Abstract
Introduction
Suspension direct microlaryngoscopy (DML) is a common procedure that combines patient positioning, internal laryngeal distention, external counterpressure, and proper equipment to achieve optimal glottic visualization for precise surgical treatment of laryngeal pathology. Known manipulations that can improve anterior endolaryngeal exposure during DML include external manual cricoid pressure and manual tongue protrusion. Previously identified anatomical factors that may influence this exposure include mandibular retrognathia, macroglossia, flaccid epiglottis, limitations of the cervical spine, mandibular tori, and other abnormalities that also make endotracheal intubation difficult. 1 There have been no known published reports on the implications of ankyloglossia and subsequent lingual frenulum procedures to obtain enhanced exposure during direct laryngoscopy.
Case Reports
Case 1
A 65-year-old male with a past medical history of adult-onset recurrent respiratory papillomatosis (RRP) presented to the Vanderbilt Voice Center for ongoing care of dysphonia associated with bilateral true vocal fold (TVF) RRP lesions to include the anterior commissure (AC). Mandibular tori were not present. When the patient was originally taken to the operating room (OR), the patient had to be intubated via a video laryngoscope due to a challenging exposure. Subsequently, DML provided only a partial view of the posterior TVFs with manual tongue protrusion and anterior laryngeal pressure. A significant amount of RRP burden remained after the case due to inadequate exposure in the OR. Given the persistent disease, the patient was recommended for in-office potassium-titanyl-phosphate (KTP) laser ablation. Unfortunately, the patient could not tolerate the procedure due to strong gagging after maximum topicalization with anesthetic. The patient eventually was taken back to the OR and again intubated with challenge by anesthesia with a video laryngoscope. After ample positioning, manual tongue protrusion and use of the Holinger laryngoscope and Garrett-Ossoff-Pilling (GOP) laryngoscope (Teleflex Inc.), only suboptimal DML exposure could be obtained even with anterior laryngeal pressure. The GOP laryngoscope is 1 cm longer than the Dedo laryngoscope and 2 cm longer than the standard Large-Ossoff-Pilling laryngoscope but has a distal end similar to a Holinger Laryngoscope and a proximal portion that allows for binocular view with the operating microscope. Therefore, the GOP laryngoscope is an option for deep and anterior airways while still allowing for free-beam carbon dioxide (CO2) laser usage. On inspection of the tongue and floor of mouth, it was noted that the patient had tethering of his tongue by a lingual frenulum formed primarily by a foreshortened mucosal fold. The ankyloglossia was addressed by a simple lingual frenotomy with electrocautery without placement of suture to improve manual tongue protrusion. Preoperative informed consent allowed for additional procedures to accomplish the intended surgery. Completing the frenotomy was in line with institutional policies and the informed consent. The frenotomy with manual tongue protrusion remarkably allowed for full exposure of the TVFs, including the AC, without anterior laryngeal pressure with the GOP laryngoscope. Near total RRP burden was removed from the TVFs by use of our usual technique with CO2 Lumenis (Boston Scientific) laser excision with the operating microscope and micromanipulator pattern generator except a unilateral AC cuff of RRP to prevent webbing. Postoperatively, the frenotomy was discussed with the patient. The patient was very appreciative that the frenotomy had been completed intraoperatively, resulting in optimized DML exposure, and leading to a greatly improved voice. The patient denied any speech, swallowing, breathing, or mastication complaints before or after the frenotomy. The frenotomy site healed well without any recurrent ankyloglossia, tongue-tie, tethering, or abnormal scaring when the site was monitored for a year postoperatively. Subsequent phonomicosurgery events in the OR for RRP for this patient were met with similar optimized DML exposure and there was no need for any further frenulum procedures.
Case 2
A 50-year-old male with a history of adult-onset RRP presented to the Vanderbilt Voice Center for care of dysphonia and laryngeal RRP lesions. When the patient was previously taken to the OR, the patient had to be intubated via a video laryngoscope due to difficult laryngeal exposure. Direct laryngoscopy with video-telescopic view provided a challenging view of the AC with manual tongue protrusion and significant anterior laryngeal pressure with use of the Holinger laryngoscope while in suspension. Only the KTP laser under video-telescopic view could be used because of the lack of line-of-sight view of the TVFs through the laryngoscope. A significant amount of RRP burden remained after the case due to suboptimal exposure in the OR. Thereafter, the patient underwent serial in-office KTP laser ablations and a series of benacizumab injections. Due to the eventual persistent burden of TVF RRP with decrement in his voice, it was decided to return the patient to the OR. On a preoperative visit it was noted that the patient had restrictive ankyloglossia with tongue protrusion and elevation but without reported speech, swallow, breathing, or mastication complaints. On inspection of the tongue and floor of mouth, it was noted that the patient had tethering of his tongue by a lingual frenulum formed primarily by a foreshortened mucosal fold. The patient was counseled on the possible improvement of surgical exposure with intraoperative frenotomy. The preoperative airway evaluation with physical examination demonstrated the following: absent mandibular tori, capacity present to protrude lower incisors anterior to the upper incisors, 47 mm maximal incisal opening, modified Mallampati grade 3, 20 mm tongue tip to frenulum length, 12.5 mm frenulum length from floor of mouth to tongue, 46.5 cm neck circumference, body mass index (BMI) of 27, 70° hyroid-mandible angle, 47° neck flexion, 55° neck extension, 2.25 cm preoperative maximum tongue protrusion from lower incisors to tongue tip. The patient was taken to the OR. Intraoperative maximum tongue protrusion from lower incisors to tongue tip, under general anesthesia, was 2.5 cm with manual tongue protrusion (Figure 1). After lingual frenotomy with electrocautery, and with manual tongue protrusion, the maximum tongue protrusion from lower incisors to tongue tip was 3.1 cm. Direct laryngoscopy exposure was substantially improved compared to prior exposures and demonstrated ample bilateral RRP burden (Figure 2). This provided considerably more visualization of the TVFs, allowing for RRP treatment with the GOP laryngoscope. Near total RRP burden was removed from the TVFs with KTP and free-beam CO2 laser under binocular view except a unilateral AC cuff of RRP to prevent further webbing. The patient denied any speech, swallowing, breathing, or mastication complaints after the frenotomy. The frenotomy site healed well without any recurrent ankyloglossia, tongue-tie, tethering, or abnormal scaring when the site was monitored for a year postoperatively. Subsequent phonomicosurgery events in the OR for RRP for this patient were met with similar optimized DML exposure and there was no need for any further frenulum procedures.
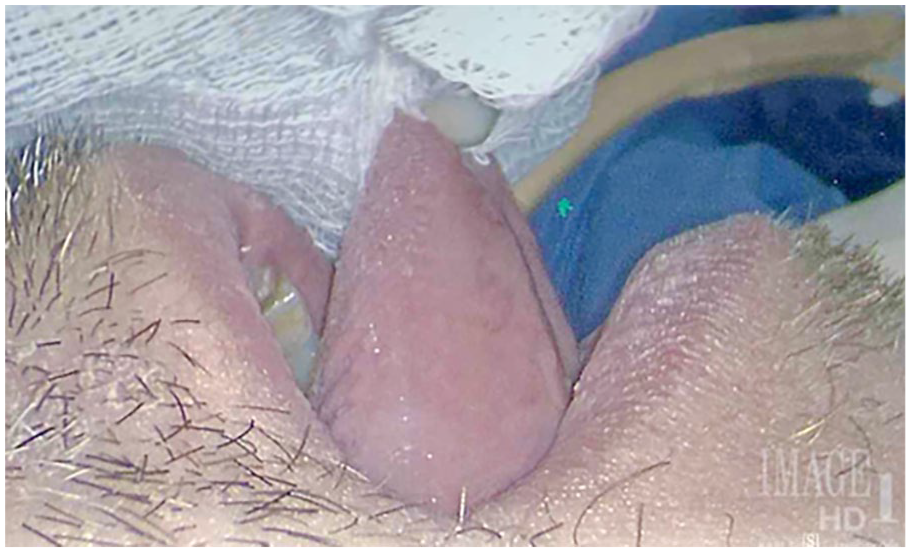
Intraoperative restrictive ankyloglossia with manual tongue protrusion on lateral view.
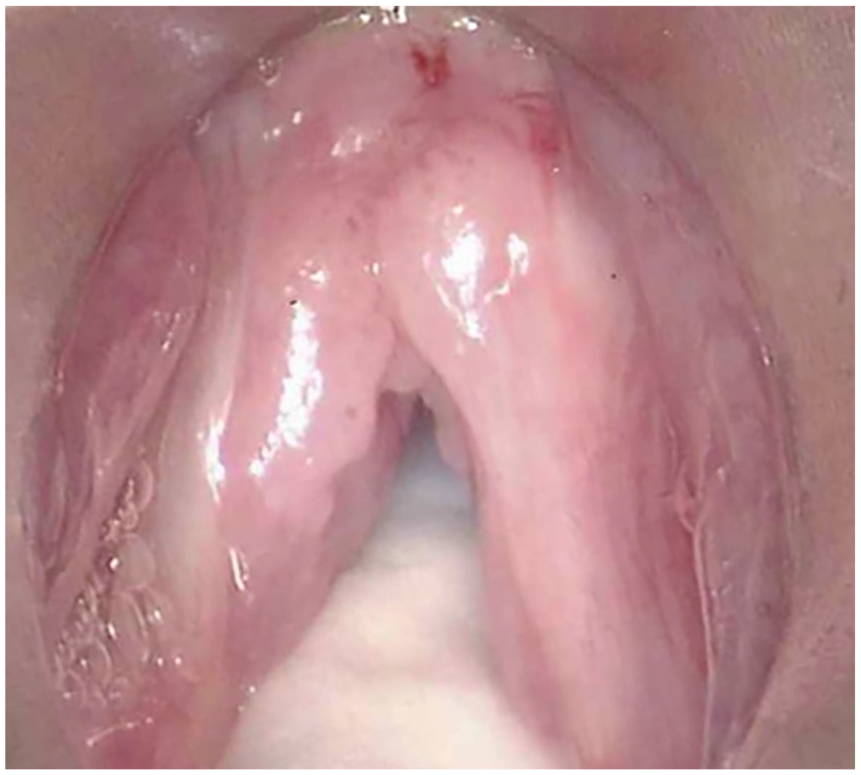
Intraoperative glottic view after frenotomy demonstrating exposure of the disease burden.
Discussion
Some common assessments used to predict difficult airways preoperatively include modified Mallampati score, mandible protrusion, neck mobility, and BMI. Tongue mobility or displacement has also been postulated to be an explanation for difficult endotracheal intubation.2-3 Large mandibular tori can displace the laryngoscope posteriorly or superiorly away from a more preferred pivot point on the oral tongue or base of tongue to prevent proper manipulation of the laryngoscope for optimal glottic exposure. Procedures to reduce mandibular tori have been reported to result in enhanced glottic exposure. 4 These reports suggest that displacement of tongue tissue in the floor of mouth may effect glottic exposure.
It is theorized in this study that lingual frenotomy enhanced direct laryngoscopy exposure with manual tongue protrusion in the OR by way of relocated mass effect of the tongue by enhanced tongue mobility. This allowed for a laryngoscope pivot point that was more conducive for AC view of the glottis. Once the ankyloglossia was rectified by frenotomy, the tongue could then be protruded more in an antegrade fashion. Tongue tissue that once resided in the floor of mouth could now be displaced more anteriorly beyond the lower incisors with manual tongue protrusion. Similarly, tongue tissue that once resided more in the base of tongue could now be rotated more anteriorly into the floor of mouth with manual tongue protrusion and therefore allowed a more anterior pivot point for DML. This is the theorized way lingual frenotomy allowed for DML AC view that once could not be obtained even with anterior laryngeal pressure and manual tongue protrusion.
There are no clear guidelines in the management of ankyloglossia for adult or adolescent patients. It should be noted that in some ankyloglossia cases, restriction of the tongue may be caused by a short mucosal fold, or sometimes by submucosal fascial fibers, and in some cases by the whole complex of mucosa, fascia, and anterior genioglossus muscle fibers (MFGG complex). There are various methods used to treat restrictive ankyloglossia to include frenotomy, frenulectomy, frenuloplasty, Z-plasty, V-Y plasty, and miofrenuloplasty. 5 The best treatment method to address ankyloglossia after a thorough history and physical exam should be considered for each individual patient.
Sleep quality, snoring, speech, swallowing, breathing, or mastication were not reported to be affected upon follow-up visits for both patients. No complications or adverse events were noted in either case. Ankyloglossia, tongue-tie, tethering, or abnormal scaring were not noted after being followed for 1 year postoperatively. These were the only 2 cases that involved frenotomy for direct laryngoscopy exposure that were known to the affiliated institutions. There are no reported cases in the literature that involve lingual frenulum procedures for direct laryngoscopy exposure.
During preoperative airway examination, tongue and floor of mouth examination may show findings of a prominent, short, or tight lingual frenulum with reduced tongue mobility. In our patients, otherwise asymptomatic ankyloglossia appeared to limit access to critical structures of the glottis during laryngoscopy. The cases presented in this study show the first reported instances of frenotomy as a viable option to facilitate glottic exposure in adult patients with inadequate glottic exposure in which ankyloglossia is concomitantly present. In conclusion, lingual frenulum procedures with manual tongue protrusion should be considered in select adult patients with restrictive ankyloglossia affecting optimal direct laryngoscopy exposure.
Footnotes
Authors’ Note
Presented at The Fall Voice Conference, Washington, DC, October 20 to 21, 2023. The views expressed herein are those of the authors and do not reflect the official policy or position of the San Antonio Military Medical Center, the Brooke Army Medical Center, the US Army Medical Department, the US Army Office of the Surgeon General, the Department of the Army, the Department of the Air Force, the Department of Defense, or the US government.
Author Contributions
Each author participated in developing the original concept for the article as well as chart review, data analysis, drafting the article, revisions, and final acceptance.
Data Availability Statement
Data are available through the patient’s electronic medical record and can be accessed through the patient’s providers only.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Statement
The institutions do not require ethical approval for reporting individual cases or case series.
Informed Consent
Informed consent was verbally obtained.
