Abstract
What does it mean to “embody” paradox? In this paper, we adopt a literal interpretation of this question, examining how physical bodies experience, enact, and respond to knotted paradoxical tensions within the context of interpersonal and structural power relationships. We draw on a qualitative study of self-employed, community midwives (N = 47) whom we interviewed jointly with their family members (N = 51). Our findings paint a rich picture of how midwives experience knotted tensions through embodied polarities of presence–absence and energy–fatigue. We also elucidate how paradox knotting and power relations combine to transform midwives’ experiences of embodied tensions into a restrictive “triple bind,” where physical depletion adds a “third dimension” of material constraint to the interpersonal and structural constraints that characterize double binds. We detail three response patterns midwives use in attempting to navigate the triple bind, highlighting both the importance and limits of interpersonal support and gendered role negotiations. Our work advances understanding of paradox as a non-rational, embodied phenomenon, the navigation of which may require radical systemic change.
Keywords
Introduction
We are the advocate for the pregnant woman and the pregnant woman’s body, and the pregnant woman’s informed choice and consent. It’s such a big thing that’s going on in her life and with her body, so you make peace with it in your head because you are doing something so important, and I think you are fully aware of all the sacrifices that come with it. Nichole, former LMC midwife I don’t know if I would still want to be doing this when I’m 60. I don’t know if my body would cope with it. Like, I’m 43 now and I feel like my body’s starting to fall apart. But then I also can’t see myself doing anything else. So, yeah, I kind of feel like I’m stuck in it, but I don’t know how that’s gonna look, like, if I’m gonna be able to maintain my current workload. Samantha, current LMC midwife
Organizational paradox scholarship has burgeoned in the past two decades with the recognition that seemingly intractable tensions can be navigated constructively using a both/and approach (Lewis & Smith, 2022). This approach requires that organizational actors embrace contradictory elements as inherently interrelated, oscillating between competing goals and demands (known as paradox “poles”) to address both while recognizing each as requiring distinct strategies and actions (Seidemann, 2024). Often termed “both/and thinking” (Smith & Lewis, 2022), this strategic, predominantly cognitive approach can be used to navigate a range of paradoxical tensions, including exploration–exploitation (Andriopoulos & Lewis, 2009), commercial–social (Sharma & Bansal, 2017), and differentiation–integration (Tuckermann, 2019).
However, not all paradoxes can be navigated using a cognitively based both/and approach. Recent scholarship has problematized the “hegemony” of both/and thinking in paradox studies (Seidemann, 2024, p. 11), noting that paradox theory could become prematurely institutionalized—a victim of its own success (Pina e Cunha & Putnam, 2019)—if cognitive and rational approaches continue to prevail. In turn, heterodox voices have initiated research examining: the role of power dynamics in shaping and constraining responses to paradox (Berti & Simpson, 2021a; Huq et al., 2017); the interplay among multiple sets of tensions and how it shapes the experience of paradox (Jarzabkowski et al., 2022; Sheep et al., 2017); how navigating paradox can be a practical and emotional exercise, as well as a cognitive and rational one (Jarzabkowski et al., 2017; Pradies, 2023); and why paradox navigation is frequently an interpersonal rather than individual endeavor (Pamphile, 2022).
In this paper, we weave together threads from these sub-streams of paradox scholarship to explore a largely overlooked phenomenon: the role of the physical body in experiencing and responding to paradox. To date, bodies remain conspicuously absent in paradox studies (Heucher et al., 2024), despite it being self-evident that anyone who experiences paradoxical tensions as “feeling states” must have a sentient body (Putnam et al., 2016, p. 68). In part, the oversight might be due to paradox’s origins in the disciplines of philosophy and psychology, where paradox is typically viewed as a highly cerebral phenomenon, defined by its ability to defy logic and rationality (Schad et al., 2016). In the organizational literature, the oversight could stem from the focus of early paradox studies on “disembodied” organizations as their main unit of analysis (Miron-Spektor et al., 2018). Nevertheless, scholars increasingly recognize that paradoxes can manifest as absurd practical situations (Berti & Simpson, 2021a) and materialize in everyday practices (Lê & Bednarek, 2017), implying they must be navigated physically as well as mentally. Therefore, as researchers have recently sought to understand how non-rational phenomena such as emotions (Pradies, 2023) and interpersonal bonds (Pamphile, 2022) influence the experience of paradox, we seek to understand the role of the physical body.
We draw on a qualitative study of community midwives working in New Zealand’s health system, whose voices are represented in our epigraph. We initially interviewed these midwives together with their family members to understand how they balance work and family responsibilities. As our study progressed, it became apparent that midwives contend with two sets of interconnected—or knotted (Sheep et al., 2017)—paradoxical tensions. First, they face work–home care tensions rooted in their competing yet interdependent gendered identities as mothers/wives and midwives. Second, due to their status as self-employed contractors, community midwives experience business–care tensions stemming from the need to provide close and personalized care to birthing women while making sufficient financial returns on the care they provide. As we dug deeper into midwives’ experiences of these knotted tensions, we realized that because midwifery is an inherently physical occupation—requiring bodily presence and energy—midwives’ primary means of experiencing and enacting the tensions is with their bodies. 1 In turn, we focused our subsequent analyses to understand (a) how midwives physically embody knotted tensions in their daily work and home roles; (b) how embodied tensions are enacted and navigated through interpersonal relations with midwives’ family members, coworkers, and clients (birthing women); and (c) how embodied tensions are shaped by dominant social and economic power structures.
Our work contributes in three interrelated ways. First, we elucidate the role of bodies in enacting, experiencing, and responding to paradox. Our findings contrast with the prevailing view of paradoxes as management problems that can be addressed strategically through both/and thinking (Smith & Lewis, 2011). Instead, we demonstrate how paradoxical tensions can be experienced and enacted physically, and how the persistence of embodied paradoxes has enduring physical, emotional, and relational impacts on individuals. Second, our focus on the body extends knowledge of the interconnections between power and paradox knotting (Fairhurst & Putnam, 2023). In particular, we introduce the concept of the “triple bind” to illustrate how bodily limitations create a “third dimension” of material constraint—compounding the relational and structural constraints of double binds—when paradoxes become knotted within a context of asymmetrical power relations. Third, we advance a novel perspective on how to assign “responsibility” for addressing paradoxes (Seidemann, 2024). Specifically, we show how individual-level experiences of paradox can be interpreted as a signal that underlying, systemic causes need addressing (Bednarek & Smith, 2024; Berti & Simpson, 2021b), contrasting the prevailing view that individual actors are responsible for navigating paradoxes (Miron-Spektor et al., 2018).
Theoretical Framing and Motivation
Navigating paradox: Cognitive and non-cognitive approaches
Broadly speaking, paradox scholarship examines tensions—oppositional conflicts between elements that exert a push–pull force on each other and provoke discomfort in those who experience them simultaneously (Putnam et al., 2016). In the past two decades, paradox theory has become an increasingly influential framework for understanding how to navigate tensions (Lewis & Smith, 2022). A key premise of this theory is that some tensions are inherently paradoxical, which is to say actors inevitably experience them as non-resolvable due to persistent interdependence between contradictory elements (Smith & Lewis, 2011). For instance, social enterprises experience persistent tension between their conflicting yet inseparable social and commercial missions (Sharma & Bansal, 2017). Due to the irresolvable nature of paradoxical tensions, paradox theory advocates accepting and embracing them with a both/and approach. The dominant way of implementing this approach is cognitively, whether through both/and thinking (Smith & Lewis, 2022), paradoxical frames (Keller et al., 2017), and/or paradox mindset (Miron-Spektor et al., 2018). These cognitive approaches enable actors to view contradictory elements as containing complementary interdependencies, obviating the need to choose between paradox poles and, in turn, generating possibilities for creative action (Lewis & Smith, 2022).
A growing body of research enriches and complicates traditional understandings of paradox navigation as a primarily cognitive achievement by revealing its non-cognitive dimensions (Pamphile, 2022; Pina e Cunha & Putnam, 2019; Pradies, 2023). Two recent studies exemplify this emerging perspective. Pradies (2023) developed an emotionally informed model of navigating paradoxes. Noting that researchers have long acknowledged how paradoxes trigger emotions, her study of veterinarians facing a business–care paradox illustrates how emotions can also help individuals work through and learn from paradoxes. Pamphile (2022) focused on the interpersonal dimensions of paradox navigation. She studied grantmakers who drew on extra-organizational peer support to protect and navigate a business–society paradox; this support was critical because senior leaders within grantmakers’ organizations failed to recognize both poles as equally important. Such studies emphasize the limitations of cognitive approaches to paradox navigation, showing that actors cannot always work through paradoxes simply by breaking down false dichotomies and reconciling contradictory elements mentally.
However, despite increasing recognition of paradox’s non-cognitive dimensions, researchers have yet to empirically examine how physical bodies experience paradox. This oversight is perhaps surprising given that cognition, emotions, and relationships come together in the physical bodies of individuals (Fairhurst & Putnam, 2023). The metaphors scholars use to describe paradoxical tensions hint at their embodied nature. For example, “paralysis”—a commonly described reaction to paradox (Lewis, 2000)—is a physical state that originates in the central nervous system but also affects the body’s periphery. Feeling “torn” between competing demands (Pradies, 2023, p. 521) implies a quasi-physical, bodily sensation. Yet, while such language hints at the centrality of bodies in the experience of paradox, researchers have barely scratched the surface of this potentially rich area for exploration (Heucher et al., 2024).
Fairhurst and Putnam’s (2023) conceptual work suggests that bodily reactions and body discourses shape how individuals make sense of paradox through narrative. When paradoxes are experienced in conditions characterized by restrictive “power-over” dynamics, negative bodily impacts can symptomize individuals’ lack of agency (Fairhurst & Putnam, 2023). Meanwhile, Michel (2011) shows how bankers neglect their bodies while experiencing the autonomy paradox, illustrating the “side effects” of paradox on bodies. Both these studies hint at the body’s crucial role in the experience of paradox. However, neither study explicitly examines how persistent and interdependent contradictions are enacted, experienced, and potentially even navigated through bodily actions.
Power relations and paradox knotting
Researchers increasingly recognize that traditional formulations of paradox theory underplay two key features of the world in which paradoxes are experienced: power relations and paradox knotting (Berti & Simpson, 2021a; Seidemann, 2024). First, paradox theory has been criticized for ignoring how power relations shape and constrain responses to paradox (Berti & Simpson, 2021a). Power relations refer to dynamic, perpetually negotiated social configurations that differentially shape individuals’ ability to act—or influence others to act—in accordance with their will (Fairhurst & Putnam, 2023). Conceptual research highlights how structural and interpersonal power disparities force actors into pragmatic paradoxes and double binds (Berti & Simpson, 2021a; Putnam & Ashcraft, 2017)— “pathological” situations where both/and thinking has no generative potential (Berti & Pina e Cunha, 2023, p. 875). Recent empirical studies support this view, highlighting how pathological paradoxes often arise in the context of nested power relationships (e.g., Greenslade-Yeats et al., 2026). Studies also show how imbalanced power structures can block attempts to constructively engage underlying paradoxes, spawning new tensions that lead to failure in managing paradox (Amaral et al., 2025).
Such research echoes a wider body of scholarship showing how paradoxical binds are often embedded in long-standing social and organizational power structures (e.g., Kark et al., 2024; Padavic et al., 2020). A key stream of this literature focusses on gendered double binds (Putnam & Ashcraft, 2017), which arise in contexts governed by oppressive power relations and manifest when making a logical or consistent choice becomes impossible for women (or another disadvantaged gender group) because all available options result in negative outcomes. For example, in managerial assessment centers, women who do not act assertively typically miss out on career progression opportunities for failing to display the necessary attributes; yet, at the same time, women who do act assertively are not promoted, either, because their behavior defies gendered expectations of femininity (Kark et al., 2024).
Paradox knotting is another expanding focus with the potential to complicate traditional formulations of paradox theory (Fairhurst & Putnam, 2023). Paradox knots are groups of tensions that must be addressed concurrently due to their interrelatedness (Sheep et al., 2017). Early research on types of tensions (e.g., performing, belonging, organizing) revealed that multiple, interwoven tensions frequently affect actors simultaneously (Lüscher & Lewis, 2008). More recently, researchers have examined knotting as a processual phenomenon occurring through discursive and interactional practices (Jarzabkowski et al., 2022; Sheep et al., 2017). Sheep et al. (2017) found that multiple tensions not only pervade organizational members’ discourse, but that these tensions can be mutually amplifying or attenuating depending on how they are constructed through communicative processes. Jarzabkowski et al. (2022) built on discourse-focused work by revealing the interactional processes involved in tensional (re)knotting, highlighting how these processes help maintain order (dynamic equilibrium) in complex social systems over time.
Yet, despite progress in understanding how power relations and knotting influence actors’ experiences of paradox independently, only limited insights are available regarding how they do so in combination (Greenslade-Yeats et al., 2026). This lack of attention leaves important questions unanswered regarding, for example, the role of paradox knotting in reinforcing—or destabilizing—imbalanced power relationships. If paradox knotting can help maintain order in complex social systems that achieve desirable goals (Jarzabkowski et al., 2022), can it do the same in systems that enforce oppressive social orders? Moreover, prior studies on knotting implicitly assume that this process occurs within the control of focal actors (Jarzabkowski et al., 2022; Sheep et al., 2017), ignoring the possibility that power relations may be responsible for knotting paradoxes beyond the control of such actors. In sum, examining the connections between power relations and paradox knotting has the potential to enrich understanding of the complexities of paradox navigation.
Research question of the present study
Our literature review shows that more research is needed to understand (a) the role of the body in paradox and (b) the interconnections between power relations and paradox knotting. We contend that these “gaps” cannot be addressed separately, for two reasons. First, the body lacks the cognitive capacities to categorize and compartmentalize discrete sets of tensions in the way minds do (Keller et al., 2017), meaning it is likely to experience multiple sets of (knotted) tensions simultaneously (Fairhurst & Putnam, 2023). Second, bodies represent both sites and targets for the enactment of power relations, especially in gendered contexts (Acker, 1990). Therefore, elucidating the role of the body in paradox necessitates also exploring the interconnections between knotting and power relations. We undertake such an exploration in a gendered care context involving self-employed, community midwives, where we ask: How do midwives physically embody and respond to knotted paradoxical tensions within the constraints of interpersonal and structural power relationships?
Research Methods
Research context
The present study developed as part of an applied research project investigating how community midwives in New Zealand (NZ) balance work and family responsibilities. The goal of our applied research was to develop practical recommendations and inform policy to improve the wellbeing of midwives and their family members. Involving these parties (midwives and families) in the co-creation of research findings and recommendations for policy-oriented solutions was a key methodological principle of the project (Greco et al., 2023).
Midwives are healthcare professionals who provide care and guidance to birthing women and families before, during, and after birth. NZ midwives work across three main settings as part of a universally funded maternity care system: (1) in the community as lead maternity carers (see below); (2) in hospitals or birthing clinics; and (3) in education, research, or regulatory roles. Midwifery has been an autonomous healthcare profession in NZ since 1990. The profession has its own regulatory body, the Midwifery Council of New Zealand, which is governed independently from medicine and nursing.
Professional autonomy is viewed as a key source of pride for NZ midwives, who place a high value on their ability to practice with a degree of independence from the constraints of traditional medical hierarchies (Clemons et al., 2021). Epitomizing this autonomous practice philosophy is the care model we focused on in our research: lead maternity care (LMC) midwifery. This model of care was established in 1996, six years after midwifery gained its status as an autonomous profession. Consequently, LMC midwifery is closely entwined with the notions of professional autonomy and autonomous practice. Most midwives in our study stated that their primary motivations for choosing LMC work were to develop personalized relationships with birthing women and to honor women’s bodies and choices.
Midwives working under the LMC model are known as lead maternity carers (or LMCs) because they play the lead role in facilitating and conducting maternity care. LMC midwives work one-on-one with birthing women (their “clients” 2 ) from early in pregnancy until six weeks after birth. They are based in the community (as opposed to hospitals or clinics), where they have the flexibility to arrange pre- and post-natal client consultations in a location that suits both parties. LMC midwives conduct births in clients’ homes, primary birthing clinics, or hospitals, depending on client preferences. Although LMC midwives sometimes work in hospitals for births and antenatal assessments, they do not work for these facilities as employees. Instead, they are self-employed contractors, paid by the NZ healthcare authorities according to how many care modules they complete for their caseload of clients.
LMCs comprise approximately 31% of NZ’s working population of midwives and are responsible for overseeing approximately 96% of births annually (Midwifery Council of New Zealand, 2023). The remainder of NZ midwives work either as employees in hospitals or birthing clinics (known as “Core” roles; ~50%) or in education, research, and/or regulatory roles (~19%). The accreditation required to work in a clinical midwifery position is standardized across settings, meaning midwives can switch between LMC and Core roles without additional training or education.
Despite its critical role in the health system, LMC midwifery is beset with ongoing recruitment and retention problems. To address the roots of such problems, we examined the impacts of LMC work arrangements on midwives and their families. NZ midwifery is a strongly female-dominated profession; at the time of our empirical research (September 2022 – June 2023), 99.6% of NZ midwives identified as female (Midwifery Council of New Zealand, 2023). Given women’s traditional roles as primary caregivers and homemakers (Padavic et al., 2020), it seemed plausible that the staffing issues affecting LMC midwifery were related to the work–family interface. Accordingly, we chose to conduct a qualitative study using in-depth, joint family interviews as our primary data collection method (Bjørnholt & Farstad, 2014). From a theoretical perspective, including family members in interviews provided insights into how knotted tensions (see Findings) were enacted and navigated through embodied encounters and negotiations.
Participants and data sources
Participants in the study were current or former LMC midwives (N = 47) and their nominated family members (N = 51). After obtaining study approval from our university’s ethics committee, we recruited midwife participants through the New Zealand College of Midwives (NZCOM), the profession’s national support body. Midwife participants were considered eligible if they (a) held an annual midwifery practicing certificate, (b) had past or present experience working as an LMC, and (c) could nominate a family member who willingly consented to participating in a joint interview. We included former LMC midwives in the study (alongside current ones) to understand how former LMCs’ experiences led to them leaving the role.
Regarding midwife participants, 32 were current LMC midwives and 15 were former LMCs. Of the 15 former LMCs, nine had moved into Core, hospital-based roles as employees; four now worked in regulatory, research, or education roles; and two were recently retired. All midwife participants identified as female; they ranged in age from 24 to 68 years (median age = 51 years); and their years of experience in midwifery ranged from one to 44 years (median experience = 14 years). All but one midwife participant had lived with dependent children at some stage while working as an LMC. Regarding family member participants, 28 were a spouse or de facto partner of the midwife, 22 were children of midwives, and one was the mother of the midwife.
Family interviews
Midwives and their family members were interviewed together, either in person (N = 20) or via Zoom (N = 27). In-person interviews took place in participants’ homes. Four interviews involved two family members alongside the midwife. Following a semi-structured guide, interviews lasted 93 minutes on average (range = 70 minutes – 2 hours, 40 minutes) and were digitally recorded. Interviews were transcribed by a professional service, and we sent transcripts to participants for accuracy and confidentiality checks before commencing analysis.
Observational notes
We made observational notes after interviews regarding our impressions of relational dynamics between midwives and their family members. We used these notes to enrich our reflexive understanding of how distinct family units experienced and responded to knotted tensions (see Findings).
Contractual documents
We gathered and read key contractual documents, such as the maternity services contract between LMC midwives and the NZ healthcare authorities (New Zealand Gazette, 2023). These documents supported our understanding of LMC midwives’ contractual obligations and payment terms and, by extension, how and why they experience business–care tensions (see Findings).
Data analysis
We analyzed data using an iterative approach (Miles et al., 2014) whereby we cycled between data and concepts from existing literature to develop theoretical insights. Consistent with prior qualitative research on paradox (e.g., Pamphile, 2022), we started analysis with a relatively amorphous idea of the ultimate theoretical conversation our work would contribute to. We refined our theoretical focus through a series of analytic “moves” (Grodal et al., 2021), each of which was inspired by (a) what we saw as most interesting and surprising about our data when compared to extant theory (Folger & Stein, 2017) and/or (b) suggestions from anonymous reviewers for refining our contributions. This meandering process of data analysis involved many false starts and unexpected dead ends. To simplify the process for readers, we describe four key “moves” that produced our eventual findings.
Descriptive coding
We began analysis by coding the entire dataset line-by-line to develop descriptive themes. The aim of descriptive coding was to understand participants’ experiences in their own words (Miles et al., 2014). We achieved this by developing a coding framework which we applied iteratively to subsets of data (King, 2012). First, all authors read a subset of transcripts and noted potential codes and themes. The first author then collated these notes to develop an initial coding template, which we uploaded to NVivo along with all interview transcripts. We coded five transcripts at a time, updating the coding framework after each subset by adding, removing, or collapsing codes and themes, until we had coded the entire dataset.
Pattern coding
We conducted pattern coding to surface themes with the potential to yield theoretical insights (Miles et al., 2014). During pattern coding—which took place over multiple rounds—we asked “questions” about the relationships between descriptive themes and codes, thus identifying theoretically interesting puzzles (Grodal et al., 2021). For example, having noticed overlaps between the themes gendered profession, motherhood, and gendered work–home tensions, we asked: How are midwives’ gendered identities as midwives and mothers/wives interconnected, and how do interdependencies between these identities generate tensions that midwives embody in their daily lives? We iteratively reconfigured our coding framework multiple times to interpret the data in line with such questions (Grodal et al., 2021). These reconfigurations involved developing new coding categories, merging others (Grodal et al., 2021), and incorporating concepts from related literature. During the final reconfiguration, and based on feedback from anonymous reviewers, we developed “embodiment of tensions” and “bodily impacts” as central themes. To deepen our understanding of these themes, we incorporated ideas from research on gender identity and power relations (e.g., Putnam & Ashcraft, 2017; Ravenswood & Harris, 2016) and paradox knotting (e.g., Sheep et al., 2017), thus developing coding categories such as “embodiment of gendered role tensions through presence–absence.”
Case summaries
We wrote detailed case summaries to gain a holistic understanding of how midwives experienced tensions within the context of each family unit. These summaries were written as narratives, drawing on observational notes and stories shared in interviews to detail how midwives and their family members experienced and responded to tensions over time and in response to changing interpersonal and structural power dynamics.
Theorization through visual depiction
We used visual depictions to theorize from themes in our data (Pradies et al., 2023). We developed visual depictions by iterating between case summaries, the themes surfaced through pattern coding, and the literature. Visual depictions were particularly appropriate for representing our findings because they enabled us to present themes as dynamic rather than static (Pradies et al., 2023).
Ensuring quality
Throughout the research process, we took steps to ensure the quality of our findings (Tracy, 2010). During the data collection phase, we took guidance from researchers with first-hand experience as LMC midwives to ensure that our questions would resonate with our participants. During analysis, we regularly met for discussions and challenged one another’s interpretations and coding choices. We also sought participants’ feedback on our preliminary findings, ensuring that our interpretations aligned with their experiences (Tracy, 2010). Finally, we kept a detailed audit trail of the entire research process (Pratt et al., 2020).
Findings
How midwives physically embody paradoxical tensions
Midwives’ physical embodiment of work–home care tensions
We found that midwives’ experiences of embodied paradox center around a persistent and interdependent tension in their work and home lives. Figure 1 illustrates this tension, showing that in both the work and home domains, midwives view themselves as carers who tend to put others first. At work, midwives put their clients first; at home, their family members. As one participant stated: “[C]learly, within me there’s a big caring part of my personality that, you know, I validate myself around caring for people” (Roxy, current LMC midwife (C-LMC)). This holistic self-concept as “selfless carers” is expressed in midwives’ interdependent gendered identities as both “good midwives” and “good mothers/wives.” Our participants often discussed how these identities were synergistic for them—implying interdependence—because the values of midwifery are closely aligned with those of motherhood: [J]ust as midwifery changed my parenting, parenting changed my midwifery. I mean, philosophically, I think motherhood’s absolutely paramount to the [midwifery] community and all that, so not only is it important for me to honor these mamas [birthing women], but it’s also important for me to, when I was there, to honor myself as a mother. Anne, C-LMC
Consistent with this notion of dual role interdependence, our participants frequently stated that they chose to become LMC midwives after positive experiences during their own pregnancy and motherhood journeys: I wanted to be an LMC since I had my daughter when I was 17. And I saw my midwife as someone that I respected and looked up to and I wanted to be like that. I wanted to be that person. And so I just found it really interesting, the whole pregnancy and birth and that relationship that LMCs have with women. So I only ever went into midwifery wanting to be an LMC, not working in a hospital or anything like that. Samantha, C-LMC
Echoing Samantha, other participants stated that their mission as LMC midwives was to empower women in their motherhood journeys: “Watching women become mums is why I do midwifery because it’s amazing. . . I very clearly believe that if there is a catalyst for change in a woman’s life, it’s being pregnant” (Beth, former LMC midwife (F-LMC)). Midwives’ family members—especially their daughters—supported this synergistic perspective of midwives’ work and home roles, discussing how their mothers’ midwifery practice had inspired and empowered them in their own lives and bodies: I think I have learnt a lot on a personal level as a woman. Growing up with a midwife mum, I know a lot about my body, I know a lot about the system, and I feel very confident and comfortable with a lot of medical things that maybe some of my friends would have no idea about, but because of my mother, [I do]. Taylor, daughter of Swift, C-LMC
Collectively, these examples suggest that midwives’ work and home roles are inherently interconnected and synergistic. Who they are at work is inseparable from who they are at home. “Motherhood” is a central concept connecting these dual roles. Through their work, midwives empower birthing women to become mothers and, in doing so, they empower themselves as mothers who empower their own family members.
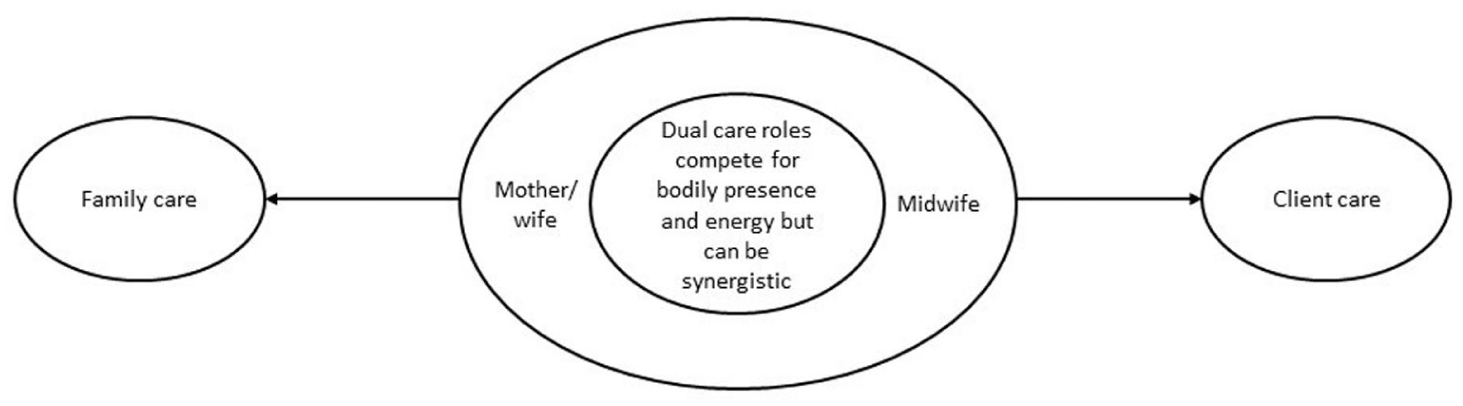
Midwives’ embodiment of work–home care tensions.
However, because of contemporary social organization, midwives often feel forced to treat their roles as separate and competing rather than connected and synergistic. More specifically, midwives’ gendered work and home roles are frequently pitted against each other in a zero-sum trade-off, where time and energy spent caring for clients is seen as detracting from family care responsibilities, and vice versa. In turn, this perceived either/or choice triggers tensions: I feel like I’m letting everybody down. It’s so hard to do a good job and be a good mum, and I’ve not been a good mum because I’m tired; I’m never there for things. I’m not a good wife because poor John has to pick up the pieces so much, and that’s not fair and it’s not fair to make people feel like this. And we work our asses off to make sure that women get what they need, and nobody gives a toss about us; nobody cares about how hard it is for us, and all I ever wanted to do was be a midwife and I did it for love. . . and [now] I feel terrible that I’ve let the kids down so much. Jane, C-LMC
As this quote implies, midwives do not merely perceive work–home care tensions cognitively and emotionally; they experience them as physical states and sensations in their bodies. Our participants reported experiencing tensions as states including absence (“I’m never there for things”), fatigue (“I’m tired”), exhaustion (“I was so tired I couldn’t talk”; Joanne), and stress (“the stress I carry is enormous”; Olivia). They also experience them as quasi-physical sensations such as feeling “torn,” “overstretched,” or “spread too thin.” Moreover, midwives’ bodies are not just “sensors” that perceive paradoxical tensions, but sites in which the tensions are persistently enacted. As illustrated in Figure 1 and captured in the following quotes, this physical embodiment of tensions occurs because midwives’ conflicting yet interdependent care roles both require presence and energy—resources that are inherently limited by physiological and material realities: You [midwife speaking to daughter in the interview] would be there with one of your brothers, and the place was in chaos, and I’d come home and I’d just go – “Don’t talk to me.” I’d shut myself in the lounge or something and I’d say – “I do not want noise, I do not want any. . .” I just needed to switch off from being needed. That’s a hard thing to do as a mother when you’re actually trying to teach and be a role model to women as to how to parent, and doing the exact opposite on the home front. Carrie, F-LMC
I’ve got a really vivid memory of the birth we were talking about where I had gone back and [my youngest son] was still needing to be [breast]fed, of sitting in the old theatre room bawling my eyes out, going – “I can’t give anyone what they need right now.” Yeah, it’s like – I can’t be a great midwife because I’ve got to be there for my kid, and I can’t be a good parent because I’ve got to be there for this woman, and just not feeling like I could do anything well. Debbie, F-LMC
Statements from midwives’ family members captured the same notion of work–home care tensions materializing in bodily limitations of presence and energy: You know how all your studies say that LMC midwifery is really great for women because they have the one-on-one care? I mean, I can pretty easily explain to you why it’s so great. You’re going through this huge change in your life, and you have the opportunity to have someone right there, right by your side; not a parent but a parental role. They’re there to answer your questions. They’re there to support you emotionally, socially, talk you through it. And what happens there is that a [midwife] is able to provide that support for their client, but gaps start to appear, and they’re maybe not able to put all of that energy into their own children if it’s going into their clients. Margaux, daughter of Cate, F-LMC
Midwives also discussed how personal and family life make it difficult to consistently show up with the presence and energy to care for clients: [After separating from my husband] I still needed to turn up to work and I still needed to turn up for those women, and I’d be sitting in the car and I’d be crying and then I’d have to wipe my eyes and put on my big girl knickers and go into a house and do a postnatal visit, or whatever. Cate, F-LMC
In sum, midwives embody a paradoxical tension between their conflicting yet interdependent work and home roles. The tension is enacted in bodily limitations of presence and energy, as recognized by both midwives and their family members. As we show next, these work–home care tensions become knotted with business–care tensions due to the structure and organization of LMC midwifery work, amplifying their embodied expression.
Knotting of embodied work–home care and business–care tensions
Under the LMC midwifery model, midwives must operate as small business owners: “We have to set up our own business. We’re our own administrators. We’ve got to sort out our own software, our own accounts, all that sort of thing” (Linda, C-LMC). At the same time, midwives have a duty of care toward their clients, which they typically internalize to the point that it constitutes an integral part of their identities: “[I]t’s about that journey with women and it just, you know, I think really it has to be in your heart and soul” (Linda). These elements of LMC midwifery create a persistent and interdependent tension between business and care imperatives, which is amplified by the funding structure of LMC midwifery. Dedicating high amounts of time and energy to client care is often at odds with the financial viability of midwives’ business operations because it detracts from their ability to earn additional income by caring for other clients. Yet, providing high-quality client care is essential to the viability of midwives’ business operations given that (a) midwives must attract their own clients and (b) clients “rate” the quality of care provided by specific midwives, which informs other prospective clients’ midwife selection decisions. One midwife captured how this interdependent business–care tension manifests in midwife–client relationships when she stated: “[Y]ou’re trying to balance trust and connection with efficiency and boundaries and getting the job done” (Cate, F-LMC).
We found that midwives’ experiences of business–care tensions become knotted with work–home care tensions in a “tripolar” paradox. Figure 2 illustrates this paradox, showing how work–home and business–care tensions are connected by their shared “client care” pole. An unwavering commitment to client care is deeply embedded in the professional values of midwifery; midwives internalize and embody this commitment to the point that it often shapes their entire self-concept: “I couldn’t imagine me not being a midwife. Like, it’s part of who I am” (Gael, C-LMC). With client care so central to midwives’ identities, it is easy for work obligations to become part of their personal lives. The structure of LMC midwifery encourages this tendency by eroding work–home boundaries. For instance, due to midwives’ on-call obligations to clients (which they must honor to get paid), midwives frequently receive and respond to calls and messages from clients while at home: “[We]’d be sitting at the dinner table and she’d take a phone call at the dinner table and continue to talk through whatever was going on in the pre-birthing process as this person’s going into labor while we’re trying to eat dinner” (Lilly, daughter of Carrie, F-LMC). In turn, “client care” connects work–home and business–care tensions in a configuration that creates an additional tension between midwives’ family care responsibilities and business imperatives (“family care–business tensions”; see Figure 2). For example, the workload of client care that midwives assume to remain financially viable detracts from the time and energy they have for their families, as do business-related tasks such as billing, documentation, and addressing client queries. At the same time, the financial returns of midwives’ business operations enable them to support their families financially, implying interdependence between family care and business imperatives.
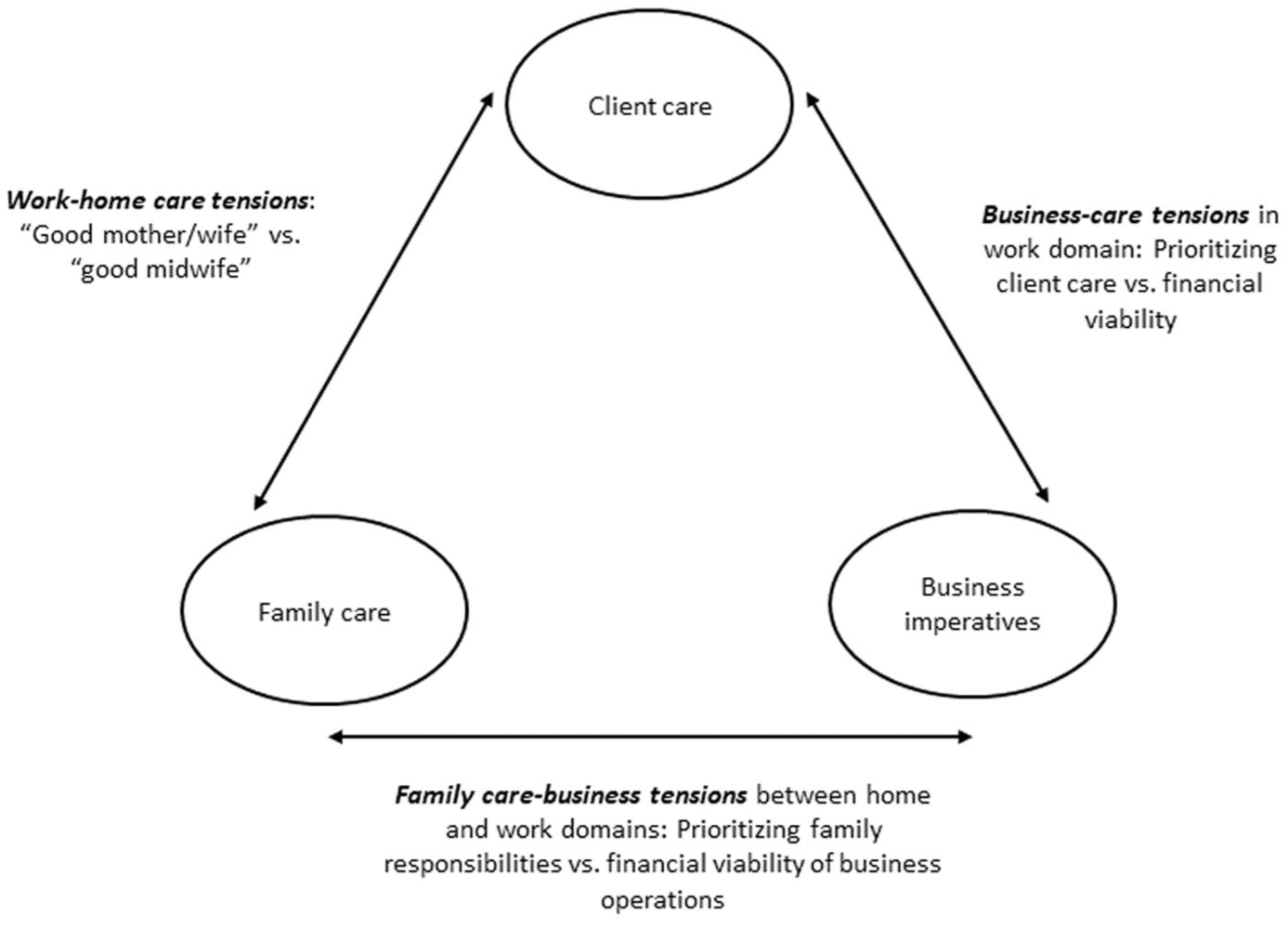
Tensional knotting produces tripolar paradox.
The configuration of paradox poles represented in Figure 2 means that midwives must attend to three sets of interconnected tensions concurrently. Our data suggest that these tensions are often mutually amplifying. For example, the following quote illustrates how family care–business tensions amplify business–care tensions: When we’re trying to earn a living and support a family, you can’t be doing all of the [care-related] things because how much we get paid is per woman; the more women you take, the more you get paid. But if we’re doing every little piece of their care, it makes it really difficult. Sarah, C-LMC
The data also show how midwives simultaneously experience and enact all three knotted tensions with their bodies, creating an immense physical burden. For instance, a former LMC midwife described a typical scenario (for her) in which her body was stretched between client care obligations, family care obligations, and business imperatives: Examples are, you come back after 28 hours up at the hospital, really hard birth, you’ve had no sleep for days, and I used to be fully pregnant at that stage as well. I’d come home and then it would be like – “What’s for dinner?” And all the kids would be there. While the kids are being looked after by my partner, and I owned the house, I paid all the bills, I owned all the vehicles as well, so it was difficult because then I was like – There’s no washing being done and no groceries being bought; no meals had been planned, the kids have had toast or whatever every day. Sometimes if they were little, they might be a bit constipated. . . So, I might come home after that 28 hours, fully pregnant, but I still had to breastfeed my other baby and be up every three hours at night, and waiting on another birth. My partners haven’t been that understanding of that, and they still want their needs met, so they still want sex, or – “You don’t seem to have as much energy,” or, “Why do you have to do that paperwork now, can’t you leave it?” It’s like – “I can’t leave it.” Or – “Do you have to work today?” It’s like – “Well, that baby that I delivered the other night is now due a blood test, so I have to go.” Bella, F-LMC
This quote hints at another important role of “the body” in midwives’ experiences of knotted tensions. Midwives not only feel paradoxical tensions as embodied states and enact them with their bodies; they also experience the tensions as being shaped by the pull of other physical bodies. For example, as implied in Bella’s quote, the timing, duration, and intensity of LMC midwives’ client care responsibilities are influenced by the physiological realities of pregnancy and birth; midwives typically have no control over when clients go into labor, and they have little control over how long births last. Likewise, family care responsibilities are influenced by bodily processes and drives (e.g., constipation, breastfeeding, libido). The two “care” poles in the paradox knot thus exert a “bodily pull” on midwives that business imperatives do not.
Often, LMC midwives accept the tensions arising from the material constraints of bodies because they view them as inevitable outcomes of physiological processes: From what I saw, Mum would come home after a birth and she’d be like – “You should have seen. . . blah blah blah blah blah; this happened and this happened.” So she’d tell me all about the birth and how much she loved it. She would never come home and be like – “That was so long.” It was always like – “Oh!” Chelsea, daughter of Debbie, F-LMC
Honoring such processes aligns with midwives’ self-concepts as experts in—and advocates for—normal, physiological approaches to pregnancy and birth: We’re experts in straightforward, normal pregnancies and maintaining that, and then experts at, I suppose, diagnosing deviations from normal or when complexity arises. . . For me, what I enjoy about [the LMC model] it is that if a woman really wants to be supported in her pregnancy, I can choose to do that with all of the clinical details of that being known to me. For example, if somebody said – “It’s my first baby, the baby’s breach, I want to have the baby at home” – I can do that for her. If I was an employed midwife in [a hospital] – “No, we don’t support home births in our region” – that woman’s then left without an option, and that sovereignty to choose her care is really important, and being able to support her to do it. Lynn, C-LMC
However, because of paradox knotting, midwives’ attempts to navigate embodied tensions are influenced not only by material constraints of others’ bodies but by the social organization of midwives’ work and home roles. As we show next, this social organization involves a complex configuration of interpersonal and structural power relationships.
Caught in a “triple bind”
Figure 3 depicts the configuration of power relationships experienced by midwives in our study, showing how it puts them in a “triple bind”—a situation where midwives’ bodies are “bound” to three distinct poles that they experience as mutually incompatible due to prevailing power relationships. We label this situation a triple bind because the embodied nature of the constituent paradoxes creates a “third dimension” of material constraint (adding to interpersonal and structural constraints), which stems from the physiological realities and limits of bodies. As discussed later, this dimension of material constraint compounds the constraints of power relationships described in this subsection.
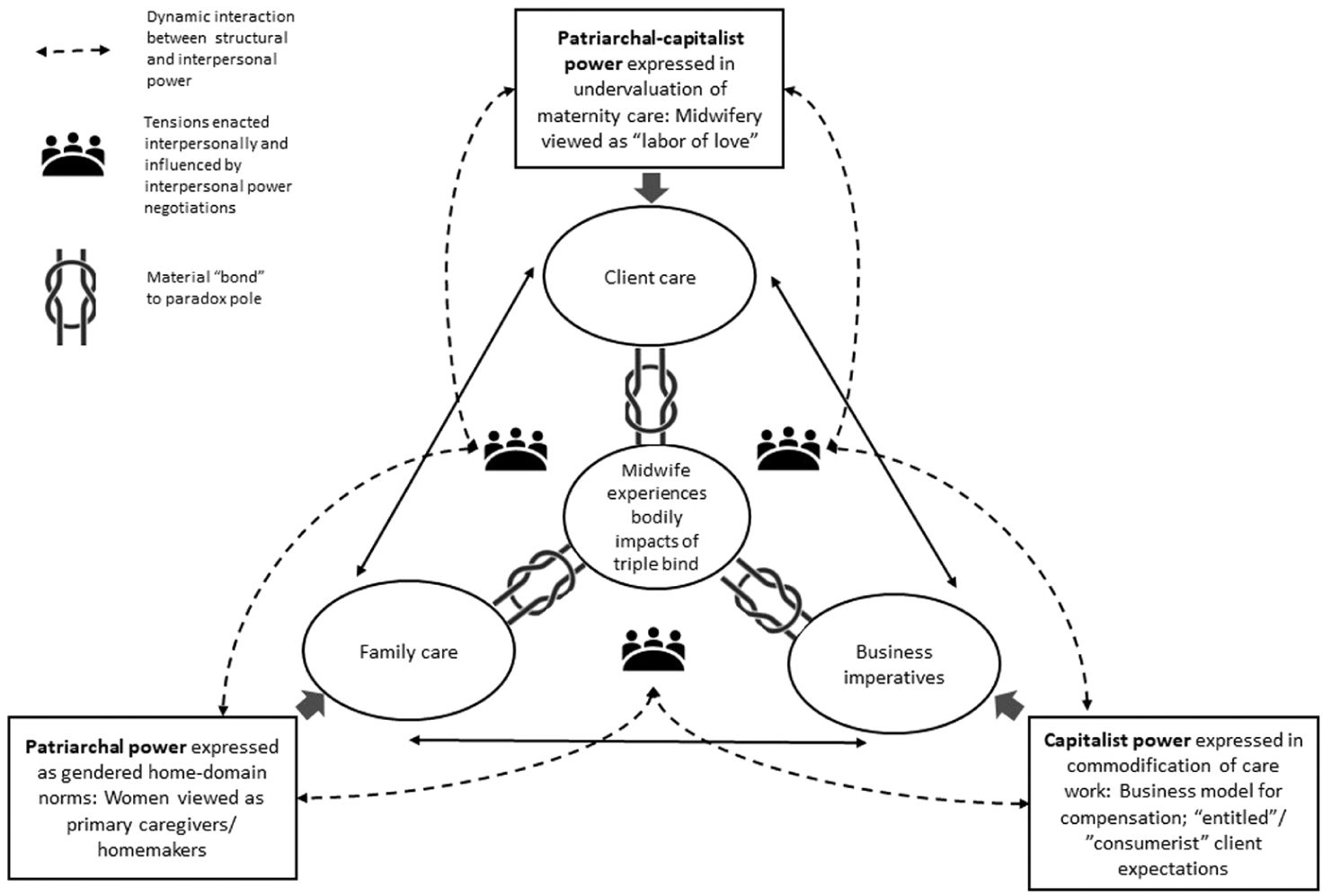
How interpersonal and structural power relations configure embodied, knotted tensions as a triple bind.
As noted, midwives embody knotted paradoxical tensions in their attempts to navigate conflicts among three interdependent roles: “client carer,” “family carer,” and “self-employed business operator” (see Figure 2). Midwives enact these roles and experience the bodily limitations associated with them in interactions with family members and clients (see Figure 3). Accordingly, midwives’ experiences of embodied tensions involve a relational negotiation with non-focal actors who can influence whether midwives experience tensions as navigable or debilitating. For example, one midwife described how her husband’s unwillingness to support her with family care responsibilities led to a debilitating breakdown during a family vacation: We decided to plan a trip to a [tropical destination] because we had the money, and I just spent the whole time there in a week-long panic attack, basically. . . And I think part of what contributed to that is – we talked a little bit about gender roles and stuff at home and housework and all that sort of stuff. When I was working full-time being the main breadwinner, I still was doing all of those things like – “Who’s got this at school, who needs to take this to school, where’s this person being picked up?” I was still doing all the mum stuff on top of the full-time working stuff. Sarah, C-LMC
Midwives recognized how such interpersonal power dynamics are entrenched in broader social structures of patriarchal power (see Figure 3). These structures create gendered behavioral expectations, implying that to be “good mothers,” midwives must take the lead role in caring for children: I think there’s always a bit of sexism that exists as well. No matter what, there’s always a thought that because I’m the female in the relationship I should be the primary caregiver, and we kind of joke about it but sometimes it’s not that funny. No matter how many times we say – “Look, you’re better to call Gary or you’re better to contact him during the day for things with the kids” – they just don’t listen, and it always comes to the mum. Sheila, C-LMC
As these examples suggest, midwives’ experiences of work–home care tensions are frequently embedded in mutually reinforcing interpersonal and structural power relations that determine how midwives “should” use their bodies (e.g., dictating that they always be present for children). Although the examples refer to interpersonal interactions and power relationships that amplify work–home care tensions, midwives can also negotiate gender role shifts with family members that challenge prevailing norms and, in turn, alleviate work–home care tensions (see later subsection on Response Patterns).
As depicted in Figure 3, midwives’ experiences of business–care and family care–business tensions are also influenced by dynamic interactions between interpersonal and structural power. More specifically, business–care tensions are shaped by interactions between clients’ interpersonal “power over” midwives and the patriarchal-capitalist structures underpinning that power. Midwives discussed how a key challenge they face is clients’ reluctance to treat them as professionals: We find women treat midwives a lot different to other health professionals, and it’s almost like they expect you to be their mother, their friend kind of thing, rather than just a [healthcare] professional. Carmen, F-LMC
This de-professionalizing treatment makes it difficult for midwives to balance business and care imperatives because time spent acting like “mother figures” or “friends” detracts from the time they have available to increase financial returns by caring for other clients. In turn, the inability to balance business–care tensions undercuts midwives’ ability to navigate family care–business tensions. Specifically, when families do not see an adequate financial return on midwives’ work, they question whether midwifery is “worth” the time midwives spend away from their home-domain care responsibilities: “It’s why I would rather you [speaking to midwife] walked away from it two years ago, because it’s pointless, it’s ridiculous, absolutely ridiculous. No financial gain, no support, why do you do it? And [speaking to interviewer] she does it because she has a love for the job” (Sam, husband of Lynn, C-LMC).
Although midwives in our study frequently expressed resentment and frustration toward clients who expect them to be “mother figures” or “friends,” they also stated that developing close and personalized relationships with birthing women is among the most rewarding aspects of LMC midwifery. Our analysis suggests that this contradiction arises from inconsistencies between the nature of maternity care work and the patriarchal-capitalist power structures that govern how such work is organized and compensated. Capitalist power structures tend to devalue care work because it is inherently relational, with benefits that are hard to measure in economic terms. Moreover, caring professions such as midwifery are staffed mostly by women. Accordingly, patriarchy and capitalism join forces in the devaluation of maternity care work: I think it’s to do with it’s a woman dominated field. I really think it’s part of that whole, you know, the pay disparity. I think we’re not viewed as professionals in the same way because we’re women and we do that touchy-feely midwifery stuff, which is all about, you know, should come from [us] being nice people. Cassandra, current LMC midwife
The societal devaluation of maternity care gives rise to a widespread view that midwifery is a “labor of love”—something done for intrinsic rewards rather than financial gains. Midwives often internalize this view: “For me it’s not about the money” (Linda, C-LMC). Yet, at the same time, LMC midwives must operate like business owners to make a living from the care they provide. Midwifery is thus subjected to a capitalist economic logic that treats care like a commodity. For example, according to the LMC payment schedule, pre-natal consultations are valued at ~$1,175; a birth is “worth” ~$1,500; and post-natal visits generate ~$650 in revenue (New Zealand Gazette, 2023). Midwives often resist the commodification of maternity care because it conflicts with their values: “It’s all very well to talk about it from a business model point of view, but it’s also like, you can’t put a price on a woman who’s really, really empowered by a really good birth and transition to motherhood” (Cate, F-LMC). However, because prevailing socio-economic power structures dictate how LMC work is organized and compensated, midwives have no choice but to treat clients (at least in part) as a means of getting paid.
This argument suggests that midwives’ resentment and frustration over de-professionalizing treatment by clients stem not from the treatment per se but from how midwife–client relationships are situated in a system of patriarchal-capitalist power. Our data indicate that the systemic commodification of maternity care filters down into how clients treat midwives, encouraging “entitled” and “consumerist” attitudes: “That’s sort of another aspect to what we mean by ‘entitled,’ it’s like – ‘You work for me, so you’ve got to do this, this, and this’” (Carmen, F-LMC). In turn, because LMC midwives depend on attracting clients to stay in business, they often feel powerless to push back against overly demanding clients: “If you come across as rude then [clients] are straight on their computer. . . they get on social media and they slag you off. . . and that’s your reputation” (Lagatha, C-LMC).
Yet, according to our analysis, clients’ perceived power over midwives is significantly less influential than another asymmetrical power relationship affecting their ability to balance care and business imperatives. Midwives are not paid directly by clients but by the NZ healthcare authorities according to fixed care modules. Midwives find this payment structure problematic because, although they are self-employed business owners operating in a “care market,” they cannot set their own pay rates: We might claim in modules but all our income comes from the Ministry of Health. They set the fees. They set the work structure. We don’t. We can’t decide to increase our charges to meet the actual cost of living. We don’t have the capacity that other self-employed professions do, where they can charge to meet the cost of running their business. Cassandra, C-LMC
Midwives’ inability to set their own pay rates precludes synergies when trying to balance financial returns with clients’ needs. For example, it means highly experienced midwives cannot charge more for higher quality care. Instead, if midwives want to increase their income, they must increase the number of women they care for (their caseload): “In order to make the sort of money that you think you should be making as a professional who’s running your own business and all those things, you end up doing these insane amounts of work” (Alan, husband of Leesa, F-LMC). Yet, midwives suggested increasing one’s caseload typically undermines quality of care: “[Some] LMCs are doing between 10 and 20 [births] a month. How the hell do you do that?! I don’t understand. You can’t give good care if you do that. . . It’s hard enough to give good care when you’ve got four a month” (Jane, C-LMC). Thus, the LMC midwifery payment model is structured in a way that makes midwives feel forced to “choose between” care and business imperatives.
In sum, interpersonal and structural power relations interact dynamically to constrain midwives’ ability to navigate knotted paradoxes, as in a double bind. Compounding these interpersonal and structural constraints is the embodied nature of demands on midwives, with the three poles of the paradox knot all requiring bodily presence and energy. Client care pulls midwives’ bodies toward quality interactions with pregnant women and families; family care pulls them to spend time and energy on their own family members; and business imperatives pull them toward maximizing client numbers and dedicating time and energy to business tasks. In turn, the combination of interpersonal, structural, and material constraints creates a triple bind. The visual depictions of “bindings” in Figure 3 represent this notion, showing how the physical reality of paradoxical demands compounds the impacts of power-constrained choices through physical depletion. For example, the embodied demands of providing both quality and quantity of care—which midwives must do to navigate business–care tensions without compromising their values—encourages midwives to overextend themselves physically. In turn, this physical depletion compounds the embodied demands of trying to be both “good mothers/wives” and “good midwives.” As one midwife stated: “There isn’t space or capacity in this job to maintain your own cares and your own needs, and I think that adds to family pressure because they’re worrying about you” (Lagatha, C-LMC).
Due to the additional layer of material constraint, the triple bind has serious consequences for midwives’ health. Participants reported bodily impacts including illness (“I did get sick a couple of times, very sick, like got put in hospital a couple of times” – Beth, F-LMC); injury (“I’ve got a chronic back ache. . . I can’t even remember when it started” –Samantha, C-LMC); weight gain and poor metabolic health (I’ve put a lot of weight on” – Lagatha C-LMC); and chronic fatigue and exhaustion (“I’ve been completely exhausted, depleted in different ways” – Rosie, C-LMC). Accordingly, it makes sense that midwives do everything in their power to navigate the triple bind, as we illustrate next.
Response patterns
We identified three main patterns in midwives’ responses to the triple bind. Pattern 1 unfolds within the constraints of the bind, while Patterns 2 and 3 involve a more radical reconfiguration of underlying paradox poles.
Living and working within the constraints of the triple bind
A triple bind suggests a practically inescapable situation, even more difficult to navigate than a double bind. Yet, many of the midwives in our study had long careers as LMCs and also raised families. How did they manage this feat and what were the consequences?
Our data suggest that because midwives experience their triple bind through bodily limitations of presence and energy, they depend primarily on interpersonal support to navigate its constraints. Such support comes from three main sources—midwives’ families, coworkers, and clients—and takes three predominant forms: embodied support, body substitutions, and body free passes. Embodied support is material assistance that helps midwives cope with the conflicting demands of their work and home roles. Family members are typically the ones providing this support to midwives, enabling them to temporarily ignore one paradox pole (e.g., family care responsibilities) to focus on the others: “I will walk out the door and go – ‘Tea [dinner] is nearly ready, you just need to do this, this and this’. . . and he [my husband] just picks up where I leave off” (Maree, C-LMC). In situations where midwives’ bodies are stretched between care and business imperatives, family members may provide embodied support by not only caring for themselves (alleviating work–home care tensions) but by actively assisting midwives to meet both client care and business obligations (such as attending back-to-back births to get paid for client care modules). For example: “Mum would have two back-to-back births, and even when I was still at home we used to drive out to [small town] to drop off food and to make sure she was ok, and bring her blankets or clothes if it was cold” (Poppy, daughter of Lucille, C-LMC).
Body substitutions occur when midwives have somebody “stand in” for them in one of their conflicting roles. LMC midwives often work within self-organized practice groups with a dedicated “backup.” Backups cover periods of short-term leave reciprocally, enabling the other midwife to, for example, attend family occasions without shirking client care obligations. However, because the arrangement is reciprocal, midwives are responsible for their backup’s full caseload of clients when it is their turn to cover. Consequently, short-term alleviation of work–home care tensions is often followed by an amplification of tensions due to workload pressures. Business imperatives ensure that midwives cannot use body substitutions excessively without negative financial repercussions (because they will lose care module fees), emphasizing the tripolar constraints of the paradox knot. Midwives’ family members—especially partners—may also act as body substitutes: “If Lagatha gets called to a birth and the kids are on their own, then I’ve got to drop my arrangement. . . and come home and look after the kids” (Graham, husband of Lagatha, C-LMC). However, without an enduring gender role switch (see Response Pattern 3), this sort of body substitution provides only temporary relief from work–home care tensions. Moreover, we found that the “tone” of body substitutions influences the experiences of associated tensions; if partners are resentful about “standing in” for midwives, their “support” may actually heighten midwives’ feelings of tensions.
Body free passes are permissions granted to midwives by family members or clients, enabling midwives to (temporarily) neglect one of the three paradox poles without it amplifying their feelings of tensions. We found that when body free passes are combined with embodied support and/or body substitutions, they are highly effective at alleviating work–home care tensions in the short term. For example, clients can be understanding that because a midwife has her own family obligations, she will get her backup to attend their birth. Similarly, family members can forgive midwives for neglecting home-domain responsibilities and missing family occasions due to work commitments; or for having no energy and needing to sleep when they get home from work; or for having to spend their evenings on business-related paperwork. One husband captured this kind of forgiveness when he said: I totally respect what she’s doing, and I think all of us are really in the position to do everything we can to support her to do that. Sometimes the house might be messier than any of us can handle but it’s all right, that’s life, we’re not going to die. As far as I know we’ve never left the kids at school and no one’s gone to pick them up, they’re still here so that’s all good. There’s no question there’s been some challenges but you’ve just got to get over it and deal with it. Bob, husband of Sarafina, C-LMC
As this quote suggests, family members are more likely to grant body free passes when they recognize and respect the value of LMC midwifery work. Conversely, they are less likely to grant such passes when they feel midwives are overworked and undervalued as part of an exploitative relationship with the government (see Response Pattern 3). This is especially true when midwives require free body passes regularly and over long periods.
The three forms of interpersonal support just described illustrate the dynamic fluidity of interpersonal power relations and how they influence midwives’ experiences of embodied tensions in short-term cycles. For example, family members and clients might temporarily relinquish their perceived power over midwives by forgiving midwives’ absences or tiredness through body free passes. However, such interpersonal support provides only temporary relief from tensions because it does not reconfigure the underlying power relationships that perpetuate tensions over time. To illustrate, a husband can look after children when a midwife gets called to a birth, and children can forgive her for missing important occasions, yet the midwife still feels guilty because she continues to embody the gendered role of primary caregiver.
Accordingly, we found that while midwives can survive the triple bind with adequate interpersonal support, they rarely thrive within its constraints. For instance, no midwives in our study described feeling “energized” by navigating family care, client care, and business imperatives simultaneously. To the contrary, most felt worn down by the cumulative fatigue and stress of trying to “be everything to everyone” (Samantha, C-LMC). A former LMC midwife captured this notion as follows: I think it was always just trying to juggle; it was always trying to not let anybody down and do the best job I could, and I guess it’s like that analogy of holding a glass of water; you can hold a glass of water out for a period of time without any problem, but the stress of trying to make sure everyone was happy and everyone was covered and catered for, and I didn’t make a mistake at work, I didn’t let anyone down, I always turned up when somebody called – the stress of that was taxing over a period of time. Joanne.
Our data suggest that cumulative fatigue and stress have enduring impacts on midwives. For example, one midwife participant had recently retired from a long career as an LMC midwife (25+ years in LMC) during which she and her husband raised two children. When asked how she balanced the responsibilities of being a mother, a midwife, and a small business operator for so long, she signaled the importance of support from her husband (embodied support, body substitutions) and understanding from her children (body free passes). But she also said: “[It] became an issue that you were exhausting yourself because you were trying to be in three places at once.” When asked how such efforts impacted her personally, she said, “I got older quicker. I got more wrinkles earlier. And yes, there is a lot of guilt.” Other participants described not only physical and emotional impacts similar to these, but a relational toll associated with relying too frequently on support from family members (especially body substitutions and body free passes). Some had broken marriages or grown children who no longer talked to them.
Notably, a shift in the “balance” among paradoxical demands occurs over time for LMC midwives. When children are younger, they require more direct energy from midwives’ bodies, amplifying tensions between family care and client care. As children grow up, they demand more financial support, amplifying family care–business tensions (and, by extension, business–care tensions). Our data suggest LMC midwives are more likely to navigate this dynamic balance “successfully” if they have adequate interpersonal support to survive periods when demands on their bodies are most intense. However, such short-term support does not always protect midwives from long-term physical, emotional, and relational impacts.
Work-domain role shift
We found that midwives who lack the interpersonal support to navigate the demands of their triple bind typically escape its confines through a work-domain role shift. Most commonly, LMC midwives move to hospital-based “Core” roles (see Research Context). This shift reconfigures the underlying paradox knot by removing the “business imperatives” pole, as shown in Figure 4. As employees in hospitals or clinics, midwives are not required to attract their own clients or manage their own finances. Instead, they enjoy a stable (though not necessarily higher) income and benefits including sick pay, annual leave, and retirement fund contributions. However, as explained later, this work role shift typically entails an “integrity sacrifice” because it reintroduces another set of restrictive power relations.
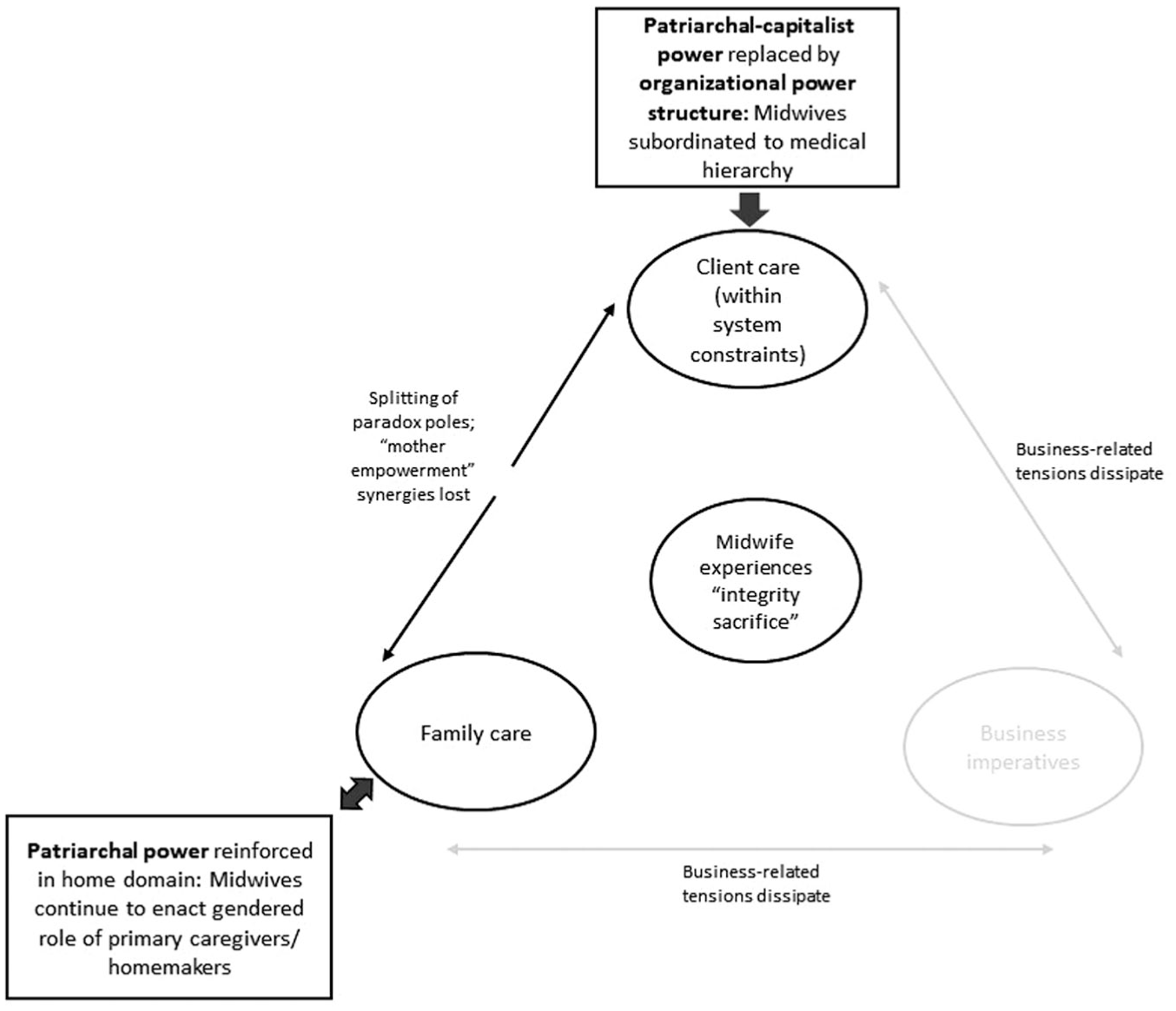
Visual depiction of Response Pattern 2: Work-domain role shift.
In our study, midwives who had shifted into Core roles frequently did so after realizing they could not navigate—or tolerate—the embodied demands of the triple bind. For example, Cate struggled to balance client care against family care and business imperatives. The ensuing tensions were amplified when she separated from her husband, leading to a body breakdown and an eventual exit from the LMC role: I remember one time I was coming out of a virus and then I got food poisoning and it was just awful, and I just knew I wasn’t coping; I knew my body wasn’t coping, I just knew that my body was just going – You can’t do this, this is too hard, this is too much, just the weight of everything, yeah. I actually went to a counsellor to try and work out how I could do my life in a way that was manageable because I loved being an LMC; I adored working with the women, I love the continuity, I love birth. . . . I love it so much and I went to see a therapist because I couldn’t understand how I could manage my life, and it was she who helped me understand I had to leave LMC midwifery. Cate, F-LMC
As illustrated by Cate’s story, midwives who left LMC work for Core roles often did so with a sense of regret. Regrets most often stemmed from losing one-on-one connections with women and the autonomy to honor women’s bodies and choices: “If you become a hospital-based midwife there’s definitely a degree of subordination that happens, that suddenly the midwifery team default to the obstetric opinion” (Lynn, C-LMC).
Our analysis suggests the regrets associated with a work-role shift are due to the loss of potential synergies between two paradox poles—client care and family care—that occurs with the unravelling of the paradox knot. As depicted in Figure 4, shifting into a Core midwifery role removes the “business imperatives” pole, obviating the need for midwives to navigate business–care and family care–business tensions. To an extent, this is beneficial as midwives must no longer contend with the patriarchal-capitalist power structures that can transform these tensions into debilitating either/or choices. However, when they move into the Core system, midwives face hierarchical organizational structures that prevent them from advocating for women’s control over their bodies. Thus, the potential for synergies between family care and client care—such as self- and family empowerment through the empowerment of birthing women—are lost. In turn, work–home care tensions become disconnected, and midwives experience an “integrity sacrifice,” feeling like they’ve lost an integral part of who they are: I’m not fulfilled in a Core role; I don’t even feel like it’s midwifery and it’s splitting off into complex care nursing but there’s no autonomy; it’s very different. I used to get so much internal reward out of the relationships I had with ladies. Bella, F-LMC
Home-domain role reversal
The final response pattern we identified is a home-domain role reversal that midwives negotiate with their partners. In this pattern, partners do not just act as temporary body substitutes but perform longer-term role reversals. As illustrated in Figure 5, such reversals relieve midwives of tensions associated with their gendered body roles as primary caregivers and homemakers. One midwife captured the essence of this approach when she stated: “I would say a midwife needs a wife, and Johan [the midwife’s husband] has been a wife” (Roxy, C-LMC). The husband of a former LMC midwife also described how they enacted a gender role reversal in their household, enabling the midwife to provide for the family as the main breadwinner: Serena was the main income. . . she definitely earned more than me. . . It’s a reverse, I suppose, of a paternalistic arrangement where it’s always the woman’s at home and the man just wanders off and does what he wants and comes back when he’s had enough. This was just the flip of that. So, it’s no different to any other family, it’s just the roles were reversed in this case. Richard, husband of Serena, F-LMC
A home-domain role reversal reconfigures the paradox knot underlying midwives’ triple bind, as shown in Figure 5. Specifically, it removes family care responsibilities requiring bodily presence and energy. Yet, the reversal simultaneously increases financial responsibilities associated with family care. Accordingly, as breadwinners, midwives experience heightened family care–business tensions and, due to paradox knotting, amplified business–care tensions. The crux is that gender role reversals are contingent on midwives earning enough to provide for their family. However, due to the LMC funding structure, LMC midwives can only increase their income by taking on more clients: “My caseload was probably about 100 a year. . . [M]y husband didn’t earn a living, so it meant I was the primary earner, and had a mortgage to pay and all the rest of it” (Olivia, C-LMC). Since increasing one’s caseload typically reduces quality of care, becoming a breadwinner amplifies business–care tensions.
Visual depiction of Response Pattern 3: Home-domain role reversal.
We found that couples who had successfully undertaken a home-domain role reversal generally did so 20+ years ago. Since then, societal changes brought about by neoliberal capitalism have made it increasingly difficult to balance business–care tensions in a way that makes the breadwinner role sustainable for LMC midwives (unless their children are grown up and fully independent). For instance, neoliberal economic policies have increased inequality in NZ, raising the prevalence of mental and physical health issues among clients, and reduced government funding for the healthcare system. In combination, such factors have increased the workload of LMC midwifery while reducing inflation-adjusted financial returns.
In the current environment, midwives trying to navigate their triple bind with a home-domain role reversal end up in a secondary bind that reinforces prevailing patriarchal-capitalist power structures. Negotiating a home-domain role reversal requires that midwives effectively balance business–care tensions. But due to the LMC funding structure, midwives experience this paradoxical tension as an either/or choice. Either they can: (1) take a business-oriented approach toward client care and, in doing so, sacrifice their integrity by tacitly submitting to patriarchal-capitalist power structures that treat care as a lowly valued commodity (an approach that may also have negative business repercussions due to clients’ “ratings” of midwives); or (2) they can sacrifice their bodies by trying to provide both quantity and quality of care: “[You] work 36 hours on the trot without [a break] ‘cause you’re so desperate to make sure that women get the care they need and deserve” (Olivia, C-LMC).
Most midwives in our study were unwilling to treat care as a commodity and instead prioritized their clients’ welfare as a means of resisting capitalist economic logic. Our participants often implied that this resistance was driven by a feminist political agenda: Because it’s women giving birth. We’re 99.9% a female workforce, so we are expected to – Oh well, just have your child, or you’ve got your period that day and you might feel tired. Well, you’re expected to go out and do that and you’re not getting any time off, and we don’t get sick days. So you carry on in your stoic bag because you’re a woman helping another woman, so it makes you even more determined to get through and advocate for them. Lucile, C-LMC
However, our analysis suggests that midwives’ resistance has the paradoxical effect of reinforcing their relative powerlessness in the healthcare system. Midwives recognized how their prioritization of care enables the healthcare authorities to take advantage of them: I think LMC midwifery possibly would’ve collapsed if it was a different type of person or men to be general, you know. No one else would put up with the conditions and the pay and the, yeah, the shit that we put up with if we weren’t nice people and everyone’s worried about their women. Amy, C-LMC
Spouses and partners concurred with these sentiments: As long as you keep enabling the system to take advantage of you [speaking to wife during interview], then in some way you’re actually part of the problem, because you’re enabling the system to take advantage of you, basically. . . I don’t think there’s a silver bullet, but I certainly think there’s a lot of things that happen simply because most of your colleagues and you just want to do right by your [clients]. Dave, husband of Kate, C-LMC
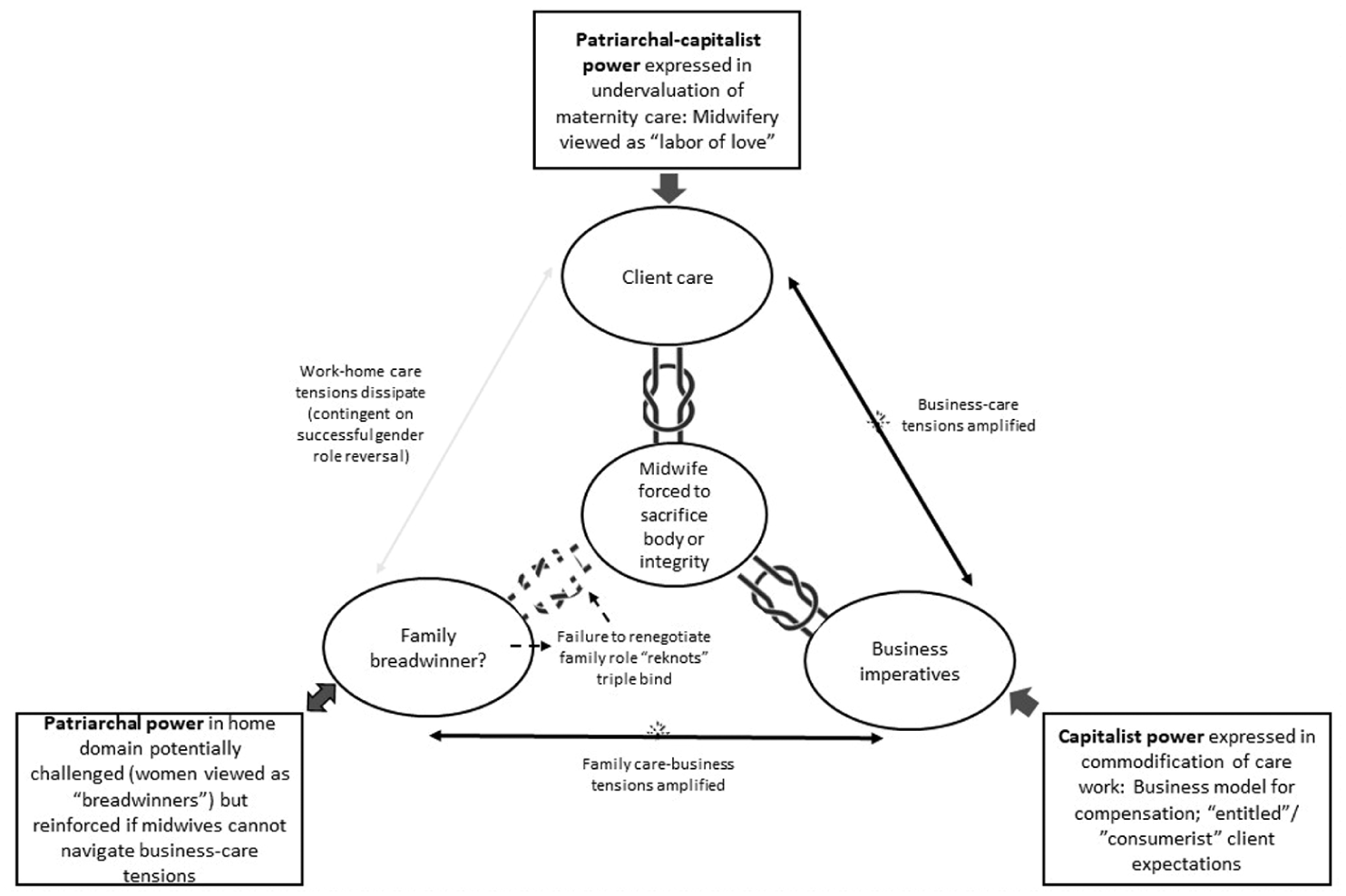
Accordingly, Response Pattern 3 shows how patriarchal-capitalist power structures that influence midwives in the work domain (by simultaneously commodifying and devaluing maternity care) prevent them from challenging patriarchal gender norms at home. Midwives struggle to negotiate gender role reversals with their spouses and partners because, ironically, the latter view LMC midwifery as an undervalued and exploitative work model. In turn, these failed negotiations reproduce the interpersonal power relations midwives were trying to renegotiate, and the triple bind “reknots” around them (see bottom left corner of Figure 5).
Discussion
We examined how midwives physically embody knotted paradoxical tensions within a dynamic web of interpersonal and structural power relationships. In doing so, we advance the literature by weaving together three emergent foci in paradox studies: the role of the body, power relations, and paradox knotting (Fairhurst & Putnam, 2023). Based on our findings, we propose the “triple bind” as a conceptual framework for unifying these foci. Triple binds emerge when imbalanced power relationships and knotted paradoxes combine in a way that creates a third dimension of material constraint on individuals, amplifying interpersonal and structural constraints through physical depletion. Next, we discuss the contributions and implications of this theoretical development for three areas of paradox research.
Contributions and implications
Non-cognitive dimensions of paradox
Our concept of the triple bind advances understanding of the non-cognitive dimensions of paradox navigation. Traditionally, paradox research has emphasized the importance of cognitive approaches such as both/and thinking (Smith & Lewis, 2022), paradoxical frames (Keller et al., 2017), and paradox mindset (Miron-Spektor et al., 2018). Recent research highlights that paradox navigation also entails emotional and relational elements (Pamphile, 2022; Pradies, 2023). Our research takes this non-cognitive perspective a step further by empirically examining the role of the physical body in experiencing, enacting, and responding to paradox. In our study, embodying paradox refers not only to when somebody represents contradictory yet interdependent poles (Bednarek et al., 2017), but to when physical bodies feel and enact paradox through materially constrained polarities such as presence–absence and energy–fatigue. Our empirical exploration of this phenomenon builds on Fairhurst and Putnam’s (2023) conceptual work, elaborating their contention that bodily reactions reflect the power conditions under which paradoxes are experienced.
Our embodied perspective supports the problematization of widespread assumptions regarding the primacy of cognitive approaches in paradox research (Berti & Simpson, 2021a; Seidemann, 2024). Our findings imply that, as delicately balanced physiological systems, bodies face material constraints in ways that cognitive systems do not. In persistently enacting complex, demanding tensions, bodies are subject to enduring physical impacts regardless of how individuals mentally conceive of the relationships among paradox poles. Indeed, the midwives we interviewed often thought of their dual identities (as “mothers/wives” and “midwives”) as interdependent and synergistic. What prevented them from leveraging these synergies were interpersonal, structural, and material constraints embedded in imbalanced power relationships. Consequently, our paper emphasizes that bodies cannot navigate power-constrained paradoxes without material and interpersonal support (Pamphile, 2022), and we illustrate how embodied support, body substitutions, and body free passes help loosen the constraints of the triple bind in short-term cycles. At the same time, our findings highlight the limits of such support to protect against long-term impacts when structural power relations constrain available responses to underlying paradoxes (see Response Patterns 1 and 3).
Our work suggests several directions for further research on the body’s role in paradox. To start, it encourages practice-based scholars to examine how physical bodies construct and enact paradox through everyday actions (Jarzabkowski et al., 2017; Lê & Bednarek, 2017). In our care-focused context, paradoxes were physically enacted in polarities of presence–absence and energy–fatigue. But what polarities are involved in the physical experience of other paradoxes? Our research also suggests that bodies not only enact paradoxical demands but give rise to such demands. We showed how “the pull of other physical bodies” influenced midwives’ experiences of embodied tensions, and how paradox poles materializing in this pull (e.g., family care, client care) were internally more compelling than “disembodied” poles (e.g., business imperatives). This finding resonates with Pradies’ (2023) work showing how veterinarians have stronger emotional identification with care imperatives than business ones. Future research could more explicitly and comprehensively examine how bodies and emotions “work together” in paradox navigation. One might assume that bodies and emotions are close collaborators—but does this assumption hold true? For example, can emotional connections encourage bodies to navigate paradoxes in ways that undermine bodily health? And can the material constraints of other bodies encourage individuals to disconnect emotionally from those bodies? Lastly, although we focused on what Berti and Pina e Cunha (2023) would call a “pathological” paradox—governed by asymmetrical power relations—our work invites scholars to examine how bodies experience more generative paradoxes. For example, when leaders adopt a both/and strategy to engage paradox, how do the physical actions of implementing that strategy impact the bodies of organizational members? Both/and approaches to paradox are seen as a source of creative energy (Miron-Spektor et al., 2018)—but do bodily limitations affect individuals’ ability to remain energized by paradox over time?
Interconnections between power and paradox knotting
Our second area of contribution is to research on the interconnections between power and paradox knotting. Prior research shows that power relations can shape individuals’ interpretations of the interplay among multiple sets of tensions (Greenslade-Yeats et al., 2026) and that power structures can spawn new sets of tensions by blocking attempts to navigate underlying paradoxes (Amaral et al., 2025). Our study builds on this work by highlighting the physical body as a site in which both power relations and knotted paradoxes are enacted. Specifically, we introduce the concept of the triple bind, where paradox knots intersect with power asymmetries and physically demanding paradoxes. Under the triple bind, physical depletion acts as a “third dimension” of (material) constraint, compounding the interpersonal and structural constraints characteristic of traditional double binds (Putnam & Ashcraft, 2017). Future research could further examine the notion of physical depletion as a third dimension of constraint and, in particular, how it influences the experience of pathological and pragmatic paradoxes. For example, pragmatic paradoxes are typically described as “paralyzing” situations (Berti & Simpson, 2021a). Yet, literally speaking, subordinates receiving unrefusable and contradictory orders are unlikely to have the luxury of responding by not moving. Therefore, how do subordinates’ bodies experience the metaphorical state of “paralysis” associated with pragmatic paradoxes? Could some pragmatic paradoxes actually be associated with physically depleting hyperactivity?
In addition to revealing the material constraints of triple binds, our work advances understanding of how power and knotting jointly shape social orders. Aligning with a processual view of paradox in which “the micro constructs the macro” (Bednarek & Smith, 2024, p. 587; Jarzabkowski et al., 2017), we found that knotted paradoxes were embodied and enacted in practices that could simultaneously express, reconfigure, and/or reinforce prevailing power structures and relationships. More specifically, our theorization illustrates the self-reinforcing ways in which gendered power relations play out in paradox knotting (Putnam & Ashcraft, 2017). Building on prior research, our findings suggest that due to the devaluation of care work in patriarchal-capitalist societies (Tronto, 2013) and enduring narratives about gendered home-domain roles (Padavic et al., 2020), women may be susceptible to restrictive forms of paradox knotting that do not affect men. In turn, we demonstrate how paradox knotting can promote and maintain undesirable forms of social order (Acker, 2006) in addition to the desirable forms of order studied by other scholars (Jarzabkowski et al., 2022). Future research could examine the converse of our findings—namely, how knotting acts as a disordering mechanism (Jarzabkowski et al., 2022; Sheep et al., 2017) that reconfigures or overturns oppressive social orders.
Responsibility for navigating paradox
Our exploration of the links among bodies, paradox knotting, and power has implications for the question of who is responsible for navigating paradoxes. The dominant view, encapsulated in what Seidemann (2024, p. 11) calls the “hegemony of both/and,” is that focal actors who experience paradoxes are responsible for navigating them (Li, 2021; Smith & Lewis, 2022). Our work not only highlights the limits of this “individual responsibility” perspective but also offers ideas for alternative ways of addressing paradoxes through policy initiatives targeting systemic change. Starting with the limits of individual responsibility, our findings illustrate how the structure of the maternity care system forces midwives to choose between sacrificing their bodies and their integrity. The system forces midwives to sacrifice their bodies by putting them in a triple bind, where physical depletion compounds interpersonal and structural constraints. As documented earlier, this bind has serious ramifications for midwives’ health, which manifest either acutely or over the long term. However, midwives often choose to live within the constraints of the triple bind because the self-employed business model underpinning it also affords them the autonomy to provide women-centered care. Providing such care is integral to midwives’ integrity. Therefore, if midwives choose to leave the bind, they may save their bodies from the bind’s long-term health consequences, but they typically sacrifice their integrity by subordinating themselves to medical hierarchies in hospitals.
Who, then, “should” be responsible for navigating the paradoxes underlying midwives’ triple bind? One perspective suggests that midwives should cope individually by “reducing [their] expectations” (Li, 2021, p. 407). For example, midwives could concede that they can either have health (but lose integrity) or have integrity (but lose health). However, this individual responsibility perspective contradicts a core normative message of paradox theory—namely, that actors should not have to choose between interdependent options (Lewis & Smith, 2022). Therefore, enabling a both/and approach for midwives requires systemic change (Amaral et al., 2025; Berti & Simpson, 2021b), implemented at the policy level. Drawing on Mary Follett as inspiration, Bednarek and Smith (2024) suggest that individuals (such as midwives) could be integrated as active participants in designing and implementing such change, enabling the oppressive power-over dynamics of the current system to shift toward generative power-with dynamics (Schrage et al., 2025). For example, midwives could work with policymakers to cocreate a system where midwifery care is treated neither as a lowly-valued commodity in a fixed price market, nor as a subordinate type of care to obstetric approaches. Such a system would undoubtedly be far from perfect—it would almost certainly still challenge midwives’ health and integrity. Yet, the power-with dynamics underpinning the system would at least alleviate most midwives of the “your-body-or-your-integrity” choice they currently perceive. While this example is specific to NZ’s maternity care system, the broader message of how to facilitate constructive paradox navigation through systemic change is likely transferable to a range of other contexts where pathological manifestations of paradox are rooted in asymmetrical power structures.
Limitations
It is worth considering how the particularities of our research methods may have shaped findings. First, we gathered data from participants in joint family interviews. Some researchers suggest that interviewing family members jointly can distort the data they share by privileging the views of a dominant partner or member (while the other person hides or downplays their real views) (Zarhin, 2018). We were attentive to this challenge and made efforts to overcome it. Specifically, we actively encouraged “quiet” family members to speak up and made notes regarding our interpretations of relational dynamics among family members following interviews. These notes enabled us to be critically reflexive (Berger, 2015) when analyzing interview data from distinct family units. We chose to conduct joint interviews for logistical, ethical, and data-quality considerations (Bjørnholt & Farstad, 2014; Reczek, 2014). However, because interpersonal power imbalances can be hard to observe and may have influenced our findings without our awareness (Zarhin, 2018), we suggest future research could benefit from employing separate interviews or separate interviews combined with joint interviews (Reczek, 2014).
Our exploration of how bodies experience and enact paradoxical tensions drew on in-depth interviews, thus relying on verbal accounts of bodily experiences. While this approach is common in research examining embodied experiences (Michel, 2011), it could be strengthened by other data collection techniques (e.g., on-site observation, video ethnography) that enable researchers to observe bodies acting in context (Lê & Bednarek, 2017). For example, how do bodies physically enact the competition–cooperation paradox in elite sports (Greenslade-Yeats et al., 2024)? Video footage of sports such as professional cycling would be easily accessible to researchers and could provide further insights into embodied paradoxes.
Conclusion
Our research illustrates how paradoxical tensions are experienced and enacted by physical bodies. Focusing on a gendered care context, we show that embodied tensions materialize in polarities of absence–presence and energy–fatigue which, over time, have enduring physical, emotional, and relational impacts. We also reveal how embodied tensions are shaped and amplified by a complex interplay of power relations and paradox knotting, creating a “triple bind.” Our findings provide further encouragement for scholars to look beyond individual, cognitively based approaches to paradox and to consider why paradox navigation may be an inherently collective feat that, in some instances, requires radical systemic change.
Footnotes
Acknowledgements
We would first like to acknowledge our midwife and family member participants, who brought this paper to life by so generously sharing their inner worlds with us. We express our gratitude to Dr Lesley Dixon (New Zealand College of Midwives) for her support with participant recruitment and study design and to Emerita Professor Gill Kirton (Queen Mary University London) for her valuable feedback on an earlier draft of this paper. A huge thank you goes to senior editor Beth Goodrick and our three anonymous reviewers for their insightful and supportive feedback and guidance; these individuals were as much co-authors as reviewers on this manuscript, and many of the most interesting ideas were theirs, not ours. We also acknowledge input from members of the sustainability track at the Australia New Zealand Academy of Management conference, 2024, hosted by University of Wollongong. Finally, this work was supported by a Health Delivery Research Project Grant (21-872) from the Health Research Council of New Zealand, awarded to Tago L. Mharapara (primary investigator).
ORCID iDs
Ethical Considerations
Approval for this study was granted by Auckland University of Technology Ethics Committee on 15 August 2022, reference number 22/161.
Consent to Participate
Participants in this research provided informed consent either via a written consent form (for in-person interviews) or via an oral consent protocol (for virtual interviews).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article. This work was supported by the Health Research Council of New Zealand [grant number 21-872].
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
