Abstract
It is generally said that neoplastic cells are immunohistochemically negative for glial fibrillary acidic protein (GFAP) in rat spontaneous astrocytomas, and there are no reports describing the existence of GFAP-positive neoplastic astrocytes in rat spontaneous oligodendrogliomas and mixed gliomas which contain neoplastic astrocytes. In the present study, to clarify whether GFAP-positive neoplastic astrocytes exist in rat spontaneous oligodendrogliomas and mixed gliomas or not, immunohistochemical examination was performed on spontaneous oligodendrogliomas (26 cases) and mixed gliomas (5 cases) collected from the carcinogenicity studies and short-term toxicity studies. The neoplastic cells that constitute oligodendrogliomas and mixed gliomas were morphologically classified into five types: round A, round B, round C, spindle, and bizarre. The cells of round A, B, and C types were thought to be neoplastic oligodendrocytes because of their positive immunostainability for Olig2. The origin of bizarre cells was obscure because they were negative for Olig2, GFAP, and nestin. The spindle cells were considered to be neoplastic astrocytes, because some of them were positive for GFAP or nestin, and GFAP-positive spindle cells could be morphologically distinguished from reactive astrocytes. In conclusion, the present study clarified for the first time that GFAP-positive neoplastic astrocytes exist in rat spontaneous gliomas.
Introduction
Glial fibrillary acidic protein (GFAP) is the principal intermediate filament of mature astrocytes, and neoplastic astrocytes show positive immunostainability for GFAP in animals other than rodents. Therefore, immunostaining for GFAP is used for diagnosis of glial tumors in such animals (Ide et al. 2010; Lopes and VandenBerg 2000; Stoica et al. 2011).
In rodents, normal and reactive astrocytes are positive for GFAP, and neoplastic astrocytes are reported to be positive for GFAP in some of the avian sarcoma virus–induced astrocytomas (Lee et al. 1986), ethylnitrosourea (ENU)-induced rat astrocytomas (Yoshimine et al. 1987; Raju et al. 1990; Zook, Simmens, and Jones 2000), and malignant gliomas in the S100β-v-erbB transgenic rats (Yokoo et al. 2008). On the other hand, there are no reports describing the existence of GFAP-positive neoplastic astrocytes in rat spontaneous astrocytomas, although detailed immunohistochemical examinations have been done by many researchers (Krinke and Germer 1993; Krinke et al. 2000; Nagatani et al. 2009; Pruimboom-Brees et al. 2004; Solleveld, Gorgacz, and Koestner 1991; Weber et al. 2011).
Among spontaneous brain tumors, besides astrocytomas, mixed tumors and oligodendrogliomas contain neoplastic astrocytes. According to the International Harmonization of Nomenclature and Diagnostic Criteria (INHAND) for lesions in rat and mouse (Kaufmann et al. 2012), mixed glioma is the neoplasm of which at least 20% is occupied by neoplastic astrocytes and oligodendrocytes each, and neoplastic astrocytes occupy less than 20% of oligodendroglioma. To date, the existence of GFAP-positive neoplastic cells has not yet been reported in spontaneous mixed gliomas and oligodendrogliomas in nontransgenic rodents.
Olig2 is a transcription factor involved in the phenotype definition of cells in the oligodendroglial lineage, Olig2 and GFAP are expressed in a mutually exclusive manner (Mokhtari et al. 2005; Yokoo et al. 2004, 2008), and nestin is an intermediate filament protein (class Type VI) expressed during the development and used as a marker for neural stem cells differentiating into astrocyte progenitors (Ma et al. 2008; Schiffer, Manazza, and Tamagno 2006).
The purpose of the present study is to clarify whether GFAP-positive neoplastic astrocytes exist in spontaneous mixed gliomas and oligodendrogliomas using immunostaining for GFAP, Olig2, and nestin.
Materials and Methods
The tissue samples were collected from control and test groups in 14 carcinogenicity studies and 2 short-term studies using F344/DuCrlCrlj rats (Charles River Japan Inc., Atsugi, Kanagawa, Japan) and Crl:CD(SD) rats (Charles River Japan Inc.), and the tests were conducted using chemicals without treatment-related effects on the central nervous system (CNS), in BOZO Research Center with permission from the Animal Care and Use Committee of BOZO Research Center.
All animals were housed individually in a wire mesh cage in an animal room under controlled conditions (23°C ± 3°C room temperature, 50% ± 20% relative humidity, and a 12-hr light/dark cycle), fed a commercial diet (CRF-1, Oriental Yeast Co., Ltd., Tokyo, Japan), and checked daily. A complete necropsy was performed, and the brain and spinal cord were fixed in 10% phosphate-buffered formalin, trimmed, and embedded in paraffin.
All tissue sections of the CNS with neoplasm were re-examined in detail. Then, a total of 31 neoplasms were diagnosed as malignant mixed glioma or malignant oligodendroglioma, according to INHAND (Kaufmann et al. 2012). Tissue sections of these neoplasms were stained with hematoxylin and eosin (HE). In addition, immunohistochemical staining for GFAP, Olig2, and nestin was also done on these neoplasms by the avidin–biotin–peroxidase complex method using EnVision kits (Dako Japan, Kyoto, Japan). The first antibodies used were as follows: (1) anti-GFAP rabbit polyclonal antibody (1:500, Dako Japan), (2) anti-human Olig2 rabbit polyclonal antibody (1:100, Immuno-Biological laboratories Co., Ltd., Gunma, Japan), and (3) anti-nestin mouse monoclonal antibody (clone: Rat-401, 1:100, Santa Cruz Biotec., Inc., CA). Positive control sections for GFAP and Olig2 were obtained from adult rat brains and those for nestin from fetal rat brains. As to immunostaining for Olig2, eight oligodendrogliomas and three mixed gliomas were evaluated. The remaining 20 cases were not evaluated because even normal oligodendrocytes did not show positive immunostainability for Olig2. In these cases, immunostainability for Olig2 might be lost after a long-term fixation of tissues with 10% phosphate-buffered formalin.
Results
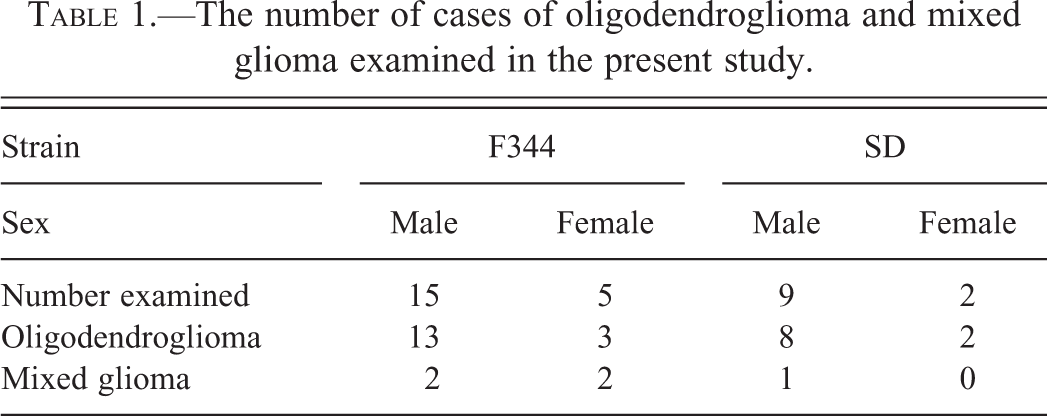
In all, 26 oligodendrogliomas and 5 mixed gliomas were obtained from 14 carcinogenicity studies and 2 short-term toxicity studies conducted in BOZO Research Center (Table 1).
The number of cases of oligodendroglioma and mixed glioma examined in the present study.

Histological Characteristics of the Tumors
In oligodendroglioma (Figure 1), a well-circumscribed focus of neoplastic cells was seen in one or multiple areas. In the tumor, neoplastic cells were arranged in sheets or rows, and microvascular proliferation with atypical endothelial hyperplasia and/or cystic changes were observed. The neoplastic cells were generally uniform but sometimes showed pleomorphism, and they were divided into three types (round A, round B, and round C types), according to their morphological characteristics as described below. The neoplastic cells of round A and B types were arranged in sheets or rows composed of single type cells or mingling type cells, and the lesion composed of round A type cells showed honeycomb structures. Round C type cells were arranged in rows, circles, or small clusters. The neoplastic cells of these three types were often embedded in mucinous or eosinophilic ground substance. Some oligodendrogliomas contained foci of mixed glioma within the above-mentioned typical oligodendroglioma lesion, and they looked like mixed glioma. However, more than 80% of neoplastic cells consisted of round A, B, and/or C type cells even in such tumors. Thus, all tumors corresponded to malignant oligodendrogliomas of high grade or to those of low grade, according to INHAND (Kaufmann et al. 2012).
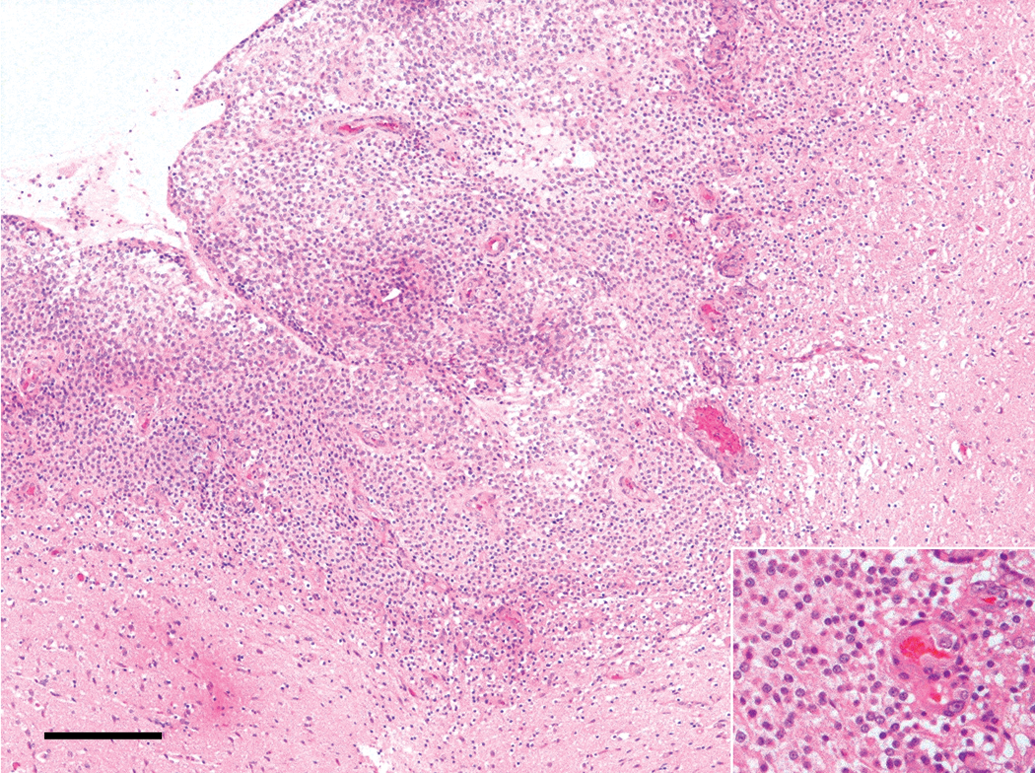
Histology of oligodendroglioma. Uniform cells with small round nuclei are arranged in sheet, and proliferation of microvessels showing atypical endothelial cell hyperplasia is seen (HE). HE, hematoxylin and eosin. Bar = 200 µm.
In the mixed glioma (Figure 2), a demarcated lesion was seen being confined to one major area, and necrosis and microvascular proliferation with atypical capillary endothelial hyperplasia which were frequently detected in the above-mentioned oligodendrogliomas were seldom observed. The neoplastic cells were morphologically classified into four different types (round A, round B, spindle, and bizarre), and they were mingled with each other in varying ratios. Spindle cells were frequently arranged in whorls closely around the vessels or in bundles, while the other type cells showed no particular pattern of arrangement. The cells of round A and B types were similar to those of oligodendrogiomas, but they were seldom arranged in sheet or row in mixed gliomas. Reactive astrocytes were sporadically observed in the border area of neoplastic lesion in almost all cases, but they were sparsely observed in the whole area of neoplastic lesion in one case. Some nerve cells remained within the lesion. All mixed tumors corresponded to low-grade malignant mixed tumor, according to INHAND (Kaufmann et al. 2012).
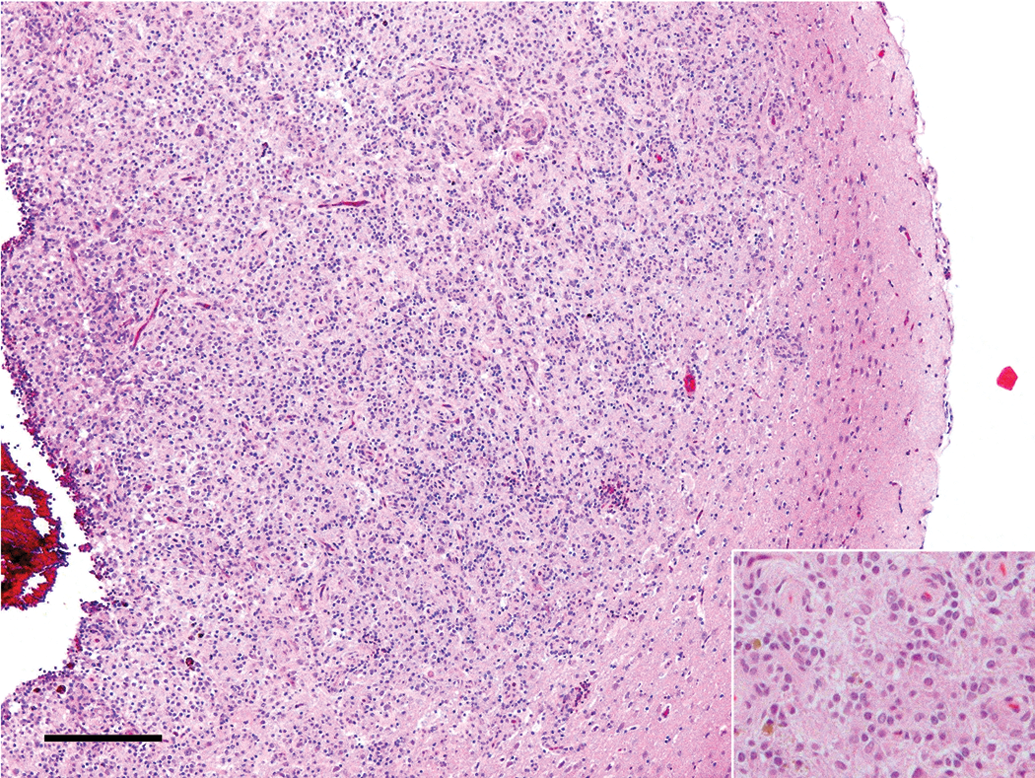
Histology of mixed glioma. Tumor is composed of both round cells with small or large round nuclei and spindle cells with oval nuclei (HE). HE, hematoxylin and eosin. Bar = 200 µm.
Histological and Immunohistochemical Characteristics of the Neoplastic Cells and Reactive Astrocytes (Table 2)
Round A type cells (Figure 3): The cells had a small round dark-staining nucleus, clear or scant eosinophilic cytoplasm, and delicate cell membrane. The cells were uniform and mitotic figures were seldom observed. Most cells were positive for Olig2, but were negative for GFAP and nestin.
Round B type cells (Figure 4): The cells had a small round pale nucleus, pale eosinophilic cytoplasm, and delicate cell membrane. The cells were uniform like round A type cells, but the nucleus was a little larger than that of round A type cells. Mitotic figures were rarely observed. Most cells were positive for Olig2, and some of the Olig2-positive cells were also positive for GFAP. However, they were negative for nestin.
Round C type cells (Figure 5): The cells had a large round or oval nucleus with a prominent nucleolus and eosinophilic cytoplasm. Mitosis and nuclear atypia were often observed in this type cells. The cells were generally positive for Olig2 but not for GFAP and nestin.
Spindle type cells: The cells were spindle in shape and had an oval, spindle, or elongated nucleus and eosinophilic cytoplasm. Some of the spindle cells were positive for GFAP (Figure 6), and some of the GFAP-negative spindle cells were positive for nestin (Figure 7). GFAP-positive cells seldom showed mitosis or nuclear atypia, while nestin-positive cells sometimes showed mitosis or atypia. Spindle cells were negative for Olig2.
Bizarre type cells: The cells were large round or polygonal in shape, and they had a large round nucleus with a prominent nucleolus and abundant eosinophilic cytoplasm. Mitosis or atypical nuclei were often observed. The morphology of bizarre type cells was similar to that of the above-mentioned round C type cells, except for having more abundant cytoplasm. Bizarre type cells were sporadically observed and were not arranged in rows, circles, or small clusters, differing from round C type cells. Bizarre type cells were negative for Olig2, GFAP, and nestin.
Reactive astrocytes (Figure 8): Reactive astrocytes were characterized by a round or oval clear nucleus and abundant pale eosinophilic cytoplasm. They were intensely positive for GFAP, and their short or long processes were also GFAP positive. On the other hand, reactive astrocytes were negative for Olig2 and nestin.
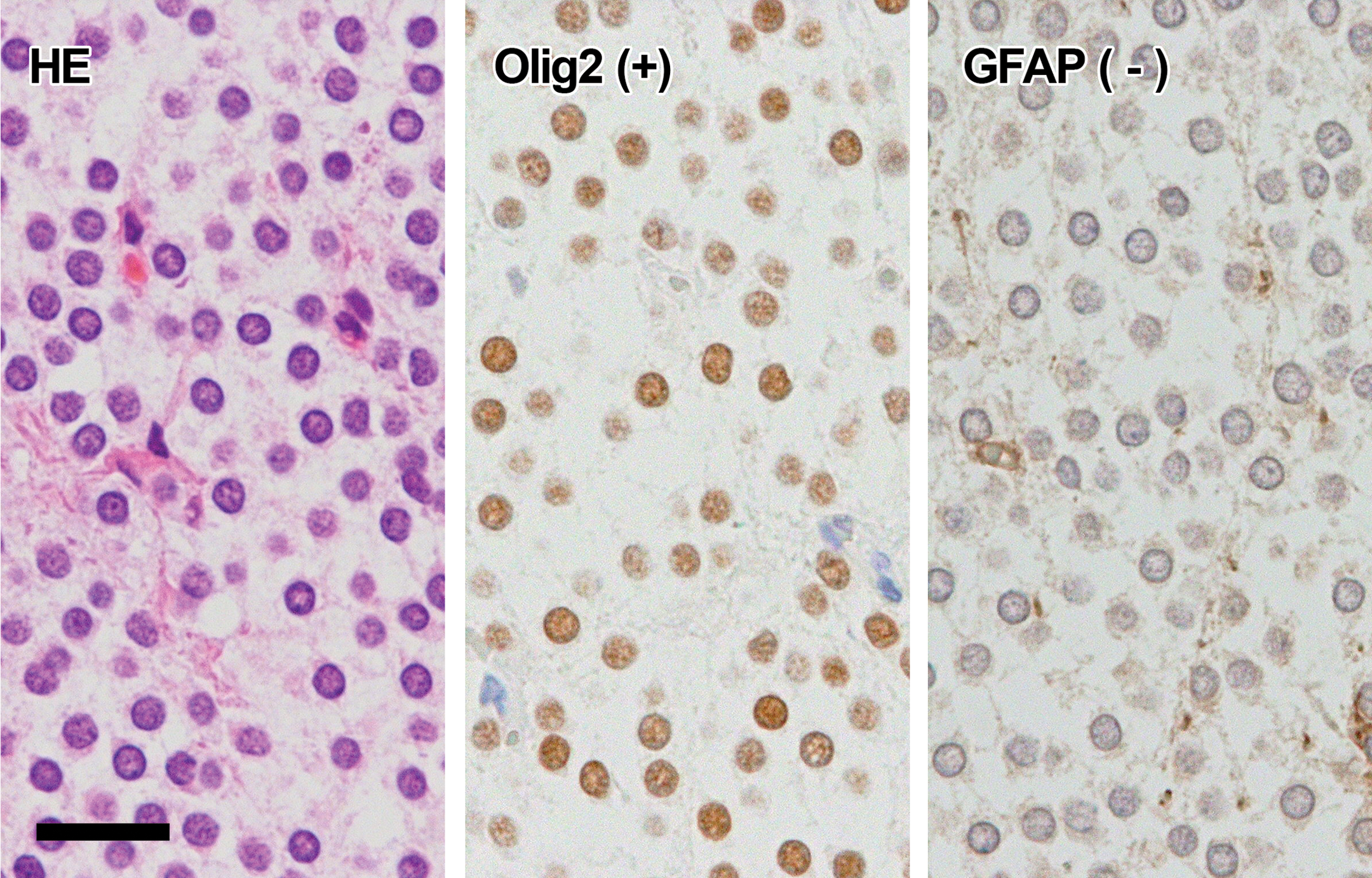
Histology and immunohistochemistry of round A type cells. The cells have small round dark-staining nuclei and clear cytoplasm (HE). Immunohistochemically, the nucleus is positive for Olig2 and the cytoplasm is negative for GFAP. GFAP, glial fibrillary acidic protein; HE, hematoxylin and eosin. Bar = 20 µm.
Characteristics of component cells of oligodendroglioma and mixed glioma examined in the present study.
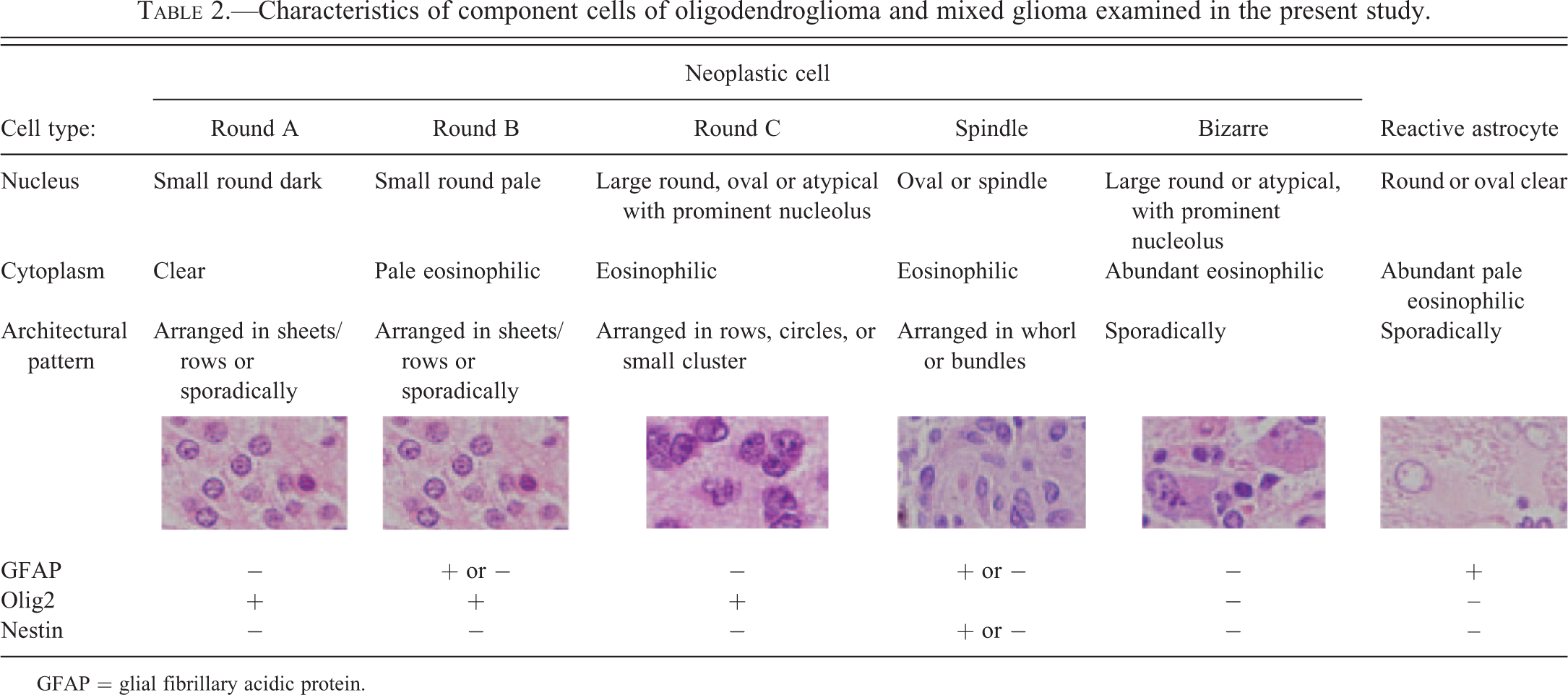
GFAP = glial fibrillary acidic protein.
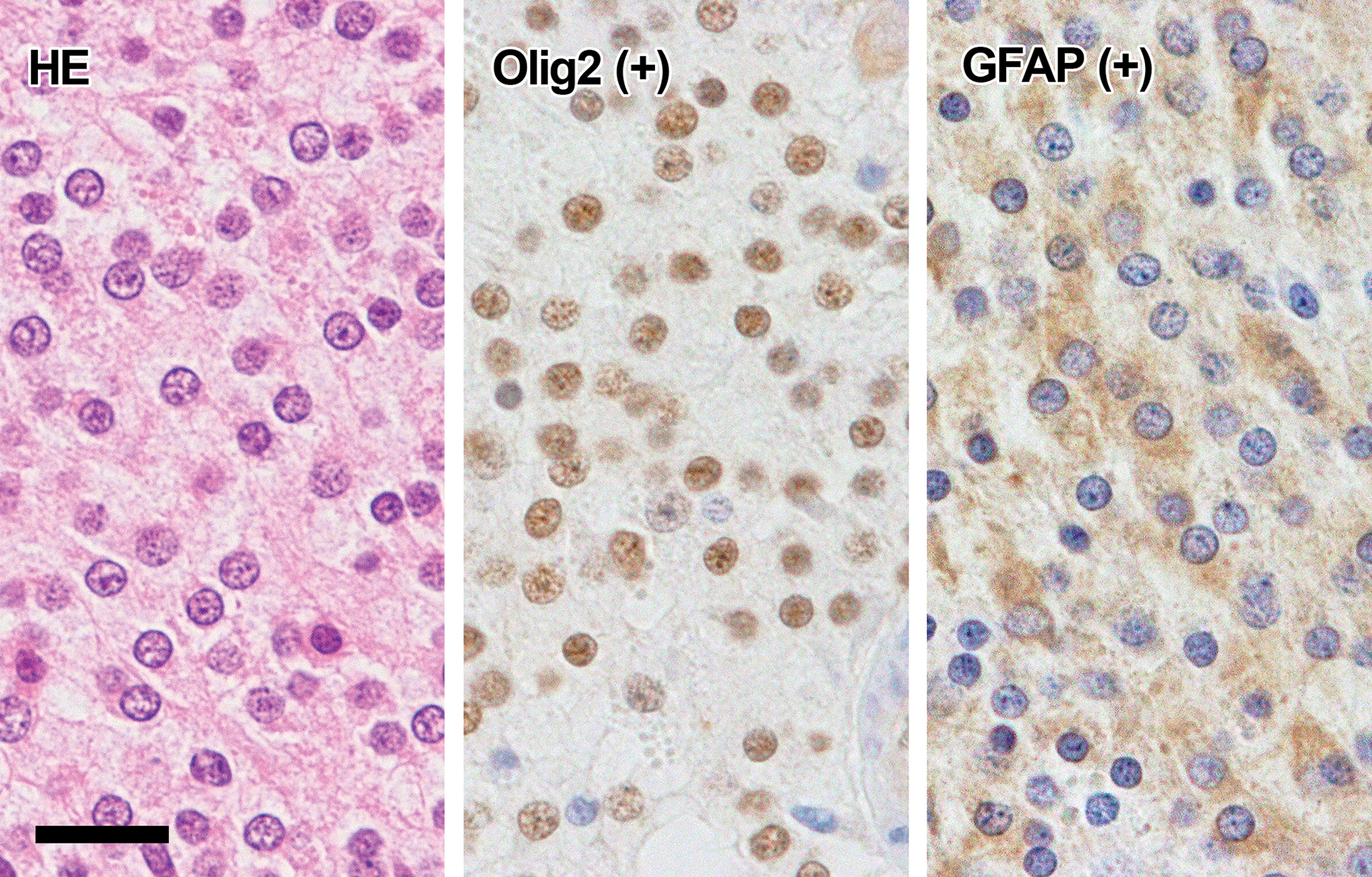
Histology and immunohistochemistry of round B type cells. The cells have small round pale-staining nuclei and pale eosinophilic cytoplasm (HE). Immunohistochemically, the nucleus is positive for Olig2 and the cytoplasm is positive for GFAP. GFAP, glial fibrillary acidic protein; HE, hematoxylin and eosin. Bar = 20 µm.
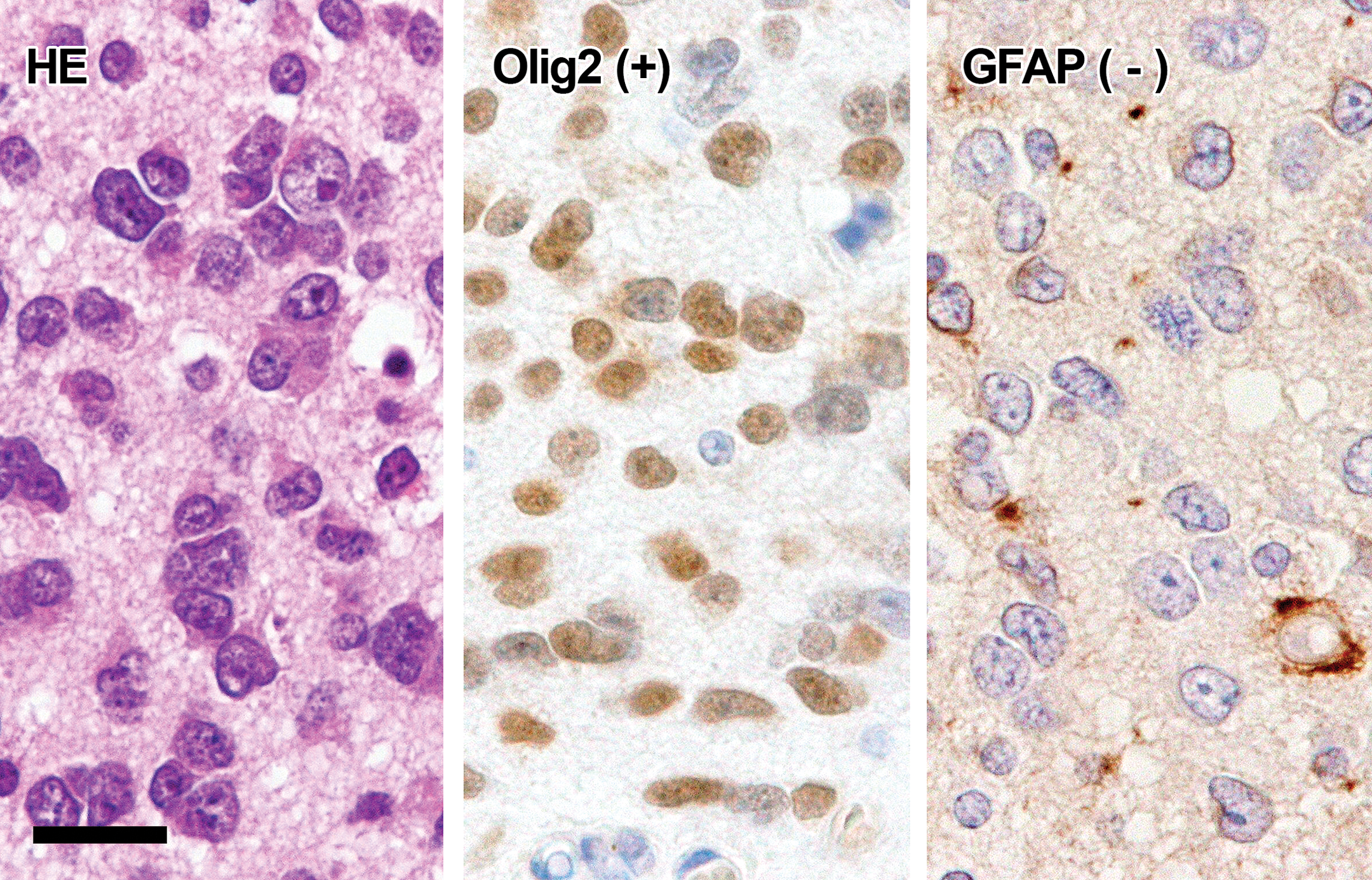
Histology and immunohistochemistry of round C type cells. The cells have large atypical nuclei with prominent nucleoli and scant eosinophilic cytoplasm (HE). Immunohistochemically, the cells are positive for Olig2 but negative for GFAP. GFAP, glial fibrillary acidic protein; HE, hematoxylin and eosin. Bar = 20 µm.
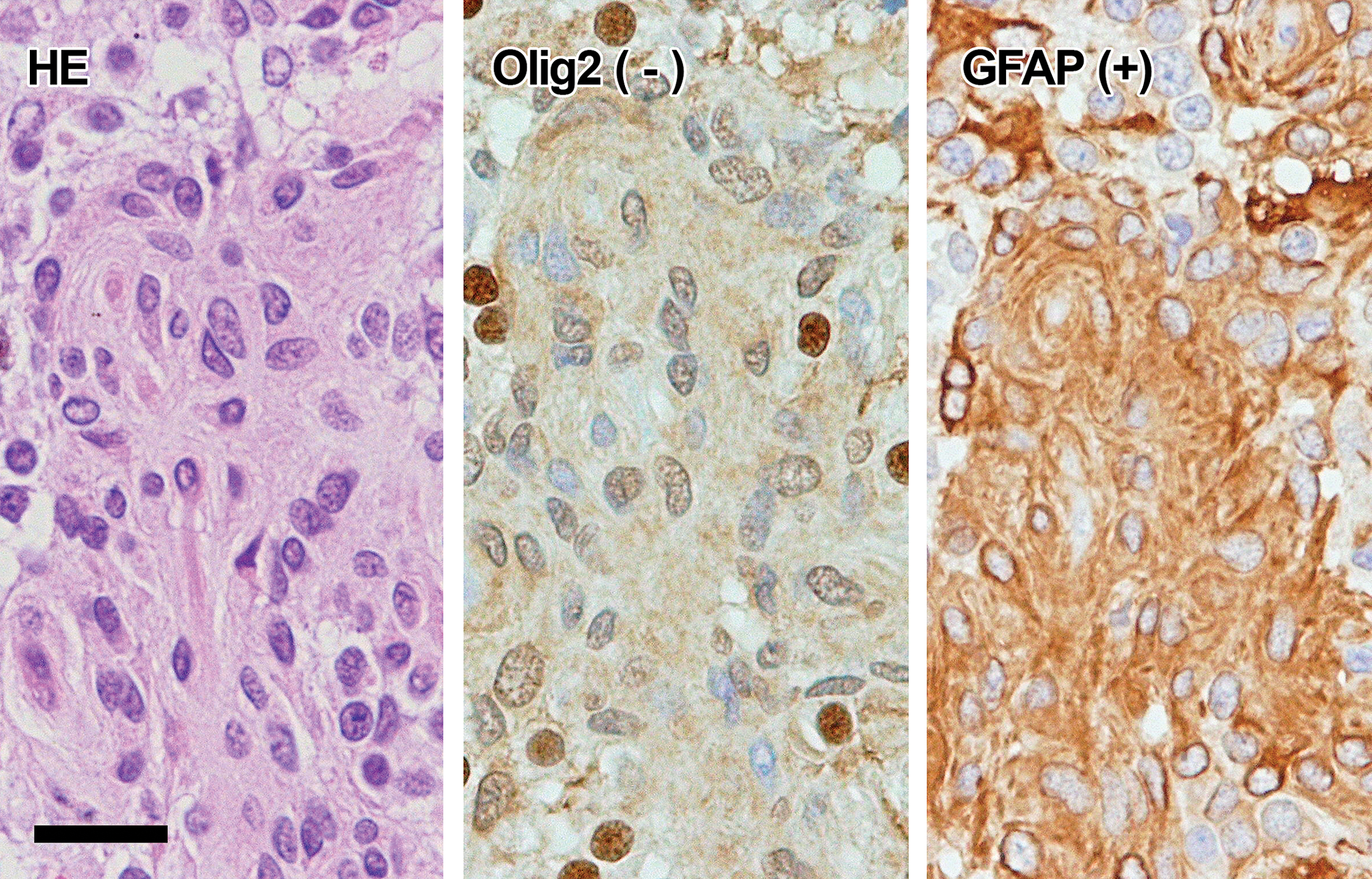
Histology and immunohistochemistry of spindle type cells (GFAP+). The cells are spindle and contain oval or elongated nuclei (HE). Immunohistochemically, the cells are positive for GFAP but negative for Olig2. GFAP, glial fibrillary acidic protein; HE, hematoxylin and eosin. Bar = 20 µm.
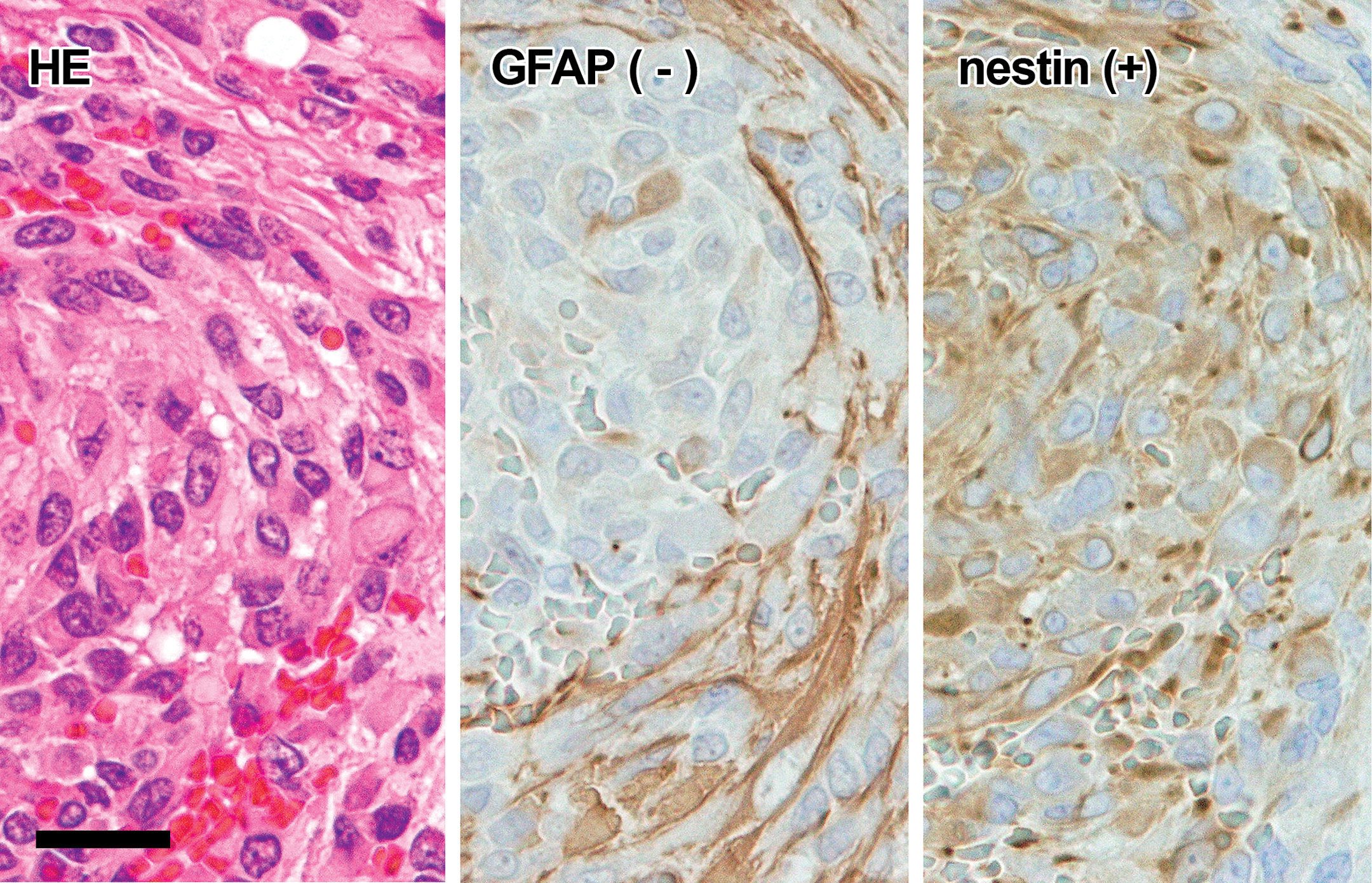
Histology and immunohistochemistry of spindle type cells (GFAP−). The cells are spindle and contain oval or elongate nuclei (HE). Immunohistochemically, the cells are negative for GFAP but positive for nestin. GFAP, glial fibrillary acidic protein; HE, hematoxylin and eosin. Bar = 20 µm.
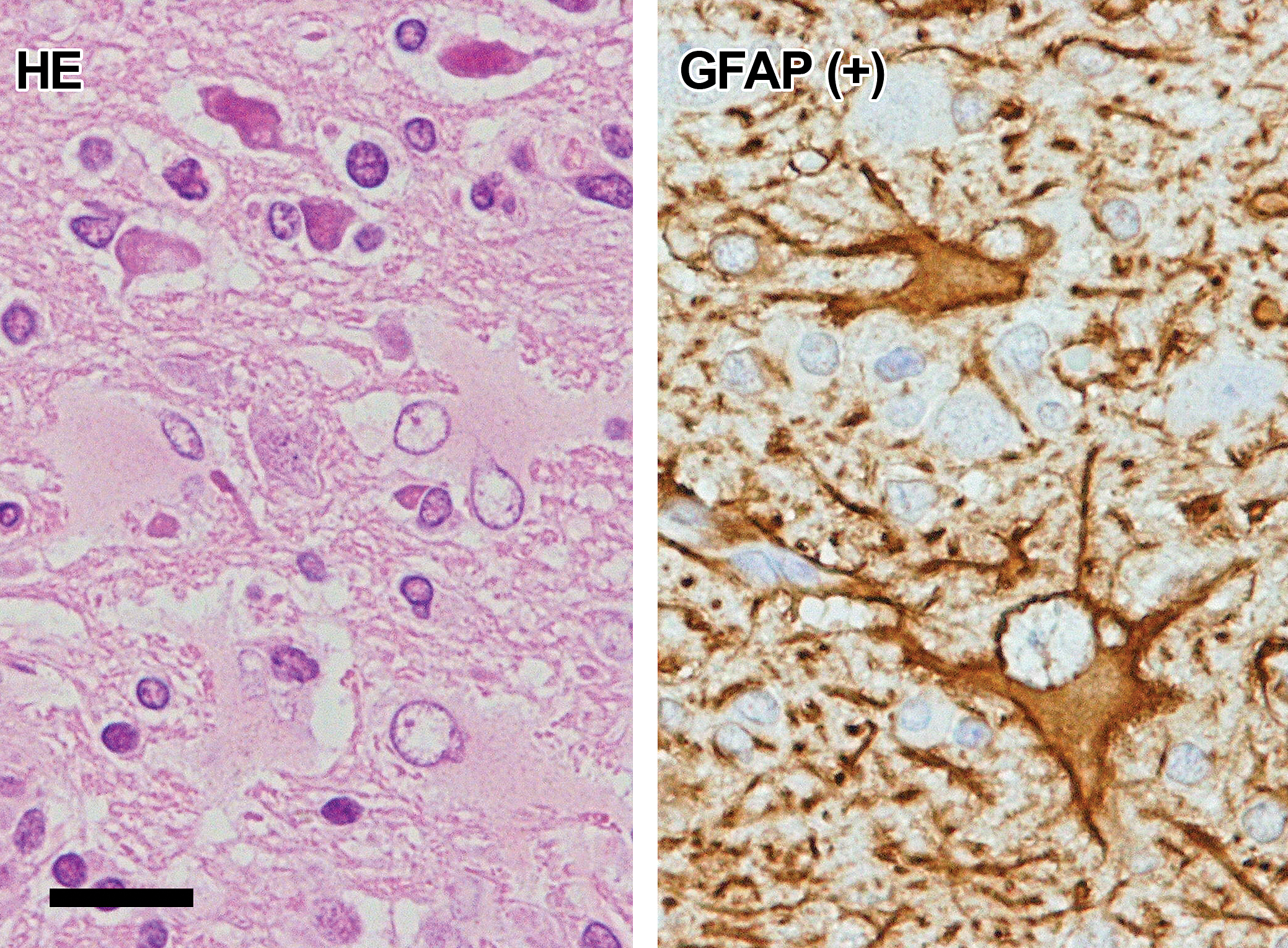
Histology and immunohistochemistry of reactive astrocytes. The cells are characterized by round or oval clear nuclei and abundant pale eosinophilic cytoplasm (HE). Immunohistochemically, GFAP-positive reactive astrocytes have long cellular processes. GFAP, glial fibrillary acidic protein; HE, hematoxylin and eosin. Bar = 20 µm.
Discussion
The present study was carried out to clarify whether GFAP-positive neoplastic cells exist in rat spontaneous mixed gliomas and oligodendrogliomas or not. Based on cell morphology and immunoreactivity for GFAP, neoplastic cells were classified into 5 types: round A, round B, round C, spindle, and bizarre. The positive immunostainability for GFAP was detected in some of the spindle and round B type cells.
In rats, it is important to distinguish GFAP-positive neoplastic cells from reactive astrocytes. In this context, the GFAP-positive spindle cells were different from reactive astrocytes in cell morphology. In addition, compared to reactive astrocytes characterized by long cell processes that were clearly detected by GFAP staining, cell processes were unclear in the GFAP-positive spindle cells. Moreover, spindle cells were often arranged in whorl patterns with close relation to blood vessels, while reactive astrocytes were observed sporadically without association with blood vessels. Spindle cells observed in the present study are similar to neoplastic astrocytes in ENU-induced mixed gliomas in rats (Zook, Simmens, and Jones 2000), and mitosis and anaplasia were seldom detected in GFAP-positive spindle cells. The GFAP-positive spindle cells, therefore, were considered to be differentiated neoplastic astrocytes.
On the other hand, some of the GFAP-negative spindle cells were positive for nestin. Mixed gliomas and oligodendrogliomas that are similar to spontaneous ones can be experimentally induced in rats by transplacental treatment with ENU (Yoshimine et al. 1987; Koestner 1990; Zook, Simmens, and Jones 2000). In the developing process of ENU-induced glioma, GFAP-negative and nestin-positive cells that are probably undifferentiated astrocytes appear (Jang et al. 2006). Therefore, GFAP-negative and nestin-positive spindle cells in the present study were also considered to be undifferentiated neoplastic astrocytes.
The round A, B, and C type cells expressed Olig2, and their morphological features were coincident with those of neoplastic oligodendroglia described in previous reports (Weber et al. 2011; Krinke et al. 2000; Solleveld, Gorgacz, and Koestner 1991), suggesting that these cells are neoplastic oligodendroglia. In the present study, round B type cells had typical features of oligodendroglia, and some of them were positive for both Olig2 and GFAP. In human, typical oligodendrocytes in oligodendrogliomas are said to be positive for GFAP (Herpers and Budka1984; Mclendon and Bigner 1994). This indicates that some of the type B cells in rats, which were positive for GFAP, resemble human oligodendroglioma cells. As reported in human cases, some minor foci of cells positive for GFAP, a marker for astrocytes, are detected in oligodendroglioma. In our opinion, this does not influence the final diagnosis of the tumor.
Bizarre cells observed in mixed gliomas were negative for Olig2, GFAP, and nestin. Morphological features of bizarre cells were similar to those of round C type cells of neoplastic oligodendroglia. However, differing from round C type cells, the bizarre cells did not have an evidence of oligodendrocytes that are positive for Olig2. The origin of bizarre cells is still obscure.
Rat spontaneous astrocytoma is said to be negative for GFAP, and, in fact, GFAP-positive spontaneous astrocytoma has not been reported in rats until today. On the other hand, this tumor has been reported to be positive for several immunohistochemical markers for macrophages or microglia (Nagatani et al. 2009; Kolenda-roberts and Hardisty 2011). Therefore, the origin of this tumor has been controversial. However, the existence of GFAP-positive neoplastic astrocytes detected for the first time by us suggests that GFAP-positive spontaneous astrocytoma may also exist in rats.
As mentioned above, differing from human and canine cases of spontaneous oligodendrogliomas and mixed gliomas, it has been said that there were no GFAP-positive neoplastic astrocytes detected in rat cases. However, in the present study on rat spontaneous oligodendrogliomas or mixed gliomas, there were some differentiated neoplastic astrocytes positive for GFAP. Thus, the present study clarified for the first time that GFAP-positive neoplastic astrocytes also exist in rat spontaneous gliomas.
Footnotes
Acknowledgments
The authors thank Dr. Kunio Doi, Professor Emeritus of the University of Tokyo, for critical review of this manuscript, and Mr. Pete Aughton, D.A.B.T., ITR Laboratory Canada, for language editing.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
