Abstract
Objective:
Otomatch.com is a public forum where otolaryngology residency applicants share anonymous impressions from subinternship rotations and interviews. We conducted a qualitative analysis of posted comments to describe the program attributes and experiences most frequently discussed on Otomatch.
Methods:
We extracted interview and subinternship comments from spreadsheets covering the 2023 to 2024 and 2024 to 2025 application cycles. Each comment was coded to a theme and sub-theme and labeled as positive, negative, or neutral.
Results:
In total, 1791 comments were coded, of which 56.8% were positive, 21.6% negative, and 21.6% neutral. Most feedback related to interpersonal relationships (30.4%). Within this theme, the most frequent positive sub-themes were interactions with residents, fellows, and attending physicians (64.0%) and overall culture (16.0%). The second most frequent theme was the subinternship rotation (17.6%), followed by surgical training (15.6%). The most negative feedback concerned interactions with resident and attending physicians, followed by criticism of call schedules.
Conclusion:
Individuals posting on Otomatch frequently described inclusive culture, robust surgical training, thoughtful interview experiences, and positive interactions with residents and attending physicians during subinternship rotations and the interview process. Conversely, negative posts most often described unfavorable experiences in these same domains. Our analysis may support program leadership reflection and targeted refinements to modifiable aspects of the residency applicant experience.
Keywords
Introduction
Otolaryngology-head and neck surgery (OHNS) is among the most competitive specialties for prospective medical students entering the match.1,2 In the modern era, hopeful applicants frequently seek guidance from social media and anonymous online communities such as Otomatch.com.3,4 Through this otolaryngology-based online public platform, students gain access to educational resources and spreadsheets containing user-generated information on residency interview dates, general announcements, subinternship rotation and interview impressions, and the desirability of individual residency programs. Although the reliability of similar forums has previously been questioned, Nathan et al 5 found the self-reporting of academic metrics on Otomatch to be generally accurate. Anonymous feedback enables medical students to obtain unfiltered reviews of the culture, surgical training, and program features of residency programs. Since the average otolaryngology applicant completes only 2 away subinternship rotations, students can gain invaluable information from such platforms to guide their decision-making when choosing which programs to signal or apply to. 6 These reviews may offer an honest look at some of the most important aspects of training considered by medical students, in a setting not censored by fear of retribution from program leadership. Considerable research has been published on the medical student attributes favored by program directors and residency leadership, but little research has examined what currently attracts highly qualified medical students to otolaryngology residency programs.
The goal of our study is to describe the residency attributes and experiences most frequently discussed in Otomatch narratives about subinternship rotations and interviews, including the sentiment of these comments, as these attributes and experiences may shape perceptions of programs during OHNS residency recruitment.
Methods
The institutional review board at Dell Medical School at the University of Texas at Austin determined this study did not meet the definition of human subjects research. We conducted a qualitative retrospective review of anonymous feedback from the spreadsheets “Interview Impressions 24,” “Away Rotation Impressions 24,” “Rotation Impressions 24-25,” and “IV Impressions 24-25” on Otomatch.com from 2023 to 2024 and 2024 to 2025 application cycles. Comments within the rotation impressions spreadsheets were only extracted from 3 columns titled “Overall Comments,” “Biggest Pro,” and “Biggest Con.” Comments within the interview impression spreadsheets were only extracted from 3 columns titled “Overall Impression,” “Positive Impressions,” and “Negative Impressions.” All the data is publicly accessible through Otomatch.com.
We obtained permission from the administrator of Otomatch.com before proceeding with extraction and analysis. First, an investigator not involved in categorizing comments deidentified all data within the spreadsheets by removing the names of residency programs, associated hospitals, and city names. Before extracting the data, themes and sub-themes were created to categorize comments within the spreadsheets. Three investigators completed a preliminary review, deriving 7 themes and 4 to 8 sub-themes per theme. The themes included interpersonal relationships, surgical training, work conditions, program features, interview, subinternship rotation, and other. Then, a single grader reviewed all comments and categorized them into appropriate themes and sub-themes. These data were further subclassified as either negative, positive, or neutral comments. A single grader was used to ensure consistency in grading. Some sentences contained more than 1 comment. For example, “Insane clinical volume and resident research” was considered 2 comments, as it addressed 2 sub-themes: 1 in the surgical training theme and the other in the program features theme. Rarely, users engaged in dialogue in the cell where comments were evaluated. This dialogue was excluded from the analysis.
Results
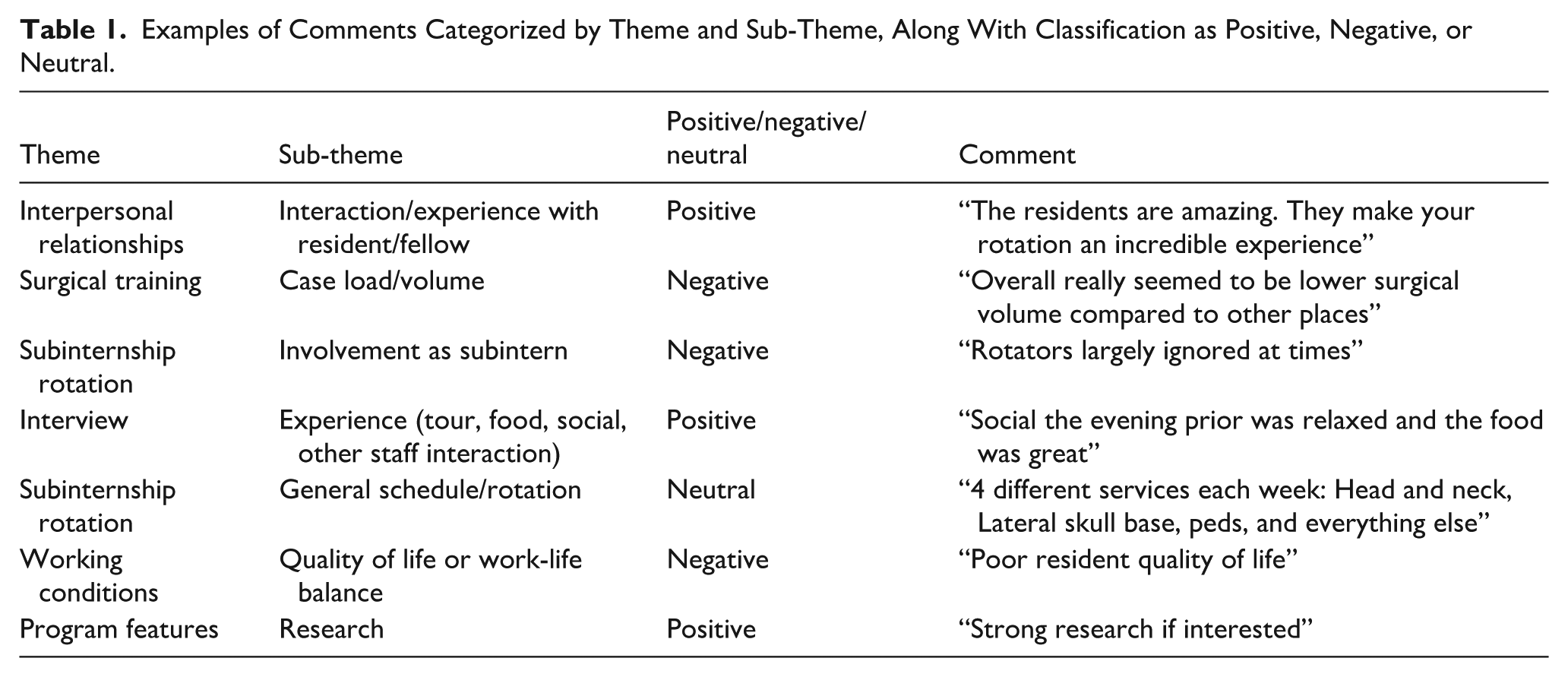
In total, 1791 comments were extracted and coded (Table 1). Of these, 1085 were extracted from subinternship rotation spreadsheets and 706 from interview spreadsheets. By application cycle, 1021 comments were from 2023 to 2024 and 770 from 2024 to 2025. Interpersonal relationships, subinternship rotation, and surgical training were the most represented themes, as seen in Figure 1. Most of the comments analyzed were classified as positive feedback (Table 2). Overall, 1017 (56.8%) were positive, 387 (21.6%) were negative, and 387 (21.6%) were neutral.
Examples of Comments Categorized by Theme and Sub-Theme, Along With Classification as Positive, Negative, or Neutral.

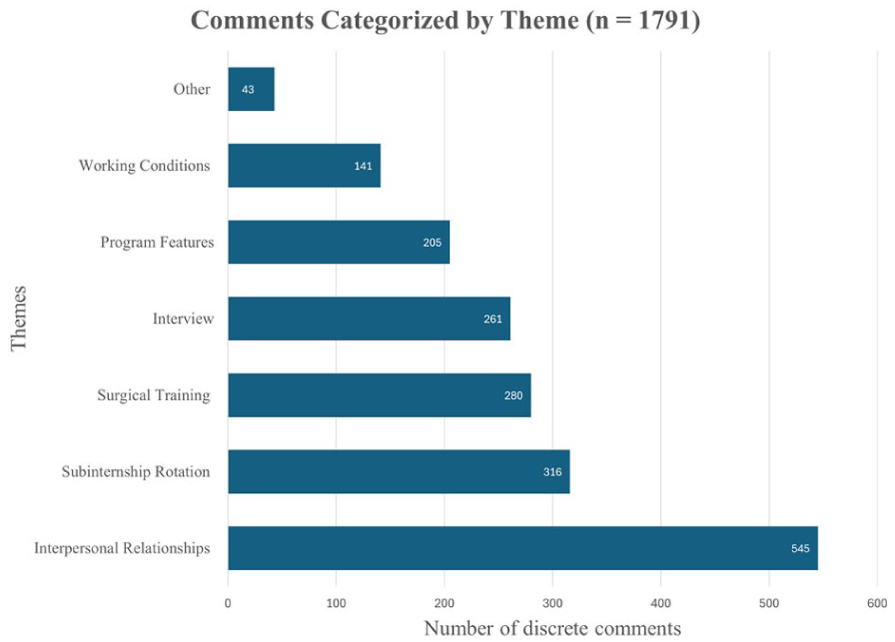
Themes with corresponding number of discrete comments.
Positive Comments Categorized by Theme and Sub-Theme.
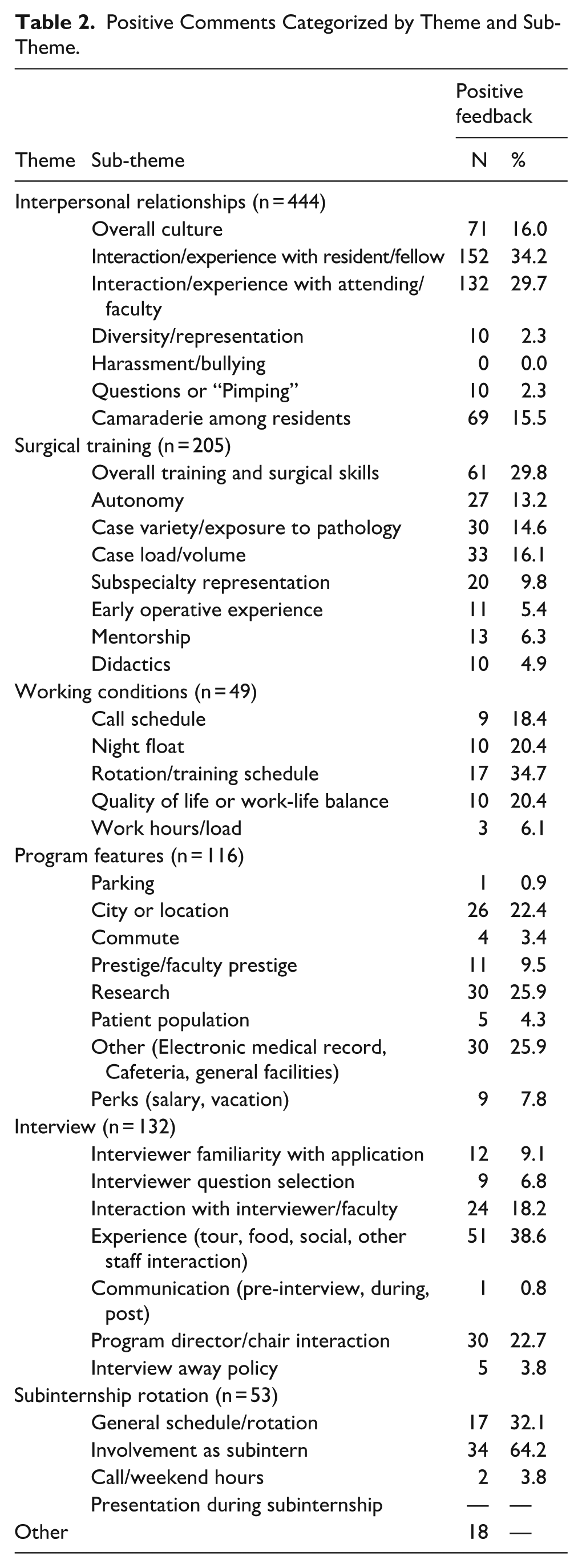
Positive Comments
The interpersonal relationships theme was the most common, accounting for 43.7% of the positive feedback, followed by surgical training (20.2%) and the interview process (13.0%). Within the interpersonal relationships theme, 63.9% of comments related to interactions with resident, fellow, or attending physicians. For comments regarding surgical training, the most common sub-themes were overall surgical training and skills (29.8%), case load/volume (16.1%), case variety (14.6%), and autonomy (13.2%). Commenters expressed the most positive feedback about their experience on interview day (38.6%), interactions with the program chair or director (22.7%), and interactions with an interviewer (18.2%) in the interview theme.
Negative Comments
Among the negative comments (Table 3), the theme of interpersonal relationships was the most frequent, comprising 23.3% of the negative feedback, followed by the interview process (19.1%) and program features (18.1%). Similar to positive comments about interpersonal relationships, interactions with resident, fellow, or attending physicians (58.9%), the overall culture (18.9%), and camaraderie among residents (11.1%) continued to be the most common sub-themes in negative feedback. Regarding the interview process, commenters voiced criticism about interactions with interviewers (28.4%), interactions with the program chair or director (24.3%), and interview question selection (21.6%). Otomatch posters most often left negative opinions about residency location (30.0%), commute (24.3%), and research (11.4%) in the program features theme.
Negative Comments Categorized by Theme and Sub-Theme.
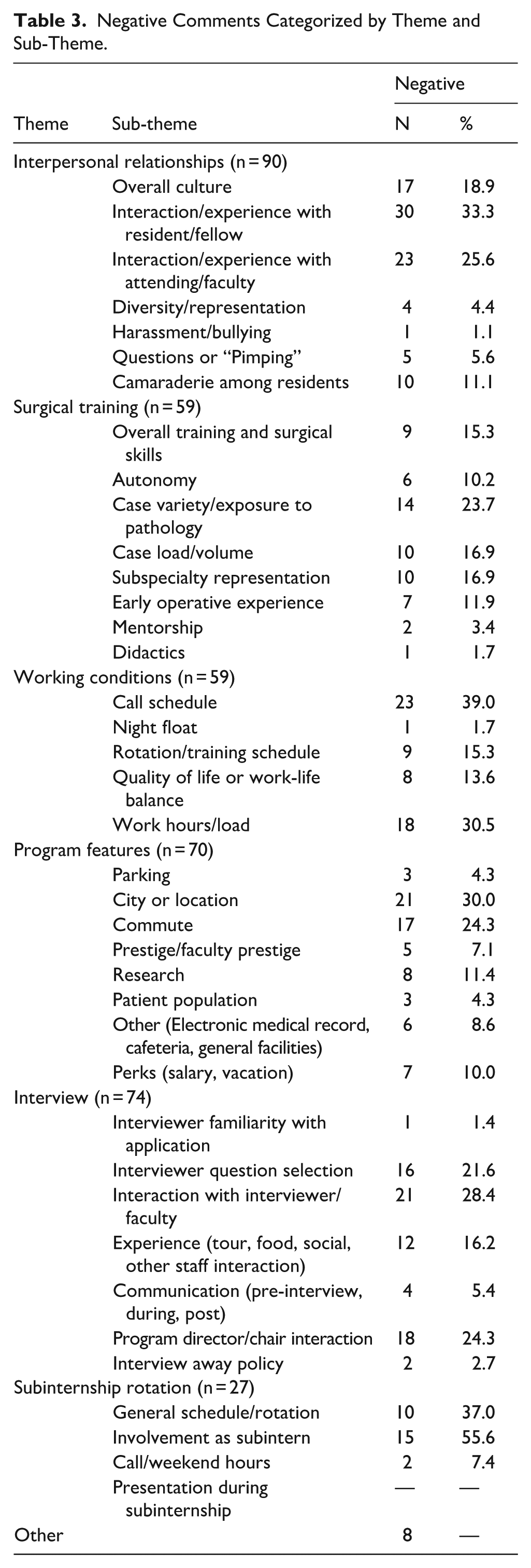
Neutral Comments
The most prevalent theme receiving neutral feedback (Table 4) was the subinternship rotation, differing from the trend noted in both positive and negative comments. Otomatch contributors frequently commented on the general schedule of the subinternship rotation (57.2%) and on call/weekend hour requirements (25.8%).
Neutral Comments Categorized by Theme and Sub-Theme.
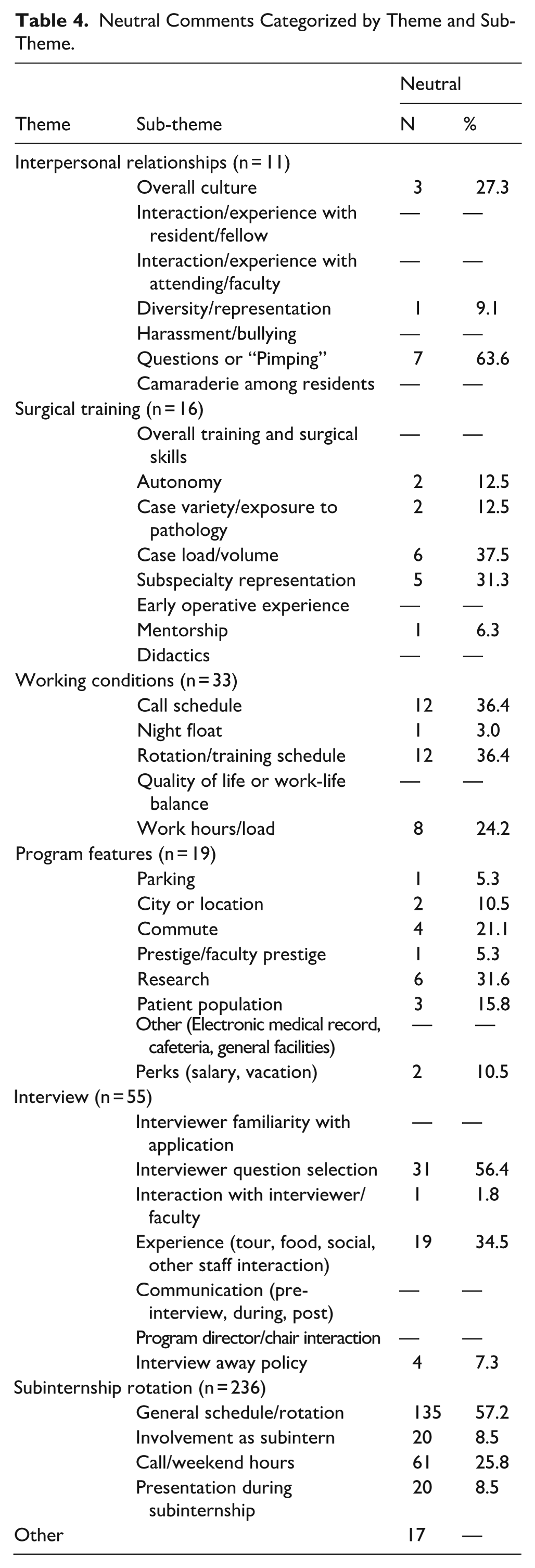
Discussion
Anonymous platforms such as Otomatch provide needed insight, from an applicant perspective, into OHNS residency culture, surgical training, and the interview process. The individuals who provided feedback on Otomatch are attracted to programs that foster an inclusive environment of resident, fellow, and attending physician engagement and trainee development. Since the majority of comments were related to interprofessional relationships, this suggests that strengths in this area may be even more attractive than strong surgical training alone. This is highlighted by the observation that most comments regarding “pimping,” a common term used by medical students to describe when resident or attending physicians question their knowledge base, were positive. Even when encountering what some may consider an intimidating process, commenters conveyed gratitude for the educational opportunity and being included in the academic rigors of residency programs. These findings suggest that interactions with resident and attending physicians should not be underestimated as factors that may attract or deter hopeful students. This aligns with recent literature across multiple medical specialties, which has similarly reported that interactions with residents and program leadership are highly influential factors for prospective applicants.3,7
Commenters were also highly interested in case volume, surgical autonomy, and exposure to a variety of pathologies. This indicates that during subinternship rotations and the interview process, residency leadership should ensure they highlight these areas of their program. As for working conditions, concerns about the call schedule were common, with most commenters expressing concerns about excessive frequency or the absence of a post-call day. Night float received positive feedback and was perceived as an enticing quality. This may represent a shift in perception of call duties, as recent literature suggests that night float is gaining popularity among residents as an alternative to the traditional 24-hour call.8 -10 The only negative comment regarding night float was addressing a residency program lacking this feature. The call schedule may not be modifiable at the leadership level, depending on the number of residents and the hospital system’s overall patient volume. For these programs, our data may be used to strengthen other modifiable aspects such as culture, research, surgical autonomy, and mentorship.
Commenters on their subinternship rotation frequently discussed their involvement in the clinic, during rounds, and in the operating room. The majority of negative comments were related to a contributor’s perception of not being given responsibility or offered the opportunity to be involved in surgical cases or the clinic. Commenters who left positive remarks were enthusiastic about suturing, being asked questions by attending physicians, and seeing patients in the clinic.
Positive comments suggested that a commenter’s overall interview-day experience was often shaped by factors outside the formal interview itself. Otomatch contributors frequently commended city and hospital tours, pre-interview socials, and other events held on or before interview day. Interactions with the residency program chair or director on interview day received significant positive and negative feedback.
There are multiple limitations of our study. Although previous literature has suggested that information on Otomatch is generally reliable, these analyses focused on quantitative measures such as United States Medical Licensing Examination (USMLE) Step scores, interview invitations, and clinical rotation grades. The accuracy of the qualitative data on Otomatch has not, and essentially cannot be confirmed due to the nature of the platform. Anyone with access to the spreadsheet can modify entries, and there is no mechanism to limit or verify the number of comments contributed by a given user. Commenters may also still be reluctant to leave negative feedback out of fear of being identified, since there are often a small number of away rotators at many sites, or the feedback may be identifiable based on the interaction. This may explain the tendency for contributors to leave positive feedback. Interview format during the 2023 to 2024 OHNS recruitment season included both virtual and in-person interviews. However, the interview modality was not consistently documented in the analyzed spreadsheets and was therefore neither coded nor used for stratified analyses. Given the descriptive, cross-sectional nature of this qualitative study, we cannot assess whether Otomatch narratives influence subsequent signaling, application, ranking, or match outcomes. Posting is self-selected and may not represent the broader applicant pool, and experiences not posted cannot be captured. Accordingly, findings should be interpreted as descriptive and hypothesis-generating rather than causal.
Conclusion
Overall, our study emphasizes that Otomatch users desire programs with a strong inclusive culture, resident camaraderie, and welcoming resident, fellow, and attending physicians. These features, paired with robust surgical training and a thoughtful interview day, may significantly enhance a program’s appeal. It is essential that residents and staff recognize their important role in recruitment, especially during interactions with subinterns and applicants on interview day. Their demeanor and engagement may significantly influence applicants’ perceptions of the program. Many of our findings are consistent with recent literature from other specialties, suggesting an accurate representation of applicants’ desires and expectations on Otomatch. To stand out in the competitive OHNS landscape, residency programs should prioritize showcasing these elements during interactions with applicants. Additionally, program leadership may need to remain flexible, when logistically and financially feasible, to implement the desired policies such as night float to attract the most qualified candidates.
Footnotes
Acknowledgements
We would like to express our appreciation for ![]() and all those who participated in providing input to the spreadsheets used in our study. All the data was extracted from Otomatch.com.
and all those who participated in providing input to the spreadsheets used in our study. All the data was extracted from Otomatch.com.
Ethical Considerations
This article does not contain any studies with human or animal participants. The institutional review board at Dell Medical School at the University of Texas at Austin determined this study did not meet the definition of human subjects research.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
