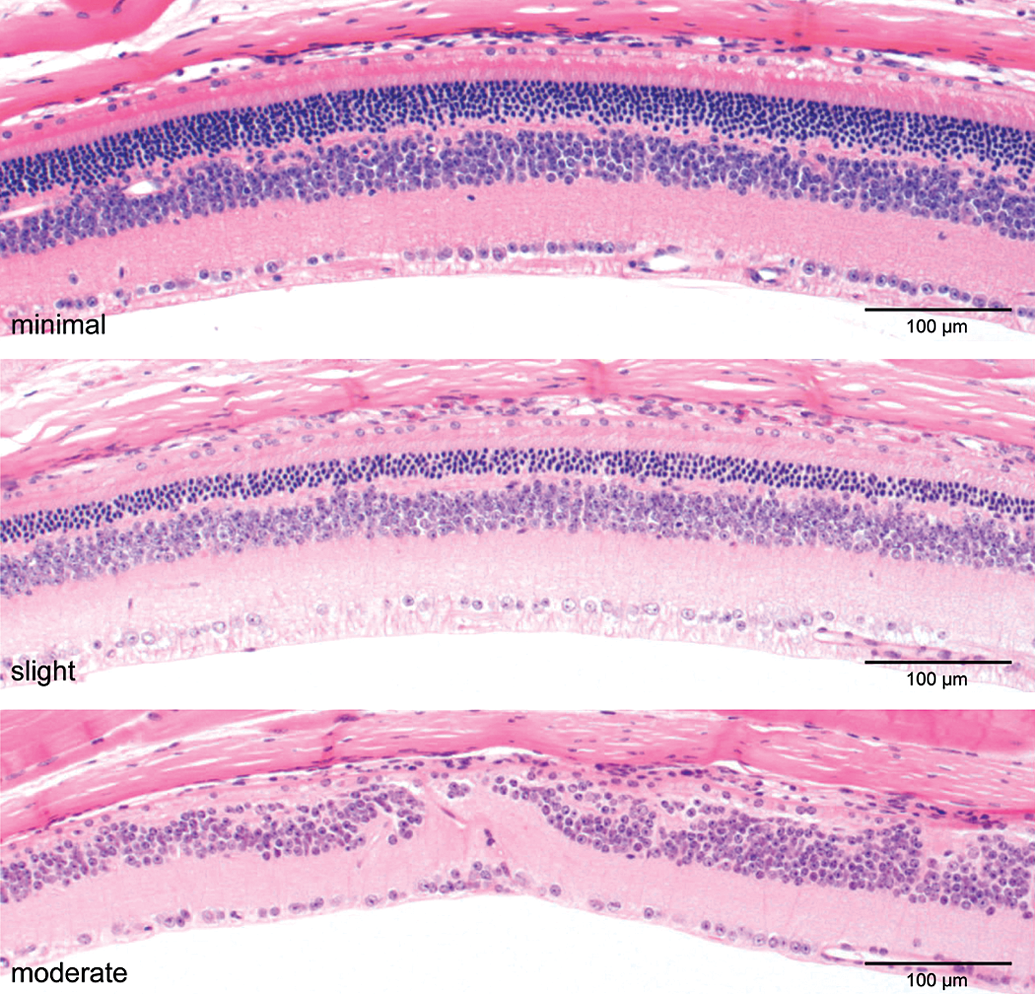
Examples of retinal atrophy findings in CD-1 mice in 2-year carcinogenicity studies. There is minimal to severe thinning of the outer nuclear layer, and loss of photoreceptors and outer nuclear layer. The inner nuclear layer is often attenuated and disorganized when outer retinal changes are extensive. H&E.
Light and Animal Housing Environment
There is an interplay between light in the animal housing environment, and the likelihood of retinal phototoxicity. Several factors come into play among which are the actual room illumination, reflective properties of the floor and walls, position of the cage in the rack, type of caging used, and, most importantly, the animal’s sensitivity to light damage (e.g., albino vs. pigmented, RPE65 Leu450Met, etc.). Older metal cages, some of which had water bottles on the front of the cage and food pellets on the top and front of the cage lid, provided sufficient shielding to minimize the illumination inside the cage. In contrast, modern cages generally are clear, and constructed of products such as plastic polycarbonate Makrolon with a stainless steel wire lid that permits greater light fluxes within the cage. As well, individually ventilated cages (IVC) have been reported to reduce cage illumination in comparison to open cages (Kemppinen et al. 2008); however, as differences in the construction material and design can vary by manufacturer, that is, polysulfone, polycarbonate, polyetherimide, this variation can affect the illumination inside the cages (M. Hargaden, Roche, Nutley, NJ, personal communication,October 18, 2012). Thus, recommending an animal room light level that is safe in terms of avoiding retinal phototoxicity is difficult and is greatly influenced by multiple factors. For these reasons, the appropriate determinant is not so much the actual room illumination, but the light levels inside the cage (see below).
Bellhorn’s 1980 study in albino rats indicated light levels of 323 lux measured at 0.91 m above the floor in the center of the room did not cause clinical signs of phototoxic retinopathy (Bellhorn 1980). Presumably, this study was used to generate the 1996 and 2010 NRC recommendations that follow closely on these values (325 lux at ∼1 m above the floor surface (NRC 2010). This illumination appears sufficient for animal care needs and study procedures, and presumably is below the light damage threshold. In this handbook, other items specific to lighting and animal care for rodents are also discussed (NRC 2010).
The light fluxes occurring in standard rodent rooms/caging indicate that light intensity is variable, and depends on cage position in the rack, being lowest in the bottom rows, and higher close to the light fixtures (Rao 1991). As well, light intensity at the sides of the rack and front of the cage also vary. Table 1 illustrates the differences in illumination measured when using standard plastic polycarbonate Makrolon cages, and overhead shaded fluorescent bulbs as illustrated in Figure 9. Table 1 demonstrates that light measurements depend on placement and orientation of the light meter in relation to the light source. Such variability can underestimate the light intensity to which rodents are exposed and lead to inconsistent retinal findings in safety studies.

Example of a typical rack holding 6 levels of 3 cages per level. Two rats are kept in each plastic polycarbonate Makrolon cage with a stainless steel wire lid. A stainless steel plate covers the uppermost shelf. Shaded fluorescent bulbs provide the light source.
Light levels (in lux) within or in front of polycarbonate cages at various locations in a typical rack used in toxicity studies (see Figure 9).
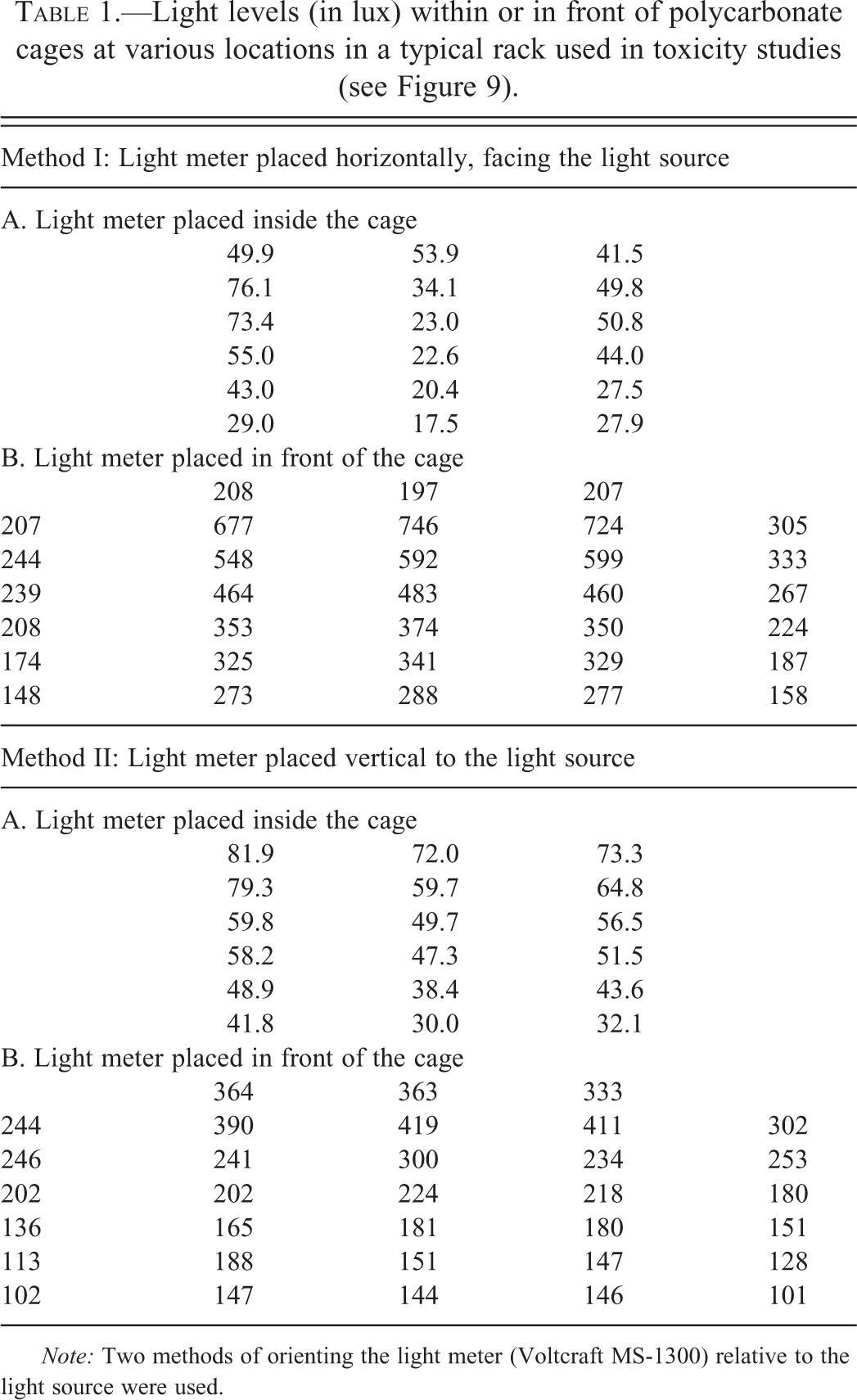
Note: Two methods of orienting the light meter (Voltcraft MS-1300) relative to the light source were used.
The light levels recommended by the NRC still may be too high for long-term studies in albino rodents, especially rats and mice that do not have the protective RPE65 SNP. In addition to maintaining rodent rooms in a cyclic light environment (12-hr dark:12-hr light), many research investigators that work on retinal light damage and neuroprotection recommend dim to very dim light levels during the light part of the cycle. To avoid confounding effects, they use light levels of 5 lux (Li, Cao, and Anderson 2003) to 20 lux to 30 lux (Organisciak et al. 1995, 1998). For SD rat strains, room light levels of no higher than 15 lux to 20 lux are recommended (R. E. Anderson, personal communication, September 6, 2006). While the NRC guidelines are important in minimizing retinal phototoxicity, it is critical to also be aware that light levels recommended will be influenced greatly by factors noted above, that is, cage type, reflectivity of floor, walls and ceiling, cage position, and so on. The illumination level that is most important, however, is the actual in cage illumination, and this should be measured, recorded, and, if possible, kept in the 20-lux range or lower. Thus, the discrepancy in the recommended light levels between those used in industry and in major retinal research laboratories highlights some of the potential confounding problems that can arise in safety studies.
Incidence of Retinal Phototoxicity—A Selected Industry Survey
In our experience, the incidence of retinal degeneration encountered in control albino rodents in safety studies has increased in recent years, and this degeneration often confounds interpretation of test article–related effects. To address this issue, we have conducted a survey of Contract Research Organizations (CROs) located in North America, Europe, and Asia using a survey questionnaire (Supplementary Table 1) that requested information on housing, illumination conditions, and incidences of retinal atrophy in control animals. Information was obtained for different strains of mice and rats commonly used in toxicology testing (6-month and carcinogenicity studies). Responses to the questionnaire were provided by 9 of the 10 CROs contacted, and meaningful data obtained from 8: North America (2), Western Europe (2), and Japan (4). Details of the survey are provided in Supplementary Tables 2 (mouse) and 3 (rats), and the results are summarized below.
General Observations
Strains and Housing Conditions
There is a great variation in caging, illumination levels, and housing condition between different CROs. Mouse strains used are CD-1 and B6C3F1, and, infrequently, C57BL/6 or NMRI. B6C3F1 and C57BL/6 are pigmented strains. Rat albino strains used are mainly Wistar, SD, and, to a lesser extent, Fischer. In principle the same cage type (material) is used for either rats or mice in 6-month chronic toxicity as well as in carcinogenicity studies within the individual CROs. Half of CROs are using clear polycarbonate (Makrolon) or polysulfone plastic cages with metal wire mesh covers, the other half use wire mesh cages with a metal cover. In all cases, a metal plate is used to cover the top of the racks reducing the illumination level for animals in the upper tier. All cages are suspended in movable racks. Rotation of racks and/or cages varies by CRO. Of the 8 CROs, only 3 rotate the cage racks on a monthly basis in the 6-month rodent studies. In the 2-year carcinogenicity studies, 5 of the 8 CROs rotate racks either monthly (3), every 2nd (1), or 6 weeks (1), respectively. In general, rotating cages versus racks may be preferred, but cage rotation is usually not done as this is more work and logistically more complex. Finally, in 3 CROs rotation is not performed for any studies using rats and mice. Animals are housed individually or in pairs (mostly rats) or in groups up to 5 animals per cage (mostly mice). Some CROs arrange housing conditions according to Sponsor’s request.
Illumination Conditions
All CROs use a similar 12-hr light to dark cycle (on: 5–7 a.m.; off: 5–7 p.m.). The range of illumination intensity varies between 150 lux and 650 lux (mean range of 210–490 lux) at a height range of 0.80 m to 1.5 m above floor. In one CRO intensity was measured at 2 m and in another CRO directly underneath the ceiling lamp although illumination values were not provided. With one exception, no information was provided on the instruments or methods used, an indication that direct comparisons between CROs are not possible. At face value, some of these light levels appear to be slightly above those of the Guide for the Care and Use of Laboratory Animals (NRC 1996, 2010).
Historical Control Data on Retinal Atrophy (Histopathology)
A higher incidence of retinal atrophy was seen in 2-year versus 6-month studies; these findings are considered light related, although an age effect cannot be excluded. The net contribution of age versus light on retinal atrophy in the 2-year studies cannot be quantified as CROs generally do not differentiate between focal (i.e., light induced in early stages) and diffuse retinal atrophy (mainly age-related although diffuse atrophy occurs in end-stage retinal light damage; Weisse, Stotzer, and Seitz 1974). These results are summarized in Supplemental Tables 2 and 3. For 2-year studies in mice, the percentage incidence (male/female) of retinal atrophy ranged from 0/0 to 56/65 in CD-1 albino mice to 0/0 to 0/1 in the B6C3F1-pigmented strain. In 2-year studies in rats, the percentage incidence (male/female) of retinal atrophy ranged from 5/5 to 24/51 in the Wistar strain to 0/3 to 21/38 in SD. In comparison, 6-month studies showed a lower incidence (Wistar: 0/0–2/4; SD: 0/0–6/9). Limited data from albino NMRI mice with a low incidence of retinal atrophy as well point to strain differences as another contributor. The status of this strain in regard to RPE65 Leu450Met is unknown. The Fischer strain was used infrequently, and only for carcinogenicity studies. Based on one study, one CRO did not report retinal atrophy while another CRO indicated incidences of retinal atrophy around 70%, and comparable between males and females in 16 studies. A possible difference in gender susceptibility to retinal atrophy was observed in studies with rats. In the majority of the studies, females tended to have a higher incidence of retinal atrophy than males.
How to Address Retinal Phototoxicity Issues in a Safety Study?
It is important to establish a priori an algorithm to differentiate test article–associated retinal damage from retinal phototoxicity or to identify the possible interaction between the drug and light that results in retinal atrophy (Figure 1). While the first two possibilities are straightforward, even though the mechanism of compound-associated retinal degeneration may be difficult to precisely define, the third possibility, that is, interaction between the drug and light, can create obstacles in the path to drug development. Drugs or their metabolites can have a direct effect on photoreceptors that are light exposed (Izumi et al. 2004), or alternatively, an indirect effect where the compound causes a change resulting in increased light damage susceptibility. For example, drugs that cause pupillary dilatation such a clonidine (Weisse et al. 1971) result in higher incidence of retinal phototoxicity. As well, drugs that cause behavioral changes such as increased locomotion or position the animal closer to the front or sides of the cage have been found to cause a higher incidence of retinal light damage (Aguirre, unpublished). These possibilities can be assessed, respectively, by either pupillometry (Aleman et al. 2004) or spontaneous activity measurements (Masuo et al. 1997).
Mechanistic studies to specifically address light damage as a direct cause of retinal atrophy would take one of the several forms. These would include studies with pigmented and albino animals receiving the test article and maintained under standard housing conditions. As the pigmented retina is more resistant to light damage, presence of retinal degeneration in albino but not pigmented animals would be interpreted as evidence in support of phototoxicity. As well, studies in which the albino animals would be maintained under dim cyclic light illumination, for example, ∼20 lux at the front of the cage without retinal damage would further support phototoxicity versus a direct compound effect on photoreceptors. In both cases, it is important to ascertain that the length of the studies are comparable to the one where the initial finding was made as duration of light exposure is a critical component. Although having a low light intensity arm to such studies is of importance, we do not recommend that a high light intensity cohort be used. As more light results in more retinal degeneration, such a group would provide no additional mechanistic information.
A critical component of any study that aims to investigate a light damage mechanism is the morphologic assessment of the topography of retinal damage. In general, direct retinal damage by compounds tends to cause diffuse rather than more locally extensive outer retinal damage. On the other hand, the retinal pathology resulting from phototoxicity is more localized and restricted to the superior–temporal regions above the optic disk at the stages when the damage is not too advanced (see Figures 2 and 3; Rapp 1980b; Organisciak et al. 1999; Tanito et al. 2008). Consequently, it is important to critically maintain section orientation in order to establish the topography of the damage.
Suitable dissection and processing of the eye for histologic evaluation is essential for proper diagnosis of retinal atrophy and to establish whether it is light induced. We recommend that the eyes be removed with the optic nerve and upper eyelid and fixed in a fixative such as Davidson’s solution. Proper orientation of the eye during embedding and sectioning is important and the dorsoventral and temporal–nasal landmarks of the globe need to be retained. The globes are oriented and trimmed in the dorsoventral plane (Figure 3A; Rapp 1980b), or, alternatively, in the supero–temporal to infero–nasal plane (Figure 3D; (Tanito et al. 2008)). Technically, it is easier to orient the globes in the dorsoventral plane. We recommend this as a routine practice as it is not possible to predict in most studies whether a retinal finding will occur that will require differentiation from retinal light damage.
The sections are then examined to record ONL thickness, preferably in terms of vertical rows of nuclei, at predetermined sites, usually in 0.5 mm intervals from the optic disk edge along the dorsal and ventral meridians, and the results graphically displayed (Figure 3A). Assessment is made at each location in the section, and the output represented as “spidergraphs.” Typically, the early stage of retinal light damage is clearly represented by a marked decrease in ONL in an ∼2 mm region above the edge of the optic disk (Figure 3A).
A point that was clearly brought out in the surveys (see Supplementary Tables 2 and 3) is the lack of consistent methodologies for measuring light intensities in animal rooms. While the NRC guidelines give suggested values and locations for measurements, the instruments and procedures used are not specified. Consequently, it was not possible to compare results across the different CROs included in the survey. For that reason, it would be important to develop a uniform industry-wide standard operating procedure (SOP) for measuring and recording light levels in the animal room, and at the front and inside of the cages. This would specify the instrument, probes, and their position and orientation in the room and cages. In this manner, it would be possible to reliably determine retinal phototoxicity in future studies and assess whether modifications in housing or husbandry ameliorate or worsen the incidence of this finding.
Summary and Conclusions
Light damage is a frequent finding in long-term safety studies of rodents and is a confounding effect in differentiating direct toxicity of the test article from environmental phototoxicity. The finding is mainly limited to albino strains and is dependent on the intensity and exposure duration. Animal-associated factors include age, gender, pigmentation, body temperature, and strain. Genetic factors include a protective SNP at Leu450Met in RPE65 where the methionine variant is protective as it markedly reduces the vitamin A cycle in the RPE. Environment-associated factors include room illumination, type of caging, and husbandry practices. A survey of 8 CROs in Western Europe, Asia, and North America indicated variability in caging and husbandry practices; likewise, there was a broad range of incidence of retinal atrophy in control animals in the different CROs. The purpose of the survey was to examine for consistencies and differences in management practices and not to establish a causal association between the incidence of retinal atrophy and specific housing or husbandry practices. The data advocate for careful monitoring of background incidences of retinal atrophy in repeated dose studies. Even though the data do not allow a precise conclusion on the role of light levels, it is expected that lower light levels should help reduce the incidence of phototoxic retinopathy without impact on study quality. Also evident from our survey is the need to develop a uniform industry-wide SOP for measuring and recording light levels in the animal room. As retinal light damage has characteristic morphology, topography, and can be prevented by decreased ambient light levels and/or pigmentation, the tools are readily available to interpret retinal findings in safety studies from the perspective of light damage unrelated to the test article.
Supplementary Material
Supplementary tables are located online at http://tpx.sagepub.com/supplemental.
Footnotes
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported in part by Foundation Fighting Blindness and NEI/NIH grants EY-06855 and -17549.
Abbreviations
Acknowledgments
The authors are grateful to Dr. Ulrich Certa of F. Hoffmann-La Roche Ltd., Basel, Switzerland, for molecular analyses of CD-1 outbred strains of mice for RPE65 polymorphisms, to Dr. Roy Bellhorn for helpful discussions and providing original material from his 1980 publication (![]() ), to Dr. Daniel Organisciak for many insightful and helpful discussions with one of the authors (G.D.A.) over many years, and to Dr. Maureen Hargaden for information regarding IVC design cages. We acknowledge the helpful participation of the following CROs for taking part in the survey: Covance Laboratories, Inc., Madison, WI; Charles River Laboratories, Senneville, Quebec, Canada; Covance Laboratories Ltd, Harrogate, UK; Harlan Laboratories Ltd., Itingen, Switzerland; Ricerca Biosciences SAS, Saint-Germain sur l'Arbresle, France; BOZO Research Center Inc., Shizuoka, Japan; Shin Nippon Biomedical Laboratories, Kagoshima, Japan; Ina Research Inc., Nagano, Japan; Mitsubishi Chemical Medience Corporation, Ibaraki, Japan. The content of this work is solely the responsibility of one of the authors (G.D.A.) and does not necessarily reflect the views of the NIH.
), to Dr. Daniel Organisciak for many insightful and helpful discussions with one of the authors (G.D.A.) over many years, and to Dr. Maureen Hargaden for information regarding IVC design cages. We acknowledge the helpful participation of the following CROs for taking part in the survey: Covance Laboratories, Inc., Madison, WI; Charles River Laboratories, Senneville, Quebec, Canada; Covance Laboratories Ltd, Harrogate, UK; Harlan Laboratories Ltd., Itingen, Switzerland; Ricerca Biosciences SAS, Saint-Germain sur l'Arbresle, France; BOZO Research Center Inc., Shizuoka, Japan; Shin Nippon Biomedical Laboratories, Kagoshima, Japan; Ina Research Inc., Nagano, Japan; Mitsubishi Chemical Medience Corporation, Ibaraki, Japan. The content of this work is solely the responsibility of one of the authors (G.D.A.) and does not necessarily reflect the views of the NIH.
Authors’ Note
Maria Cristina De Vera Mudry, Sven Kronenberg, and Shun-ichiro Komatsu equally contributed to the study. Drs. Maria Cristina De Vera Mudry and Sven Kronenberg are employed by F. Hoffmann-La Roche Ltd., Basel, Switzerland, and Dr. Shun-ichiro Komatsu is employed by Chugai Pharmaceutical Co., Ltd., Shizuoka, Japan.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
