Abstract
Keywords
Introduction
Pyriform fossa (PF) branchial apparatus anomalies (PFBAA) are rare congenital malformations of branchial cleft and pouch,1,2 originating from the third or fourth branchial apparatus remnants. 3 Third branchial apparatus anomalies (TBAA) are believed to originate from the base (cranial end) of the PF and pass above the superior laryngeal nerve (SLN). In contrast, the fourth branchial apparatus anomalies (FBAA) originate from the apex (caudal end) of the PF and pass through the cricothyroid membrane beneath the SLN. 4 They are collectively referred to as PFBAA since both TBAA and FBAA originate from the PF, and their clinical presentations are quite similar. 5
In most cases, no external orifice or obvious clinical symptoms and signs can be found in children and neonates during the noninfectious period. Instead, common presentations include cervical redness and swelling, deep neck abscess or suppurative thyroiditis, pain, dysphagia, and fever, which could present in the infectious period. 6 Nevertheless, critical conditions have been reported, like tracheal compression and respiratory distress in neonates5,7 and mediastinal abscess in adults. 8 However, in adults, delayed diagnosis of PFBAA and iterative neck abscess formation is common, necessitating multiple cervical incisions and drainage, which might result in noticeable skin scars and severe cervical inflammation, granulation, and adhesion.9,10
Multiple endoscopic modalities have been applied to obliterate the internal orifice (IO) of PFBAA to achieve minimally invasive treatment, including electrocautery, chemical cauterization, CO2 laser cauterization, plasma coblation, and other similar strategies. 11 However, the success rates for these endoscopic obliteration strategies vary widely from 50% to 91%, with some cases requiring multiple procedures. 10 Iterative cervical infection could be quite troublesome economically, physically, cosmetically, and psychologically in adult patients with PFBAA. Hence, open neck surgery might be inevitable in adults with repetitive episodes of acute infection, especially after the failure of endoscopic attempts. 5 Our department has devised a paradigm combining endoscopic procedures and open neck surgery to achieve higher success rates in treating such patients, which is reported in this article.
Patients and Methods
A retrospective review was undertaken for PFBAA cases treated at our tertiary medical institution between July 2020 and November 2023. Data of interest were collected from case archives. The protocol of this research project was approved by the institutional review board. It conformed to the provisions of the Declaration of Helsinki. Informed written consent was obtained from the patients included.
Diagnosis
Presenting symptoms included repeated cervical pain and swelling, acute deep neck abscess formation, and suppurative thyroiditis. Fiberoptic laryngoscopy can be applied to identify the IO (Figure 1B). Barium esophageal study can demonstrate the communication between PF and cervical lesions (Figure 2C). In addition, cervical computed tomography/magnetic resonance imaging (CT/MRI), with or without a contrast medium, can help understand the scale of cervical lesions and the involvement of important structures (Figures 1 and 2). These are routine preoperative (PO) evaluations for PFBAA at our department. Although a single modality of the aforementioned evaluations might not always yield a positive result, their combination can help establish a diagnosis and outline surgical plans (Table 1).
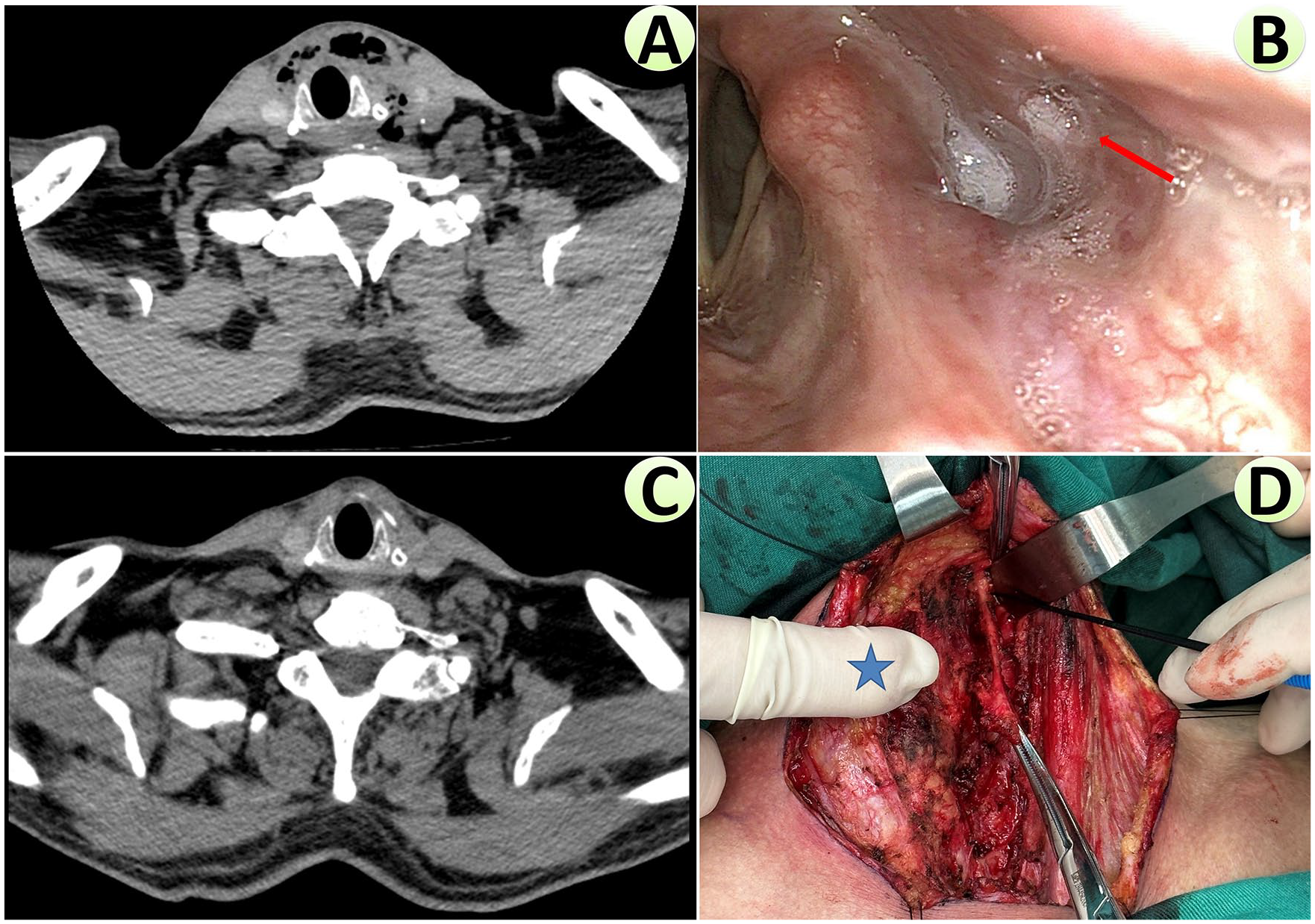
Preoperative evaluation and intraoperative findings of Case 7 with left TBAA. (A) Preoperative cervical CT scan showing deep neck abscess and gas formation on the left and front of thyroid and cricoid cartilages. (B) The patient gradually recovered after emergency incision/drainage and endoscopic plasma coblation of internal orifice mucosa. Six weeks later, another fiberoptic laryngoscopy showed that the internal orifice on the upper lateral wall (indicating TBAA) was not obliterated (red arrow). (C) CT scan at 6 weeks after emergency surgery showed his deep neck infection had recovered, and he was scheduled for an open neck surgery. (D) After flap elevation, granulation and scar tissue was dissected. Further careful dissection revealed a sinus tract (held by a clamp) extending to the thyrohyoid membrane (at the tip of the stimulating probe, indicating TBAA). The thyroid lamina was pushed medially by the index finger of the first assistant (blue asterisk). TBAA, third branchial apparatus anomaly.
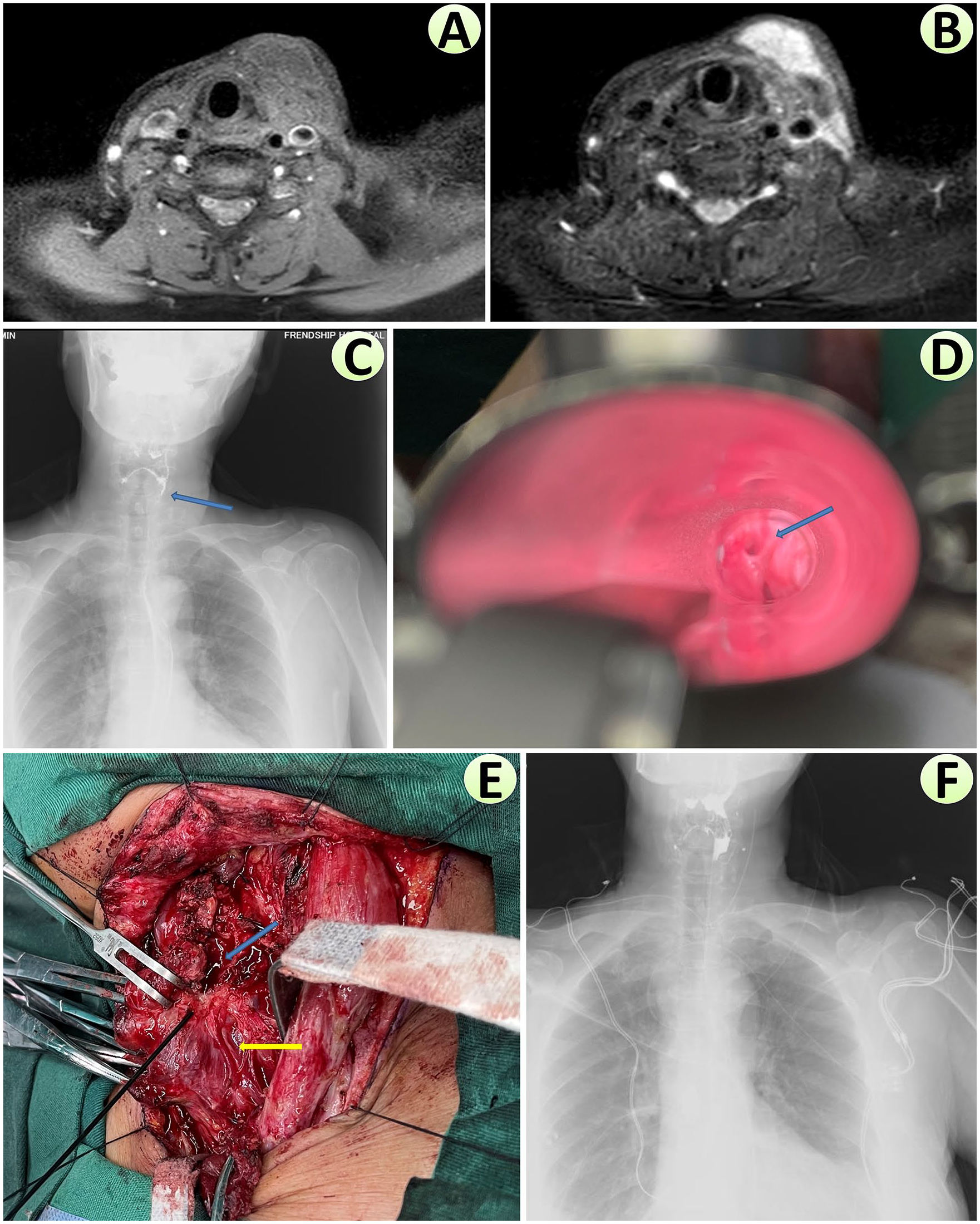
Pre- and postoperative evaluation and intraoperative findings of Case 5 with a left FBAA. (A) Isointense signal of left cervical lesion on T1-weighted image of preoperative cervical MRI scan. (B) Hyperintense signal of left cervical lesion on T2-weighted image of preoperative MRI scan, indicating an inflammatory condition. (C) Although preoperative fiberoptic laryngoscopy (figure not shown) did not identify the internal orifice in the left PF, a preoperative barium esophageal study did demonstrate outflow from the apex of left PF, indicating the condition was FBAA. (D) Direct laryngoscopy after general anesthesia identified the internal orifice (blue arrow) on the apex of the left PF. (E) After flap elevation, inflammatory and granulation tissue was resected. Further careful dissection revealed the course of the left recurrent laryngeal nerve (yellow arrow). Posterosuperior to the cricothyroid joint (at the tip of the stimulating probe), a patch of blue-stained area was revealed. This site was carefully dissected, and the sinus tract was securely ligated, with an additional purse-string suture. (F) A barium esophageal study was undertaken on the seventh postoperative day, and no outflow from the left PF was observed. FBAA, fourth branchial apparatus anomaly; PF, pyriform fossa.
Demographic Data, PO Examination and Classification of PF PFBAA.
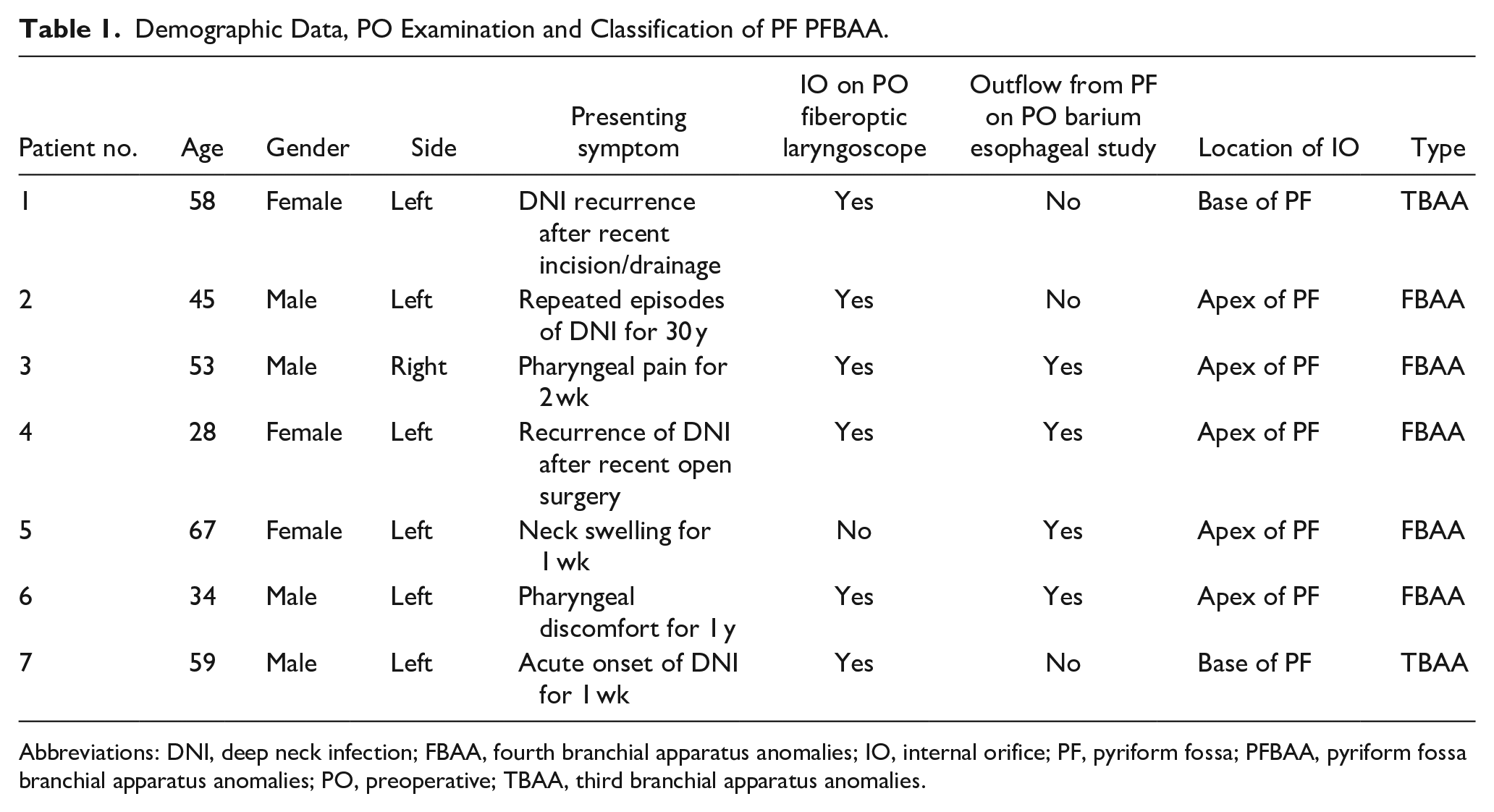
Abbreviations: DNI, deep neck infection; FBAA, fourth branchial apparatus anomalies; IO, internal orifice; PF, pyriform fossa; PFBAA, pyriform fossa branchial apparatus anomalies; PO, preoperative; TBAA, third branchial apparatus anomalies.
Open neck surgery was scheduled for several (usually 6) weeks after the acute infection had resolved in case reactive edema and inflammation might close the sinus tract in the acute infectious phase. 5
Surgical Procedures
The paradigm of surgical procedures included 3 steps after general anesthesia.
First, direct laryngoscopy was set up to evaluate the ipsilateral PF thoroughly and identify the IO (Figure 2D). If TBAA was suspected, the base (or upper lateral wall) of PF was the focus, whereas, for FBAA, the apex of PF was scrutinized. When the IO was identified, the suspension of the direct laryngoscope was established, methylene blue was injected into the IO, and outflow was controlled by suction to keep the surgical field clean. Then, suspension was relieved, but the direct laryngoscope was left in place, taking care to prevent the patient’s face from abrasion by the direct laryngoscope.
Second, the neck was disinfected and draped, and space was left so the second assistant could manipulate the direct laryngoscope near the head. The skin incision was designed to include the previous scar. The incision was long enough so that the subplatysmal flap could be elevated to the level of surgical plans: in TBAA, the flap was elevated to the hyoid bone level, whereas in FBAA, the flap was elevated to the thyroid notch level. Then, a careful dissection of the cervical lesion was undertaken. Recurrent laryngeal nerve (RLN) monitoring was routinely used so that the course of RLN could be mapped and protected. After the mobilization of cervical inflammatory tissue and granulation, its communication with the PF was identified. If blue-stained sinus tracts could be identified on the thyrohyoid membrane (TBAA) or near the cricothyroid joint (FBAA, see Figure 2E), then the sinus tract was ligated securely immediately outside of PF, and a purse-string suture was applied to further secure this ligation. If no blue-stained area could be identified inside the inflammatory tissue and granulation, a blunt probe could be introduced through the direct laryngoscope and through the IO into the cervical lesion by the second assistant. This probe could be felt in the cervical lesion, which could help with dissection and the eventual ligation of the communication between the cervical lesion and PF. Then, the surgical field was irrigated with peroxide, diluted iodophor, and saline. A negative-pressure drain was placed, and the incision was closed.
Finally, the suspension was applied to the direct laryngoscope again. Then, plasma coblation of the mucosa of the IO was undertaken. Care was taken to manipulate only the mucosa to protect important adjacent structures, especially RLN. 12 Then, a nasogastric feeding tube (NG-FT) was inserted under direct observation to avoid injury to the IO.
Follow-Up
The patients included in the present study were followed up every month after surgery for postoperative complications, especially pharyngeal fistulae. After complete recovery, they were followed up every 3 months for recurrence.
Results
Seven cases were included, with 4 male and 3 female patients. Their age range was 28 to 67 years (average and median ages were 49.1 and 53, respectively). Six lesions were on the left side, while 1 was on the right side (Table 1). Presenting symptoms were various. Six patients had suffered from multiple episodes of acute cervical infection and iterative incision and drainage. A young female patient (Case 4) had undergone open neck surgery in another hospital previously and was referred to our department after recurrence. One patient (Case 7) suffered from acute deep neck abscess formation as his first acute infection; however, plasma coblation (performed during emergency incision and drainage in our department) did not obliterate the IO after 6 weeks of observation.
PO fiberoptic laryngoscopy identified the IO in 6 patients, while a PO barium esophageal study identified outflow from PF in 4 patients. Fortunately, no patient was found to be negative on both examinations, and a preliminary diagnosis could be established (Table 1).
The IOs in all the 7 patients were identified intraoperatively, with 2 on the base of PF (TBAA) and 5 on the apex of PF (FBAA), in accordance with PO diagnosis. The surgical procedures were all uneventful. In 3 patients with negative PO barium esophageal study, sinus tracts were not stained satisfactorily, necessitating the identification of the communication between PF and cervical lesion with the blunt probe. Sometimes, the insertion through the IO needed effort, which might be because the sinus tracts were quite impeded. The dissection of the cervical lesion could be quite challenging, requiring experience and expertise.
No postoperative complications (especially pharyngeal fistula and vocal cord paralysis) were observed. Recovery was uneventful in all the patients. The drain was removed when daily drainage was <10 mL. A barium esophageal study was undertaken on the seventh postoperative day. If no outflow was detected (Figure 2F), oral fluid intake would be resumed. And indeed, all the patients in this series had no outflow detected on the barium esophageal study on the seventh postoperative day. NG-FTs were removed on the next day, and they were discharged.
The follow-up continued for 6 to 40 months (average and median durations were 22 and 27 months, respectively). No recurrence was documented.
Discussion
Although the majority of literature reporting PFBAA refers to this subsite of hypopharynx as the pyriform “sinus,”11,13,14 the term “sinus” is also used to describe the developmental anomalies of interest here. Hence, we are constantly confused when we have to distinguish between an anatomic location and a developmental anomaly. Therefore, we prefer to refer to this anatomic site as a “fossa,” which is also used in the literature, 6 albeit much less commonly. Furthermore, the term “fistula” refers to anatomic anomalies that have both internal (pharyngeal) and external (cutaneous) orifices. 15 In addition, we believe the term “pyriform fossa fistula” is not accurate enough to describe all the branchial apparatus anomalies originating from this site, especially sinuses and cysts. 5 Hence, we prefer to refer to them as PFBAA, which are highly prone to occur on the left side, 11 with sporadic case reports of right-sided PFBAA in the literature;16,17 furthermore, bilateral PFBAA has been reported. 18 The classic description is based on understanding the segmental branchial anatomy. It involves the persistence of the pharyngobranchial duct, which connects the third and fourth pharyngeal pouches to the pharynx and typically degenerates during the seventh week of development. 17
Delayed diagnosis of PFBAA is commonly encountered, mainly due to its rarity, the resultant low index of suspicion, and low rate of recognition, in addition to the fact that its presentation could be rather unspecific, including hoarseness, 19 contralateral neck infection, 20 retropharyngeal abscess, 21 pleural effusion and pneumonia, 8 thyroid nodules with ultrasound characteristics raising suspicion for maligancy, 14 and post-thyroidectomy pharyngeal fistula. 22 In addition, fine needle aspiration of the thyroid nodule mimicking thyroid cancer in a 34-year-old male patient resulted in the rapid onset of neck pain, swelling, fever, and dyspnea sequentially. Emergency tracheostomy was needed to deal with diffuse swelling of the hypopharynx and supraglottic larynx and rapid progression of respiratory distress; finally, a PFBAA was identified and endoscopically obliterated. 14
Management of PFBAA could be challenging. Although endoscopic procedures are minimally invasive, recurrence is not uncommon. Concerning PFBAA in adults with iterative episodes of infection, open neck surgery is usually unavoidable and considered the most thorough treatment.5,23 To further complicate this matter, PFBAA could present with double tracts, with both communicating with the pharynx after pathological confirmation of foreign bodies inside the tracts. 13 Should only one tract be ligated intraoperatively, recurrence might have been inevitable. Indeed, the open neck surgery for PFBAA should be performed by senior, experienced surgeons.
Our paradigm of applying surgical modalities is consistent with some literature, 24 but quite different from others. 25 In a well-written article in 2022, Lei et al reported their paradigm. After exposing the internal fistula with a suspension laryngoscope and endoscope, they would perform an internal fistulectomy with a CO2 laser to maximize the removal of the lining epithelium of the internal fistula. Then, they would place an absorbable gelatin sponge soaked with a blue staining agent in the bottom of the surgical wound and close the wound with sutures. Subsequently, NG-FT was inserted, the laryngoscope was withdrawn, and external surgical procedures were undertaken; finally, after tracing the fistula along its longitudinal axis to the “blue” mark outside the hypopharynx, they could complete external fistulectomy. 25 We admire Prof Lei’s effort to minimize the procedure into only 2 sections: internal fistulectomy with a suspension laryngoscope and then complete switching to external fistulectomy with open surgery. However, although there are 3 steps in our paradigm, it is our assumption that our paradigm also has several advantages: (1) Our staining agent (methylene blue) was injected into the IO, which could presumably stain longer sinus tracts with less time, rather than simply leaving this staining to the diffusion of agents soaked in the gelatin sponge placed within the IO, which could make it difficult for sinus tracts that were somewhat impeded. (2) In some of our external surgical explorations, blue-stained sinus tracts could not be adequately observed inside massive granulation tissues, especially in cases with a negative PO barium esophageal study, which might be attributed to the impeded sinus tract; and a blunt probe (or a guide wire, 24 or a Fogarty catheter 5 ) introduced through direct laryngoscope (without suspension) and then through the IO into the cervical surgical field, could be quite valuable for confirming the communication between PF and cervical lesion, leading to the successful ligation of whole external sinus tract. (3) Our modality of choice to manipulate the mucosa of the IO is plasma coblation under a direct laryngoscope with suspension, mainly due to its low temperature, limited depth of heat penetration, and relative ease of mastery.
The IOs of TBAA and FBAA are located quite differently, with TBAA on the rostral end of PF and FBAA on the apex of PF. 5 Identifying different locations of IOs is quite valuable for surgical planning, especially if achieved preoperatively. Since TBAA leaves PF through the thyrohyoid membrane (Figure 1D), while FBAA exits near the cricothyroid joint, it means that the elevation of flaps for TBAA should be higher to the level of the hyoid bone, whereas elevation of flaps for FBAA could be lower to the thyroid notch level. More important, this distinction could guide our search for the communication between PF and cervical lesion, whose accurate ligation is crucial for the success of the whole treatment procedure.
Furthermore, we believe that the key to the successful treatment of PFBAA is the intraoperative identification of the IO by direct laryngoscopy, which could be the basis for any following endeavor, including the dyeing of sinus tracts, open neck surgery, and/or various modalities to manipulate the IO mucosa. This notion is consistent with the literature, 24 and indeed, the only recurrence in our previous series was attributed to the failure of this identification. 15 Hence, we strongly recommend that this identification be performed at the beginning of surgical procedures for PFBAA. When this identification fails in patients in the noninfectious period, the following procedures should be aborted, and patients should be closely monitored. 24 However, if it occurs in patients in the infectious period, incision and drainage should be performed, and antibiotics should be administered.
The major limitation of this study is the small number of included patients, although PFBAA is a truly rare condition. The paradigm of our institution in managing this condition is also developing, based on advancement reported in literature. And we hope to share our experience to benefit such patients.
Conclusion
PFBAA is a rare clinical entity that can result in iterative cervical infection, severely compromising patients’ quality of life. Endoscopic dyeing of sinus tracts and plasma coblation of the mucosa of the IO are important procedures that are very beneficial for success in open neck surgeries, especially in adult patients.
Footnotes
Acknowledgements
Not applicable.
Author Contributions
Xiao-Ying Jia and Kai-Xuan He reviewed medical records, analyzed data, acquired institutional review board’s approval, and participated in patient follow-up and literature review. Yu-He Liu made contributions to revising manuscripts. Yan-Bo Dong participated in treatment of patients, participated in data analysis and illustration. Cheng Lu participated in treatment of patients, and made major contributions to the revising of multiple versions of manuscripts. Wan-Xin Li participated in treatment of patients, reviewed literature, and wrote multiple versions of manuscripts.
Availability of Data and Materials
All data, models, and code generated or used during the study appear in the submitted article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Beijing Hospitals Authority’s Ascent Plan [grant number DFL20220102], Beijing Friendship Hospital Seed Project, Capital Medical University [grant number YYZZ202125], National Natural Science Foundation of China for Young Scholars [grant number 82303642], and the Foundation for Scientific Research and Cultivation, Capital Medical University [grant number PYZ22076].
Ethics Approval
The protocol for the research project has been approved by Bioethics Committee of Beijing Friendship Hospital, Capital Medical University.
Statement of Human and Animal Rights
All procedures in this study were conducted in accordance with the institutional review board’s approved protocols (2020-P2-146-01).
Statement of Informed Consent
Written informed consent was obtained from the patients for their anonymized information to be published in this article.
