Abstract
Background and Objectives
There are approximately 47.9 million unpaid caregivers in the United States supporting adult family or friends with health or functional needs (National Alliance for Caregiving and AARP, 2020). Due to the emotional, physical, and time demands of providing care, these caregivers are at elevated risk for adverse mental health and quality of life outcomes (Anderson et al., 2013; Hopps et al., 2017). Social isolation and loneliness are common among caregivers (Hajek et al., 2021), which may increase subsequent risk for psychological distress (Liang et al., 2024). Caregivers who report higher life meaning and purpose ratings, however, appear to be protected against caregiving-related stress and psychopathology (Chang et al., 2021). Over 600 interventions to support caregivers’ mental health and wellbeing have been developed and tested (Cheng & Zhang, 2020; Smith et al., 2019). Nonetheless, caregivers continue to have worse mental health relative to their non-caregiving peers (Kilmer, 2024). The efficacy of many psychological caregiver interventions appears to be moderated by caregiver age (Cheng et al., 2020; Secinti et al., 2023), yet little research has been conducted to understand how caregivers’ mental health differs across different caregiver age groups or generations. Characterizing the mental health needs of caregivers by age group or generation is important to identify caregiving cohorts in disproportionate need of psychological intervention and inform how such intervention may need to differ across generations.
Caregiver generational status is an often overlooked sociodemographic factor in caregiver intervention research (Ploeg et al., 2018). This is a missed opportunity as generation offers a unique factor that distinguishes groups of individuals with many shared characteristics, thus making it ripe for intervention tailoring and targeting (Pew Research Center, 2015). From the cohort based, life course framework put forth by Elder & George, a generational cohort may reflect individual’s (a) current life cycle phase (i.e., middle-aged parent versus retiree) and (b) some shared attitudes, behaviors, and preferences (Elder & George, 2016). Common attitudes, behaviors, and preferences within a generation are often due to significant national events, circumstances, and trends (e.g., pandemics, technological changes) that occur during a specific life cycle phase for that generation (Pew Research Center, 2015). Generational status is a valuable, yet seldom used, heuristic to group caregivers to identify at-risk groups with potentially common socioenvironmental stressors and provide targeted intervention. For example, a recent (non-caregiver) behavioral cardiometabolic intervention adapted for 18–25 year-olds was more efficacious with this age group compared to previous interventions that had not been culturally tailored to this age band (LaRose et al., 2022). This suggests that behavioral interventions adapted for a specific age cohort or generation may increase intervention efficacy with the target sample.
With regards to psychological health in the general population, emerging generations [Millennials (born 1981–1996) and Generation Z (Gen Z; born >1996)] have higher rates of mental health stress than older generations [Generation X (Gen X; born 1965–1980) and Baby Boomers (born 1946–1964)] (Grelle et al., 2023; Pew Research Center, 2015). These generational differences in mental health are not exclusively explained by young adulthood life-cycle stressors (i.e., occupational uncertainty, family planning, child rearing, home purchasing) since young adult Americans currently have more mental health symptoms than young adult Americans in previous decades (Goodwin et al., 2020; Twenge, 2015). Importantly, there are other generational patterns with Millennials and Gen Z that might contribute to increased mental health issues in younger generations. For example, younger generations report higher rates of loneliness (79% Gen Z and 71% Millennials vs. 50% Baby Boomers) and lower rates of religious affiliation, which has historically been an important source of social connection (American Survey Center, 2022; Cigna, 2020). Additionally, younger generations often use social media for connection, which may paradoxically amplify feelings of loneliness (Bonsaksen et al., 2023). While generational differences in mental health have been studied in the general population and there are known emotional strains related to family caregiving, there have been no prior studies that we are aware of examining these differences among caregivers. The psychological distress of caregiving may be amplified in younger generations due to greater time scarcity in early to middle adulthood life cycle phases (e.g., may be caring for an adult while simultaneously parenting and working for an income) and shrinking family sizes over time, leaving fewer siblings and relatives to share family care burden for aging adults (Hansen & Slagsvold, 2015; Redfoot et al., 2013).
To address this gap in the literature, we investigate whether caregiver generations differ with regard to aspects of mental and social health. The results of this investigation will help inform appropriate targets for intervention by caregiver generation. Specifically, the goals of this analysis of a nationally representative U.S. survey are to compare mental and social health outcomes between those who do (caregivers) and do not (non-caregivers) provide unpaid care for an adult family member or friend, within and across generations. As outlined above, while prior research has found mental health differences between caregivers and non-caregivers, regardless of age (Janson et al., 2022), and between generations, regardless of caregiving status (Grelle et al., 2023), this would be a first investigation of how these risk factors interact. We expect a significant interaction between generation and caregiving status, such that younger caregivers will report particularly elevated psychological distress, social isolation, and lower life meaning relative to older generations of caregivers and their non-caregiving peers.
Research Design and Methods
Study Design and Participants
We analyzed data from a cross-sectional survey study conducted in 2022 by the National Cancer Institute (NCI): Health Information National Trends Survey, Version 6, Cycle 1 (HINTS 6) (NCI, 2023). HINTS is a large, nationally representative survey administered to English- or Spanish-speaking adults living in America. HINTS focuses on understanding health information support needs in the population. The HINTS six subsample analyzed to address our present study aims consisted of n = 1,074 adults (n = 537 caregivers and n = 537 demographically matched non-caregivers).
Caregiver Group (n = 537)
Caregivers self-identified as the primary, unpaid caregiver for an adult with a chronic health condition. This was operationalized as participants who answered affirmatively to the item, “Are you currently caring for or making health care decisions for someone with a medical, behavioral, disability or some other condition?” Caregivers who exclusively reported providing care for a child were excluded from this analysis due to the distinct nature of providing care for a child with special care needs (Chen & Lukens, 2011; Penning & Wu, 2016). Due to this paper’s focus on generational status and mental health, caregivers were excluded if age (and therefore generational status) was missing or if two or more (of three) mental health variables were missing.
Non-caregiver Group (n = 537)
Participants for the non-caregiver group in this analysis were selected using the Case-Control Matching tool in IBM SPSS v29. Non-caregivers (i.e., those answering “No” to the aforementioned adult family caregiving item) were matched to caregivers based on age, generation, sex at birth, education (dichotomized to less than or equal to high school versus greater than high school), and race/ethnicity (re-coded to combine non-Hispanic Asian and non-Hispanic other). Caregivers with missing matching variables values (e.g., missing sex) were matched to non-caregivers who were also missing a value for the relevant variable. Match tolerances were set to 0 (i.e., exact matches were required) for all matching variables except for age, which had a match tolerance of ±5 years (but within the same generational age bracket). To be evaluated as a match, the non-caregivers must have had valid, available data for age and all investigated mental health variables.
Case-control matching produced a non-caregiver group of n = 537 who were matched to the n = 537 caregiver group on generation, sex, and education. Only one caregiver did not have an exact match in the non-caregiver group, however an approximate match was randomly selected from the pool with consistent generation, sex, and education; race/ethnicity for the target caregiver was “Non-Hispanic Asian” and the selected non-caregiver had a missing value for race/ethnicity. As expected, age did not significantly differ between caregiver and non-caregiver groups. Within both the caregiver and non-caregiver group, <2.0% of participants were missing sex and education. Race/ethnicity was missing for 5.40% and 5.59% of participants in the caregiver and non-caregiver groups, respectively.
Measures
Demographic, Socioeconomic, and Caregiving Characteristics
Sample Demographics and Caregiving Characteristics
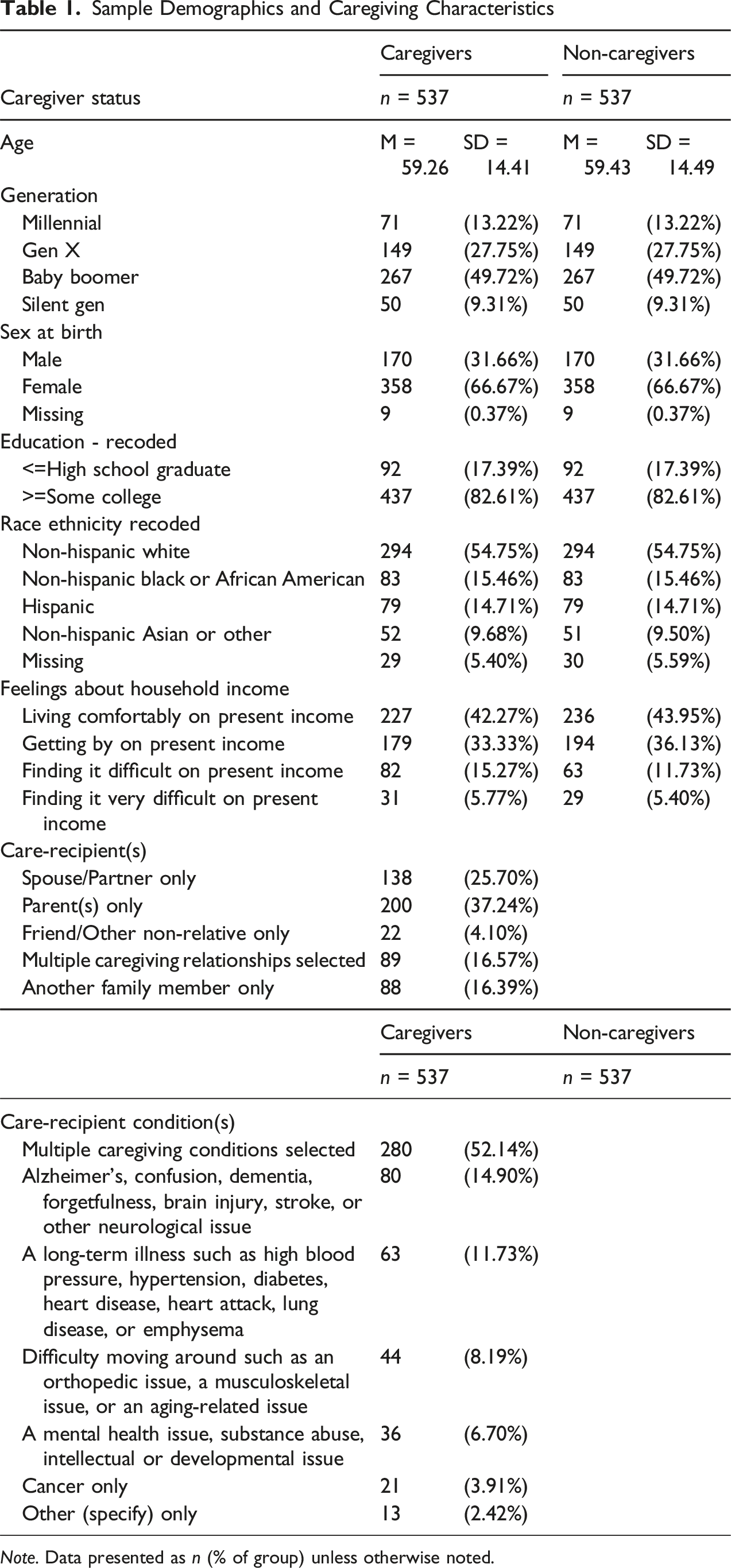
Note. Data presented as n (% of group) unless otherwise noted.
Mental and Social Health
The HINTS six survey included three measures related to mental and social health: psychological distress, social isolation, and life meaning.
Psychological Distress was measured by participants’ total score on the four-item Patient Health Questionnaire for Depression and Anxiety (PHQ-4). The PHQ-4 assesses the frequency [ranging from Not at all (0) to Nearly Every Day (3)] of the following bothersome symptoms over the previous 2 weeks: (1) Little interest or pleasure in doing things; (2) Feeling down, depressed, or hopeless; (3) Feeling nervous, anxious, or on edge; and (4) Not being able to stop or control worrying. The PHQ-4 total score is the sum of all four items and ranges from 0 to 12, with higher scores representing greater distress.
Social Isolation was measured by participants’ total score on the Patient-Reported Outcomes Measurement Information System (PROMIS) four-item Social Isolation item bank. The item bank assesses the frequency [ranging from Never (1) to Always (5)] of the following feelings: (1) I feel left out; (2) I feel that people barely know me; (3) I feel isolated from others; (4) I feel that people are around me but not with me. The raw score total is then rescaled into a standardized T-score with a mean of 50 and a standard deviation (SD) of 10, with higher scores representing higher self-reported levels of social isolation (PROMIS Social Isolation, n.d).
Life Meaning was measured by participants’ total score on the four-item PROMIS Meaning and Purpose item bank. The form assesses the participant’s level of agreement [ranging from Very Much (1) to Not at All (5)] with the following statements: (1) My life has meaning; (2) I have a clear sense of direction in life; (3) I experience deep fulfillment in my life; (4) My life has purpose. The Meaning and Purpose total raw score is rescaled into a standardized T-score, with higher scores representing stronger feelings of life meaning and purpose (PROMIS Meaning and Purpose Measure Differences, n.d).
Statistical Analyses
All analyses were conducted using IBM SPSS Statistics v.29. Descriptive statistics for demographic and caregiving characteristics included means with standard deviations or frequencies, as appropriate. Differences in key socioeconomic factors (sex, race/ethnicity, education, and household income attitude) across generations were evaluated using chi-square tests within the entire sample, the caregiver only group, and the non-caregiver only group. These analyses were conducted to inform the need for post-hoc sensitivity analyses for main hypothesis testing.
To compare mental and social health outcomes between caregivers and non-caregivers across generations, we conducted three individual analyses of variance (ANOVAs), one for each respective dependent variable of psychological distress, social isolation, and life meaning. Three individual ANOVAs were selected over a single multivariate analysis of variance (MANOVA) due to high correlations among dependent variables (rs ≥ ±.515) within caregivers and across the entire sample, which may inappropriately reduce power (Cole et al., 1994). For each ANOVA, the independent variables were generation, caregiver status, and the interaction term of generation-by-caregiver status.
An alpha threshold of p < .05 was used for main hypothesis testing. Where group-wise differences were detected, post-hoc pairwise comparisons were made and adjusted for multiple comparisons (a Bonferroni correction of p < .0083 was used for multiple (six) comparisons across generations). Given our goal of understanding whether caregiver generations differ with regard to aspects of mental and social health, we also explored post-hoc pairwise comparisons of generations within caregivers only (a Bonferroni correction of p < .0083 was again utilized). Taylor’s Series variance estimation bootstrapping was used to estimate standard errors, which reduces bias and, therefore, type I error, for main hypothesis testing. These procedures are in accordance with published HINTS analysis recommendations (NCI, 2023).
Results
See Table 1 for sample sociodemographic and caregiving characteristics. Chi-square, sensitivity testing revealed that within the entire sample, the caregiver group only, and the non-caregiver group only, there were generational differences in sex, race/ethnicity, and feelings about household income (ps < .05), but not education. Specifically, the Silent Gen had higher proportions of males relative to younger generations, Millennials had lower proportions of non-Hispanic White participants relative to older generations (i.e., they were more racially/ethnically diverse), and Millennials reported more financial instability. Differences between caregiver and non-caregiver groups were not assessed, as these groups were deliberately matched for sociodemographic factors.
Psychological Distress
Impact of Caregiver Status and Generation on Mental and Social Health
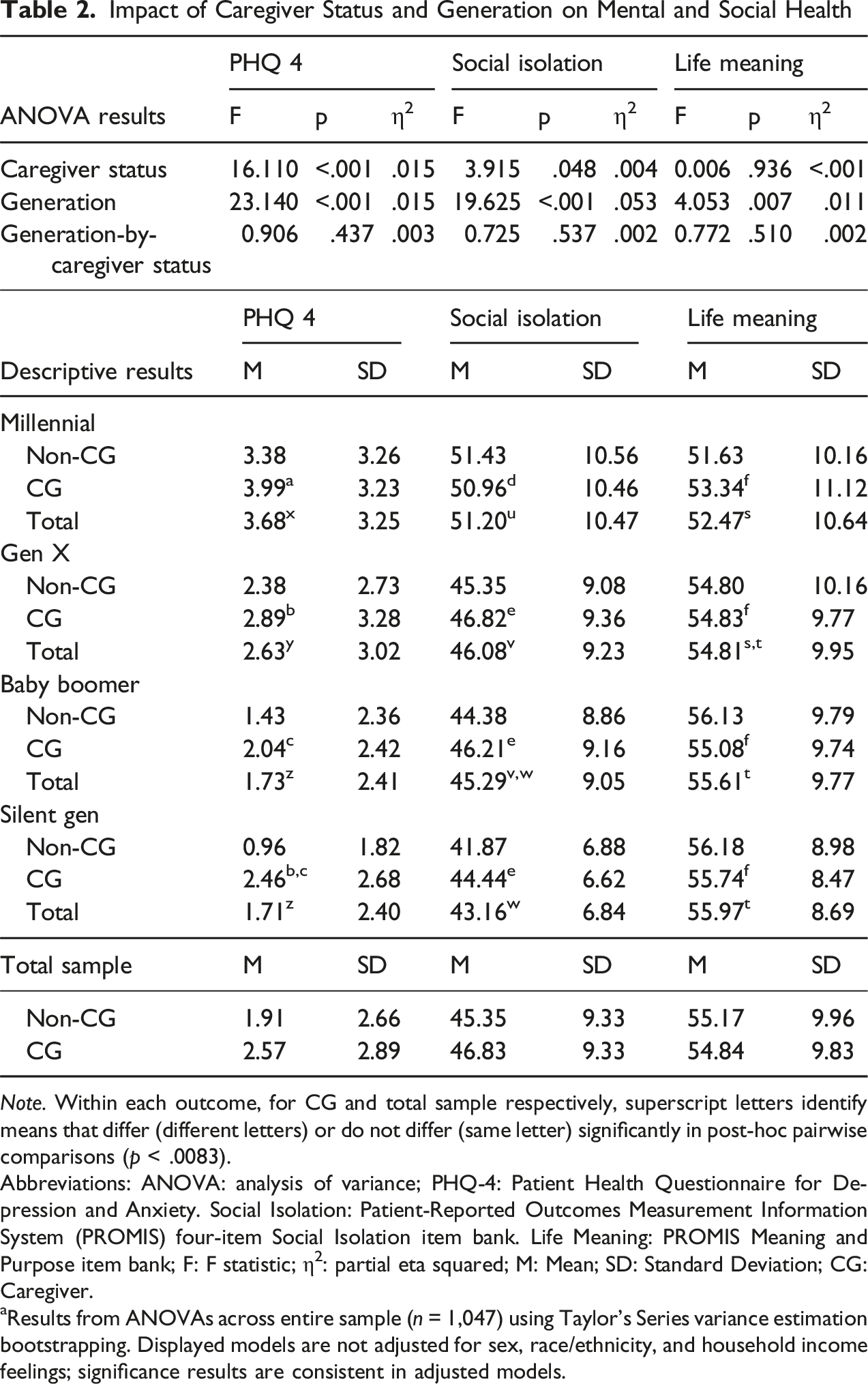
Note. Within each outcome, for CG and total sample respectively, superscript letters identify means that differ (different letters) or do not differ (same letter) significantly in post-hoc pairwise comparisons (p < .0083).
Abbreviations: ANOVA: analysis of variance; PHQ-4: Patient Health Questionnaire for Depression and Anxiety. Social Isolation: Patient-Reported Outcomes Measurement Information System (PROMIS) four-item Social Isolation item bank. Life Meaning: PROMIS Meaning and Purpose item bank; F: F statistic; η2: partial eta squared; M: Mean; SD: Standard Deviation; CG: Caregiver.
aResults from ANOVAs across entire sample (n = 1,047) using Taylor’s Series variance estimation bootstrapping. Displayed models are not adjusted for sex, race/ethnicity, and household income feelings; significance results are consistent in adjusted models.
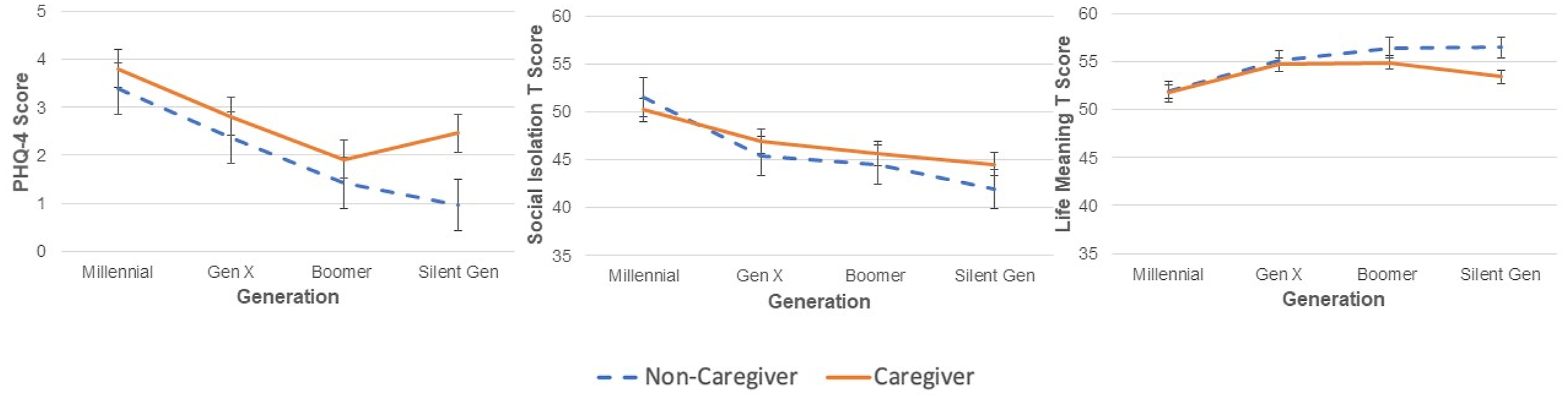
Mental and Social Health by Caregiver Status and Generation.
Social Isolation
ANOVA testing revealed a main effect of caregiver status and a main effect of generation, but no interaction effect of generation-by-caregiver status, on PROMIS Social Isolation scores (see Table 2 and Figure 1). Post-hoc testing of the main effects revealed that, for caregiving status, caregivers had higher PROMIS Social Isolation scores relative to non-caregivers (p = .048), though the difference was small. For generation, Millennials reported significantly greater social isolation relative to older generations, and Gen X reported significantly greater social isolation relative to Silent Gen (ps < .006). Among caregivers only, Millennials again reported greater social isolation compared to older generations of caregivers (ps <.002), but there was no longer a significant difference between Gen X and Silent Gen (p = .111).
Life Meaning
ANOVA testing revealed a main effect of generation, but no main effect of caregiver status or effect of generation-by-caregiver status, on PROMIS Life Meaning scores (see Table 2 and Figure 1). Post-hoc testing of the main effect for generation revealed that Millennials had significantly weaker feelings of life meaning and purpose relative to Baby Boomers and Silent Gen (ps < .008). Among caregivers only, there were no significant differences between generations on life meaning ratings (ps > .192).
Sensitivity Testing
Results of hypothesis testing were consistent (statistically significant results remained so) when models were adjusted for participant sex, race/ethnicity, and income feelings, with the exception of the social isolation ANOVA. For social isolation, the main effect of caregiver status became a trend (p = .092) once covariates were added to the model (versus p = .048 in the unadjusted model).
Discussion and Implications
This analysis of survey results from a diverse U.S.-national sample is the first to evaluate whether known disparities in psychological distress between caregivers and non-caregivers, as well as across generations, interact. Findings regarding the main effects of these factors largely replicated past research, with caregivers (regardless of generation) reporting significantly higher psychological distress and social isolation relative to non-caregivers and Millennials (regardless of caregiver status) reporting higher psychological distress, higher social isolation, and (relative to Baby Boomer and Silent Gen only) lower life meaning. Additionally, Gen X (regardless of caregiver status) reported higher psychological distress relative to older generations, and greater social isolation relative to Silent Gen only. However, there was no significant interaction effect between caregiver status and generation, meaning there was not an exacerbation of caregiving status among younger generations regarding psychological and social health. While there was no detrimental synergy between these factors, it remains that Millennial caregivers appear to be at particular risk for poor mental and social health outcomes as part of two at-risk groups: Millennial generation and caregivers.
Examining the caregiver sample alone, Millennial caregivers reported greater psychological distress and social isolation relative to all older generations of caregivers. Millennial caregivers comprise 25% of all family caregivers in the United States, with the number of Millennial caregivers expected to grow exponentially in coming decades as their parents and siblings age (National Alliance for Caregiving and AARP, 2020). This particular cohort of caregivers faces significant psychological and social challenges given changing family size and reproductive rates, and the unique sociodemographic makeup of this generation of caregivers relative to prior cohorts. Specifically, Millennial caregivers face greater family caregiving demands relative to prior caregiving generations due to shrinking family size, leaving less siblings and children to share the caregiving burden of older relatives (Redfoot et al., 2013). In comparison to older generations of caregivers, Millennial caregivers are more racially/ethnically diverse, are more often male, have more sexual/gender minority individuals, and are less financially secure than older caregiving generations (Flinn, 2018). Increased representation in historically disadvantaged subgroups may render this cohort of caregivers vulnerable to poor mental and social health outcomes.
Although Gen X caregivers in this study reported lower psychological distress compared to Millennial caregivers, they did report greater psychological distress compared to Baby Boomer counterparts. In general, adults in Gen X tend to have greater financial wellbeing relative to Millennials (Shobba & Kumar, 2020), which may help explain greater psychological wellbeing among Gen X caregivers relative to Millennials. By contrast, Gen X caregivers (aged 42–57 at time of data collection) may be more distressed compared to Baby Boomer caregivers (aged 58–76) due to the greater likelihood of Gen Xers having children in the home and working for income (leading to higher time scarcity) during the life cycle phase at time of data collection relative to Baby Boomers.
Despite this clear elevated risk of psychological distress among younger generations, little research has been conducted to understand the efficacy, use, or reach of existing caregiver interventions with younger cohorts of caregivers, particularly Millennials (Hebdon et al., 2022). As such, it is imperative that interventions are developed, tailored, and/or tested with this rapidly expanding group of caregivers. As an effective, low-cost, and highly scalable way to deliver psychosocial support, digital health interventions hold significant promise for supporting Millennial caregivers given their status as digital natives (Fry, 2019; Gallagher et al., 2024). Fully automated Internet-based interventions that do not require the involvement of healthcare providers or peers are a particularly cost-efficient way to deliver support, and caregivers have expressed the flexibility of these programs make them easily integrated into their hectic schedules (Shaffer et al., 2024). While these benefits stem from the lack of input needed from other people, this characteristic fails to address (or likely improve) caregivers’ social isolation. Balancing the need for connection with others against program feasibility will need to be carefully considered in the intervention development process for Millennial caregivers (Hebdon et al., 2023).
There are limitations to this analysis that should be considered when interpreting findings. The HINTS six survey only included three self-reported metrics of mental and social health, limiting our investigation to these areas. Additionally, previous data suggested that nearly half of Millennial caregivers are men (Flinn, 2018), whereas in this sample only 31% of Millennial caregivers were men. As such, this sample of Millennial caregivers may underrepresent men, who historically differentially report mental health distress compared to women (Sigmon et al., 2005). It is possible that some of the generational differences in mental and social health distress may be due to differences in willingness to report negative symptoms and experiences by birth cohort (Twenge, 2015). However, prior research has demonstrated that generational differences persist even when accounting for openness to responding psychometrically (Buecker et al., 2021). Further, rates of suicide and non-suicidal self-injury have also increased among young people over time, which provides behavioral, rather than solely self-report, data for worse psychological distress among young adults (Martínez-Alés et al., 2021; Mercado et al., 2017). This study is also limited by the broad definition of caregiver used in HINTS six methodology (i.e., caring for or making healthcare decisions for an adult with a medical, behavioral, disability or some other condition). With this definition, it is possible that individuals were included within the caregiver group who have limited day-to-day engagement with the care recipient. Psychological distress may vary based on caregiving role and amount of caregiving intensity. Future studies should use a more specific definition of caregiving and characterize the scope, frequency, intensity, and duration of caregiving responsibilities.
In conclusion, younger generations of caregivers, especially Millennials, are high-risk for psychological distress and social isolation relative to relatively older generations of caregivers. Millennial caregivers in particular warrant increased attention from research and policy communities. Without effective support for younger generations of caregivers, we risk leaving this cohort of family carers, who are expected to have increased family caregiving demands compared to prior generations, extremely vulnerable to the mental, physical, functional, and quality of life consequences of caregiving burden (Anderson et al., 2013; Hopps et al., 2017).
Supplemental Material
Supplemental Material - Caregiver Mental Health Across Generations
Supplemental Material for Caregiver Mental Health Across Generations by Virginia T. Gallagher, Ashleigh Patterson, Megan Hebdon, Carol A. Manning, and Kelly M. Shaffer in Journal of Family Issues
Footnotes
Acknowledgments
The data for this publication originated from the Health Information National Trends Survey (HINTS). HINTS was developed by the Health Communication and Informatics Research Branch (HCIRB) of the Division of Cancer Control and Population Sciences (DCCPS) as an outcome of the National Cancer Institute’s Extraordinary Opportunity in Cancer Communications.
Ethical Considerations
The HINTS six general population survey was designated “exempt research” under 45 CFR 46.104 and approved by the Westat IRB on May 10, 2021 (Project # 6632.03.51), with a subsequent amendment approved on November 24, 2021 (Amendment ID #3597). HINTS six also received a “Not Human Subjects Research” determination from the NIH Office of IRB Operations on August 16, 2021 (iRIS reference number: 562,715).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The HINTS 6 was sponsored by the National Cancer Institute, Food and Drug Administration (FDA), and ONC (Office of the National Coordinator for Health Information Technology). The authors were not involved in data collection and are not affiliated with the sponsor organizations. Virginia T. Gallagher is an iTHRIV Scholar. The iTHRIV Scholars Program is supported in part by the National Center for Advancing Translational Sciences of the National Institutes of Health under Award Numbers UL1TR003015 and KL2TR003016, the UVA Brain Institute, and the UVA Department of Neurology. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data from the Health Information National Trends Survey is available from https://hints.cancer.gov (Winston, 2021).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
